Management of Extravasation Injuries and Psychogenic Hand Deformities
Key Takeaway
Extravasation injuries in the upper extremity represent an iatrogenic emergency capable of causing profound tissue necrosis. Management is dictated by the extravasated volume and agent toxicity, with vesicants requiring emergent surgical washout. Concurrently, orthopedic surgeons must recognize complex non-structural pathologies, such as psychogenic hand deformities, to avoid unnecessary surgical interventions. This guide details the operative protocols for extravasation, ballistic soft-tissue trauma, and the clinical differentiation of psychogenic postures.
INTRODUCTION TO COMPLEX SOFT TISSUE AND NON-STRUCTURAL HAND DISORDERS
The practice of operative orthopedics and hand surgery frequently intersects with complex, non-traumatic, and iatrogenic pathologies. Among the most critical of these are extravasation injuries, which represent a true surgical emergency capable of causing irreversible deep tissue necrosis, neurovascular compromise, and severe upper extremity morbidity.
In addition to iatrogenic soft-tissue emergencies, the hand surgeon must be adept at managing penetrating soft-tissue trauma (such as ballistic injuries) and identifying non-structural, psychiatric-driven presentations, notably psychogenic hand deformities. Misdiagnosis of the latter can lead to unnecessary, morbid surgical interventions. This comprehensive guide delineates the pathophysiology, clinical evaluation, and evidence-based surgical management of these diverse but critical upper extremity conditions.
EXTRAVASATION INJURIES
Extravasation is defined as the inadvertent leakage of intravenously administered medications or fluids into the surrounding perivascular soft tissues. With a reported incidence ranging from 0.5% to 6% in clinical settings, extravasation of chemotherapeutic agents and radiographic contrast materials remains a leading cause of iatrogenic tissue injury.
Pathophysiology and Agent Classification
The severity of an extravasation injury is highly variable and is primarily dictated by the pharmacological properties of the offending agent. Substances are broadly categorized into two distinct groups:
- Vesicants: These are highly toxic agents capable of causing full-thickness tissue death, blistering, severe pain, and progressive necrosis. Vesicants often bind to cellular DNA (e.g., doxorubicin), leading to a vicious cycle of cell death, release of the toxic agent into adjacent tissues, and further necrosis. Common vesicants include doxorubicin, bleomycin, nitrogen mustards, bacille Calmette-Guérin (BCG), and 5-fluorouracil (5-FU).
- Irritants: These agents cause localized pain, aching, and tightness at the injection site, typically without a severe inflammatory component or progression to full-thickness necrosis.
The pathophysiological mechanisms of injury secondary to extravasation are multifactorial:
1. Ischemic Necrosis: Direct microvascular thrombosis and endothelial damage.
2. Cellular Toxicity: Direct chemical destruction of cellular membranes and DNA.
3. Mechanical Compression: Large volume extravasation (e.g., contrast media) leading to localized compartment syndrome.
4. Osmotic Damage: Hyperosmolar solutions drawing fluid into the interstitial space, exacerbating swelling and ischemia.
5. Bacterial Proliferation: Secondary infection occurring beneath a necrotic eschar.
Clinical Pearl: Doxorubicin (an anthracycline) is particularly notorious for causing indolent, progressive necrosis. Because it intercalates into DNA, it is not metabolized rapidly and is continuously released from dying cells to destroy adjacent healthy cells, necessitating aggressive surgical excision if conservative measures fail.
Etiology and Risk Factors
Extravasation is rarely a random event; it is typically the result of mechanical or anatomical failures during intravenous administration. Linder et al. identified several critical factors that precipitate extravasation injuries:
* Infusion under high mechanical pressure (e.g., power injectors for contrast media).
* Failure to release a proximal tourniquet prior to infusion.
* Utilization of fragile, inadequate, or sclerotic veins.
* Thrombosis of proximal venous structures.
* Venospasm at previous venipuncture sites.
* Active thrombophlebitis.
* Veins with multiple puncture holes proximal to the infusion site, allowing retrograde leakage.
Clinical Evaluation and Volumetric Assessment
Most authorities agree that immediate recognition and treatment are paramount. However, there is no universal consensus on pharmacological antidotes, making surgical and mechanical management the cornerstone of treatment for significant extravasations.
Management algorithms are heavily dictated by the volume of the extravasated solution. Plain radiographs are highly efficacious for estimating the volume and anatomical extent of extravasation when radiopaque contrast materials are involved.
Volume-Based Treatment Algorithm
- Insignificant Extravasations (< 5 mL):
- Management: Conservative.
- Protocol: Immediate cessation of the infusion, elevation of the affected extremity strictly above heart level, and application of warm or cold compressive dressings (temperature depends on the specific agent; e.g., cold for doxorubicin to localize the toxin, warm for vinca alkaloids to promote vasodilation and absorption).
- Moderate Extravasations (5 to 20 mL):
- Management: Dictated by clinical presentation.
- Protocol: If the patient exhibits severe soft tissue reaction, intractable pain, or progressive swelling, emergency surgical intervention is indicated. If symptoms are mild, conservative management with hyper-vigilant serial examinations may be employed.
- Significant Extravasations (> 20 mL):
- Management: Emergency surgical drainage and wound lavage.
- Protocol: Surgery must be performed preferably within 6 hours of the extravasation event to prevent irreversible osmotic and compressive damage.
Surgical Technique: Drainage and Lavage (The Gault Technique)
When surgical intervention is indicated, the goal is to mechanically flush the toxic or hyperosmolar agent from the interstitial space before cellular uptake or irreversible ischemia occurs.
- Positioning and Anesthesia: The patient is positioned supine with the arm extended on a hand table. Regional anesthesia (axillary or supraclavicular block) or general anesthesia is utilized. A tourniquet is applied but not inflated initially, to allow assessment of tissue perfusion.
- Incision: Multiple small (3-5 mm) stab incisions are made at the periphery of the extravasation zone, guided by the area of erythema, induration, or radiographic contrast spread.
- Blunt Dissection: A blunt-tipped cannula or a small hemostat is introduced through the incisions to gently break up loculations within the subcutaneous tissue.
- Lavage: Copious irrigation (typically 500 to 1,500 mL of normal saline) is flushed through the cannula. The fluid is allowed to egress freely through the adjacent stab incisions.
- Intraoperative Imaging: If contrast media was extravasated, intraoperative fluoroscopy is utilized to confirm the complete mechanical removal of the radiopaque solution.
- Wound Management: The stab incisions are left open to allow for continued drainage. If frank tissue necrosis is already present during the index procedure, radical debridement is performed.
- Delayed Closure: Definitive wound closure or soft tissue coverage (e.g., split-thickness skin grafting or local flap transfer) is delayed for 3 to 5 days until the zone of necrosis has fully demarcated.
Surgical Warning: Never attempt primary closure over an area of known vesicant extravasation. The risk of ongoing microscopic necrosis and secondary infection beneath the closure is exceptionally high.
BALLISTIC AND PENETRATING SOFT TISSUE TRAUMA
While iatrogenic injuries like extravasation cause chemical necrosis, penetrating trauma causes direct kinetic and mechanical tissue destruction. Hand surgeons frequently encounter ballistic injuries, which require meticulous soft-tissue management to preserve hand function.
Mechanism and Evaluation of Gunshot Wounds to the Hand
The severity of a ballistic injury is determined by the kinetic energy of the projectile ($KE = \frac{1}{2}mv^2$). Civilian handgun injuries are typically low-velocity (< 1,000 ft/sec) and cause damage primarily through the direct crush and laceration of tissue in the projectile's path.
Close-range ballistic injuries present with distinct cutaneous signs due to the deposition of unburned propellant and hot gases.
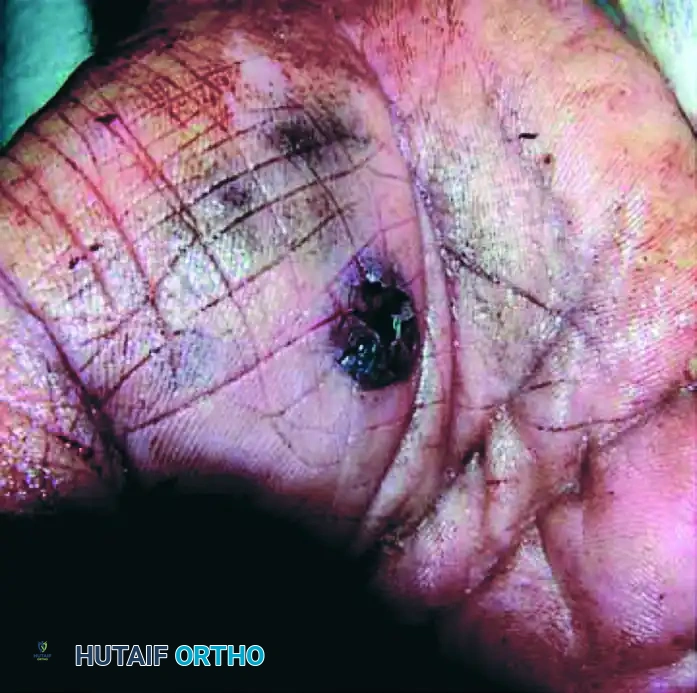
FIGURE 70-13 (A): Close-range gunshot injury demonstrating the entry wound on the palmar aspect of the hand. Note the extensive tattooing from gunpowder embedded in the dermis, indicative of a muzzle-to-target distance of less than 2 feet.
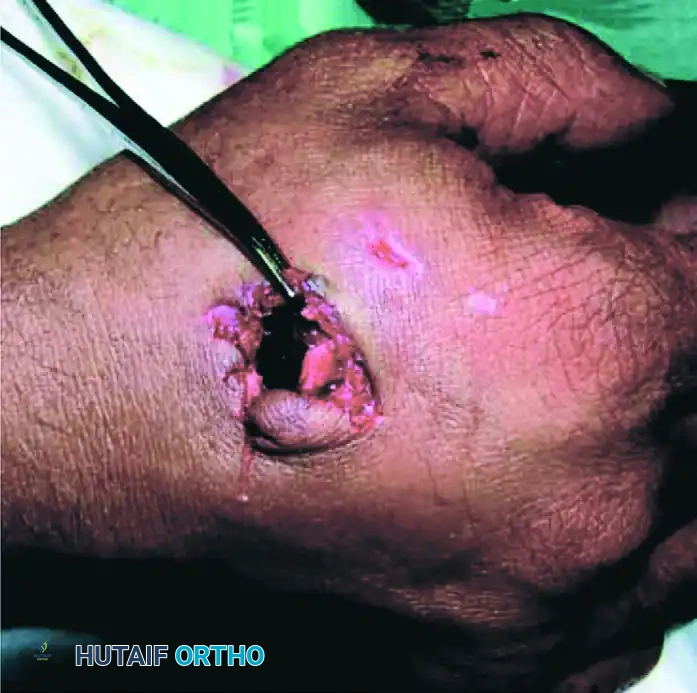
FIGURE 70-13 (B): The corresponding exit wound on the dorsal aspect of the hand. Exit wounds are typically larger, more irregular, and exhibit outward beveling of the soft tissues compared to the punched-out appearance of entry wounds.
Surgical Management of Ballistic Hand Trauma
- Initial Debridement: Low-velocity injuries without structural (bone/tendon/nerve) compromise may occasionally be managed with local wound care. However, close-range injuries with significant contamination (gunpowder tattooing, clothing debris) require formal surgical debridement.
- Irrigation: Low-pressure, high-volume pulsatile lavage is used to remove foreign debris and reduce the bacterial load.
- Tattooing Management: Gunpowder tattooing (as seen in Fig 70-13 A) must be aggressively scrubbed or sharply debrided within the first 24 hours; otherwise, the carbon particles become permanently encapsulated by macrophages, resulting in a permanent traumatic tattoo.
- Closure: Similar to extravasation necrosis, ballistic wounds are left open for delayed primary closure or secondary intention healing to prevent deep space infections.
PSYCHOGENIC HAND DEFORMITIES
Moving from structural and chemical trauma, the orthopedic surgeon must also be highly vigilant in diagnosing non-organic, psychiatric-driven pathologies. Psychogenic hand deformities are rare but highly morbid conditions where patients present with fixed, abnormal postures of the hand without an underlying neurological, musculoskeletal, or rheumatological etiology.
If misdiagnosed, these patients may undergo unnecessary surgical releases, which inevitably fail and often exacerbate the psychiatric condition. There is no predilection for the minor or dominant hand.
The Psychoflexed Hand (Clenched Fist Syndrome)
The most common presentation is the psychoflexed hand, often referred to clinically as "clenched fist syndrome."
- Clinical Presentation: The entire fist is tightly clenched, but the ulnar three digits (middle, ring, and small fingers) are predominantly involved. The fingers are held in rigid flexion at the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and distal interphalangeal (DIP) joints.
- Complications of Posturing: If left uncorrected, the posture interferes severely with the hygiene of the hand. Maceration of the palmar skin occurs, causing an offensive odor. Furthermore, secondary infections and deep palmar ulcerations can occur from the chronic, unrelenting pressure of the fingernails driving into the palmar crease.
- Long-Term Sequelae: While the initial deformity is purely psychiatric, chronic posturing will eventually lead to true structural pathology. The volar plates, collateral ligaments, and flexor tendons will contract, rendering the deformity permanently uncorrectable even if the underlying psychiatric condition resolves.
The Psychoextended Hand
The second, less common posture is the psychoextended hand.
- Clinical Presentation: This posture is characterized by the ulnar three digits being held in rigid hyperextension at the PIP joints and in flexion at the MCP joints.
- Functional Preservation: Interestingly, this posture often permits a partially functioning hand. A pinch mechanism is usually preserved between the thumb and the index finger. The index finger MCP joint is held in flexion, but active flexion and extension are preserved at the PIP joint, permitting opposition to the thumb pulp.
- Paradoxical Movement: Sometimes these patients permit passive extension at the MCP joint, but any attempt by the examiner to passively flex the PIP joints is met with rigid, active resistance from the patient's extensor mechanism.
Differential Diagnosis and Clinical Evaluation
An experienced surgeon can usually distinguish psychogenic conditions easily, but it requires a meticulous clinical examination to rule out organic disease. The psychoflexed and psychoextended hands must be carefully differentiated from:
- Dupuytren Contracture: Look for palpable, painless cords and nodules in the palmar fascia. Dupuytren's rarely involves the DIP joints and does not present with sudden onset rigid posturing.
- Arthrogryposis Multiplex Congenita: A congenital condition characterized by multiple joint contractures present at birth.
- Spastic Hand Deformities: Secondary to upper motor neuron lesions (e.g., stroke, cerebral palsy, traumatic brain injury). These will present with other upper motor neuron signs (hyperreflexia, positive Hoffman's sign, spastic catch on rapid passive stretch).
- Volkmann Ischemic Contracture: Secondary to missed compartment syndrome. Will present with a history of trauma/ischemia and a positive stretch test of the ischemic muscles.
Clinical Pearl: To definitively diagnose a psychogenic deformity, the surgeon may utilize a regional anesthetic block (e.g., a Bier block or median/ulnar nerve blocks) or examine the patient under brief general anesthesia. In a purely psychogenic deformity, once the patient is anesthetized, the rigid contracture will completely melt away, revealing perfectly supple joints. If the joints remain contracted under anesthesia, a structural contracture has developed.
Management of Psychogenic Deformities
The management of psychogenic hand deformities is notoriously difficult and requires a multidisciplinary approach.
- Avoid Surgery: Operative intervention (e.g., flexor tendon lengthening, joint capsule release) is strictly contraindicated for the primary psychogenic posturing, as it will not cure the underlying psychiatric disorder and often leads to worsening of the symptoms or transfer of the deformity to another limb.
- Psychiatric Intervention: Immediate referral to a psychiatrist or psychologist is the primary treatment modality. Cognitive-behavioral therapy (CBT) and management of underlying depression, anxiety, or conversion disorders are essential.
- Hand Therapy: Gentle, non-confrontational hand therapy is employed to maintain joint suppleness and prevent secondary structural contractures while the psychiatric treatment takes effect.
- Hygiene Management: In severe clenched fist syndrome, the interposition of soft, antimicrobial padding (e.g., silver-impregnated foam) between the fingernails and the palm is critical to prevent palmar ulceration and secondary osteomyelitis of the metacarpals.
You Might Also Like
