Navigating Superior Glenohumeral Dislocation: Diagnosis & Care
Introduction & Epidemiology
Superior glenohumeral dislocation (SGD) represents a rare and challenging injury, constituting a small fraction of all glenohumeral dislocations. While inferior glenohumeral dislocation (luxatio erecta) is more commonly described, pure superior dislocation of the humeral head above the glenoid fossa is exceedingly uncommon, often occurring in the setting of high-energy trauma. Its rarity contributes to a paucity of large prospective studies, with much of the current literature comprising case reports and small series.
This injury typically involves significant disruption of both static and dynamic stabilizers of the shoulder, including the glenohumeral capsule, glenoid labrum, rotator cuff tendons (particularly the supraspinatus and subscapularis), and often the long head of the biceps tendon. Due to the substantial forces required to displace the humeral head superiorly, SGD is frequently associated with concomitant osseous injuries. These can include fractures of the acromion, clavicle, coracoid process, and humeral tuberosities (greater and lesser). Furthermore, injury to the acromioclavicular (AC) joint is a common associated finding, reflecting the disruption of the superior shoulder girdle.
A critical aspect of SGD is the high incidence of neurovascular compromise. The brachial plexus, particularly the superior trunk (C5-C6 nerve roots), and the axillary vessels are at significant risk of stretch, compression, or direct injury due to the superior displacement of the humeral head and potential fracture fragments. Therefore, a meticulous neurovascular assessment is paramount in the initial evaluation and throughout the management course.
Surgical Anatomy & Biomechanics
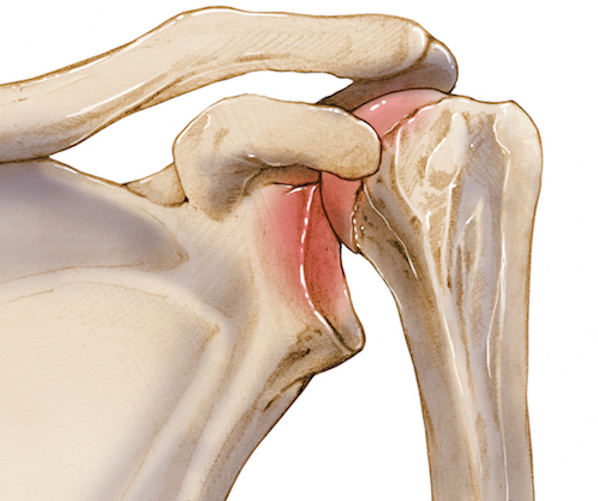
The inherent instability of the glenohumeral joint, a ball-and-socket articulation designed for vast mobility, relies heavily on a complex interplay of static and dynamic stabilizers. The glenoid fossa, being shallow and pear-shaped, provides minimal bony constraint. This is augmented by the glenoid labrum, which effectively deepens the socket. The glenohumeral capsule, reinforced by the superior, middle, and inferior glenohumeral ligaments, provides passive stability. However, the primary static restraint against superior migration of the humeral head is the coracoacromial arch, formed by the acromion, coracoacromial ligament, and coracoid process. The integrity of this arch, along with the intact rotator cuff tendons and the long head of the biceps tendon, is crucial in preventing superior translation of the humeral head.
In the context of superior glenohumeral dislocation, these critical superior restraints are profoundly compromised. The mechanism typically involves an extreme anterior and superior directed force applied to an adducted upper extremity. This force, often from a fall from a significant height directly onto the shoulder or a direct superior impact, drives the humeral head forcefully into and through the coracoacromial arch. This often results in a "bursting" injury pattern, disrupting the supraspinatus and subscapularis tendons, tearing the superior capsule, and frequently fracturing components of the coracoacromial arch itself. The long head of the biceps tendon, which acts as a superior depressor of the humeral head, is also commonly injured, either avulsed or subluxed.
The proximity of vital neurovascular structures, namely the brachial plexus (especially the superior trunk and axillary nerve) and the axillary artery and vein, renders them highly susceptible to injury. The superiorly displaced humeral head or associated fracture fragments can directly impinge, stretch, or lacerate these structures. Understanding this intricate anatomy and the biomechanical consequences of the injury mechanism is fundamental to both accurate diagnosis and effective surgical planning. The stability of the AC joint and the integrity of the conoid and trapezoid ligaments are also often disrupted, contributing to superior displacement.
Indications & Contraindications
The management of superior glenohumeral dislocation is primarily surgical, given the high-energy nature of the injury, the frequent association with significant soft tissue and osseous pathology, and the imperative to restore stability and function while minimizing neurovascular sequelae.
Indications for Operative Management:
- Irreducible Dislocation: The most common indication. Closed reduction attempts are often unsuccessful and can carry a high risk of iatrogenic neurovascular injury or further soft tissue damage, particularly in SGD with interposed soft tissues (e.g., torn rotator cuff, long head of biceps, capsular remnants) or fracture fragments blocking the glenoid.
-
Associated Fractures Requiring Fixation:
- Displaced acromion fractures (especially those compromising the subacromial space or affecting the deltoid origin).
- Displaced clavicle fractures (particularly those contributing to superior instability or affecting the AC joint).
- Coracoid fractures with significant displacement or involvement of the coracoacromial ligament/conjoint tendon origin.
- Displaced greater or lesser tuberosity fractures of the humerus, indicative of significant rotator cuff avulsion and requiring repair for cuff integrity.
- Glenoid rim fractures leading to instability or articular incongruity.
- Significant Rotator Cuff Tears: Acute, reparable full-thickness tears, particularly of the supraspinatus and subscapularis, which are integral to restoring superior stability.
- Neurovascular Compromise: While acute vascular injury often necessitates immediate intervention by a vascular surgeon, nerve entrapment or persistent neurological deficit despite reduction may require exploration and decompression.
- Open Dislocation: Requires urgent surgical debridement, reduction, and stabilization to prevent infection and facilitate healing.
- Young, Active Patients: To optimize functional recovery and minimize long-term sequelae such as recurrent instability or post-traumatic arthritis.
Indications for Non-Operative Management:
Non-operative management of pure superior glenohumeral dislocation is exceedingly rare and generally reserved for specific, highly selected patient populations or scenarios.
- Severe Medical Comorbidities: Patients with prohibitive surgical risks where the risks of anesthesia and surgery outweigh the potential benefits of operative stabilization.
- Non-Ambulatory or Sedentary Patients: In whom shoulder function is not a primary concern and pain can be managed conservatively, provided neurovascular integrity is maintained and no significant instability or impending skin breakdown.
- Minimally Displaced or Stable Associated Fractures: In conjunction with a reducible dislocation, if the overall stability of the shoulder can be achieved through immobilization and rehabilitation, and there is no interposition. (This is rarely the case for SGD itself).
- Patient Refusal: After thorough discussion of the risks and benefits of both operative and non-operative approaches.
| Category | Operative Indications | Non-Operative Indications (Rarely Applicable for SGD) |
|---|---|---|
| Dislocation Status | Irreducible dislocation (common for SGD) | Mildly symptomatic, spontaneously reduced (extremely rare), or long-standing chronic dislocation in an elderly, low-demand patient with stable pseudoarthrosis and acceptable function. |
| Associated Fractures | Displaced acromion, clavicle, coracoid, glenoid rim, or humeral tuberosity fractures requiring fixation for stability or articular congruence. | Minimally displaced, stable associated fractures (e.g., hairline greater tuberosity), not contributing to instability or blocking reduction. |
| Soft Tissue Injury | Acute, reparable full-thickness rotator cuff tears (supraspinatus, subscapularis). Significant labral tears affecting stability. | Partial rotator cuff tears without significant instability, or diffuse capsular injury managed by immobilization and rehabilitation in a low-demand patient, provided reduction is achieved and maintained. |
| Neurovascular | Neurovascular compromise (nerve entrapment, vascular injury) requiring exploration and repair. | Transient neuropraxia that resolves spontaneously after reduction and without ongoing compression. |
| Patient Factors | Young, active patients aiming for full functional recovery. Open dislocations. | Severe medical comorbidities precluding surgery. Non-ambulatory, very elderly, or extremely low-demand patients where surgical risk outweighs functional benefit. Patient refusal of surgery after informed consent. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for managing superior glenohumeral dislocation, given its complexity and potential for significant morbidity.
Initial Assessment and Stabilization:
Upon presentation, immediate assessment includes a thorough primary and secondary trauma survey. Special attention is directed to the affected upper extremity.
*
Clinical Examination:
The patient typically presents with a foreshortened upper extremity held in adduction. A clinical examination invariably reveals a palpable humeral head above the level of the acromion, often with associated crepitus. Neurovascular injuries are common and must be ruled out through a detailed assessment of motor function, sensation (including axillary nerve distribution), and distal pulses. Documentation of pre-operative neurovascular status is paramount.
*
Pain Management & Immobilization:
Adequate analgesia is provided, and the limb is immobilized in an adducted position using a sling and swathe to minimize further soft tissue damage and pain.
Imaging Studies:
-
Plain Radiographs:
A trauma series of the affected shoulder is obtained, including:
- Anteroposterior (AP) view: The AP radiograph is typically diagnostic, clearly demonstrating dislocation of the humeral head superior to the acromion process. This view must be carefully scrutinized for associated fractures, which are common and may be clinically not detected because of a diffusely painful shoulder.
- Scapular-Y view: Helps to confirm the superior displacement relative to the glenoid and acromion in a different plane.
- Axillary view: Crucial for confirming the direction of dislocation (superior, not anterior or posterior) and assessing the integrity of the glenoid rim. Often difficult to obtain in severe pain or with significant displacement.
-

-
Computed Tomography (CT) Scan:
Essential for comprehensive evaluation. A CT scan with 3D reconstructions provides detailed information regarding:
- Precise location and orientation of the humeral head.
- Identification and characterization of associated fractures (acromion, clavicle, coracoid, glenoid, humeral tuberosities), including their displacement and articular involvement.
- Detection of incarcerated fracture fragments or soft tissue blocking reduction.
- Assessment of glenoid bone loss.
-
Magnetic Resonance Imaging (MRI):
While not typically an emergency study, MRI can be valuable for assessing the extent of rotator cuff tears, labral injury, and capsular disruption once the dislocation is reduced. In complex cases, it may be obtained pre-operatively if the surgical plan hinges on specific soft tissue repairs, though often the full extent of injury is only appreciated intraoperatively.
-
(This image could represent a CT or MRI scan if it provides more detailed anatomical information than a plain radiograph, or it could be placed to illustrate internal fixation post-reduction, depending on its actual content).
-
Consultations:
- Vascular Surgery: Mandated if any signs of arterial or venous compromise are present.
- Neurosurgery/Neurology: If significant or persistent neurological deficit is identified, especially with concern for brachial plexus avulsion or severe nerve laceration.
Anesthesia and Patient Positioning:
- Anesthesia: General endotracheal anesthesia is standard. An interscalene brachial plexus block can be a valuable adjunct for both intraoperative and post-operative pain management, minimizing opioid requirements.
-
Patient Positioning:
- Beach Chair Position: This is the preferred position for most open shoulder procedures, offering excellent access to the superior, anterior, and lateral aspects of the shoulder. The patient is semi-recumbent, with the torso elevated, and the head secured in a headrest. The affected arm is freely draped to allow for full range of motion intraoperatively. Adequate padding of all pressure points is crucial.
- Lateral Decubitus Position: An alternative, particularly if a more posterior or lateral approach is anticipated, or if extensive fracture fixation on the posterior aspect of the acromion or scapula is required. However, direct access to the superior aspect for primary reduction of SGD can be more challenging.
Surgical Planning:
Based on the comprehensive imaging and clinical assessment, a detailed surgical plan is formulated. This includes:
* Choice of surgical approach (often superior or combined deltopectoral and superior).
* Anticipated techniques for reduction (open vs. attempted closed).
* Specific implants for fracture fixation (plates, screws, tension bands).
* Strategy for rotator cuff or capsular repair (suture anchors, transosseous sutures).
* Contingency plans for neurovascular injury or irreducible dislocation.
* Discussion of potential need for bone grafting in large defects.
Detailed Surgical Approach / Technique
Surgical management of superior glenohumeral dislocation typically involves an open reduction due to the inherent instability, high probability of interposed soft tissues or bony fragments, and the need to address associated injuries. The goal is to achieve anatomic reduction, stabilize the joint, and repair damaged structures.
1. Incision and Initial Exposure:
The choice of incision depends on the specific injury pattern and associated fractures.
*
Superior Approach (Saber-cut/Transdeltoid):
Often preferred for direct access to the superiorly displaced humeral head, acromion, and rotator cuff. An incision is made from the posterior aspect of the acromion, curving anteriorly along its lateral border, and then extending distally onto the deltoid.
*
Deltoid Split:
The deltoid muscle fibers can be carefully split longitudinally, typically between the anterior and middle portions, or through the middle deltoid, taking extreme care to avoid the axillary nerve, which runs approximately 5-7 cm distal to the lateral acromion.
*
Deltopectoral Approach:
While primarily used for anterior shoulder pathology, an extended deltopectoral approach can be combined with a superior exposure if anterior structures (e.g., subscapularis, coracoid) also require extensive repair or fixation. The interval between the deltoid and pectoralis major is identified (cephalic vein typically runs in this groove, retracted laterally with the deltoid).
*
Combined Approach:
In complex cases involving extensive damage to multiple structures, a combination of superior and deltopectoral approaches may be necessary.
2. Neurovascular Protection:
Upon exposure, meticulous identification and protection of the brachial plexus and axillary vessels are paramount. These structures are often stretched, compressed, or even directly injured by the displaced humeral head or fracture fragments.
* The axillary nerve is particularly vulnerable at the inferior aspect of the glenoid and as it courses around the surgical neck of the humerus.
* The brachial plexus elements (especially the superior trunk) lie superior and medial to the humeral head.
3. Assessment and Debridement:
- Once exposed, the surgeon directly visualizes the dislocated humeral head, the glenoid fossa, and the surrounding soft tissues.
-
Identify any structures blocking reduction:
- Torn rotator cuff (supraspinatus, subscapularis).
- Long head of biceps tendon (often torn or dislocated).
- Interposed capsular tissue.
- Loose osteochondral fragments from the glenoid or humeral head.
- Fractured portions of the acromion, coracoid, or tuberosities.
- Debride any devitalized or severely contaminated tissue, particularly in open dislocations.
- Carefully release any soft tissue or bony incarceration preventing reduction.
4. Open Reduction of the Humeral Head:
- Achieve strong longitudinal traction on the abducted and externally rotated arm by an assistant.
- Using blunt instruments (e.g., elevators, Kocher clamps) or a femoral head skid, gently disengage the humeral head from its superior position.
- Once freed, a combination of direct pressure on the humeral head and manipulation of the arm (gentle internal rotation and adduction) is used to guide the head back into the glenoid fossa. Avoid excessive force to prevent further iatrogenic injury.
- Confirm reduction visually and by palpation of a stable joint.
5. Repair of Associated Injuries and Stabilization:
Once reduced, the focus shifts to addressing the extensive associated soft tissue and osseous injuries to restore stability.
-
Rotator Cuff Repair:
- The supraspinatus and subscapularis tendons are commonly avulsed or lacerated. These require meticulous repair to their footprints on the greater and lesser tuberosities, respectively.
- Techniques include transosseous sutures, suture anchors (single-row or double-row configurations), or a combination, ensuring strong fixation.
- If the biceps long head is ruptured or significantly unstable, tenodesis or tenotomy may be performed.
-
Capsular and Labral Repair:
- The superior glenohumeral capsule and labrum are often torn. These are repaired using suture anchors placed into the glenoid rim to restore the capsulolabral complex.
-
Fracture Fixation:
- Acromion Fractures: Depending on the pattern (e.g., Neer Type I, II, III), fixation may involve plates and screws, tension band wiring, or K-wires, ensuring restoration of the superior support structure and subacromial space.
- Clavicle Fractures: Displaced clavicle fractures often require plate and screw fixation to restore shoulder girdle stability.
- Coracoid Fractures: If displaced, particularly those involving the base or apex, screws can be used for fixation, protecting the conjoint tendon.
- Humeral Tuberosity Fractures: These are often avulsion fractures associated with rotator cuff tears. Fixation typically involves suture anchors (integrating with cuff repair) or small screws for larger fragments.
- Glenoid Fractures: Small rim fractures may be reattached with suture anchors. Larger articular fragments or glenoid Fx-dislocations may require screw fixation.
6. Verification and Closure:
- Perform a thorough assessment of the reduced shoulder's stability through a full range of motion. Confirm there is no impingement or further dislocation.
- Re-check neurovascular status.
- Irrigate the wound thoroughly.
- Close the deltoid and other muscle layers, subcutaneous tissue, and skin in a layered fashion. A drain may be considered if extensive dissection or bleeding is anticipated.
Complications & Management
Superior glenohumeral dislocation is associated with a high rate of complications due to the severity of the initial trauma and the complexity of the reconstructive surgery. Prognosis is largely dependent on the extent of initial soft tissue and neurovascular injury.
| Complication | Incidence | Salvage Strategies |
|---|---|---|
| Neurological Injury | High (reported 20-50% in shoulder dislocations; higher in SGD, particularly superior trunk/axillary nerve, often neuropraxia) |
Mild Neuropraxia:
Observation, electrodiagnostic studies (EMG/NCS) at 3-6 weeks. Physical therapy for joint mobility.
Persistent Deficit/Laceration: Early neurosurgical consultation, exploration, neurolysis, direct repair, or nerve grafting. Tendon transfers for chronic deficits. |
| Vascular Injury | Rare but devastating (axillary artery/vein) | Acute: Immediate vascular surgery consultation and surgical repair (e.g., primary repair, vein graft). |
| Irreducible Dislocation | Common (due to interposed soft tissue/bone, especially in SGD) | Open reduction (as primary surgical strategy). Careful release of entrapped structures (rotator cuff, biceps tendon, capsule, fracture fragments). |
| Recurrent Instability/Dislocation | Variable (depending on initial injury, repair quality, and patient compliance; can be high if underlying pathology not fully addressed) | Revision surgery with soft tissue stabilization (capsular shift, labral repair, rotator cuff repair augmentation), bony procedures (glenoid bone grafting, Latarjet procedure for bone loss), or arthroplasty in severe, recurrent cases with articular damage. |
| Shoulder Stiffness/Adhesive Capsulitis | Moderate to high (due to extensive soft tissue injury, immobilization, and inflammatory response) |
Early:
Aggressive physical therapy, stretching, active/passive range of motion exercises.
Persistent: Manipulation under anesthesia (MUA), arthroscopic capsular release, open capsulotomy. |
| Osteonecrosis of Humeral Head | Low (primarily associated with fracture-dislocations, especially if reduction is delayed or vascular supply compromised) |
Early/Limited:
Conservative management, activity modification.
Progressive: Humeral head resurfacing, hemiarthroplasty, or total shoulder arthroplasty (TSA) if glenoid also involved. |
| Infection (Superficial/Deep) | Low (typical for orthopedic surgery, 1-3%) |
Superficial:
Oral antibiotics, local wound care.
Deep: Surgical debridement, intravenous antibiotics, irrigation, possible implant retention if stable, or staged implant removal and reimplantation. |
| Nonunion/Malunion of Associated Fractures | Variable (depending on fracture type, fixation quality, patient factors; particularly challenging for acromial/coracoid) |
Nonunion:
Revision fixation with bone grafting (autograft/allograft), electrical stimulation.
Malunion: Osteotomy to correct deformity, or arthroplasty if joint mechanics significantly compromised. |
| Post-Traumatic Arthritis | Variable (long-term complication, especially with articular damage or recurrent instability) |
Early/Mild:
Conservative management (NSAIDs, injections, physical therapy).
Progressive/Severe: Humeral head resurfacing, hemiarthroplasty, total shoulder arthroplasty, or reverse total shoulder arthroplasty (rTSA) if significant rotator cuff deficiency. |
| Hardware-Related Complications | Low to moderate (implant prominence, screw loosening/breakage) | Symptomatic hardware removal after fracture healing. Revision fixation if implant failure leads to loss of reduction or nonunion. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following surgical repair of superior glenohumeral dislocation is a critical determinant of functional outcome. Protocols are individualized based on the extent of soft tissue and bony injury, the stability achieved intraoperatively, and the specific repairs performed (e.g., rotator cuff repair, fracture fixation). The general principles emphasize protection during early healing, followed by progressive restoration of motion, strength, and function.
Phase I: Protection and Early Motion (0-6 weeks)
- Goals: Protect surgical repairs, minimize pain and inflammation, prevent stiffness, initiate early passive range of motion.
-
Immobilization:
- Sling immobilization is typically maintained for 4-6 weeks, with removal only for hygiene and exercises. The arm is kept in slight internal rotation and adduction (neutral position).
- Specific rotator cuff repairs (e.g., large supraspinatus/subscapularis) may necessitate a longer period of immobilization or use of an abduction pillow.
-
Passive Range of Motion (PROM):
- Initiate gentle, controlled passive range of motion within a protected arc, typically starting with forward flexion to 90 degrees, external rotation to 30 degrees (or less depending on specific repairs), and internal rotation.
- Pendulum exercises (Codman exercises) are initiated early to promote joint nutrition and gentle motion without active muscle contraction.
- Manual therapy from a physical therapist for gentle PROM and soft tissue mobilization.
-
Precautions:
- Absolutely NO active range of motion (AROM) or active contraction of the deltoid or rotator cuff muscles.
- No lifting, pushing, pulling, or weight-bearing with the affected arm.
- Avoid sudden movements or uncontrolled arm positions.
- Pain Management: Cryotherapy, NSAIDs (if not contraindicated by fracture healing concerns), and analgesics as needed.
Phase II: Controlled Active Motion (6-12 weeks)
- Goals: Gradually restore active range of motion, initiate gentle strengthening, improve dynamic stability.
- Discontinuation of Sling: Typically around 6 weeks, contingent on surgeon assessment of healing.
-
Active-Assistive & Active Range of Motion (AAROM/AROM):
- Progress from passive to active-assisted, then full active range of motion, gradually increasing arcs of motion in all planes.
- Emphasize pain-free motion.
-
Gentle Strengthening:
- Isometric exercises for the deltoid and rotator cuff (supraspinatus, infraspinatus, teres minor, subscapularis) are introduced cautiously, starting at low intensity.
- Scapular stabilization exercises to promote proper scapulothoracic rhythm.
-
Precautions:
- Avoid heavy lifting, sudden movements, or activities that place excessive stress on the healing tissues.
- No overhead lifting or resisted external rotation beyond tolerated limits.
- Careful monitoring for any signs of instability or pain with motion.
Phase III: Strengthening and Return to Activity (12+ weeks)
- Goals: Achieve full functional range of motion, progressively increase strength and endurance, prepare for return to sport or demanding activities.
-
Progressive Resistance Exercises:
- Advance strengthening for rotator cuff, deltoid, and periscapular musculature using resistance bands, light weights, and bodyweight exercises.
- Focus on eccentric strengthening and proprioceptive training.
-
Functional & Sport-Specific Training:
- Begin activities that mimic work or sport demands, gradually increasing intensity and complexity.
- Plyometric exercises for athletes, if appropriate.
- Emphasis on dynamic shoulder stability.
-
Return to Activity:
- Return to sport or heavy labor is individualized and depends on the specific injury, surgical repair, and the patient's progress. This typically ranges from 4-6 months, and sometimes longer for high-demand activities.
- Full strength, endurance, and pain-free motion are prerequisites.
Throughout all phases, regular communication between the surgeon, physical therapist, and patient is essential to adjust the protocol based on clinical findings and patient response. Neurological recovery from any associated nerve injury is also closely monitored, often requiring specific nerve gliding exercises and electrical stimulation if indicated.
Summary of Key Literature / Guidelines
Superior glenohumeral dislocation, owing to its extreme rarity, lacks the robust evidence base of large, randomized controlled trials or systematic reviews that characterize more common orthopedic conditions. The existing literature is primarily composed of case reports, small retrospective series, and expert opinion. Despite this, several guiding principles emerge from the collective experience:
- High-Energy Trauma and Associated Injuries: The literature consistently emphasizes that SGD is a consequence of high-energy trauma and is highly correlated with significant osseous and soft tissue injuries. Associated fractures of the acromion, clavicle, coracoid, and humeral tuberosities are common, as are extensive rotator cuff tears and capsuloligamentous disruptions. This necessitates a thorough evaluation for these concomitant injuries.
- Meticulous Neurovascular Assessment: A critical and recurring theme across all publications is the imperative for a detailed pre-operative neurovascular examination. The brachial plexus (especially the superior trunk and axillary nerve) and the axillary vessels are at high risk of injury. Post-reduction neurovascular status must also be meticulously documented. Delayed presentation or persistent deficits warrant further investigation (e.g., EMG/NCS, vascular studies) and potential neurosurgical or vascular consultation.
- Role of Advanced Imaging: While plain radiographs identify the dislocation, computed tomography (CT) with 3D reconstructions is considered indispensable for comprehensively assessing associated fracture patterns, glenoid involvement, and identifying any incarcerated fragments that might impede reduction. MRI can further delineate soft tissue injuries, though often performed post-reduction or when the extent of soft tissue damage will significantly alter the surgical plan.
- Predominance of Open Reduction: Closed reduction of superior glenohumeral dislocations is rarely successful and carries a significant risk of further neurovascular or soft tissue damage due to the extensive tearing and impaction typically involved. The consensus is that open reduction and internal fixation (ORIF) of associated fractures, along with repair of rotator cuff and capsulolabral structures, is the treatment of choice for most acute SGDs. This allows for direct visualization of interposed structures, meticulous reduction, and comprehensive stabilization.
- Stabilization and Reconstruction: The primary goal of operative intervention is to achieve stable anatomical reduction and to restore the integrity of both the bony and soft tissue stabilizers of the shoulder. This includes fixation of any displaced fractures and repair of the rotator cuff and capsule to prevent recurrent instability. The integrity of the coracoacromial arch and the AC joint should also be addressed.
- Complex Rehabilitation: Post-operative rehabilitation protocols must be carefully tailored to the individual patient's injury pattern and the specifics of the surgical repair. They typically involve an extended period of protection, followed by gradual progression of passive, active-assisted, and active range of motion, and finally, progressive strengthening. Recovery can be prolonged due to the extensive nature of the initial injury.
- Outcomes and Complications: While functional outcomes can be favorable with meticulous surgical management, the incidence of complications remains notable. These include persistent neurological deficits, shoulder stiffness, recurrent instability, and post-traumatic arthritis. Early identification and appropriate management of these complications are crucial for optimizing long-term results.
In summary, despite the limited high-level evidence, the guiding principles for superior glenohumeral dislocation emphasize urgent, thorough assessment, liberal use of advanced imaging, and a predominantly operative approach focusing on anatomical reduction and comprehensive stabilization of all injured structures. A collaborative, multidisciplinary approach involving trauma surgeons, orthopedic surgeons, and rehabilitation specialists is often beneficial for achieving the best possible patient outcomes.