INTRODUCTION TO CORONOID FRACTURES AND ELBOW STABILITY
The ulnar coronoid process is the keystone of elbow stability. Functioning as the primary anterior buttress of the greater sigmoid notch, it provides critical resistance against posterior subluxation of the ulna and acts as a primary restraint to varus stress. Coronoid fractures occur in 10% to 15% of all elbow dislocations. Because of the complex ligamentous and tendinous attachments—including the anterior band of the medial collateral ligament (AMCL) at the sublime tubercle, the anterior joint capsule, and the brachialis tendon—displaced fractures of the coronoid rarely occur in isolation. They are typically herald lesions of profound ligamentous disruption and complex elbow instability.
Historically, the management of coronoid fractures was dictated by the size of the fragment on lateral radiographs. However, modern orthopedic traumatology recognizes that even seemingly diminutive fragments can represent catastrophic capsuloligamentous avulsions, necessitating a highly nuanced, anatomically based approach to surgical reconstruction.
CLASSIFICATION SYSTEMS
The Regan and Morrey Classification
Historically, coronoid fractures were classified into three types based on the lateral radiographic appearance, as described by Regan and Morrey:
* Type I: Fracture of the intra-articular tip of the coronoid. Originally thought to impart no long-term instability, modern evidence reveals these are often capsular avulsions associated with the "terrible triad" of the elbow.
* Type II: Fracture involving half or less of the coronoid process. This significantly affects ulnohumeral stability and often requires fixation.
* Type III: Fracture involving more than half of the coronoid process. This results in profound posterior instability and loss of the anterior buttress.
The O’Driscoll Classification
More recently, the classification system developed by O’Driscoll et al. has superseded the Regan and Morrey system. Based on three-dimensional computed tomography (3D CT), this system more reliably predicts associated capsuloligamentous injuries, pathomechanics, and guides precise treatment decisions.
- Type 1 (Transverse Tip): Involves the transverse tip of the coronoid. Subtypes depend on the size of the fragment. These are classically associated with terrible triad injuries (valgus posterolateral rotatory instability).
- Type 2 (Anteromedial Facet): Involves the anteromedial facet. These occur from a varus force to the elbow. If left untreated, they result in rapid-onset posteromedial rotatory instability (PMRI) and early arthrosis.
- Type 3 (Basal): Involves the base of the coronoid, often associated with trans-olecranon fracture-dislocations.
Clinical Pearl: Because a coronoid fracture fragment may appear deceptively small on a standard lateral radiograph, or may be obscured by or confused with a radial head fracture, a CT scan with 3D reconstructions is strictly recommended whenever a coronoid fracture is suspected.
CLINICAL EVALUATION AND IMAGING
A meticulous physical examination is paramount. The elbow must be assessed for resting alignment, soft tissue envelope integrity, and neurovascular status—paying particular attention to the ulnar and anterior interosseous nerves.
Standard anteroposterior (AP) and lateral radiographs are the first line of imaging. The "double crescent sign" on a lateral radiograph is pathognomonic for an anteromedial facet fracture. However, radiographs alone are insufficient for surgical planning. 3D CT is mandatory to identify all components of the injury, delineate the fracture morphology, and template for internal fixation.
SURGICAL ALGORITHM AND APPROACHES
Displaced coronoid fractures should be anatomically reduced and stabilized with rigid fixation. Careful assessment is mandatory to ensure that the coronoid fracture is not part of a more serious, unrecognized injury pattern.
Algorithm for Management of O’Driscoll Types I and II
The surgical approach is dictated by the specific fracture pattern and associated instability:
- O’Driscoll Type I (Terrible Triad / Valgus Posterolateral Rotatory Instability):
- Approach: Single posterior universal incision or separate lateral and medial approaches.
- Sequence: Deep to superficial repair. 1. Coronoid fixation, 2. Radial head repair or replacement, 3. Lateral Collateral Ligament (LCL) repair.
- Fixation: Smaller fragments are managed with capsular repair or suture lasso techniques. Larger fragments may accept screw fixation.
- O’Driscoll Type II (Anteromedial Facet / Varus Posteromedial Rotatory Instability):
- Approach: Medial approach (over-the-top or through the FCU split) or a medial window of a posterior approach. A lateral window is required for LCL repair.
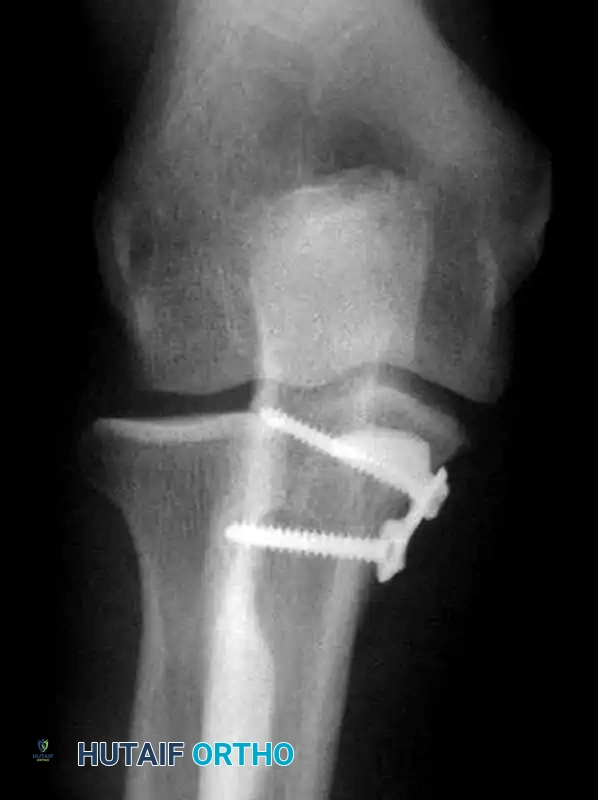
- Fixation: Anteromedial buttress plate.
Surgical Positioning
The patient is typically positioned supine with the arm draped across the chest, or in the lateral decubitus position with the arm resting over a padded post. A sterile tourniquet is applied high on the brachium. The lateral decubitus position is highly advantageous as it allows gravity to assist in reducing posterior subluxation and provides excellent access to both the medial and lateral aspects of the joint.
Fixation Techniques
- Suture Lasso Technique: Sutures can be used for the fixation of small coronoid fracture fragments (Type I tip fractures). Heavy non-absorbable sutures are passed through the anterior capsule and the fracture fragment, then shuttled through trans-osseous drill holes exiting the dorsal proximal ulna, and tied over a bone bridge.
- Lag Screws: Anterior-to-posterior or posterior-to-anterior lag screws can be used for larger fragments (Type II or III).
- Buttress Plating: Essential for anteromedial facet fractures to resist the shear forces of the distal humerus.
SPECIFIC INJURY PATTERNS
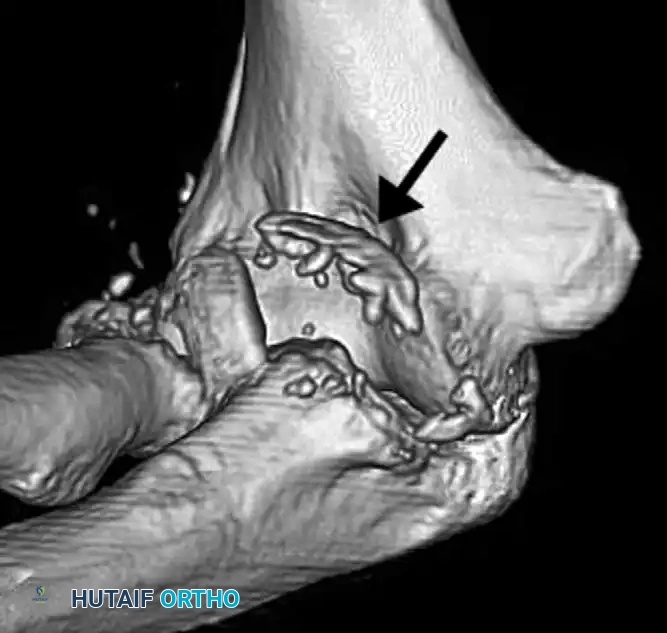
Anteromedial Facet Fractures
A distinct type of coronoid fracture, the fracture of the anteromedial facet, occurs from a varus force to the elbow combined with an axial load. This mechanism shears off the anteromedial rim of the coronoid and invariably ruptures the lateral collateral ligament (LCL) complex.
If left untreated, this injury results in posteromedial rotatory instability (PMRI). The ulna subluxates posteromedially, leading to rapid, catastrophic wear of the medial radiocapitellar joint and ulnohumeral arthrosis.
Surgical Warning: The sublime tubercle may be involved in anteromedial facet fractures. However, the AMCL often remains attached to the fractured fragment. Therefore, repairing the fracture effectively restores medial stability.
Treatment necessitates an aggressive surgical approach. Repair of the lateral collateral ligament and Open Reduction and Internal Fixation (ORIF) of the coronoid are strictly recommended. Fixation is best achieved using a contoured anteromedial buttress plate applied through a medial approach, supporting the fragment against the varus shear forces.
Simple Elbow Dislocations
Simple elbow dislocations are defined as dislocations of the ulnohumeral and radiocapitellar joints without an associated fracture. They are termed “simple” strictly due to the absence of osseous injury; however, the soft tissue disruption is extensive, typically involving complete rupture of the LCL, anterior capsule, and often the MCL.
Management of Simple Dislocations
Treatment is almost always conservative.
1. Closed Reduction: Must be performed emergently after a thorough neurovascular examination. Reduction is achieved with longitudinal traction, supination (to clear the radial head), and gentle flexion.
2. Stability Assessment: The propensity to redislocate is evaluated after reduction. The elbow is taken through a full range of motion. The "hanging arm test" can be used to assess stability in extension.
3. Immobilization: Radiographs must confirm a concentric reduction. Initially, the elbow is splinted in 90 degrees of flexion.
4. Rehabilitation: If the elbow is stable after reduction, active range-of-motion (ROM) is begun at 5 to 10 days after injury to prevent debilitating stiffness. More unstable injuries may require splinting for up to 2 or 3 weeks with a protected, hinged-brace ROM program.
Complex Fracture-Dislocations of the Elbow
Fracture-dislocations of the elbow usually result from a fall on the outstretched hand (FOOSH) with a significant shearing component to the injury. As the proximal ulnar-radial complex is driven posteriorly, fractures of the radial head, radial neck, or coronoid process—or combinations of these—occur.
In adults, valgus-directed stress combined with supination leads to the classic "terrible triad." In adolescents, valgus stress can result in avulsion of the medial epicondyle rather than a ligamentous tear. The medial collateral ligament and lateral collateral ligamentous complex are invariably torn in complete dislocations.
Surgical Rationale for Fracture-Dislocations
Posterior fracture-dislocations of the elbow in adults are almost exclusively treated surgically. The combination of fracture and ligamentous disruption renders these dislocations profoundly unstable.
Fracture of the coronoid process or radial head (or both) destroys the anterior and lateral bony buttresses, rendering the elbow significantly unstable even after closed reduction. Untreated injury to the collateral ligamentous complex (LCL and MCL) after repair of the osseous components will leave residual instability. Conversely, lengthy immobilization to treat this instability conservatively greatly increases the risk of severe, permanent joint stiffness. Therefore, open reduction and stable fixation must be performed to allow early, safe motion.
Step-by-Step Management
- Emergent Closed Reduction: Should be done as soon as possible to relieve tension on the neurovascular structures and articular cartilage.
- Advanced Imaging: Radiographs often are necessary after reduction to define the osseous injury completely. 3D CT is necessary to identify all components of the injury and template for surgery.
- Dynamic Assessment: Under fluoroscopy or clinical exam, the elbow should be carefully moved through a flexion-extension arc. Subluxation or impending dislocation at 30 degrees or more from full extension indicates critical instability, and surgical stabilization is required.
- Surgical Execution:
- Restore the anterior buttress (Coronoid ORIF).
- Restore the lateral column (Radial head ORIF or arthroplasty).
- Restore the lateral tension band (LCL repair to the lateral epicondyle using suture anchors).
- Assess the medial column. If the elbow remains unstable in extension after the first three steps, the MCL must be repaired or a hinged external fixator applied.
Pitfall: Attempting to salvage a highly comminuted radial head in a terrible triad injury often leads to early failure and recurrent instability. If the radial head cannot be rigidly fixed with less than 3 screws, primary radial head arthroplasty is the gold standard to restore the lateral column buttress.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The ultimate goal of surgical intervention in coronoid fractures and elbow dislocations is to achieve a joint stable enough to permit early active motion.
- Phase I (0-14 Days): The elbow is immobilized in a posterior splint at 90 degrees of flexion with the forearm in neutral or slight pronation (to protect the LCL repair) for 7 to 10 days. At the first postoperative visit, the splint is removed. If fixation is robust, active and active-assisted ROM is initiated. Extension is often limited to 30 degrees initially to protect the anterior capsule and coronoid fixation.
- Phase II (2-6 Weeks): A hinged elbow brace is utilized. The extension block is gradually reduced by 10 degrees per week. Patients are instructed to avoid shoulder abduction during elbow flexion/extension exercises, as this places a deleterious varus stress across the healing LCL and anteromedial facet.
- Phase III (6-12 Weeks): The brace is discontinued. Strengthening exercises are initiated. Maximum medical improvement regarding range of motion may take up to 12 to 18 months.
In the rare situation of a stable, concentric reduction managed non-operatively, the patient can be started on early active exercises at 2 to 3 weeks, with extremely close radiographic follow-up. If subluxation or spontaneous redislocation occurs at any point, the elbow must be surgically stabilized without delay.
📚 Medical References
- coronoid fractures: surgical technique, J Bone Joint Surg 87A(suppl 1 pt 1):22, 2005.
- McKee MD, Wilson TL, Winston L, et al: Functional outcome following surgical treatment of intraarticular distal humeral fractures through a posterior approach, J Bone Joint Surg 82A:1701, 2000.
- McLaren AC: Prophylaxis with indomethacin for heterotopic bone after open reduction of fractures of the acetabulum, J Bone Joint Surg 72A:245, 1990.
- Mehne DK, Matta J: Bicolumn fractures of the adult humerus. Paper presented at the 53rd Annual Meeting of the American Academy of Orthopaedic Surgeons, New Orleans, 1986.
- Miller GK, Drennan DB, Maylahn DJ: Treatment of displaced segmental radial-head fractures: long-term follow-up, J Bone Joint Surg 63A:712, 1981.
- Moed BR, Ede DE, Brown TD: Fractures of the olecranon: an in vitro study of elbow joint stresses after tension-band wire fi xation versus proximal fracture fragment excision, J Trauma 53:1088, 2002.
- Morrey BF: General deep approaches to the elbow: posterior approaches, Tech Shoulder Elbow Surg 3:6, 2002.
- Morrey BF, Chao EY, Hui FC: Biomechanical study of the elbow following excision of the radial head, J Bone Joint Surg 61A:63, 1979.
- Murphy DF, Greene WB, Dameron TB Jr: Displaced olecranon fractures in adults: clinical evaluation, Clin Orthop Relat Res 224:215, 1987.
- Neer CS II: Articular replacement for the humeral head, J Bone Joint Surg 25A:1607, 1964.
- Netz P, Strömberg L: Non-sliding pins in traction absorbing wiring of fractures: a modifi ed technique, Acta Orthop Scand 53:355, 1982.
- Newell RLM: Olecranon fractures in children, Injury 7:33, 1975.
- O’Driscoll SW: The triceps-refl ecting anconeus pedicle (TRAP) approach for distal humeral fractures and nonunions, Orthop Clin North Am 31:91, 2000.
- O’Driscoll SW, Jupiter JB, Cohen MS, et al: Diffi cult elbow fractures: pearls and pitfalls, Instr Course Lect 52:113, 2003.
- Pollock FH, Drake D, Bovill EG, et al: Treatment of radial neuropathy associated with fractures of the humerus, J Bone Joint Surg 63A:239, 1981.
- Post M: Fractures of the upper humerus, Orthop Clin North Am 11:239, 1980.
- Pugh DMW, Wild LM, Schemitsch EH, et al: Standard surgical protocol to treat elbow dislocations with radial head and coronoid fractures, J Bone Joint Surg 86A:1122, 2004.
- Regan W, Morrey B: Fractures of the coronoid process of the ulna, J Bone Joint Surg 71A:1348, 1989.
- Ring D, Gulotta L, Chin K, et al: Olecranon osteotomy for exposure of fractures and nonunions of the distal humerus, J Orthop Trauma 18:446, 2004.
- Ring D, Jupiter JB: Fractures of the distal humerus, Orthop Clin North Am 31:103, 2000.
- Ring D, Jupiter JB, Gulotta L: Articular fractures of the distal part of the humerus, J Bone Joint Surg 85A:232, 2003.
- Ring D, Jupiter JB, Zilberfarb J: Posterior dislocation of the elbow with fractures of the radial head and coronoid, J Bone Joint Surg 84A:547, 2002.
- Ring D, Quintero J, Jupiter JB: Open reduction and internal fi xation of fractures of the radial head, J Bone Joint Surg 84A:1811, 2002.
- Riseborough EJ, Radin EL: Intercondylar T fractures of the humerus in the adult: a comparison of operative and nonoperative treatment in twenty-nine cases, J Bone Joint Surg 51A:130, 1969.
- Ritter MA, Gioe TJ: The effect of indomethacin on para-articular ectopic ossifi cation following
