Intertrochanteric Hip Fractures: Surgical Anatomy, Biomechanics, and Current Management Strategies
14 Apr 2026
45 min read
91 Views
Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Intertrochanteric Hip Fractures: Surgical Ana...
00:00
Start Quiz
Question 1High Yield
Slide 1 Slide 2
A 12-year-old girl was successfully treated for a flexible flatfoot deformity on the left foot. A clinical photograph (Slide 1) of her foot and a lateral radiograph (Slide 2) are presented. What is the purpose of the implant noted under the talus in the radiograph:
A 12-year-old girl was successfully treated for a flexible flatfoot deformity on the left foot. A clinical photograph (Slide 1) of her foot and a lateral radiograph (Slide 2) are presented. What is the purpose of the implant noted under the talus in the radiograph:
Explanation
The subtalar arthroerisis, as demonstrated in the radiograph, is used to control eversion of the subtalar joint during the foot flat phase of gait. A subtalar arthroerisis limits excessive eversion but does not restrict subtalar motion further. This procedure is indicated for a patient who has a flexible flatfoot deformity and can be used either as the sole or an adjunctive procedure for correction.
Question 2High Yield
Slide 1 Slide 2 Slide 3
A patient with diabetes and severe peripheral neuropathy has been treated for a C harcot ankle deformity for 9 months (Slide 1, Slide 2, and Slide 3). An ankle foot orthosis has been used for 4 months. No skin breakdown occurred in the brace. Swelling is present but has decreased over the past month. Ankle range of motion is limited, and crepitus is present upon examination of the ankle. Which surgical procedure is most consistent with the future treatment of this patient:
A patient with diabetes and severe peripheral neuropathy has been treated for a C harcot ankle deformity for 9 months (Slide 1, Slide 2, and Slide 3). An ankle foot orthosis has been used for 4 months. No skin breakdown occurred in the brace. Swelling is present but has decreased over the past month. Ankle range of motion is limited, and crepitus is present upon examination of the ankle. Which surgical procedure is most consistent with the future treatment of this patient:
Explanation
The indication for surgery is intractable deformity, which is refractory to all forms of bracing. By refractory, one implies that skin breakdown or imminent infection is present. If surgery were performed, then it would consist of a tibiotalocalcaneal arthrodesis. There are no indications for this surgery in this patient. Once the neuropathic process has reached a stable point, a deformity is not likely to progress.
Question 3High Yield
A 6-year-old African-American boy is brought to the emergency department with acute onset, severe pain through his right leg and left arm. His medical history is significant for sickle cell disease (HgbSS). His clinical exam is consistent with increased warmth and erythema to touch over his extremities, though he can move them, and his inflammatory markers are slightly elevated. He has no fever upon presentation. What is the best next step in the management of this child?
Explanation
■
Sickle cell disease (SCD) is the most common single gene disorder in African Americans, affecting approximately 1 of 375 persons of African ancestry. A vaso-occlusive crisis can manifest as pain in the chest, abdomen; back; or limbs, occurring when red blood cells sickle and cause local ischemia. Vaso-occlusive crisis affecting the bone is the most common acute clinical manifestation in children with SCD. Children with SCD are also prone to increased risk of bacterial sepsis and bone infection. Children with osteomyelitis often present with fever and a painful, swollen, tender limb with limited range of motion, signs and symptoms that are similar to those found in patients with vaso-occlusive crisis. Therefore, diagnosing osteomyelitis in children with SCD can be extremely difficult.
Children with vaso-occlusive crisis tend to have many fewer days with fever, and their inflammatory markers are often only mildly elevated. In the study of Berger and associates, the probability of osteomyelitis increased by 80% for each day a child had fever before presentation, and by 20% for each day a child had pain before presentation. Patients were 8.4 times more likely to have osteomyelitis if they presented with documented swelling of the affected limb. The risk of osteomyelitis was decreased by 30% for each additional painful site if more than one painful site was present.
Plain radiographs obtained during the early phases of either condition often have normal findings or only show soft-tissue swelling. At 2 weeks, both conditions may show periosteal reaction, and radiographs are of limited utility in differentiating the two conditions. Both radionuclide bone marrow and bone scan and Gadoliniumenhanced MRI could be effectively used in differentiating acute osteomyelitis from vaso-occlusive crisis, if needed.
Bone cultures could be helpful but are reported to be positive in only 30% to 86% of cases. Blood cultures could be utilized for definitive diagnosis but they could be even less specific.
Initial management for suspected cases of vaso-occlusive crisis includes intravenous fluids, oxygenation, NSAIDS and parenteral opioids. Patients who do not respond to this regimen may need to undergo advanced imaging and have their cultures taken while they are placed on empiric antibiotics covering salmonella and Staphylococcus aureus until a definitive diagnosis is made.
Sickle cell disease (SCD) is the most common single gene disorder in African Americans, affecting approximately 1 of 375 persons of African ancestry. A vaso-occlusive crisis can manifest as pain in the chest, abdomen; back; or limbs, occurring when red blood cells sickle and cause local ischemia. Vaso-occlusive crisis affecting the bone is the most common acute clinical manifestation in children with SCD. Children with SCD are also prone to increased risk of bacterial sepsis and bone infection. Children with osteomyelitis often present with fever and a painful, swollen, tender limb with limited range of motion, signs and symptoms that are similar to those found in patients with vaso-occlusive crisis. Therefore, diagnosing osteomyelitis in children with SCD can be extremely difficult.
Children with vaso-occlusive crisis tend to have many fewer days with fever, and their inflammatory markers are often only mildly elevated. In the study of Berger and associates, the probability of osteomyelitis increased by 80% for each day a child had fever before presentation, and by 20% for each day a child had pain before presentation. Patients were 8.4 times more likely to have osteomyelitis if they presented with documented swelling of the affected limb. The risk of osteomyelitis was decreased by 30% for each additional painful site if more than one painful site was present.
Plain radiographs obtained during the early phases of either condition often have normal findings or only show soft-tissue swelling. At 2 weeks, both conditions may show periosteal reaction, and radiographs are of limited utility in differentiating the two conditions. Both radionuclide bone marrow and bone scan and Gadoliniumenhanced MRI could be effectively used in differentiating acute osteomyelitis from vaso-occlusive crisis, if needed.
Bone cultures could be helpful but are reported to be positive in only 30% to 86% of cases. Blood cultures could be utilized for definitive diagnosis but they could be even less specific.
Initial management for suspected cases of vaso-occlusive crisis includes intravenous fluids, oxygenation, NSAIDS and parenteral opioids. Patients who do not respond to this regimen may need to undergo advanced imaging and have their cultures taken while they are placed on empiric antibiotics covering salmonella and Staphylococcus aureus until a definitive diagnosis is made.
Question 4High Yield
A 17-year-old football player is unable to flex the distal interphalangeal (DIP) joint of his ring finger. He states that he injured the finger 6 weeks ago while attempting to tackle another player who pulled free from his grip, but he did not inform his coach at the time of the injury. Current radiographs show an observable fleck of bone volar to the base of the proximal phalanx. Treatment should consist of
Explanation
Flexor digitorum profundus ruptures are classified into three types. In type I, the tendon retracts into the palm. In type II, the tendon retracts to the level of the proximal phalanx, the vinculum remains intact, and the blood supply is preserved to the tendon. A small fleck of bony fragment observed at the A2 pulley is pathognomonic for a type II rupture. Successful primary repair of the type II rupture has been reported as late as 2 months after the injury. Type III injuries have large fragments of the distal phalanx attached and are caught distally by the A1 pulley. Type III ruptures can be repaired up to several months after the injury.
REFERENCES: Leddy JP: Avulsions of the flexor digitorum profundus. Hand Clin
1985;1:77-83.
Kiefhaber TR: Closed tendon injuries in the hand. Oper Tech Sports Med 1996;4:227-241.
REFERENCES: Leddy JP: Avulsions of the flexor digitorum profundus. Hand Clin
1985;1:77-83.
Kiefhaber TR: Closed tendon injuries in the hand. Oper Tech Sports Med 1996;4:227-241.
Question 5High Yield
Ganglions of the distal interphalangeal (DIP) joints of the fingers are called:
Explanation
Ganglions arising at the DIP joints are called mucous cysts and ganglions from the flexor tendon in the palm are called retinacular cysts.
Bouchard nodes are osteophytes that develop at the proximal interphalangeal joint.
Heberden nodes are bony spurs at the dorsal aspect of the DIP joint and are present in osteoarthritis. Inclusion cysts are mobile, nonadherent to skin, and can occur anywhere on a hand.
Bouchard nodes are osteophytes that develop at the proximal interphalangeal joint.
Heberden nodes are bony spurs at the dorsal aspect of the DIP joint and are present in osteoarthritis. Inclusion cysts are mobile, nonadherent to skin, and can occur anywhere on a hand.
Question 6High Yield
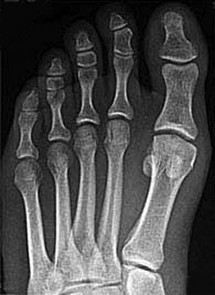
Figure 99 is the radiograph of an 18-year-old National Collegiate Athletic Association Division I basketball player who jumped for a basket. After
landing, he was unable to put weight on his left great toe. He developed pain, swelling, and ecchymosis maximally around the sesamoids. When assessing stability of the first metatarsophalangeal joint, he appears to have more laxity on the left. What is the best next step?
landing, he was unable to put weight on his left great toe. He developed pain, swelling, and ecchymosis maximally around the sesamoids. When assessing stability of the first metatarsophalangeal joint, he appears to have more laxity on the left. What is the best next step?
Explanation
This patient jumped on his forefoot and landed with pain in his great toe. His radiograph shows possible increased space between the sesamoids and the base of the phalanx. A comparison radiograph on the other side will reveal if this position is normal for this patient. If findings are asymmetric, turf toe injury is a possibility based on this patient's symptoms and mechanism of injury.
RECOMMENDED READINGS
[Waldrop NE 3rd, Zirker CA, Wijdicks CA, Laprade RF, Clanton TO. Radiographic evaluation of plantar plate injury: an in vitro biomechanical study. Foot Ankle Int. 2013 Mar;34(3):403-8. doi: 10.1177/1071100712464953. Epub 2013 Jan 14. PubMed PMID: 23520299. ](http://www.ncbi.nlm.nih.gov/pubmed/23520299)[View](http://www.ncbi.nlm.nih.gov/pubmed/23520299)
[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23520299)
[McCormick JJ, Anderson RB. The great toe: failed turf toe, chronic turf toe, and complicated sesamoid injuries. Foot Ankle Clin. 2009 Jun;14(2):135-50. doi: 10.1016/j.fcl.2009.01.001. Review. PubMed PMID: 19501799. ](http://www.ncbi.nlm.nih.gov/pubmed/19501799)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19501799)
RECOMMENDED READINGS
[Waldrop NE 3rd, Zirker CA, Wijdicks CA, Laprade RF, Clanton TO. Radiographic evaluation of plantar plate injury: an in vitro biomechanical study. Foot Ankle Int. 2013 Mar;34(3):403-8. doi: 10.1177/1071100712464953. Epub 2013 Jan 14. PubMed PMID: 23520299. ](http://www.ncbi.nlm.nih.gov/pubmed/23520299)[View](http://www.ncbi.nlm.nih.gov/pubmed/23520299)
[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23520299)
[McCormick JJ, Anderson RB. The great toe: failed turf toe, chronic turf toe, and complicated sesamoid injuries. Foot Ankle Clin. 2009 Jun;14(2):135-50. doi: 10.1016/j.fcl.2009.01.001. Review. PubMed PMID: 19501799. ](http://www.ncbi.nlm.nih.gov/pubmed/19501799)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19501799)
Question 7High Yield
Figure 1 is the radiograph of a 15-year-old boy with scoliosis. He has back pain and spinal asymmetry. Examination reveals a spinal curvature without cutaneous manifestations. Neurological examination reveals a normal motor and sensory examination, normal deep tendon reflexes, present superficial abdominal reflexes, and negative Babinski sign. His MRI scans are shown in Figures 2 and

Explanation
■
The MRI scans reveal a spinal cord with a noted central spinal canal syrinx. The patient has a normal neurological examination. There is no evidence of Chiari malformation or tethered spinal cord. Thus, for this patient, a neurosurgical evaluation is not required nor is a cerebral spinal fluid shunt. As the deformity has progressed past 50° in a skeletally immature teenager, brace treatment is no longer appropriate, and surgical correction of the scoliosis is the most appropriate treatment.
The MRI scans reveal a spinal cord with a noted central spinal canal syrinx. The patient has a normal neurological examination. There is no evidence of Chiari malformation or tethered spinal cord. Thus, for this patient, a neurosurgical evaluation is not required nor is a cerebral spinal fluid shunt. As the deformity has progressed past 50° in a skeletally immature teenager, brace treatment is no longer appropriate, and surgical correction of the scoliosis is the most appropriate treatment.
Question 8High Yield
A 70-year-old woman has a preoperative anterior interscalene block prior to undergoing a total shoulder arthroplasty. After seating her in the beach chair position, she becomes acutely hypotensive. What is the most likely cause for the hypotension?
Explanation
The beach chair position may cause sudden hypotension and bradycardia as a result of the Bezold-Jarisch reflex. This reflex occurs when venous pooling and increased sympathetic tone induce a low-volume, hypercontractile ventricle, resulting in activation of the parasympathetic nervous system and sympathetic withdrawal. The reported incidence of this phenomenon associated with the sitting position is between 13% to 24%. Left untreated, the result may be cardiac arrest. Pneumothorax or central nervous system toxicity after interscalene block is rare and has an incidence of less than 0.2%. Laryngeal nerve block associated with interscalene nerve block can occur but usually results in hoarseness secondary to ipsilateral vocal cord palsy.
REFERENCES: Long T, Wass C, Burkle C: Perioperative interscalene blockade: An overview of its history and current clinical use. J Clin Anesthesia 2002;14:546-556.
Norris T (ed): Orthopaedic Knowledge Update: Shoulder and Elbow 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 433-442.
REFERENCES: Long T, Wass C, Burkle C: Perioperative interscalene blockade: An overview of its history and current clinical use. J Clin Anesthesia 2002;14:546-556.
Norris T (ed): Orthopaedic Knowledge Update: Shoulder and Elbow 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 433-442.
Question 9High Yield
When performing a Green transfer for cerebral palsy—flexor carpi ulnaris (FCU) to extensor carpi radialis brevis (ECRB)—in addition to improving wrist extension, what other motion may be improved if the FCU is routed around the ulna instead of through the interosseous membrane?
Explanation
The typical upper extremity deformity in spastic hemiplegic cerebral palsy consists of shoulder internal rotation, elbow flexion, forearm pronation and wrist flexion, and ulnar deviation. The pronation position of the forearm can make bimanual activities more challenging for the child. The wrist flexion and ulnar deviation deformity interferes with finger function and therefore with grasp and release patterns. By transferring the FCU tendon to the ECRB, the deforming force is released, and central wrist extension is augmented. This transfer can lead to a supination moment when it is routed around the ulna to the ECRB insertion on the dorsum of the wrist. Thumb and finger extension are not affected by an FCU-to-ECRB _tendon transfer. Forearm supination, not pronation, is potentially improved with this tendon transfer._
Question 10High Yield
Figure 1 is the MR arthrogram of a 24-year old professional baseball pitcher who complains of worsening right elbow pain and decreased pitch velocity over the past 2 months. He was initially managed with rest and forearm strengthening, but continues to complain of medial elbow pain during the long toss portion of his throwing program. What is the most appropriate treatment at this time?
Explanation
The MR arthrogram shows a rupture of the ulnar collateral ligament (UCL) from the ulnar insertion, with the classic T-sign of contrast extravasation. Medial UCL reconstruction, using either ipsilateral palmaris longus or allograft tendon, is
indicated for UCL injuries that fail nonsurgical management. Primary repair has been shown to be successful in select cases, but appropriate patient selection is essential. An arthroscopic elbow debridement would be indicated for early elbow arthritis or intra-articular loose body, which is not demonstrated here. An ulnar nerve decompression would be indicated in the setting of cubital tunnel syndrome, but this patient has no complaints of paresthesias.
40
indicated for UCL injuries that fail nonsurgical management. Primary repair has been shown to be successful in select cases, but appropriate patient selection is essential. An arthroscopic elbow debridement would be indicated for early elbow arthritis or intra-articular loose body, which is not demonstrated here. An ulnar nerve decompression would be indicated in the setting of cubital tunnel syndrome, but this patient has no complaints of paresthesias.
40
Question 11High Yield
Initial enthusiasm of cemented femoral stems in total hip arthroplasty was tempered by:
Explanation
Early outcomes were characterized by poor survivorship in the young population, a situation that corrected with subsequent polyethylene improvements and cement techniques.
Question 12High Yield
Figures 1 and 2 are the radiographs of a 21-year-old man who has a long history of thoracic back pain. His lumbar spine is asymptomatic. He has failed prolonged nonsurgical treatment. Surgical correction should consist of

Explanation
■
When planning surgical intervention for Scheuermann kyphosis, it is imperative that the instrumentation and fusion extend across the entirety of the deformity. Distally, this means extending across the first lordotic disk space. In this scenario, this disk is the L1-L2 disk, which means the fusion needs to extend to L2. Shorter and longer fusions are not necessary or appropriate.
When planning surgical intervention for Scheuermann kyphosis, it is imperative that the instrumentation and fusion extend across the entirety of the deformity. Distally, this means extending across the first lordotic disk space. In this scenario, this disk is the L1-L2 disk, which means the fusion needs to extend to L2. Shorter and longer fusions are not necessary or appropriate.
Question 13High Yield
What is the likelihood of this patient’s children having a similar condition?
Explanation
- 50%_
Question 14High Yield
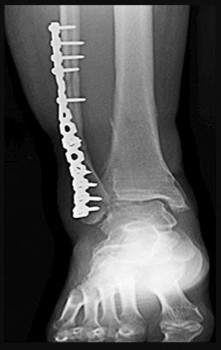
A 27-year-old man who underwent ankle ORIF 5 years ago is experiencing continuous ankle pain that has worsened over time (Figures 41a and 41b).
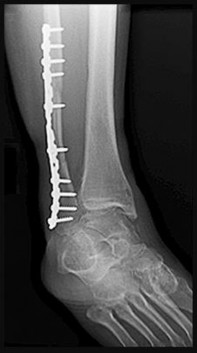
Explanation
- Ankle distraction arthroplasty_
Question 15High Yield
Which complication is most frequently encountered after revision surgery to treat junctional kyphosis?
Explanation
- Adjacent segment degeneration
Question 16High Yield
Injury to the popliteal artery during total knee arthroplasty (TKA) is most likely to occur when placing a
sharp retractor
sharp retractor
Explanation
Vascular complications during TKA are rare but do occur. Traditionally, it was taught that the popliteal artery was situated posterior to the PCL; however, more recent anatomic dissections have demonstrated that this artery is usually located posterolateral to the PCL.
Question 17High Yield
The best index to measure acetabular deficiency in the coronal plane is:
Explanation
Literature from Europe and North America suggests that a patient with acetabular dysplasia whose anteroposterior radiograph shows a center edge angle of Wiberg less than 15° is a good candidate for periacetabular osteotomy
Question 18High Yield
Phonopheresis is:
Explanation
Phonopheresis is delivery of medicine through the skin using ultrasound. Although there is some question as to whether the medications are more effectively absorbed or delivered with ultrasound use, this is a described modality.
Question 19High Yield
Figure 1 is the MR image of a 14-year-old football player who injured his right knee during a game. He describes feeling a "pop" and then needing help walking off the field. His knee is visibly swollen. The patient undergoes surgery to repair/reconstruct the damaged structure and has no postsurgical complications and begins physical therapy rehabilitation. The boy and his parents stress they want to “get the therapy over with as fast as possible" to expedite his return to sports, and the surgeon and rehabilitation team consider their request. Compared with nonaccelerated rehabilitation, patients who follow an early accelerated rehabilitation protocol experience
---
---
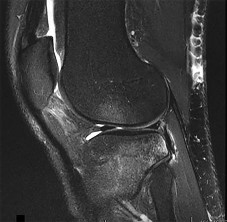
Explanation
The MR image shows bone bruises (“kissing contusions”) consistent with an ACL tear. During the ACL subluxation event, the posterolateral tibial plateau subluxes anteriorly, making contact with the mid portion of the lateral femoral condyle and resulting in this characteristic bone bruise pattern on MRI. Randomized clinical trials comparing early accelerated versus nonaccelerated rehabilitation programs have demonstrated no significant differences in long-term results with regard to function, reinjury, and successful return to play. These studies did not address timing of return to play with an early accelerated rehabilitation program. At 2 and 3 years postsurgically, there are no differences in laxity, number of graft _failures, or KOOS scores._
Question 20High Yield
Aneurysmal bone cyst of the spine is most common in which of the following regions:
Explanation
Aneurysmal bone cyst of the spine is most common in the lumbar spine, followed by the cervical spine. Aneurysmal bone cyst of the spine is treated with embolization and/or surgical resection and reconstruction.
Question 21High Yield
Which factor is most important when making a decision regarding surgery with this patient?
Explanation
- The patient's other injuries
Question 22High Yield
Rupture of the structure shown in the axial cross and the sagittal sections in Figures 100a and 100b causes weakness in
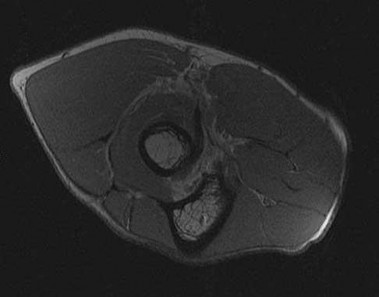
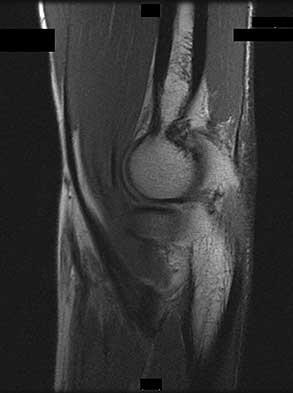
Explanation
87
The structure identified is the distal biceps tendon. Rupture of this tendon causes weakness in both flexion and supination. The biceps tendon does not affect extension or pronation.
RECOMMENDED READINGS
1. [Baker BE, Bierwagen D. Rupture of the distal tendon of the biceps brachii. Operative versus non-operative treatment. J Bone Joint Surg Am. 1985 Mar;67(3):414-7. PubMed PMID: 3972865. ](http://www.ncbi.nlm.nih.gov/pubmed/3972865)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3972865)
2. [Mazzocca AD, Spang JT, Arciero RA. Distal biceps rupture. Orthop Clin North Am. 2008 Apr;39(2):237-49, vii. doi: 10.1016/j.ocl.2008.01.001. Review. PubMed PMID: 18374814. ](http://www.ncbi.nlm.nih.gov/pubmed/18374814)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/18374814)
The structure identified is the distal biceps tendon. Rupture of this tendon causes weakness in both flexion and supination. The biceps tendon does not affect extension or pronation.
RECOMMENDED READINGS
1. [Baker BE, Bierwagen D. Rupture of the distal tendon of the biceps brachii. Operative versus non-operative treatment. J Bone Joint Surg Am. 1985 Mar;67(3):414-7. PubMed PMID: 3972865. ](http://www.ncbi.nlm.nih.gov/pubmed/3972865)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3972865)
2. [Mazzocca AD, Spang JT, Arciero RA. Distal biceps rupture. Orthop Clin North Am. 2008 Apr;39(2):237-49, vii. doi: 10.1016/j.ocl.2008.01.001. Review. PubMed PMID: 18374814. ](http://www.ncbi.nlm.nih.gov/pubmed/18374814)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/18374814)
Question 23High Yield
Arthrodesis of the ankle in a 34-year-old woman should be performed with the ankle positioned in:
Explanation
Although the woman may wish to wear shoes of varying height, there is sufficient plantarflexion occurring through the transverse tarsal joint to permit the wearing of high-heel shoes. Any plantarflexion of the fusion will cause arthritis of the transverse tarsal joint, particularly the talonavicular joint. Dorsiflexion of an ankle arthrodesis is associated with a calcaneus position and heel pain. The ankle should be fused in a similar position for both male and female patients.
Question 24High Yield
A 39-year-old female presents with the following motor vehicle crash with the injury seen in Figure A (immobilized in a pelvic binder). The iatrogenic neurologic injury most commonly caused by placement of the anterior construct for this injury, as shown in Figure B, would cause which of the following?
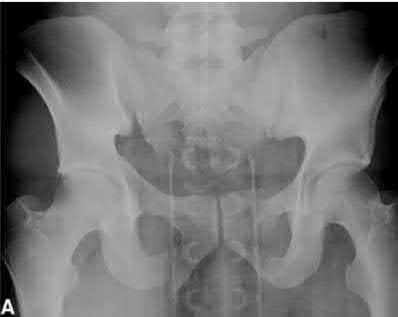
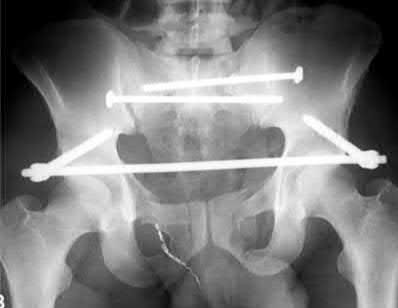
Explanation
This patient was treated with posterior stabilization, and an anterior subcutaneous internal fixator (ASIF). The most common neurologic injury seen following placement of the ASIF construct is irritation of the lateral femoral cutaneous nerve (LFCN), causing numbness and/or pain of the lateral thigh.
Unstable pelvic fractures can be treated in a multitude of ways. The ASIF construct is typically created by placing long pelvic screws or polyaxial pedicle screws in the supraacetabular region, similar to the supraacetabular pins for an
anterior external fixator. Then a curved bar is placed subcutaneously and connected to the supraacetabular screws. They are typically removed after 3-4 months when fracture healing is complete.
Vaidya et al. present a retrospective review of the use of ASIF as definitive treatment of unstable pelvic fractures. All patients in the study tolerated the construct well. LFCN irritation was seen in 30% of patients, and resolved in all but one patient.
Müller et al. present a retrospective review of the use of posterior stabilization and ASIF. They report an acceptably low complication rate, and good to excellent outcomes in 64.5% of patients.
Figure A is a radiograph demonstrating a right APC3 and left APC2 pelvic injury, imaged in a pelvic binder. Figure B is a postoperative radiograph following posterior stabilization and ASIF.
Incorrect answers:
Answer 1: Weakness of hip flexion would be due to injury to the femoral nerve, which is not commonly associated with this construct.
Answer 2: Weakness of ankle dorsiflexion would be due to injury to the L5 nerve root, which does not occur due to ASIF placement.
Answer 3: Numbness of the medial thigh is due to injury to the obturator nerve, which is not commonly associated with this construct.
Answer 5: Numbness of the perineum is due to injury to the sacral nerve roots, which is not commonly associated with this construct.
Unstable pelvic fractures can be treated in a multitude of ways. The ASIF construct is typically created by placing long pelvic screws or polyaxial pedicle screws in the supraacetabular region, similar to the supraacetabular pins for an
anterior external fixator. Then a curved bar is placed subcutaneously and connected to the supraacetabular screws. They are typically removed after 3-4 months when fracture healing is complete.
Vaidya et al. present a retrospective review of the use of ASIF as definitive treatment of unstable pelvic fractures. All patients in the study tolerated the construct well. LFCN irritation was seen in 30% of patients, and resolved in all but one patient.
Müller et al. present a retrospective review of the use of posterior stabilization and ASIF. They report an acceptably low complication rate, and good to excellent outcomes in 64.5% of patients.
Figure A is a radiograph demonstrating a right APC3 and left APC2 pelvic injury, imaged in a pelvic binder. Figure B is a postoperative radiograph following posterior stabilization and ASIF.
Incorrect answers:
Answer 1: Weakness of hip flexion would be due to injury to the femoral nerve, which is not commonly associated with this construct.
Answer 2: Weakness of ankle dorsiflexion would be due to injury to the L5 nerve root, which does not occur due to ASIF placement.
Answer 3: Numbness of the medial thigh is due to injury to the obturator nerve, which is not commonly associated with this construct.
Answer 5: Numbness of the perineum is due to injury to the sacral nerve roots, which is not commonly associated with this construct.
Question 25High Yield
A patient has pain 2 years after undergoing a metal-on-metal (MOM) left total hip arthroplasty (THA). Which
test(s) best correlate with a prognosis if this patient is having a reaction to metal debris?
test(s) best correlate with a prognosis if this patient is having a reaction to metal debris?
Explanation
Painful MOM THA and taper corrosion can cause substantial damage to a patient's hip if left untreated. In this case, the workup for a painful MOM THA starts the same as a workup for a painful metal-on- polyethylene bearing couple. Infection must be ruled out in every case with a set of inflammatory markers. If these markers are remotely elevated, this is an indication for joint aspiration. In patients with metal debris, the pathology report often indicates too many cells to count or cellular debris. Metal ion levels do not seem to correlate with prognosis. There are well-functioning patients with high ion levels and poor- functioning patients with low ion levels. Advanced imaging with MARS MRI to evaluate for peritrochanteric fluid collection, a soft-tissue mass, or synovial/capsular hypertrophy will reveal signs of a metal reaction that indicate the need for a revision discussion. A CT scan can show more advanced bony destruction as an indicator of poor prognosis. These films can be used to determine the need for a structural graft or augments for reconstruction of bone loss attributable to metal debris.
Question 26High Yield
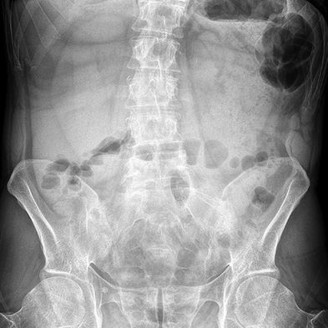
The condition shown in Figures 64a through 64d is overrepresented among craniosynostosis syndromes with mutations in
Explanation
- FGFR-1, FGFR-2, and FGFR-3.
Question 27High Yield
A 22-year-old swimmer underwent thermal capsulorrhaphy treatment for recurrent anterior subluxation. Following 3 weeks in a sling, an accelerated rehabilitation program allowed him to return to swimming in 3 1/2 months. While practicing the butterfly stroke, he sustained an anterior dislocation. He now continues to have symptoms of anterior instability and has elected to have further surgery. Surgical findings may
include a
include a
Explanation
Complications of thermal capsule shrinkage or accelerated rehabilitation include capsule ablation. Since the original surgery did not include labral reattachment, findings of a Bankart lesion or a glenoid fracture from a nontraumatic injury are unlikely. Subscapularis detachment or biceps subluxation is a postoperative complication of open repairs. Failure of early postoperative instability treatment should not produce loose bodies.
REFERENCES: Abrams JS: Thermal capsulorrhaphy for instability of the shoulder: Concerns and applications of the heat probe. Instr Course Lect 2001;50:29-36.
Hecht P, Hayashi K, Lu Y, et al: Monopolar radiofrequency energy effects on joint capsular tissue: Potential treatment for joint instability. An in vivo mechanical, morphological, and biochemical study using an ovine model. Am J Sports Med 1999;27:761-771.
REFERENCES: Abrams JS: Thermal capsulorrhaphy for instability of the shoulder: Concerns and applications of the heat probe. Instr Course Lect 2001;50:29-36.
Hecht P, Hayashi K, Lu Y, et al: Monopolar radiofrequency energy effects on joint capsular tissue: Potential treatment for joint instability. An in vivo mechanical, morphological, and biochemical study using an ovine model. Am J Sports Med 1999;27:761-771.
Question 28High Yield
A 10‘/2-year-old boy sustained the injury shown in Figure 72 when he fell out of a tree. This is a closed, neurologically intact injury and the patient has no head injury or loss of consciousness. He weighs 115 pounds and is otherwise healthy. What is the optimal treatment option for this injury?


Explanation
DISCUSSION: Although flexible intramedullary nails are a good treatment alternative for femoral shaft fractures in older children, patients weighing more than 100 pounds have a higher incidence of complications that include bending of the nails. Therefore, transtrochanteric solid intramedullary nail fixation is most likely the best option for this patient. Using a greater trochanteric entry point avoids the piriformis fossa and the possibility of osteonecrosis. External fixation is not a good alternative for this patient because of the transverse nature of the fracture. External fixation of this fracture pattern has been associated with a high refracture rate. Traction and casting can be performed but results in a lengthy hospital stay and a very large cast in an overweight 10-year-old child.
REFERENCES: Flynn JM, Schwend RM: Management of pediatric femoral shaft fractures. J Am Acad Orthop Surg 2004;12:347-359.
Gordon JE, Swenning TA, Burd TA, et al: Proximal femoral radiographic changes after lateral transtrochanteric intramedullary nail placement in children. J Bone Joint Surg Am 2003;85:1295-1301.
62 • American Academy of Orthopaedic Surgeons
Figure 71a Figure 71b Figure 71c Figure 71d Question 71
A 10-year-old child was referred for spinal curvature and a 2-year history of back pain. She has pain during the day and pain at night that wakes her from sleep and is temporarily relieved with nonsteroidal anti-inflammatory drugs. Examination shows very tight hamstrings and an irritative spinal curvature. Figures 71a through 7Id show radiographs, a bone scan, and a CT scan. What is the most appropriate treatment?
1. ##### Bracing with a thoracolumbosacral orthosis (TLSO)
2. ##### Observation with repeat radiographs of the scoliosis in 3 months and nonsteroidal antiinflammatory drugs for the pain
3. ##### MRI of the neuro-axis
4. ##### Surgical removal
5. ##### Radiofrequency ablation
PREFERRED RESPONSE: 4
DISCUSSION: The history, examination findings, and studies are consistent with an osteoid osteoma. The CT scan shows a classic “target” lesion, and the bone scan has intense uptake at the site of the osteoid osteoma. The child has had a 2-year history of pain that even wakes her from sleep, so observation and anti-inflammatory drugs is not a preferred treatment. Bracing will not help with the discomfort because the pain is not mechanical in nature. MRI would not be needed in addition to the studies already completed. The osteoid osteoma is close to the spinal cord so radiofrequency ablation is not preferred. Surgical removal and biopsy is the treatment of choice.
REFERENCES: Frassica FJ, Waltrip RL, Sponseller PD, et al: Clinicopathologic features and treatment of osteoid osteoma and osteoblastoma in children and adolescents. Orthop Clin North Am 1996;27:559-
574/. Cantwell CP, Obyme J, Eustace S: Current trends in treatment of osteoid osteoma with an emphasis on radiofrequency ablation. Eur Radiol 2004;14:607-617.
2010 Pediatric Orthopaedic Examination Answer Book • 63
Figure 72
DISCUSSION: Although flexible intramedullary nails are a good treatment alternative for femoral shaft fractures in older children, patients weighing more than 100 pounds have a higher incidence of complications that include bending of the nails. Therefore, transtrochanteric solid intramedullary nail fixation is most likely the best option for this patient. Using a greater trochanteric entry point avoids the piriformis fossa and the possibility of osteonecrosis. External fixation is not a good alternative for this patient because of the transverse nature of the fracture. External fixation of this fracture pattern has been associated with a high refracture rate. Traction and casting can be performed but results in a lengthy hospital stay and a very large cast in an overweight 10-year-old child.
REFERENCES: Flynn JM, Schwend RM: Management of pediatric femoral shaft fractures. J Am Acad Orthop Surg 2004;12:347-359.
Gordon JE, Swenning TA, Burd TA, et al: Proximal femoral radiographic changes after lateral transtrochanteric intramedullary nail placement in children. J Bone Joint Surg Am 2003;85:1295-1301.
62 • American Academy of Orthopaedic Surgeons
Figure 71a Figure 71b Figure 71c Figure 71d Question 71
A 10-year-old child was referred for spinal curvature and a 2-year history of back pain. She has pain during the day and pain at night that wakes her from sleep and is temporarily relieved with nonsteroidal anti-inflammatory drugs. Examination shows very tight hamstrings and an irritative spinal curvature. Figures 71a through 7Id show radiographs, a bone scan, and a CT scan. What is the most appropriate treatment?
1. ##### Bracing with a thoracolumbosacral orthosis (TLSO)
2. ##### Observation with repeat radiographs of the scoliosis in 3 months and nonsteroidal antiinflammatory drugs for the pain
3. ##### MRI of the neuro-axis
4. ##### Surgical removal
5. ##### Radiofrequency ablation
PREFERRED RESPONSE: 4
DISCUSSION: The history, examination findings, and studies are consistent with an osteoid osteoma. The CT scan shows a classic “target” lesion, and the bone scan has intense uptake at the site of the osteoid osteoma. The child has had a 2-year history of pain that even wakes her from sleep, so observation and anti-inflammatory drugs is not a preferred treatment. Bracing will not help with the discomfort because the pain is not mechanical in nature. MRI would not be needed in addition to the studies already completed. The osteoid osteoma is close to the spinal cord so radiofrequency ablation is not preferred. Surgical removal and biopsy is the treatment of choice.
REFERENCES: Frassica FJ, Waltrip RL, Sponseller PD, et al: Clinicopathologic features and treatment of osteoid osteoma and osteoblastoma in children and adolescents. Orthop Clin North Am 1996;27:559-
574/. Cantwell CP, Obyme J, Eustace S: Current trends in treatment of osteoid osteoma with an emphasis on radiofrequency ablation. Eur Radiol 2004;14:607-617.
2010 Pediatric Orthopaedic Examination Answer Book • 63
Figure 72
Question 29High Yield
With a full-thickness articular cartilage injury, the body’s healing response produces cartilage mainly composed of what type of collagen?
Explanation
With a full-thickness articular cartilage injury, a healing response is initiated with hematoma, stem cell migration, and vascular ingrowth. This response produces type I collagen and resultant fibrous cartilage rather than desired hyaline cartilage as produced by chondrocytes. This repair cartilage has diminished resiliency, stiffness, poor wear characteristics, and the predilection for arthritis. Type I collagen is also found in the annulus of intervertebral disks, tendon, bone, meniscus, and skin. Type II is found in articular cartilage and nucleus pulposus of intervertebral disks. Type III is found in skin and blood vessels, type IV is found in basement membranes, and type X is found in the calcified layer of cartilage.
REFERENCES: Arendt EA (ed): Orthopaedic Knowledge Update: Sports Medicine 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 19-28.
Brinker M: Basic Science in Review of Orthopaedics, ed 3. Philadelphia, PA,
WB Saunders, 2000.
REFERENCES: Arendt EA (ed): Orthopaedic Knowledge Update: Sports Medicine 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 19-28.
Brinker M: Basic Science in Review of Orthopaedics, ed 3. Philadelphia, PA,
WB Saunders, 2000.
Question 30High Yield
A 66-year-old woman presents with pain and a worsening deformity of her right knee after a total knee arthroplasty (TKA) 5 years ago. She has a complete work-up and is diagnosed with aseptic loosening of the tibia. She is 5’6” in height and 185 pounds. Her preoperative nasal screening shows she is negative for methicillin-resistant Staphylococcus aureus. Based on laxity on physical examination and bone loss, she was indicated for a full revision procedure. She has no known drug allergies and her past medical history is significant for osteoarthritis, hypertension and hypercholesterolemia. The patient undergoes an uncomplicated revision TKA with intraoperative testing confirming aseptic loosening. Based on the patient’s history, what is the most appropriate antibiotic prophylaxis for this patient?
Explanation
89
Historically, cefazolin has been used as a common prophylactic antibiotic for total hip arthroplasty (THA) and TKA. Traditionally, a 1-gram dose was given to patients; however, this has more recently evolved to weight-based dosing. Recommended dosing is currently 1 gram if less than 60 kg, 2 grams if between 60 kg to 120 kg and 3 grams if weighing >120 kg. Rondon and associates recently showed that underdosed patients, a situation that commonly occurs, are at higher risk for periprosthetic joint infection. Our patient falls between 60 kg to 120 kg and should receive 2-gram dosing. As she is not allergic to penicillin or cephalosporins, clindamycin is not an appropriate choice. Further, recent studies have shown no benefit in extended antibiotic use in cases of aseptic revision THA or TKA. This makes the dosing of <24 hours the most appropriate option.
Historically, cefazolin has been used as a common prophylactic antibiotic for total hip arthroplasty (THA) and TKA. Traditionally, a 1-gram dose was given to patients; however, this has more recently evolved to weight-based dosing. Recommended dosing is currently 1 gram if less than 60 kg, 2 grams if between 60 kg to 120 kg and 3 grams if weighing >120 kg. Rondon and associates recently showed that underdosed patients, a situation that commonly occurs, are at higher risk for periprosthetic joint infection. Our patient falls between 60 kg to 120 kg and should receive 2-gram dosing. As she is not allergic to penicillin or cephalosporins, clindamycin is not an appropriate choice. Further, recent studies have shown no benefit in extended antibiotic use in cases of aseptic revision THA or TKA. This makes the dosing of <24 hours the most appropriate option.
Question 31High Yield
The most common type of chronic inflammatory arthritis in childhood is:
Explanation
Forty percent to 60% of children afflicted with juvenile rheumatoid arthritis (JRA) have the pauciarticular subtype. Polyarticular JRA is the second most common type occurring in 30%-40%. Systemic onset JRA is the least common form and occurs in approximately 20% of children. Seronegative spondyloarthropathy is more rare in patients 8 years of age. It is associated with haplotype HLA-B27. The long-term prognosis in these children is generally good.
Question 32High Yield
A 13-year-old boy hyperextends his knee while playing basketball and reports a pop that is followed by a rapid effusion. A lateral radiograph is shown in Figure 4. Initial management consists of attempted reduction with extension, with no change in position of the fragment. What is the next most appropriate step in management?
Explanation
Avulsion fractures of the tibial spine are rare injuries that result from rapid deceleration or hyperextension of the knee in skeletally immature individuals. This injury is the equivalent of ruptures of the anterior cruciate ligament in adults. These fractures are classified as types 1 through 3. Type 1 is a minimally displaced fracture, type 2 fractures have an intact posterior hinge, and type 3 fractures have complete separation. The radiograph demonstrates a completely displaced, or type III, tibial spine avulsion. Surgical reduction is indicated in type 2 fractures that fail to reduce with knee extension and in all type 3 fractures. Reduction may be arthroscopic or open, with fixation of the bony fragment using a method that maintains physeal integrity and prevents later growth arrest. Preferred techniques would be with suture or an intra-epiphyseal screw
REFERENCES: Wiley JJ, Baxter MP: Tibial spine fractures in children. Clin Orthop 1990;255:54-60.
Mulhall KJ, Dowdall J, Grannell M, et al: Tibial spine fractures: An analysis of outcome in surgically treated type III injuries. Injury 1999;30:289-292.
Owens BD, Crane GK, Plante T, et al: Treatment of type III tibial intercondylar eminence fractures in skeletally immature athletes. Am J Orthop 2003;32:103-105.
Vocke AK, Vocke AR: Cartilaginous avulsion fracture of the tibial spine. Orthopedics 2002;25:1293-1294.
REFERENCES: Wiley JJ, Baxter MP: Tibial spine fractures in children. Clin Orthop 1990;255:54-60.
Mulhall KJ, Dowdall J, Grannell M, et al: Tibial spine fractures: An analysis of outcome in surgically treated type III injuries. Injury 1999;30:289-292.
Owens BD, Crane GK, Plante T, et al: Treatment of type III tibial intercondylar eminence fractures in skeletally immature athletes. Am J Orthop 2003;32:103-105.
Vocke AK, Vocke AR: Cartilaginous avulsion fracture of the tibial spine. Orthopedics 2002;25:1293-1294.
Question 33High Yield
Thoracic disk herniations most typically occur at what level of the thoracic spine?
Explanation
Most thoracic disk herniations occur in the lower (caudal) third of the thoracic spine. This predilection may be related to the unique anatomic and biomechanical environment of that region. The 11th and 12th ribs do not join the rib cage anteriorly and do not form a true articulation with the transverse processes posteriorly.
Furthermore, flexion and torsional forces tend to concentrate between T10 and L1.
Furthermore, flexion and torsional forces tend to concentrate between T10 and L1.
Question 34High Yield
What is the most common physical finding in myelopathic patients?
Explanation
The Hoffman sign is the most common finding, occurring in 80% of myelopathic patients,and it is more common with increasing severity of the myelopathy. The prevalence of hyperreflexia has been shown to be no different from the prevalence in individuals without myelopathy. Sustained clonus and Babinski signs have been shown to occur in only one third of the patients with myelopathy.
Question 35High Yield
An 18-month-old boy presents with a clawing deformity of the right hand. He was born full term after a difficult delivery complicated by shoulder dystocia. He weighed 9.5 lbs at birth. The patient had a brief episode of apnea with an APGAR score of
5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patientâs right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Hornerâs syndrome and the grasp reflex is absent.
The level of the lesion in this patient is:
5 at birth and needed resuscitation and admission to the neonatal intensive care unit. A tender bump was noted on the patientâs right clavicle, which was diagnosed as clavicle fracture. A week later, the patient could not flex the fingers of his right hand. The neonatologist informed the parents that the fracture was managed conservatively and the absence of finger flexion was due to fracture and would recover. However, recovery can be prolonged and may take up to two years. The patient has grown and his immunization is complete. His right hand has extension at all the metacarpal joints of the fingers while the proximal interphalangeal and distal interphalangeal joints are flexed. The thumb is in an adducted position, and it is difficult to passively bring the thumb to full abduction. There is obvious wasting of the hand and forearm. The patient moves the arm well with no abnormalities noticed at the shoulder, elbow, and wrist. Radiograph of the chest shows a healed clavicle fracture with no evidence of diaphragmatic paralysis. There is no evidence of Hornerâs syndrome and the grasp reflex is absent.
The level of the lesion in this patient is:
Explanation
It is difficult to clinically differentiate between a pre- and postganglionic lesion of C 8, T1 in a child. Absence of Hornerâs syndrome and hemi-diaphragmatic palsy in this case indicates that this is not a preganglionic lesion. The ability of the patient to hold his
head suggests that the paravertebral muscles are functional, as is true in postganglionic lesions.
head suggests that the paravertebral muscles are functional, as is true in postganglionic lesions.
Question 36High Yield
Figures 74a and 74b are the MR images of a 36-year-old man with a 3-month history of excruciating left leg pain. Which finding upon examination would be most consistent with the MR images?
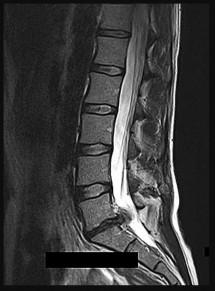
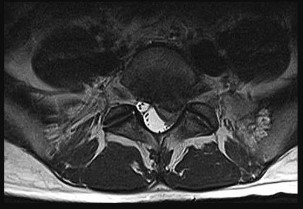
Explanation
The MR images show a classic posterolateral disk herniation at L5-S1. This location affects the traversing nerve root (at L5-S1, the S1 nerve root). The S1 dermatome innervates the plantar aspect of the foot and primarily contributes to ankle plantar flexion and foot eversion. Hip adduction and quadriceps are controlled via the obturator nerve L2-4 innervation, and ankle dorsiflexion is controlled via L4 or L5 innervation. The L2 and L3 dermatomes provide sensation in the anteromedial thigh, L4 provides sensation along the anterolateral leg down to the medial malleolus, L5 provides sensation along the anterolateral leg to the dorsum of the foot, and S1 provides sensation along the posterior leg to the lateral foot.
RECOMMENDED READINGS
14. [Rhee JM, Schaufele M, Abdu WA. Radiculopathy and the herniated lumbar disk: controversies regarding pathophysiology and management. Instr Course Lect.2007;56:287-99. Review. PubMed PMID: 17472314. ](http://www.ncbi.nlm.nih.gov/pubmed/17472314)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17472314)
15. Mixter WJ, Barr JS. Rupture of the intervertebral disk with involvement of the spinal canal. N Engl J Med. 1934: 211: 210-5.
RECOMMENDED READINGS
14. [Rhee JM, Schaufele M, Abdu WA. Radiculopathy and the herniated lumbar disk: controversies regarding pathophysiology and management. Instr Course Lect.2007;56:287-99. Review. PubMed PMID: 17472314. ](http://www.ncbi.nlm.nih.gov/pubmed/17472314)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17472314)
15. Mixter WJ, Barr JS. Rupture of the intervertebral disk with involvement of the spinal canal. N Engl J Med. 1934: 211: 210-5.
Question 37High Yield
Because of the ongoing pain and instability and the demonstration of radiographic instability when the ankle is stressed, what surgical procedure should be performed to restore stability to the ankle joint based on the CT findings?
Explanation
_**
**_
_**DISCUSSION FOR QUESTIONS 107 AND 108:**_
The fracture at the insertion of the AITFL into the fibula represents a syndesmosis injury. In some cases, a direct repair of the fracture will stabilize the syndesmosis, but in most cases this injury should most likely be reinforced by placing a screw or suture tensioning device across the syndesmosis for additional support.A Brostrom or allograft reconstruction is indicated for an ankle sprain involving the ATFL or CFL.Simply excising the fragment will leave the patient with an incompetent syndesmosis. Repairing the SPR with or without a groove deepening procedure is indicated if there is evidence of subluxated or dislocated peroneal tendons, which is not demonstrated on the CT scans. The bone has been avulsed off the fibula by the portion of the AITFL that attaches to the fibula, therefore indicating that there is a syndesmosis injury. Allograft lateral ligament reconstruction and excision of loose body/fracture fragment are incorrect procedures based on location. The deltoid is a medial structure and this fracture is lateral. The ATFL and CFL attach at the inferior margin of the fibula near the lateral process of the talus and calcaneus. A SPR avulsion would present as an avulsion off the lateral wall of the fibula, not superior and not into the syndesmotic space as shown on the CT scans.
**_
_**DISCUSSION FOR QUESTIONS 107 AND 108:**_
The fracture at the insertion of the AITFL into the fibula represents a syndesmosis injury. In some cases, a direct repair of the fracture will stabilize the syndesmosis, but in most cases this injury should most likely be reinforced by placing a screw or suture tensioning device across the syndesmosis for additional support.A Brostrom or allograft reconstruction is indicated for an ankle sprain involving the ATFL or CFL.Simply excising the fragment will leave the patient with an incompetent syndesmosis. Repairing the SPR with or without a groove deepening procedure is indicated if there is evidence of subluxated or dislocated peroneal tendons, which is not demonstrated on the CT scans. The bone has been avulsed off the fibula by the portion of the AITFL that attaches to the fibula, therefore indicating that there is a syndesmosis injury. Allograft lateral ligament reconstruction and excision of loose body/fracture fragment are incorrect procedures based on location. The deltoid is a medial structure and this fracture is lateral. The ATFL and CFL attach at the inferior margin of the fibula near the lateral process of the talus and calcaneus. A SPR avulsion would present as an avulsion off the lateral wall of the fibula, not superior and not into the syndesmotic space as shown on the CT scans.
Question 38High Yield
A 86-year-old man slips on the ice and falls sustaining the injury shown in Figure A. He has Type 2 diabetes mellitus, atrial fibrillation, coronary artery disease, end-stage renal disease on dialysis and chronic obstructive lung disease. All of the following variables are associated with increased mortality at one year after injury EXCEPT?
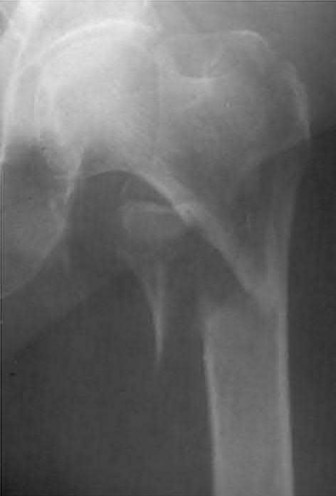
Explanation
Operative fixation within 48 hours is not associated with increased mortality. However, operative delay of 3 or more days results in increased mortality.
Medical optimization and surgery for hip fractures in elderly patients should be performed as soon as possible following admission to hospital. Surgical intervention in elderly hip fracture patients reduces morbidity and mortality.
Postoperatively, weightbearing as tolerated decreases the risk for poor outcomes and decreases complications e.g. muscle atrophy, pressure sores, pneumonia, urinary retention.
Zuckerman et al. reviewed mortality associated with operative delay in older patients with hip fractures. They found that operative delay of 3 or more calendar days results in greater 1-year mortality. Other predictors of mortality include age >85yrs, male sex, presence of 2 or more pre-existing medical conditions, ASA grade III or IV, and inter-trochanteric fracture.
Switzer et al. reviewed perioperative considerations in the geriatric patient. They showed that hip fracture repair after 2 days results in decrease in independent living, pressure sores and longer hospital stay. They found with early surgery, pain, length of hospital stay and 1-month mortality was reduced.
Figure A shows unstable intertrochanteric fracture. Incorrect Answers:
Answers 1, 2, 3: These conditions are all associated with increased 1-year
mortality.
Answer 4: One-year mortality after hip fracture is greater in men (25-30%) than in women (20%).
Medical optimization and surgery for hip fractures in elderly patients should be performed as soon as possible following admission to hospital. Surgical intervention in elderly hip fracture patients reduces morbidity and mortality.
Postoperatively, weightbearing as tolerated decreases the risk for poor outcomes and decreases complications e.g. muscle atrophy, pressure sores, pneumonia, urinary retention.
Zuckerman et al. reviewed mortality associated with operative delay in older patients with hip fractures. They found that operative delay of 3 or more calendar days results in greater 1-year mortality. Other predictors of mortality include age >85yrs, male sex, presence of 2 or more pre-existing medical conditions, ASA grade III or IV, and inter-trochanteric fracture.
Switzer et al. reviewed perioperative considerations in the geriatric patient. They showed that hip fracture repair after 2 days results in decrease in independent living, pressure sores and longer hospital stay. They found with early surgery, pain, length of hospital stay and 1-month mortality was reduced.
Figure A shows unstable intertrochanteric fracture. Incorrect Answers:
Answers 1, 2, 3: These conditions are all associated with increased 1-year
mortality.
Answer 4: One-year mortality after hip fracture is greater in men (25-30%) than in women (20%).
Question 39High Yield
Figure 43 shows the lateral radiograph of a patient who underwent anterior cruciate ligament reconstruction. Based on the tunnel placement shown in the radiograph, evaluation of postoperative knee range of motion will most likely show
Explanation
The radiograph shows the correct tibial tunnel and anterior femoral tunnel; therefore, range of motion will most likely show loss of flexion.
REFERENCES: Brown CH Jr, Carson EW: Revision anterior cruciate ligament surgery. Clin
Bernhardt DT, Landry GL: Sports injuries in young athletes. Adv Pediatr 1995;42:465- Sports Med 1999;18:109-171.
Brown HR, Indelicato PA: Complications of anterior cruciate ligament reconstruction. Op Tech Orthop 1992;2:125-135.
REFERENCES: Brown CH Jr, Carson EW: Revision anterior cruciate ligament surgery. Clin
Bernhardt DT, Landry GL: Sports injuries in young athletes. Adv Pediatr 1995;42:465- Sports Med 1999;18:109-171.
Brown HR, Indelicato PA: Complications of anterior cruciate ligament reconstruction. Op Tech Orthop 1992;2:125-135.
Question 40High Yield
Advanced imaging, to include MRI and CT, have been obtained in the workup of patients with low back pain. What imaging finding has been associated with reasons for back pain?
Explanation
■
Low back pain remains a common presenting condition to not only primary care physicians, but to subspecialists. Studies assessing the anatomy of the spine, to include the intervertebral disks, vertebral body morphology, facet joints, and the paraspinal muscles have been performed. Spinal stenosis is the only advanced imaging finding that has been associated with reproducible reasons for back pain.
Low back pain remains a common presenting condition to not only primary care physicians, but to subspecialists. Studies assessing the anatomy of the spine, to include the intervertebral disks, vertebral body morphology, facet joints, and the paraspinal muscles have been performed. Spinal stenosis is the only advanced imaging finding that has been associated with reproducible reasons for back pain.
Question 41High Yield
-Clinical staging of osteomyelitis using the Cierney-Mader classification system takes into account which of the following factors?
Explanation
No detailed explanation provided for this question.
Question 42High Yield
1220) A 29-year-old obese patient is transferred from an outside facility for the management of a closed-head injury and the fracture shown in Figure A. He presents to the trauma bay as a transient responder to blood products, and undergoes urgent pre-surgical angiography embolization. Surgery is performed within 8 hours from the time of injury. The patient develops a deep wound infection 1 week post-operatively. Which of the following factors would be considered the MOST statistically significant predictor for post-operative infection in this patient.
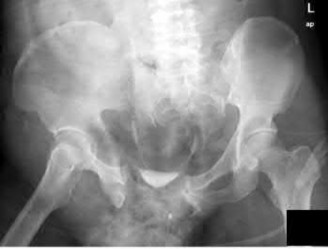
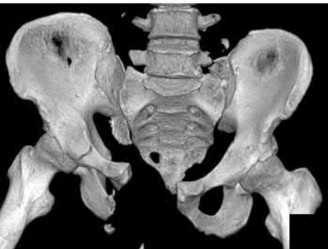
Explanation
From the following options, only obesity has been shown to be associated with a statistically higher incidence of wound complications following pelvic and acetabular fracture fixation for trauma.
Wound complications following pelvic and acetabular fracture fixation is relatively uncommon. Literature suggests and prevalence of 2-8% with closed fracture injuries. Factors shown to increase infection rates include both patient and surgical factors. They include obesity, diabetes, immunocompromised, elderly, pre-operative embolization and open fractures.
Sagi et al. looked at the factors contributing to wound infection after pelvic and acetabular surgery. Open pelvic or acetabular fractures were excluded. Of all the factors, only obesity (OR 8, PPV 33%), obesity plus leukocytosis (OR 12, PPV 39%), and preoperative angioembolization (OR 11, PPV 67%) were strong predictors of postoperative infection.
Manson et al. aimed to determine if embolization of pelvic arterial injuries before open reduction and internal fixation (ORIF) of acetabular fractures is associated with an increased rate of deep surgical site infection. They retrospective reviewed 1440 patients who underwent ORIF of acetabular fractures. They found a 58% infection rate of the patients who underwent embolization before ORIF vs, historical controls (2%-5%) and angiography without embolization (14%).
Figure A shows an AP radiograph and 3D CT reconstruction of a APC3 pelvic ring fracture.
Incorrect Answers:
Answer 1: Head injury has not been shown to increase infection rates. It has been shown to increase heterotrophic ossification.
Answer 3: Gender has not shown to increase infection rates
Answer 4: Early surgery has not been shown to affect infection rates. Answer 5: Transfer from an outside facility has not been shown to affect infection rates.
Wound complications following pelvic and acetabular fracture fixation is relatively uncommon. Literature suggests and prevalence of 2-8% with closed fracture injuries. Factors shown to increase infection rates include both patient and surgical factors. They include obesity, diabetes, immunocompromised, elderly, pre-operative embolization and open fractures.
Sagi et al. looked at the factors contributing to wound infection after pelvic and acetabular surgery. Open pelvic or acetabular fractures were excluded. Of all the factors, only obesity (OR 8, PPV 33%), obesity plus leukocytosis (OR 12, PPV 39%), and preoperative angioembolization (OR 11, PPV 67%) were strong predictors of postoperative infection.
Manson et al. aimed to determine if embolization of pelvic arterial injuries before open reduction and internal fixation (ORIF) of acetabular fractures is associated with an increased rate of deep surgical site infection. They retrospective reviewed 1440 patients who underwent ORIF of acetabular fractures. They found a 58% infection rate of the patients who underwent embolization before ORIF vs, historical controls (2%-5%) and angiography without embolization (14%).
Figure A shows an AP radiograph and 3D CT reconstruction of a APC3 pelvic ring fracture.
Incorrect Answers:
Answer 1: Head injury has not been shown to increase infection rates. It has been shown to increase heterotrophic ossification.
Answer 3: Gender has not shown to increase infection rates
Answer 4: Early surgery has not been shown to affect infection rates. Answer 5: Transfer from an outside facility has not been shown to affect infection rates.
Question 43High Yield
Which of the following molecules play an important role in cartilage hypertrophy during growth plate development and ossification in fracture healing:
Explanation
Important concepts to remember regarding signaling proteins include:
Indian hedgehog (IHH) and core binding factor alpha 1 (Cbfa1) influence embryoniCbone formation and fracture healing. Vascular endothelial growth factor (VEGF) plays a role in cartilage hypertrophy at the growth plate and during fracture healing.
Transforming growth factor-beta (TGF-B) and platelet derived growth factor (PDGF) are found in early fracture hematoma, and these factors modulate cell proliferation and differentiation.
Bone morphogenetiCprotein and interleukin 1 and 6 are expressed during cartilage formation. Correct Answer: Vascular endothelial growth factor (VEGF)
Indian hedgehog (IHH) and core binding factor alpha 1 (Cbfa1) influence embryoniCbone formation and fracture healing. Vascular endothelial growth factor (VEGF) plays a role in cartilage hypertrophy at the growth plate and during fracture healing.
Transforming growth factor-beta (TGF-B) and platelet derived growth factor (PDGF) are found in early fracture hematoma, and these factors modulate cell proliferation and differentiation.
Bone morphogenetiCprotein and interleukin 1 and 6 are expressed during cartilage formation. Correct Answer: Vascular endothelial growth factor (VEGF)
Question 44High Yield
..If the patient were a college pitcher with a similar presentation and examination, what structure would most likely be injured?
Explanation
- Plain radiographs of both elbows PREFERRED RESPONSE: 1- To evaluate for apophyseal injury PREFERRED RESPONSE: 1- Ulnar collateral ligament
Question 45High Yield
Figure 1 is the T2 coronal MRI scan of a 52-year-old woman with a 6- month history of shoulder pain. She does not recall a history of trauma. Physical therapy is recommended. What is the most significant predictor of failure of nonoperative treatment?
Explanation
The MRI reveals a large full thickness supraspinatus tear. A large, prospective study showed that physical therapy can be effective in the treatment of atraumatic full-thickness rotator cuff tears. Patient expectations regarding the role of rehabilitation were the strongest predictor of surgery. Other
factors associated with surgery were higher activity level and not smoking. Anatomic features of the rotator cuff tear and the severity of patient’s reported pain did not predict failure of nonoperative treatment. Patients who have low expectations regarding the effectiveness of physical therapy are more likely to fail nonoperative treatment.
factors associated with surgery were higher activity level and not smoking. Anatomic features of the rotator cuff tear and the severity of patient’s reported pain did not predict failure of nonoperative treatment. Patients who have low expectations regarding the effectiveness of physical therapy are more likely to fail nonoperative treatment.
Question 46High Yield
A 28 year-old-male presents with the injury pattern seen in Figure A. Which of the following is a risk factor for wound complications following operative treatment?
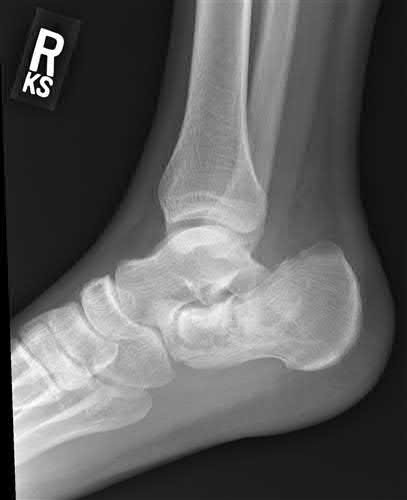
Explanation
According to the referenced study by Folk et al, the risk of early wound complications is highest in open injuries, diabetics, and smokers.
No significant differences were seen in complication rates in terms of: age, sex, other pre-existing medical conditions, social history, mechanism of injury, time from injury to surgical stabilization, the type of incision used, use of preoperative antibiotics, or type of wound closure.
Notably, 25% of the patients had some sort of early wound complication, and 21% of the patients required surgical treatment due to their wound complication.
Their conclusion: "Smoking, diabetes, and open fractures all increase the risk of wound complication after surgical stabilization of calcaneus fractures.
Cumulative risk factors increase the likelihood of wound complications."
No significant differences were seen in complication rates in terms of: age, sex, other pre-existing medical conditions, social history, mechanism of injury, time from injury to surgical stabilization, the type of incision used, use of preoperative antibiotics, or type of wound closure.
Notably, 25% of the patients had some sort of early wound complication, and 21% of the patients required surgical treatment due to their wound complication.
Their conclusion: "Smoking, diabetes, and open fractures all increase the risk of wound complication after surgical stabilization of calcaneus fractures.
Cumulative risk factors increase the likelihood of wound complications."
Question 47High Yield
A 69-year-old patient with diabetes has had acute-onset back pain and difficulty with ambulation for several hours. Evaluation reveals a temperature of 38.3°C, a white blood cell (WBC) count of 14000/µL (reference range [rr], 4500-11000/µL), C-reactive protein (CRP) level of 120 mg/L (rr, 0.08-3.1 mg/L), erythrocyte sedimentation rate of 130 mm/h (rr, 0-20 mm/h), normal rectal examination findings, and normal sensation to light touch. Motor function testing of the lower extremities reveals 3/5 ankle dorsiflexion and 4/5 plantar flexion strength bilaterally. An MR image reveals a large epidural abscess from L1-5. What is the most appropriate treatment at this time?
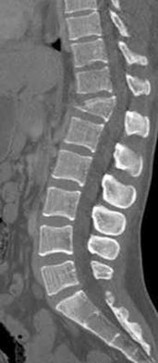
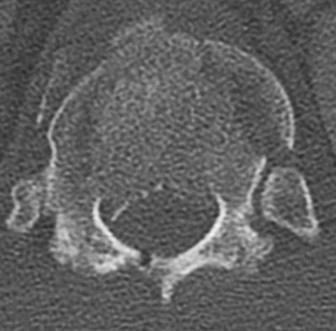
Explanation
Epidural abscess is a serious and potentially disastrous condition. Although medical management is effective in some situations, surgical decompression is considered urgent with the presence of a neurological deficit. Medical management can be considered in the case of a neurologically intact patient, particularly when the microorganism has been identified. If medical management is chosen, careful observation and serial examination for neurologic deterioration is required. Surgical decompression is indicated if a patient's neurologic status worsens or if medical management failure is noted. Additionally, diabetes, a CRP level higher than 115 mg/L, WBC higher than 12500/µL , and bacteremia have proven predictive of medical treatment failure. This patient would be a better candidate for urgent surgical decompression and subsequent IV antibiotics than for medical management.
RECOMMENDED READINGS
[Patel AR, Alton TB, Bransford RJ, Lee MJ, Bellabarba CB, Chapman JR. Spinal epidural abscesses: risk factors, medical versus surgical management, a retrospective review of 128 cases. Spine J. 2014 Feb 1;14(2):326-30. doi: 10.1016/j.spinee.2013.10.046. Epub 2013 Nov 12. PubMed PMID: 24231778.](http://www.ncbi.nlm.nih.gov/pubmed/24231778)[View ](http://www.ncbi.nlm.nih.gov/pubmed/24231778)[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24231778)
Kim SD, Melikian R, Ju KL, Zurakowski D, Wood KB, Bono CM, Harris MB. Independent predictors of failure of nonoperative management of spinal epidural abscesses. Spine J. 2014 Aug 1;14(8):1673-9. doi: 10.1016/j.spinee.2013.10.011. Epub 2013 Oct 30. PubMed PMID:
[24373683/. ](http://www.ncbi.nlm.nih.gov/pubmed/24373683)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24373683)
CLINICAL SITUATION FOR QUESTIONS 96 AND 97
Figures 96a and 96b are the CT scans of a 32-year-old man who was thrown from his motorcycle. He has humeral shaft and femoral shaft fractures. A secondary survey reveals substantial tenderness to his lower thoracic spine. He is awake and alert and his movement is limited by pain secondary to the extremity fractures. He is otherwise neurologically intact.
A B
RECOMMENDED READINGS
[Patel AR, Alton TB, Bransford RJ, Lee MJ, Bellabarba CB, Chapman JR. Spinal epidural abscesses: risk factors, medical versus surgical management, a retrospective review of 128 cases. Spine J. 2014 Feb 1;14(2):326-30. doi: 10.1016/j.spinee.2013.10.046. Epub 2013 Nov 12. PubMed PMID: 24231778.](http://www.ncbi.nlm.nih.gov/pubmed/24231778)[View ](http://www.ncbi.nlm.nih.gov/pubmed/24231778)[Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24231778)
Kim SD, Melikian R, Ju KL, Zurakowski D, Wood KB, Bono CM, Harris MB. Independent predictors of failure of nonoperative management of spinal epidural abscesses. Spine J. 2014 Aug 1;14(8):1673-9. doi: 10.1016/j.spinee.2013.10.011. Epub 2013 Oct 30. PubMed PMID:
[24373683/. ](http://www.ncbi.nlm.nih.gov/pubmed/24373683)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24373683)
CLINICAL SITUATION FOR QUESTIONS 96 AND 97
Figures 96a and 96b are the CT scans of a 32-year-old man who was thrown from his motorcycle. He has humeral shaft and femoral shaft fractures. A secondary survey reveals substantial tenderness to his lower thoracic spine. He is awake and alert and his movement is limited by pain secondary to the extremity fractures. He is otherwise neurologically intact.
A B
Question 48High Yield
A 55-year-old man with a 4-part proximal humerus fracture with intra-articular comminution and a large greater tuberosity fragment
Explanation
- Hemiarthroplasty_
Question 49High Yield
**CLINICAL SITUATION**
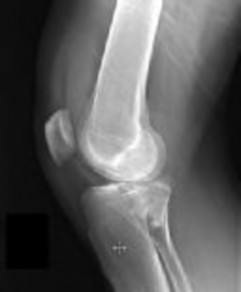
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
This knee injury is best described as a
---
---
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
This knee injury is best described as a
---
---
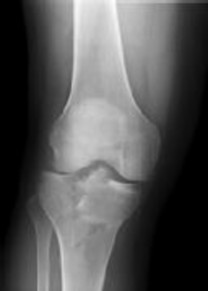
Explanation
Posterior partial articular tibial plateau fractures are rare. Failure to recognize this pattern can lead to poor patient outcomes secondary to poor surgical decision making. Pathognomonic findings on the lateral radiograph include maintenance of continuity between the anterior articular surface and tibial shaft along with subluxation of the knee joint with excessively anterior tibial station (the femoral condyles remain with the fractured posterior articular pieces while the remainder of the tibia subluxes anteriorly).
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Question 50High Yield
Which finding is associated with the highest positive predictive value for the presence of a spiral cord?
Explanation
- Proximal interphalangeal (PIP) joint flexion contracture_
You Might Also Like

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon