Full Question & Answer Text (for Search Engines)
Question 1:
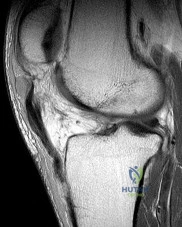
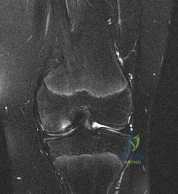
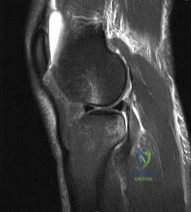
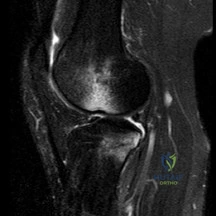
A 45-year-old recreational athlete presents with acute medial knee pain after feeling a 'pop' while deep squatting. MRI demonstrates an extrusion of the medial meniscus of 4 mm and a complete radial tear at the posterior root. Which of the following best describes the primary biomechanical consequence of this specific injury pattern?
Options:
- Increased anterior tibial translation at 30 degrees of knee flexion
- Loss of hoop stresses leading to peak contact pressures equivalent to a total meniscectomy
- Increased varus laxity in full extension
- Decreased contact area restricted primarily to the patellofemoral joint
- Increased shear forces leading directly to a rupture of the anterior cruciate ligament
Correct Answer: Loss of hoop stresses leading to peak contact pressures equivalent to a total meniscectomy
Explanation:
A posterior medial meniscus root tear disrupts the circumferential hoop stresses that the intact meniscus relies on to dissipate axial loads. Biomechanical studies demonstrate that a posterior root tear is functionally equivalent to a total meniscectomy in terms of decreasing contact area and dramatically increasing peak tibiofemoral contact pressures, leading to rapid chondrolysis and osteoarthritis if left untreated.
Question 2:
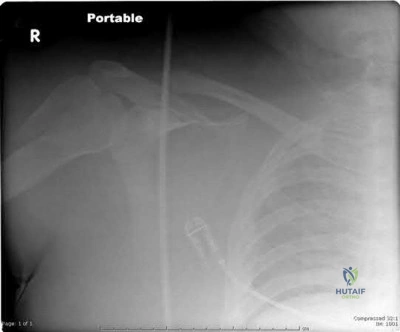
During a Latarjet procedure for recurrent anterior shoulder instability with significant glenoid bone loss, the coracoid process is osteotomized and transferred to the anterior glenoid rim. Which nerve is most at risk of injury due to overzealous medial retraction of the conjoint tendon?
Options:
- Axillary nerve
- Suprascapular nerve
- Musculocutaneous nerve
- Median nerve
- Radial nerve
Correct Answer: Musculocutaneous nerve
Explanation:
The musculocutaneous nerve typically enters the coracobrachialis muscle 3 to 8 cm distal to the tip of the coracoid process. During the Latarjet procedure, aggressive medial retraction of the conjoint tendon can stretch or compress this nerve. The axillary nerve runs inferiorly but is more at risk during capsular release or inferior glenoid preparation.
Question 3:
A 16-year-old female undergoes medial patellofemoral ligament (MPFL) reconstruction for recurrent patellar instability. Intraoperative fluoroscopy is used to determine the anatomic femoral attachment site (Schöttle's point). Which of the following radiographic landmarks correctly identifies this location on a strict lateral radiograph?
Options:
- 2 mm anterior to the posterior cortex line, 5 mm distal to the medial epicondyle, and on Blumensaat's line
- 1 mm anterior to the posterior cortex line, 2.5 mm distal to the posterior origin of the medial femoral condyle, and proximal to Blumensaat's line
- 5 mm posterior to the posterior cortex line, exactly on Blumensaat's line
- Directly over the adductor tubercle, 10 mm proximal to the medial epicondyle
- 1 mm posterior to the posterior cortex line, 5 mm proximal to the medial epicondyle, and distal to Blumensaat's line
Correct Answer: 1 mm anterior to the posterior cortex line, 2.5 mm distal to the posterior origin of the medial femoral condyle, and proximal to Blumensaat's line
Explanation:
Schöttle's point is the radiographic landmark for the femoral origin of the MPFL. On a strict lateral radiograph, it is found 1 mm anterior to a line extending from the posterior femoral cortex, 2.5 mm distal to the posterior articular border of the medial femoral condyle, and proximal to the posterior projection of Blumensaat's line.
Question 4:
A 22-year-old professional baseball pitcher presents with pain during the late cocking and early acceleration phases of throwing. MR arthrography reveals a Type II SLAP tear. What is the widely accepted primary pathomechanical mechanism for this specific injury in overhead throwers?
Options:
- Direct axial loading of the adducted and internally rotated arm
- The 'peel-back' mechanism of the biceps anchor during maximal external rotation and abduction
- Eccentric firing of the biceps brachii during the deceleration phase
- Chronic microtrauma to the inferior glenohumeral ligament (IGHL) causing superior migration of the humeral head
- Traction injury from the triceps during the follow-through phase
Correct Answer: The 'peel-back' mechanism of the biceps anchor during maximal external rotation and abduction
Explanation:
In overhead throwers, the 'peel-back' mechanism occurs during the late cocking phase of throwing when the shoulder is in maximal abduction and external rotation. This position causes a torsional force at the base of the long head of the biceps tendon, peeling the superior labrum off the posterior glenoid rim.
Question 5:
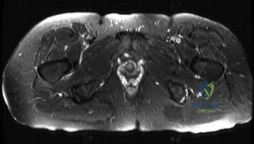
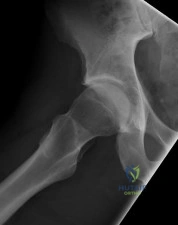
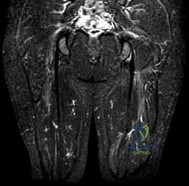
A 24-year-old collegiate hockey player presents with persistent anterior groin pain exacerbated by hip flexion and internal rotation. Radiographs demonstrate an alpha angle of 72 degrees on the Dunn view. Which of the following best describes the primary pathomechanical pattern of chondral damage associated with this morphology?
Options:
- Global full-thickness chondrolysis of the femoral head
- Contrecoup cartilage lesions in the posteroinferior acetabulum due to levering
- Delamination of the anterosuperior acetabular cartilage due to outside-in shear forces
- Crushing of the labrum with secondary ossification of the acetabular rim
- Ligamentum teres avulsion leading to medial joint space narrowing
Correct Answer: Delamination of the anterosuperior acetabular cartilage due to outside-in shear forces
Explanation:
An alpha angle > 55 degrees indicates Cam-type femoroacetabular impingement (FAI). Cam morphology causes outside-in shear forces against the anterosuperior acetabular rim during hip flexion and internal rotation. This selectively damages the transitional zone cartilage, causing delamination of the articular cartilage off the subchondral bone while often leaving the labrum initially intact. Pincer impingement typically causes labral crushing and contrecoup chondral lesions.
Question 6:
During surgical reconstruction of the posterolateral corner (PLC) of the knee, anatomic placement of the fibular collateral ligament (FCL) and popliteus tendon (PT) grafts is critical. What is the precise anatomical relationship of the femoral footprint of the popliteus tendon relative to the FCL femoral footprint?
Options:
- Popliteus originates 18.5 mm anterior and inferior (distal) to the FCL
- Popliteus originates 10 mm posterior and superior (proximal) to the FCL
- Popliteus originates 18.5 mm posterior and inferior (distal) to the FCL
- Popliteus originates directly medial to the FCL within the same footprint
- Popliteus originates 10 mm anterior and superior (proximal) to the FCL
Correct Answer: Popliteus originates 18.5 mm anterior and inferior (distal) to the FCL
Explanation:
The anatomic footprint of the popliteus tendon (PT) on the lateral femoral condyle is located approximately 18.5 mm anterior and inferior (distal) to the footprint of the fibular collateral ligament (FCL). Recognizing this relationship is essential to restore proper biomechanics during anatomic PLC reconstruction.
Question 7:
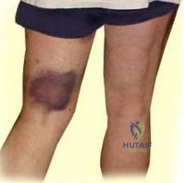
A 30-year-old powerlifter presents with sudden, severe pain and ecchymosis over the anterior axilla after heavy bench pressing. Examination reveals loss of the anterior axillary fold contour and weakness in internal rotation. MRI confirms a rupture of the pectoralis major. Which segment of the pectoralis major is usually the first to rupture, and where does it anatomically insert on the humerus relative to the other segment?
Options:
- Clavicular head; inserts deep and proximal to the sternal head
- Clavicular head; inserts superficial and distal to the sternal head
- Sternal head; inserts deep and proximal to the clavicular head
- Sternal head; inserts superficial and distal to the clavicular head
- Abdominal head; inserts deep and medial to the coracobrachialis
Correct Answer: Sternal head; inserts deep and proximal to the clavicular head
Explanation:
The pectoralis major tendon undergoes a 180-degree twist before inserting onto the lateral lip of the bicipital groove. Because of this twist, the inferior (sternal) head inserts deep and proximal, while the superior (clavicular) head inserts superficial and distal. The sternal head is under maximal tension during eccentric loading with the arm extended and abducted (bench press) and is typically the first segment to tear.
Question 8:
A 21-year-old collegiate runner presents with bilateral exertional leg pain localized to the anterolateral aspect of the lower legs. Pain begins 15 minutes into a run and resolves after 30 minutes of rest. Intracompartmental pressure testing is ordered. According to the Pedowitz criteria, which of the following values confirms the diagnosis of chronic exertional compartment syndrome (CECS)?
Options:
- Pre-exercise resting pressure > 5 mm Hg
- 1-minute post-exercise pressure > 30 mm Hg
- 5-minute post-exercise pressure > 10 mm Hg
- 15-minute post-exercise pressure > 5 mm Hg
- A difference of > 10 mm Hg between the anterior and lateral compartments at rest
Correct Answer: 1-minute post-exercise pressure > 30 mm Hg
Explanation:
The Pedowitz criteria for diagnosing chronic exertional compartment syndrome (CECS) require one or more of the following: 1) Pre-exercise resting pressure ≥ 15 mm Hg; 2) 1-minute post-exercise pressure ≥ 30 mm Hg; or 3) 5-minute post-exercise pressure ≥ 20 mm Hg.
Question 9:
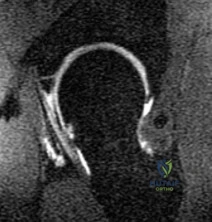
A 27-year-old male sustains an acromioclavicular (AC) joint separation following a fall onto the point of his shoulder. Radiographs demonstrate 150% superior displacement of the clavicle relative to the acromion. Regarding the coracoclavicular (CC) ligaments ruptured in this injury, which statement accurately reflects their anatomy and biomechanical function?
Options:
- The conoid ligament is anterolateral and primarily restrains anterior-posterior translation
- The trapezoid ligament is posteromedial and primarily restrains superior-inferior translation
- The conoid ligament is posteromedial and provides the primary restraint to superior-inferior translation
- The trapezoid ligament is posteromedial and provides the primary restraint to axial compression
- Both ligaments blend together identically to provide equal restraint against posterior translation of the distal clavicle
Correct Answer: The conoid ligament is posteromedial and provides the primary restraint to superior-inferior translation
Explanation:
The coracoclavicular (CC) ligaments consist of the conoid and trapezoid. The conoid ligament is located posteromedial and is the primary restraint to superior translation of the clavicle. The trapezoid ligament is located anterolateral and is the primary restraint to axial compression (resisting medial displacement of the scapula relative to the clavicle).
Question 10:
During arthroscopic evaluation of the shoulder for an overhead athlete, the surgeon encounters an isolated, full-thickness tear of the subscapularis tendon. The 'comma sign' is prominently observed. What specific anatomic structures compose this arthroscopic landmark?
Options:
- The coracoacromial ligament and the long head of the biceps tendon
- The medial edge of the supraspinatus tendon retracting from the greater tuberosity
- The superior glenohumeral ligament (SGHL) and the coracohumeral ligament (CHL)
- The middle glenohumeral ligament (MGHL) and the inferior glenohumeral ligament (IGHL) complex
- The transverse humeral ligament and the superior labrum
Correct Answer: The superior glenohumeral ligament (SGHL) and the coracohumeral ligament (CHL)
Explanation:
The 'comma sign' is a highly reliable arthroscopic indicator of a subscapularis tear. It is formed by the superior glenohumeral ligament (SGHL) and the coracohumeral ligament (CHL), which avulse from their attachments on the lesser tuberosity and retract medially with the superolateral corner of the torn subscapularis tendon, creating a comma-shaped tissue band.
Question 11:
A 25-year-old tennis player presents with posterior shoulder pain during the cocking phase of serving. Exam shows profound Glenohumeral Internal Rotation Deficit (GIRD). MR arthrogram shows articular-sided fraying of the posterior supraspinatus. What is the primary underlying pathomechanism for internal impingement in this athlete?
Options:
- Subacromial spurring causing bursal-sided cuff tearing
- Posteroinferior capsular contracture leading to obligate posterosuperior shift of the humeral head in maximal external rotation
- Anterior capsular laxity resulting in obligate anteroinferior subluxation during external rotation
- Hypertrophy of the coracoacromial ligament impinging the subscapularis
- Congenital glenoid retroversion causing dynamic instability
Correct Answer: Posteroinferior capsular contracture leading to obligate posterosuperior shift of the humeral head in maximal external rotation
Explanation:
Internal impingement is primarily caused by a posteroinferior capsular contracture (associated with GIRD) which creates a dynamic tether. When the arm is brought into maximal abduction and external rotation (late cocking phase), this tether forces an obligate posterosuperior shift of the humeral head, pinching the posterosuperior labrum and the articular surface of the supraspinatus/infraspinatus.
Question 12:
A 32-year-old male suffers an acute mid-substance Achilles tendon rupture playing basketball. He is discussing operative vs. non-operative management. Based on level I evidence comparing modern treatment protocols (e.g., Willits et al.), which of the following is true?
Options:
- Operative treatment significantly decreases the re-rupture rate regardless of the rehabilitation protocol
- Non-operative treatment with early functional rehabilitation yields a statistically similar re-rupture rate to operative repair
- Non-operative management mandates rigid cast immobilization in plantarflexion for 12 weeks to prevent elongation
- Operative treatment is associated with a significantly higher rate of deep vein thrombosis than non-operative treatment
- Non-operative treatment leads to significantly better plantarflexion peak torque at 1 year post-injury
Correct Answer: Non-operative treatment with early functional rehabilitation yields a statistically similar re-rupture rate to operative repair
Explanation:
Multiple Level I randomized controlled trials (such as Willits et al.) have demonstrated that when an early functional rehabilitation protocol (early weight-bearing and early range of motion in a functional brace) is utilized, the re-rupture rate between operative and non-operative groups is statistically similar. Operative treatment has a higher rate of minor complications (like superficial wound infections).
Question 13:
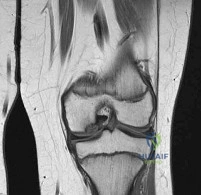
During posterior cruciate ligament (PCL) reconstruction, understanding bundle biomechanics is essential. Which of the following best describes the function and tensioning pattern of the native PCL bundles?
Options:
- The anterolateral bundle is the primary restraint to posterior translation in extension and is lax in flexion
- The posteromedial bundle is the primary restraint to posterior translation at 90 degrees of flexion
- The anterolateral bundle is the primary restraint to posterior translation at 90 degrees of flexion and tightens in flexion
- The posteromedial bundle is the primary restraint to internal rotation at 30 degrees of flexion
- Both bundles are equally tensioned throughout the entire arc of motion
Correct Answer: The anterolateral bundle is the primary restraint to posterior translation at 90 degrees of flexion and tightens in flexion
Explanation:
The PCL consists of the larger anterolateral (AL) bundle and the smaller posteromedial (PM) bundle. The AL bundle is lax in extension and becomes tight in flexion, acting as the primary restraint to posterior tibial translation at 90 degrees of knee flexion. Conversely, the PM bundle is tight in extension and lax in flexion.
Question 14:
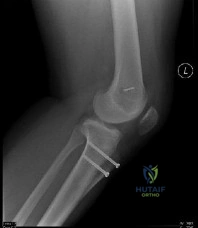
A 23-year-old collegiate basketball player sustains a fracture of the fifth metatarsal at the metaphyseal-diaphyseal junction (Jones fracture). He demands the quickest safe return to play. What is the current standard of care for a competitive athlete with an acute Jones fracture?
Options:
- Non-weight bearing short leg cast for 6 weeks
- Weight-bearing in a stiff-soled boot for 4 weeks
- Percutaneous intramedullary screw fixation
- Open reduction internal fixation with a lateral neutralization plate
- Excision of the proximal fragment and peroneus brevis advancement
Correct Answer: Percutaneous intramedullary screw fixation
Explanation:
Acute Jones fractures (Zone II) in high-level competitive athletes are best treated with intramedullary screw fixation. This approach significantly decreases the time to clinical and radiographic union, decreases the nonunion rate, and allows for a much earlier return to play compared to conservative management.
Question 15:
A 29-year-old overhead athlete presents with vague posterior shoulder pain, weakness in external rotation, and no sensory deficits. MRI reveals isolated atrophy and fatty infiltration of the teres minor. The neurovascular structure most likely compressed in this condition exits through an anatomical space. Which of the following defines the borders of this space?
Options:
- Teres minor (superior), teres major (inferior), long head of triceps (medial), humeral shaft (lateral)
- Teres major (superior), latissimus dorsi (inferior), long head of triceps (lateral), short head of biceps (medial)
- Teres minor (superior), teres major (inferior), long head of triceps (lateral), humeral shaft (medial)
- Supraspinatus (superior), infraspinatus (inferior), spine of scapula (medial), glenoid neck (lateral)
- Subscapularis (superior), teres major (inferior), coracobrachialis (lateral), rib cage (medial)
Correct Answer: Teres minor (superior), teres major (inferior), long head of triceps (medial), humeral shaft (lateral)
Explanation:
The patient has Quadrilateral Space Syndrome, causing compression of the axillary nerve and posterior circumflex humeral artery. This leads to isolated teres minor atrophy. The quadrilateral space is bordered by the teres minor (superior), teres major (inferior), long head of the triceps (medial), and surgical neck of the humerus (lateral).
Question 16:
A 19-year-old football player undergoes primary anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone (BPTB) autograft. In comparing the biomechanical properties of the graft to the native ACL, which of the following statements is true regarding stiffness?
Options:
- The BPTB graft is significantly less stiff than the native ACL
- The BPTB graft has equivalent stiffness to the native ACL
- The BPTB graft is approximately 3 to 4 times stiffer than the native ACL
- A quadrupled hamstring graft is less stiff than the native ACL
- The native ACL is structurally stiffer than all available autograft choices
Correct Answer: The BPTB graft is approximately 3 to 4 times stiffer than the native ACL
Explanation:
The native ACL has a stiffness of approximately 242 N/mm. A 10-mm BPTB graft has a stiffness of approximately 620 N/mm (some studies cite up to 3x, or ~730 N/mm depending on exact width and testing parameters), making it significantly stiffer than the native ACL. A quadrupled hamstring graft is even stiffer, typically around 800 N/mm.
Question 17:
A 28-year-old female presents with lateral 'snapping' of the hip when walking and ascending stairs. The snap is palpable over the greater trochanter and reproduced when moving the hip from flexion to extension. A diagnosis of external snapping hip syndrome is made. If conservative management fails, surgical release of which structure is most indicated?
Options:
- Iliopsoas tendon
- Iliotibial (IT) band
- Rectus femoris
- Gluteus medius tendon
- Ligamentum teres
Correct Answer: Iliotibial (IT) band
Explanation:
External snapping hip (coxa saltans externa) is caused by the iliotibial (IT) band or the anterior border of the gluteus maximus snapping over the greater trochanter during hip flexion and extension. Internal snapping hip is caused by the iliopsoas tendon snapping over the iliopectineal eminence or the femoral head.
Question 18:
A 24-year-old professional baseball pitcher requires ulnar collateral ligament (UCL) reconstruction (Tommy John surgery). During the procedure, the surgeon aims to reconstruct the primary restraint to valgus stress at the elbow. Which specific band of the UCL complex is the most critical to reconstruct?
Options:
- Posterior bundle
- Transverse ligament (Cooper's ligament)
- Anterior band of the anterior bundle
- Posterior band of the anterior bundle
- Radial collateral ligament
Correct Answer: Anterior band of the anterior bundle
Explanation:
The anterior bundle of the UCL is the primary restraint to valgus stress at the elbow from 30 to 120 degrees of flexion. It is subdivided into the anterior and posterior bands. The anterior band is the primary restraint to valgus stress at lower angles of flexion (up to 90 degrees) and is the most critical component to reconstruct in overhead throwers.
Question 19:
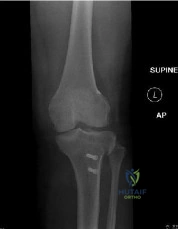
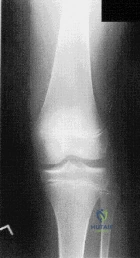
A 15-year-old male presents with chronic knee pain. MRI reveals a stable Osteochondritis Dissecans (OCD) lesion of the knee. Which of the following anatomic locations is the classic and most common site for an OCD lesion in the knee?
Options:
- Lateral aspect of the medial femoral condyle
- Medial aspect of the medial femoral condyle
- Central weight-bearing surface of the lateral femoral condyle
- Posterior aspect of the lateral tibial plateau
- Inferior pole of the patella
Correct Answer: Lateral aspect of the medial femoral condyle
Explanation:
The classic and most common location for an osteochondritis dissecans (OCD) lesion in the knee is the lateral aspect of the medial femoral condyle (often remembered by the mnemonic 'LAME': Lateral Aspect Medial Epicondyle/Condyle). It accounts for approximately 70-80% of knee OCD lesions.
Question 20:
A 40-year-old active female undergoes hip arthroscopy for labral repair. Postoperatively, she reports numbness in the perineal region and labia majora. Which of the following intraoperative factors is most highly associated with this complication?
Options:
- Use of an undersized perineal post
- Application of traction force exceeding 150 lbs
- Traction time exceeding 2 hours
- Fluid extravasation into the retroperitoneal space
- Placement of the anterolateral portal too close to the ASIS
Correct Answer: Traction time exceeding 2 hours
Explanation:
Pudendal neuropraxia is a known complication of hip arthroscopy, typically resulting from compression against the perineal post during traction. The risk significantly increases with prolonged traction time (generally recommended to be kept under 2 hours or completely released if longer time is needed) and the use of an oversized or unpadded perineal post.