Revascularization and Replantation of the Digits
Introduction and Epidemiology
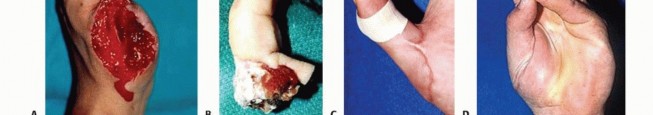
Replantation is strictly defined as the surgical reattachment of a completely amputated body part, a procedure intrinsically dependent upon the precise restoration of arterial inflow and venous outflow to ensure the survival of the appendage. Revascularization, conversely, refers to the restoration of circulation and the comprehensive repair of all injured structures in an incompletely amputated, dysvascular body part. By definition, revascularization mandates the microscopic repair of blood vessels to reestablish blood flow to an ischemic, yet partially attached, segment. Revision amputation is the definitive ablative procedure performed at the level of amputation to obtain durable soft tissue coverage, optimize residual limb length, and address concomitant injuries when replantation is deemed physiologically inappropriate, technically impossible, or functionally detrimental.

The clinical algorithm dictating the choice between replantation, revascularization, or revision amputation is highly multifactorial. It requires a rapid, comprehensive assessment of patient demographics, physiological reserve, mechanism of injury, ischemia time, and the specific functional demands of the patient. The historical foundation of this field was laid by Malt and McKhann, who performed the first successful replantation of a human limb in 1962. This was followed shortly by the landmark achievement of Komatsu and Tamai in 1968, who executed the first successful microvascular replantation of a completely amputated digit. Since these pioneering efforts, continuous advancements in operating microscopes, precision microsurgical instruments, and ultra-fine monofilament sutures have elevated digit replantation to a standard, albeit highly technically demanding, procedure within the armamentarium of hand and upper extremity surgery.

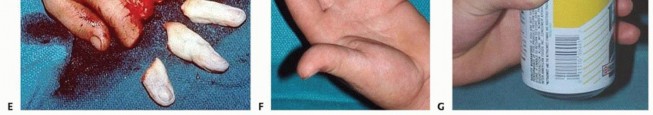
Epidemiologically, digit amputations exhibit a strong predilection for young, working-age males, frequently occurring secondary to high-energy occupational hazards involving power saws, industrial presses, or heavy mechanical doors. Mechanisms of injury are broadly stratified into guillotine (sharp), crush, and avulsion injuries. Guillotine amputations yield the most favorable prognosis for replantation due to the highly localized nature of the tissue damage. In stark contrast, crush and avulsion injuries impart a severe, longitudinal "zone of injury" that extends far proximal and distal to the visible wound margins. This extensive intimal and soft tissue trauma drastically increases the complexity of the microvascular reconstruction and exponentially raises the risk of postoperative microvascular thrombosis.
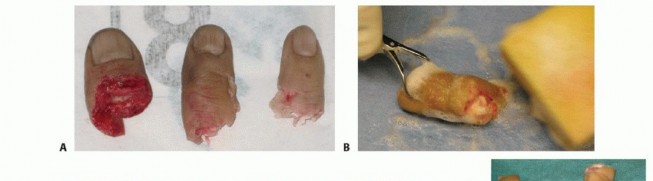
The economic and psychological burden of digit amputation is profound. The loss of a digit, particularly the thumb or multiple digits, results in a significant decrement in grip strength, pinch kinematics, and fine motor dexterity. The primary goal of replantation is not merely the survival of the amputated part, but the restoration of a functional, sensate, and pain-free digit that contributes to the overall utility of the hand. The pathophysiology of ischemia-reperfusion injury plays a critical role in the success or failure of these procedures. Prolonged ischemia leads to the depletion of intracellular adenosine triphosphate, failure of the sodium-potassium pump, and subsequent cellular swelling. Upon reperfusion, the sudden influx of oxygen generates reactive oxygen species, leading to endothelial damage, microvascular thrombosis, and the no-reflow phenomenon. Understanding these cellular mechanisms is paramount for managing ischemia times and optimizing postoperative pharmacological protocols.
Surgical Anatomy and Biomechanics
An intimate, three-dimensional understanding of the anatomy over the complete length of the digit is the cornerstone of successful replantation and revascularization. The anatomical configuration of the thumb is fundamentally distinct from that of the four lesser digits, dictating specific surgical approaches for exposure, skeletal fixation, and soft tissue repair.
Fascial Structures and Ligaments
The palmar and dorsal cutaneous ligaments are critical for maintaining the position of the neurovascular bundle during the dynamic range of motion of the digit. The Grayson ligament is situated palmar to the neurovascular bundle; it originates from the volar aspect of the fibro-osseous flexor tendon sheath and inserts onto the overlying palmar skin. Conversely, the Cleland ligament travels dorsal to the neurovascular bundle, extending robustly from the lateral aspect of the phalanx to the overlying lateral integument. Recognizing and preserving these ligaments is critical during microsurgical dissection, as the proper digital neurovascular bundles are reliably localized in the intervening space between them.

Arterial Anatomy and Dominance
The arterial supply to the digits is derived from the superficial and deep palmar arches, which give rise to the common digital arteries. At the level of the metacarpophalangeal joint, these bifurcate into the proper digital arteries. A fundamental concept in digital microvascular surgery is arterial dominance. For the index and middle fingers, the ulnar proper digital artery is typically dominant, whereas for the ring and small fingers, the radial proper digital artery is dominant. The thumb receives its primary supply from the princeps pollicis artery, which branches into the ulnar and radial proper digital arteries of the thumb. During replantation, restoring flow through the dominant artery is preferred, although anastomosing both arteries, when technically feasible, significantly improves survival rates and cold tolerance.
Venous Drainage Systems
Venous drainage of the digits is highly asymmetric, relying predominantly on the dorsal venous network. The volar venous system is relatively diminutive and less reliable for primary venous outflow reconstruction. The dorsal veins coalesce into larger venous channels proximal to the proximal interphalangeal joint. A critical anatomical consideration is the thin-walled, fragile nature of these dorsal veins, which makes them highly susceptible to desiccation and iatrogenic injury during dissection. Successful replantation mandates meticulous identification and preservation of these dorsal veins, with a general surgical principle advocating the repair of two veins for every one artery anastomosed to prevent postoperative venous congestion.
Neurologic Anatomy
Sensory innervation to the digits is provided by the proper digital nerves, which travel in the neurovascular bundle volar to the proper digital arteries. Proximal to the distal interphalangeal joint, the proper digital nerves give off dorsal branches that supply sensation to the dorsal skin and nail bed. The proper digital nerves are characterized by a well-defined epineurium and distinct fascicular architecture, which facilitates precise microsurgical coaptation. Restoration of protective sensation is a primary functional goal of replantation; failure to achieve adequate nerve regeneration results in a blind, insensate appendage that patients frequently bypass during functional tasks, rendering the replantation functionally obsolete.

Indications and Contraindications
The decision to proceed with replantation versus revision amputation requires rigorous clinical judgment. The surgeon must balance the technical feasibility of the procedure against the anticipated functional outcome and the physiological cost to the patient. The indications for replantation have evolved significantly, moving away from a purely survival-based paradigm to one focused heavily on long-term functional utility.
Absolute Indications
Absolute indications for replantation represent clinical scenarios where the functional deficit of amputation is so profound that the extensive surgical effort is unequivocally justified. The thumb is the most critical digit, contributing approximately forty to fifty percent of total hand function through its role in opposition, pinch, and grasp. Therefore, thumb amputations at any level are considered an absolute indication for replantation. Multiple digit amputations also constitute an absolute indication to preserve the biomechanical width of the palm and maintain a functional grasp. Amputations in children are universally attempted due to their superior regenerative capacity, neuroplasticity, and excellent long-term functional outcomes. Finally, single digit amputations distal to the insertion of the flexor digitorum superficialis (Zone I) are generally indicated, as the replanted digit typically regains excellent motion at the proximal interphalangeal joint and provides critical length for pinch kinematics.
Relative Indications and Contraindications
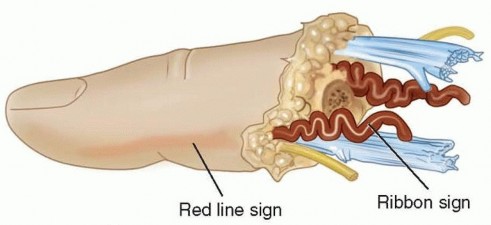
Relative indications include single digit amputations in Zone II (proximal to the flexor digitorum superficialis insertion). Historically, replantation in this zone was discouraged due to the high incidence of flexor tendon adhesions and resultant stiffness, leading to the moniker "no man's land." However, advancements in flexor tendon rehabilitation protocols and tenolysis techniques have made Zone II replantations viable in highly selected patients, particularly those with specific occupational demands or strong aesthetic concerns.
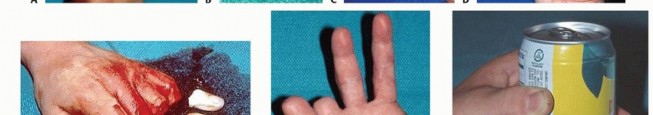
Absolute contraindications are primarily dictated by patient safety and the physiological limits of tissue survival. Prolonged warm ischemia time exceeding twelve hours for digits with muscle tissue, or severe crush and avulsion injuries where the vascular intima is destroyed over a long segment, preclude successful replantation. Concomitant life-threatening injuries (e.g., severe traumatic brain injury, massive hemorrhage) mandate damage control orthopedics, rendering lengthy microvascular procedures contraindicated. Relative contraindications include severe psychiatric illness, medical non-compliance, and heavy tobacco use, as nicotine-induced vasospasm drastically increases the rate of microvascular thrombosis.
Indications and Contraindications Summary
| Category | Replantation/Revascularization Criteria |
|---|---|
| Absolute Indications | Thumb amputations (any level) |
| Multiple digit amputations | |
| Amputations in pediatric patients | |
| Single digit amputation in Zone I (distal to FDS insertion) | |
| Amputations through the palm, wrist, or forearm (macro-replantation) | |
| Relative Indications | Single digit amputation in Zone II (patient-specific) |
| Ring avulsion injuries (depending on classification/vascular status) | |
| Bilateral amputations | |
| Absolute Contraindications | Concomitant life-threatening polytrauma |
| Severe crush/avulsion with non-reconstructable vessels | |
| Prolonged warm ischemia (>12 hours for digits, >6 hours for major limb) | |
| Physiologically unstable patient | |
| Relative Contraindications | Severe systemic illness (e.g., advanced peripheral vascular disease) |
| Heavy tobacco use / nicotine dependence | |
| Severe psychiatric instability or inability to comply with rehabilitation | |
| Extreme contamination |
Pre Operative Planning and Patient Positioning
The success of a microvascular replantation begins long before the patient enters the operating theater. The initial management of the amputated part and the physiological optimization of the patient are critical determinants of microvascular patency and tissue survival.
Ischemia Time and Part Preservation
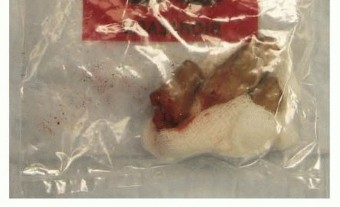
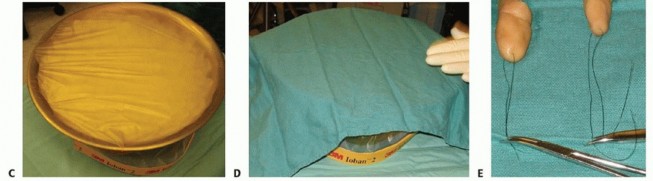
The tolerance of tissue to ischemia is directly proportional to its metabolic rate and muscle content. Digits, lacking substantial muscle bellies, can tolerate up to twelve hours of warm ischemia and up to twenty-four hours of cold ischemia. Conversely, major limb amputations containing significant muscle mass are limited to approximately six hours of warm ischemia. The amputated part must be handled meticulously. It should be wrapped in saline-moistened gauze, placed inside a sealed, watertight plastic bag, and then immersed in an ice-water slurry. Direct contact between the amputated tissue and ice must be strictly avoided to prevent irreversible frostbite and cellular lysis.

Anesthetic Considerations
The choice of anesthesia significantly impacts the microvascular environment. Continuous regional anesthesia, such as an axillary or supraclavicular brachial plexus block, is heavily favored over general anesthesia. Regional blocks provide an essential sympathectomy effect, inducing profound peripheral vasodilation, maximizing arterial inflow, and mitigating vasospasm. Furthermore, regional anesthesia provides excellent postoperative analgesia, reducing the release of endogenous catecholamines associated with pain, which can otherwise trigger detrimental peripheral vasoconstriction. If general anesthesia is required due to patient anxiety or anticipated prolonged operative duration, supplemental regional blocks or continuous peripheral nerve catheters should be strongly considered.
Operating Room Setup and Tourniquet Management
Patient positioning must optimize surgeon ergonomics, given the prolonged duration of microvascular procedures. The patient is positioned supine with the affected extremity extended on a radiolucent hand table. A pneumatic tourniquet is applied to the upper arm. Tourniquet time must be managed judiciously; while a bloodless field is essential for the initial macroscopic debridement and skeletal fixation, the tourniquet must be deflated prior to microvascular anastomosis to assess the adequacy of proximal arterial flow (the "spurt test") and to prevent prolonged ischemic injury to the proximal stump. The operating microscope is positioned opposite the primary surgeon, ensuring a clear line of sight and unimpeded access for the assistant.

Detailed Surgical Approach and Technique
The surgical sequence for digit replantation follows a highly structured, logical progression designed to establish a stable skeletal foundation before proceeding with delicate soft tissue and microvascular repairs. The standard sequence is: 1) Identification and tagging of structures, 2) Debridement, 3) Skeletal shortening and fixation, 4) Extensor tendon repair, 5) Flexor tendon repair, 6) Arterial anastomosis, 7) Nerve coaptation, 8) Venous anastomosis, and 9) Skin coverage.
Debridement and Structure Identification
The procedure commences with simultaneous, two-team preparation if possible—one team preparing the amputated part on a back table while the other prepares the proximal stump. Radical debridement of all non-viable, crushed, or contaminated tissue is paramount. Under loupe magnification, the neurovascular bundles, flexor tendons, and extensor tendons are systematically identified. The proper digital arteries and nerves are carefully dissected free from the surrounding adventitia and perineurium. Small vascular clips or fine sutures are used to tag these structures to facilitate rapid identification under the operating microscope.
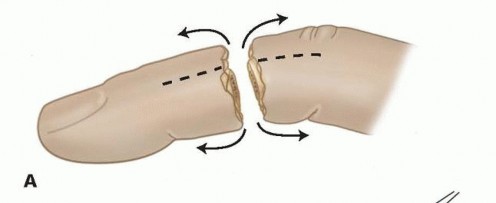
Skeletal Shortening and Fixation
Skeletal shortening is a non-negotiable principle in replantation surgery. Shortening the phalanx by 5 to 10 millimeters is essential to allow for tension-free repair of the neurovascular structures and primary closure of the skin. Attempting to maintain native length in the setting of segmental soft tissue loss inevitably leads to anastomotic tension, vasospasm, and subsequent failure. Following shortening with an oscillating saw, rigid skeletal fixation is achieved. The choice of fixation depends on the level of amputation and fracture geometry. Longitudinal or crossed Kirschner wires (K-wires) provide rapid, effective fixation and are the most commonly employed modality. Intraosseous wiring (e.g., 90-90 wiring) or mini-fragment plates and screws may be utilized for transverse diaphyseal amputations to provide absolute stability and facilitate early active motion.

Extensor and Flexor Tendon Reconstruction
Following skeletal stabilization, the extensor mechanism is repaired. A robust repair using a figure-of-eight or modified Kessler technique with 4-0 or 5-0 non-absorbable suture is performed. Repairing the extensor tendon early adds secondary stability to the skeletal fixation and prevents volar subluxation of the digit.
The flexor tendon repair is technically demanding, particularly in Zone II. The flexor digitorum profundus is repaired using a multi-strand core suture technique (e.g., 4-strand or 6-strand cruciate) with a 3-0 or 4-0 braided synthetic suture, augmented by a running epitendinous repair using 6-0 monofilament. The flexor sheath and critical pulleys (A2 and A4) must be preserved or reconstructed to prevent bowstringing. If the flexor digitorum superficialis is severely damaged, it may be excised to reduce bulk within the fibro-osseous canal and facilitate smooth gliding of the profundus tendon.
Microvascular Arterial Anastomosis
The operating microscope is introduced for the vascular and neural repairs. The proximal arterial stump is assessed for pulsatile flow. If flow is inadequate, the vessel must be resected proximally until healthy, uninjured intima is encountered. The adventitia is aggressively stripped from the vessel ends to prevent thrombogenic material from entering the lumen. The vessel ends are gently dilated using micro-vessel dilators.
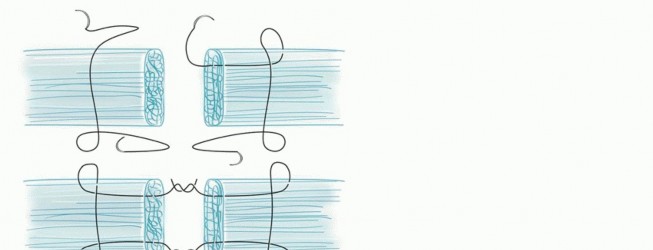
Anastomosis is typically performed using 9-0 or 10-0 nylon on a spatulated micro-needle. The standard technique involves placing two stay sutures at 120-degree intervals to triangulate the vessel, preventing accidental suturing of the back wall. Alternatively, the back-wall-first technique may be employed in tight spaces. If a tension-free primary anastomosis is impossible due to the extent of the zone of injury, reversed interpositional vein grafts—typically harvested from the volar forearm or dorsal foot—must be utilized. Attempting to bridge a gap under tension is the most common technical error leading to replantation failure.

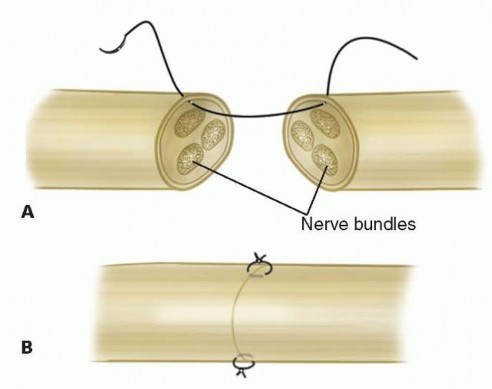
Nerve Coaptation
Following arterial reperfusion, the digit should immediately become pink, and capillary refill should be brisk. The proper digital nerves are then repaired. Precise fascicular alignment is critical for optimal sensory recovery. An epineurial repair is performed using 8-0 or 9-0 nylon sutures. If a segmental nerve defect exists, primary repair should not be forced; instead, nerve grafting or the use of a nerve conduit should be considered, though primary shortening of the bone often mitigates the need for nerve grafts.
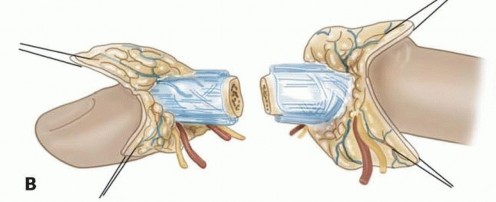
Venous Anastomosis and Soft Tissue Coverage
Venous anastomosis is frequently the most challenging aspect of the procedure due to the thin, friable nature of the dorsal veins. The digit is turned, and the dorsal veins are mobilized. As a general rule, two veins should be repaired for every artery anastomosed to ensure adequate outflow and prevent venous congestion. The technique is similar to arterial anastomosis, utilizing 10-0 or
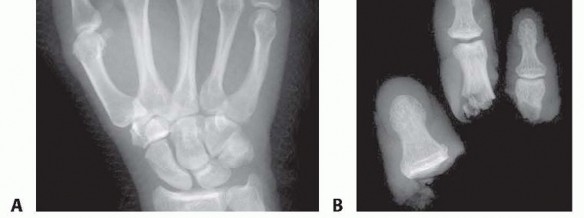
Clinical & Radiographic Imaging
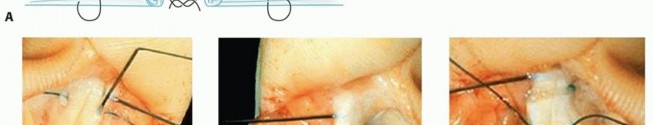
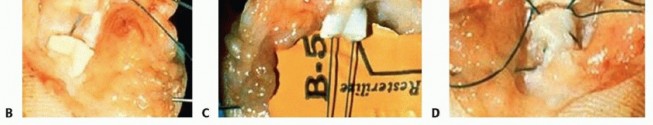
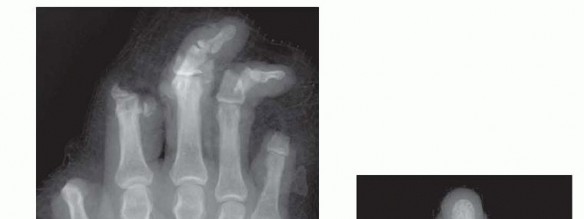
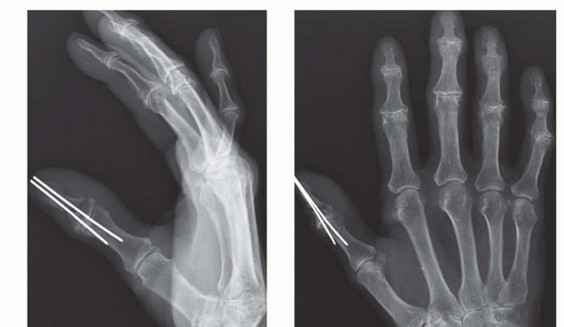
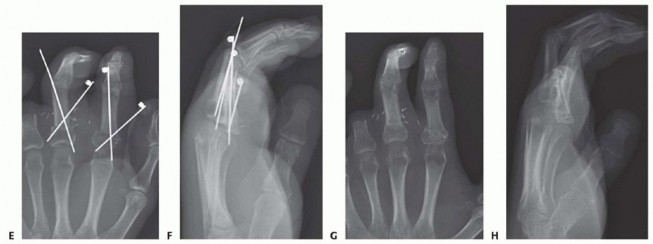
You Might Also Like

