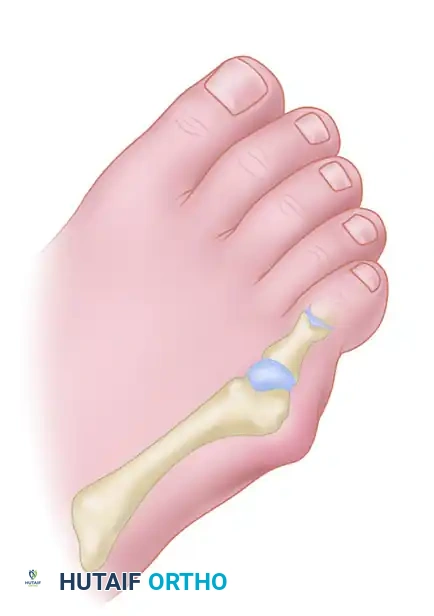
Uniportal Endoscopic Decompression of the Interdigital Nerve for Morton's Neuroma: A Surgical Masterclass
Key Takeaway
Join us in the OR for a masterclass on uniportal endoscopic decompression of Morton's neuroma. We'll meticulously cover patient positioning, a 1cm incision, precise TIML release using a 30-degree scope and specialized knife, and critical anatomical considerations. Learn essential pearls, potential pitfalls, and comprehensive postoperative management to optimize patient outcomes and minimize complications.
Alright team, let's get started. Today, we're tackling a common and often debilitating condition: Morton's neuroma, specifically utilizing the uniportal endoscopic decompression technique. This approach, a refined modification of Barrett and Pignetti's original concept, offers significant advantages over traditional open procedures—think smaller incisions, faster recovery, and a reduced risk of hematoma and infection. Our goal is to decompress the intermetatarsal nerve by releasing the transverse intermetatarsal ligament (TIML), thereby alleviating the entrapment without resecting the nerve, preserving sensation, and avoiding the dreaded stump neuroma.
Understanding Morton's Neuroma: Anatomy and Pathophysiology
Before we make any incisions, a thorough understanding of the underlying pathology and relevant anatomy is paramount. Morton's neuroma is essentially an entrapment neuropathy where the intermetatarsal nerve, most commonly in the second or third web space, becomes compressed by the transverse intermetatarsal ligament. This chronic compression leads to perineural fibrosis and nerve enlargement.
Comprehensive Surgical Anatomy
Let's review the critical structures we'll encounter:
- The Intermetatarsal Nerve: This is our target. It lies plantar to the transverse intermetatarsal ligament. In cases of neuroma, it often appears thickened distally, gradually tapering to a more normal caliber proximally. During our endoscopic approach, with the cannula properly positioned, the nerve should be protected and not directly visualized as we divide the TIML. However, if we rotate our cannula 180 degrees to the 6 o'clock position, we can often visualize it, especially if it's bulbous or obscured by fat.
- The Transverse Intermetatarsal Ligament (TIML): This is the primary culprit in nerve compression. It's a robust, fibrous band, a continuation of the plantar plates, spanning between the metatarsal heads. It typically measures 10 to 15 mm long and 2 to 3 mm thick. Biomechanically, it becomes taut during the late midstance and push-off phases of gait, exacerbating nerve compression. Our entire procedure hinges on precisely identifying and releasing this ligament.
- The Lumbrical Tendon: Situated on the plantar lateral aspect of the TIML. This structure is the most likely to be inadvertently severed during endoscopic decompression. While some literature, including my own experience, suggests that inadvertent severing has not resulted in adverse sequelae, meticulous identification and avoidance are always preferred.
- The Plantar Interossei Muscles: These muscles are located superior to the TIML in the second, third, and fourth intermetatarsal spaces. They serve as a dorsal boundary to our dissection plane.
- Metatarsal Heads and Necks: These bony landmarks define the intermetatarsal space. The relationship of the soft tissues to these bony structures is key for accurate instrument placement.
- Neurovascular Considerations: Beyond the intermetatarsal nerve itself, remember the digital arteries and veins that accompany the nerve. While the endoscopic approach minimizes broad dissection, precise identification of the TIML and maintaining a tight relationship with the cannula ensures these structures, particularly the nerve, are not inadvertently damaged during the cutting phase.
Clinical Presentation and Diagnostic Workup
Patients typically present with dull, aching pain in the ball of the foot, often radiating into the affected toes (second, third, or fourth). This may be accompanied by tingling, burning, or numbness. Symptoms often worsen with narrow-toed shoes or high heels and are sometimes relieved by removing the shoe.
Physical Findings:
* Localized tenderness in the affected web space.
* Subtle swelling.
* Slight separation of adjacent toes.
* Mulder's Click: A palpable snap elicited by compressing the forefoot and simultaneously applying plantar and dorsal pressure to the interspace.
* Metatarsal Compression Test: Positive if squeezing the patient's forefoot reproduces symptoms.
Imaging and Diagnostic Studies:
* Plain Films: Always perform preoperatively to rule out other pathologies like metatarsal stress fractures or Freiberg disease (avascular necrosis of the metatarsal head).
* Sonography (Ultrasound): In experienced hands, this is highly accurate. A neuroma appears as a hypoechoic oval mass in the interspace at the level of the metatarsal heads, and its size can be measured. It's excellent for confirming the diagnosis and pinpointing the exact web space.
* MRI: While not operator-dependent, it can yield a higher percentage of false-negative and false-positive findings and is significantly more costly than sonography.
* Diagnostic Lidocaine Injection: Can precisely identify the symptomatic web space. If both the second and third web spaces are symptomatic, consider endoscopy on both.
Differential Diagnosis
It's crucial to differentiate Morton's neuroma from other forefoot pathologies:
* Metatarsal stress fracture
* Freiberg disease
* Synovitis (e.g., MTP synovitis)
* Intermetatarsal bursitis
* Peripheral neuropathy
* Lumbar radiculopathy
* Tarsal tunnel syndrome
* Vascular claudication
* Spinal stenosis
Indications for Surgery
Surgery is indicated only after a minimum of 6 months of failed conservative treatment. This includes metatarsal pads, orthotics, shoes with a wide toe box, steroid injections, and alcohol injections. In our experience, conservative measures are successful in about 70% of patients. When these fail, and the patient's quality of life remains significantly impacted, surgical decompression becomes a viable option.
Preoperative Planning and Patient Positioning
Now, let's prepare our patient and the operating field.
Patient Positioning
- Supine on the Operating Table: The patient will be positioned supine.
- Leg Alignment: We'll place a bump under the ipsilateral buttock and thigh to prevent the leg from externally rotating. This ensures the foot is stable and in a neutral position for optimal access.
- Foot Placement: The toes should extend just beyond the end of the table, allowing for manipulation and tensioning of the forefoot, while the heel firmly rests on the table. This provides stability and allows for dorsiflexion of the metatarsophalangeal (MTP) joints, which can help open the interspace.
Anesthesia and Prophylaxis
- Anesthesia Choice: Anesthesia can be general or regional (popliteal or ankle block).
- Crucial Warning: Local anesthesia should be avoided in the immediate surgical field as it can distort the delicate endoscopic anatomy, making identification of the TIML more challenging.
- Prophylactic Antibiotics: Administer prophylactic intravenous antibiotics as the patient enters the operating room.
- Tourniquet: We will routinely use an ankle tourniquet, inflated to 250 mm Hg, to ensure a bloodless field, which is essential for clear endoscopic visualization.
Equipment Setup
Ensure the following specialized equipment is ready:
* AM Surgical Set: This includes the specialized elevator, slotted cannula, obturator, locking device, and disposable knife blade.
* Endoscope: A 30-degree, 4-mm scope. This angle provides excellent visualization within the narrow interspace.
Uniportal Endoscopic Decompression: Step-by-Step Intraoperative Execution
Alright fellows, we're scrubbed in, the patient is prepped and draped, and the tourniquet is up. Let's begin.
Step 1: Incision and Initial Dissection
"Scalpel, please. We're making a small, 1-cm vertical incision in the appropriate web space. Remember, we've confirmed this with preoperative ultrasound and palpation."
- Make the incision directly over the affected interspace, centered just proximal to the metatarsal heads.
- "Now, take the blunt Stevens scissors. Gently spread the subcutaneous tissue to create a working channel. We want to be careful here, avoiding any aggressive dissection that could damage superficial neurovascular structures or create unnecessary tissue trauma."
Step 2: Cannula Insertion and Initial Visualization
"Next, we'll introduce our slotted cannula and obturator. This is a critical step for establishing our endoscopic plane."
- "Insert the slotted cannula and obturator through the same path we just created. Feel for the TIML with the tip of the obturator. We want to advance it just plantar to and scraping against the TIML."
- "Ensure the slot of the cannula is facing dorsally, at the 12 o'clock position." This orientation is crucial for protecting the nerve, which lies plantar to the TIML.

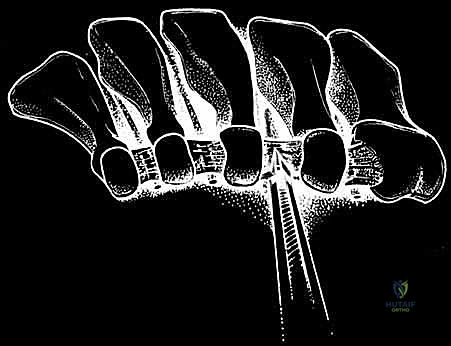
TECH FIG 1 • Surgical technique for uniportal endoscopic decompression of the intermetatarsal nerve. Cannula is in the interspace just plantar to the transverse intermetatarsal ligament and dorsal to the intermetatarsal (interdigital) nerve. The transverse intermetatarsal ligament is being transected from distal to proximal. (Courtesy of AM Surgical.)
- "Once the cannula is in position, remove the obturator. We often get some fat or fluid egressing. Use absorbent cotton-tipped applicators to clear any debris or fluid from the cannula. A clear field is paramount for visualization."
Step 3: Endoscopic Exploration and TIML Identification
"Now, let's get our eyes in there."
- "Insert the short 4-mm, 30-degree scope into the cannula."
- "Advance the scope slowly. You should now be able to visualize the entire transverse intermetatarsal ligament (TIML). It appears as a dense, white, fibrous band spanning across the interspace."
- "Look carefully. The lumbrical tendon can often be seen just lateral to the TIML on its plantar aspect. Identify it, but remember, our target is the TIML itself."
Step 4: Ligament Delamination and Nerve Protection
"Before we cut, we need to ensure our plane is clear and the nerve is well-protected."
- "Take the AM Surgical elevator. Insert it through the cannula alongside the scope."
- "Use the elevator to palpate and gently separate the TIML from the surrounding soft tissues. Scrape the elevator both dorsal and plantar to the TIML." This maneuver helps create a clear working space and ensures the nerve is pushed plantarward, away from the ligament, further enhancing its protection.
Step 5: Optional Nerve Visualization
"Sometimes, for academic purposes or if there's any doubt about the pathology, we might want to glimpse the nerve itself."
- "If you wish to visualize the intermetatarsal nerve, carefully rotate the cannula 180 degrees so that the slot is now facing plantar, at the 6 o'clock position."
- "With this rotation, the nerve can often be seen, unless it's obscured by significant adipose tissue. You'll observe its characteristic appearance: often thickened distally, gradually tapering proximally. Once you've confirmed its location, return the cannula to the 12 o'clock position to ensure the nerve is protected beneath the solid portion of the cannula during the cutting phase."
- "Now, remove the scope from the cannula for a moment."
Step 6: Assembling and Introducing the Endoscopic Knife
"We're ready to prepare our cutting instrument."
- "Take the disposable endoscopic knife and slide it onto the locking device, ensuring the lever is in the open position."
- "Insert this knife and locking device assembly into the scope. Advance the knife blade until it nearly touches the lens of the scope. The blade should also be parallel to the lens for optimal visualization and controlled cutting."
- "Once positioned, push the lever of the locking device forward until it's finger tight. This secures the blade."

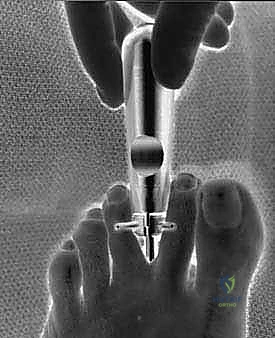
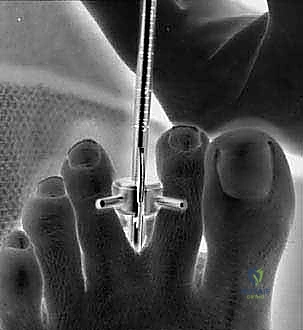
TECH FIG 5 • Intraoperative view of knife mounted to scope in position in cannula ready to enter second web space and transect the transverse intermetatarsal ligament.
Step 7: Transecting the Transverse Intermetatarsal Ligament
"This is the money shot, fellows. Precision is key here."
- "Advance the scope and knife assembly through the cannula."
- "Under direct endoscopic visualization, you will clearly see the knife blade. Carefully visualize the knife blade transecting the TIML from distal to proximal."
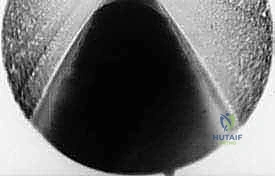
TECH FIG 6 • A. Endoscopic view of transverse intermetatarsal ligament.
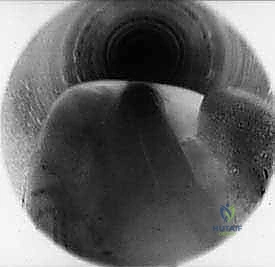
TECH FIG 6 • B. Endoscopic view of knife blade transecting the transverse intermetatarsal ligament.
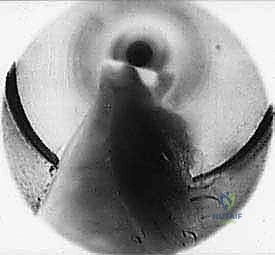
TECH FIG 6 • C. Endoscopic view of knife blade transecting the transverse intermetatarsal ligament.
> SURGICAL WARNING: Hugging the TIML
> While cutting the TIML, it is absolutely critical to maintain the cannula tight against the ligament. This ensures the underlying intermetatarsal nerve is maximally protected by the solid, plantar aspect of the cannula. Any deviation risks injury to the nerve.
- "To provide additional tension on the TIML, which facilitates a clean cut, use a finger of your non-dominant hand to place gentle manual digital pressure between the adjacent metatarsal necks." This maneuver makes the ligament more prominent and taut for the blade.
TECH FIG 6 • D. Endoscopic view after release of transverse intermetatarsal ligament.
Step 8: Confirmation of Complete Transection
"Once you believe the ligament is fully transected, we must confirm it."
- "Withdraw the scope and knife assembly. Remove the knife from the scope."
- "Reinsert the scope alone into the cannula."
- "Carefully inspect the interspace endoscopically. You should see the divided edges of the ligament. To further confirm, apply manual digital pressure between the adjacent metatarsal heads; you should observe the divided ligament edges further separating, indicating a complete release."
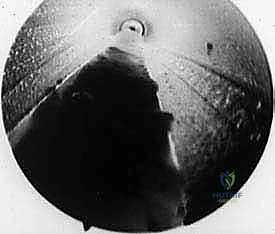
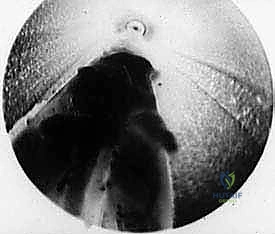
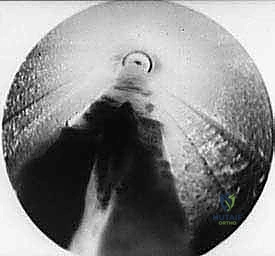
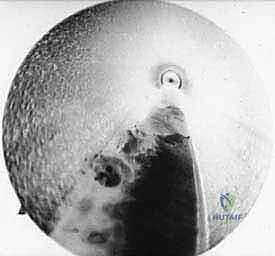
Step 9: Irrigation and Palpation
"Let's clean up the field and perform a final tactile check."
- "Irrigate the wound thoroughly through the cannula to remove any blood or debris."
- "Remove the cannula. Now, insert the elevator into the wound and palpate the interspace. The previously taut TIML should no longer be palpable. This tactile feedback provides an additional confirmation of successful release."
Step 10: Wound Closure and Dressing
"We're almost done here."
- "Deflate the tourniquet. Allow for reperfusion and ensure hemostasis."
- "Irrigate the wound again."
- "Close the small incision with one or two interrupted mattress sutures. I prefer mattress sutures for good eversion and skin approximation."
- "Apply a soft compression dressing and fit the patient with a postoperative shoe."
Alternative: Neurectomy (If Indicated)
"A quick note on neurectomy. While our primary goal with this endoscopic technique is decompression to avoid the complications of nerve resection, there are rare instances where a neurectomy might be considered."
- "If, during your initial assessment or even intraoperatively, you encounter a nerve that is exceptionally large and bulbous, and you believe decompression alone might be insufficient, you have the option to convert to an open approach. In such cases, the incision can be extended proximally 1 to 2 cm, and a neurectomy can be performed in the routine fashion. However, remember the trade-offs: loss of sensation and the potential for a stump neuroma, which can be more debilitating than the original condition."
Pearls and Pitfalls
Let's discuss what can go wrong and how to avoid or manage it.
💡 Pearls and Pitfalls
- Hugging the TIML with the cannula while cutting is absolutely paramount. This is your primary safeguard for the interdigital nerve. Deviating from this principle is the most common cause of iatrogenic nerve injury.
- If you are unable to clearly visualize the TIML endoscopically, abort the endoscopic procedure and convert to an open procedure. Attempting to cut blindly or with poor visualization is a recipe for disaster. It's always safer to convert than to cause irreversible damage.
- Incomplete Release: A common pitfall. Ensure you visualize the full length of the TIML and confirm complete transection both visually (separation of edges) and tactilely (loss of palpable tautness). An incomplete release will lead to persistent symptoms.
- Lumbrical Tendon Injury: While reported to have no adverse sequelae, meticulous identification of the lumbrical tendon, which lies plantar lateral to the TIML, and careful avoidance during dissection and cutting, is best practice.
- Fat or Fluid Obstruction: The interspace can be filled with fat or accumulate fluid/blood, obscuring visualization. Frequent irrigation and clearing with cotton-tipped applicators are essential for maintaining a clear endoscopic view.
- Metatarsal Head Injury: Aggressive manipulation or misdirection of instruments can potentially damage the articular cartilage of the metatarsal heads. Always work within the soft tissue envelope of the interspace.
- Misdiagnosis: Ensure your preoperative workup is thorough. Operating on a patient with a stress fracture or Freiberg's disease under the assumption of a neuroma will not yield a good result.
Postoperative Care and Complication Management
Our job isn't done until the patient is fully recovered.
Postoperative Care Protocol
- Immediate Postoperative Period (First 48-72 hours):
- Ice and elevation are strongly recommended to minimize swelling and pain.
- The patient will remain in the postoperative shoe.
- Weight-bearing as tolerated is permitted in the surgical shoe. Provide crutches or a walker as needed for comfort and stability, especially in the first few days.
- Suture Removal: Sutures are typically removed in 12 to 14 days postoperatively. We revised our protocol from 10-14 days to specifically 12-14 days after experiencing two wound dehiscences early on, which has since eliminated this issue.
- Shoe Progression: After suture removal, the patient may transition to a comfortable shoe or sandal. Avoid narrow-toed shoes or high heels for several weeks to months to prevent recurrence of symptoms.
- Rehabilitation: Encourage early, gentle range of motion of the MTP joints to prevent stiffness. Formal physical therapy is typically not required for this procedure, but patient education on activity modification and appropriate footwear is crucial.
Potential Complications and Management
- Infection: In our initial series of 50 patients, we had no infections, which is a testament to the minimally invasive nature of the procedure and strict sterile technique. Should an infection occur, standard wound care, oral antibiotics, and potentially surgical debridement would be indicated.
- Wound Dehiscence: As mentioned, we observed two cases early on, which healed uneventfully with conservative management. Adjusting our suture removal protocol to 12-14 days has prevented further occurrences. Ensure proper skin edge approximation and avoid tension during closure.
- Persistent Pain/Incomplete Release: If the patient's symptoms persist postoperatively, it's crucial to re-evaluate. This could indicate an incomplete release, a misdiagnosis, or the presence of another concurrent pathology. Re-imaging with ultrasound or MRI may be necessary. Revision surgery, potentially an open approach, might be considered if an incomplete release is confirmed.
- Stump Neuroma: A significant advantage of decompression over neurectomy is the avoidance of stump neuroma formation. This complication is typically associated with nerve resection, where the transected nerve stump can form a painful neuroma.
- Recurrence of Symptoms: While rare with proper technique, recurrence can occur if the ligament scarifies or if the underlying biomechanical issues (e.g., inappropriate footwear, foot deformities) are not addressed.
- DVT Prophylaxis: Follow your institutional guidelines for deep vein thrombosis prophylaxis, especially for patients with additional risk factors.
This uniportal endoscopic decompression technique, when performed meticulously, offers excellent outcomes for patients suffering from Morton's neuroma. Remember the critical anatomical relationships, prioritize nerve protection, and ensure a complete release. Any questions, fellows? Let's review the images one more time.
REFERENCES
-
Vigorous activities such as running or racquet sports should be avoided for 4 to 6 weeks.
-
Barrett SL, Pignetti TT. Endoscopic decompression for routine neuroma: preliminary study with cadaveric specimen: early clinical results. J Foot Ankle Surg 1994;33:503–508.
-
Dellon AL. Treatment of Morton’s neuroma as a nerve compression; the role for neurolysis. J Am Podiatr Med Assoc 1992;82:399–402.
-
Gauthier GT. Morton’s disease: a nerve entrapment syndrome: a new surgical technique. Clin Orthop Relat Res 1979;142:90–92.
-
Graham CE, Graham DM. Morton’s neuroma: a microscopic evaluation. Foot Ankle 1984;5:150–153.
-
Shapiro PS, Shapiro SL. Sonographic evaluation of interdigital neuroma. Foot Ankle 1995;16:604–606.
-
Shapiro SL. Endoscopic decompression of the intermetatarsal nerve for Morton’s neuroma. Foot Ankle Clin North Am 2004;9:297–304.
-
Patients should be advised that complete resolution of symptoms may take up to 4 months.
OUTCOMES
- Barrett and Pignetti reported 88% good and excellent results in over 40 patients. 1
- In our first 24 patients, there were 82% good and excellent results at 6 months postoperatively.
You Might Also Like