Management of Malunited Fractures: Comprehensive Surgical Principles and Techniques
Key Takeaway
Malunion occurs when a fracture heals in a non-anatomic position, leading to altered biomechanics, functional impairment, and premature arthrosis. Successful management requires meticulous preoperative planning, precise osteotomy execution, and robust fixation. This guide details the principles of malunion reconstruction across major anatomical regions, emphasizing the role of conventional internal fixation and advanced circular frame techniques for complex deformities involving bone loss or prior infection.
Introduction to Malunited Fractures
A malunion is defined as a fracture that has healed in a non-anatomic position, resulting in a deformity that may be angular, rotational, translational, or characterized by a discrepancy in limb length. While some degree of malalignment is tolerated depending on the anatomical region and the patient's physiological demands, significant malunions alter joint reaction forces, impair kinematics, and predictably lead to premature post-traumatic arthrosis.
The surgical management of malunited fractures is among the most challenging endeavors in orthopedic surgery. It requires a profound understanding of three-dimensional biomechanics, meticulous preoperative planning, and mastery of both internal and external fixation techniques.
Clinical Pearl: The primary goal of malunion surgery is not merely cosmetic correction, but the restoration of the mechanical axis, joint congruity, and soft-tissue balance to prevent long-term degenerative changes and restore maximal function.
Principles of Deformity Evaluation
Clinical Evaluation
A thorough clinical evaluation must precede any surgical intervention. The surgeon must assess:
* Gait and Function: Observe for antalgic gait, thrust, or compensatory mechanisms.
* Rotational Profile: Assess torsional deformities (e.g., thigh-foot angle, hip internal/external rotation).
* Soft Tissue Envelope: Evaluate previous surgical incisions, skin quality, and the presence of adherent scars. Previous infection drastically alters the surgical approach.
* Neurovascular Status: Chronic deformities may tether neurovascular structures, increasing the risk of iatrogenic injury during acute correction.
Radiographic Evaluation
Standardized imaging is the cornerstone of preoperative planning.
* Full-Length Standing Radiographs: Essential for lower extremity malunions to calculate the Mechanical Axis Deviation (MAD) and the Center of Rotation of Angulation (CORA).
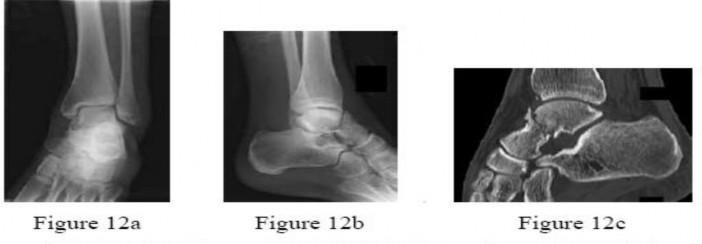
* Computed Tomography (CT): Mandatory for intra-articular malunions (e.g., distal radius, tibial plateau, calcaneus) to assess joint step-offs, gap formation, and 3D architecture. 3D reconstructions are invaluable for planning complex multi-planar osteotomies.
* Scanograms: Utilized for precise limb-length discrepancy measurements.
The Role of Circular Fixation in Complex Malunions
While conventional open reduction and internal fixation (ORIF) with osteotomy remains the gold standard for many malunions, circular fixation techniques (e.g., Ilizarov apparatus, Taylor Spatial Frame) have revolutionized the management of complex deformities.
Circular fixation has a definitive role in malunion surgery, particularly for the restoration of length and when previous infection has rendered conventional open reduction techniques inappropriate.
Surgical Warning: The use of circular frames requires detailed instruction and extensive experience. The success of these techniques relies heavily on precise frame design and construction, intensive patient counseling, and rigorous postoperative physical therapy.
Indications for Circular Fixation:
* Malunions associated with significant bone loss requiring distraction osteogenesis.
* History of osteomyelitis or infected nonunions/malunions where internal hardware is contraindicated.
* Severe multi-planar deformities that require gradual correction to prevent neurovascular compromise.
* Poor soft-tissue envelopes that cannot tolerate extensive surgical stripping.
Lower Extremity Malunions
Femur and Hip
Femoral malunions frequently present with a combination of shortening, angulation, and malrotation.
Femoral Shaft
Malunions of the femoral shaft alter the mechanical axis of the lower extremity, leading to abnormal stresses across the knee joint.
* Surgical Approach: Correction typically involves a diaphyseal osteotomy.
* Fixation: Intramedullary nailing (antegrade or retrograde) is the preferred fixation method following a transverse or short oblique osteotomy. If the deformity is purely rotational, a transverse osteotomy stabilized by a locked intramedullary nail allows for immediate correction and early weight-bearing.
Trochanteric and Cervicotrochanteric Region
Malunions in this region often result in coxa vara, leading to abductor weakness (Trendelenburg gait) and limb shortening.
* Subtrochanteric Osteotomy: A closing wedge or dome osteotomy is utilized to restore the neck-shaft angle. Fixation is typically achieved with a fixed-angle device, such as a dynamic condylar screw (DCS) or a proximal femoral locking plate.
Condyles and Supracondylar Femur
Distal femoral malunions (lateral, medial, or both condyles) disrupt the mechanical axis, often causing severe valgus or varus thrust at the knee.
* Technique: Intra-articular step-offs require arthrotomy, osteotomy of the malunited fragment, and rigid fixation with headless compression screws or periarticular locking plates. Extra-articular supracondylar deformities are managed with opening or closing wedge osteotomies stabilized by distal femoral locking plates.
Tibia and Fibula
Shafts of the Tibia and Fibula
Tibial diaphyseal malunions are poorly tolerated due to the subcutaneous nature of the bone and the parallel orientation of the ankle and knee joints.
* Correction Strategy: The CORA is identified. If the osteotomy is performed at the CORA, pure angular correction is achieved without translation.
* Fixation: Depending on the location, intramedullary nailing (often requiring blocking screws to maintain alignment) or plate osteosynthesis is utilized. For complex or infected cases, circular external fixation is the treatment of choice.
Condyles of the Tibia
Malunion of the tibial plateau (including inverted-Y fractures and intercondylar eminence fractures) leads to rapid joint destruction.
* Intra-articular Osteotomy: Requires meticulous elevation of the depressed articular segment, structural bone grafting (autograft or allograft), and buttress plating.
Foot and Ankle
Talus
- Talar Neck: Malunion typically occurs in varus, leading to a rigid, supinated foot, lateral border overload, and subtalar arthrosis. Correction requires a medial opening wedge osteotomy of the talar neck with structural bone grafting.
- Talar Body: Often results in severe tibiotalar and subtalar incongruity. Salvage via tibiotalocalcaneal (TTC) arthrodesis is frequently required.
Calcaneus
Calcaneal malunions are characterized by loss of height, increased width, varus deformity of the tuberosity, and subfibular impingement.
* Surgical Management: A lateral extensile approach is used to perform a lateral wall exostectomy (to relieve subfibular impingement) combined with a subtalar arthrodesis. In cases of severe height loss, a distraction bone block arthrodesis is indicated to restore the talocalcaneal angle and correct the varus deformity.
Ankle Arthrodesis for Malunited Fractures
When a malunited ankle fracture leads to end-stage post-traumatic arthrosis, joint-sparing osteotomies are no longer viable.
* Technique: Ankle arthrodesis is performed, ensuring the foot is positioned in neutral dorsiflexion, 0-5 degrees of valgus, and 5-10 degrees of external rotation. Fixation is achieved via crossed lag screws or an anterior locking plate.
Upper Extremity Malunions
Distal Radius
Distal radius malunions are among the most common orthopedic deformities, significantly impacting wrist kinematics, grip strength, and distal radioulnar joint (DRUJ) function.
Clinical and Radiographic Evaluation
Patients present with pain, limited flexion/extension, and restricted forearm rotation. Radiographs typically reveal loss of radial inclination, loss of radial length (positive ulnar variance), and either dorsal (Colles-type) or volar (Smith-type) tilt.
Extra-articular Malunion with Dorsal Angulation
- Indications: Symptomatic deformity with >15 degrees of dorsal tilt, >3 mm of radial shortening, or significant DRUJ incongruity.
- Surgical Approach: A volar (modified Henry) approach is preferred. The flexor carpi radialis (FCR) sheath is opened, and the pronator quadratus is elevated.
- Osteotomy and Grafting: A transverse osteotomy is performed parallel to the articular surface at the site of the previous fracture. The distal fragment is mobilized, and the deformity is corrected (restoring volar tilt and radial length). The resulting volar gap is filled with a structural autograft (iliac crest) or allograft.
- Fixation: A volar locking plate provides rigid stabilization, allowing for early range of motion.
Pitfall: Failure to release the brachioradialis insertion from the radial styloid will tether the distal fragment, making restoration of radial length and inclination nearly impossible.
Extra-articular Malunion with Volar Angulation
- Technique: These are typically approached volarly. An opening wedge osteotomy is performed, but the structural graft is placed dorsally if a dorsal approach is used, or the deformity is corrected via a volar approach using a specialized volar locking plate designed to buttress the volar cortex.
Intra-articular Malunions and DRUJ Incongruity
Intra-articular step-offs greater than 2 mm inevitably lead to radiocarpal arthrosis.
* Salvage Procedures: If the cartilage is preserved, an intra-articular osteotomy can be attempted. However, in cases of established arthrosis, salvage procedures such as proximal row carpectomy (PRC), four-corner fusion, or total wrist arthrodesis are indicated.
* DRUJ Arthrosis: Malunions causing severe DRUJ incongruity may require a Darrach procedure (distal ulnar resection), a Suave-Kapandji procedure (DRUJ arthrodesis with proximal ulnar pseudoarthrosis), or ulnar shortening osteotomy if the primary issue is ulnar impaction syndrome.
Forearm (Radius and Ulna)
Forearm malunions severely restrict pronation and supination due to the disruption of the complex rotational axis between the radius and ulna.
Proximal Third of the Radius and Ulna
- Radial Head and Neck: Malunions here block rotation. Symptomatic cases in adults are often treated with radial head excision and prosthetic replacement.
- Monteggia Malunions: A malunited proximal ulna fracture with a chronic anterior dislocation of the radial head.
- Treatment: Requires an opening wedge osteotomy of the proximal ulna to restore length and dorsal angulation, which indirectly reduces the radial head. Annular ligament reconstruction may be necessary.
- Synostosis: Cross-union between the radius and ulna completely abolishes forearm rotation. Excision of the synostosis is fraught with high recurrence rates. Interposition of vascularized fat, muscle, or synthetic barriers, combined with immediate postoperative radiation or indomethacin, is required to prevent recurrence.
Shafts of the Radius and Ulna in Adults
Diaphyseal malunions require precise restoration of the radial bow to restore forearm rotation.
* Technique: Osteotomies are performed at the apex of the deformity. Rigid fixation with 3.5mm dynamic compression plates (DCP) or locking compression plates (LCP) is mandatory. Bone grafting is routinely performed due to the high risk of nonunion at the osteotomy site.
Humerus and Clavicle
Midshaft Malunions of the Clavicle
While clavicle malunions are often well-tolerated, symptomatic shortening (>2 cm) alters shoulder girdle biomechanics, leading to scapular dyskinesia, weakness, and thoracic outlet-type symptoms.
* Surgical Management: An opening wedge osteotomy with structural intercalary bone grafting and robust superior or anteroinferior plating restores the length and alignment of the shoulder girdle.
Humerus
Humeral malunions (Anatomical Neck, Surgical Neck, Proximal Third, Middle Third, Distal Humerus) are generally better tolerated than lower extremity malunions due to the compensatory motion of the shoulder and elbow.
* Indications for Surgery: Severe angular deformities (>20 degrees anterior/posterior, >30 degrees varus/valgus) or rotational deformities that limit hand-to-mouth or hand-to-perineum function.
* Distal Humerus: Malunions here (e.g., cubitus varus following pediatric supracondylar fractures) are treated with corrective closing wedge or dome osteotomies to restore the carrying angle and prevent tardy ulnar nerve palsy.
Pelvis
Pelvic malunions result in severe mechanical back pain, sitting imbalance, and apparent limb length discrepancies.
* Three-Stage Reconstruction: Severe pelvic malunions may require a complex three-stage approach:
1. Anterior release and osteotomy (e.g., symphysis pubis or pubic rami).
2. Posterior release, osteotomy of the sacroiliac joint or sacrum, and mobilization.
3. Definitive posterior and anterior rigid fixation once the hemipelvis is reduced.
This is a massive surgical undertaking reserved for highly symptomatic patients and requires a multidisciplinary surgical team.
Postoperative Protocols and Rehabilitation
The success of malunion reconstruction is inextricably linked to the postoperative rehabilitation protocol.
* Internal Fixation: When rigid internal fixation is achieved, early active range of motion of adjacent joints is instituted to prevent stiffness. Weight-bearing is typically restricted until radiographic evidence of bridging callus is observed at the osteotomy site (usually 6-8 weeks).
* Circular External Fixation: Patients require intensive physical therapy to maintain joint motion during the distraction and consolidation phases. Pin site care protocols must be strictly adhered to in order to prevent superficial infections that could compromise the frame or necessitate premature removal.
Clinical Pearl: Patient psychology plays a massive role in the success of malunion surgery, particularly when circular frames are utilized. Preoperative counseling regarding the duration of treatment, the pain associated with distraction, and the rigorous demands of physical therapy cannot be overstated.
You Might Also Like