Solve Sports Medicine Cases: Uncover Why the Correct Answer Is E
Key Takeaway
We review everything you need to understand about Solve Sports Medicine Cases: Uncover Why the Correct Answer Is E. Anterior knee pain in athletes often stems from conditions like Patellofemoral syndrome (runner's knee), Plica syndrome, or ACL tears. These conditions are diagnosed by symptoms such as overuse, instability, and specific pain locations. Treatments involve rest, strengthening vastus medialis, anti-inflammatories, and activity modification. For a holistic approach to patient care, the correct answer is e: comprehensive diagnostic and management strategies.
Detailed Patient Presentation and Mechanism of Injury
Initial Clinical Encounter and History of Present Illness
A 22-year-old female recreational jogger presents to the orthopedic sports medicine clinic complaining of insidious, progressively worsening right anterior knee pain over the preceding three months. As a dedicated runner, she typically logs 25 to 30 miles per week and is currently in the advanced stages of training for a competitive five-mile road race. Her training regimen recently underwent a significant modification, specifically the incorporation of aggressive hill training and interval sprints, which chronologically correlates with the onset of her symptoms. She denies any acute traumatic event, popping sensation, or mechanical locking.
The patient describes the pain as a dull, aching sensation centered directly around and deep to the patella, which occasionally sharpens during specific activities. She reports minimal to no visible effusion but notes a pronounced exacerbation of symptoms when ascending or descending stairs, squatting, or rising from a seated position after prolonged periods of rest (a classic positive "theater sign"). Furthermore, she complains of palpable and audible crepitus within the anterior compartment of the knee during active extension. Her past medical history is unremarkable, and she has no prior history of lower extremity surgeries or significant musculoskeletal injuries.
Biomechanics of the Patellofemoral Joint in Runners
To truly understand the etiology of this patient's presentation, one must delve into the complex biomechanics of the patellofemoral joint (PFJ), particularly under the extreme loads generated during running. The PFJ is subjected to immense reactive forces, which are exponentially magnified during activities requiring eccentric quadriceps contraction, such as downhill running or descending stairs. During level walking, the patellofemoral joint reaction force (PFJRF) is approximately 0.5 times body weight. However, during running, this force escalates to 3 to 4 times body weight, and during deep squats or downhill deceleration, it can reach up to 7 to 8 times body weight.
The patella acts as a mechanical pulley, increasing the moment arm of the extensor mechanism. Its stability within the trochlear groove is dictated by a delicate interplay of static restraints (the bony architecture of the trochlea, medial patellofemoral ligament, and lateral retinaculum) and dynamic stabilizers (the quadriceps muscle group, specifically the vastus medialis obliquus and vastus lateralis). In this patient, the abrupt addition of hill training introduced repetitive, high-magnitude eccentric loading cycles. If there is even a subtle imbalance in the dynamic stabilizers or a proximal kinetic chain deficit, the patella will maltrack, typically shifting and tilting laterally. This lateralization drastically reduces the contact area between the patellar facets and the trochlea, thereby increasing focal focal chondral stress and precipitating the inflammatory cascade recognized as Patellofemoral Pain Syndrome (PFPS).
Evolution of Symptoms and the Three-Month Follow-Up
Following her initial evaluation, the patient was diagnosed with Patellofemoral Pain Syndrome (runner's knee) and was prescribed a conservative regimen consisting of activity modification, non-steroidal anti-inflammatory drugs (NSAIDs), and targeted physical therapy. The physical therapy prescription emphasized vastus medialis obliquus (VMO) strengthening, core stabilization, and proprioceptive retraining. Despite strict adherence to the protocol, she returns to the clinic three months later with a modified symptom profile.
While her diffuse anterior aching has somewhat subsided, she now presents with recurrent, sharp right knee pain strictly localized medial to the patella. This new pain is acutely exacerbated by knee flexion, particularly between 30 and 60 degrees. She reports a sensation of a "snapping" or "catching" cord on the medial aspect of her knee during her running stride. This evolution in symptoms requires a high index of suspicion and a pivot in our diagnostic paradigm, moving away from generalized PFPS and focusing on specific secondary pathologies that arise from chronic patellar maltracking and synovial irritation.
Comprehensive Clinical Examination Findings
Visual Inspection and Gait Analysis
A meticulous clinical examination begins the moment the patient walks into the examination room. Gait analysis reveals a subtle dynamic valgus collapse of the right knee during the stance phase, accompanied by ipsilateral pelvic drop (a compensated Trendelenburg gait). This observation immediately points toward proximal weakness in the hip abductors and external rotators, a frequent underlying culprit in anterior knee pain.
Standing inspection demonstrates normal lower extremity alignment without excessive genu varum or valgum. However, an assessment of her foot biomechanics reveals mild bilateral pes planus with excessive subtalar pronation during weight-bearing. This excessive pronation drives obligate internal tibial rotation, which in turn increases the dynamic Q-angle and exacerbates lateral patellar tracking forces. Visual inspection of the knee itself shows no gross effusion, erythema, or ecchymosis. The vastus medialis obliquus appears slightly atrophic compared to the contralateral side, indicating chronic disuse or neuromuscular inhibition secondary to pain.
Palpation, Range of Motion, and Provocative Testing
Palpation of the anterior knee reveals no focal tenderness over the inferior pole of the patella (ruling out patellar tendinopathy) or the tibial tubercle (ruling out Osgood-Schlatter disease). However, there is exquisite tenderness along the medial patellar facet and the medial parapatellar soft tissues. A palpable, thickened band of tissue is appreciated rolling beneath the examiner's fingers over the medial femoral condyle as the knee is passively flexed and extended—highly indicative of a symptomatic medial synovial plica.
Range of motion is full and symmetric, from 0 degrees of extension to 140 degrees of flexion. Provocative testing for patellofemoral instability and pain is performed. The patellar apprehension test is negative, suggesting no history of frank dislocation. The patellar glide test reveals a lateral glide of 3 quadrants (hypermobile) and a medial glide of only 1 quadrant (restricted), indicating a tight lateral retinaculum. The patellar tilt test demonstrates an inability to elevate the lateral edge of the patella above the horizontal plane, further confirming lateral retinacular tightness. Clarke's test (patellar grind) elicits moderate discomfort and crepitus, confirming chondral irritation.

Neuromuscular and Kinetic Chain Assessment
In sports medicine, examining the knee in isolation is a critical error; the knee is simply a hinge caught between the hip and the foot. A thorough kinetic chain assessment is mandatory. The Ober test is profoundly positive bilaterally, indicating severe tightness of the iliotibial (IT) band and tensor fasciae latae. This tightness contributes to the lateral pull on the patella via the iliopatellar band.
Manual muscle testing reveals 4/5 strength in the right gluteus medius and gluteus maximus, compared to 5/5 on the left. Core stability is assessed via a single-leg squat test, which reproduces her dynamic valgus collapse and medial knee pain. This confirms that her patellofemoral mechanics are heavily compromised by poor proximal control. The lack of hip external rotation and abduction strength allows the femur to internally rotate underneath the patella during the stance phase of running, effectively lateralizing the patella within the trochlear groove and bowstringing the medial plica across the medial femoral condyle.
Advanced Imaging and Diagnostics
Standard Radiographic Evaluation
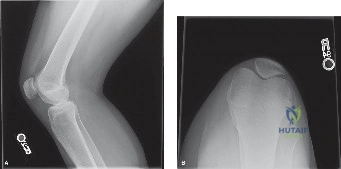
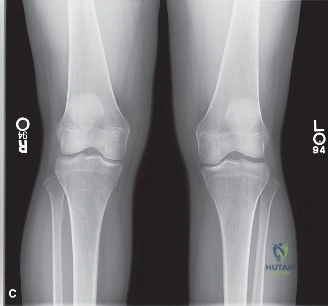
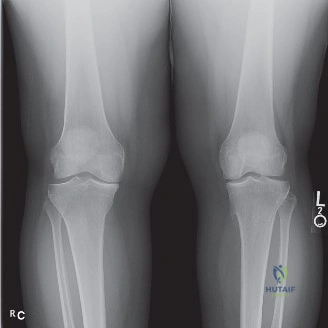
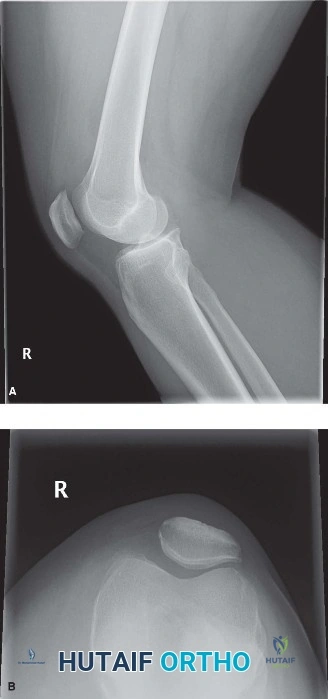
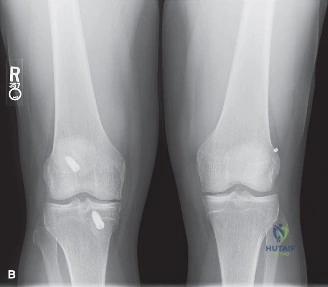
Standard radiographic evaluation of the knee is the first-line imaging modality for anterior knee pain. The patient's initial X-rays (Figures 9-1 A-C) include a weight-bearing anteroposterior (AP), a true lateral at 30 degrees of flexion, and an axial (Merchant or Sunrise) view.
The AP view demonstrates normal tibiofemoral joint spaces with no evidence of osteochondral lesions, loose bodies, or degenerative changes. The lateral view is scrutinized for patellar height. The Insall-Salvati ratio (the ratio of the patellar tendon length to the greatest diagonal length of the patella) is calculated at 1.05, which falls within the normal range (0.8 to 1.2), ruling out patella alta or baja. The lateral view also shows no evidence of trochlear dysplasia; the crossing sign is absent, and the trochlear bump is not prominent.
The Merchant view is arguably the most critical radiograph for this patient. It reveals a subtle lateral tilt of the patella and mild lateral subluxation. The sulcus angle measures 138 degrees (normal is typically <145 degrees), indicating adequate trochlear depth. However, the congruence angle is slightly lateralized, confirming the clinical suspicion of lateral patellar maltracking. There is no evidence of advanced patellofemoral osteoarthritis, osteophyte formation, or subchondral sclerosis.
Advanced Modalities and Magnetic Resonance Imaging
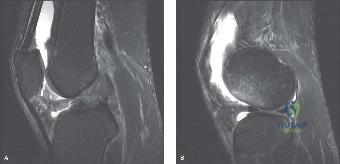
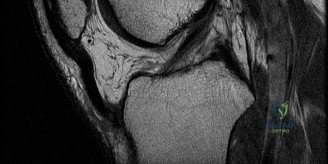
Given the patient's refractory symptoms at the three-month mark and the new onset of localized medial catching, advanced imaging via Magnetic Resonance Imaging (MRI) is indicated to evaluate the soft tissue structures and articular cartilage. MRI provides unparalleled visualization of the chondral surfaces, the medial patellofemoral ligament (MPFL), and the synovial plicae.
The axial T2-weighted fat-suppressed images reveal a thickened, fibrotic medial synovial plica extending from the medial capsule and impinging upon the medial femoral condyle during flexion. There is associated focal bone marrow edema in the medial patellar facet and the opposing medial femoral condyle, representing early chondromalacia patellae (Grade II chondral fissuring). The MPFL is intact with no signs of acute or chronic tearing. The tibial tubercle-trochlear groove (TT-TG) distance is measured at 14 mm, which is within the normal limits (<15 mm is normal, 15-20 mm is borderline, >20 mm is abnormal), suggesting that her maltracking is driven by soft tissue imbalance and dynamic kinetic chain deficits rather than static bony malalignment.
Dynamic Ultrasonography and Biomechanical Mapping
While MRI provides excellent static anatomic detail, dynamic ultrasonography can be an invaluable adjunct in the clinic to visualize the snapping medial plica in real-time. Under ultrasound guidance, the transducer is placed transversely over the medial parapatellar region while the knee is actively flexed and extended. The thickened plica can be seen snapping over the medial femoral condyle between 30 and 45 degrees of flexion, perfectly correlating with the patient's mechanical symptoms.
Furthermore, biomechanical mapping using a 3D motion capture system during treadmill running can quantify the exact degree of dynamic valgus, hip internal rotation, and pelvic drop. While typically reserved for elite athletes or highly refractory cases in specialized centers, this data provides objective metrics to guide the physical therapy rehabilitation protocol, shifting the focus from isolated knee treatments to comprehensive kinetic chain optimization.
Exhaustive Differential Diagnosis
Differentiating Anterior Knee Pain Syndromes
The differential diagnosis for anterior knee pain in a young, active female is broad and requires precise clinical differentiation. While Patellofemoral Pain Syndrome (PFPS) is the most common etiology, it is often a diagnosis of exclusion.
Osgood-Schlatter disease, an apophysitis of the tibial tubercle, is common in adolescents but highly unlikely in a skeletally mature 22-year-old. Femoral or patellar stress fractures must be considered in runners who rapidly increase their mileage or intensity, particularly those with the female athlete triad (energy deficiency, menstrual disturbances, decreased bone mineral density). However, stress fractures typically present with unremitting pain that occurs with weight-bearing and persists at rest, unlike the mechanical, activity-dependent pain seen in this patient.
Meniscal tears, particularly of the anterior horns, can cause localized anterior joint line pain. However, meniscal pathology is usually associated with a specific twisting injury, joint line tenderness, mechanical locking, and a positive McMurray's test—all of which are absent here. Similarly, an ACL rupture presents with a history of a distinct traumatic event (often a non-contact deceleration and pivoting injury), an audible "pop," acute hemarthrosis, and gross instability (positive Lachman and pivot-shift tests).
The evolution of the patient's symptoms at the three-month mark strongly points toward Medial Plica Syndrome. The synovial plica is an embryological remnant of the synovial septa. When subjected to repetitive friction from patellar maltracking or altered kinematics, it becomes inflamed, fibrotic, and thickened, acting like a bowstring across the medial femoral condyle and causing localized pain and mechanical snapping.
Markdown Table: Differential Diagnosis of Anterior Knee Pain
| Pathology | Key Historical Feature | Hallmark Clinical Exam Finding | Diagnostic Imaging Hallmark |
|---|---|---|---|
| Patellofemoral Pain Syndrome | Insidious onset, pain with stairs/sitting | Positive theater sign, lateral patellar tracking | Lateral tilt on Merchant view, normal TT-TG |
| Medial Plica Syndrome | Medial snapping/catching with flexion | Palpable fibrotic band over medial condyle | Thickened plica on axial T2 MRI |
| Osgood-Schlatter Disease | Adolescent jumping athlete | Exquisite tenderness at tibial tubercle | Fragmentation of tibial tubercle apophysis |
| Patellar Tendinopathy | Pain localized to inferior patellar pole | Tenderness at the tendon origin (jumper's knee) | Thickened tendon with increased signal on MRI |
| Femoral Stress Fracture | Rapid increase in training volume, pain at rest | Pain with fulcrum test, deep thigh/knee ache | Bone marrow edema or fracture line on MRI |
| Meniscal Tear | Twisting injury, mechanical locking | Joint line tenderness, positive McMurray's | High signal extending to articular surface on MRI |
Complex Surgical Decision Making and Classifications
Non-Operative Paradigm as the Gold Standard
The foundational tenet of managing anterior knee pain, including PFPS and symptomatic plica syndromes, is that non-operative management is the absolute gold standard. Surgery is rarely indicated as a first-line treatment. The initial phase of treatment correctly focused on activity modification (reducing running volume, eliminating hill training), NSAIDs, and physical therapy.
However, the question arises: why did this patient fail her initial conservative management? The answer lies in the title of our Grand Rounds: "Solve Sports Medicine Cases: Uncover Why the Correct Answer Is E."
Consider this high-yield board-style question that often perplexes residents:
In a patient with refractory patellofemoral pain, dynamic valgus, and recurrent medial plica irritation who has failed 6 months of isolated quadriceps strengthening, what is the most critical overlooked biomechanical intervention required to achieve long-term resolution?
A. Lateral retinacular release
B. Tibial tubercle anteromedialization (Fulkerson osteotomy)
C. Intra-articular corticosteroid injection
D. Isolated open kinetic chain hamstring strengthening
E. Proximal kinetic chain optimization targeting the gluteus medius and external hip rotators
The correct answer is E. The failure of her initial therapy was likely due to a myopic focus on the VMO and the knee joint itself, neglecting the proximal drivers of her malalignment. The hip dictates the knee. Without addressing the hip abductor weakness and dynamic valgus, the femur continues to internally rotate beneath the patella, perpetuating the lateral tracking and plica irritation.
Indications for Operative Intervention in Refractory Cases
Despite a revised, comprehensive physical therapy program focusing on the proximal kinetic chain (Answer E), a small subset of patients will remain highly symptomatic due to irreversible fibrotic changes in the medial plica or established chondral defects. Operative intervention is considered only after a minimum of 6 to 9 months of dedicated, supervised, and mechanically sound physical therapy has failed to provide relief.
In this patient, the presence of a palpable, mechanical snapping plica that prevents her from participating in her sport, combined with MRI evidence of early chondromalacia, constitutes a reasonable indication for arthroscopic evaluation and intervention. The surgical goals are straightforward: remove the mechanical irritant (the plica), address any unstable chondral flaps, and assess dynamic patellar tracking under direct visualization.
Classification Systems for Patellofemoral Tracking
When evaluating patellofemoral pathology, several classification systems guide surgical decision-making. The Sakakibara classification is used to grade synovial plicae based on arthroscopic appearance:
* Type A: A mere cord-like elevation in the synovial wall.
* Type B: A shelf-like appearance but does not cover the anterior surface of the medial femoral condyle.
* Type C: A large, shelf-like plica that covers the anterior surface of the medial femoral condyle (most likely to be symptomatic).
* Type D: A plica with a central defect or fenestration.
Additionally, the Dejour classification of trochlear dysplasia evaluates the bony morphology of the trochlea on true lateral radiographs and axial CT/MRI scans. While our patient does not exhibit severe dysplasia, understanding these classifications is paramount for the orthopedic surgeon to differentiate between soft-tissue driven maltracking (amenable to soft tissue balancing/therapy) and bony driven maltracking (requiring complex osteotomies).
Step-by-Step Surgical Technique and Intervention
Rationale for Arthroscopic Evaluation and Medial Plica Excision
The patient is taken to the operating room for a right knee diagnostic arthroscopy, medial plica excision, and possible lateral retinacular lengthening. The procedure is performed under general anesthesia with a proximal thigh tourniquet. Standard anterolateral and anteromedial portals are established.
The initial diagnostic sweep confirms a normal anterior cruciate ligament, intact menisci, and normal articular cartilage in the tibiofemoral compartments. Attention is then turned to the patellofemoral compartment. A thick, fibrotic Type C medial synovial plica is identified extending from the medial capsule and impinging heavily on the medial femoral condyle during dynamic flexion of the knee from 30 to 70 degrees.
Using an arthroscopic punch and a motorized shaver, the plica is meticulously resected back to its synovial base. It is critical to resect the entire fibrotic band to prevent recurrence, utilizing a radiofrequency wand to maintain hemostasis and ablate any remaining reactive synovium.
Lateral Retinacular Lengthening versus Release
Following plica excision, patellar tracking is evaluated dynamically. The arthroscope is placed in the superolateral portal to view the PFJ from above. As the knee is flexed, the patella is noted to have a persistent lateral tilt, though it centralizes by 40 degrees of flexion.
Historically, an isolated lateral retinacular release was a common procedure for anterior knee pain. However, modern orthopedic literature has heavily condemned the isolated lateral release due to the high risk of iatrogenic medial patellar instability and hemarthrosis. Instead, if the lateral retinaculum is structurally tight and causing a fixed tilt, a lateral retinacular lengthening is preferred. In this patient, given the mild nature of the tilt and the primary pathology being the plica, the lateral retinaculum is left intact to preserve the stabilizing function of the lateral patellofemoral ligament. The focus remains on postoperative proximal rehabilitation.
Articular Cartilage Restoration Techniques
Evaluation of the medial patellar facet reveals a 1.5 cm x 1.0 cm area of Grade II/III chondromalacia, corresponding to the area of plica impingement. The cartilage is fibrillated but not exposed down to subchondral bone. A careful mechanical chondroplasty is performed using a motorized shaver to debride the unstable cartilage flaps to stable, vertical margins. The goal is not to remove all abnormal cartilage, but simply to eliminate the loose, fibrillated edges that cause mechanical catching and chemical synovitis. No marrow stimulation techniques (microfracture) are indicated as the subchondral bone plate is intact.
Strict Post-Operative Protocol and Rehabilitation Stages
Phase I: Acute Protection and Activation
Post-operative rehabilitation must be initiated immediately to prevent arthrofibrosis and quadriceps inhibition. Phase I (Weeks 0-2) focuses on controlling inflammation, restoring full passive range of motion, and reactivating the quadriceps. The patient is allowed weight-bearing as tolerated with crutches, utilizing a hinged knee brace locked in extension during ambulation to protect against buckling from quadriceps shutdown.
Cryotherapy and elevation are paramount. Physical therapy emphasizes superior and inferior patellar mobilizations to prevent capsular adhesions. Quadriceps sets, straight leg raises, and ankle pumps are initiated on post-operative day one. The key milestone to progress to Phase II is the ability to perform a straight leg raise without an extensor lag, indicating adequate VMO activation.
Phase II: Strength, Proprioception, and Load Tolerance
Phase II (Weeks 2-6) transitions to restoring functional strength and addressing the proximal kinetic chain deficits that originally precipitated the pathology. Open kinetic chain (OKC) knee extension exercises are strictly limited, particularly between 0 and 45 degrees, as this arc generates the highest patellofemoral joint reaction forces.
Instead, rehabilitation focuses heavily on closed kinetic chain (CKC) exercises, such as mini-squats, leg presses (limited to 0-60 degrees), and wall slides. Crucially, the "Answer E" protocol is heavily enforced: aggressive strengthening of the gluteus medius, gluteus maximus, and hip external rotators using clamshells, lateral band walks, and single-leg Romanian deadlifts. Blood Flow Restriction (BFR) training may be utilized to maximize muscle hypertrophy while minimizing mechanical load on the healing patellofemoral joint.
Phase III: Return to Sport and Plyometric Integration
Phase III (Weeks 6-12+) bridges the gap between basic strength and athletic performance. The patient is a competitive runner, so her return to sport must be meticulously programmed. Plyometric training is introduced to improve neuromuscular control during dynamic deceleration. Drop jumps and single-leg hops are evaluated using video analysis to ensure the absence of dynamic valgus collapse.
A graduated return-to-run program is initiated, beginning with an anti-gravity treadmill or deep-water running to reduce impact forces. She is educated on modifying her running mechanics, specifically increasing her cadence by 5-10% and adopting a midfoot strike pattern, both of which have been biomechanically proven to reduce patellofemoral joint loading. Hill training is strictly prohibited until she can run 5 miles on flat ground completely pain-free.
High-Yield Clinical Pearls and Pitfalls
Diagnostic Pearls
- The Hip Dictates the Knee: Always evaluate the proximal kinetic chain. The knee is often the victim of poor hip biomechanics. A positive Trendelenburg sign or dynamic valgus on a single-leg squat is a massive red flag for proximal weakness.
- Listen to the Story: The evolution of symptoms from diffuse anterior aching to localized, sharp medial catching is the hallmark of a secondary plica syndrome developing from chronic PFPS.
- Merchant View is Mandatory: A standard AP and lateral radiograph will miss subtle patellar tilt and subluxation. Always obtain an axial view (Merchant, Sunrise, or Laurin) to evaluate the patellofemoral articulation.
Management Pitfalls
- The Trap of the Isolated Lateral Release: Never perform an isolated lateral retinacular release for generalized anterior knee pain. It does not correct the underlying maltracking and often leads to catastrophic medial patellar instability.
- Ignoring the Kinetic Chain in Rehab: Prescribing generic "knee physical therapy" is a setup for failure. The prescription must explicitly detail proximal hip strengthening and core stabilization.
- Premature Return to Impact: Allowing a runner to return to hill training before achieving symmetric hip strength and perfect dynamic neuromuscular control will inevitably result in symptom recurrence. Progression must be criteria-based, not strictly time-based.
