- ** Arthritides (** Table 1.20)
- Osteoarthritis
- Progressive loss of cartilage structure and function
- Most common form of arthritis
- May be idiopathic
- May be secondary to:
- Genetics ( Col2 defect); women affected more than men
- Overload: obesity, labor, dysplasia/femoral acetabular impingement, varus/valgus
- Trauma: fractures, ligament injuries, impact
- Tissue changes:
- Cartilage: enzymatic degradation and loss as discussed previously ( Fig. 1.30)
- Synovium: inflammation, vascular hypertrophy
- Ligaments: tightened on concave side of deformity
- Bone: sclerosis, osteophytes, and subchondral cysts
-
Osteophyte formation due to pathologic activation of endochondral ossification by periarticular chondrocytes through Indian hedgehog (Ihh) mechanism
- Muscles: atrophied from inactivity
- Radiographic findings (Figs. 1.31 and 1.32)
- Joint space narrowing, often asymmetric, with osteophyte formation
- Eburnation of bone
- Subchondral cysts “geodes”
- Treatment discussed within individual chapters (see Chapter 5, Adult Reconstruction)
- Neuropathic arthropathy (Charcot joint disease)
- Extreme form of arthritis caused by disturbed sensory innervation
-
Unstable, painless, swollen, red joint
- Effusion may show hemarthrosis
- Histologic findings: osteochondral fragments imbedded in synovium
- Less pain than would be expected radiographically
- Etiology: two theories
- Neuropathic loss of proprioception
- Repetitive trauma causes microfractures
- Hyperemia due to loss of sympathetic control
- Stimulates osteoclasts, weakens bones
- Radiographic findings ( Fig. 1.33)
- Severe destructive changes on both sides of the joint
- Scattered “chunks” of bone embedded in fibrous tissue
- Joint distension by fluid
- Heterotopic ossification
- Charcot arthropathy versus osteomyelitis
- May be difficult with physical examination and radiograph
- Both display swelling, warmth, and erythema and are common in diabetic patients
- Indium (In) 111–labeled WBC scan results
- “Hot” (positive) for osteomyelitis
- “Cold” (negative) for Charcot arthropathy
- Treatment includes bracing or casting (see Chapter 6)
- Neuropathic arthropathy also seen in
- Syringomyelia (see Fig. 1.33C and D)
- Most common cause of upper extremity neuroarthropathy
- 80% of cases in shoulder and elbow (see Fig. 1.33D)
- Joint disease develops in 25% of patients with syringomyelia.
- Leprosy (Hansen disease)
- Second most common cause in upper extremity
- Other neurologic problems
- Myelomeningocele: ankle and foot
- Spina bifida and spinal trauma (see Fig. 1.33G)
- Congenital insensitivity to pain
- Rheumatoid arthritis (see Table 1.20)
- Most common inflammatory arthritis
- Affects 0.5%–1% of population; three times more common in women
- 15% concordance rate in monozygotic twins
- Clinical presentation (see Fig. 1.32)
- Insidious subacute onset over 6 weeks
- Fatigue, malaise, anemia
- Morning stiffness and polyarthritis with swelling
- Hand and foot deformities are most common and are discussed in respective subsequent chapters
- Also common in the knees, elbows, shoulders, ankles, and cervical spine
- Subcutaneous rheumatoid nodules ( Fig. 1.34)
- Juxtaarticular erosions and periarticular osteopenia on radiographs
- 2010 American College of Rheumatology Classification Criteria for RA are summarized in Table 1.21.
- Diagnosis requires score 6 or more
- Criteria include
- Number of joints involved and duration of involvement
- Positive laboratory test results often found
- Erythrocyte sedimentation rate (ESR), C-reactive protein (CRP)
- Pathogenesis
- Rheumatoid factor (RF) titer
- Antibody (immunoglobulin [Ig] M) against the Fc (crystallizable fragment) portion of IgG
- Positive result in about 80%
- Test for anticyclic citrullinated protein (anti-CCP) antibodies
- Also known as anti-CCP antibodies (ACPAs)
- Most sensitive and specific test (≈90% specific)
- Presence linked to more aggressive disease
- T cell–mediated immune response from an infectious or environmental antigen (smoking is one known trigger) in a genetically susceptible individual (HLA-DR4 and HLA-DW4)
- Mononuclear cells are primary mediator of RA tissue damage
- Initial response in soft tissues— neovascularization and synovitis
- CD4+ T lymphocytes (helper cells) activate synovial cells through direct cell-cell contact
- Synoviocytes produce cytokines
- Macrophages (type A): main source for TNF-α, IL-1
- Fibroblast (type B): main source for MMPs, proteases, and RANKL
- B lymphocytes (plasma cells): make RF, anti-CCP antibodies
- TNF-α, IL-1, IL-6, IL-7 upregulated
- IL-1: Regulator of inflammation and matrix destruction
- TNF-α:
- Upregulates endothelial adhesion molecules and stimulates angiogenesis
-
Table 1.20 Comparison of Common Arthritides Age Incidence Arthritis Group By Sex Affected ---
Noninflammatory Osteoarthritis | Elderly
| M > F Neuropathic | Elderly
| M > F Acute rheumatic fever | Children
| M = F Ochronosis | Adults
| M = F
Inflammatory Rheumatoid | Young
adults
| F > M Systemic lupus erythematosus | Young
adults
| F > M Juvenile rheumatoid arthritis | Children
| F > M Relapsing polychondritis | Elderly
| M = F
Spondyloarthropathies Ankylosing spondylitis | Young
adults
| M > F
| | Reactive arthritis (Reiter syndrome) | Young
adults
| M > F
| ---|---|---| Psoriatic | Young
adults
| M = F Enteropathic | Young
adults
| M > F Age Incidence Arthritis Group By Sex S Affected ---
Crystal Deposition Disease Gout | Young
| M > F
| Chondrocalcinosis | Elderly
| M = F
| Infectious Pyogenic | All
| M = F
| Tuberculous | Elderly
| M > F
| Lyme disease | Young
| M = F
| Fungal | All
| M > F
| Hemorrhagic Hemophilia | Young
| M
| Sickle cell disease | Young
| M = F
| Pigmented villonodular synovitis | Young
| M = F
| ↓ , Decreased; AFB, acid-fast bacilli; ASO, antistreptolysin O; CPK, creatine phosphokinase; PTT, partial thromboplastin time.

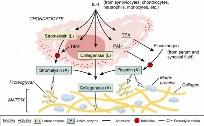
--- FIG. 1.30 Enzyme cascade of IL-1–stimulated degradation of articular cartilage. TPA, Tissue plasminogen activator. From Simon SR, editor: Orthopaedic basic science, Rosemont, IL, 1994, American Academy of Orthopaedic Surgeons, p 40.

--- FIG. 1.31(A) Radiograph showing joint space narrowing, osteophytes, and bony sclerosis. (B) Macrosection of an osteoarthritic human femoral head demonstrating subarticular cysts, sclerotic bone formation, and a superior femoral head osteophyte. (C) Low-power micrograph of osteoarthritis showing fibrillation, fissures, and cartilage loss. D, Gross pathology of femoral head demonstrating cartilage thinning (1) ,
subarticular cyst (2
[“geode”]), and normal hyaline cartilage remaining (3) . A Courtesy Marc DeHart, MD, and Texas Orthopedics; B from Simon SR, editor: Orthopaedic basic science, Rosemont, IL, 1994, American Academy of Orthopaedic Surgeons; C and D from Horvai A: Bones, joints, and soft tissue tumors. In Kumar V et al, editors: Robbins and Cotran pathologic basis of disease, ed 9,
Philadelphia, 2015,
Elsevier, Fig. 26-93.

--- FIG. 1.32 Differences between rheumatoid arthritis and osteoarthritis. Left side of illustration demonstrates the main historical characteristics of RA, including symmetric involvement (both right and left joints as well as both medial and lateral compartments of the knees). Bilateral hand involvement is characteristic and usually involves wrist joints and proximal metacarpal joints. Right side of figure demonstrates osteoarthritis, which often is much more severe in one joint or one compartment of the knee. Hand involvement more commonly involves the distal interphalangeal joints (Heberden nodes) and proximal interphalangeal joints (Bouchard nodes) joints as well as the base of the thumb. - Promotes influx of leukocytes and activates synovial fibroblasts
- Later response
- Promotes pain receptor pathways
- Drives osteoclastogenesis
- Synovial cells invade cartilage “pannus” and release MMPs, causing chondrolysis
- Periarticular bone erosions
- Cytokines stimulate osteoblasts and synovial B cells to make RANKL, which joins with RANK to activate osteoclasts. Responsible for bone destruction.
-
Osteoclasts secrete cathepsin K and carbonic anhydrase.



 FIG. 1.33
Neuropathic arthritis. Arthritic degeneration due to lack of sensation can be caused by many diseases. All share radiographic findings that are more severe than the symptoms (often painless) and the fragments from bony destruction. Often findings take many years to develop. (A and B) Diabetic Charcot arthropathy of the foot is easily recognized by most of the industrialized world. (C and D) The most common cause of upper extremity neuropathic joint is syringomyelia (
syrinx
= fluid-filled sac in central cord that causes insidious loss of pain and temperature early). (E–G) Tabetic arthropathy (tertiary syphilis) is the most common neuropathic arthritis of the knee and can often involve the hip.
FIG. 1.33
Neuropathic arthritis. Arthritic degeneration due to lack of sensation can be caused by many diseases. All share radiographic findings that are more severe than the symptoms (often painless) and the fragments from bony destruction. Often findings take many years to develop. (A and B) Diabetic Charcot arthropathy of the foot is easily recognized by most of the industrialized world. (C and D) The most common cause of upper extremity neuropathic joint is syringomyelia (
syrinx
= fluid-filled sac in central cord that causes insidious loss of pain and temperature early). (E–G) Tabetic arthropathy (tertiary syphilis) is the most common neuropathic arthritis of the knee and can often involve the hip.
From Yablon CM et al: Areview of Charcot neuroarthropathy of the midfoot and
hindfoot: what every radiologist needs to know, Curr Probl Diagn Radiol 39:187–199, 2010; Atalar AC et al: Neuropathic arthropathy of the shoulder associated with syringomyelia: a report of six cases, Acta Orthop Traumatol Turc 44:328–336, 2010; and Allali F et al: Tabetic arthropathy. Areport of 43 cases, Clin Rheumatol 25:858–860, 2006.



 FIG. 1.34 Upper extremity changes in common arthritis types. Left side of figure shows rheumatoid changes. (A) Swan neck deformity of index, middle, and ring fingers, with PIP joints extended and DIP joints flexed. (B) Boutonnière deformity: PIP joints flexed, DIP joints extended. (C) Bilateral wrist swelling with both ulnar metacarpal phalangeal joint deformities and swan neck deformities of fingers and left thumb. (D) Rheumatoid nodes noted on posterior olecranon region. Right side of figure shows osteoarthritic changes. (E) DIP changes (Heberden nodes) and PIP changes (Bouchard nodes). (F) Radiograph showing osteoarthritic changes at the base of the thumb. From O’Dell JD: Rheumatoid arthritis. In Goldman L, Schafer AI, editors:
Goldman-
FIG. 1.34 Upper extremity changes in common arthritis types. Left side of figure shows rheumatoid changes. (A) Swan neck deformity of index, middle, and ring fingers, with PIP joints extended and DIP joints flexed. (B) Boutonnière deformity: PIP joints flexed, DIP joints extended. (C) Bilateral wrist swelling with both ulnar metacarpal phalangeal joint deformities and swan neck deformities of fingers and left thumb. (D) Rheumatoid nodes noted on posterior olecranon region. Right side of figure shows osteoarthritic changes. (E) DIP changes (Heberden nodes) and PIP changes (Bouchard nodes). (F) Radiograph showing osteoarthritic changes at the base of the thumb. From O’Dell JD: Rheumatoid arthritis. In Goldman L, Schafer AI, editors:
Goldman-
Cecil medicine, Philadelphia, 2016, Elsevier, Fig. 264-3; Sweeney SE et al: Clinical features of rheumatoid arthritis. In Firestein GS et al: Kelley’s textbook of rheumatology, Philadelphia, 2013, Elsevier, Fig. 70-4; and http://medsci.indiana.edu/c602web/602/c602web/jtcs/docs/heber1.html - Systemic manifestations
- Rheumatoid vasculitis
- Distal splinter hemorrhage
- Cutaneous ulcers (pyoderma gangrenosum)
- Visceral arteritis
- Pericarditis and pericardial effusion
- Pulmonary disease including nodules and fibrosis
- Felty syndrome: severe erosive RA with splenomegaly and leukopenia
- Treatments and their perioperative considerations
- Regimen variable and often employs multiple agents
- NSAIDs: help symptoms early—antiinflammatory effects
- Should be held for 7–10 days preoperatively.
- Low-dose steroids
- Decrease prostaglandins and leukotrienes
- Used initially as “bridge therapy” to disease-modifying antirheumatic drugs (DMARDs)
- “Stress dose” steroid should be used perioperatively for patients on longterm steroid therapy
- DMARDs
- Intended to address underlying autoimmune response
- Conventional DMARDs take 2–6 months to work
- Methotrexate: folate analogue
- Inhibits purine metabolism and T-cell activation
- Inhibits neovascularization
- Adverse reactions (ADRs): toxic to bone marrow, liver, and lung
- Usually can continue through surgery
- Azathioprine: immunosuppressive agent
- ADR: neutropenia
- Cyclosporine: immunosuppressive agent
-
Inhibits activation of
CD4+ T cells - ADRs: nephrotoxicity, neurotoxicity, gingival hyperplasia
- Hydroxychloroquine (Plaquenil)
- Inhibits toll-like receptor 9 (TLR9)
- ADR: retinal toxicity (requires ophthalmology followup)
-
Table 1.21 The 2010 ACR-EULAR Classification Criteria for Rheumatoid Arthritis Criteria Score ---
A. Joint Involvement 1 Large Joint | 0 2–10 Large Joints | 1 1–3 Small Joints | 2 4–10 Small Joints | 3 > 10 Joints (at least 1 small joint) | 5
B. Serology (at least 1 test result is needed) Negative RF and negative ACPA | 0 Low-positive RF or low-positive ACPA | 2 High-positive RF or high-positive ACPA | 3
C. Acute-Phase Reactants (at least 1 test result is needed) Normal CRP and normal ESR | 0 Abnormal CRP or abnormal ESR | 1
D. Duration of Symptoms < 6 weeks | 0 > 6 weeks | 1
From Aletaha D et al: 2010 rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative, Arthritis Rheum 62:2569–2581, 2010. - Usually can continue through surgery
- Sulfasalazine
- Decreases synthesis of inflammatory mediators
- ADRs: granulocytopenia, hemolytic anemia (glucose-6-phosphate dehydrogenase [G6PD])
- Usually can continue through surgery
- Minocycline
- Inhibits MMP collagenase
- ADR: cutaneous hyperpigmentation
- Biologic DMARDs
-
Target TNF-α: etanercept, infliximab, adalimumab
-
Targets IL-1: anakinra
- Targets CD20: rituximab
- Surgery should be scheduled at end of dosing cycle (e.g., in a patient taking etanercept schedule, surgery should occur the second week after the first withheld dose).
-
Risks of opportunistic infection and lymphoma
- Surgical treatment is discussed within respective chapters.
- Juvenile idiopathic arthritis (JIA) is discussed in Chapter 3, Pediatric Orthopaedics.
- Systemic lupus erythematosus ( Fig. 1.35 ; see Table 1.20)
- Chronic inflammatory disease of unknown origin
- 90% of cases in women (blacks > whites)
- Initially mediated by tissue-binding autoantibodies and immune complexes (type III hypersensitivity)
- Pathophysiology
- Susceptible genetics stimulated by environment
- Immune system autoregulatory failure
- Sustained production of antibody to self-antigens
- Antinuclear antibodies (ANAs)—best screen; positive in 95%
- Anti-dsDNA, anti-Sm, anti-La (SS-B), antihistone antibodies—drug-induced lupus
- Immune complexes accumulate in various tissues and cause chronic inflammation
- Clinical findings
- Skin/joints—rash and arthritis
- Heart/kidney—pericarditis/nephritis
- Blood vessels—vasculitis
- Bone and joint involvement—most common feature
- Nonerosive polyarthritis affects over 75% (hand and wrist most common).
- Osteonecrosis (especially with steroids)
- Butterfly malar rash—classic feature
- Fever, pancytopenia
- Pharmacologic treatment similar to that for RA.
- Seronegative spondyloarthropathies
- Characterized by negative RF titer result and, often, positive HLA-B27 test result
- Symptoms
- Inflammatory back pain
- Peripheral arthritis
- Enthesitis—heel pain
- Dactylitis—sausage digit
- Eye—uveitis (iritis), conjunctivitis
- Skin, mucosal, GI, urethral
- Similar treatment routines, including NSAIDs, steroids, and DMARDs
- Ankylosing spondylitis (AS) ( Fig. 1.36 ; see Table 1.20)
- Male/female ratio 3:1; ages 20–40 years
- Most common in Northern European whites
- 90% HLA-B27 positive ( Table 1.22)
- Symptoms and findings
- Bilateral sacroiliitis (earliest symptom)
- Improves with exercise, not better with rest, pain at night
- Associated morning stiffness
- Progressive spinal flexion deformities over life
- Chin-on-chest deformity
- Modified Schober test (loss of lumbar flexion) (see Fig. 1.36C)
- Two marks are made10 cm apart over lumbar spine in erect patient.
-
With patient in maximum spinal
flexion, increase of less than 4 cm between marks indicates loss of flexion. - Hip involvement at young age—poor prognosis
- Enthesitis: inflammation of tendon insertion
- Loss of chest expansion
- Uveitis: red, painful eye in 40%
- Aortic insufficiency and heart block
- Radiographic changes
- Squaring of the vertebrae
- Vertical syndesmophytes
- Bamboo spine
- Autofusion of sacroiliac joints (see Fig. 1.36B)
- Whiskering of the entheses
- Surgical treatment for AS is discussed within Chapter 8, Spine.
- Reactive arthritis (Reiter syndrome) ( Fig. 1.37 ; see Table 1.20)
- Classical triad presentation: “Can’t see, can’t pee, can’t climb a tree.”
- Young white males (18–40 years)
- Follows an infection at another site (hence “reactive”)
- Chlamydia, Shigella, Yersinia, Salmonella
- Findings
-
Conjunctivitis, urethritis, and oligoarticular arthritis

 FIG. 1.35 Systemic lupus erythematosus. (A) Autoantibodies to DNA and DNA-binding proteins form immune complexes that stimulate immune system–directed inflammation throughout the body (type III hypersensitivity reaction). (B) Direct immunofluorescence with anti–immunoglobulin G antibodies shows immune complex deposits at two different places: a bandlike deposit along the epidermal basement membrane—positive result of lupus band test—and within the nuclei of the epidermal cells (ANAs). (C) Most patients have skin and joint involvement. The classic butterfly rash of SLE occurs in 10%–50% of patients with acute SLE. (D) The same immune complexes are seen in the basement membrane of the renal glomerulus. (E) Flea-bitten appearance of kidney specimen, with lupus nephritis causing various degrees of proteinuria, hematuria, and cellular casts. From Habif TP:
Clinical dermatology,
ed 5, St Louis,
FIG. 1.35 Systemic lupus erythematosus. (A) Autoantibodies to DNA and DNA-binding proteins form immune complexes that stimulate immune system–directed inflammation throughout the body (type III hypersensitivity reaction). (B) Direct immunofluorescence with anti–immunoglobulin G antibodies shows immune complex deposits at two different places: a bandlike deposit along the epidermal basement membrane—positive result of lupus band test—and within the nuclei of the epidermal cells (ANAs). (C) Most patients have skin and joint involvement. The classic butterfly rash of SLE occurs in 10%–50% of patients with acute SLE. (D) The same immune complexes are seen in the basement membrane of the renal glomerulus. (E) Flea-bitten appearance of kidney specimen, with lupus nephritis causing various degrees of proteinuria, hematuria, and cellular casts. From Habif TP:
Clinical dermatology,
ed 5, St Louis,
Mosby/Elsevier, 2009; Wikimedia Commons: Diffuse proliferative lupus nephritis.
http://en.wikipedia.org/wiki/Lupus_nephritis#mediaviewer/File:Diffuse_pr oliferat
; and Wikimedia Commons: Lupus band test. http://en.wikipedia.org/wiki/Systemic_lupus_erythematosus#mediaviewer/File:L - Sudden asymmetric swelling and pain in knee , ankle, hip
- May persist 3–5 months
- Feet affected more often than hands (heel pain)
- Calcaneal periostitis and metatars al head erosion
-
Dactylitis: sausage digit of one finger/toe (see
Fig.
1.37E) - 60% of patients with chronic disease have sacroiliitis.
- Painless mucocutaneous ulcers (penile) and oral stomatitis (see Fig. 1.37B)
- Urethritis (dysuria), prostatitis, or cervicitis
- Pustular lesions on the extremities, palms, and soles (keratoderma blennorrhagicum)
-
Treatment: NSAIDs and PT



 FIG. 1.36 Ankylosing spondylitis is an axial seronegative spondyloarthropathy that causes progressive cervical and thoracic kyphosis and bamboo spine but has earliest involvement in the sacroiliac joints. (A) Early sacroiliitis demonstrated by loss of clarity and sclerosis in the lower third of the sacroiliac joints, particularly affecting the iliac side of the right sacroiliac joint (hip joints are normal). (B) Advanced disease with ankylosis or fusion of both the sacroiliac and hip joints. (C) Schober test; two marks made 10 cm apart on lumbar spine in erect stance should be less than 14 to 15 cm during forward flexion.
FIG. 1.36 Ankylosing spondylitis is an axial seronegative spondyloarthropathy that causes progressive cervical and thoracic kyphosis and bamboo spine but has earliest involvement in the sacroiliac joints. (A) Early sacroiliitis demonstrated by loss of clarity and sclerosis in the lower third of the sacroiliac joints, particularly affecting the iliac side of the right sacroiliac joint (hip joints are normal). (B) Advanced disease with ankylosis or fusion of both the sacroiliac and hip joints. (C) Schober test; two marks made 10 cm apart on lumbar spine in erect stance should be less than 14 to 15 cm during forward flexion.
From Raychaudhuri S: The classification and diagnostic criteria of ankylosing spondylitis, J
Autoimmun 48–49:128–133, 2014. - Psoriatic arthropathy (PsA) (see Table 1.20)
- Affects 5%–30% of patients with psoriasis
- Usually skin disease precedes arthritis
- Men and women (aged 30–40 years) equally affected
- Characteristic changes
- Distal interphalangeal (DIP) involvement (rare in other inflammatory arthritides)
- Nail changes in 90%
- Pitting, fragmentation, and discoloration
- 30% have sausage digits
- Prominent enthesitis and tenosynovitis
- Arthritis mutilans—most destructive form
- Telescoping (shortening) of digits
- Pathophysiology
- Upregulated RANKL in synovium (B-type cells)
- Marked increase in osteoclast precursors
- Radiographic findings
- Pencil-in-cup deformity, DIP
- Small joint ankylosis
- Osteolysis of metacarpal (MC) and phalangeal bone
- Periostitis and bony enthesitis
- Enteropathic arthritis (see Tables 1.20 and 1.22)
- Arthritis in presence of inflammatory bowel disease
- Varied clinical picture, but joint erosions uncommon
- 10%–50% of patients experience peripheral joint arthritis.
- Acute monoarticular synovitis precedes bowel symptoms.
- Nondeforming arthritis
- More common in large weight-bearing joints
- 10%–15% of cases associated with ankylosing spondylitis
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding arthritides
