Patient Presentation & History
A 48-year-old right-hand dominant male presented to the emergency department following a fall from a ladder, approximately a 3-meter height, landing directly onto his outstretched left arm. He reported immediate, severe pain and deformity in his left elbow, accompanied by an inability to move the joint. There was no reported loss of consciousness or head injury. He denied any numbness, tingling, or weakness distal to the elbow immediately post-injury, though his current pain level precluded active assessment.
The patient's past medical history is significant for well-controlled hypertension and Type 2 Diabetes Mellitus, managed with oral hypoglycemic agents. He has no known allergies. His surgical history includes an uncomplicated appendectomy 15 years prior. He is a non-smoker and occasionally consumes alcohol. His occupation is a self-employed carpenter, necessitating high levels of upper extremity strength and dexterity. He expresses a strong desire to return to his previous functional capacity.
Clinical Examination
Upon initial assessment, the patient was in significant distress due to pain.
Inspection:
The left elbow exhibited marked swelling, ecchymosis, and a visible posterolateral deformity consistent with a dislocation. The olecranon was prominent posteriorly, and the epicondyles appeared to be in an altered relationship to the olecranon. There were no open wounds or signs of impending skin compromise.
Palpation:
Tenderness was exquisite globally around the elbow joint. There was palpable crepitus with any attempt at passive movement. The radial head was noted to be displaced. Palpation of the coronoid region elicited severe pain. No abnormal motion was appreciated in the forearm or wrist. The shoulder and hand were visually inspected and palpated, revealing no obvious deformity or acute tenderness, although detailed assessment was limited by the elbow injury.
Range of Motion (ROM):
Active and passive ROM of the left elbow was severely restricted due to pain and mechanical block. Flexion was limited to approximately 30-40 degrees, and extension was fixed at about 90 degrees. Pronation/supination was not reliably assessed due to pain and gross instability.
Neurological Assessment:
Initial gross assessment revealed intact sensation to light touch in the median, ulnar, and radial nerve distributions. Motor function of the wrist and hand was limited by pain, but he was able to weakly flex and extend his fingers and wrist. Specifically, thumb abduction (median), finger abduction/adduction (ulnar), and wrist extension (radial) were present but weak. A more detailed neurological examination was deferred until initial analgesia and stabilization.
Vascular Assessment:
Radial and ulnar pulses were strong and symmetric compared to the contralateral limb. Capillary refill was brisk in all digits. No pallor or paresthesia was reported.
Imaging & Diagnostics
Initial imaging focused on plain radiographs of the left elbow (AP, lateral, and oblique views), which confirmed a terrible triad injury of the elbow.
X-ray Findings:
*
Lateral View:
Demonstrated a posterolateral dislocation of the ulna relative to the humerus. A comminuted radial head fracture (Mason Type III) was clearly visualized, with multiple articular fragments and depression. A fracture of the coronoid process (O'Driscoll Type III) was also evident, involving more than 50% of the coronoid height. There was significant incongruity of the ulnohumeral articulation.
*
AP View:
Confirmed the lateral displacement of the radial head and the severe disruption of the normal osseous anatomy.
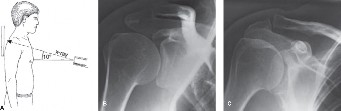
Figure 1: Pre-operative lateral radiograph depicting a complex elbow dislocation with associated radial head and coronoid fractures (terrible triad injury).
CT Scan Indications & Findings:
A Computed Tomography (CT) scan with 3D reconstructions was obtained immediately post-reduction (which was attempted but not stable, or was highly unstable after reduction) to thoroughly evaluate the fracture patterns and assess for subtle additional injuries. This was crucial for surgical planning.
*
Coronoid Fracture:
The CT detailed the size, comminution, and displacement of the coronoid fracture, confirming an O'Driscoll Type III injury, involving the sublime tubercle and a significant portion of the coronoid body. The fragment was displaced proximally and medially.
*
Radial Head Fracture:
The CT provided a more precise assessment of the radial head fracture, delineating the number, size, and displacement of fragments, confirming it as a highly comminuted Mason Type III fracture unsuitable for internal fixation alone due to the number of pieces and severe articular impaction.
*
Soft Tissue Injury:
The CT also allowed for indirect assessment of soft tissue damage, revealing significant capsular disruption and likely injury to the lateral ulnar collateral ligament (LUCL) complex, consistent with a posterolateral rotatory instability pattern. A possible medial collateral ligament (MCL) avulsion was also suspected based on fluid collection and fragment location.
Templating: Pre-operative templating was performed meticulously, particularly for potential radial head replacement. This involved using contralateral elbow radiographs (if available) and comparing dimensions on CT reconstructions to available radial head implant sizes. Various head sizes, stem lengths, and neck lengths were considered for the radial head prosthesis. For the coronoid, strategies for suture passage and anchor placement were templated to ensure adequate fixation and stability.
Differential Diagnosis
Given the presentation of a painful, deformed elbow after trauma, several differential diagnoses were considered, although the initial radiographs quickly narrowed the field.
| Feature | Terrible Triad Injury | Simple Elbow Dislocation | Complex Distal Humerus Fracture | Olecranon Fracture-Dislocation |
|---|---|---|---|---|
| Mechanism | Fall on outstretched arm, valgus/supination force. | Fall on outstretched arm, axial load +/- rotation. | Direct trauma, axial load, high-energy. | High-energy, valgus/varus stress, axial compression. |
| Deformity | Gross posterolateral deformity, swelling. | Posterolateral deformity, less swelling/crepitus. | Varying deformity, significant swelling, crepitus. | Often obvious posterior olecranon displacement. |
| Imaging - X-ray | Posterolateral dislocation, radial head fx (Mason III), coronoid fx (O'Driscoll III). | Posterolateral dislocation, no significant fx. | Supracondylar, intercondylar (C1-C3), column fx. | Posterior dislocation, comminuted olecranon fx. |
| Imaging - CT | Defines radial head & coronoid comminution, LUCL/MCL injury. | Confirms no fx, assesses subtle chondral injury. | Detailed fx pattern, articular involvement, soft tissue. | Detailed fx pattern, articular involvement, stability. |
| Key Instability | Posterolateral rotatory instability (PLRI), +/- varus/valgus. | Primarily PLRI, reducible with intact osseous/ligamentous. | Varus/valgus instability (fracture dependent). | Posteromedial instability with forearm displacement. |
| Surgical Management | Always operative. Radial head replacement, coronoid repair, LUCL repair. | Often non-operative if stable post-reduction. | Often operative (ORIF), total elbow if comminuted. | Always operative (ORIF, sometimes replacement). |
| Prognosis | High risk of stiffness, instability, arthritis. | Good if stable. | Variable, high risk of stiffness/nonunion. | Variable, high risk of stiffness/post-traumatic arthritis. |
Discussion of Differentials:
A
simple elbow dislocation
was considered, but the obvious bony fragments on X-ray ruled this out immediately. A "simple" dislocation implies no significant associated fractures that contribute to instability.
A
complex distal humerus fracture
(e.g., intercondylar C-type) can present with severe pain and deformity. However, the X-rays clearly showed the primary dislocation with separate radial head and coronoid fractures, rather than a primary fracture of the distal humerus articular surface. While such a fracture could coexist, it was not the dominant pattern.
An
olecranon fracture-dislocation
often involves a specific type of coronoid fracture (e.g., terrible triad pattern or specific subsets like trans-olecranon fracture-dislocations). Our patient's radial head fracture and posterolateral instability pattern made terrible triad the more appropriate diagnosis. The critical distinction lies in the primary injury vector and the key stabilizers disrupted.
In our case, the immediate radiological evidence of a posterolateral dislocation coupled with clear fractures of the radial head and coronoid process unequivocally led to the diagnosis of a terrible triad injury. The extent of these fractures and the inherent instability warranted prompt surgical intervention.
Surgical Decision Making & Classification
The decision for operative intervention in this case was straightforward and immediate, driven by the diagnosis of a terrible triad injury of the elbow. This injury pattern is inherently unstable and invariably requires surgical stabilization to restore joint congruity, stability, and function, thereby minimizing the risk of recurrent dislocation, progressive instability, and debilitating post-traumatic arthritis.
Why Operative vs. Non-operative?
*
Inherent Instability:
The terrible triad involves disruption of the primary static stabilizers of the elbow: the LUCL complex (implied by posterolateral dislocation), the radial head (a secondary valgus and rotational stabilizer), and the coronoid process (the primary anterior stabilizer and significant buttress against posterior subluxation). Without surgical repair of these structures, particularly the coronoid and radial head, the elbow remains grossly unstable, precluding even brace protection.
*
Poor Prognosis with Non-operative Management:
Non-operative treatment of terrible triad injuries inevitably leads to persistent instability, recurrent dislocations, severe pain, stiffness, and ultimately a poor functional outcome with high rates of chronic disability and early osteoarthritis.
*
Articular Damage:
Both the radial head and coronoid fractures involve critical articular surfaces. Accurate reduction and stable fixation (or replacement for severe radial head comminution) are essential to prevent progressive joint degeneration.
Classifications Guiding Decision Making:
1.
Mason Classification of Radial Head Fractures:
*
Type I:
Nondisplaced or minimally displaced (<2mm), no mechanical block.
*
Type II:
Displaced (>2mm) or angulated, no comminution.
*
Type III:
Comminuted and displaced.
*
Type IV (Hotchkiss modification):
Mason Type I-III with associated elbow dislocation.
Our patient presented with a Mason Type III radial head fracture with elbow dislocation (making it effectively a Type IV by some classifications), indicating significant articular disruption and comminution that would likely preclude successful open reduction and internal fixation (ORIF) alone. This strongly favored radial head replacement over ORIF.
2.
O'Driscoll Classification of Coronoid Fractures:
*
Type I:
Tip fractures.
*
Type II:
Anteromedial facet fractures (often with varus posteromedial instability).
*
Type III:
Body fractures (trans-coronoid, often with PLRI or terrible triad).
Our patient's coronoid fracture involved more than 50% of the coronoid height and extended into the body, fitting an O'Driscoll Type III pattern. This indicates a substantial loss of the anterior buttress against posterior subluxation and confirms the need for strong fixation. The sublime tubercle involvement often signifies injury to the anterior bundle of the MCL, further compromising stability.
3.
Overall Stability Assessment (Post-Reduction):
While a formal stability assessment under anesthesia would confirm, the extensive bony pathology suggested gross instability even after attempted reduction in the ED. The combined loss of the anterior coronoid buttress, the radial head's contribution to valgus and rotational stability, and the evident LUCL disruption (due to posterolateral dislocation) indicated a universally unstable joint.
The surgical plan therefore focused on a comprehensive approach: addressing the radial head, coronoid, and the lateral collateral ligament complex, in sequence, to restore concentric reduction and achieve stable range of motion.
Surgical Technique / Intervention
The surgical intervention aimed at restoring elbow stability through a stepwise approach: addressing the coronoid fracture, managing the radial head, and repairing the lateral collateral ligament complex.
Patient Positioning: The patient was positioned supine on the operating table with a beanbag, allowing for the ipsilateral arm to be draped freely across the chest. This position facilitates both anterior and posterior approaches if needed, but for a terrible triad, a posterolateral approach is typically used. A pneumatic tourniquet was applied to the upper arm. The entire arm, shoulder, and hand were prepped and draped to allow full visualization and manipulation.
Surgical Approach:
A standard posterolateral approach to the elbow was utilized.
1. An incision was made between the lateral epicondyle and the olecranon, extending proximally along the supracondylar ridge and distally along the ulnar shaft.
2. Careful dissection was performed, protecting the posterior cutaneous nerve of the forearm.
3. The anconeus muscle was reflected subperiosteally off the ulna, exposing the capitellum, radial head, and lateral aspect of the joint.
4. The common extensor origin was elevated anteriorly to expose the lateral epicondyle and the lateral ulnar collateral ligament (LUCL) footprint.
5. A medial incision was not initially planned but prepared for, should medial instability be evident after lateral-sided repair.
Reduction Techniques & Fixation Construct:
-
Coronoid Fracture Fixation (Initial Step for Anterior Stability):
- The posterolateral dislocation was gently reduced. The joint was then opened to visualize the coronoid fracture.
- The large, displaced O'Driscoll Type III coronoid fragment was identified, typically located within the joint or medially.
- A common technique involves using a posterior approach to access the anterior aspect of the coronoid. This can be achieved by carefully reflecting the triceps and identifying the interval between the triceps and the medial head of the gastroc. Alternatively, through a medial approach if associated medial soft tissue injury is significant. For an isolated posterolateral approach, visualization can be challenging, often requiring an additional medial window or using specific retractors. Correction for clarity : For significant coronoid fractures in terrible triad, a separate medial approach between the flexor-pronator mass and the triceps often provides the best visualization and access for strong fixation, especially if the fragment is large and displaced medially, or if suture anchors are planned. If the fragment is small and mainly anterior, passage of sutures via the lateral approach through the joint can be performed. For this case, given the O'Driscoll Type III, a medial approach was utilized to maximize fixation strength.
- A separate 5-cm medial incision was made between the medial epicondyle and the olecranon, carefully protecting the ulnar nerve which was identified and temporarily transposed anteriorly.
- The flexor-pronator mass was elevated from the medial epicondyle.
- The coronoid fragment was reduced anatomically using a dental pick or small periosteal elevator.
- Fixation was achieved using a single or double coronoid suture anchor technique. Two 2.0 mm suture anchors were placed into the base of the coronoid fragment. The sutures were then passed through drill holes created in the proximal ulna, just distal to the coronoid, from anterior to posterior, and tied over the posterior cortex of the ulna. This provided a strong buttress effect and restored the anterior stability.
- Alternatively, for very large fragments, a small plating system (e.g., specific coronoid plate or fragment plate) could be used via the medial approach. Given the significant comminution of the radial head, the goal was to achieve the strongest possible coronoid fixation.
-
Radial Head Management (Secondary Stabilizer):
- After coronoid fixation, attention was turned to the radial head fracture. Given the comminuted Mason Type III fracture, unsuitable for ORIF, a radial head arthroplasty was performed.
- The fractured radial head fragments were carefully excised, ensuring no damage to the capitellum or articular cartilage.
- The radial neck was prepared using appropriate reamers.
- Trial implants (monoblock or modular) were inserted to assess proper sizing, stem length, and congruence with the capitellum and proximal ulna. The aim was to restore radial length and provide stability without overstuffing the radiocapitellar joint.
- Once optimal size was determined, the definitive radial head prosthesis was implanted, typically without cement. The radial stem was placed within the medullary canal of the proximal radius.
- Intraoperative Test for Stability: The elbow was ranged through flexion and extension, pronation and supination, while observing stability. The prosthesis provided a crucial secondary stabilizer against valgus stress and axial migration.
-
Lateral Ulnar Collateral Ligament (LUCL) Repair:
- Following radial head replacement, the elbow's stability was re-assessed. Often, terrible triad injuries involve a tear of the LUCL at its humeral origin.
- The avulsed LUCL was identified at its footprint on the lateral epicondyle.
- A suture anchor repair was performed. One or two 3.0 mm suture anchors were placed into the isometric point of the lateral epicondyle (just proximal and posterior to the center of rotation).
- Strong non-absorbable sutures were then passed through the substance of the avulsed LUCL.
- The sutures were tied with the elbow in approximately 30 degrees of flexion and neutral pronation-supination to restore appropriate tension, providing posterolateral stability.
- If the LUCL was found to be severely attenuated or non-repairable, an augmentation with triceps fascia or a graft could be considered, though primary repair is usually the first line.
Final Stability Assessment:
After all components were addressed, the elbow was stressed dynamically through its full range of motion. Concentric reduction was confirmed. There should be no signs of instability (subluxation, apprehension) under varus, valgus, or rotational stress. The ability to achieve a stable arc of motion (typically from 30 to 130 degrees of flexion with full pronation/supination) without signs of instability is the primary goal.
Closure: The joint capsule and muscle layers were meticulously closed. The subcutaneous tissues and skin were closed in layers. The ulnar nerve was transposed back to its native bed (or kept anteriorly if transposed for fixation and concern for future irritation existed). A sterile dressing was applied, and the arm was placed in a hinged elbow brace in 90 degrees of flexion.
Post-Operative Protocol & Rehabilitation
Post-operative management is as critical as the surgery itself for achieving a successful outcome in terrible triad injuries. The primary goals are to protect the repair, control pain and swelling, gradually restore range of motion, and regain strength.
Phase 1: Protection and Early Motion (Weeks 0-4)
*
Immobilization:
The elbow was initially placed in a hinged elbow brace, locked in 90 degrees of flexion with the forearm in neutral rotation. This position protects the coronoid and LUCL repairs. The brace was typically worn continuously, even during sleep, for the first 1-2 weeks.
*
Pain Management:
Aggressive pain management, including multimodal analgesia (NSAIDs, acetaminophen, neuropathic agents, and short-term opioids), was crucial.
*
Early Motion:
*
Week 0-1:
Gentle active and passive range of motion (AROM/PROM) initiated within a restricted arc, typically 30-90 degrees of flexion/extension, and controlled pronation/supination within a protective range determined by intraoperative stability. This was performed with the brace on, adjusting the hinge limits. Supervised by a hand therapist.
*
Week 1-2:
Progressive increase in range of motion, extending from 20-100 degrees flexion/extension, and gradually increasing pronation/supination as tolerated, ensuring no signs of instability.
*
Continuous Passive Motion (CPM):
Some surgeons advocate for CPM machines, particularly overnight, to prevent stiffness.
*
Edema Control:
Elevation, cryotherapy, and gentle hand/wrist exercises to minimize swelling.
*
Wound Care:
Regular wound checks. Sutures/staples typically removed at 10-14 days.
Phase 2: Progressive Motion and Light Strengthening (Weeks 4-12)
*
Brace Weaning:
The hinged brace was gradually unlocked and worn primarily for protection during activities or sleep, often discontinued by week 6-8, depending on clinical stability and patient progress.
*
Full AROM/PROM:
Emphasis on regaining full elbow flexion, extension, pronation, and supination. Manual therapy by the therapist to address joint stiffness and soft tissue restrictions.
*
Isometric Strengthening:
Introduction of gentle isometric exercises for elbow flexors, extensors, pronators, and supinators.
*
Light Isotonic Strengthening:
By week 8-10, light resistance exercises with low weights or resistance bands, focusing on endurance rather than maximal strength.
*
Scar Management:
Massage and desensitization of surgical scars.
Phase 3: Advanced Strengthening and Return to Activity (Weeks 12-24+)
*
Functional Strengthening:
Progressive increase in resistance and weight-bearing activities. Introduction of sport-specific or work-specific exercises.
*
Proprioception and Coordination:
Exercises to improve neuromuscular control and joint awareness.
*
Endurance Training:
Building overall upper extremity endurance.
*
Gradual Return to Activity:
Controlled return to light work activities by 3-4 months, with full return to heavy labor or contact sports typically not before 6 months, and often up to 9-12 months for full recovery.
*
Monitoring:
Regular follow-up appointments with radiographs to monitor hardware integrity, joint space, and development of heterotopic ossification (HO). Prophylaxis for HO (e.g., indomethacin or radiation) may be considered in high-risk patients.
Potential Complications & Monitoring:
*
Stiffness:
The most common complication. Aggressive therapy is crucial. Manipulation under anesthesia may be considered for refractory cases.
*
Instability/Recurrent Dislocation:
Managed by meticulous surgical technique and adherence to the rehabilitation protocol. Revision surgery may be necessary.
*
Heterotopic Ossification (HO):
Monitored clinically (pain, decreased ROM) and radiographically.
*
Post-traumatic Arthritis:
A long-term risk due to articular damage, particularly if reduction was not perfectly anatomical or if stiffness leads to altered biomechanics.
*
Ulnar Nerve Neuropathy:
Can occur from direct injury, prolonged compression during surgery, or irritation from implants.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
*
Comprehensive Assessment:
Always perform detailed neurological and vascular exams, even if painful. Document thoroughly.
*
Imaging Protocol:
Plain films are a start, but a
CT scan with 3D reconstructions is mandatory
for terrible triad injuries to fully characterize coronoid and radial head fractures for surgical planning.
*
Pre-operative Templating:
Essential for radial head replacement to ensure correct size and avoid overstuffing or undersizing.
*
Surgical Order:
The established "holy trinity" of terrible triad repair:
1.
Coronoid:
Restore the anterior buttress first. Strong fixation (suture anchors or plate) is paramount. If a significant anteromedial coronoid fracture is present (O'Driscoll Type II or III affecting the sublime tubercle), a medial approach is often superior for direct visualization and stable fixation, protecting the MCL attachment.
2.
Radial Head:
Replace if comminuted (Mason Type III/IV). Repair (ORIF) if Mason Type II and amenable. Restoration of radial length is crucial to prevent proximal migration of the radius and maintain valgus stability. Avoid overstuffing.
3.
LUCL:
Repair directly to the lateral epicondyle using suture anchors. This restores posterolateral stability.
4.
MCL (if required):
Inspect the MCL from the medial approach; repair if avulsed or clearly incompetent after bony and lateral ligament repair. This is less common in pure terrible triads but can occur.
*
Intraoperative Stability:
Confirm concentric reduction and a stable range of motion (often 30-130 degrees of flexion with full pronation/supination) after each step of the repair. If unstable, re-evaluate fixation or consider a hinged external fixator.
*
Early, Controlled Mobilization:
The key to preventing stiffness, which is the most common complication. Hinged brace with a defined arc of motion, guided by a skilled hand therapist.
Pitfalls:
*
Inadequate Coronoid Fixation:
Weak or insufficient fixation of the coronoid is a recipe for recurrent instability and failure. Small, intra-articular fragments can be deceptively challenging.
*
Overstuffing the Radiocapitellar Joint:
Using too large a radial head prosthesis can lead to pain, stiffness, early capitellar arthritis, and even component failure. Always use trials and confirm joint space.
*
Missed Instability:
Not adequately assessing stability intraoperatively can lead to early failure. Always test the elbow through full functional ROM under image guidance if needed.
*
Ulnar Nerve Injury:
A risk during medial approaches for coronoid fixation or MCL repair. Prophylactic ulnar nerve transposition may be considered if there is concern for irritation from hardware or post-operative swelling.
*
Heterotopic Ossification (HO):
A common sequela, especially in high-energy trauma. Consider prophylaxis in high-risk patients (e.g., polytrauma, head injury, prior HO).
*
Non-adherence to Rehab:
Patients must understand the critical importance of disciplined, controlled rehabilitation. Lack of compliance can lead to stiffness or re-dislocation.
Brief Considerations on Acromioclavicular (AC) Joint Arthritis Pain:
While not the primary focus of this specific terrible triad case, AC joint arthritis pain is a common orthopedic complaint, particularly in the trauma population (post-traumatic arthritis after AC joint separation). When assessing upper extremity pain, particularly in the shoulder region, AC joint pathology must always be in the differential.
*
Diagnosis:
*
History:
Pain localized to the superior aspect of the shoulder, exacerbated by overhead activities, cross-body adduction, and reaching across the body. History of prior trauma (e.g., fall on the point of the shoulder) is common.
*
Examination:
Localized tenderness over the AC joint. Positive provocative tests: cross-body adduction test, O'Brien's test (with pain localized to AC joint). Pain with resisted shoulder elevation.
*
Imaging:
AP shoulder radiograph with bilateral comparative views, Zanca view (10-15 degrees cephalic tilt) to isolate the AC joint. MRI can show articular cartilage degeneration, subchondral edema, and osteophytes.
*
Management Principles:
*
Conservative:
NSAIDs, activity modification, physical therapy (rotator cuff strengthening, scapular stabilization), corticosteroid injections into the AC joint (diagnostic and therapeutic).
*
Surgical:
Indicated for refractory pain after conservative failure. Typically involves a
distal clavicle excision (DCE)
, either open or arthroscopic (Mumford procedure). This involves resecting 8-10mm of the distal clavicle to create a pain-free space between the clavicle and acromion.
*
Post-operative:
Early motion, progressive strengthening, similar to many shoulder procedures, with expected return to full activity in 3-6 months.
This dual focus on acute, complex elbow trauma and chronic AC joint pathology highlights the broad spectrum of upper extremity conditions encountered by an orthopedic trauma surgeon. While distinct entities, thorough understanding of both acute injury management and chronic arthritic conditions is essential for comprehensive patient care.
