Congenital Hand Reconstruction: Toe-Phalanx Transplantation and Ring Syndrome
Key Takeaway
Congenital hand anomalies, including symbrachydactyly and amniotic band sequence, require meticulous surgical intervention to restore function and aesthetics. This guide details the non-vascularized toe-phalanx transplantation technique for absent digits and the staged Z-plasty release for congenital constriction rings. Emphasizing biomechanics, soft-tissue handling, and postoperative protocols, these procedures are essential for optimizing pediatric hand development and preventing progressive neurovascular compromise.
INTRODUCTION TO CONGENITAL HAND RECONSTRUCTION
The management of congenital hand anomalies demands a profound understanding of pediatric biomechanics, longitudinal growth potential, and microvascular anatomy. Among the most challenging presentations are aphalangia (often associated with symbrachydactyly) and Congenital Ring Syndrome (Amniotic Band Sequence). Surgical intervention in these conditions is not merely cosmetic; it is fundamentally reconstructive, aiming to provide a stable, sensate, and functional prehensile unit while mitigating progressive neurovascular compromise.
This comprehensive masterclass details two critical reconstructive pillars: the non-vascularized toe-phalanx transplantation for the absent digit, and the systematic release and reconstruction of congenital constriction rings and associated acrosyndactyly.
TOE-PHALANX TRANSPLANTATION (NON-VASCULARIZED)
Non-vascularized toe-phalanx transfer, pioneered and refined by Toby et al., remains a cornerstone technique for the treatment of symbrachydactyly and transverse deficiencies where a soft-tissue envelope (nubbin) is present but lacks osseous support. The primary goal is to provide longitudinal stability, enhance pinch kinematics, and stimulate the growth of the soft-tissue envelope.
Indications and Patient Selection
The ideal candidate is an infant (typically between 6 and 18 months of age) presenting with symbrachydactyly featuring flail, unsupported digital nubbins. Early intervention is critical to harness the maximal osteogenic and chondrogenic potential of the transferred phalanx and to capitalize on the brain's neuroplasticity for incorporating the new digit into functional prehension.
💡 Clinical Pearl: Growth Potential
Non-vascularized phalangeal transfers rarely achieve normal longitudinal growth. The physes often close prematurely due to transient ischemia before revascularization. However, the transfer reliably provides critical structural stability and prevents the soft-tissue nubbin from contracting, serving as a functional post for opposition.
Preoperative Planning and Biomechanics
Radiographic evaluation of both the hands and feet is mandatory. The proximal phalanx of the third or fourth toe is typically selected as the donor graft. These digits offer the most appropriate size match for the hand while minimizing donor-site morbidity in the foot. The biomechanical success of the transfer relies heavily on harvesting the phalanx extraperiosteally with its capsuloligamentous structures intact, which preserves the chondrocytes and provides a scaffold for soft-tissue adherence in the recipient bed.
Surgical Technique: Step-by-Step
1. Recipient Site Preparation
- Incision: Under tourniquet control and loupe magnification, make a volar zigzag (Bruner-type) incision over the distal palm, extending into the soft-tissue bud of the absent digit.
- Neurovascular Protection: Meticulously identify and protect the rudimentary neurovascular elements. In symbrachydactyly, these structures are often hypoplastic and aberrantly located.
- Pouch Creation: Using a small hemostat, perform blunt dissection to gently spread the soft tissue, creating a precise, well-vascularized cavity (pouch) to accommodate the toe phalanx. Avoid excessive electrocautery to preserve the delicate vascular bed necessary for graft revascularization.
- Tendon Management: Dissect the flexor tendons and their rudimentary anlagen leading to the absent digit. It is imperative to preserve their distal attachments to the soft-tissue pouch.
- Adhesiolysis: Lyse any adhesions proximal to the distal insertion to maximize the excursion of the flexor tendon, which will impart dynamic stability to the reconstructed digit.
2. Donor Site Harvest (Third or Fourth Toe)
- Incision: Make a dorsal diagonal or lazy-S incision over the proximal phalanx of the selected toe.
- Extraperiosteal Dissection: Harvest the phalanx extraperiosteally. Maintaining the periosteal sleeve is critical for preserving the osteoprogenitor cells required for graft survival and potential growth.
- Joint Disarticulation: Incise the soft-tissue attachments of the proximal interphalangeal (PIP) joint flush with the bone.
- En Bloc Resection: At the metatarsophalangeal (MTP) joint, incise the volar plate and collateral ligaments at their metatarsal origins. Remove the toe phalanx capsule, volar plate, medial and lateral collateral ligaments, and accessory collateral ligaments as a single, contiguous unit.
⚠️ Surgical Warning: Donor Site Morbidity
When harvesting the proximal phalanx, ensure meticulous closure of the dead space in the toe. Syndactylization of the donor toe to the adjacent toe (e.g., 3rd to 4th toe) is highly recommended to prevent a "floppy toe" deformity and ensure normal footwear fitting later in life.
3. Graft Placement and Fixation
- Preparation: Pass a small-diameter Kirschner wire (0.028 or 0.035 inch) retrogradely into the proximal aspect of the harvested toe phalanx.
- Insertion: Place the composite phalanx transfer into the prepared soft-tissue pouch in the hand.
- Fixation: Advance the Kirschner wire distally through the soft-tissue envelope, and then drive it proximally into the metacarpal to achieve rigid axial stability. Ensure the volar plate of the graft is oriented volarly to prevent hyperextension deformity.
- Closure: Close the skin with fine absorbable sutures. A bulky, non-compressive soft dressing and a long-arm cast are applied.
Postoperative Protocol
The hand is immobilized in a long-arm cast for 4 to 6 weeks. Following radiographic confirmation of graft incorporation and clinical stability, the Kirschner wire is removed in the clinic. Occupational therapy is initiated immediately to encourage active use, sensory re-education, and integration of the digit into gross motor grasp and fine pinch.
CONGENITAL RING SYNDROME (AMNIOTIC BAND SEQUENCE)
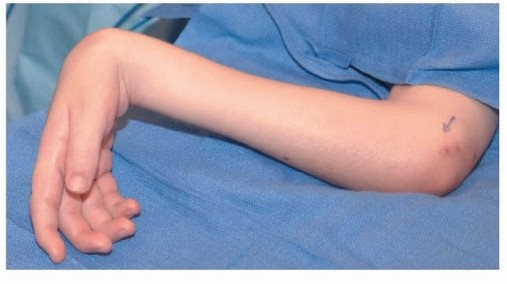
Congenital Ring Syndrome, also known as Amniotic Band Sequence or Streeter Dysplasia, is a complex congenital anomaly characterized by fibrous bands that entangle fetal parts in utero. This results in a spectrum of deformities ranging from simple constriction rings to severe acrosyndactyly and intrauterine amputations.
Pathogenesis and Clinical Presentation
The widely accepted extrinsic theory posits that early rupture of the amnion leads to the formation of mesodermic fibrous bands that encircle fetal limbs.
- Systemic Associations: While generally lacking visceral malformations, 40% to 50% of patients present with associated anomalies such as clubfoot, cleft lip, cleft palate, and cranial defects. (Note: Flatt reported a rare association with patent ductus arteriosus).
- Asymmetry: The malformations are characteristically asymmetrical and sporadic.
- Local Presentation: The grooves vary in depth. Shallow rings may mimic misplaced skin creases. Deep rings cause distal lymphedema, cyanosis, and vascular impairment. Superficial veins and lymphatics are obliterated by the ring, whereas deep arterial structures usually remain intact.
💡 Clinical Pearl: The Progressive Nature of Deep Rings
Constriction rings are not static. A deep, unrelenting ring can cause progressive necrosis, worsening lymphedema, and severe vascular impairment postnatally. Urgent surgical release is mandated if signs of impending ischemia or severe venous congestion are present.
Surgical Management of Constriction Rings
Indications for Surgery
- Emergent/Urgent: Deep rings causing distal cyanosis, severe lymphedema, or impending necrosis.
- Elective: Shallow rings causing cosmetic deformity or mild contour abnormalities, typically addressed after the loss of "baby fat" if they do not resolve spontaneously.
Staged Z-Plasty Technique
Simple excision with direct everting closure is strictly contraindicated due to the high risk of circumferential scar contracture.
- Staging: If the ring completely encircles the digit or limb, the safest, most evidence-based approach is a staged excision. Release only 50% to 60% of the circumference during the first procedure. The remaining portion is released 2 to 3 months later. This prevents catastrophic disruption of the remaining venous and lymphatic drainage.
- Excision: Excise the fibrotic, dysplastic tissue of the ring down to healthy, normal subcutaneous tissue and deep fascia.
- Flap Design: Design multiple 60-degree Z-plasties along the excised groove. The transposition of these triangular flaps lengthens the scar, breaks up the linear contracture, and recruits healthy subcutaneous fat into the deficient area.
- Alternative Approaches: While some authors advocate for simple excision with direct advancement of normal proximal and distal fasciocutaneous tissue, the classic Z-plasty or W-plasty remains the gold standard for preventing recurrent constriction.
Management of Acrosyndactyly
Acrosyndactyly—where the digits are fused distally but possess proximal epithelialized fenestrations (sinus tracts)—is a hallmark of severe amniotic band sequence. The fingertips are often bound together in a disorganized mass, tethering growth and causing progressive joint deformity.
Timing of Release
- Border Digits (Thumb and Small Finger): Release must be performed early, within the first 6 months of life. Freeing the border digits allows for the development of independent pinch and grasp.
- Central Digits: Release of the central digits is typically staged when the child is approximately 18 months old.
Surgical Principles for Acrosyndactyly
- Preservation of Fenestrations: The proximal epithelialized tracts should be preserved and incorporated into the web space reconstruction whenever possible.
- Separation: The distal fusion mass is carefully separated. Because the anatomy is highly distorted, meticulous dissection is required to identify and protect the shared neurovascular bundles.
- Skin Grafting: Full-thickness skin grafts (harvested from the groin or lower abdomen) are almost universally required to cover the extensive soft-tissue defects on the facing aspects of the separated digits.
- Complication Management: Finger stiffness, particularly at the proximal interphalangeal (PIP) joints, is a common postoperative complication due to the underlying symphalangism or prolonged tethering. Aggressive postoperative hand therapy is essential.
Thumb Reconstruction in Ring Syndrome
The thumb is frequently amputated or severely hypoplastic in congenital ring syndrome. Because prehension accounts for 40% to 50% of hand function, restoring thumb length and mobility is paramount.
- Web Space Deepening: For mild shortening, a simple four-flap Z-plasty or dorsal rotational flap to deepen the first web space may provide sufficient relative length to restore opposition.
- Distraction Osteogenesis: For moderate shortening, lengthening of the first metacarpal or proximal phalanx via callus distraction (Ilizarov principles) can yield excellent functional length.
- Søiland’s On-Top Plasty: In cases of severe thumb amputation combined with a severely damaged, non-functional index finger, the Søiland technique is highly effective. This involves transposing the remnant of the shortened index finger onto the top of the thumb residuum as a neurovascular island flap, thereby restoring a functional, sensate thumb post.
Conclusion
The surgical management of congenital hand anomalies requires a master-level synthesis of microvascular precision, biomechanical foresight, and longitudinal planning. Whether executing a delicate extraperiosteal toe-phalanx harvest to reconstruct a symbrachydactyly nubbin, or meticulously staging Z-plasties to salvage a limb from a constricting amniotic band, the orthopedic surgeon must adhere to strict, evidence-based principles. Through timely and precise intervention, profound functional and aesthetic restoration can be achieved, fundamentally altering the developmental trajectory of the pediatric patient.
You Might Also Like