Introduction and Epidemiology
Charcot neuroarthropathy of the foot and ankle represents a severe and debilitating complication of peripheral neuropathy, most commonly associated with diabetes mellitus. This progressive, destructive process of bones and joints results from repetitive microtrauma to an insensate foot, leading to a cascade of inflammation, bone resorption, fragmentation, subluxation, dislocation, and eventually gross deformity. The term rocker bottom foot classically describes a severe midfoot collapse characterized by plantar convexity, often with a prominent talar head, cuboid, or navicular, predisposing to chronic ulceration, osteomyelitis, and ultimately amputation if not managed effectively.
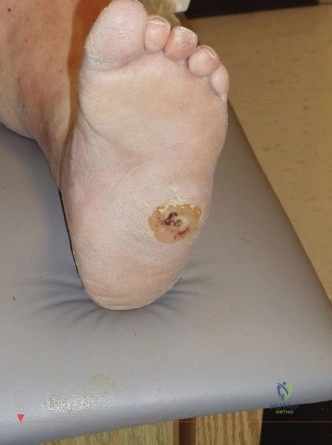
The primary diagnostic challenge in Charcot neuroarthropathy lies in differentiating an acute exacerbation from active infection, particularly osteomyelitis. Both conditions present with warmth, erythema, and edema, making clinical distinction difficult. Misdiagnosis can lead to inappropriate treatment, exacerbating morbidity. The incidence of Charcot neuroarthropathy is estimated to be between 0.1% and 7.5% in diabetic patients, with a higher prevalence in those with long-standing neuropathy, retinopathy, and nephropathy. Once a deformity such as the rocker bottom develops, the risk of plantar ulceration and subsequent infection rises dramatically, with amputation rates reaching 12-50% in infected Charcot feet.
Pathophysiology of Charcot Neuroarthropathy
Two primary theories have historically described the pathogenesis of Charcot neuroarthropathy, though contemporary understanding views them as synergistic. The neurotraumatic theory posits that a loss of protective sensation allows repetitive, unrecognized microtrauma to accumulate, leading to ligamentous laxity, joint subluxation, and periarticular fractures. The neurovascular theory suggests that an autonomic neuropathy leads to a hyperemic state via loss of sympathetic tone, resulting in increased osteoclastic activity and subsequent osteopenia, rendering the bone susceptible to mechanical failure.
Modern molecular biology has further elucidated the inflammatory cascade driving this process. The Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL) and Osteoprotegerin (OPG) pathway plays a central role. Pro-inflammatory cytokines, particularly Interleukin-1 (IL-1) and Tumor Necrosis Factor-alpha (TNF-alpha), upregulate RANKL expression in the setting of acute trauma. In the diabetic, neuropathic patient, this response is exaggerated and uncoupled from normal bone formation, leading to aggressive, unchecked osteoclastic bone resorption.
Clinical Presentation and Diagnostic Challenges
The natural history of the disease is classically described by the Eichenholtz classification. Stage 0 (prodromal) presents with unilateral erythema, edema, and warmth, with normal radiographs. Stage I (developmental/fragmentation) is characterized by active bone destruction, periarticular debris, and subluxation. Stage II (coalescence) involves the absorption of fine debris and early fusion of large fragments. Stage III (remodeling) is defined by the consolidation of the deformity, decreased sclerosis, and a fixed, often non-plantigrade foot.
Distinguishing Stage 0 or Stage I Charcot from osteomyelitis requires a high index of suspicion. The elevation test can be a useful clinical adjunct; elevating the affected limb for 5 to 10 minutes will typically result in the resolution of erythema in acute Charcot, whereas erythema secondary to infection will persist. Advanced imaging, particularly magnetic resonance imaging (MRI), is the gold standard for differentiating the two, with Charcot demonstrating primary joint-based marrow edema and osteomyelitis showing contiguous bone marrow edema adjacent to a soft tissue ulceration or sinus tract.
Surgical Anatomy and Biomechanics
The anatomical substrate of Charcot neuroarthropathy primarily involves the tarsal and metatarsal bones, ligaments, and joints, reflecting the areas subjected to peak plantar pressures during ambulation. Understanding the architectural collapse requires a detailed appreciation of the columnar organization of the foot and the deforming forces acting upon it.
Columnar Anatomy of the Foot
The foot can be functionally divided into three main columns, each playing a distinct biomechanical role:
* Medial Column: Comprising the talus, navicular, three cuneiforms, and the first three metatarsals. This column provides the primary arch support and is the rigid lever required for the push-off phase of gait.
* Lateral Column: Comprising the calcaneus, cuboid, and the fourth and fifth metatarsals. This column provides stability and flexibility, allowing the foot to adapt to uneven terrain.
* Posterior Column: Comprising the calcaneus and talus, forming the hindfoot complex which dictates the position of the transverse tarsal joint.
In Charcot neuroarthropathy, the midfoot (Lisfranc and Chopart joints) is most frequently affected, accounting for approximately 45% of cases. Hindfoot involvement accounts for roughly 30%, and ankle involvement for 10%. The Brodsky classification categorizes these anatomical patterns: Type 1 involves the midtarsal and tarsometatarsal joints; Type 2 involves the subtalar, talonavicular, or calcaneocuboid joints; Type 3A involves the tibiotalar joint; Type 3B involves the calcaneal tuberosity; and Type 4 involves a combination of areas.
Pathomechanics of the Rocker Bottom Deformity
The pathognomonic rocker bottom deformity results from the catastrophic failure of the medial longitudinal arch, typically at the naviculocuneiform and cuneiform-metatarsal joints. This collapse is heavily driven by biomechanical imbalances, most notably an equinus contracture. Tightness in the gastrocnemius-soleus complex creates a significant plantarflexion force on the calcaneus. During the stance phase of gait, as the tibia advances over the foot, the inability of the ankle to dorsiflex transfers immense bending moments to the midfoot.
In the setting of neuropathic osteopenia and ligamentous failure, the midfoot cannot withstand these forces. The resulting collapse leads to:
* Plantar migration and protrusion of the talar head, navicular, or cuboid: Creating the convex plantar surface that defines the rocker bottom.
* Dorsal displacement of the metatarsals: Leading to relative dorsal impingement and shortening of the foot.
* Abduction of the forefoot: Resulting in a transverse plane deformity often described as a boat-shaped foot.
The biomechanical consequence is an abnormal redistribution of plantar pressures, particularly over the apex of the bony prominence. This focal high-pressure area, combined with an insensate foot, inevitably leads to skin breakdown, chronic ulceration, and a direct portal for bacterial invasion.
Indications and Contraindications
Surgical management of Charcot neuroarthropathy is primarily aimed at achieving a stable, plantigrade foot that can be braced effectively and remains free of recurrent ulceration or infection. The decision to operate is complex and must balance the severe risks of surgery in a compromised host against the natural history of progressive deformity and amputation.
Operative Indications
Operative intervention is typically reserved for patients who have failed conservative management or present with deformities that preclude functional bracing. The presence of a severe rocker bottom deformity, especially with active ulceration or impending skin breakdown, often necessitates surgical reconstruction. Surgery is generally performed during Eichenholtz Stage II or III (coalescence or consolidation) when the inflammatory process has subsided, though there is a growing consensus for early intervention in highly unstable Stage I joints to prevent severe soft tissue compromise.
Specific indications include:
* Severe malalignment preventing the use of a Total Contact Cast (TCC) or Charcot Restraint Orthotic Walker (CROW).
* Recurrent plantar ulceration recalcitrant to aggressive offloading and wound care.
* Gross instability of the midfoot or hindfoot leading to progressive deformity.
* Chronic osteomyelitis associated with a bony prominence, requiring simultaneous resection and stabilization.
* Acute, irreducible dislocations or displaced intra-articular fractures (e.g., severe ankle Charcot) where conservative management guarantees a non-functional limb.
Contraindications to Surgery
Contraindications are largely centered around the patient's physiological ability to heal bone and soft tissue, as well as their capacity to adhere to a strict, prolonged postoperative rehabilitation protocol.
- Inadequate Vascular Inflow: Severe Peripheral Arterial Disease (PAD) without the possibility of revascularization is an absolute contraindication. A toe pressure less than 40 mmHg or an Ankle-Brachial Index (ABI) less than 0.5 indicates a high risk of incisional necrosis and amputation.
- Active Eichenholtz Stage I: Operating during the acute, hyperemic fragmentation phase is generally contraindicated due to poor bone stock, high risk of hardware failure, and exacerbation of the inflammatory cascade, unless the deformity is acutely unstable and limb-threatening.
- Severe Medical Comorbidities: Poorly controlled diabetes (HbA1c > 8.5%), end-stage renal disease on hemodialysis, or severe malnutrition significantly increase the risk of perioperative mortality and catastrophic surgical failure.
- Non-compliance: Inability to maintain strict non-weight-bearing status postoperatively.
Summary of Operative vs Non Operative Indications
| Clinical Scenario | Recommended Management | Rationale / Key Considerations |
|---|---|---|
| Acute Eichenholtz Stage 0/I (Stable) | Non-Operative | Strict immobilization (TCC). Bone is hyperemic and osteopenic; hardware failure is highly likely. |
| Acute Eichenholtz Stage I (Highly Unstable) | Controversial / Operative | External fixation may be required to prevent catastrophic soft tissue compromise or impending ulceration. |
| Eichenholtz Stage II/III (Stable, Braceable) | Non-Operative | Custom orthotics (CROW boot) or accommodative footwear. Surgery poses unnecessary risk if the foot is ulcer-free. |
| Eichenholtz Stage II/III (Unstable, Unbraceable) | Operative | Arthrodesis and deformity correction required to restore a plantigrade foot and prevent ulceration. |
| Chronic Ulceration over Bony Prominence | Operative | Exostectomy (shaving the prominence) with or without corrective arthrodesis to offload the focal pressure point. |
| Concomitant Osteomyelitis | Operative | Surgical debridement, bone biopsy, and stabilization (often via external fixation) are required to eradicate infection. |
| Severe Peripheral Arterial Disease | Non-Operative | Absolute contraindication to major reconstruction until successful endovascular or open revascularization is performed. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of successful Charcot reconstruction. The surgeon must evaluate the vascular, neurological, and osseous status of the limb, while simultaneously optimizing the patient's systemic health.
Clinical and Radiographic Evaluation
Vascular assessment is paramount. Palpable pulses do not rule out microvascular disease. Non-invasive vascular studies, including Ankle-Brachial Indices (ABIs) and Toe-Brachial Indices (TBIs), should be obtained. In diabetic patients with calcified vessels, ABIs may be falsely elevated; therefore, transcutaneous oxygen measurements (TcPO2) or arterial duplex ultrasonography are often required. A TcPO2 greater than 40 mmHg is generally predictive of successful wound healing.
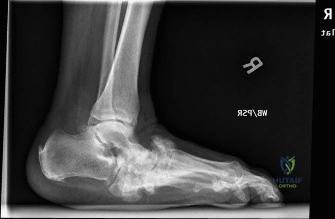
Radiographic evaluation begins with standard weight-bearing anteroposterior, lateral, and oblique views of the foot and ankle. Key radiographic parameters include Meary's angle (the talus-first metatarsal angle), the calcaneal pitch, and the talocalcaneal angle. In a rocker bottom deformity, Meary's line is typically broken with apex plantar angulation, and the calcaneal pitch is significantly decreased or negative.
Computed Tomography (CT) is essential for evaluating bone stock, identifying areas of fragmentation, and planning osteotomies. Three-dimensional reconstructions aid in visualizing the complex multiplanar deformities. If osteomyelitis is suspected, MRI with and without intravenous contrast is indicated to evaluate the extent of marrow involvement and to identify occult soft tissue abscesses.
Patient Positioning and Preparation
Patients are typically positioned supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a neutral position and allowing access to both the medial and lateral columns. A thigh tourniquet is applied but should be used judiciously. In patients with severe calcific atherosclerosis, tourniquet inflation may cause plaque rupture or acute limb ischemia; in such cases, the procedure is performed without a tourniquet, utilizing meticulous hemostasis.
Preoperative templating is critical. The surgeon must determine the apex of the deformity, calculate the size of the necessary wedge osteotomies, and select the appropriate fixation constructs. Given the compromised bone quality, standard AO principles of fixation are often insufficient, necessitating the use of specialized techniques.
Detailed Surgical Approach and Technique
The surgical reconstruction of a rocker bottom Charcot foot is a formidable undertaking that requires a systematic approach. The goals are to resect infected or prominent bone, correct the deformity to a plantigrade position, and achieve rigid internal or external fixation that can withstand the forces of early rehabilitation.
Soft Tissue Balancing and Equinus Correction
Deformity correction must begin with soft tissue balancing, primarily addressing the Achilles tendon. An equinus contracture is universally present and acts as a major deforming force. Attempting to correct a midfoot collapse without lengthening the Achilles tendon will result in excessive tension on the midfoot reconstruction and inevitable hardware failure.
A percutaneous Tendo-Achilles Lengthening (TAL) or an open gastrocnemius recession (Strayer or Baumann procedure) is performed. The choice depends on the severity of the contracture and whether the tightness is isolated to the gastrocnemius (positive Silfverskiöld test) or involves the entire triceps surae complex. Adequate lengthening is achieved when the ankle can be passively dorsiflexed to at least 10 degrees beyond neutral with the knee fully extended.
Osseous Resection and Deformity Correction
The surgical approach is dictated by the location of the deformity and the planned fixation. A dual incision technique is frequently utilized. A medial utility incision is made extending from the medial malleolus to the first metatarsophalangeal joint, exposing the talonavicular, naviculocuneiform, and first tarsometatarsal joints. A lateral incision over the calcaneocuboid joint and base of the fourth and fifth metatarsals allows access to the lateral column. Care must be taken to maintain an adequate skin bridge (at least 5 to 7 centimeters) between incisions to prevent angiosome necrosis.
Once the joints are exposed, all fibrotic tissue, cartilage, and sclerotic bone must be aggressively debrided down to bleeding, healthy cancellous bone. In the setting of a rigid rocker bottom deformity, a biplanar closing wedge osteotomy is often required. The apex of the wedge is typically located dorsally, allowing for the correction of the plantar sag and the restoration of the medial longitudinal arch. The osteotomy is provisionally stabilized with heavy Kirschner wires or Steinmann pins, and intraoperative fluoroscopy is used to confirm the restoration of Meary's line and a neutral calcaneal pitch.
Superconstruct Fixation Principles
Standard osteosynthesis techniques frequently fail in Charcot neuroarthropathy due to the profound osteopenia and impaired healing capacity. Consequently, the concept of "superconstructs," pioneered by Sammarco, has become the standard of care. Superconstructs are defined by four primary principles:
1. Fusion must extend beyond the zone of injury to include normal, healthy bone.
2. Bone resection must be adequate to allow for deformity correction without placing undue tension on the soft tissue envelope.
3. The strongest fixation devices possible must be utilized.
4. Hardware should be applied in a position that maximizes its biomechanical advantage.
Intramedullary Beaming:
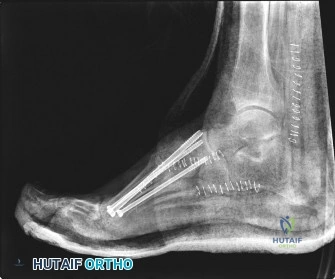
A highly effective technique for medial and lateral column stabilization is intramedullary beaming. Large-diameter (typically 5.0 mm to 7.0 mm), solid, fully threaded or partially threaded screws are introduced percutaneously or through small incisions. For the medial column, a screw is driven from the head of the first metatarsal, across the tarsometatarsal and naviculocuneiform joints, and into the body of the talus. A parallel beam can be placed down the lateral column from the fourth or fifth metatarsal into the calcaneus. These beams act as internal splints, distributing forces across the entire length of the foot rather than concentrating stress at a single arthrodesis site.
Plating Techniques:
Plating is often used in conjunction with beaming or as a standalone technique. Plantar plating provides the greatest biomechanical advantage by acting as a tension band against the dorsiflexion forces that cause midfoot collapse. However, the plantar approach carries a higher risk of soft tissue complications. Medial column locking plates, specifically designed for Charcot reconstruction, are frequently utilized. These plates are thick, robust, and allow for the insertion of multiple locking screws into the talus, navicular, cuneiforms, and metatarsals, providing rigid angular stability.
Circular External Fixation:
In cases of active infection, severe soft tissue compromise, or profound bone loss where internal fixation is contraindicated, circular external fixation (Ilizarov methodology) is the treatment of choice. Fine wire tensioned frames allow for rigid stabilization, gradual deformity correction, and simultaneous management of soft tissue defects. The frame transfers weight-bearing forces directly from the tibia to the ground, completely offloading the compromised foot.
Complications and Management
The surgical management of Charcot neuroarthropathy is fraught with complications. The combination of neuropathy, compromised vascularity, poor bone quality, and an immunocompromised state makes these procedures some of the most high-risk in orthopedic surgery. Surgeons must maintain a high index of suspicion for early signs of failure and intervene promptly.
Hardware Failure and Nonunion
Hardware failure is the most common mechanical complication. Due to the osteopenic nature of Charcot bone, screw pullout, plate fracture, and beam migration are frequent occurrences. Nonunion or delayed union is also highly prevalent, given the impaired local biology.
Management depends on the clinical presentation. Asymptomatic nonunions with stable hardware and a plantigrade, braceable foot can often be observed. However, if hardware failure leads to recurrent deformity, instability, or impending skin breakdown, revision surgery is mandatory. Revision strategies typically involve the removal of broken hardware, re-debridement of the nonunion site, utilization of orthobiologics (e.g., autologous bone graft, bone morphogenetic proteins), and the application of more robust fixation, often transitioning from internal to external fixation.
Infection and Soft Tissue Compromise
Deep surgical site infections and wound dehiscence are catastrophic complications that can rapidly lead to limb loss. The insensate nature of the foot means that patients may not present with classic symptoms of pain, making regular, meticulous postoperative examinations critical.
Superficial wound dehiscence can often be managed with local wound care and Negative Pressure Wound Therapy (NPWT). Deep infections involving hardware or bone require immediate surgical debridement, hardware removal (if loose or non-essential for stability), and targeted intravenous antibiotic therapy based on deep tissue cultures. In cases of recalcitrant osteomyelitis or ascending infection, a major lower extremity amputation (typically below-knee or through-knee) becomes a life-saving necessity.
Table of Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Salvage Strategy / Management |
|---|---|---|
| Superficial Wound Dehiscence | 15% - 25% | Local wound care, NPWT, prolonged immobilization. Avoid early suture removal. |
| Deep Surgical Site Infection | 5% - 15% | Urgent operative I&D, deep cultures, hardware removal if unstable, IV antibiotics, potential application of external fixator. |
| Hardware Failure (Screw Pullout/Breakage) | 20% - 30% | If stable/plantigrade: Observation and bracing. If unstable/deforming: Revision surgery with larger implants or external fixation. |
| Aseptic Nonunion | 10% - 25% | Prolonged NWB. If symptomatic or unstable: Revision arthrodesis with autograft/allograft and orthobiologics (BMP-2). |
| Recurrent Ulceration | 10% - 20% | Aggressive offloading (CROW). Surgical evaluation for new bony prominences requiring exostectomy or revision osteotomy. |
| Amputation (Failure of Salvage) | 5% - 15% | Below-Knee Amputation (BKA) or Syme amputation depending on soft tissue viability and vascular inflow. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation phase is arguably as critical as the surgical execution. The biological healing time for neuropathic bone is significantly prolonged compared to normal bone, often taking two to three times longer to achieve radiographic consolidation.
Immediate Post Operative Phase
Immediately following surgery, the limb is placed in a well-padded, bulky Jones splint to accommodate postoperative edema. Strict non-weight-bearing (NWB) status is enforced. The patient is typically transitioned to a fiberglass Total Contact Cast (TCC) or a rigid bivalved cast at two to three weeks postoperatively, once the incisions have healed and the sutures are removed.
The duration of NWB is highly variable but typically ranges from 12 to 16 weeks, and in complex reconstructions, may extend up to 6 months. Serial radiographs are obtained every 4 to 6 weeks to monitor for hardware position, maintenance of alignment, and signs of osseous bridging.
Transition to Weight Bearing
The transition to weight-bearing is a gradual, phased process. Once clinical and radiographic evidence of consolidation is confirmed, the patient is transitioned from a NWB cast to a weight-bearing cast or a Charcot Restraint Orthotic Walker (CROW) boot. The CROW boot is a custom-molded, rigid orthosis that provides total contact and offloads the plantar surface while stabilizing the ankle and hindfoot.
Patients typically remain in the CROW boot for an additional 3 to 6 months. Long-term, lifelong bracing is often required. Even after successful arthrodesis, the foot remains insensate and at risk for recurrent breakdown or the development of adjacent joint disease. Transition to custom-molded, extra-depth diabetic footwear with rigid rocker soles is the ultimate goal, coupled with rigorous, routine podiatric or orthopedic surveillance.
Summary of Key Literature and Guidelines
The evolution of Charcot neuroarthropathy management has been shaped by several pivotal studies and consensus guidelines. Familiarity with this literature is essential for the academic orthopedic surgeon.
- Eichenholtz (1966): Established the foundational staging system (Development, Coalescence, Reconstruction) based on clinical and radiographic progression, which remains the standard language for describing the natural history of the disease.
- Brodsky and Rouse (1993): Defined the anatomical classification of Charcot joints, highlighting the midfoot (Type 1) as the most common site of involvement and guiding anatomically specific surgical approaches.
- Sammarco et al. (2009): Introduced and validated the concept of "superconstructs" for midfoot reconstruction. Their work demonstrated that extending fusions beyond the zone of injury and utilizing robust fixation significantly reduced the rates of mechanical failure in osteopenic bone.
- Pinzur (2004, 2012): A pioneer in the use of circular external fixation for complex Charcot deformities, particularly in the setting of active osteomyelitis or severe soft tissue compromise. His outcome studies validated the Ilizarov method as a reliable limb salvage tool when internal fixation is contraindicated.
- Frykberg et al. (Diabetic Foot Disorders Guidelines): Provides comprehensive, multidisciplinary consensus guidelines emphasizing the critical importance of early diagnosis, aggressive offloading in the acute phase, and the optimization of glycemic and vascular status prior to any surgical intervention. These guidelines reinforce that surgery is a salvage procedure, not a primary treatment for acute, uncomplicated Charcot neuroarthropathy.
