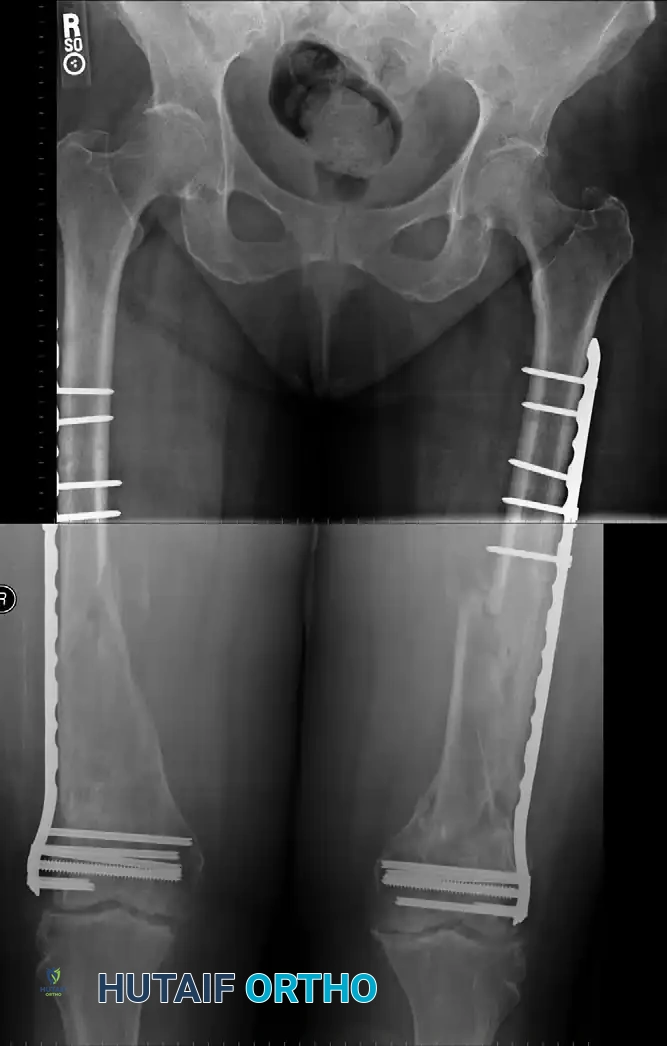
Osteotomy for Femoral Malunion: Comprehensive Surgical Principles
Key Takeaway
Femoral malunion alters lower extremity biomechanics, leading to joint degeneration and functional impairment. Corrective osteotomy aims to restore mechanical alignment, length, and rotation. This comprehensive guide details the surgical principles of femoral osteotomy, including preoperative planning, surgical approaches, and fixation strategies using interlocking intramedullary nails or compression plating. Special considerations for pediatric remodeling and adult biomechanical restoration are also thoroughly examined to optimize postoperative outcomes.
PATHOMECHANICS AND INDICATIONS FOR CORRECTIVE OSTEOTOMY
Femoral malunion is a complex and debilitating sequela of conservatively managed or inadequately stabilized femoral shaft fractures. It presents as a multiplanar deformity encompassing angular (varus/valgus, procurvement/recurvatum), rotational, and translational deviations, frequently accompanied by a clinically significant leg-length discrepancy (LLD).
The primary indication for corrective osteotomy is the restoration of the lower extremity's mechanical axis. A malunited femur shifts the weight-bearing axis, leading to asymmetric loading of the knee and hip joints. For instance, a severe varus malunion shifts the mechanical axis medially, exponentially increasing the contact pressures within the medial compartment of the knee, thereby predisposing the patient to early-onset, accelerated osteoarthritis. Furthermore, rotational malunions—particularly excessive internal or external torsion—alter the patellofemoral tracking mechanics and gait kinematics, leading to anterior knee pain and increased energy expenditure during ambulation.
Preoperative Evaluation and Planning
Meticulous preoperative planning is the cornerstone of a successful corrective osteotomy. The surgeon must precisely quantify the deformity to determine the optimal site and geometry of the osteotomy.
- Clinical Assessment: Evaluate the patient's gait, rotational profile (hip internal/external rotation in extension and flexion), and true leg-length discrepancy using block testing.
- Radiographic Analysis: Full-length, weight-bearing anteroposterior (AP) and lateral radiographs of both lower extremities are mandatory. The mechanical axis deviation (MAD), mechanical lateral distal femoral angle (mLDFA), and mechanical medial proximal femoral angle (mMPFA) must be calculated.
- Advanced Imaging: A computed tomography (CT) scan with rotational cuts (hip, knee, and ankle) is the gold standard for quantifying femoral version and rotational malalignment.
- CORA Principles: The Center of Rotation of Angulation (CORA) must be identified. The ideal osteotomy corrects the deformity exactly at the site of the fracture (the CORA). If the osteotomy is performed at a level different from the CORA, a compensatory translation must be incorporated into the surgical correction to realign the mechanical axis.
Clinical Pearl: While rotational deformity does not remodel significantly, it is usually well tolerated by the patient and rarely requires isolated surgical treatment unless it exceeds 15 to 20 degrees and causes symptomatic gait disturbances or patellofemoral instability.
PEDIATRIC CONSIDERATIONS AND REMODELING POTENTIAL
The approach to femoral malunion in the pediatric population differs drastically from that in adults due to the robust remodeling potential of the immature skeleton. The physis possesses a remarkable ability to correct angular deformities over time, guided by the principles of the Hueter-Volkmann law.
In children younger than 13 years of age, a malunion of up to 25 degrees in any plane typically remodels sufficiently to restore normal alignment of the joint surfaces. Because of this profound remodeling capacity, surgical intervention should be approached with caution and patience.
If a significant angular deformity persists after fracture union, corrective osteotomy should be delayed for at least 1 year, allowing the natural biological remodeling process to occur, unless the deformity is exceptionally severe and immediately impairs function.
Age-Specific Osteotomy Strategies
- Juvenile Patients: In younger children where the deformity is near the joint, a metaphyseal osteotomy of the proximal or distal femur may be preferable to a diaphyseal cut, as metaphyseal bone heals more rapidly and the correction can be placed closer to the joint line.
- Adolescent Patients: In older children and adolescents presenting with midshaft deformities, a diaphyseal osteotomy followed by rigid fixation with an interlocking intramedullary nail is the preferred technique, mirroring adult principles.
Clinical Case Example: Pediatric Femoral Malunion
The following imaging demonstrates the natural history and surgical management of a severe pediatric femoral malunion.

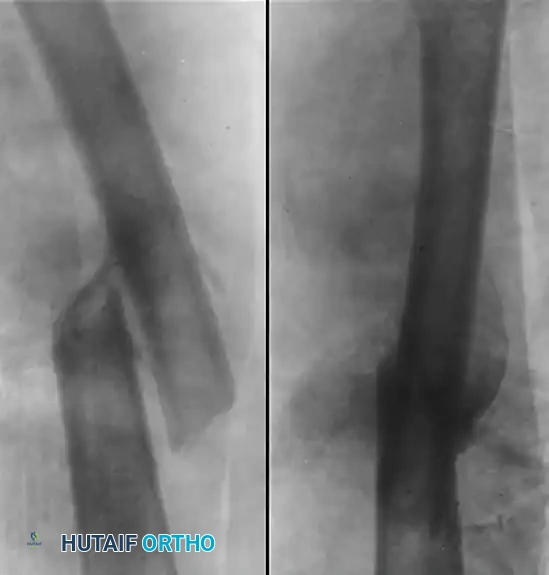
Figure A: Demonstrates a severely malunited fracture of the femur with significant overlapping of fragments and angular deformity in an 11-year-old boy. At this degree of shortening and angulation, spontaneous remodeling alone is insufficient to restore normal biomechanics.
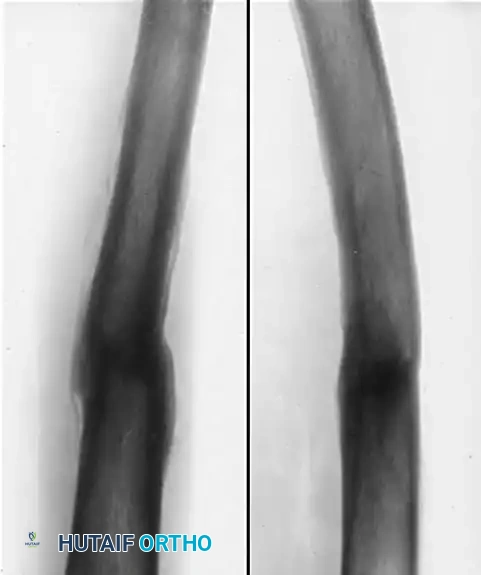
Figure B: Radiographic appearance five months after open reduction and corrective osteotomy. The procedure involved the insertion of a Kirschner wire through the distal femur and the application of a spica cast incorporating the wire to maintain length and alignment. Through this intervention, the length of the limb and the functional mechanics of the knee were successfully regained, allowing subsequent growth to finalize the remodeling process.
SURGICAL ANATOMY AND PATIENT POSITIONING
For diaphyseal femoral osteotomies, the patient is typically positioned supine on a radiolucent fracture table or a flat Jackson table, depending on the planned fixation method (intramedullary nail vs. plate). If an antegrade intramedullary nail is planned, the torso is adducted to allow unimpeded access to the piriformis fossa or greater trochanter.
The Surgical Approach
After determining the precise site of the osteotomy preoperatively, the area of malunion is exposed through an appropriate anterolateral or lateral incision.
- Lateral Approach: The incision is made along the line connecting the greater trochanter to the lateral epicondyle. The fascia lata is incised, and the vastus lateralis is elevated from the lateral intermuscular septum. Perforating branches of the profunda femoris artery must be meticulously identified, ligated, or cauterized to prevent postoperative hematoma.
- Anterolateral Approach: Utilizes the internervous plane between the rectus femoris (femoral nerve) and the vastus lateralis (femoral nerve). This approach provides excellent exposure to the anterior and lateral aspects of the femoral shaft.
SURGICAL TECHNIQUE: STEP-BY-STEP OSTEOTOMY
1. Periosteal Exposure and Preparation
Once the malunion site is reached, incise the periosteum longitudinally for a distance of 6 to 8 cm. This extensive exposure is particularly necessary if interlocking nail techniques are to be utilized over the area of maximal deformity, ensuring adequate visualization for the osteotomy and subsequent hardware placement. Meticulous subperiosteal dissection should be performed to preserve the osteogenic cambium layer, which is vital for postoperative bone healing.
2. Executing the Osteotomy Cut
The method of dividing the bone depends on the density of the callus and the geometry of the planned correction.
- Motorized Saw Technique: Divide the bone transversely with a reciprocating or oscillating motor saw under continuous saline irrigation to prevent thermal necrosis of the bone ends.
- Drill and Osteotome Technique (Preferred for Dense Bone): If preferable, or if the malunion callus is highly sclerotic, drill several holes transversely through the bone using a 2.5 mm or 3.2 mm drill bit. Divide the bone in the plane of the holes with a sharp osteotome to form broad, even surfaces for maximal apposition.
Surgical Pearl: Drilling multiple holes not only ensures that the osteotomy is perfectly transverse, but also—because the malunited femur is often exceedingly dense and sclerotic—saves operative time, decreases the physical effort required of the surgeon, and significantly mitigates the risk of thermal necrosis associated with prolonged saw use.
3. Deformity Correction and Canal Preparation
Once the osteotomy is complete, correct the deformity by manual force. This may require the release of contracted soft tissues, particularly the linea aspera or the fascia lata, depending on the chronicity of the malunion.
Next, open the medullary canal of both the proximal and distal fragments. In long-standing malunions, the medullary canal is frequently obliterated by dense endosteal bone. Use rigid reamers, curettes, or a cannulated drill over a guide wire to meticulously recanalize the medullary space, ensuring that the anatomical axis of both fragments is restored.
4. Internal Fixation Strategies
In adults, the reduction of a femoral osteotomy is inherently unstable, especially in the proximal half of the femur where powerful muscle forces (e.g., iliopsoas, gluteus medius, adductors) exert deforming vectors. End-to-end apposition and proper alignment of the fragments can be maintained with certainty only by rigid internal fixation.
Option A: Interlocking Intramedullary Nailing (Gold Standard)
Use an interlocking intramedullary nail within the levels ordinarily indicated for intramedullary nailing of fresh fractures of the femoral shaft.
* Pass a ball-tipped guide wire down the reamed proximal fragment, across the osteotomy site, and into the distal fragment, centering it in the distal epiphysis.
* Sequentially ream the canal to 1.0 mm to 1.5 mm larger than the planned nail diameter.
* Insert the nail and secure it with proximal and distal interlocking screws to control rotation and maintain length. The intramedullary nail acts as a load-sharing device, positioned close to the mechanical axis, which biomechanically favors early weight-bearing and secondary bone healing.
Option B: Compression Plating
Alternatively, the fragments can be fixed with a heavy-duty broad dynamic compression plate (DCP) or a locking compression plate (LCP). Plating is particularly useful for periarticular malunions (where an IM nail would not provide sufficient distal or proximal purchase) or when the medullary canal is completely obliterated and cannot be safely reamed. The plate should be applied to the tension band side of the femur (typically lateral) and secured with a minimum of eight cortices of fixation above and below the osteotomy.
5. Bone Grafting
Regardless of the fixation method chosen, the biological environment of an osteotomy site in a malunited bone is often compromised due to sclerosis and diminished local vascularity. Therefore, cancellous bone grafts should be placed circumferentially at the osteotomy site. Autologous bone graft (harvested from the iliac crest or utilizing the reamings from the medullary canal) provides the optimal triad of osteogenesis, osteoinduction, and osteoconduction required to ensure rapid and robust union.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The postoperative rehabilitation protocol is dictated by the stability of the fixation achieved intraoperatively.
- Intramedullary Nailing: If rigid interlocking intramedullary fixation is achieved, patients are typically allowed immediate toe-touch or partial weight-bearing (10-15 kg) with crutches or a walker. Active and active-assisted range of motion (ROM) exercises for the hip and knee are initiated on postoperative day one to prevent arthrofibrosis and muscle atrophy.
- Compression Plating: If plate fixation is utilized, weight-bearing is generally restricted to toe-touch for the first 6 to 8 weeks, or until radiographic evidence of bridging callus is observed.
- Radiographic Monitoring: Serial radiographs (AP and lateral) are obtained at 2, 6, 12, and 24 weeks postoperatively to monitor the progression of bone healing and the maintenance of the mechanical alignment. Progression to full weight-bearing is permitted once radiographic union is confirmed.
COMPLICATIONS AND PITFALLS
Surgeons undertaking corrective osteotomies for femoral malunion must be prepared to manage several potential complications:
- Nonunion or Delayed Union: The sclerotic nature of the malunion site increases the risk of nonunion. Meticulous decortication, rigid fixation, and the liberal use of autologous cancellous bone graft are critical preventative measures.
- Hardware Failure: Premature weight-bearing in the presence of delayed union can lead to fatigue failure of the intramedullary nail or plate.
- Neurovascular Injury: Aggressive soft tissue retraction or errant drill bit placement can injure the profunda femoris artery or the sciatic nerve. Careful adherence to anatomical internervous planes is mandatory.
- Infection: As with any major open orthopedic procedure, deep surgical site infection is a catastrophic complication. Strict aseptic technique, prophylactic intravenous antibiotics, and meticulous soft tissue handling are imperative.
By adhering to strict biomechanical principles, executing precise preoperative planning, and employing rigid internal fixation, the orthopedic surgeon can successfully correct femoral malunions, thereby restoring limb length, optimizing joint kinematics, and significantly improving the patient's functional quality of life.
You Might Also Like