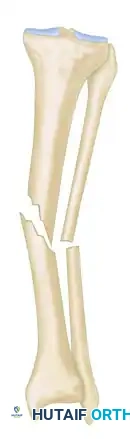
Dynamic External Fixation of PIP Joint Fracture-Dislocations: An Intraoperative Masterclass

Key Takeaway
This masterclass guides fellows through dynamic external fixation for proximal interphalangeal (PIP) joint fracture-dislocations. We meticulously cover surgical anatomy, preoperative planning, and granular, real-time intraoperative execution, including precise K-wire placement and bending techniques. Emphasis is placed on preventing complications, ensuring joint stability, and guiding postoperative rehabilitation for optimal functional recovery.
Welcome, fellows, to the operating theater. Today, we're addressing a challenging yet common injury: the proximal interphalangeal (PIP) joint fracture-dislocation. This procedure, dynamic external fixation, is a powerful tool in our armamentarium for restoring stability and promoting early motion, which is paramount for functional outcomes in the hand. Observe closely, ask questions, and let's delve into the intricacies of this technique.
Understanding PIP Joint Fracture-Dislocations
Let's begin by reviewing the fundamental pathology.
Pathoanatomy and Classification
Pilon fractures, as we often encounter them, represent compression injuries primarily affecting the base of the middle phalanx. Less commonly, they can involve the distal phalanx or the thumb's proximal phalanx. These fractures are characterized by a central articular depression and a splaying of the articular margins, a testament to the axial loading force that causes them.
Injuries to the PIP joint can broadly be categorized based on the affected articular surface:
* Convex-side injuries: These involve the distal end of the proximal phalanx. They are typically simpler, often two-fragment injuries, and are generally amenable to open reduction and internal fixation (ORIF) when surgical intervention is warranted.
* Concave-side injuries: These involve the base of the middle phalanx and are frequently comminuted, presenting either as fracture-subluxations, dislocations, or the pilon fracture pattern we just discussed.
Fracture-subluxations and dislocations most commonly involve a dorsal displacement of the main dorsal fragment of the middle phalanx.
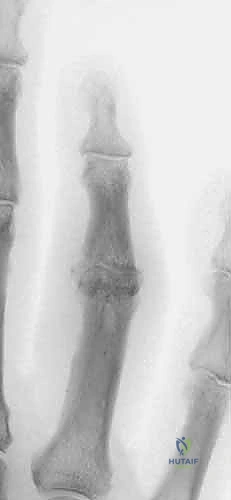
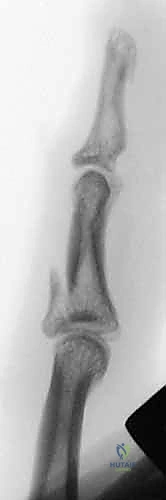
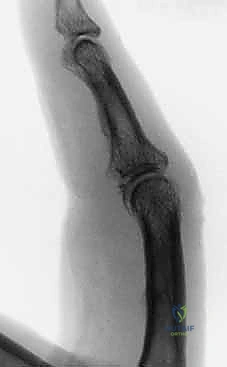
Figure 1A demonstrates a typical, more severe dorsal fracture-dislocation, involving approximately 65% of the volar articular surface.
While less common, we also encounter volar and lateral subluxations and dislocations.
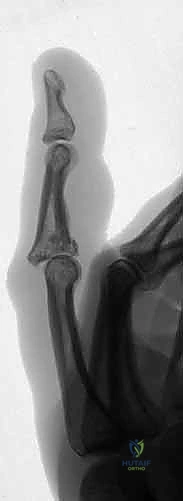
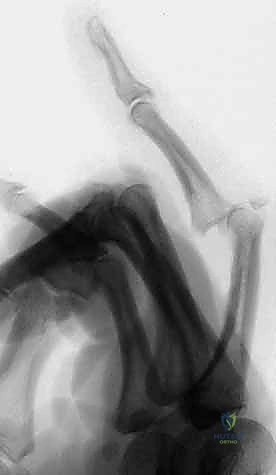
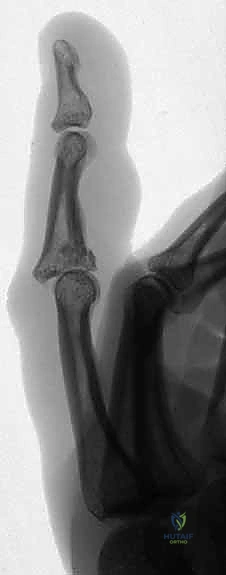
Figures 1B and 1C illustrate proximal interphalangeal joint volar dislocations.
Pilon fractures, specifically, show marked comminution of the middle phalanx base.
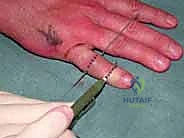
Figures 1D and 1E depict proximal interphalangeal joint pilon fractures.
These injuries typically result from a longitudinal, end-on force, crushing the middle phalanx base, often seen in sports like cricket or baseball, or from a simple fall. Longitudinal fracture extension, reaching most of the middle phalanx length, can also be associated with these injuries.
Biomechanics of Instability
Let's review the critical anatomy that governs PIP joint stability.
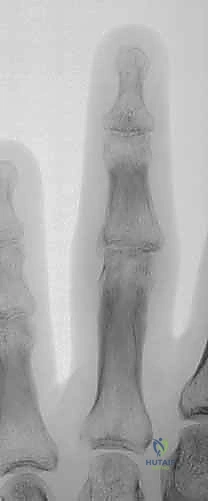
Figure 2A shows the distal end of the proximal phalanx, a convex surface composed of two condyles, articulating with the concave surface of the proximal end of the middle phalanx.
The stability of this joint relies heavily on its ligamentous restraints.

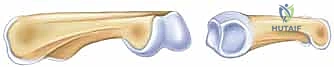
Figure 2B highlights the strong volar plate and the volar parts of the lateral collateral ligaments. These are crucial structures that resist dorsal subluxation of the PIP joint when subjected to load.
The primary structures resisting dorsal subluxation are the volar plate and the radial and ulnar collateral ligaments. The volar plate, a thick fibrocartilaginous structure, is tethered to the proximal phalanx proximally and inserts broadly into the base of the middle phalanx distally. Its integrity is paramount. The collateral ligaments, originating from the proximal phalanx condyles and inserting into the middle phalanx, provide critical mediolateral stability throughout the range of motion.
Regarding tendon attachments, the extensor mechanism's central slip provides relatively weak dorsal proximal force, while the flexor digitorum superficialis (FDS) tendon slips provide strong volar distal force. This inherent imbalance means that flexor forces typically dominate extensor forces. When the volar restraint, particularly the volar plate, fails in a dorsal fracture-dislocation, these dominant flexor forces, coupled with the joint's geometry, create a powerful lever arm that leads to dorsal subluxation and proximal migration of the main dorsal fracture fragment of the middle phalanx.
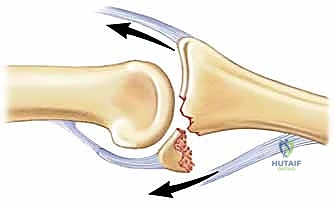
Figure 3A diagrams this fracture-dislocation mechanism, illustrating the interplay of forces.
Research and clinical experience have shown that the PIP joint will generally remain stable if up to 42% of the volar half of the middle phalanx articular surface is damaged, as assessed on a true lateral radiograph.
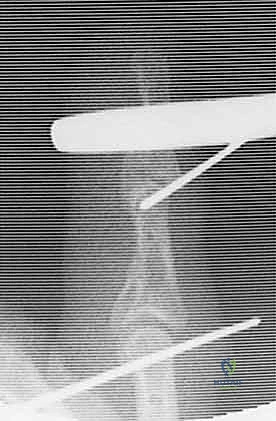
Figure 3B visually represents this concept of volar loss and its implications for instability.
However, fellows, be aware that in practice, subluxation can occur with as little as 10% to 15% joint surface loss, though this is less common. More severe injuries, involving a greater portion of the volar lip, are longitudinally unstable, leading to persistent PIP joint subluxation and the clinical findings we'll discuss. For pilon fractures, the proximal phalanx condyles are driven into the middle phalanx base, displacing the central articular surface distally and splaying the dorsal-volar and lateral margins. This injury pattern is inherently longitudinally unstable, resulting in proximal migration, diminution or obliteration of the joint space, and significant articular incongruity.
Clinical Presentation and Diagnostic Workup
Patients typically present within a few days, though delayed presentations (up to 2-3 weeks, or even beyond 6 weeks) are common, often due to underestimation of injury severity by the patient or initial medical staff. The affected finger will be swollen and tender, centered around the PIP joint. Angular deformity or clinically evident subluxation (visually or by palpation) may be present. Range of motion will be significantly reduced, especially at the PIP joint.
Imaging Studies:
The cornerstone of diagnosis is plain radiology. Crucially, we need true posteroanterior (PA) and lateral radiographs centered specifically on the injured PIP joint. Hand radiographs alone, often taken in the emergency department, are inadequate.
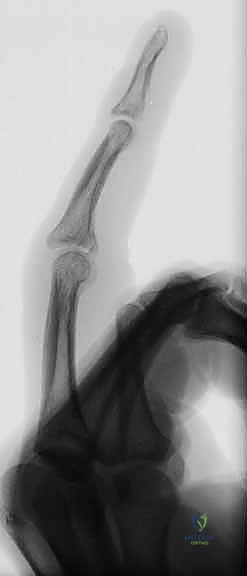
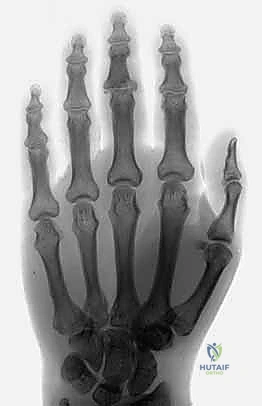
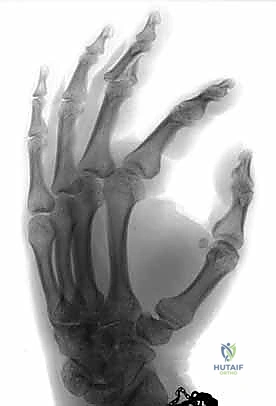
Figures 5A-C emphasize that hand radiographs are only interpretable with a true lateral view of the PIP joint.
Fluoroscopy is invaluable for assessing injury dynamics and joint stability in real-time. It helps differentiate stable from unstable injuries, whether fracture-subluxations, dislocations, or pilon fractures. Subluxation and dislocation are best visualized on the lateral radiograph and can be subtle, appearing as joint incongruity or the "triangle sign" (dorsal overhang of the middle phalanx base).
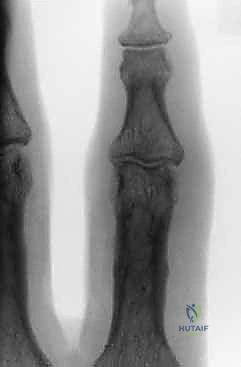
Figure 4E illustrates dorsal fracture-subluxation with joint incongruity and the classic V-sign.
Differential Diagnosis
When evaluating PIP joint injuries, consider:
* Soft Tissue Injuries: Volar plate injury, collateral ligament injury, central slip injury.
* Bone Injuries: Proximal phalanx condylar injury, proximal phalanx distal diaphyseal injury, middle phalanx proximal diaphyseal injury.
Nonoperative Management Considerations
For stable injuries, early protected mobilization is the mainstay. Most mild injuries, involving limited volar plate avulsion, reduce spontaneously or with assistance under local anesthesia.
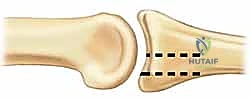
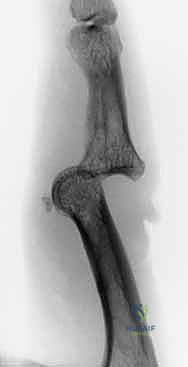
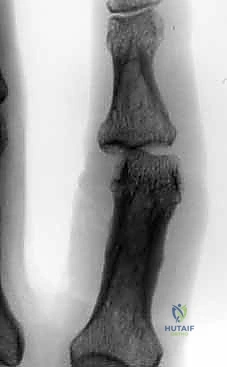
Figures 4A-D show a dorsal lateral fracture-dislocation with a small avulsion fragment before and after reduction, highlighting the potential for successful nonoperative reduction.
These injuries are longitudinally stable. Early mobilization focuses on regaining extension, which is commonly lost. An extension block splint for up to 6 weeks is only needed for significant pre-existing volar plate laxity (often seen in young women). Most patients regain near-full movement, though minor swelling, stiffness, and mild cold discomfort may persist. Heavy activity may cause discomfort. Persistent synovitis in about 5% of patients beyond 6 weeks usually resolves with a steroid injection.
If the joint is unstable but has limited volar joint damage (less than about 30 degrees), it may reduce when held in flexion with a dorsal block splint. This position must be documented radiologically, ensuring joint reduction and congruity, and should not require more than about 50 degrees of joint flexion to prevent unacceptable stiffness. Patients are encouraged to flex and extend to the splint, with weekly reviews and gradual reduction of splint flexion by 10 degrees each week. At each increase in extension, radiological confirmation of reduction is critical.
For pilon fractures, the minority with minimal displacement (<1mm) and a reasonable joint space are usually stable and can be managed with early gentle mobilization and part-time splint protection for 4 weeks. Most achieve excellent range of motion. However, if there is greater displacement, surgery is almost always required to achieve longitudinal stability and facilitate early movement.
Preoperative Planning: The Foundation of Success
Successful surgery begins long before the first incision.
Patient Assessment and History
A thorough history is vital. We need to understand the mechanism of injury, the timing, and any prior attempts at reduction. Any co-morbidities, particularly those affecting bone quality or healing, must be noted. Detailed physical examination assessing swelling, tenderness, deformity, and neurovascular status is paramount. Crucially, we must test for stability throughout the full arc of motion, identifying any positions that induce instability.
Diagnostic Imaging and Interpretation
As discussed, true PA and lateral radiographs of the PIP joint are non-negotiable. We meticulously assess the percentage of volar articular surface involvement, the degree of comminution, and any associated fractures. Fluoroscopy in the clinic can be invaluable for dynamic assessment of stability.
Surgical Indications and Contraindications
Indications for dynamic external fixation include:
* Unstable PIP joint fracture-dislocations that cannot be maintained concentrically reduced by closed means or dorsal block splinting.
* Pilon fractures with significant displacement, requiring longitudinal stability and distraction to restore joint space and allow early motion.
* Fractures with greater than 42% volar articular surface involvement (or less, if clinically unstable).
Contraindications:
* Severe soft tissue compromise or active infection precluding percutaneous pin placement.
* Extremely comminuted fractures where no stable bone segment exists for pin fixation (though rare with this technique).
* Patient factors precluding surgery (e.g., severe medical co-morbidities).
Anesthesia and Patient Preparation
This procedure is ideally performed under local anesthesia. My preference is a mid-metacarpal level block with at least 10 mL of plain 0.5% bupivacaine. Administering this before skin preparation allows ample time for the bupivacaine to take full effect by the time we begin, providing prolonged postoperative analgesia for 12 to 36 hours. This also allows the patient to participate during the operation, providing real-time feedback on comfort and motion, which can be invaluable.
A digital tourniquet is applied to the injured finger for a bloodless field, and a proximal arm tourniquet is placed as a backup, though rarely needed for this procedure.
Prophylactic Antibiotics: We administer 1.5 grams of cefuroxime preoperatively. There is no need for postoperative antibiotics for this percutaneous procedure unless there are signs of infection.
Skin Preparation: The skin is meticulously prepared with chlorhexidine in an alcohol solution, often with a pink dye, ensuring all fingers are thoroughly prepped. If the finger has had adhesive dressings or is not meticulously clean, we scrub the anesthetized finger thoroughly before final skin preparation.
Informed Consent: Fellows, remember to thoroughly discuss the risks and benefits of all treatment options – conservative and surgical – with the patient. Potential risks include infection (especially pin track), stiffness, scar tenderness, nerve injury, nonunion, malunion, and the possibility of revision procedures.
Patient Positioning and Surgical Setup
The patient is positioned supine, with the affected hand placed on a specialized armboard, abducted at 90 degrees to the operating table. This standard hand surgery position provides optimal access and ergonomics. The entire operated arm is draped sterilely. The fluoroscopy unit (C-arm) is positioned to allow for immediate, unobstructed true PA and lateral views of the PIP joint without repositioning the hand. This is critical for accurate K-wire placement. The digit is clearly marked to prevent wrong-site surgery, especially if the patient is under general anesthesia (which is rare for this procedure).
Instrumentation and Hardware Selection
For this procedure, we perform a closed, percutaneous insertion of K-wires.
K-wire Selection: My strong recommendation is 1.1-mm K-wires. I've found 0.9-mm wires too flexible, prone to bending during insertion or under load, leading to inadequate fixation. Conversely, 1.6-mm wires are too rigid, increasing the risk of bone damage or fracture during insertion, and potentially leading to excessive stiffness. While 1.2-mm wires have been used successfully, and wires from 1.0 to 1.3 mm are generally acceptable, the 1.1-mm wire offers the optimal balance of rigidity and flexibility for this application.
Intraoperative Execution: The Dynamic External Fixation Masterclass
Now, let's get scrubbed in, fellows. We'll proceed systematically, focusing on precision and anatomical awareness.
The Surgical Approach: Closed Percutaneous Technique
Our approach is entirely closed, utilizing percutaneous K-wires. This minimizes soft tissue dissection, reducing surgical morbidity and promoting faster recovery.
Proximal K-Wire Insertion: Establishing the Pivot
This is arguably the most critical step, as the proximal wire defines the axis of motion for our dynamic construct.
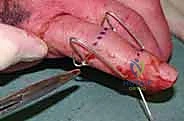
- Identify the Center of Rotation: Under image intensifier guidance, precisely identify the anatomical center of rotation of the PIP joint. This is where the condyles of the proximal phalanx articulate with the base of the middle phalanx. Mark this level clearly on the skin with a surgical pen.
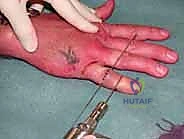
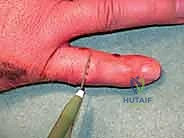
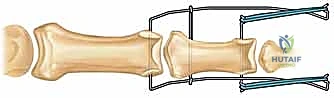
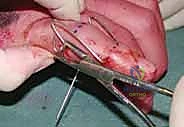
Figures 1A and 1B (TECH FIG 1A,B) show us marking the position for the first wire at the level of the center of rotation of the PIP joint, confirmed with the image intensifier.
-
Determine Entry Point: Aim to insert the wire 1 to 2 mm proximal to the marked center of rotation.
> SURGICAL WARNING: Aiming slightly proximal is crucial. The joint capsule reflects proximally from the articular margin. By staying 1-2mm proximal, we ensure the wire remains extracapsular. A distal wire, penetrating the joint capsule, significantly increases the risk of joint infection if pin track sepsis develops, leading to catastrophic outcomes. Conversely, placing this wire too far proximally in the diaphysis of the proximal phalanx will restrict full joint movement, defeating the purpose of a dynamic fixator. This balance is key. -
Initial Wire Insertion: Take your 1.1-mm K-wire and, under direct visualization and fluoroscopic guidance, initiate insertion through the skin and subcutaneous tissue. Aim for the center of the proximal phalanx in both PA and lateral planes. Ensure it is perpendicular to the long axis of the finger and parallel to the intended plane of rotation of the joint.
> PEARL: As you insert, you should feel the resistance of the cortical bone. Advance slowly, using a drill with a controlled, oscillating motion to prevent thermal necrosis of the bone. -
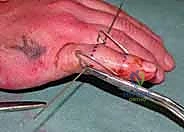
Fluoroscopic Confirmation (Partial Insertion): Insert the wire partially through the proximal phalanx, ensuring it crosses the head of the proximal phalanx. Immediately check its position with both true posteroanterior (PA) and lateral projections on the image intensifier.

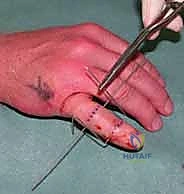
Figure 1C (TECH FIG 1C) confirms the wire inserted across the head of the proximal phalanx, verified on the image intensifier, before further advancement.
- Finalize Proximal Wire Placement: Once confirmed, advance the wire fully through the bone, ensuring equal lengths are present on either side of the finger. This symmetry, while less critical for the proximal wire, will serve as a useful guide for balancing the distal wire later.
Distal K-Wire Insertion: Securing the Segment
With the proximal pivot established, we now secure the mobile middle phalanx segment.
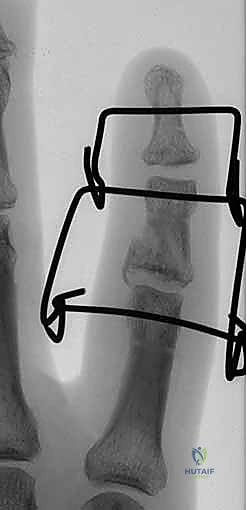
- Identify Distal Wire Level: Under image intensifier guidance, identify an appropriate level in the distal half to two-thirds of the middle phalanx. This placement must be distal to any fracture extension in the shaft of the middle phalanx to ensure adequate purchase in healthy bone. Mark this level on the skin.
> PEARL: For pilon fractures with significant distal extension, the distal wire can be placed as far distally as the head of the middle phalanx, or even near the center of rotation of the distal interphalangeal (DIP) joint. The middle phalanx is often narrowest proximally, so a more distal placement often provides a wider bone segment for easier and more secure wire placement. I have never encountered a fracture so distal that adequate fixation could not be achieved.
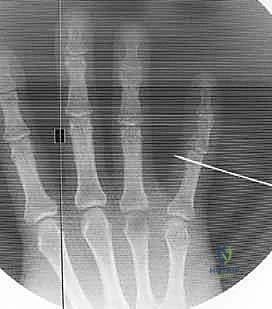
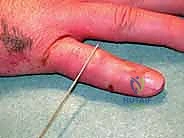
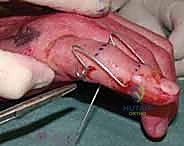
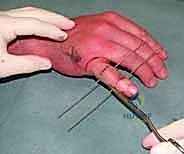
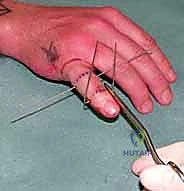
Figures 1D and 1E (TECH FIG 1D,E) illustrate finding and marking the position of the distal wire. Note how this placement is more distal than average, towards the head of the middle phalanx, due to an associated DIP joint injury, providing ample bone for fixation.
-
Initial Distal Wire Insertion: Similar to the proximal wire, insert the 1.1-mm K-wire percutaneously, aiming for the center of the middle phalanx. This wire must be perpendicular to the long axis of the finger and, crucially, parallel to both the plane of rotation of the PIP joint and the previously inserted proximal wire. This parallelism is essential for creating a functional dynamic construct.
-
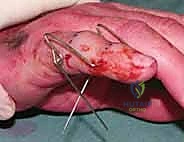
Fluoroscopic Confirmation (Partial Insertion): Insert the wire partially through the middle phalanx and check its position carefully with both PA and lateral views on the image intensifier.
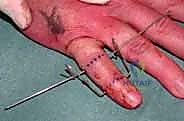
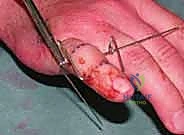
*Figures 1F and 1G (TECH FIG 1F,G) confirm the insertion and position of the distal wire on the image intens
Additional Intraoperative Imaging & Surgical Steps

REFERENCES
-
Fahmy NRM. The Stockport serpentine spring system for the treatment of displaced comminuted intra-articular phalangeal fractures. J Hand Surg Br 1990;15B:303–311.
-
Grant I, Berger AC, Tham SK. Internal fixation of unstable fracture dislocations of the proximal interphalangeal joint. J Hand Surg Br 2005;30B:492–498.
-
Hamilton SC, Stern PJ, Fassler PR, et al. Mini-screw fixation for the treatment of proximal interphalangeal joint dorsal fracture-dislocations. J Hand Surg Am 2006;31A:1349–1354.
-
Hastings H, Carroll C. Treatment of closed articular fractures of the metacarpophalangeal and proximal interphalangeal joints. Hand Clin 1988;4(3):503–527.
-
Inanami H, Ninomiya S, Okutsu I, et al. Dynamic external finger fixator for fracture dislocation of the proximal interphalangeal joint. J Hand Surg Am 1993;18A:160–164.
-
Kiefhaber T, Stern PJ. Fracture-dislocations of the proximal interphalangeal joint. J Hand Surg Am 1998;23A:368–380.
-
Krakauer JD, Stern PJ. Hinged device for fractures involving the proximal interphalangeal joint. Clin Orthop Relat Res 1996;327:29–37.
-
Schenk RR. The dynamic traction method: combined movement and traction for interarticular fractures of the phalanges. Hand Clin 1994; 10:187–198.
-
Seno N, Hashizume H, Inoue H, et al. Fractures of the base of the middle phalanx of the finger: classification, management and longterm results. J Bone Joint Surg Br 1997;79B:758–763.
-
Weiss AP. Cerclage fixation for fracture dislocation of the proximal interphalangeal joint. Clin Orthop Relat Res 1996;327:21–28.
-
Agee JM. Unstable fracture dislocation of the proximal interphalangeal joint. Clin Orthop Relat Res 1987;214:101–112.
-
Aladin A, Davis TR. Dorsal fracture-dislocation of the proximal interphalangeal joint: a comparative study of percutaneous Kirschner wire fixation versus open reduction and internal fixation. J Hand Surg Br 2005;30B:120–128.
-
Allison DM. Fractures of the base of the middle phalanx treated by dynamic external fixation. J Hand Surg Br 1996;21B:305–310.
-
Badia A, Riano F, Ravikoff J, et al. Dynamic intradigital external fixation for proximal interphalangeal joint fracture dislocations. J Hand Surg Am 2005;30A:154–160.
-
Deitch M, Kiefhaber T, Rodney Comisar B, et al. Dorsal fracture dislocations of the proximal interphalangeal joint: surgical complications and long-term results. J Hand Surg Am 1999;24A:914–923.
-
Deshmukh SC, Kumar D, Mathur K, et al. Complex fracture-dislocation of the proximal interphalangeal joint of the hand: results of a modified pins and rubbers traction system. J Bone Joint Surg 2004; 86B:406–412.
-
De Smet L, Boone P. Treatment of fracture-dislocation of the proximal interphalangeal joint using the Suzuki external fixator. J Orthop Trauma 2002;16(9):668–671. 8. de Soras X, de Mourgues P, Guinard D, et al. Pins and rubbers traction system. J Hand Surg Br 1997;22B:730–735.
-
Duteille F, Pasquier P, Lim A, et al. Treatment of complex interphalangeal joint fractures with dynamic external traction: a series of 20 cases. Plast Reconstr Surg 2003;15:1623–1629.

You Might Also Like