Introduction & Epidemiology
Medial elbow pain in the skeletally immature overhead throwing athlete, colloquially known as "Little League Elbow" (LLE), represents a spectrum of pathologies primarily affecting the developing medial epicondyle physis and associated soft tissues. While the term "Little League Elbow" most commonly refers to medial epicondyle apophysitis, it frequently encompasses more severe conditions such as medial epicondyle avulsion fractures and ulnar collateral ligament (UCL) injuries, which are also caused by repetitive valgus stress.
The incidence of LLE and related throwing injuries in youth athletes has been a growing concern, driven by increased participation in organized sports, early single-sport specialization, and year-round competition. Epidemiological studies indicate that medial epicondyle apophysitis is the most common diagnosis, with rates varying depending on the study population and diagnostic criteria. For instance, surveys among youth baseball players report medial elbow pain in up to 20-50% of athletes, with a significant proportion attributable to LLE.
Key risk factors for the development of LLE pathologies include:
*
Age and Skeletal Immaturity:
The medial epicondyle physis is particularly vulnerable during periods of rapid growth due to its cartilaginous composition and relatively weak attachment compared to the surrounding bone and tendons. Fusion typically occurs between 14-16 years of age.
*
Repetitive Overhead Throwing:
The sheer volume and intensity of throwing, particularly high-velocity pitches, are paramount contributors.
*
Pitch Count and Rest:
Lack of adherence to established pitch count limits and insufficient rest periods between throwing sessions and seasons significantly increase injury risk.
*
Poor Throwing Mechanics:
Inefficient or faulty mechanics can exacerbate valgus stress on the medial elbow.
*
Pitch Type:
Throwing curveballs and sliders at a young age, particularly before skeletal maturity, is often implicated in increased medial elbow stress.
*
Fatigue:
Cumulative fatigue can lead to a breakdown in throwing mechanics, placing greater stress on vulnerable structures.
*
Upper Extremity Strength and Flexibility Deficits:
Weakness in the shoulder girdle, core, or inflexibility can contribute to altered biomechanics.
Understanding the progression from simple apophysitis to avulsion fractures and UCL injuries is critical for timely diagnosis and appropriate management, especially given the potential long-term implications for a young athlete's career and elbow health.
Surgical Anatomy & Biomechanics
A thorough understanding of the medial elbow's complex anatomy and its biomechanical response to throwing is fundamental to diagnosing and treating LLE pathologies.
Medial Elbow Anatomy
The medial epicondyle serves as the primary origin for the flexor-pronator mass (FPM) and the anterior bundle of the ulnar collateral ligament (aUCL), both critical stabilizers against valgus stress.
- Medial Epicondyle Physis: This cartilaginous growth plate is the weakest link in the medial elbow complex in skeletally immature athletes. It provides the attachment site for the FPM, which includes the pronator teres, flexor carpi radialis, palmaris longus, flexor digitorum superficialis, and flexor carpi ulnaris. The anterior bundle of the UCL also originates proximally from this region. Its vulnerability to repetitive tensile stress makes it susceptible to apophysitis, stress reactions, and avulsion fractures.
-
Ulnar Collateral Ligament (UCL):
The main static stabilizer of the elbow against valgus stress. It comprises three distinct bundles:
- Anterior Bundle (aUCL): The strongest and most important stabilizer, taut throughout the entire range of motion, with anterior fibers taut in extension and posterior fibers taut in flexion. It originates from the anterior-inferior aspect of the medial epicondyle and inserts onto the sublime tubercle of the ulna. This bundle is most susceptible to injury in overhead throwing athletes.
- Posterior Bundle: Thicker and fan-shaped, originating from the posterior aspect of the medial epicondyle and inserting onto the medial olecranon. It is taut primarily in flexion.
- Transverse Bundle (Cooper's ligament): Connects the olecranon to the coronoid, providing minimal valgus stability.
- Flexor-Pronator Mass (FPM): Originating predominantly from the medial epicondyle, these muscles dynamically stabilize the medial elbow. Their contracture during throwing helps resist valgus forces.
- Ulnar Nerve: The ulnar nerve courses through the cubital tunnel, located posterior to the medial epicondyle, between the two heads of the flexor carpi ulnaris. It is vulnerable to traction injury, compression, or direct trauma, especially in cases of medial epicondyle avulsion fractures or post-surgical scarring. Its proximity necessitates careful identification and protection during any medial elbow surgical procedure.
Biomechanics of Overhead Throwing
The overhead throwing motion is a highly kinetic chain event that imposes immense forces on the elbow. The critical phase for medial elbow injury is the late cocking and early acceleration phase , where maximal valgus stress is generated.
- Valgus Stress: As the arm moves from maximal external rotation in late cocking into acceleration, a tremendous valgus torque is applied to the elbow. This torque generates significant tensile forces across the medial elbow compartment, specifically on the medial epicondyle physis and the UCL. The FPM musculature attempts to counteract this valgus moment dynamically.
- Tensile Forces: Repetitive tensile loading on the medial epicondyle physis can lead to inflammation (apophysitis), stress fractures, or frank avulsion of the physis due to the pull of the FPM and UCL origin. Similarly, the UCL experiences high tensile forces, which can result in microtears, sprains, or complete rupture.
- Compressive Forces: Concurrently, compressive forces are generated on the lateral compartment, which can lead to osteochondral lesions of the capitellum (e.g., Panner's disease or osteochondritis dissecans), a common differential diagnosis for elbow pain in throwers, though distinct from LLE proper.
- Shear Forces: Posterior shear forces also occur, which can predispose to olecranon stress fractures or apophysitis.
The repetitive nature of throwing, coupled with peak forces that can exceed the tensile strength of the young athlete's developing bone and ligamentous structures, creates a fertile ground for the development of LLE pathologies.
Indications & Contraindications
The management of medial elbow pathologies in the skeletally immature athlete ranges from conservative measures to complex surgical interventions. The decision-making process hinges on precise diagnosis, the severity of injury, patient skeletal maturity, activity level, and expectations for return to sport.
Non-Operative Indications
Non-operative management is the cornerstone for the majority of LLE presentations, particularly in skeletally immature athletes.
-
Medial Epicondyle Apophysitis (Classic LLE):
This is the most common presentation.
- Uncomplicated apophysitis without significant physeal widening or displacement on imaging.
- Pain localized to the medial epicondyle, exacerbated by throwing, but typically without mechanical symptoms or gross instability.
- Absence of significant ulnar nerve symptoms.
- Patients willing and able to comply with a structured rest and rehabilitation program.
-
Undisplaced Medial Epicondyle Avulsion Fractures:
- Fractures with minimal displacement (<2 mm) and no intra-articular entrapment of the fragment or associated soft tissues.
- Clinically stable elbow on valgus stress testing.
- No signs of ulnar nerve compromise.
-
Ulnar Collateral Ligament (UCL) Sprains (Grade I/II):
- Partial tears of the UCL with a stable elbow on valgus stress testing.
- Symptoms resolving with rest and targeted physical therapy.
- Considered for athletes not intending to return to high-level overhead throwing.
-
Mild Ulnar Neuropathy:
- Intermittent or mild paresthesias in the ulnar nerve distribution without motor weakness or significant activity limitation.
- Absence of a clearly identifiable anatomical compression requiring surgical release.
Operative Indications
Surgical intervention is reserved for specific conditions where non-operative management has failed or where the nature of the injury dictates an immediate surgical approach to restore function and prevent long-term sequelae.
-
Displaced Medial Epicondyle Avulsion Fractures:
- Displacement greater than 2-3 mm (some sources use 5 mm as a threshold, but 2-3 mm is often cited for younger athletes).
- Intra-articular entrapment of the fracture fragment (often seen as a "coin-in-the-joint" sign on radiographs).
- Associated ulnar nerve compromise (e.g., nerve entrapment within the fracture site or acute, severe ulnar neuropathy).
- Open fractures.
- Symptomatic nonunion after a trial of conservative care, particularly in older adolescents or skeletally mature individuals.
-
Ulnar Collateral Ligament (UCL) Rupture (Grade III) or Chronic Instability:
- Complete rupture of the UCL, particularly in high-level overhead throwing athletes who desire to return to competitive play.
- Symptomatic chronic Grade II sprains with persistent valgus instability despite comprehensive non-operative management (typically >3-6 months).
- Young athletes approaching skeletal maturity with significant UCL laxity and functional limitations.
-
Persistent Ulnar Neuropathy:
- Ulnar nerve symptoms that are severe, progressive, or fail to resolve with non-operative measures, especially if related to anatomical compression (e.g., within the cubital tunnel or due to fracture fragments).
- Motor weakness in the ulnar nerve distribution.
Contraindications
General medical contraindications to surgery apply (e.g., acute infection, uncontrolled systemic disease). Specific orthopedic contraindications related to LLE include:
* Unwillingness or inability to comply with the rigorous post-operative rehabilitation protocol.
* Acute infection at the surgical site.
* Severe underlying medical comorbidities precluding safe anesthesia and surgery.
* For UCL reconstruction, patients who do not intend to return to high-level overhead throwing may be managed non-operatively, given the inherent risks and extensive rehabilitation.
Operative vs. Non-Operative Indications
| Condition / Pathophysiology | Non-Operative Management | Operative Management |
|---|---|---|
| Medial Epicondyle Apophysitis (LLE) | First-line treatment: Activity modification, complete cessation of throwing, NSAIDs, physical therapy focusing on pain management, restoring ROM, strengthening core and shoulder musculature, and correcting throwing mechanics. Gradual return to activity. | Rarely indicated for isolated apophysitis. Consideration only for persistent, debilitating symptoms refractory to >6-12 months of conservative care, potentially involving debridement of hypertrophic tissue or fragment excision (rare). |
| Medial Epicondyle Avulsion Fracture | Undisplaced (<2-3mm displacement), non-intra-articular, no ulnar nerve compromise: Sling immobilization for 2-4 weeks, gentle active/passive ROM, progressive strengthening. | Displaced (>2-3mm displacement), intra-articular entrapment, ulnar nerve symptoms, open fracture, or symptomatic nonunion: Open Reduction Internal Fixation (ORIF) with K-wires, screws, or tension band wiring. |
| UCL Sprain (Grade I/II) | Rest, short-term bracing for comfort, gradual progressive physical therapy addressing strength, stability, and biomechanics. Gradual throwing progression. | Chronic, symptomatic Grade II sprain refractory to conservative management (typically >3-6 months) in high-level throwers: UCL primary repair (in select cases of acute avulsion) or reconstruction (Tommy John surgery). |
| UCL Rupture (Grade III) | Selected cases in non-throwing athletes, low-demand athletes, or those not desiring return to high-level overhead throwing. | Acute, symptomatic Grade III rupture in throwing athletes desiring return to high-level sport: UCL reconstruction (Tommy John surgery). Primary repair may be considered for acute, proximal avulsions with good tissue quality. |
| Ulnar Neuropathy (in LLE context) | Mild, intermittent symptoms. Rest, activity modification, splinting, nerve gliding exercises, NSAIDs. | Persistent or worsening symptoms, motor weakness, anatomical compression (e.g., by fracture fragment, hypertrophic tissue). Ulnar nerve decompression, often with anterior transposition (subcutaneous or submuscular) depending on specific pathology and surgeon preference. |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is paramount for successful outcomes and minimizing complications in medial elbow surgery.
Pre-operative Imaging
- Plain Radiographs: AP, lateral, and oblique views of the elbow are standard. Bilateral radiographs, including a contralateral comparison, are often crucial for assessing physeal width and morphology in the skeletally immature patient. Stress radiographs (e.g., valgus stress view) can be performed to assess UCL laxity, although findings can be difficult to interpret in the acute setting due to pain and guarding.
-
Magnetic Resonance Imaging (MRI):
The gold standard for soft tissue evaluation. An MRI with and without contrast (gadolinium) is essential for:
- Assessing UCL integrity (identifying full-thickness tears, partial tears, or chronic attenuation).
- Evaluating the medial epicondyle physis for edema, stress reactions, or non-displaced avulsion fractures.
- Identifying other associated injuries such as osteochondritis dissecans of the capitellum, flexor-pronator muscle strains, or ulnar nerve pathology.
- Computed Tomography (CT) Scan: Indicated for complex or comminuted medial epicondyle avulsion fractures to delineate fragment size, displacement, and intra-articular extension more precisely, particularly when planning for Open Reduction Internal Fixation (ORIF).
- Nerve Conduction Studies/Electromyography (NCS/EMG): May be considered in cases of suspected chronic ulnar neuropathy to assess nerve function and localize the site of compression.
Patient Education
Comprehensive discussion with the patient and their family regarding the diagnosis, treatment options (surgical vs. non-surgical), potential risks and benefits of surgery, expected recovery timeline, and the demanding nature of post-operative rehabilitation is crucial for setting realistic expectations and ensuring compliance.
Anesthesia
General anesthesia is typically employed, often supplemented with a regional anesthetic block (e.g., interscalene block or supraclavicular block) for excellent post-operative analgesia.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Arm Board/Hand Table: The affected arm is abducted approximately 90 degrees and externally rotated, placed on a radiolucent hand table. This provides unrestricted access to the medial aspect of the elbow.
- Shoulder Position: Ensure the shoulder is supported and not excessively abducted or externally rotated to prevent brachial plexus strain.
- Tourniquet: A pneumatic tourniquet is applied high on the arm to maintain a bloodless field, typically inflated to 250-300 mmHg or 100 mmHg above systolic pressure.
- Ulnar Nerve Protection: Meticulous padding of all bony prominences, especially the contralateral elbow and heel, is critical. The ulnar nerve in the operative arm should be carefully protected throughout positioning.
- Sterile Preparation and Draping: The surgical field extends from the shoulder to the hand, ensuring adequate exposure for graft harvest if UCL reconstruction is planned (e.g., palmaris longus or hamstring autograft).
Detailed Surgical Approach / Technique
Surgical intervention for Little League Elbow pathologies primarily involves Open Reduction Internal Fixation (ORIF) for displaced medial epicondyle avulsion fractures or Ulnar Collateral Ligament (UCL) reconstruction for symptomatic instability. Ulnar nerve management is often a concomitant procedure.
General Principles
- Meticulous soft tissue handling to minimize devascularization and scarring.
- Prioritize ulnar nerve protection throughout the entire procedure.
- Achieve stable, anatomic reduction and fixation.
- Respect physeal plates in skeletally immature patients.
Medial Epicondyle Avulsion Fracture ORIF
This procedure focuses on reducing the avulsed medial epicondyle fragment and securing it back to its anatomical position.
- Incision: A longitudinal or slightly oblique incision is made over the medial epicondyle, approximately 5-7 cm in length. It should be centered over the medial epicondyle and extend distally enough to allow for ulnar nerve identification and proximal enough for good exposure.
-
Dissection:
- Skin and Subcutaneous Tissues: Incise the skin and subcutaneous fat.
- Medial Antebrachial Cutaneous Nerve (MABCN): Identify and protect branches of the MABCN, which typically cross the field. Careful blunt dissection can help avoid injury.
- Ulnar Nerve Identification: This is a crucial step. The ulnar nerve is identified in the cubital tunnel, posterior to the medial epicondyle. It is carefully mobilized from the cubital tunnel and retracted anteriorly. Depending on the extent of fracture displacement and surgeon preference, or if there is pre-existing ulnar nerve compromise, an anterior ulnar nerve transposition (subcutaneous or submuscular) may be performed at this stage. If transposition is not planned, the nerve must be protected with a vessel loop or Penrose drain throughout the case.
- Flexor-Pronator Mass (FPM) Origin: The avulsed fragment often has the FPM and UCL attached. Carefully dissect around the fragment. If the fragment is large and displaced, partial release of the FPM origin may be necessary to visualize the fracture bed and achieve reduction. The specific approach to the FPM can vary: some surgeons will split the FPM longitudinally, others will detach a portion from its origin for better exposure, which will then be repaired.
-
Reduction:
- Once the fragment is exposed, identify the fracture bed on the humerus.
- The fragment is typically pulled distally and anteriorly by the FPM. Gentle traction on the forearm (in valgus) can help reduce the fragment back to its anatomical position.
- Direct manipulation with a small periosteal elevator or a blunt hook can aid in achieving an anatomical reduction.
-
Verify reduction visually and by palpation. Provisional fixation is achieved with one or two small K-wires (e.g., 0.045-0.062 inches). Ensure the K-wires are not inadvertently placed into the joint or across the physis if growth plate preservation is critical.
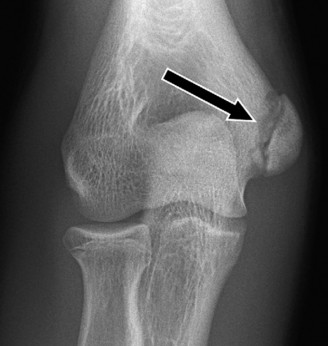
Note: The image above could illustrate the medial elbow anatomy with the medial epicondyle physis and UCL, or perhaps a radiograph depicting a displaced avulsion fracture, providing a visual reference for the anatomical context of the discussion.
-
Fixation:
- K-wires: For very small fragments or in younger patients where physeal preservation is paramount, smooth K-wires (typically two, divergent) can be used. They are usually left proud and removed 3-6 weeks post-operatively.
- Screws: The most common method. Small cannulated screws (e.g., 2.0 mm, 2.7 mm, or 3.5 mm cortical screws) are placed across the fracture site, perpendicular to the fracture plane if possible, to achieve interfragmentary compression. Care must be taken to avoid violating the articular surface or the physis unnecessarily. If the physis is open, small screws can be placed across the physis, but this should be done with caution to minimize growth disturbance.
- Tension Band Wiring: May be considered for comminuted fragments or if strong compression is desired, particularly in older adolescents with more robust bone quality.
- Confirm stability and ensure hardware does not impinge on the ulnar nerve or joint.
-
Closure:
- Reattach any detached portions of the FPM.
- Ensure the ulnar nerve is in a stable, decompressed position.
- Layered closure of the subcutaneous tissues and skin.
Ulnar Collateral Ligament (UCL) Reconstruction (Tommy John Surgery)
This procedure involves replacing the damaged UCL with an autograft tendon.
- Incision: A longitudinal incision approximately 8-10 cm in length is made over the medial aspect of the elbow, centered on the medial epicondyle.
-
Ulnar Nerve Management:
- Identify the ulnar nerve in the cubital tunnel. Mobilize it proximally and distally to ensure adequate decompression.
- Anterior Transposition: In most cases, the ulnar nerve is transposed anteriorly (subcutaneously or submuscularly) to prevent post-operative irritation or re-entrapment due to swelling, scarring, or anatomical changes from the UCL reconstruction itself. Submuscular transposition, underneath the FPM, offers excellent protection but is more technically demanding.
-
Harvest Autograft:
- The most common autograft is the palmaris longus tendon (if present and of adequate size), harvested via a separate distal forearm incision.
- Other options include ipsilateral or contralateral gracilis, semitendinosus, or occasionally toe extensors.
- Prepare the graft by removing muscle tissue and sizing it for the reconstruction technique.
-
Exposure of UCL and Native Footprints:
- The flexor-pronator mass is either split longitudinally or partially detached from its origin to expose the remnants of the native UCL and its attachment sites.
- The humeral origin (anterior-inferior medial epicondyle) and ulnar insertion (sublime tubercle) of the anterior bundle are identified. These are the isometric points for graft placement.
-
Drilling Bone Tunnels (Docking Technique - common example):
- Ulnar Tunnels: Two divergent bone tunnels are drilled into the sublime tubercle of the ulna. A small trough may be created between them. The tunnels should be sized appropriately for the graft limbs.
- Humeral Tunnel: A single central humeral tunnel is drilled from the isometric point on the medial epicondyle, through the medial condyle, exiting laterally. Then, two smaller divergent docking holes are drilled from the medial epicondyle to connect to the central tunnel.
- The tunnels must be positioned accurately to ensure isometric graft placement and avoid neurovascular structures. Guide pins and fluoroscopy can be used to confirm tunnel placement.
-
Graft Passage and Tensioning:
- The graft is passed through the humeral tunnel (central hole), creating two limbs.
- Each limb is then passed into one of the ulnar tunnels.
- The elbow is flexed to 30-70 degrees and the forearm pronated. This position is considered isometric for the UCL.
- The graft is then tensioned firmly and secured. For the docking technique, the graft limbs exiting the ulnar tunnels are sutured to each other over a bone bridge, and the proximal end is secured by suturing the two limbs within the humeral tunnel, often with non-absorbable sutures.
- Variations exist (e.g., Interference screws, cortical button fixation for one or both ends).
- Stability Assessment: The elbow's valgus stability is assessed throughout the range of motion.
-
Closure:
- The FPM is meticulously repaired over the reconstructed ligament.
- The ulnar nerve is positioned appropriately (if transposed).
- Layered closure of the subcutaneous tissues and skin.
Complications & Management
Despite meticulous surgical technique and comprehensive pre-operative planning, complications can occur following medial elbow surgery for LLE pathologies. Awareness of these potential issues and their management strategies is critical.
Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (%) | Salvage / Management Strategy |
|---|---|---|
| Ulnar Neuropathy | 5-20 |
Mild (paresthesias, dysesthesias):
Observation, NSAIDs, activity modification, nerve gliding exercises.
Persistent/Severe (motor weakness, intractable pain): Surgical exploration, neurolysis, ulnar nerve decompression, +/- anterior transposition if not already performed. Revision surgery if entrapment identified. |
| Infection | <1-5 |
Superficial:
Oral antibiotics, local wound care.
Deep (osteomyelitis, septic arthritis): Aggressive surgical debridement, IV antibiotics tailored to culture sensitivities. Hardware removal may be required, especially in chronic cases. |
| Nonunion / Malunion (Avulsion Fx) | 5-15 |
Symptomatic nonunion:
Revision ORIF with bone grafting (autograft or allograft), potentially with more robust fixation.
Symptomatic malunion (angular deformity, impingement): Corrective osteotomy. Asymptomatic malunion often managed conservatively. |
| Hardware Irritation / Prominence | 5-10 | Symptomatic: Hardware removal once fracture healing is confirmed (typically 6-12 months post-op). Asymptomatic hardware generally left in situ. |
| Stiffness / Loss of Range of Motion | 10-25 |
Mild to Moderate:
Aggressive physical therapy, stretching, dynamic splinting.
Severe / Refractory: Surgical capsular release (arthroscopic or open) for contracture. |
| Re-injury / Graft Failure (UCL) | 5-10 |
Minor re-sprains:
Non-operative management, rest, rehabilitation.
Symptomatic graft failure (instability, pain): Revision UCL reconstruction. Often involves a different graft source or technique due to scarred tissue. |
| Physeal Arrest / Growth Disturbance | <1-5 |
Mild:
Observation.
Significant angular deformity or limb length discrepancy: Corrective osteotomy or guided growth procedures (e.g., hemiepiphysiodesis) depending on remaining growth potential. More common with repeated trauma or across-the-physis screw placement. |
| Complex Regional Pain Syndrome (CRPS) | Rare | Multidisciplinary approach: Aggressive physical therapy, pain management specialists (nerve blocks, sympathetic blocks), pharmacotherapy, psychological support. Early recognition is key. |
Additional Complications
- Vascular Injury: Extremely rare, but possible during deep dissection or tunnel drilling. Requires immediate vascular surgery consultation and repair.
- Compartment Syndrome: Very rare in elbow surgery. If suspected, immediate fasciotomy is indicated.
- Heterotopic Ossification (HO): Formation of new bone in soft tissues around the elbow. Prophylaxis with NSAIDs or radiation may be considered in high-risk patients. If symptomatic and limiting ROM, surgical excision may be required once mature.
- Post-operative Pain: Managed with multimodal analgesia (regional blocks, NSAIDs, acetaminophen, opioids). Persistent, severe pain may warrant investigation for other complications.
- Delayed Return to Sport: Even with successful surgery, returning to pre-injury performance levels can be challenging and prolonged, especially for high-level throwing athletes.
- Scarring/Cosmetic Issues: While generally not a functional complication, significant scarring can be a concern for some patients.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself for optimizing outcomes and ensuring a safe return to sport. Protocols vary based on the specific procedure (ORIF vs. UCL reconstruction), surgeon preference, and patient-specific factors, but generally follow a phased approach. The timeline presented here is typical for UCL reconstruction, with adaptations for medial epicondyle ORIF.
General Principles
- Protection of Repair: The primary goal in the early phases is to protect the surgically repaired or reconstructed structures from excessive stress.
- Gradual Progression: Rehabilitation is a progressive process, increasing demands on the elbow as healing advances.
- Pain-Free Motion: All exercises should be performed without pain.
- Kinetic Chain Integration: Rehabilitation must address the entire kinetic chain, including the shoulder girdle, scapular stabilizers, core, and lower extremities.
- Patient Education and Compliance: Strict adherence to the protocol is essential.
Phase I: Immediate Post-operative (Weeks 0-2/4)
Goals:
Protect repair, control pain and swelling, initiate gentle motion in a protected range.
*
Immobilization:
*
UCL Reconstruction:
Typically a posterior splint or hinged elbow brace locked at 30-90 degrees of flexion for 1-2 weeks.
*
Medial Epicondyle ORIF:
Posterior splint for 2-3 weeks, followed by a hinged brace.
*
Pain and Edema Control:
Ice, elevation, analgesics.
*
Early Motion:
* Gentle, active wrist and hand range of motion (ROM).
* Shoulder pendulum exercises and passive/active-assisted ROM for the shoulder (flexion, extension, internal/external rotation within pain limits).
*
Ulnar Nerve Glides:
Initiated if ulnar nerve transposition was performed, ensuring gentle tension.
*
Avoid:
Valgus stress, active elbow flexion against resistance.
Phase II: Early Motion & Protection (Weeks 2/4 - 6/8)
Goals:
Restore full, non-painful elbow ROM, begin gentle strengthening.
*
Brace Progression:
*
UCL Reconstruction:
Transition to a hinged elbow brace, gradually increasing ROM by 10-15 degrees per week. Aim for full extension/flexion by week 6-8.
*
Medial Epicondyle ORIF:
Transition to hinged brace, progress ROM more rapidly towards full flexion/extension as tolerated, typically achieving full ROM by week 4-6 if fixation is stable.
*
Elbow ROM:
Continue active-assisted and active elbow flexion/extension. Forearm pronation/supination.
*
Isometric Strengthening:
* Gentle, pain-free isometrics for biceps, triceps, wrist flexors/extensors.
* Scapular stabilization exercises (e.g., serratus anterior punches, low-level rows).
* Rotator cuff isometrics.
*
Avoid:
Lifting heavy objects, sudden forceful movements, valgus stress.
Phase III: Intermediate Strengthening (Weeks 8 - 16)
Goals:
Restore full strength and endurance of the upper extremity, initiate proprioceptive training.
*
Brace:
Discontinued (UCL Reconstruction by week 8-10, ORIF often earlier).
*
Progressive Strengthening:
*
Elbow:
Concentric and eccentric strengthening for elbow flexors and extensors (light weights, resistance bands).
*
Forearm:
Progressive strengthening for wrist flexors/extensors and pronators/supinators.
*
Shoulder:
Advanced rotator cuff and scapular strengthening (e.g., rows, overhead press, external/internal rotation with bands/weights).
*
Core:
Continue with comprehensive core strengthening.
*
Proprioceptive Drills:
Begin proprioceptive exercises for the elbow and shoulder (e.g., perturbation training, unstable surface exercises).
*
Initiate Light Plyometrics:
Bodyweight plyometric exercises (e.g., medicine ball throws with two hands).
*
Avoid:
Any high-impact or valgus-stress activities involving the elbow.
Phase IV: Advanced Strengthening & Return to Throwing (Months 4-6+)
Goals:
Prepare for sport-specific activities, begin interval throwing program.
*
Maximal Strength and Endurance:
Continue progressive resistance training with increased loads.
*
Power and Agility:
Sport-specific agility drills, advanced plyometrics for the entire kinetic chain.
*
Interval Throwing Program (ITP):
* Gradual, progressive throwing program, beginning with short distances and light effort, advancing incrementally in distance and intensity.
* Focus on mechanics, avoiding pain.
* Throwing off a mound and increasing velocity are the final stages.
*
UCL Reconstruction:
Typically begins around 4-6 months post-op.
*
Medial Epicondyle ORIF:
May begin earlier, around 3-4 months post-op, once bony healing is confirmed by radiographs.
*
Biomechanical Analysis:
Often beneficial to have a coach or therapist analyze throwing mechanics to identify and correct any faults that could contribute to re-injury.
Phase V: Return to Competition (Months 9-12+ for UCL Recon; Variable for ORIF)
Goals:
Full, pain-free return to competitive sport.
*
UCL Reconstruction:
Return to competitive pitching often takes 12-18 months.
*
Medial Epicondyle ORIF:
Return to competitive throwing generally occurs earlier, typically 4-6 months, but depends on fracture healing and pain.
*
Criteria for Return to Play:
* Full, pain-free ROM.
* Strength symmetry (isokinetic testing often used, target >90% strength compared to contralateral limb).
* Successful completion of the entire interval throwing program without pain or symptoms.
* Clearance from both the surgeon and physical therapist.
*
Maintenance Program:
Continue with a structured strength and conditioning program to prevent re-injury. Adherence to pitch count guidelines and adequate rest periods remain critical.
Summary of Key Literature / Guidelines
The understanding and management of Little League Elbow and related medial elbow pathologies in youth throwers have evolved significantly, driven by extensive research and guidelines from prominent orthopedic and sports medicine organizations.
Epidemiology and Risk Factors
- Youth Baseball Injury Surveillance: Studies from organizations like the American Sports Medicine Institute (ASMI) consistently highlight repetitive overhead throwing as the primary etiology. ASMI guidelines, spearheaded by Dr. James Andrews and others, have been instrumental in establishing pitch count limits and mandatory rest periods based on age.
- Pitch Counts and Rest Days: Multiple prospective studies have demonstrated a direct correlation between higher pitch counts, pitching on consecutive days, and pitching for multiple teams concurrently with an increased risk of elbow and shoulder injuries in youth athletes.
- Pitch Type: Throwing breaking pitches (curveballs, sliders) at a young age, particularly prior to skeletal maturity, has been identified as a significant risk factor, as these pitches often impose greater valgus stress and torque on the elbow.
- Fatigue and Inefficient Mechanics: Literature consistently points to fatigue leading to altered throwing mechanics and insufficient strength/conditioning of the kinetic chain (core, glutes, scapular stabilizers) as critical predisposing factors.
Diagnosis
- Clinical Examination: A thorough history and physical examination remain foundational. Key findings include tenderness over the medial epicondyle physis, pain with valgus stress, and sometimes a positive moving valgus stress test for UCL pathology. Assessment of the entire kinetic chain is crucial.
-
Imaging Modalities:
- Radiographs: Essential initial imaging to rule out displaced avulsion fractures, demonstrate physeal widening, or reveal other bony pathologies. Bilateral views are often recommended for comparison.
- MRI: Considered the gold standard for soft tissue evaluation, especially to assess UCL integrity and detailed physeal status (edema, stress reaction). High-resolution MRI has significantly improved diagnostic accuracy for partial and complete UCL tears.
- Ultrasound: Dynamic ultrasound has emerged as a useful, non-invasive tool for assessing UCL integrity and valgus instability, particularly in skilled hands.
Treatment Algorithms
-
Non-Operative Management:
The vast majority of medial epicondyle apophysitis cases and undisplaced avulsion fractures are successfully managed non-operatively.
- Rest: The cornerstone of treatment for apophysitis is cessation of throwing.
- Rehabilitation: Comprehensive physical therapy focusing on pain control, restoring ROM, strengthening the entire kinetic chain, and correcting throwing mechanics is universally recommended.
-
Surgical Indications:
Consensus guidelines support surgical intervention for:
- Displaced Medial Epicondyle Avulsion Fractures: Generally >2-3 mm displacement or intra-articular entrapment. ORIF is the standard.
- Symptomatic UCL Insufficiency: In high-level throwing athletes desiring return to competition, a complete UCL rupture (Grade III) or a chronic, symptomatic Grade II tear refractory to conservative management warrants UCL reconstruction (Tommy John surgery).
- Chronic Ulnar Neuropathy: If conservative measures fail or clear anatomical compression is identified.
Outcomes
- Apophysitis: Outcomes for medial epicondyle apophysitis treated conservatively are excellent, with a high return-to-sport rate when pitch count guidelines are followed and rehabilitation is adhered to.
- Medial Epicondyle ORIF: Generally good outcomes for displaced avulsion fractures following ORIF, with high rates of union and return to sport, often earlier than UCL reconstruction.
- UCL Reconstruction: Modern UCL reconstruction techniques boast successful return-to-sport rates of 80-90% for professional athletes, though return to the same pre-injury performance level can be variable. The rehabilitation period is prolonged (12-18 months).
Prevention
- Pitch Count Guidelines: Adherence to age-specific pitch count and rest day recommendations (e.g., ASMI, USA Baseball) is the most critical preventative measure.
- Delayed Specialization: Encouraging multi-sport participation rather than early single-sport specialization can reduce cumulative stress on specific joints.
- Proper Biomechanics: Coaching to ensure efficient and safe throwing mechanics.
- Strength and Conditioning: Comprehensive programs focusing on core strength, hip mobility, and shoulder girdle stability are vital for force transmission and injury prevention.
- Warm-up and Cool-down: Proper pre- and post-throwing routines.
Key Literature and Guidelines often referenced include:
* American Sports Medicine Institute (ASMI) position statements and research.
* American Academy of Orthopaedic Surgeons (AAOS) clinical practice guidelines.
* American Orthopaedic Society for Sports Medicine (AOSSM) consensus statements.
These resources continually emphasize a proactive approach to prevent LLE, highlighting the importance of physician education, coaching education, and parental awareness in protecting the health of young athletes.
