Patient Presentation & History
A 58-year-old male, a professional carpenter, presented to the Emergency Department following a fall from a height of approximately 2.5 meters. He reported landing directly onto his outstretched right upper extremity, sustaining a hyperextension injury to the elbow and a direct impact to the lateral aspect of his shoulder. Initial chief complaint was severe pain and deformity of the right elbow, accompanied by generalized shoulder pain which he described as less severe than the elbow pain.
His past medical history included well-controlled hypertension and Type 2 Diabetes Mellitus managed with oral medications. He was a non-smoker and consumed alcohol occasionally. No known allergies. He denied any preceding neurological symptoms, numbness, or weakness in the upper limb.
Upon presentation, the patient was hemodynamically stable. Paramedics had applied a splint to the right elbow. Initial assessment in the trauma bay focused primarily on the obvious elbow deformity, with a cursory examination of the shoulder revealing diffuse tenderness but no gross deformity. The patient’s acute pain made a comprehensive neurological assessment challenging in the initial phase.
Clinical Examination
Following initial resuscitation and pain management, a detailed examination of the right upper extremity was performed.
Inspection:
*
Elbow:
Gross posterior-lateral deformity of the right elbow, significant swelling around the joint, and ecchymosis extending distally and proximally. Skin appeared intact with no open wounds.
*
Shoulder:
Moderate swelling over the deltoid region and lateral shoulder. No obvious dislocation or fracture deformity. The contour of the deltoid appeared slightly flattened compared to the contralateral side.
Palpation:
*
Elbow:
Exquisite tenderness over the radial head, lateral epicondyle, medial epicondyle, and olecranon. There was palpable crepitus with any attempted passive movement.
*
Shoulder:
Diffuse tenderness over the greater tuberosity, surgical neck of the humerus, and deltoid insertion. No crepitus was elicited on gentle palpation.
Range of Motion (ROM):
*
Elbow:
Severely restricted due to pain and instability. Passive flexion-extension arc was estimated to be 30-70 degrees (normal 0-140), with significant instability noted in varus and valgus stress. Forearm pronation and supination were also severely limited.
*
Shoulder:
Limited active and passive ROM due to pain. Active abduction was severely compromised, reaching only approximately 30 degrees, primarily through scapulothoracic motion rather than glenohumeral. External rotation was also significantly reduced.
Neurological Assessment:
This was the critical component that began to unravel the "mystery" of this multi-region injury.
*
Median Nerve:
Sensation intact in thumb, index, middle finger and thenar eminence. Motor intact for thumb opposition and flexion of index finger.
*
Ulnar Nerve:
Sensation intact in little finger and medial half of ring finger. Motor intact for finger abduction/adduction.
*
Radial Nerve:
Sensation intact in dorsal first web space. Motor intact for wrist extension and finger extension.
*
Musculocutaneous Nerve:
Sensation intact over lateral forearm. Motor intact for biceps (elbow flexion).
*
Axillary Nerve:
*
Motor:
Markedly diminished active deltoid contraction. The patient was unable to actively abduct the arm against gravity past 30 degrees, and no significant deltoid contraction was palpable. Teres minor function (external rotation from adducted position) was also weak (MMT 2/5).
*
Sensory:
Anesthesia/hypoesthesia noted over the "regimental badge" area on the lateral aspect of the shoulder, indicative of axillary nerve involvement.
Vascular Assessment: Radial and ulnar pulses were palpable and strong. Capillary refill was brisk in all digits. No signs of compartment syndrome were present.
The presence of a clear axillary nerve palsy in the context of an obvious elbow injury, with only non-specific shoulder pain, immediately raised suspicion for a concomitant, potentially overlooked, shoulder pathology. This initiated a focused and expanded imaging protocol for the shoulder.
Imaging & Diagnostics
Initial Radiographs (Emergency Department):
*
Right Elbow (AP, Lateral, Oblique views):
Revealed a complex elbow dislocation (posterior-lateral type), a comminuted radial head fracture (Mason-Morrey Type III), and a large coronoid process fracture (O'Driscoll Type IIB). Evidence of lateral collateral ligament complex avulsion was also noted.
*
Right Shoulder (AP, Scapular Y views):
Initial interpretation reported "no acute fracture or dislocation." However, a careful re-evaluation after the neurological findings suggested a subtle cortical irregularity along the surgical neck of the humerus, initially interpreted as an artifact. There was also minimal anterior humeral head displacement relative to the glenoid, consistent with a
reduced
anterior glenohumeral dislocation, which was not documented on presentation.
Advanced Imaging (Post-Neurological Assessment):
*
Right Shoulder Computed Tomography (CT) with 3D Reconstructions:
This was crucial. It definitively demonstrated a Neer 2-part surgical neck fracture of the right humerus, minimally displaced but with significant periosteal disruption. Importantly, the CT confirmed findings consistent with a reduced anterior glenohumeral dislocation, specifically a Hill-Sachs lesion on the posterior-superior aspect of the humeral head and a bony Bankart lesion on the anterior-inferior glenoid rim. This explained the mechanism of axillary nerve injury.
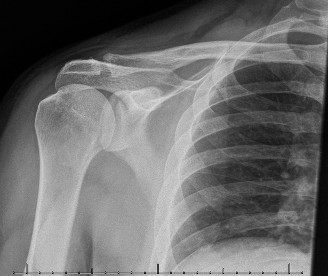
Figure 1: CT 3D reconstruction of the right shoulder, illustrating a Neer 2-part surgical neck fracture of the humerus. The fracture line is visible through the surgical neck, with minimal displacement. Features suggestive of a reduced anterior dislocation (Hill-Sachs, bony Bankart) were also identified on detailed slice analysis.
-
Right Elbow Computed Tomography (CT) with 3D Reconstructions: Confirmed the comminution of the radial head fracture, delineating the extent of articular involvement. The coronoid fracture fragment size and displacement were precisely mapped, crucial for pre-operative planning. It also confirmed the posterior-lateral dislocation.
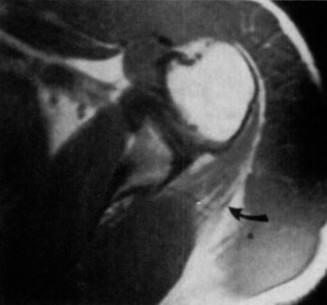
Figure 2: CT 3D reconstruction of the right elbow, demonstrating a complex terrible triad injury. A comminuted radial head fracture (Mason-Morrey Type III) is evident, alongside a significant coronoid process fracture (O'Driscoll Type IIB). The posterior-lateral dislocation of the ulna relative to the humerus is also clearly depicted. -
Magnetic Resonance Imaging (MRI) – Optional but often considered for ligamentous injuries: An MRI of the elbow would be considered to further delineate the extent of lateral ulnar collateral ligament (LUCL) complex injury and medial collateral ligament (MCL) integrity, though often not strictly necessary with CT findings of a terrible triad. For the shoulder, an MRI could assess rotator cuff integrity and labral tears, particularly if long-term instability is suspected after a dislocation, but was deferred in the acute setting given the fracture and nerve injury focus.
Differential Diagnosis
The primary diagnostic challenge in this case was not identifying the severe elbow injury, but rather attributing the axillary nerve palsy correctly in a polytrauma setting, particularly when the shoulder pathology was initially subtle. Below is a differential diagnosis for axillary nerve palsy in the context of upper limb trauma:
| Condition | Key Features | Diagnostic Clues in This Case | Why it Fits/Doesn't Fit |
|---|---|---|---|
| 1. Axillary Nerve Palsy due to Shoulder Trauma (Fracture/Dislocation) | Weakness/paralysis of deltoid and teres minor, sensory loss in "regimental badge" area. Often associated with anterior shoulder dislocations, proximal humerus fractures, or direct trauma to the quadrangular space. | Patient had an anterior shoulder dislocation (now reduced) and a surgical neck humerus fracture, which are direct mechanisms for axillary nerve injury. Neurological exam precisely mapped to axillary nerve distribution. | Fits perfectly. The CT findings confirmed the shoulder pathology, and the specific motor and sensory deficits are pathognomonic for axillary nerve injury. The mechanism (fall onto outstretched hand/shoulder) supports this. |
| 2. Brachial Plexus Injury (Upper Trunk/C5-C6) | Weakness in deltoid, supraspinatus, infraspinatus, biceps, brachialis. Sensory loss over lateral shoulder/arm. Often associated with high-energy trauma, traction injuries. | While deltoid weakness is present, there was no significant weakness in biceps, supraspinatus, or infraspinatus (though shoulder pain made full assessment difficult initially). Sensory loss was only in regimental badge area. | Less likely, but important to rule out. If other C5-C6 innervated muscles (e.g., biceps, supraspinatus) were also significantly involved, or if sensory loss extended beyond the regimental badge area, a brachial plexus injury would be more probable. |
| 3. Cervical Radiculopathy (C5-C6) | Neck pain, radicular symptoms down the arm, deltoid/biceps weakness, diminished C5-C6 reflexes. Can be acute traumatic or chronic degenerative. | No significant neck pain reported. No radicular symptoms. No obvious C5-C6 reflex changes. Onset was acute with trauma. | Unlikely. In the acute trauma setting, isolated C5-C6 radiculopathy causing just deltoid weakness without other findings (neck pain, arm pain, other motor deficits, reflex changes) is improbable. |
| 4. Deltoid Muscle Contusion/Rupture | Localized pain, swelling, ecchymosis over deltoid. Mechanical weakness in abduction. Sensory innervation would be intact. | Patient exhibited sensory loss in the axillary nerve distribution, which would not be present with a purely muscular injury. | Does not fit. While a contusion might cause pain and weakness, the associated sensory deficit conclusively rules out a purely muscular injury as the sole cause of the motor weakness. |
| 5. Quadrangular Space Syndrome | Compression of the axillary nerve and posterior circumflex humeral artery within the quadrangular space (teres minor, teres major, triceps, humerus). Often seen in overhead athletes or due to fibrous bands. | Presents with nerve symptoms similar to this case. However, it is usually a chronic or subacute presentation, not typically an acute traumatic event causing such an immediate, profound palsy. No vascular compromise was evident. | Unlikely as an acute traumatic cause. While the nerve courses through this space, acute traumatic compression of this magnitude causing a complete palsy would be unusual without a significant adjacent bone injury which was found. |
Based on the clinical presentation and definitive imaging, the diagnosis was: Right complex elbow terrible triad injury (posterior-lateral dislocation, Mason-Morrey Type III radial head fracture, O'Driscoll Type IIB coronoid fracture) with concomitant right Neer 2-part surgical neck humerus fracture and acute traumatic axillary nerve palsy secondary to a reduced anterior glenohumeral dislocation.
Surgical Decision Making & Classification
Given the multi-system trauma, a staged approach to surgical intervention was planned. The elbow injury, being highly unstable and involving articular fractures, was deemed an acute operative emergency. The shoulder fracture, while significant, was considered for initial non-operative management given its minimally displaced nature, allowing for concurrent management of the axillary nerve palsy.
Elbow Injury Classification & Decision:
*
Posterior-lateral Elbow Dislocation:
Requires reduction and stabilization due to high recurrence risk and instability.
*
Radial Head Fracture (Mason-Morrey Type III):
Comminuted, displaced, and involving greater than one-third of the articular surface. This type typically requires surgical intervention (ORIF or radial head arthroplasty) to restore joint congruity, stability, and facilitate early motion. Given the patient's age and activity level, and the extent of comminution, a radial head arthroplasty was favored for predictable stability and earlier rehabilitation.
*
Coronoid Process Fracture (O'Driscoll Type IIB):
Involving 30-50% of the coronoid height. This contributes significantly to elbow instability, especially in the context of posterior-lateral dislocations. Surgical fixation is mandated to restore anterior stability and prevent recurrent dislocation.
*
Lateral Ulnar Collateral Ligament (LUCL) Injury:
Implied by the posterior-lateral dislocation and avulsion fracture. Repair is essential for elbow stability.
Combined, these injuries constitute a "Terrible Triad" of the elbow, which is inherently unstable and requires surgical stabilization to achieve a functional, stable, and mobile joint. Non-operative management leads to persistent instability, pain, and poor functional outcomes.
Shoulder Injury Classification & Decision:
*
Neer 2-part Surgical Neck Humerus Fracture:
The CT showed minimal displacement and good cortical opposition. While the fracture contributes to shoulder pain, its minimally displaced nature makes it amenable to initial non-operative management, particularly in the context of the axillary nerve palsy. The primary concern for the shoulder was the axillary nerve injury.
*
Axillary Nerve Palsy:
As this was a presumed neuropraxia secondary to the dislocation and/or fracture, the initial management is observation and expectant management for recovery. Surgical exploration of the axillary nerve is typically reserved for cases with no signs of recovery after 3-6 months.
Therefore, the surgical plan was Open Reduction and Internal Fixation (ORIF) of the coronoid fracture, Radial Head Arthroplasty, and Lateral Collateral Ligament (LCL) repair for the elbow , with non-operative management of the proximal humerus fracture and close monitoring of the axillary nerve palsy .
Surgical Technique / Intervention
The surgical procedure was performed approximately 48 hours after admission to allow for soft tissue swelling reduction and optimize patient comorbidities.
I. Elbow Reconstruction:
Patient Positioning: The patient was positioned supine on the operating table. The right arm was draped free and placed on a hand table, allowing full manipulation and fluoroscopic access. A pneumatic tourniquet was applied to the upper arm.
Surgical Approaches:
1.
Lateral Approach (Kocher Interval):
An approximately 8 cm curvilinear incision was made centered over the lateral epicondyle, extending proximally along the supracondylar ridge and distally along the ulna. The interval between the anconeus and extensor carpi ulnaris (ECU) was developed. The common extensor origin was carefully elevated. The lateral ulnar collateral ligament (LUCL) complex was identified and confirmed to be avulsed from the lateral epicondyle. The radial head fracture was exposed.
2.
Medial Approach:
A separate approximately 6 cm incision was made over the medial epicondyle, dissecting through the interval between the flexor carpi ulnaris (FCU) and the flexor digitorum superficialis (FDS) or by splitting the FCU. The ulnar nerve was identified, neurolysed, and gently retracted posteriorly to protect it. This approach provided direct visualization of the coronoid process.
Surgical Steps:
1.
Radial Head Management:
The comminuted radial head fracture fragments were assessed. Due to the Mason-Morrey Type III nature, significant comminution, and desire for predictable stability and early motion, a
radial head arthroplasty
was performed. The fractured radial head was excised. The medullary canal of the proximal radius was prepared. A appropriately sized unipolar radial head implant was inserted and cemented into place, ensuring appropriate height and fit.
2.
Coronoid Process Fixation:
Through the medial approach, the O'Driscoll Type IIB coronoid fracture fragment was identified. It was mobilized and reduced anatomically. Fixation was achieved using two small cannulated screws placed from an anterior-medial to posterior-lateral direction, providing stable compression. Care was taken to avoid over-penetration into the posterior cortex or articular surface. The brachialis muscle origin, if avulsed with the fragment, was reattached.
3.
Lateral Ulnar Collateral Ligament (LUCL) Repair:
Through the lateral approach, the avulsed LUCL complex was identified. Its footprint on the lateral epicondyle was prepared. Suture anchors (typically two) were placed into the lateral epicondyle. Non-absorbable sutures were then passed through the substance of the avulsed ligament, allowing for a robust repair and tensioning to restore varus stability. The elbow was taken through a full range of motion under direct visualization to confirm stability. Dynamic fluoroscopy was used to ensure concentric reduction and stability throughout the arc of motion.
4.
Capsular Repair and Closure:
The lateral capsule was repaired over the implant and LUCL repair. Medial capsule was also repaired. Layered closure was performed. The ulnar nerve was confirmed to be free in its groove before skin closure.
II. Shoulder Management:
No surgical intervention was performed for the minimally displaced surgical neck fracture. The shoulder was placed in a sling for comfort and protected motion.
Post-Operative Protocol & Rehabilitation
Elbow:
*
Immobilization:
The right elbow was initially immobilized in a hinged elbow brace, locked at 90 degrees of flexion with the forearm in neutral rotation, for 1 week. This allowed initial soft tissue healing.
*
Early Motion (Weeks 1-6):
At the first post-operative visit (Day 7), the brace was unlocked. Supervised active-assisted and passive range of motion exercises were initiated, progressively increasing flexion and extension within pain tolerance. The brace was worn at all times except during exercises, gradually increasing the allowable arc of motion (e.g., 30-90 degrees in week 2, 20-110 in week 3, etc.). Gravity-assisted exercises and gentle stretching were encouraged. Forearm pronation/supination exercises were also started.
*
Strengthening (Weeks 6-12):
Once pain subsided and a functional arc of motion was achieved, progressive strengthening exercises for the elbow flexors, extensors, pronators, and supinators were introduced. Light resistance bands and hand weights were used.
*
Advanced Rehabilitation (Months 3-6):
Emphasis on functional activities, sport-specific (if applicable) or work-specific movements. Gradual return to full activities, avoiding heavy lifting or repetitive strenuous tasks initially.
*
Heterotopic Ossification Prophylaxis:
Given the extent of trauma and surgery, a course of NSAIDs (Indomethacin) for 3-6 weeks was prescribed.
Shoulder (Proximal Humerus Fracture & Axillary Nerve Palsy):
*
Immobilization:
The shoulder was protected in an arm sling for 4-6 weeks to allow fracture healing.
*
Early Motion (Weeks 1-6):
During the sling immobilization period, pendulum exercises were initiated on day 3 post-op to encourage gentle glenohumeral motion and reduce stiffness. Passive range of motion for the shoulder was also started within pain limits, with a focus on external rotation and forward flexion to prevent adhesive capsulitis.
*
Axillary Nerve Monitoring:
Serial neurological examinations were performed at each clinic visit. The patient was instructed to attempt gentle deltoid contraction and report any return of sensation.
*
Nerve Rehabilitation (Weeks 6 onwards):
*
Active-assisted abduction and external rotation:
As tolerated, using the contralateral hand or a pulley system.
*
Gentle isometric exercises for deltoid and teres minor:
Once some initial motor recovery was noted.
*
Electrical stimulation:
May be considered to prevent muscle atrophy and encourage reinnervation.
*
Formal Neurophysiologic Studies:
If there was no clinical evidence of axillary nerve recovery (motor or sensory) by 6-8 weeks post-injury, an Electromyography (EMG) and Nerve Conduction Study (NCS) would be performed to assess the extent of nerve injury (neurapraxia vs. axonotmesis vs. neurotmesis) and guide further management.
*
Surgical Exploration:
If EMG/NCS indicates complete denervation with no signs of reinnervation, and no clinical recovery is observed by 3-6 months, surgical exploration of the axillary nerve would be considered.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Polytrauma Assessment: Always maintain a high index of suspicion for associated injuries, especially in high-energy trauma. The "mystery" of axillary nerve palsy in an "elbow case" highlights the need for a comprehensive secondary survey.
- Systematic Neurological Exam: Perform a thorough, systematic neurological assessment before and after any intervention. Detailed documentation of motor and sensory deficits is paramount. In trauma, it's easy to focus on obvious injuries and miss subtle neurological findings or non-contiguous injuries.
- Recognize Non-Contiguous Injury Patterns: An injury in one joint (e.g., elbow) does not preclude a separate, potentially silent, injury in an adjacent or distant joint (e.g., shoulder, wrist, hand). The mechanism of injury often provides clues (e.g., fall onto outstretched hand can cause both elbow and shoulder injuries).
- Appropriate Imaging: Don't hesitate to extend imaging beyond the primary injury site if clinical findings warrant it. In this case, the axillary nerve palsy mandated dedicated, detailed shoulder imaging (CT with 3D reconstructions).
- Axillary Nerve Prognosis: Most axillary nerve neuropraxias secondary to blunt trauma or dislocation recover spontaneously within 3-6 months. However, careful monitoring is essential.
- Terrible Triad Management: A terrible triad is inherently unstable. Surgical stabilization of all components (radial head, coronoid, LUCL) is crucial for a stable, mobile, and functional outcome. Radial head arthroplasty often offers more predictable stability and allows earlier rehabilitation than ORIF for comminuted fractures.
- Early Protected Motion: For both elbow and shoulder, early protected range of motion is critical to prevent stiffness, contractures, and heterotopic ossification, while allowing for soft tissue and fracture healing.
Pitfalls:
- Tunnel Vision: Focusing solely on the obvious elbow injury and missing the concomitant shoulder pathology and axillary nerve palsy. This could lead to delayed diagnosis, inappropriate management, and potentially poorer outcomes.
- Inadequate Neurological Assessment: A hurried or incomplete neurological exam, especially in a painful, swollen limb, can lead to missed nerve injuries.
- Misinterpreting Nerve Palsy: Assuming all post-traumatic nerve palsies are transient neurapraxias without adequate follow-up or diagnostic studies. Failure to perform EMG/NCS at appropriate intervals can delay crucial decision-making regarding nerve exploration.
- Inadequate Elbow Stability: Insufficiently addressing all components of a terrible triad (e.g., not repairing the LUCL or inadequately fixing the coronoid) will result in persistent instability, recurrent dislocations, and poor long-term function.
- Failure to Prophylax for HO: In complex elbow trauma, especially after multiple ligament/fracture repairs, the risk of heterotopic ossification is high. Prophylaxis with NSAIDs or radiation should be considered.
- Premature Aggressive Rehabilitation: Pushing too hard too soon can compromise fracture healing or repair integrity, leading to implant failure or recurrent instability.
- Neglecting the "Silent" Injury: While the elbow was the focus, allowing the minimally displaced humerus fracture to displace further or developing shoulder stiffness due to lack of early motion are also potential pitfalls.
