Anatomic Double-Bundle ACL Reconstruction: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on anatomic double-bundle ACL reconstruction. We'll meticulously cover patient positioning, precise portal placement, detailed anatomical marking, and the sequential drilling of femoral and tibial tunnels. Learn graft preparation, secure fixation techniques, and critical intraoperative pearls to restore both anterior and rotational knee stability, ensuring optimal patient outcomes.
Comprehensive Introduction and Patho-Epidemiology
Welcome, colleagues and fellows, to the operating theater. Today, we are undertaking a definitive exploration of the anatomic double-bundle anterior cruciate ligament (ACL) reconstruction. This procedure represents a significant evolutionary leap in sports medicine, designed specifically to restore the complex, multi-planar kinematics of the knee more accurately than traditional isometric single-bundle techniques. The transition from single-bundle to double-bundle reconstruction was born out of the clinical observation that while single-bundle grafts effectively control anterior tibial translation, a subset of patients continues to experience residual rotational instability, clinically manifested as a persistent pivot shift. This residual laxity is a known precursor to early-onset osteoarthritis and graft failure, necessitating a more anatomically faithful reconstructive approach.
The epidemiology of ACL injuries underscores the critical need for optimal surgical solutions. Affecting hundreds of thousands of individuals annually, particularly young, high-demand athletes, the classic non-contact valgus pivoting injury mechanism exerts catastrophic sheer and rotational forces across the knee joint. When the native ACL ruptures, the knee loses its primary restraint to anterior tibial translation and its vital secondary restraint to internal rotation. The patho-epidemiology reveals that failure to adequately restore these restraints not only precludes a return to pre-injury levels of athletic performance but also alters the contact mechanics of the tibiofemoral joint, leading to accelerated chondral degradation and meniscal pathology.
The pathomechanics of the pivot-shift phenomenon are central to understanding the rationale for the double-bundle technique. The pivot shift is a dynamic subluxation and reduction of the lateral tibial plateau relative to the lateral femoral condyle. Traditional single-bundle reconstructions, often placed high and deep in the intercondylar notch (the "over-the-top" position), fail to replicate the lateralized, distal footprint of the native ACL, thereby leaving the lateral compartment vulnerable to rotational subluxation. By reconstructing both the anteromedial and posterolateral bundles, surgeons can effectively re-establish the native structural geometry of the knee, directly addressing both sagittal and axial plane instabilities.
This is a highly nuanced surgery, demanding meticulous attention to detail, advanced arthroscopic spatial awareness, and a profound, three-dimensional understanding of knee anatomy. The margin for error is exceedingly narrow; malpositioning of either bundle can lead to tunnel convergence, graft impingement, or severe kinematic restriction. Therefore, mastering this intraoperative masterclass requires not only technical dexterity but also a rigorous comprehension of the biomechanical principles that govern the native anterior cruciate ligament.

Detailed Surgical Anatomy and Biomechanics
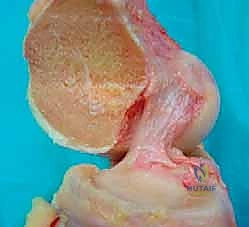
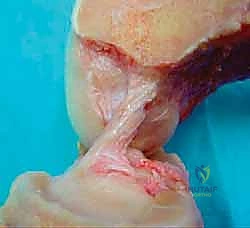
The anterior cruciate ligament is not a single, homogeneous cord, but rather a complex, multifascicular structure enveloped in a synovial fold. Anatomically and functionally, it is divided into two distinct bundles: the anteromedial (AM) bundle and the posterolateral (PL) bundle. These bundles are named relative to their insertion sites on the tibial footprint, rather than their femoral origins. Understanding the precise topography of these footprints is the foundational prerequisite for anatomic double-bundle reconstruction.
The posterolateral (PL) bundle is located posterior and lateral on the tibial footprint. On the femur, its origin is situated more distally and anteriorly relative to the AM bundle, positioned low on the lateral wall of the intercondylar notch adjacent to the articular cartilage margins. Morphologically, the PL bundle is the shorter and thicker of the two, averaging 19.7 mm in length and 6.4 mm in width. In contrast, the anteromedial (AM) bundle inserts anteriorly and medially on the tibia. Its femoral origin is located more proximally and posteriorly (higher and deeper) in the notch. The AM bundle is significantly longer, averaging 38.5 mm in length and 7.0 mm in width. Together, these bundles form a broad, C-shaped or oval footprint that covers a substantial surface area, which a single cylindrical graft cannot fully replicate.
Dynamic Tensioning and Kinematic Function
The biomechanical interplay between the AM and PL bundles is a marvel of evolutionary engineering, providing dynamic stability throughout the entire arc of motion. During knee extension, the PL bundle is under maximal primary tension, while the AM bundle remains moderately lax. In this extended position, the PL bundle acts as the primary restraint against hyperextension and limits anterior tibial translation. Consequently, injuries isolated to the PL bundle often present with subtle anterior laxity in extension but profound rotational instability.
As the knee transitions into flexion, a reciprocal tensioning pattern emerges. The AM bundle progressively tightens, assuming the role of the primary restraint to anterior translation at 90 degrees of flexion, while the PL bundle simultaneously becomes lax. This dynamic, non-isometric behavior allows for normal, uninhibited knee flexion while maintaining continuous anterior stability. Furthermore, the bundles exhibit complex behavior under rotational loads. With internal and external rotation of the tibia at varying degrees of flexion, the PL bundle tightens significantly, contributing massively to rotational control and mitigating the pivot-shift phenomenon.
Understanding this dynamic tensioning is paramount for the operating surgeon. A non-anatomic single-bundle reconstruction, while effective in limiting anterior tibial translation in the sagittal plane, often falls short in restoring the combined rotatory load of internal and valgus torque. This is precisely where the double-bundle technique excels. By independently tensioning the AM graft in flexion and the PL graft in near-extension, the surgeon can restore the native reciprocal tensioning pattern, thereby re-establishing the intricate, coupled biomechanics of the human knee.
Exhaustive Indications and Contraindications
The decision to proceed with an anatomic double-bundle ACL reconstruction must be highly individualized, weighing the biomechanical advantages against the increased technical complexity and operative time. The primary indication is a symptomatic patient with recurrent instability or episodes of "giving way" that severely impact their activities of daily living or high-level sports participation, particularly those involving cutting, pivoting, and sudden deceleration. This technique is especially beneficial for patients demonstrating high-grade rotational laxity on clinical examination, such as a Grade III pivot shift, where a single-bundle graft may be insufficient to control the lateral compartment.
Furthermore, the double-bundle approach is highly advantageous in revision ACL reconstruction scenarios. Frequently, primary single-bundle failures are the result of non-anatomic femoral tunnel placement—specifically, tunnels placed too vertically or too anteriorly in the "over-the-top" position. In these revision cases, the native anatomic footprints for both the AM and PL bundles are often pristine and untouched by the previous surgery. The double-bundle technique allows the surgeon to drill two new, anatomically correct femoral tunnels without structurally interfering with or converging into the pre-existing, malpositioned primary tunnel.
However, careful patient selection requires acknowledging definitive contraindications. Skeletally immature patients with open physes are absolute contraindications for standard double-bundle techniques due to the unacceptably high risk of physeal arrest from drilling four separate transphyseal tunnels. Additionally, patients with a severely stenotic intercondylar notch (notch width less than 12-14 mm) may not accommodate two distinct grafts without significant impingement, necessitating either a notchplasty (which alters native anatomy) or defaulting to a single-bundle construct. Severe, advanced osteoarthritis and complex multiligamentous knee injuries requiring staged reconstructions also generally preclude the use of the double-bundle technique.
| Category | Specific Criteria | Clinical Rationale |
|---|---|---|
| Indications | High-demand, pivoting athletes | Requires maximal rotational stability to return to elite play. |
| Indications | Severe rotational laxity (Grade III Pivot Shift) | Single bundle often fails to control profound lateral compartment subluxation. |
| Indications | Revision ACL Reconstruction | Allows anatomic placement bypassing previous non-anatomic "over-the-top" tunnels. |
| Indications | Partial ACL tears (one bundle intact) | Augmentation of the ruptured bundle while preserving the intact, proprioceptive bundle. |
| Contraindications | Skeletally immature patients (open physes) | High risk of iatrogenic physeal arrest and subsequent angular deformity. |
| Contraindications | Narrow intercondylar notch (< 12 mm) | Insufficient spatial volume to accommodate two grafts without severe impingement. |
| Contraindications | Severe, advanced osteoarthritis | Altered joint kinematics and poor tissue healing environment. |
| Contraindications | Severe multiligamentous knee injuries | Increased surgical complexity and risk of fluid extravasation/compartment syndrome. |
Pre-Operative Planning, Templating, and Patient Positioning
Comprehensive preoperative planning is the cornerstone of a successful double-bundle reconstruction. Before entering the operating room, a meticulous radiographic workup is mandatory. Standard plain radiographs must include a 30-degree flexion weight-bearing posteroanterior (PA) view to accurately assess joint space narrowing and dynamic coronal alignment. A true lateral view is required to evaluate patellar height (Insall-Salvati ratio) and overall sagittal alignment, while a sunrise or Merchant view assesses the patellofemoral articulation. Crucially, a long-leg mechanical axis alignment view should be obtained in cases of suspected coronal angular deformity; significant varus or valgus malalignment can exponentially increase sheer forces on the healing grafts, potentially necessitating a concomitant osteotomy.
Beyond plain films, Magnetic Resonance Imaging (MRI) is indispensable. It not only confirms the diagnosis of an ACL tear but provides a high-resolution map of the joint's internal derangement. The surgeon must scrutinize the MRI for concomitant pathology, including meniscal tears (particularly ramp lesions of the medial meniscus or root tears of the lateral meniscus), chondral defects, and injuries to the collateral ligaments or posterolateral corner. Furthermore, MRI helps characterize the specific pattern of the ACL injury—whether it is a midsubstance rupture, a femoral avulsion, or an isolated tear of a single bundle. Bone bruise patterns, typically seen on the lateral femoral condyle and posterolateral tibial plateau, serve as a radiographic footprint of the pivot-shift mechanism.
Anesthesia, EUA, and Patient Setup
Prior to any surgical incision, a rigorous Evaluation Under Anesthesia (EUA) is performed. Muscular relaxation allows for an uninhibited assessment of joint laxity. The surgeon must meticulously document the range of motion (ROM) compared to the contralateral limb. Ligamentous testing, including the Lachman test, pivot-shift test, anterior/posterior drawer, and varus/valgus stress testing at 0 and 30 degrees, confirms the diagnosis and rules out occult multiligamentous instability that may have been masked by patient guarding in the clinic.
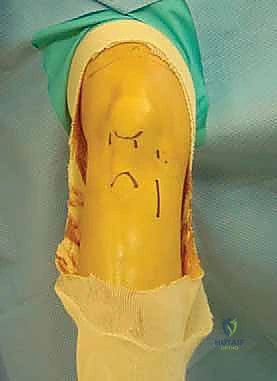
Patient positioning demands precision to ensure optimal arthroscopic access and intraoperative safety. The patient is positioned supine on the operating table. The nonoperative leg is carefully placed in a well-leg holder in an abducted lithotomy position, ensuring meticulous padding over the fibular head to prevent common peroneal nerve neuropraxia. A pneumatic tourniquet is applied high on the operative thigh. Following exsanguination via limb elevation for three minutes, the tourniquet is insufflated (typically 300 to 350 mm Hg). The operative leg is then secured in a rigid arthroscopic leg holder positioned at the level of the tourniquet. This setup is critical, as it allows the surgeon to apply valgus stress and control knee flexion from 0 to 120 degrees seamlessly—a maneuver absolutely essential during femoral tunnel drilling. The limb is then prepped and draped in a standard sterile fashion, ensuring a wide operative field for graft harvest.
Step-by-Step Surgical Approach and Fixation Technique
The establishment of precise arthroscopic portals is the gateway to anatomic reconstruction; malpositioned portals will invariably lead to malpositioned tunnels. We utilize a three-portal technique tailored specifically for double-bundle access. The Anterolateral Portal is established first, placed slightly more superior than in standard arthroscopy, at the level of the inferior pole of the patella, adjacent to the lateral border of the patellar tendon. This provides an optimal panoramic view of the tibial footprint. The Central Anteromedial Portal is critical; placed just below the inferior pole of the patella and approximately 1 cm lateral to the medial edge of the patellar tendon (often intratendinous), it serves as the primary viewing portal during femoral tunnel creation, offering an unparalleled look at the lateral wall of the intercondylar notch. Finally, the Accessory Anteromedial Portal is established under direct intra-articular visualization using a spinal needle. Placed medially and distally to the central portal, just above the anterior horn of the medial meniscus, this portal provides the necessary trajectory to drill the femoral tunnels anatomically, independent of the tibial tunnels.
Upon entering the joint, a systematic diagnostic arthroscopy is performed, evaluating all compartments, chondral surfaces, and menisci. Any associated meniscal or chondral pathology must be addressed prior to ACL reconstruction to establish a stable joint environment. Attention is then turned to the ACL remnant. Using a radiofrequency ablation device, the ruptured tissue is carefully debrided. Crucially, the surgeon must strive to preserve the intact synovial envelope and the tibial/femoral footprint remnants. These remnants contain vital mechanoreceptors and proprioceptive nerve fibers that enhance postoperative neuromuscular control and aid in graft revascularization. The exact anatomic insertion sites of both the AM and PL bundles on the femur and tibia are then meticulously marked with the thermal device.
Femoral Tunnel Creation: Independent Drilling
Femoral tunnel creation begins with the Posterolateral (PL) bundle. Viewing through the central anteromedial portal, a 3/32 Steinmann pin is introduced via the accessory anteromedial portal. The tip is placed precisely on the marked PL footprint, low and shallow on the lateral notch wall, approximately 8 mm from the anterior articular cartilage and 5 mm from the distal articular cartilage.
SURGICAL WARNING - PERONEAL NERVE PROTECTION: Once the pin is positioned, the knee MUST be hyperflexed to 120 degrees or more. This hyperflexion drops the posterior structures away from the posterior femoral condyle, dramatically increasing the safety margin between the drill tip and the common peroneal nerve. Failure to hyperflex during independent femoral drilling is a primary cause of iatrogenic foot drop.
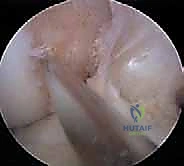
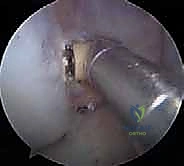
With the knee hyperflexed, the guidewire is advanced. It is then over-drilled using a 7-mm acorn drill to a depth of 25 to 30 mm, taking extreme care not to scuff the medial femoral condyle with the drill shaft. The far cortex is subsequently breached with a 4.5-mm EndoButton drill, and the total channel length is measured to calculate the appropriate suspensory fixation loop length.
Attention then shifts to the Anteromedial (AM) femoral tunnel. The guidewire is placed on the marked AM footprint, which is proximal and posterior (higher and deeper) relative to the PL tunnel. A critical technical pearl here is ensuring a minimum 2 to 3 mm bone bridge remains between the two femoral tunnels to prevent tunnel confluence and subsequent loss of fixation. The AM tunnel is drilled in a similar fashion, again utilizing hyperflexion, typically utilizing an 8-mm or 9-mm acorn drill depending on the measured diameter of the prepared AM graft.
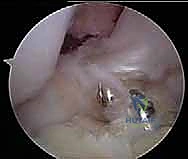
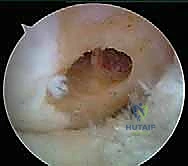
Tibial Tunnel Creation and Graft Passage
Tibial tunnel creation requires equal precision to avoid convergence. We typically utilize a standard tibial aiming guide set at 45 to 50 degrees. The PL tibial tunnel is drilled first. The guide is introduced through the anteromedial portal, and the tip is placed on the posterior and lateral aspect of the native tibial footprint. The extra-articular starting point is positioned on the anteromedial tibia, slightly more distal and medial than a standard single-bundle starting point. A guidewire is advanced, followed by a reamer matched to the PL graft diameter (usually 7 mm).
Next, the AM tibial tunnel is created. The guide is positioned on the anterior and medial aspect of the native footprint. To prevent the tunnels from converging within the proximal tibia, the extra-articular starting point for the AM tunnel must be distinct—typically placed more proximal and lateral to the PL starting point, creating divergent trajectories. The AM tunnel is then reamed to the appropriate diameter.
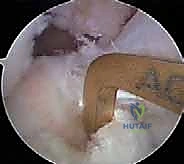
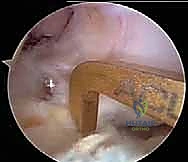
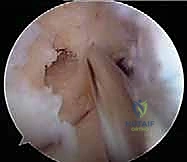
With all four tunnels prepared and cleared of debris, graft passage commences. Passing sutures are retrieved from the femoral tunnels out through the respective tibial tunnels. The PL graft is passed first to avoid entanglement, drawn up into the PL femoral socket, and secured with its suspensory cortical button. The AM graft is subsequently passed and secured in the AM femoral socket.
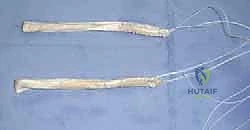
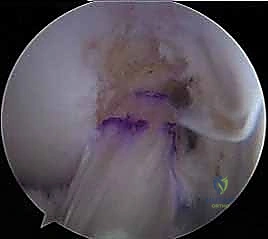
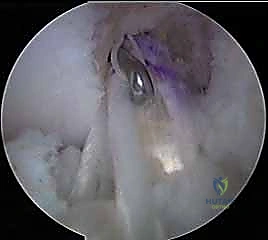
Differential Tensioning and Tibial Fixation
The final, and arguably most critical biomechanical step, is differential graft tensioning. Fixation must occur at the specific flexion angles where each native bundle experiences maximal tension. The knee is cycled through a full range of motion 20 times to precondition the grafts and allow for stress relaxation.
The PL bundle is tensioned and fixed first. The knee is placed in near full extension (0 to 15 degrees of flexion), and a posterior drawer force is applied to reduce the tibia. The PL graft is tensioned to approximately 20-30 Newtons and secured within the tibial tunnel, typically using an interference screw or a suspensory button.
The knee is then flexed to 45 to 60 degrees. At this angle, the AM bundle is tensioned to approximately 40-50 Newtons and secured. This differential fixation sequence ensures that the reciprocal tensioning pattern of the native ACL is perfectly reproduced, preventing over-constraint of the joint while eliminating both sagittal and rotational laxity.
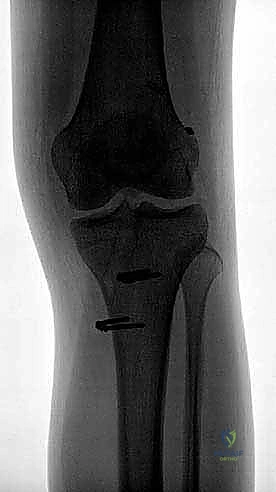
Complications, Incidence Rates, and Salvage Management
While the anatomic double-bundle technique offers superior biomechanical restoration, it inherently carries a higher profile of surgical complexity and potential complications compared to single-bundle reconstruction. The most unique and detrimental complication is tunnel convergence (confluence). Because four distinct tunnels are drilled within the restricted bony confines of the distal femur and proximal tibia, slight deviations in trajectory can cause the tunnels to merge. This compromises bone stock, weakens fixation, and can lead to catastrophic graft failure. Prevention relies on meticulous spatial awareness, maintaining a minimum 2-3 mm bone bridge on the femur, and utilizing divergent starting points on the tibia.
Iatrogenic neurologic and chondral injuries represent severe morbidities. As previously emphasized, drilling the low accessory PL femoral tunnel without adequate knee hyperflexion places the common peroneal nerve at direct risk of transection or thermal necrosis from the drill bit exiting the posterior cortex. Furthermore, passing instruments through the accessory anteromedial portal carries a risk of scuffing the articular cartilage of the medial femoral condyle. Surgeons must maintain direct arthroscopic visualization of all instruments entering the joint space.
Postoperative stiffness and arthrofibrosis are also more prevalent if grafts are improperly tensioned. Over-tensioning the PL bundle in deep flexion, or the AM bundle in full extension, will "capture" the joint, severely restricting the patient's range of motion and leading to altered patellofemoral mechanics. If stiffness persists despite aggressive physical therapy, arthroscopic lysis of adhesions and manipulation under anesthesia may be required.
| Complication | Estimated Incidence | Prevention and Salvage Management |
|---|---|---|
| Tunnel Convergence | 1% - 4% | Prevention: Divergent guide pin placement; maintain 3mm bone bridges. Salvage: If confluence occurs, abandon DB; convert to a large single-bundle graft using the combined tunnel space. |
| Peroneal Nerve Injury | < 1% | Prevention: Hyperflex knee >120° during femoral drilling. Salvage: Immediate neurosurgical consultation; AFO bracing for foot drop; potential nerve exploration. |
| Articular Cartilage Scuffing | 2% - 5% | Prevention: Direct visualization of drill bits; use of portal cannulas. Salvage: Debridement of loose flaps; microfracture if full-thickness defect occurs. |
| Arthrofibrosis / Stiffness | 3% - 7% | Prevention: Anatomic tensioning angles (PL in extension, AM in flexion). Salvage: Aggressive early ROM therapy; Arthroscopic lysis of adhesions if refractory > 3 months. |
| Graft Failure / Re-rupture | 4% - 8% | Prevention: Proper tunnel placement; adherence to biologic healing timelines. Salvage: Revision ACLR; may require bone grafting of widened |
