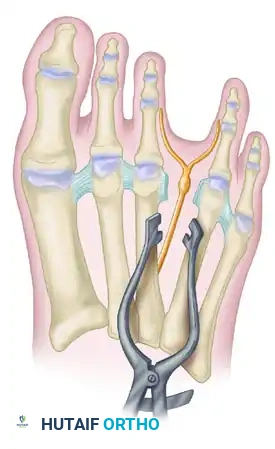
Neuroma Transection and Proximal Burial in the Foot and Ankle: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on neuroma transection and proximal burial in the foot and ankle. We'll meticulously cover comprehensive surgical anatomy, precise patient positioning, and granular, real-time intraoperative execution. Learn critical pearls, avoid common pitfalls, and master the art of managing chronic neuropathic pain through advanced surgical techniques, ensuring optimal patient outcomes.
Alright, fellows, gather 'round. Welcome to the operating theater. Today, we're tackling a challenging, yet incredibly rewarding, problem: the recalcitrant painful neuroma of the foot and ankle. This isn't just about cutting a nerve; it's about meticulous identification, precise transection, and strategic burial to provide lasting relief from what can be truly debilitating neuropathic pain. Our goal here is to transform a patient's life, and to do that, we need to be masters of both anatomy and technique.
This procedure, while seemingly straightforward, demands an intimate understanding of the peripheral nervous system in the lower limb, an area notorious for its anatomical variability. Remember, these nerves don't always read the textbooks, so constant vigilance and careful dissection are paramount.
Understanding the Enemy: Pathophysiology and Natural History of Neuromas
Let's begin by appreciating the genesis of these painful lesions. A neuroma, fundamentally, is a disorganized proliferation of nerve tissue that forms at the site of a nerve injury. When a nerve is transected or severely damaged, the proximal nerve stump attempts to regenerate, sending out axonal sprouts. If these sprouts cannot find a distal pathway to reconnect, they form a tangled, often hypersensitive mass – the neuroma.
Several mechanisms can lead to nerve damage in the foot and ankle, often culminating in neuroma formation:
- Direct Contusion: A blunt impact or crush injury can directly damage nerve fibers.
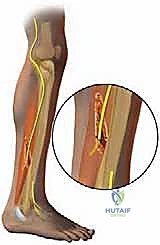
- Stretch Injury: This is particularly common in the foot and ankle. Consider a severe ankle inversion sprain or a complex ankle fracture. The extreme motion can stretch nerves beyond their elastic limit, causing Wallerian degeneration. The superficial peroneal nerve, for instance, is highly susceptible to stretch injury with severe ankle inversion, as is the sural nerve.
- Iatrogenic Insult: Unfortunately, this is the most common cause in the foot and ankle. Surgical incisions, retractors, sutures, or even misplaced arthroscopic portals can inadvertently injure nerves. Think about a Lisfranc fracture open reduction and internal fixation (ORIF) or a second metatarsal–cuneiform arthrodesis – these procedures inherently challenge the superficial and deep peroneal nerves in the midfoot. Bunion procedures, especially along the dorsomedial hallux, famously threaten the dorsomedial cutaneous nerve, a distal branch of the superficial peroneal nerve. Calcaneal ORIF and fifth metatarsal ORIF incisions place the sural nerve at significant risk. Even Achilles tendon procedures and Haglund resections can damage the sural nerve, particularly its posterior branch. Arthroscopic ankle lateral portal placement is another classic example, often endangering the superficial peroneal nerve.
Neuromas present along a spectrum, from a small, benign bulb neuroma, often asymptomatic, to a massive accumulation of angry, hypersensitive nerve endings that generate independent nerve signals, leading to severe, crippling pain. Some nerve injuries may heal slowly with distal progression of symptoms, but many are unpredictable in their natural course. Our goal today is to address those unpredictable, painful neuromas that have failed conservative management.
The Anatomical Battlefield: Comprehensive Neurovascular Mapping
Before we make any incision, fellows, we must have an encyclopedic knowledge of the regional anatomy. The foot and ankle possess five primary sensory nerves, but remember, anatomical variability is the rule, not the exception.
- The Superficial Peroneal Nerve (SPN):
- Course: Emerging from the common peroneal nerve, it descends in the lateral compartment of the leg, superficial to the peroneal muscles (peroneus longus and brevis). Approximately two-thirds down the leg, it pierces the deep fascia to become superficial. It then courses anterior to the fibula, dividing into its terminal branches (medial dorsal cutaneous nerve and intermediate dorsal cutaneous nerve) which innervate the dorsum of the foot.
- Risk: Highly vulnerable during ankle fracture ORIF (especially lateral approaches), arthroscopic ankle lateral portal placement, and any lateral midfoot surgery.
- Specific Branch Risk: Its terminal medial branch, the dorsomedial cutaneous nerve, is particularly at risk with bunionectomy along the dorsomedial hallux.
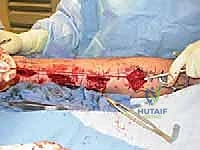
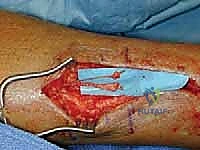
* Clinical Pearl: This nerve is often adherent to muscle and fascia after severe stretch injury, as seen in this classic image (FIG 2). This adherence can make dissection challenging and increase the risk of iatrogenic injury if not approached meticulously.
-
The Deep Peroneal Nerve (DPN):
- Course: Originating from the common peroneal nerve, it runs with the anterior tibial artery and veins as a neurovascular bundle along the anterior tibia. It passes under the extensor retinaculum at the ankle.
- Innervation: Primarily motor to the muscles of the anterior compartment (tibialis anterior, extensor hallucis longus, extensor digitorum longus, peroneus tertius). It also provides sensory innervation to the first web space (between the first and second toes) and some sensory components to the flexor hallucis brevis muscle and the sinus tarsi.
- Risk: At risk with dorsal foot injuries, Lisfranc ORIF, and any procedures involving the anterior ankle or midfoot. While motor nerves are generally not resected due to the functional deficit, the motor loss of the DPN branches is relatively well tolerated compared to the posterior tibial nerve.
-
The Sural Nerve:
- Course: Formed by the union of the medial sural cutaneous nerve (from the tibial nerve) and the lateral sural cutaneous nerve (from the common peroneal nerve). It runs superficially to the gastrocnemius muscle, then descends between the peroneals and the Achilles tendon. It courses along the posterolateral aspect of the ankle and foot.
- Innervation: Sensory to the lateral foot, lateral malleolus, and the lateral aspect of the fifth toe.
- Risk: Highly susceptible to injury during calcaneal ORIF, fifth metatarsal ORIF, Achilles tendon procedures, Haglund resections, and lateral ankle ligament reconstructions.
- Clinical Pearl: This nerve is perhaps the easiest to find surgically due to its superficial course, but anecdotally, it has proved difficult postoperatively with nerve regrowth, necessitating a very proximal burial site.
-
The Saphenous Nerve:
- Course: An extension of the femoral nerve, it descends along the medial aspect of the leg, often accompanying the great saphenous vein. It passes anterior to the medial malleolus.
- Innervation: Sensory to the medial leg, medial ankle, and medial foot.
- Risk: At significant risk during medial ankle fracture ORIF (e.g., medial malleolus fractures), great saphenous vein stripping, and any medial ankle or foot surgery.
- Clinical Pearl: Its close association with the great saphenous vein makes careful dissection crucial to avoid vascular injury.
-
The Tibial Nerve (and its plantar branches):
- Course: Descends posterior to the medial malleolus, through the tarsal tunnel. It then splits into the medial and lateral plantar nerves.
- Innervation: This is a mixed motor and sensory nerve. The medial plantar nerve innervates the abductor hallucis, flexor digitorum brevis, flexor hallucis brevis, and first lumbrical, and provides sensation to the medial two-thirds of the plantar foot and the first three and a half toes. The lateral plantar nerve innervates the remaining intrinsic foot muscles and provides sensation to the lateral one-third of the plantar foot and the lateral one and a half toes.
- Risk: Primarily associated with tarsal tunnel syndrome due to entrapment. Resection of the posterior tibial nerve is reserved only for salvage procedures, often as a precursor to possible amputation, given the significant motor loss.
- Clinical Pearl: While not typically a target for transection and burial due to its motor component, understanding its role in tarsal tunnel syndrome and its differential diagnosis from neuromas is crucial.
Preoperative Masterclass: Planning for Precision
Fellows, the success of this surgery hinges heavily on meticulous preoperative planning and patient selection. This is not a procedure to be taken lightly; the resection of a nerve is essentially a "one-way street."
-
Patient History and Physical Findings:
- Pathogenesis Review: We've discussed common causes. Always consider the full spectrum of potential etiologies, including systemic conditions like leprosy, diabetic neuropathy, peripheral vascular disease, rheumatoid arthritis, or local issues like joint arthrosis, synovitis, tenosynovitis, ganglion cysts, lipomas, neurilemmomas, abscesses, fractures, malalignment, or even plantar fasciitis.
- Pain Characteristics: Neuropathic pain is often described as burning, shooting, tingling, or electrical. It can be constant or intermittent.
- Physical Examination: This is critical. We're looking for areas of hypersensitivity (allodynia or hyperalgesia) or hyposensitivity (numbness) in the skin and subcutaneous tissues, rather than deep tissues. Palpate along the course of the suspected nerve. A positive Tinel's sign (reproduction of symptoms with percussion over the nerve) is often highly indicative.
- Prior Surgeries: Always ask about previous interventions. Prior surgery can result in confusing symptoms and altered anatomy.
- Misdiagnosis: Be aware that many nerve injuries are initially misdiagnosed.
-
Nonoperative Management: Exhausting All Avenues:
- We only proceed with surgery after a comprehensive trial of nonoperative measures. These include:
- Physical Support: Braces, splints, or periods of immobilization (short-leg cast or walking boot) can allow neuritic symptoms to subside, especially if traction causes pain, and prevent recurrent stretching injuries to nerves like the superficial and deep peroneal.
- Orthotics: For mechanical imbalances, such as acquired pes planus secondary to posterior tibial tendon dysfunction causing tarsal tunnel symptoms, orthotic devices can restore foot balance.
- Pharmacologic Interventions:
- Nonsteroidal anti-inflammatories (NSAIDs) for concomitant inflammation.
- Neuromodulators: Gabapentin, pregabalin, or tricyclic antidepressants (e.g., amitriptyline) are often first-line to quiet nerve hypersensitivity.
- Clonazepam and similar benzodiazepines may lessen nerve reactivity.
- Narcotics: Use with extreme caution due to addiction potential, especially with chronic nerve pain.
- Topical agents: Lidoderm patches (lidocaine hydrochloride released over time) applied directly over the symptomatic area. Compounding pharmacies can create absorbent gels with neuromodulators, local anesthetics, and nonsteroidals.
- Injections:
- Steroid Injections: Combined with local anesthetic, these serve a dual role as both therapeutic and diagnostic agents. While sometimes useful, symptomatic relief is often temporary. Limit injections to no more than two in a 1-year period due to risks like skin discoloration, tendon rupture, atrophy of subcutaneous fat, and collateral ligament attenuation.
- Ethanol Injections: 4% ethanol in a Marcaine solution has been anecdotally useful for interdigital neuromas (Morton's neuroma protocol: four injections a week apart, followed by three more if partial improvement). The theoretical benefit is loss of nerve conduction without post-resection neuroma formation.
- We only proceed with surgery after a comprehensive trial of nonoperative measures. These include:
-
Diagnostic Studies:
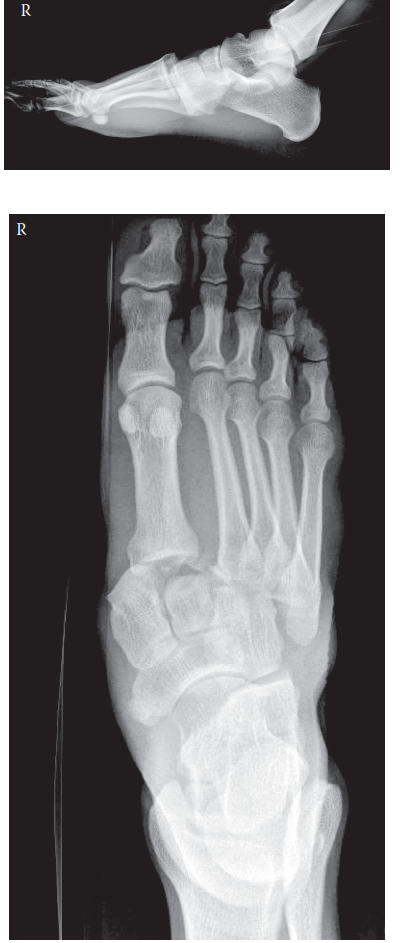
- Routine Radiographs: May reveal mechanical imbalance, irritation from a cyst or tumor, or osteophyte formation suggesting entrapment.
- MRI: Excellent for defining soft tissue irritation, ruling out impinging structures (tumor, cyst), and illuminating areas of inflammation. Exception: MRI has proven less accurate for interdigital neuromas.
- Electrodiagnostic Studies (Nerve Conduction Studies/EMG): Helpful for differentiating local from more proximal nerve pathology (e.g., cervical or lumbosacral impingement, generalized neuropathies). Essential for suspected tarsal tunnel syndrome (sensory nerve conduction velocity may approach 90% sensitivity). Limitation: Not helpful for interdigital neuromas or many small sensory nerves.
- Diagnostic Nerve Block: This is arguably the best preoperative indicator of success. A local anesthetic block using 1% or 2% lidocaine hydrochloride, 0.5% Marcaine hydrochloride, and a few drops of sodium bicarbonate (to titrate acidity and ease injection pain) is performed along the course of the suspected nerve. Crucially, the physician must return a few minutes after the injection to reexamine the patient for symptom relief, rather than waiting for the next office visit. This confirms the location of nerve tenderness and helps predict surgical outcome.
-
Patient Education and Informed Consent:
- Thorough discussion with the patient is paramount. They must understand that nerve resection is a "one-way street." Explain the potential for nerve ending regrowth and possible neuroma formation even after surgery. Manage expectations regarding complete pain relief versus significant improvement. Discuss the potential for numbness in the area previously innervated by the resected nerve.
-
Anesthesia Considerations:
- Regional or General Anesthesia: Either may be used.
- Epidural Anesthesia for CRPS/RSD: If the patient has a history of reflex sympathetic dystrophy (RSD) or complex regional pain syndrome (CRPS) involving the leg, consider performing the surgery under epidural anesthesia. The theory is that diminishing painful stimulation during the procedure may reduce the chance of triggering further hypersensitivity reactions.
-
Optimal Nerve Burial Site Selection:
- This is a critical decision. The final location of the proximal end of the nerve should be in a "safe haven" – an area protected from direct pressure, trauma, or tethering.
- Muscle Burial: Often preferred for superficial and deep peroneal nerves. The soft, vascular muscle tissue provides a cushioned environment and is thought to reduce the likelihood of neuroma formation by providing a less hostile environment for nerve regeneration.
- Bone Burial: Can be considered for nerves like the saphenous or sural, where a stable bony tunnel can protect the nerve end.
- Proximal Resection: Always aim for the most proximal possible transection and burial site, away from areas of previous trauma or potential future pressure. For instance, resecting the saphenous nerve just above the ankle in a patient who wears boots that might hit this level would be undesirable; a more proximal burial site would be advised. For the sural nerve, current best practice favors very proximal burial in the leg.
Patient Positioning and OR Setup: Foundation for Success
Alright, team, let's get our patient positioned. Proper positioning is crucial for optimal exposure and minimizing iatrogenic injury.
-
OR Table Setup:
- Ensure the table is equipped with appropriate attachments for patient safety and positioning. We'll need arm boards, safety straps, and potentially a beanbag.
- Have fluoroscopy available, although it's often not needed for soft tissue neuroma excisions, it's essential if we plan a bone burial.
-
Tourniquet Management:
- A pneumatic tourniquet should be available on the proximal thigh. While it can help with exposure by providing a bloodless field, we often choose not to inflate it for nerve explorations. Why? Because visualizing the small vessels accompanying the nerve helps us differentiate the nerve from adjacent vascular structures. In a bloodless field, a vein can look remarkably similar to a nerve, and we absolutely cannot make that mistake. If we need a clearer field, we might inflate it briefly, but generally, meticulous hemostasis with electrocautery is preferred.
-
Specific Nerve Positioning:
- Saphenous Nerve: Patient positioned supine. The leg will be externally rotated to facilitate medial exposure of the ankle and distal leg.
- Superficial and Deep Peroneal Nerves: Patient positioned supine. A rolled towel placed beneath the ipsilateral hip can help internally rotate the limb slightly, presenting the anterior and lateral aspects of the leg and foot more favorably.
- Sural Nerve: For distal resections, a rolled towel beneath the ipsilateral hip can provide better access to the nerve as it courses posteriorly. However, for the current choice of very proximal burial in the leg, we will position the patient in a semilateral decubitus position with the use of a beanbag. This allows excellent access to the posterolateral leg.
Intraoperative Execution: A Step-by-Step Surgical Journey (The Master Surgeon's View)
Now, let's get scrubbed in. We've identified our target, planned our approach, and our patient is positioned. Let's begin.
General Principles of Incision and Dissection
"Scalpel, please. We'll make our initial incision with a #15 blade. Remember, fellows, our approach should be an extensile exposure, following the anticipated line of the neurovascular structures. This allows us ample room for identification and dissection, especially given the variability of these nerves."
-
Skin Incision:
- "We begin just distal to the point of maximal tenderness, extending proximally along the anticipated course of the nerve. Make a clean, deliberate incision through the skin."
-
Subcutaneous Dissection:
- "Now, pick up the dissecting scissors. Deeper dissection is usually performed with these, carefully spreading tissue planes. We want to identify the nerve and separate it from surrounding soft tissues and, critically, from any accompanying vessels. Use gentle, blunt dissection as much as possible to avoid further nerve trauma."
- "Remember, the variability of several nerves, especially the superficial peroneal nerve, warrants extreme caution. Don't rush this step. Take your time. We're looking for that characteristic longitudinal orientation and whitish appearance of the nerve."
SURGICAL WARNING: "Fellows, this is absolutely critical. Under tourniquet, or even without, a vessel and a nerve can look remarkably similar in cross-section. The lesser saphenous vein, for instance, courses right alongside the sural nerve. You must examine the cross-section of the presumed nerve at the time of surgery. Even the most experienced surgeons have been fooled by a vein impersonating a nerve. Better to know at surgery than to be told by the pathologist the next day that you resected a vessel. A nerve will not have a lumen; a vein will."
-
Full Nerve Exposure:
- "Once identified, fully expose the nerve. Use appropriate retractors – small, delicate retractors are key here – to gently hold back surrounding tissue without compressing the nerve. Separate the nerve completely from any accompanying vessels before proceeding with resection and burial."
- "Dissection usually proceeds from distal to proximal. This allows us to identify the nerve in healthier tissue first, then trace it proximally to the point of injury or neuroma formation."
Sural Nerve Resection and Proximal Burial
"Let's walk through the sural nerve first, as it's a common target and best illustrates our principles."
- Incision and Initial Dissection:
- "Our patient is in a semilateral decubitus position. I'm making an incision along the posterolateral ankle and posterior leg, starting just distal to the area of maximal tenderness and extending proximally. We can use several skip incisions if the neuroma is extensive, typically three or four, to minimize the overall scar length, but for a good proximal burial, a single, longer incision often provides the best exposure."
- "As we deepen the incision, identify the lesser saphenous vein. This is our key landmark in the posterior leg, as it courses alongside the sural nerve."
- "Carefully dissect through the subcutaneous tissue. The sural nerve lies quite superficially here. Use fine dissecting scissors, spreading and cutting, to isolate the nerve."
- "See how it's becoming apparent? It's a whitish, cord-like structure. Confirm it's not a vessel by gently rolling it between your forceps – there's no lumen."
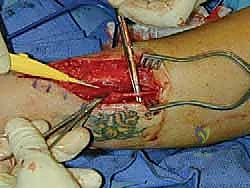
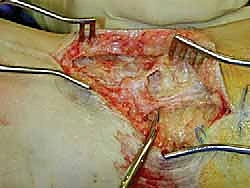
* "Here, you can see a small, nonpainful bulb neuroma from a superior peroneal nerve, buried in muscle (FIG 3). While this specific image shows the superior peroneal, the principle of identifying the nerve and its neuroma is the same for the sural. Our goal is to resect this bulb and bury the healthy proximal end."
-
Nerve Resection:
- "We'll trace the nerve proximally, well past the neuroma or injury site, into healthy, unscarred tissue. For the sural nerve, our current choice for burial is very proximally in the leg to minimize the chance of regrowth and subsequent neuroma formation in a weight-bearing or pressure area. This often means resecting a significant length of nerve."
- "Once we've identified our desired proximal transection point, use a fresh #15 blade to make a sharp, clean transection. A sharp cut minimizes crush injury to the nerve end, which theoretically might reduce neuroma formation. The resected nerve is usually quite long, as you can see in typical surgical images (TECH FIG 3 from the original text, though not provided here, implies a long segment)."
- "On the distal fragment, we can use electrocautery to coagulate the nerve end. This is thought to prevent nerve regeneration by producing neurotrophic signals that discourage axonal regrowth."
-
Proximal Burial into Muscle:
- "Now for the burial. We've identified a healthy muscle belly proximally – for the sural nerve, this might be the gastrocnemius or soleus. Create a small pocket within the muscle belly using blunt dissection or a small hemostat. Ensure it's deep enough to completely encapsulate the nerve end and away from any fascial planes or bony prominences."
- "Place the freshly cut, proximal nerve end deeply into this muscle pocket. Use a few interrupted absorbable sutures (e.g., 3-0 Vicryl) to close the muscle over the nerve end, effectively burying it. The goal is to provide a soft, vascular, protected environment, preventing the nerve from tethering or forming a new symptomatic neuroma."
- "Make sure there is no tension on the nerve end. It should lie comfortably within its new muscle bed."
Saphenous Nerve Transection and Burial
"For the saphenous nerve, our patient is supine with the leg externally rotated."
-
Incision and Identification:
- "Incision along the medial aspect of the distal leg and ankle. Carefully identify the great saphenous vein – the nerve runs closely with it. Dissect the nerve free from the vein and surrounding tissues."
- "Trace the nerve proximally, well above the ankle joint, to a site protected from boot tops or shoe pressure."
-
Resection and Burial:
- "Transect the nerve sharply. We'll create a muscle pocket, perhaps in the tibialis anterior or the medial head of the gastrocnemius, depending on our proximal dissection. Bury the nerve end deep within the muscle, securing it with absorbable sutures."
- "Alternatively, if the bone is readily accessible and a muscle belly isn't ideal, we might consider bone burial for the saphenous nerve. If burying into bone, we need to expose the area of bone to receive the nerve. Incise the periosteum, then use a small drill with a 2.5-mm or 3.5-mm drill bit and a drill sleeve to create an appropriate hole. The nerve end is then placed into this bone tunnel, and the periosteum or a small bone plug can be used to secure it."
Superficial Peroneal Nerve Transection and Burial
"Patient remains supine, with the hip roll facilitating exposure of the anterolateral leg and dorsum of the foot."
-
Incision and Identification:
- "Incision along the anterolateral aspect of the leg or dorsum of the foot, depending on the neuroma's location. This nerve has significant anatomical variability, so careful, layer-by-layer dissection is paramount."
- "Identify the main trunk or its medial and intermediate dorsal cutaneous branches. Trace it proximally, ensuring we're past any areas of scarring or injury."
-
Resection and Burial:
- "Transect the nerve sharply. We'll typically bury this into the tibialis anterior muscle belly. Create a deep muscle pocket, place the nerve end, and close the muscle over it with absorbable sutures. Ensure it's well away from any bony prominences or areas of potential direct pressure from footwear."
Deep Peroneal Nerve Transection and Burial
"Again, patient supine. This nerve is typically found deeper, accompanying the anterior tibial artery."
-
Incision and Identification:
- "Incision along the anterior ankle or dorsum of the foot, often in line with the first web space where its sensory branch terminates. Careful dissection is needed to identify the nerve, often alongside its vascular bundle. Remember its motor components to the anterior compartment muscles and FHB, so we're typically targeting its sensory branch or a specific neuroma."
- "Given its proximity to major vessels, meticulous hemostasis and careful blunt dissection are critical."
-
Resection and Burial:
- "Transect the sensory component or the neuroma sharply. Burial is usually into an adjacent muscle belly, such as the tibialis anterior or extensor digitorum brevis. Create a secure, tension-free muscle pocket and close over the nerve end."
- "While motor nerves can be sectioned, remember the higher cost in terms of functional deficit. The motor loss of the DPN branches is relatively well tolerated compared to the posterior tibial nerve, but still, we aim to preserve motor function where possible."
Dorsomedial Cutaneous Nerve Transection and Burial
"This is a specific branch of the superficial peroneal nerve, often injured during bunionectomies."
-
Incision and Identification:
- "Incision along the dorsomedial aspect of the hallux, often through the previous bunionectomy scar. Careful dissection is required to find this small, delicate nerve branch, which may be entangled in scar tissue."
-
Resection and Burial:
- "Once identified, trace it proximally to healthy tissue. Transect sharply. Due to its small size and superficial location, burial can be challenging. We aim for a small muscle belly, like the abductor hallucis, or deep into the subcutaneous fat, well away from the incision line and any potential pressure points. A small, secure pocket is paramount."
Wound Closure
"Once the nerve is successfully buried, we'll proceed with meticulous wound closure. Irrigate the wound thoroughly. Close the deep fascia, if opened, with absorbable sutures. Then, close the subcutaneous layer to obliterate dead space. Finally, a neat skin closure, either with staples or fine absorbable sutures, followed by a sterile dressing. A soft compressive dressing is usually sufficient."
Pearls and Pitfalls: Navigating the Surgical Minefield
Fellows, this is where experience truly shines. Anticipating problems and knowing how to react is key.
- Pitfall 1: Misidentification of Nerve vs. Vessel.
- Pearl: As discussed, always examine the cross-section. A nerve is solid; a vein has a lumen. If in doubt, do not transect. Trace further proximally or distally to confirm identity. Use electrical stimulation if available and appropriate for motor nerves (though less useful for purely sensory neuromas).
- Pitfall 2: Incomplete Resection or Insufficient Proximal Burial.
- Pearl: Always resect the nerve well into healthy tissue, proximal to the neuroma and any scar tissue. The goal is to get the nerve end into a soft, protected environment where it won't be irritated. If the burial site is too superficial or under tension, a new neuroma can form.
- Pitfall 3: Injury to Adjacent Structures.
- Pearl: Meticulous, layer-by-layer dissection with blunt instruments where possible. Identify and protect all other neurovascular structures. Always have a clear understanding of the 3D anatomy.
Additional Intraoperative Imaging & Surgical Steps
REFERENCES
references ( TECH FIG 2 ).
-
Subcutaneous and skin sutures are usually bioresorbable to avoid any irritation in neuritic patients.
-
Identify the nerve proximally beneath the gastrocnemius fascia.
-
Tension is placed on the proximal end of the nerve while it is sharply cut in an oblique fashion and allowed to retract into the surrounding tissues.


TECH FIG 3 • A long incision exposing the sural nerve with a neuroma at its end.
DEEP PERONEAL NERVE RESECTION AND BURIAL
- The deep peroneal nerve runs along the anterior border of the distal tibia; thus, the bone offers a fine burial site for the proximal nerve ending.
-
Isolate and cut the nerve distally and cauterize the distal end.
-
Bring the proximal nerve to a resting location over the tibia.
-
A straight anterolateral incision over the distal lateral border of the tibia works well; in cases of simultaneous superior peroneal nerve resection, a curved-S incision from this site more proximal and posterior allows an easy dual procedure.
-
The periosteum can be incised and drilled as above. Use a drill sleeve and round off or bevel the proximal edge of the hole to avoid a sharp edge for the nerve entry.
-
Incise the superficial retinaculum over the extensors in line with the incision and bluntly separate the muscles. The deep peroneal nerve usually lies between the extensor digitorum longus and the extensor hallucis longus muscles. Two large anterior tibial veins and the artery are close by the nerve; careful dissection avoids a messy field.
-
Copiously irrigate the wound and then place the nerve into the distal tibial hole without tension.
-
Allow the muscles to fall back over top the burial site. Repair the retinaculum if possible.
-
Subcutaneous and skin sutures are bioabsorbable.
SUPERIOR PERONEAL NERVE RESECTION AND BURIAL
- Start with a longitudinal incision over the anterior compartment of the leg.
-
Find the superficial peroneal nerve as it pierces the crural fascia about 10 to 12 cm proximal to the tip of the fibula.
-
The course is variable; the surgeon may need a more distal exposure to find the nerve and then trace it back proximally.
-
Isolate the nerve and decide on the burial site in the fibula ( TECH FIG 4 ) or into muscle ( TECH FIG 5 ).
-
The peroneal muscles can be split manually and the bone easily palpated.
-
The fibula can then be held in easy exposure with two small Hohmann retractors on each side of the bone.
-
The flat anteromedial wall of the fibula provides a fine resting place for the nerve.
-
Incise the periosteum longitudinally if it is thick enough to merit such action.
TECH FIG 6 • Drilling unicortical hole in fibula for transected superior peroneal nerve ending. (Note: drill guard removed for illustrative purposes.)
-
The periosteum does not need to be sutured to the nerve epineurium to hold position.
-
Gently remove the retractors, allowing the muscle to fall back over the fibula.
-
Close the subcutaneous tissues with resorbable suture and close the skin with a resorbable suture as well, eliminating the need for suture removal.
-
Cut the nerve sharply in the distal aspect of the dissection.
-
Careful observation for a proximal split and a high medial superior peroneal nerve branch is important. If found, bury both branches or resect the nerve before the split.
-
A splint is optional, depending on concomitant procedures and the amount of dissection.
-
Hold the distal portion of the nerve with a hemostat and cauterize it to prevent leakage of neurotrophic hormones.
-
With a 3.5-mm drill bit, make a unicortical drill hole 3 to 4 cm proximal to the distal extent of the cut superior peroneal nerve to allow sufficient slack to bury the nerve without tension ( TECH FIG 6 ). Carefully retract the nerve to prevent it from getting caught in the drill. Once the hole is made, angle the drill proximally to bevel the edge, allowing soft entry into the bone.
-
Place the cut end of the proximal superior peroneal nerve into the hole after irrigation ( TECH FIG 7 ).
-
The nerve should have little tension on it and should be stable with ankle plantarflexion or dorsiflexion.
DORSOMEDIAL CUTANEOUS NERVE
- This nerve is commonly damaged near the first metatarsal head in bunion surgery ( TECH FIG 8 ). If a local block at the base of the metatarsal or cuneiform relieves the pain, then distal burial is a preferred solution.
the hole proximally to allow a smooth gliding entrance for the nerve.
-
Irrigate the wound and place the nerve into the hole; a tagging suture is usually unnecessary.
-
Close the skin and subcutaneous tissues in a standard fashion with resorbable suture.
-
The incision often incorporates a prior incision over the dorsal metatarsal and is brought proximally over the cuneiform. Visualize the nerve and transect it as distally as possible; the surgeon need not find the distal neuroma if a proximal block relieved the pain. Cauterize the distal end and dissect the proximal end free.
-
Using a 2.5-mm drill bit, drill a hole in the base of the first metatarsal or the medial cuneiform, whichever bone seems best anatomically for the nerve to inhabit. Bevel
SAPHENOUS NERVE RESECTION AND BURIAL
- Make a longitudinal incision over the lesser saphenous vein in the supramalleolar region of the medial ankle. The deep dissection should allow identification of the vein as well as the saphenous nerve. The nerve can be deceptively small here and has sometimes been found directly behind the vein. Take care to look for any branching ( TECH FIG 9 ).
-
Cut the nerve distally and cauterize all distal branches to limit postoperative leakage of any chemoattractants.
-
Dissect the proximal nerve ending free and clear an appropriate spot on the medial tibia.
-
Incise the periosteum and use a 2.5-mm or 3.5-mm drill bit (depending on the size of the nerve) to drill a unicortical hole. Tilt the drill bit proximally to round off the proximal edge and allow atraumatic nerve entry.
-
Perform final irrigation of the wound. Place the nerve in the bone hole without tension. A suture from the periosteum to the epineurium is optional but rarely used any more.
-
Close the subcutaneous tissues and then the skin with absorbable suture to limit any postsurgical irritation of the surgical site.
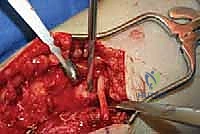
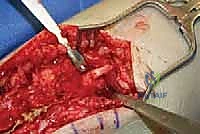
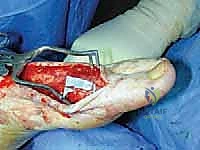
TECH FIG 9 • Saphenous nerve neuroma and small anterior branch.
MEDIAL PLANTAR NERVE
- Make a longitudinal incision along the course of the nerve on the plantar foot, attempting to avoid the heel and the ball, the primary weight-bearing areas.
-
Transect the nerve distally and bring it as far proximally in the midfoot as possible. Cut the nerve obliquely with an adequate length to allow burial into the deep musculature of the quadratus ( TECH FIG 11 ).
-
Gently carry the dissection through the subcutaneous tissues. The nerve lies just under the deep fascia. Take care to dissect the various branches to ensure adequate denervation ( TECH FIG 10 ).
-
Close the subcutaneous tissues and skin with resorbable suture.
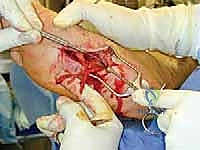
TECH FIG 10 • Dissection of the medial plantar nerve and branches.
TIBIAL NERVE
- Approach the tibial nerve in the supramalleolar space, similar to the tarsal tunnel incision. Resection of this nerve is for extreme salvage as a possible precursor to amputation.
-
Obliquely resect the nerve proximally, leaving a length adequate for tension-free burial into the medial tibia.
-
Using a 3.5to 5.0-mm drill, acquire a burial site in the tibia. Bevel the unicortical hole proximally to allow an easy slide of the nerve into the tibia without a sharp edge.
-
Resect the tibial nerve and branches, including possible high calcaneal branches, as distally as possible, cauterizing the distal ends to reduce chemoattractants.
-
Close the subcutaneous tissues and skin with bioresorbable suture.
💡 Pearls and Pitfalls
Diagnosis
- The nerve injury can be difficult to discern and may be associated with other pathology, which is usually addressed at the same surgical procedure.Nerve resection level
- The nerve should be cut above the level of multiple branching to simplify burial. The worry about ob- scure branches of other nerves providing innervation to the distal nerve remains.Burial of nerve into
- The surgeon should beware of an inadequate retraction and the mistake of wrapping the nerve in bone hole the drill bit; a tissue protector should be used when possible.
The foot, ankle, and knee are ranged while observing the nerve before closure.
A more proximal hole can always be drilled to eliminate tension on the nerve.
One case of fibular fracture occurred at the nerve burial hole. The patient did very well with conserva-
tive treatment.
Postoperative pain
- Hypersensitivity often occurs in the early postoperative period as neighboring nerves react to the loss of a neighbor.
- “Zingers” will often occur 1 to 3 weeks postoperatively and represent growth of the proximal nerve ending. These nerve pains will ease with time and are much better tolerated when the patient expects such a reaction to nerve resection.
Postoperative Care
-
The Postoperative Rehabilitation Must Strike A Balance Between Early Return Of Motion And Avoidance Of Mechanical Trauma To The Resected Nerve.
-
If the nerve is buried, immobilization time allows scarring into place.
-
Many of these patients have some element of complex regional pain syndrome or reflex sympathetic dystrophy, so any stiffness will take a great deal of rehabilitation to recover full motion.
-
Dellon and Aszmann 2 reviewed 11 cases of superior peroneal nerve resection into anterior muscle with good or excellent results. They recommended compartment release as well.
-
Miller 3 reviewed nine cases of dorsomedial cutaneous nerve resection and burial into the dorsal bones of the foot, with a verbal analogue scale improvement from 8.6 to 2.0 (on a 0-to10 scale). All patients had relief of symptoms but most had a concurrent procedure to correct foot abnormality.
-
The use of resorbable suture material seems especially prudent in these nerve patients, who are often hypersensitive after surgery.
-
For simple neurectomy, the patient should have a soft compressive dressing with early range-of-motion exercises. Desensitization and nerve retraining should begin early.
COMPLICATIONS
- Most patients will have some degree of adjacent sensory nerve hypersensitivity; it can be better tolerated with advance warning.
-
Wound infection
-
Neuroma
-
Many patients also get “zingers” starting at 7 to 14 days or so and lasting up to a month or so. These “electric” jolts of pain follow the resected nerve’s distal sensory distribution and represent irritation of the cut proximal nerve ending. They usually begin to lessen in frequency and intensity after a week or so and gradually disappear. Again, discussion with the patient beforehand eliminates frantic office calls about the nerve growing back so quickly.
-
For nerve resection and burial, the patient usually has a fairly high amount of pain simply from the mobilization of the muscle to allow nerve implantation. A well-padded splint similar to a Robert Jones dressing gives nice compression and stabilization for the initial 12to 14-day postoperative period. After this time, a simple compressive wrapping will usually be sufficient and allows gradual recovery of range of motion.
OUTCOMES
- Chiodo and Miller 1 compared superior peroneal nerve resection and burial into muscle versus bone; the results favored burial into the fibula when possible.
-
Sixteen patients had burial into muscle, with improvement in the verbal analogue pain score (0 to 10) of 3.1 points and 46% relief of pain. Four required reoperation for neuroma.
-
Fifteen patients had burial into bone, with improvement in the pain score (0 to 10) of 5.4 points and 75% pain relief (statistically better than the muscle group).
-
Neuroma can be expected to form at the end of a cut nerve as the nerve tries to reconnect with the distal end. Nerves can grow into:
-
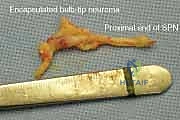
Bulb neuroma: a small thickening on the end of the nerve; usually causes little pain ( FIG 4 )
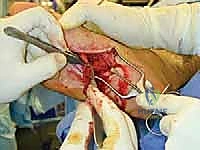
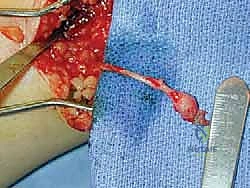
FIG 4 • Simple bulb neuroma after sural nerve resection.
was missed at the prior surgery or if a new branch developed ( FIG 5 ).
-
Adjacent nerves can sometimes provide an unexpected “feeder” innervation to the distal aspect of the resected nerve.
-
Dysesthesias can be troublesome, with persistent pain in the distal nerve distribution.
-
Denervation hyperesthesias can be horrible, with difficulty eradicating pain from nerve surgery.
-
Chiodo CP, Miller SD. Surgical treatment of superficial peroneal neuromas. Foot Ankle Int 2004;25:689–694.
-
Dellon AL, Aszmann OC. Treatment of superficial and deep peroneal neuromas by resection and translocation of the nerves in the anterolateral compartment. Foot Ankle Int 1998;19:300–303.
-
Miller SD. Dorsomedial cutaneous nerve syndrome: treatment with nerve transection and burial into bone. Foot Ankle Int 2001;22: 198–202.
-
O’Neill PJ, Parks BG, Walsh R, et al. Excursion and strain of superficial peroneal nerve strain during inversion ankle sprain. J Bone Joint Surg Am 2007;89A:979–986.
-
Redfern DJ, Sauve PS, Sakellariou A. Investigation of incidence of superficial peroneal nerve injury following ankle fracture. Foot Ankle Int 2003;24:771.
-
Schon, LC, Anderson, CD, Easley ME, et al. Surgical treatment of chronic lower extremity neuropathic pain. Clin Orthop Relat Res 2001;389:156–164.
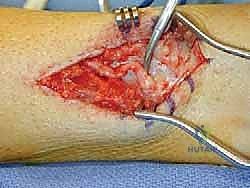
FIG 5 • Previous burial of superior peroneal nerve into bone with mild neuritis and small more proximal branch.
-
Unorganized neuroma: a thick mass of nerve endings, usually with small very irritable extensions causing pain
-
Nerve can regrow and reinnervate the distribution.
-
The speed of nerve regrowth should be 1 mm/day but can be faster.
-
Nerves can sprout new “rootlets” that will attempt to reinnervate the target area. Sometimes it may be difficult to determine whether a more proximal branch
You Might Also Like