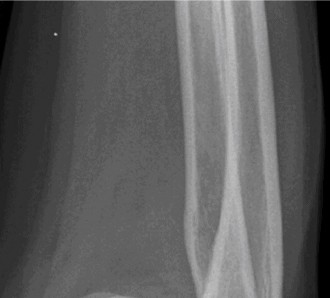
Patient Presentation & History
We present the case of a 44-year-old right-hand dominant male who sustained a high-energy injury following a fall from a height of approximately 3 meters while working on a ladder. He landed directly on his outstretched right upper extremity, sustaining significant force transmission through his hand and forearm to the elbow joint. He presented to the emergency department with acute, severe pain in his right elbow, obvious deformity, and complete inability to move the joint. There was no reported loss of consciousness.
His medical history was unremarkable, with no known chronic conditions, previous surgeries, or allergies. He denied tobacco or illicit drug use, and consumed alcohol socially. His primary occupation involves manual labor, underscoring the critical need for optimal functional recovery of his dominant limb. The mechanism of injury, a Fall On Outstretched Hand (FOOSH) with an axial load component, is highly characteristic for elbow dislocation and associated complex injuries. The severity of the fall suggested a potentially complex injury pattern involving both osseous and ligamentous structures.
Clinical Examination
Upon initial assessment in the emergency department, the patient was alert and in significant distress due, to pain.
Inspection
Gross deformity of the right elbow was immediately apparent. The olecranon was prominently displaced posteriorly, with the forearm appearing shortened relative to the humerus. Significant swelling was evident around the elbow joint, and early ecchymosis was noted, suggestive of substantial soft tissue disruption. No open wounds or skin tenting suggestive of an impending open fracture were observed.
Palpation
Palpation revealed diffuse tenderness across the entire elbow joint. The bony landmarks, specifically the epicondyles and olecranon, were severely disrupted, making the classic triangular relationship difficult to ascertain accurately. The radial head could not be palpated in its normal position, suggesting either dislocation or a fracture with displacement. There was no palpable crepitus, which could be attributed to significant soft tissue tension or displacement preventing bony apposition.
Range of Motion
Active and passive range of motion of the elbow was severely limited and exquisitely painful. The joint was held in approximately 30-40 degrees of flexion, with any attempt at movement eliciting severe guarding and pain. Forearm pronation and supination were also severely restricted.
Neurological/Vascular Assessment
A thorough neurovascular examination was performed given the potential for neurovascular compromise in elbow dislocations.
*
Radial Nerve:
Sensation to the dorsal first web space was intact. Wrist extension and thumb extension were strong (Medical Research Council (MRC) grade 5/5).
*
Median Nerve:
Sensation to the volar tip of the index finger and thumb was intact. Thumb opposition and finger flexion (flexor digitorum profundus to index, flexor pollicis longus) were strong (MRC grade 5/5).
*
Ulnar Nerve:
Sensation to the volar tip of the fifth finger was intact. Finger abduction and adduction were strong (MRC grade 5/5).
*
Vascular Status:
Radial and ulnar pulses were palpable and strong bilaterally. Capillary refill in the digits was brisk (<2 seconds). No signs of compartment syndrome were present in the forearm.
Despite intact neurovascular status, the profound deformity and severe pain necessitated urgent imaging and reduction.
Imaging & Diagnostics
Immediate radiographic evaluation was performed in the emergency department.
X-ray Findings
Anteroposterior (AP) and lateral radiographs of the right elbow were obtained.
-
Initial AP and Lateral Radiographs:
These views clearly demonstrated a posterior dislocation of the ulnohumeral joint. The olecranon was positioned posterior to the distal humerus. Crucially, the radiographs revealed associated fractures.
- There was a comminuted fracture of the radial head (Mason Type III).
- A significant coronoid process fracture was identified, involving approximately 50% of the coronoid height, consistent with a Regan-Morrey Type II fracture.
- Evidence of avulsion fractures from the medial epicondyle (consistent with MCL injury) and lateral epicondyle (consistent with LCL complex injury) were also noted, indicating extensive soft tissue disruption.

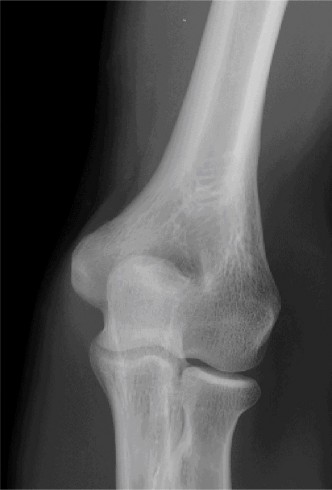
(Representative initial lateral radiograph demonstrating posterior elbow dislocation with associated coronoid and radial head fractures.)
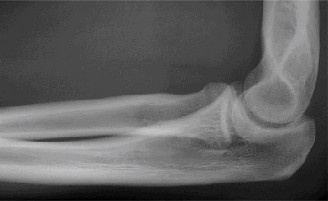
(Representative initial AP radiograph illustrating the elbow dislocation and comminuted radial head fracture.)
Given these findings, a diagnosis of a terrible triad injury of the elbow was made.
CT/MRI Indications
Following initial X-rays, a Computed Tomography (CT) scan of the right elbow was obtained for a more detailed assessment of the fracture morphology, particularly for surgical planning.
- CT Scan: The CT scan provided invaluable three-dimensional detail, confirming the comminuted nature of the radial head fracture, outlining the precise size and displacement of the coronoid fracture fragment, and ruling out any intra-articular loose bodies or additional occult fractures not clearly visible on plain radiographs. The CT confirmed the Regan-Morrey Type II coronoid fracture and Mason Type III radial head fracture, which were critical for determining the reconstructive strategy. The extent of articular involvement for both fractures was meticulously assessed.
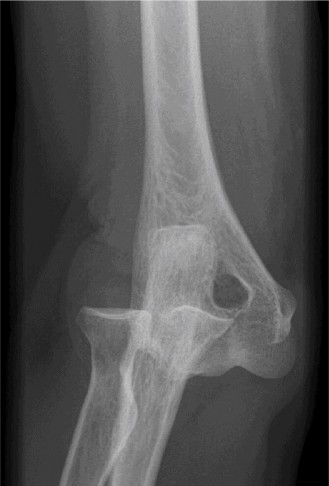
(Representative sagittal CT reconstruction highlighting the coronoid fracture and posterior ulnohumeral displacement.)
MRI was not deemed immediately necessary as the CT provided sufficient bony detail for operative planning and there was no persistent neurological deficit or strong suspicion of isolated chondral injury after reduction. However, in cases of persistent instability despite adequate bony fixation or unexplained pain/stiffness post-operatively, MRI may be considered to assess soft tissue and ligamentous integrity more definitively.
Templating
Pre-operative templating was performed, particularly for the radial head component. Given the comminuted nature of the radial head fracture (Mason Type III), consideration was given to both open reduction internal fixation (ORIF) and radial head arthroplasty. Templating involved reviewing various radial head prosthesis sizes and designs to ensure appropriate fit and alignment, should arthroplasty be required. For the coronoid fracture, templating involved assessing the fragment size and determining the most appropriate fixation method (e.g., suture fixation, small fragment screw fixation, or an anterior coronoid plate).
Differential Diagnosis
The presentation of acute elbow pain, deformity, and limited motion requires a systematic approach to differential diagnosis.
| Feature | Simple Elbow Dislocation (Posterior) | Complex Elbow Dislocation (Terrible Triad) | Monteggia Equivalent Injury | Transolecranon Fracture-Dislocation |
|---|---|---|---|---|
| Pathoanatomy | Ulnohumeral joint dissociation, MCL/LCL rupture. No significant associated fractures. | Posterior dislocation, comminuted radial head fracture, coronoid fracture (Regan-Morrey Type I-III), MCL/LCL disruption. | Proximal ulna fracture (diaphyseal/metaphyseal) with associated radial head dislocation. | Olecranon fracture extending into trochlear notch, with ulnohumeral dislocation. |
| Mechanism | FOOSH with axial load and valgus/varus stress. | High-energy FOOSH, valgus/axial load, often with rotational component. | Direct blow to forearm, hyperpronation, or hyperextension force. | High-energy trauma, direct force to olecranon, or FOOSH. |
| Clinical Presentation | Pain, gross deformity, limited ROM, often stable post-reduction. | Severe pain, marked swelling, significant deformity, often grossly unstable post-reduction. | Forearm pain, deformity, palpable radial head dislocation (anterior, posterior, or lateral). | Pain, swelling, palpable olecranon deformity, instability. |
| Imaging | X-ray: Ulnohumeral dissociation. No significant bony fracture. | X-ray: Dislocation, radial head fx, coronoid fx (often subtle). CT essential for detailed fx morphology. | X-ray: Ulna fx, radial head dislocation. Angulation and translation of ulna fx directly impact radial head position. | X-ray: Olecranon fracture, ulnohumeral dislocation. CT for articular involvement. |
| Stability Post-Reduction | Typically stable in a functional arc; may have endpoint laxity. | Frequently unstable due to loss of critical osseous and ligamentous stabilizers. | Unstable until definitive ulna fixation and radial head reduction. | Highly unstable; requires stable olecranon fixation for ulnohumeral stability. |
| Treatment Strategy | Closed reduction, early protected motion, bracing/sling. | ORIF of coronoid/radial head, MCL/LCL repair/reconstruction, often with temporary hinged external fixator. | ORIF of ulna fracture, reduction of radial head. | ORIF of olecranon fracture, often with tension band or plate and screws. |
| Potential Complications | Stiffness, recurrent instability (rare), heterotopic ossification (HO). | Stiffness, recurrent instability, HO, malunion/nonunion, post-traumatic arthritis, nerve injury. | Nonunion/malunion, radial nerve injury, chronic radial head dislocation, stiffness. | Nonunion, malunion, post-traumatic arthritis, HO, stiffness, nerve injury. |
Surgical Decision Making & Classification
The patient's injury, a posterior elbow dislocation combined with a comminuted radial head fracture (Mason Type III) and a significant coronoid process fracture (Regan-Morrey Type II), unequivocally classifies it as a terrible triad injury of the elbow . This specific constellation of injuries is recognized for its inherent instability and high propensity for poor outcomes if not adequately managed.
Why Operative vs. Non-operative?
The decision for operative intervention in this case was straightforward and immediate due to several critical factors:
1.
Inherent Instability:
Terrible triad injuries are notoriously unstable due to the disruption of all three primary elbow stabilizers: the osseous buttress of the coronoid, the lateral collateral ligament (LCL) complex (disrupted by the radial head fracture and dislocation), and often the medial collateral ligament (MCL).
2.
Associated Fractures:
The presence of a comminuted radial head fracture and a large, displaced coronoid fracture fragment necessitates surgical repair to restore articular congruity, establish a stable bony foundation, and prevent late instability and post-traumatic arthritis.
3.
High Risk of Recurrent Dislocation:
Without surgical stabilization of both the osseous and ligamentous structures, the likelihood of recurrent dislocation is exceedingly high, leading to chronic pain, dysfunction, and severe arthritis.
4.
Poor Functional Outcome with Non-operative Management:
Non-operative treatment of terrible triad injuries almost invariably leads to poor outcomes, including persistent instability, severe stiffness, and debilitating pain.
Therefore, closed reduction, while a necessary initial step in the emergency setting (if possible and safe), would not provide definitive stability in this complex fracture-dislocation. Surgical stabilization was imperative.
Classification Systems Applied
To guide surgical planning and prognostication, the following classification systems were utilized:
- Elbow Dislocation Classification (General): This was a posterior dislocation , the most common type.
- Hotchkiss Classification (Post-Reduction Stability): Although the elbow was dislocated on presentation, surgical planning anticipated that even after closed reduction, the elbow would remain grossly unstable (Hotchkiss Type III) due to the significant bony and ligamentous disruptions. This high degree of instability mandated surgical intervention.
- Mason Classification for Radial Head Fractures: The comminuted radial head fracture was classified as a Mason Type III . These fractures typically involve significant articular comminution, are often unreconstructible, and frequently lead to impaction and instability, often necessitating radial head replacement or meticulous ORIF.
- Regan-Morrey Classification for Coronoid Fractures: The coronoid fracture, involving approximately 50% of the coronoid height, was classified as a Regan-Morrey Type II . These fractures represent a larger fragment of the coronoid, which is crucial for ulnohumeral stability. Its repair is paramount for preventing recurrent dislocation.
- Broberg and Morrey Classification: While not a separate classification per se , the combination of posterior elbow dislocation, radial head fracture, and coronoid fracture is often collectively referred to as a "Terrible Triad Injury" , a term coined by Broberg and Morrey to emphasize its severe nature and challenging management.
The surgical strategy was thus aimed at reconstructing the osseous stabilizers (radial head, coronoid) and repairing the essential ligamentous structures (LCL complex, and often the MCL), followed by early controlled mobilization.
Surgical Technique / Intervention
The patient was taken to the operating theater emergently after optimization.
Patient Positioning
The patient was positioned supine on the operating table. A high-arm tourniquet was applied to the right upper arm. The arm was prepped and draped in a sterile fashion, allowing free manipulation of the elbow joint. A specialized radiolucent hand table was used to facilitate full range of motion testing and fluoroscopic imaging throughout the procedure.
Surgical Approach
A dual-incision approach was planned to address all components of the injury.
- Lateral Approach (Kocher interval): An approximately 8 cm curvilinear incision was made over the lateral aspect of the elbow, centered over the radial head. The interval between the anconeus and extensor carpi ulnaris (ECU) was utilized to access the radial head and the lateral collateral ligament complex. The common extensor origin was carefully elevated.
- Medial Approach (Posteromedial interval): A separate curvilinear incision, approximately 6 cm in length, was made posteromedially, posterior to the medial epicondyle. The interval between the flexor carpi ulnaris (FCU) and the medial epicondyle allowed access to the medial collateral ligament (MCL) and, if needed, the coronoid fracture from an anterior approach, carefully retracting the ulnar nerve. A thorough identification and protection of the ulnar nerve were performed at this stage.
Reduction Techniques & Initial Stabilization
Under general anesthesia, a closed reduction was attempted. With the patient in supine position, gentle longitudinal traction was applied to the forearm with the elbow in slight flexion. Countertraction was applied to the humerus. A direct anterior-to-posterior force was applied to the distal humerus while simultaneously applying a posterior-to-anterior force to the olecranon to guide it over the trochlea. The reduction was successful, confirmed by fluoroscopy.
Following reduction, the elbow remained grossly unstable, particularly in valgus and varus stress tests, and prone to redislocation with early flexion. This confirmed the need for comprehensive surgical stabilization.
Fixation Construct
-
Radial Head Reconstruction/Replacement:
- Through the lateral approach, the comminuted radial head fracture (Mason Type III) was exposed. Despite careful assessment, the fragments were deemed too small and numerous for reliable open reduction and internal fixation (ORIF) with mini-fragment screws, especially given the articular involvement.
- A decision was made for radial head arthroplasty . The fragmented radial head was meticulously excised, preserving the annular ligament whenever possible. The radial neck was prepared, and a modular radial head prosthesis of appropriate size (determined by pre-operative templating and intra-operative trial) was implanted and cemented into place. Care was taken to restore radial length and ensure unimpeded forearm rotation.
- Crucial Step: Once the radial head prosthesis was in place, stability was re-assessed. This significantly improved the varus stability and reduced the tendency for posterior subluxation.
-
Coronoid Process Fixation:
- The coronoid fracture (Regan-Morrey Type II) was addressed. Access was gained via the medial incision. The coronoid fragment was reduced under direct visualization, using fluoroscopy to confirm anatomical alignment.
- Given the fragment size, a small fragment screw fixation was not considered sufficient alone. A buttress plate (specifically, an anterior coronoid plate) was applied to the anterior aspect of the coronoid and secured with low-profile screws, providing robust fixation and resisting posterior displacement. This was a critical step in restoring the anterior osseous stability of the ulnohumeral joint.
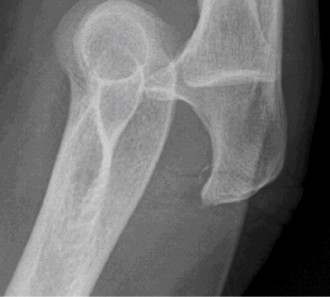
(Representative intra-operative image showing placement of an anterior coronoid plate for fixation of a coronoid fracture.)
-
Ligamentous Repair:
- Lateral Collateral Ligament (LCL) Complex Repair: Through the lateral approach, the avulsed origin of the LCL complex from the lateral epicondyle was identified. It was directly repaired back to its anatomical footprint using suture anchors . Strong, non-absorbable sutures were passed through the ligamentous tissue and tied down to the anchors, ensuring tension-free repair.
- Medial Collateral Ligament (MCL) Repair: Through the medial approach, the torn MCL, specifically the anterior bundle, was identified. It was repaired to its humeral origin (medial epicondyle) using suture anchors . The ulnar nerve was carefully protected throughout this step.
(Representative intra-operative image depicting suture anchor repair of the medial collateral ligament (MCL) to the medial epicondyle.)
Final Stability Assessment
After all components were addressed, the elbow joint was rigorously tested for stability throughout a full range of motion. The elbow was found to be stable from full extension to approximately 120 degrees of flexion, with no evidence of subluxation or dislocation under valgus or varus stress. Pronation and supination were also stable. There was no need for a hinged external fixator due to the achievement of excellent intrinsic stability.
The wounds were irrigated, and closure was performed in layers. A sterile dressing was applied, and the elbow was placed in a hinged elbow brace, locked initially in 30 degrees of flexion to 90 degrees of flexion to protect the repairs.
Post-Operative Protocol & Rehabilitation
The post-operative protocol for a terrible triad injury is meticulously structured to balance protection of the surgical repairs with early, controlled motion to prevent stiffness and optimize functional recovery.
Immediate Post-Operative Phase (Days 0-14)
- Immobilization: The elbow was placed in a hinged elbow brace, initially locked from 30° flexion to 90° flexion, allowing a protected arc of motion. The forearm was positioned in neutral to slight pronation.
- Pain Management: Multimodal analgesia, including regional nerve blocks, oral opioids, and NSAIDs, was utilized.
- Edema Control: Elevation of the extremity, gentle hand exercises (fist clenching), and cryotherapy were initiated to minimize swelling.
- Wound Care: Daily inspection of surgical incisions for signs of infection.
- Neurological Assessment: Serial neurovascular examinations to monitor for any delayed nerve compromise or compartment syndrome.
- Goals: Protect repairs, control pain and swelling, maintain distal joint function.
Early Motion Phase (Weeks 2-6)
- Hinged Brace Management: The hinged elbow brace remained in place. Under the guidance of a hand therapist, the allowed range of motion was gradually increased by 10-15 degrees per week, primarily focusing on extension, with the flexion limit remaining at 90-100 degrees for initial weeks.
- Active-Assisted Range of Motion (AAROM): Gentle, active-assisted exercises were initiated within the protected arc of motion, focusing on flexion/extension and pronation/supination. Passive range of motion was avoided initially to prevent undue stress on ligamentous repairs.
- Isometrics: Gentle isometric exercises for the biceps, triceps, and forearm musculature were introduced, ensuring no movement at the elbow joint.
- Scar Management: Gentle scar massage commenced once incisions were well-healed to prevent adhesion formation.
- Goals: Restore gradual, controlled motion, prevent stiffness, protect healing structures.
Strengthening Phase (Weeks 6-12)
- Brace Weaning: Depending on clinical stability and progression, the brace was gradually weaned, initially for light activities, and eventually for full-time use, typically around 8-10 weeks post-op.
- Progressive ROM: Full active range of motion was encouraged. Gentle passive range of motion could be introduced if a significant flexion or extension deficit persisted, but with extreme caution to avoid overstressing the repaired structures.
- Progressive Strengthening: Light resistive exercises were introduced using bands, light weights, and putty. Emphasis was placed on balanced strengthening of the elbow flexors, extensors, pronators, and supinators.
- Endurance Training: Low-resistance, high-repetition exercises to improve muscular endurance.
- Goals: Regain full functional range of motion, improve strength and endurance.
Advanced Activity & Return to Sport/Work (Weeks 12+)
- Functional Progression: Sport-specific or work-specific activities were gradually introduced.
- High-Impact Activities: High-impact or heavy lifting activities were deferred until at least 4-6 months post-operatively, depending on individual progress and stability.
- Return to Play/Work: Full return to unrestricted activities was permitted only after demonstration of full strength, range of motion, and absence of pain or instability.
- Goals: Return to pre-injury activity level, maximize functional independence.
Throughout rehabilitation, close monitoring for signs of heterotopic ossification (HO), recurrent instability, or nerve irritation was paramount. Prophylaxis for HO (e.g., NSAIDs or low-dose radiation) was considered, especially in high-risk patients. Regular clinical and radiographic follow-up was maintained to assess healing and guide rehabilitation progression.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion for Complexity: Always assume a simple elbow dislocation may be complex. A thorough clinical exam and adequate imaging (AP/Lateral X-rays) are paramount. If doubt exists or stability is poor post-reduction, obtain a CT scan. The terrible triad injury is a classic example.
- Meticulous Neurovascular Assessment: Pre- and post-reduction neurovascular status is non-negotiable. Document carefully. Any deficit necessitates urgent investigation and consideration of open reduction.
- Anatomical Reduction is Key: The primary goal is to restore congruent joint surfaces. Even temporary subluxation will predispose to instability and poor outcomes.
-
Order of Surgical Stabilization (Terrible Triad):
A consistent approach often works best:
- Radial head (ORIF or arthroplasty) to restore lateral column height and stability.
- Coronoid fracture (ORIF, plate, or suture repair) to restore anterior buttress.
- Lateral collateral ligament (LCL) complex repair to provide posterolateral stability.
- Medial collateral ligament (MCL) repair (if significantly unstable in valgus) to enhance medial stability.
- Assess stability throughout the repair process.
- Coronoid Management is Critical: Even small coronoid fractures can lead to instability. Regan-Morrey Type I (tip avulsion) can often be managed with LCL repair alone, but Type II and III fractures require direct repair or plating. Anterior buttress plating offers excellent resistance to posterior displacement.
- Radial Head Arthroplasty for Comminuted Fractures: For Mason Type III radial head fractures, arthroplasty provides immediate stability, restores radial length, and facilitates early motion, often yielding superior results compared to excisional arthroplasty or complex ORIF in unsuitable fractures.
- Consider a Hinged External Fixator: For grossly unstable elbows even after comprehensive internal fixation and ligamentous repair, a hinged external fixator provides dynamic stability, allowing controlled early motion while protecting the soft tissue and bony repairs. This can be a game-changer for challenging cases.
- Early Controlled Motion: This is paramount to prevent stiffness and heterotopic ossification. The stability achieved intra-operatively dictates the aggression of the post-operative rehabilitation. "Static progressive" or "dynamic" bracing may be indicated.
- Ulnar Nerve Protection: The ulnar nerve is vulnerable, particularly during medial approaches for MCL repair or coronoid fixation. Always identify and protect it.
Pitfalls
- Missed Injuries: Failing to identify associated fractures (especially subtle coronoid fractures on plain films) or significant ligamentous tears can lead to chronic instability and poor outcomes.
- Inadequate Reduction or Fixation: Leaving residual subluxation or unstable fixation is a recipe for disaster, leading to recurrent dislocation, nonunion, or stiffness.
- Over-Aggressive Rehabilitation: Pushing range of motion too quickly, particularly passive range of motion, can stress healing ligamentous repairs or bony fixation, leading to re-dislocation or failure of fixation. Adherence to a protected protocol is crucial.
- Ignoring Neurovascular Status: Failing to recognize or address neurovascular compromise promptly can result in permanent neurological deficits or limb-threatening ischemia.
- Failure to Address the "Terrible Triad" Holistically: Treating only one component (e.g., radial head) while neglecting the coronoid or ligaments will invariably lead to failure. All destabilizing factors must be addressed.
- Heterotopic Ossification (HO): The elbow is highly susceptible to HO after trauma and surgery. Prophylaxis (e.g., indomethacin or low-dose radiation) should be considered, especially in high-risk patients (burns, head injury, prolonged immobilization).
- Post-Traumatic Stiffness: Despite best efforts, elbow stiffness is a common complication. Careful surgical technique, meticulous soft tissue handling, and appropriate early rehabilitation are crucial to minimize this risk. Persistent stiffness may necessitate subsequent manipulation under anesthesia or even arthrolysis.
- Chronic Instability: Inadequate repair or poor rehabilitation can lead to chronic instability, requiring complex revision surgery or potentially leading to severe degenerative changes.
Clinical & Radiographic Imaging