Radial Nerve Palsy Tendon Transfers: An Intraoperative Masterclass

Key Takeaway
Welcome, fellows, to an immersive surgical masterclass on tendon transfers for radial nerve palsy. We'll meticulously restore wrist, finger, and thumb extension, covering detailed anatomy, preoperative planning, and granular intraoperative execution. Learn precise donor harvest, optimal tensioning, and crucial neurovascular protection to achieve excellent functional outcomes for our patients.
Comprehensive Introduction and Patho-Epidemiology
The profound functional deficit resulting from radial nerve palsy represents one of the most debilitating peripheral nerve injuries encountered in orthopedic and hand surgery. The hallmark "wrist drop" is not merely an aesthetic deformity; it fundamentally dismantles the biomechanical foundation of the hand. Without active wrist extension, the flexor tendons lose their mechanical advantage, operating at the extreme shortened end of their length-tension curve. Consequently, grip strength is reduced by up to seventy-five percent, rendering the hand virtually useless for powerful prehension or fine motor manipulation. The inability to extend the metacarpophalangeal (MCP) joints and the thumb further compromises the hand's ability to open and accept objects, effectively eliminating the patient's independence in activities of daily living.
Epidemiologically, radial nerve injuries most frequently arise in the setting of humeral shaft fractures, particularly those involving the middle and distal thirds (the classic Holstein-Lewis fracture). The nerve's intimate application to the posterior humerus in the spiral groove makes it uniquely vulnerable to traction, contusion, or laceration by sharp fracture fragments. Iatrogenic injuries also account for a significant proportion of cases, often occurring during open reduction and internal fixation of the humerus, lateral elbow surgical approaches, or even from prolonged tourniquet application. Penetrating trauma, gunshot wounds, and severe crush injuries to the upper extremity represent other common etiologies, often resulting in more severe, structurally disruptive nerve lesions (Sunderland Grade IV or V) that possess a poorer prognosis for spontaneous recovery.
The pathophysiology of the nerve injury dictates the timeline and algorithm for intervention. Neurapraxic injuries, characterized by focal demyelination without axonal disruption, typically recover spontaneously within weeks to a few months. Axonotmetic injuries, where the axon is disrupted but the endoneurial tubes remain intact, recover at a predictable rate of approximately one millimeter per day. However, if the distance from the zone of injury to the target motor endplates is excessively long, irreversible muscle atrophy and motor endplate fibrosis may occur before the regenerating axons can reinnervate the muscle. This temporal constraint is the critical factor driving the decision-making process for tendon transfers.
Historically, the management of irreversible radial nerve palsy relied exclusively on static splinting, which, while preventing contractures, failed to restore dynamic function. The evolution of tendon transfers has revolutionized the treatment paradigm. The goal is no longer simply to tether the wrist in a functional position, but to meticulously rebalance the hand by reallocating expendable, synergistic muscle-tendon units to replace the lost functions of wrist extension, finger extension, and thumb extension/abduction. This requires a profound understanding of excursion, work capacity, and the complex biomechanics of the forearm and hand.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of the radial nerve's intricate course and the musculature it innervates is paramount before any surgical intervention is contemplated. The radial nerve, a direct continuation of the posterior cord of the brachial plexus (C5-T1), embarks on a journey through the posterior compartment of the upper arm, supplying the triceps brachii. As it spirals distally, it pierces the lateral intermuscular septum to enter the anterior compartment, descending between the brachialis and brachioradialis muscles. This anatomical relationship is critical during surgical exploration of the distal humerus or proximal forearm.
Within the proximal forearm, the radial nerve typically divides into its two terminal branches: the superficial radial nerve (SRN), which is purely sensory, and the deep radial nerve (DRN), which transitions into the posterior interosseous nerve (PIN) after passing beneath the fibrous arch of the supinator muscle (the Arcade of Frohse). The innervation sequence of the radial nerve is highly predictable and orderly, occurring in a proximal-to-distal fashion. This sequence is a vital diagnostic tool; the presence or absence of specific muscle function allows the clinician to precisely localize the level of the nerve lesion.
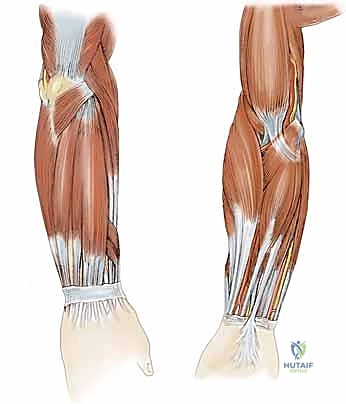
The proximal radial nerve proper innervates the brachioradialis (BR), a powerful elbow flexor, followed by the extensor carpi radialis longus (ECRL), a primary wrist extensor and radial deviator. The extensor carpi radialis brevis (ECRB), the central workhorse of wrist extension, often receives dual innervation from both the proper radial nerve and the PIN. Once the PIN exits the supinator, it sequentially innervates the extensor digitorum communis (EDC), extensor carpi ulnaris (ECU), extensor digiti minimi (EDM), abductor pollicis longus (APL), extensor pollicis brevis (EPB), extensor pollicis longus (EPL), and the extensor indicis proprius (EIP). Understanding this sequence is crucial for distinguishing a high radial nerve palsy (affecting the BR, ECRL, and all distal muscles) from a pure PIN palsy (which spares the BR and ECRL, resulting in a radially deviated wrist extension but loss of digit extension).
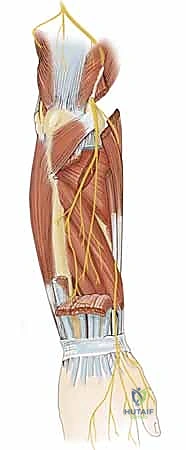
From a biomechanical perspective, successful tendon transfer relies on matching the physiological properties of the donor muscle to the functional requirements of the recipient. The two most critical parameters are excursion (amplitude of tendon travel) and work capacity (cross-sectional area). The wrist extensors require approximately 3 to 4 centimeters of excursion, while the digital extensors require 5 to 7 centimeters. The pronator teres (PT), with an excursion of roughly 3 centimeters, is an ideal biomechanical match for the ECRB. Conversely, transferring a muscle with inadequate excursion to the digital extensors will result in a tenodesis effect, where full finger extension is only possible with simultaneous wrist flexion.
Throughout these procedures, the surgeon must remain exquisitely aware of critical neurovascular structures. The radial artery runs along the radial aspect of the forearm and is vulnerable during volar radial approaches for PT or flexor carpi radialis (FCR) harvest. The superficial radial nerve (SRN) emerges from beneath the brachioradialis in the distal third of the forearm; injury to this sensory nerve can lead to a devastating, recalcitrant neuroma that may overshadow the functional gains of the transfer. Furthermore, the anterior interosseous nerve (AIN) and ulnar neurovascular bundle must be protected during the harvest of deep volar flexors or the flexor carpi ulnaris (FCU).
Exhaustive Indications and Contraindications
The decision to proceed with tendon transfer surgery for radial nerve palsy is highly nuanced, requiring a careful assessment of the injury timeline, the patient's physiological status, and the likelihood of spontaneous or surgically assisted nerve recovery. Tendon transfers are primarily indicated when there is a documented, irreversible loss of radial nerve motor function. This is typically established after a period of observation (usually 12 to 18 months) during which serial clinical examinations and electrodiagnostic studies (EMG/NCS) fail to demonstrate progressive reinnervation.
However, the paradigm has shifted in recent years, with an increasing role for "early" or "internal splint" tendon transfers. In cases of massive nerve trauma where the gap precludes primary repair, or in elderly patients where the rate of nerve regeneration is predictably poor, an early PT to ECRB transfer can immediately restore wrist extension. This eliminates the need for cumbersome external splinting, improves grip strength immediately, and facilitates the rehabilitation of concurrent nerve repairs or nerve transfers. Early transfers are also indicated in patients who are intolerant of splinting or whose livelihood demands a rapid return to functional capacity.
Before embarking on tendon transfers, several absolute prerequisites must be met. The patient must possess full, unrestricted passive range of motion in the wrist, MCP, and interphalangeal joints. Tendon transfers lack the power to overcome fixed joint contractures; any stiffness must be aggressively managed preoperatively with serial casting or dynamic splinting, or addressed intraoperatively with capsulotomies. Furthermore, the selected donor muscles must be of normal or near-normal strength (Medical Research Council [MRC] Grade 4 or 5). Transferring a weakened muscle will inevitably lead to a failed outcome, as the muscle will lose approximately one grade of strength following the transfer.
Contraindications to tendon transfer include severe, unmanageable joint contractures, lack of available or adequately strong donor muscles (as seen in severe brachial plexus injuries or multi-trauma), and severe cognitive impairment or lack of patient compliance. The postoperative rehabilitation protocol is demanding, requiring the patient to actively participate in motor re-education to achieve cortical remapping. If a patient cannot comprehend or adhere to the strict postoperative splinting and therapy regimens, the transferred tendons are at a high risk of rupture or severe adhesion formation.
| Variable | Favorable Indication for Transfer | Relative/Absolute Contraindication |
|---|---|---|
| Time from Injury | > 12-18 months with no clinical/EMG recovery | < 3 months (unless early internal splinting planned) |
| Passive Joint ROM | Supple, full passive extension of wrist/digits | Fixed flexion contractures of wrist or MCP joints |
| Donor Muscle Strength | MRC Grade 5 (Normal) | MRC Grade 3 or less |
| Tissue Bed/Soft Tissue | Pliable, well-vascularized soft tissue envelope | Severe scarring, active infection, inadequate skin coverage |
| Patient Compliance | High motivation, reliable for complex rehab | Severe cognitive deficit, non-compliant, active substance abuse |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the bedrock of a successful tendon transfer. The surgeon must meticulously select the combination of tendon transfers that will best restore the triad of radial nerve function: wrist extension, finger extension, and thumb extension/abduction. The classic combinations are the Boyes transfer (utilizing FDS tendons) and the Jones transfer (utilizing the FCU). However, modern algorithms frequently employ a modified FCR transfer, which preserves the FCU as an important ulnar stabilizer of the wrist.
The standard "FCR-based" transfer scheme, which we will detail in this masterclass, typically involves: 1) Pronator Teres (PT) to Extensor Carpi Radialis Brevis (ECRB) for wrist extension; 2) Flexor Carpi Radialis (FCR) to Extensor Digitorum Communis (EDC) for finger extension; and 3) Palmaris Longus (PL) to Extensor Pollicis Longus (EPL) for thumb extension. If the PL is absent (which occurs in roughly 15% of the population), the FDS of the ring finger (FDS IV) is an excellent alternative donor for the EPL. During the clinical examination, the presence and strength of the PL, FCR, and PT must be explicitly documented.
Electrodiagnostic studies (EMG/NCS) are critical components of the preoperative workup. An initial baseline study at 4 to 6 weeks post-injury confirms the extent of axonal loss. Subsequent studies at 3-month intervals track the progress of reinnervation. Once the EMG demonstrates a plateau in recovery with persistent clinical deficits, the indication for tendon transfer is solidified. Radiographs of the forearm and hand are also obtained to rule out occult fractures, post-traumatic arthritis, or carpal instability that might compromise the mechanical efficiency of the transfers.
In the operating room, the patient is positioned supine with the operative arm extended on a radiolucent hand table. A pneumatic tourniquet is applied high on the brachium. The entire upper extremity, from the fingertips to the axilla, is prepped and draped to allow for full visualization of the limb's resting cascade and to permit unhindered intraoperative manipulation. Loupe magnification (typically 2.5x to 3.5x) is essential for the meticulous dissection required to protect delicate neurovascular structures and to perform precise tendon weaves.
Prior to inflation of the tourniquet, the limb is exsanguinated with an Esmarch bandage. The planned incisions are meticulously marked. A single, expansile volar-radial incision can often access the PT, FCR, and PL, while a separate dorsal longitudinal incision over the distal forearm provides access to the recipient extensor tendons (ECRB, EDC, EPL). The surgeon must mentally rehearse the routing of each transfer, ensuring that the line of pull is as direct as possible and that the transfers do not cross each other in a manner that would cause friction or bowstringing.
Step-by-Step Surgical Approach and Fixation Technique
The execution of multiple tendon transfers demands a systematic, highly organized approach. We begin by harvesting all donor tendons, followed by the preparation of the recipient tendons, and conclude with the critical tensioning and weaving phase.
Pronator Teres to Extensor Carpi Radialis Brevis Transfer
The restoration of wrist extension is the paramount functional goal. The PT is an ideal donor due to its robust cross-sectional area and appropriate excursion. We rely on the ECRB rather than the ECRL as the recipient because the ECRB inserts centrally on the base of the third metacarpal, providing pure, balanced wrist extension without the radial deviation moment associated with the ECRL.
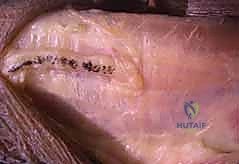
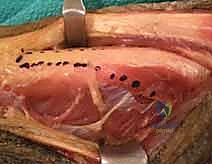
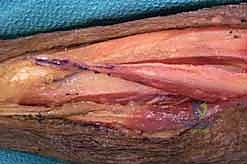
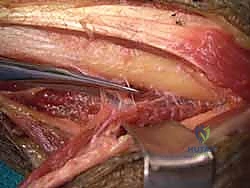
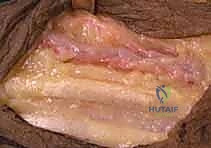
A longitudinal incision is made along the radial border of the mid-forearm. The superficial fascia is divided, and the interval between the brachioradialis (BR) and the flexor carpi radialis (FCR) is developed. The superficial radial nerve (SRN) and radial artery are identified and carefully retracted. The broad, flat insertion of the PT onto the lateral aspect of the radius is visualized.

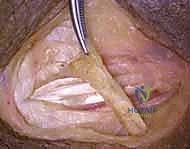
To maximize the length of the donor tendon, a strip of periosteum (approximately 1.5 to 2 cm) is harvested in continuity with the PT insertion from the radius. This periosteal extension is crucial, as the PT tendon itself is quite short. Once detached, the PT is mobilized proximally. Care must be taken not to dissect too aggressively on the deep surface of the proximal PT, as this risks injury to its median nerve motor branches.
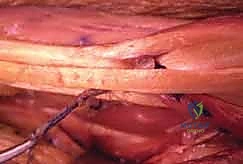
Next, the ECRB and ECRL tendons are identified dorsally. The ECRB is located slightly more ulnar and deep to the ECRL. The PT tendon is routed subcutaneously over the BR to reach the ECRB. The routing must be superficial to the BR to avoid compression of the transfer during muscle contraction.
Flexor Carpi Radialis to Extensor Digitorum Communis Transfer
For finger extension, the FCR is a highly reliable donor. Through the same volar incision, the FCR tendon is identified. It is transected distally at the wrist crease, just proximal to the trapezium. The FCR muscle belly is mobilized proximally to the mid-forearm to ensure adequate excursion.
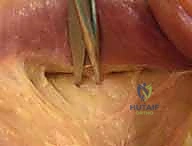
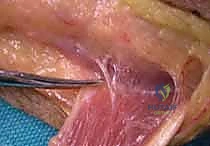
A dorsal longitudinal incision is made over the distal forearm, centered over the fourth extensor compartment. The extensor retinaculum is partially divided to expose the EDC tendons. The EDC tendons to the index, middle, ring, and small fingers are identified and grouped together.
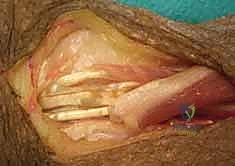
The FCR tendon is then passed from volar to dorsal. This can be done subcutaneously around the radial border of the forearm, or via a trans-interosseous membrane route. The subcutaneous route is generally preferred as it avoids the potential for adhesions at the interosseous membrane and protects the anterior interosseous nerve (AIN). The FCR is routed directly toward the grouped EDC tendons.
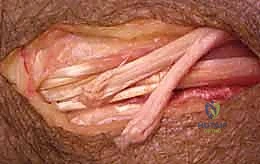

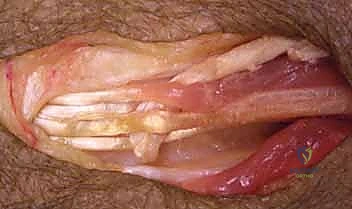
Palmaris Longus to Extensor Pollicis Longus Transfer
Restoring independent thumb extension is achieved by transferring the Palmaris Longus (PL) to the Extensor Pollicis Longus (EPL). The PL is harvested at the wrist crease and mobilized proximally.
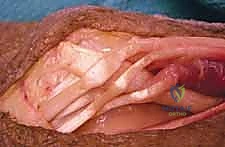
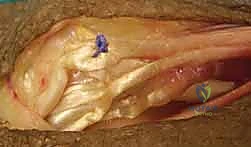
Through the dorsal incision, the EPL tendon is identified as it angles around Lister's tubercle. The EPL is transected proximally at its myotendinous junction. It is then rerouted out of the third extensor compartment and transposed radially into the subcutaneous tissues. This rerouting provides a more direct line of pull for thumb extension and abduction.
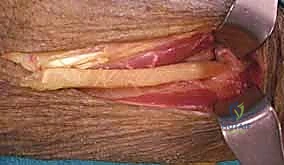
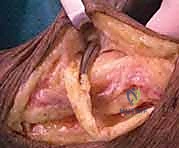
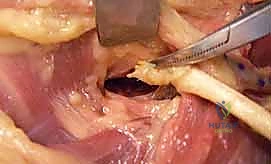
The PL tendon is routed subcutaneously to meet the rerouted EPL. The line of pull should be straight, avoiding any acute angles that could compromise the transfer's mechanical efficiency.
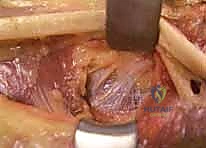
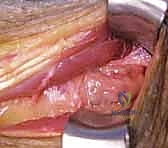
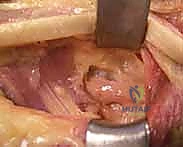
Tensioning, Weaving, and Final Fixation
Tensioning is the most critical and technically demanding aspect of the procedure. A perfectly executed weave will fail if the tension is incorrect. The general principle is to set the tension such that the resting cascade of the hand is restored, and the donor muscle operates at the peak of its Blix length-tension curve.
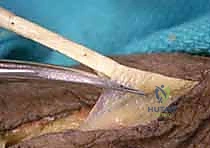
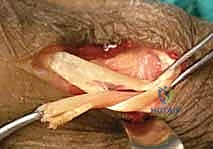
We utilize a Pulvertaft weave for all tendon anastomoses. This technique involves passing the donor tendon through the recipient tendon multiple times (typically 3 to 4 passes) at 90-degree angles. This creates a biomechanically superior construct that allows for immediate, gentle active mobilization if desired. Non-absorbable braided suture (e.g., 3-0 or 4-0 Ethibond or Ticron) is used to secure each pass.
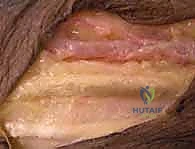
The order of tensioning is crucial. We first tension the PT to ECRB transfer. The wrist is held in approximately 30 to 45 degrees of extension. The PT is pulled distally to remove slack, and the weave is performed.
Next, the FCR to EDC transfer is tensioned. With the wrist held in 30 degrees of extension, the MCP joints are held in neutral (0 degrees of extension), and the PIP/DIP joints are allowed to rest in slight flexion. The FCR is woven into the grouped EDC tendons. It is critical to ensure uniform tension across all four digits to prevent a lagging finger.
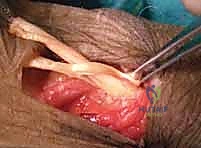
Finally, the PL to EPL transfer is tensioned. The wrist is maintained in extension, and the thumb is brought into maximal palmar abduction and extension. The PL is woven into the EPL under moderate tension.
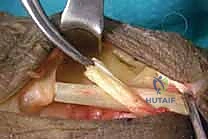
After all weaves are completed, the tenodesis effect is visually confirmed. Flexing the wrist should cause the fingers and thumb to automatically extend, while extending the wrist should allow the digits to fall into a natural flexed cascade. The wounds are irrigated and closed in layers, and a bulky, non-compressive dressing is applied, followed by a rigid volar plaster splint holding the wrist in 45 degrees of extension, the MCPs in neutral, and the thumb in extension.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, complications following tendon transfers for radial nerve palsy can occur. The most common complication is the formation of dense peritendinous adhesions, which restrict tendon excursion and limit functional outcome. Adhesions are particularly problematic when tendons are routed through the interosseous membrane or beneath tight fascial retinacula. Prevention relies on meticulous hemostasis, gentle tissue handling, and the implementation of a structured, early-mobilization rehabilitation protocol when biomechanically safe.
Incorrect tensioning is the second major pitfall. Under-tensioning results in a lag; the patient will have strong muscle contraction but incomplete joint extension. Over-tensioning can lead to a fixed extension contracture, severely compromising the patient's ability to make a fist or grasp objects. If a transfer is significantly under-tensioned, surgical revision and re-weaving may be necessary. Over-tensioning can sometimes be managed with aggressive stretching and dynamic flexion splinting, but severe cases also require surgical lengthening.
Neuromas of the superficial radial nerve (SRN) represent a devastating complication. The SRN is exquisitely sensitive, and injury during the harvest of the PT or the routing of tendons can lead to chronic, debilitating neuropathic pain. If a neuroma develops, conservative management with desensitization and gabapentinoids is initiated. If refractory, surgical excision of the neuroma and burying the proximal nerve stump deep into the brachioradialis muscle belly is indicated.
Tendon rupture is rare when utilizing a robust Pulvertaft weave with multiple passes, occurring in less than 2% of cases. Ruptures typically occur in the early postoperative period due to patient non-compliance or a sudden, forceful eccentric load. Immediate surgical re-exploration and repair are mandated if a rupture is identified.
| Complication | Estimated Incidence | Prevention Strategy | Salvage / Management |
|---|---|---|---|
| Tendon Adhesions | 10 - 15% | Atraumatic technique, subcutaneous routing, early guided rehab | Intensive hand therapy, tenolysis (rarely required before 6 months) |
| Under-tensioning (Lag) | 5 - 10% | Tensioning with wrist in 30-45° extension, MCPs neutral | Prolonged dynamic extension splinting; surgical revision/shortening |
| Over-tensioning (Stiffness) | 5 - 10% | Avoid maximal tension; confirm tenodesis effect intraoperatively | Dynamic flexion splinting; surgical fractional lengthening |
| SRN Neuroma |
Clinical & Radiographic Imaging Archive

