INTRODUCTION TO RADIOCARPAL AND RADIOULNAR SALVAGE
The management of complex distal radius malunions, physeal growth arrests, and advanced radiocarpal arthrosis presents a formidable challenge to the orthopedic hand and wrist surgeon. When joint-preserving osteotomies are no longer viable due to irreversible chondral damage or severe articular incongruity, salvage procedures must be employed to alleviate pain while maximizing residual wrist function.
Radiolunate arthrodesis is a powerful, motion-preserving salvage operation that fuses the radius to the lunate, thereby stabilizing the radiocarpal joint while allowing continued flexion and extension through the midcarpal articulation. Concurrently, dysfunction of the distal radioulnar joint (DRUJ) is a frequent and debilitating source of persistent complaints following distal radius trauma. Addressing DRUJ incongruity—whether through ulnar shortening osteotomy, joint-preserving radial osteotomies, or ablative procedures—is a critical component of comprehensive wrist reconstruction.
This masterclass details the indications, biomechanical rationale, and step-by-step surgical execution of radiolunate arthrodesis (Saffar technique), proximal row carpectomy (PRC), and DRUJ reconstruction.
BIOMECHANICS AND PATHOANATOMY
Understanding the intricate kinematics of the wrist is paramount before undertaking salvage arthrodesis or DRUJ reconstruction. The radiocarpal and distal radioulnar joints function synergistically; an anatomical derangement in one frequently precipitates rapid degeneration in the other.
The Impact of Radial Deformity on the DRUJ
Radioulnar arthrosis is clinically more prevalent than radiocarpal arthrosis following distal radius fractures. Approximately 70% of patients who develop radioulnar arthritis will ultimately require surgical intervention. The deterioration of the DRUJ is primarily driven by shortening and angular deformities of the distal radius:
* Radial Shortening: Cadaveric studies demonstrate that radial shortening produces the most profound kinematic disruptions. A mere 6 mm of radial shortening is sufficient to cause severe DRUJ dysfunction and subluxation.
* Ulnar Variance: A biomechanical analysis reveals that increasing positive ulnar variance by just 2.5 mm dramatically exponentially increases the axial load borne by the distal ulna and the triangular fibrocartilage complex (TFCC), leading to ulnar impaction syndrome.
* Angular Deformity: Decreased radial inclination and loss of normal volar tilt lead to moderate kinematic changes, whereas pure dorsal displacement causes minimal changes in isolated joint kinematics but significantly affects tendon excursion and grip strength.
Clinical Pearl: Significant extra-articular deformities of the distal radius adversely affect DRUJ function by altering the tension of the distal interosseous membrane and the volar/dorsal radioulnar ligaments. Restoring radial length is often the most critical step in DRUJ joint-preserving surgery.
RADIOLUNATE ARTHRODESIS (SAFFAR TECHNIQUE)
Radiolunate arthrodesis is indicated when degenerative changes are isolated to the radiolunate articulation, or in cases of severe ulnar translation of the carpus where the midcarpal joint remains pristine.
Preoperative Evaluation
A meticulous assessment of the midcarpal joint is mandatory. The success of a radiolunate arthrodesis relies entirely on a healthy articulation between the head of the capitate and the distal lunate/scaphoid. If the capitate cartilage is compromised, a total wrist arthrodesis or total wrist arthroplasty must be considered instead.
Surgical Technique: Step-by-Step
1. Positioning and Approach
* Place the patient supine with the operative arm on a radiolucent hand table. Apply a well-padded proximal tourniquet.
* Approach the wrist through a longitudinal dorsal incision, centered over Lister's tubercle.
* Incise the extensor retinaculum over the third dorsal compartment. Transpose the extensor pollicis longus (EPL) tendon radially.
* Elevate the second and fourth compartment tendons subperiosteally to expose the dorsal wrist capsule. Perform a ligament-sparing dorsal capsulotomy to expose the radiocarpal joint.
2. Articular Assessment and Preparation
* Directly visualize and assess the status of the midcarpal cartilage, paying special attention to the head of the capitate.
* Once midcarpal health is confirmed, proceed to excise the remaining articular cartilage from the lunate fossa of the distal radius and the proximal articular surface of the lunate. Use a combination of sharp curettes and a high-speed burr to expose bleeding subchondral bone, ensuring a highly vascularized bed for arthrodesis.
3. Carpal Distraction and Alignment
* Apply manual longitudinal distraction to the hand. This maneuver is critical to regain normal carpal height and to allow the scaphoid—which is often rotary subluxated—to return to its anatomical alignment.
* Temporary Kirschner wire (K-wire) fixation between the scaphoid and capitate, or radius and scaphoid, may be utilized to hold this distracted, realigned position during graft placement.
4. Graft Harvesting and Trough Creation
* Harvest a robust corticocancellous bone graft from the ipsilateral iliac crest.
* Create a precise, rectangular trough in the dorsomedial aspect of the distal radius and extending into the dorsal lunate.
* Alternative: A local sliding graft can be fashioned from the dorsal distal radius and translated distally to bridge the radiolunate articulation, though iliac crest provides superior osteogenic potential.
5. Graft Interposition and Impaction
* Interpose the corticocancellous graft into the prepared trough. The graft serves a dual purpose: it acts as a biological bridge for fusion and a structural spacer to restore normal carpal height, effectively disimpacting the carpus from the radius.
* Pack any surplus cancellous bone tightly into the remaining interstices between the radius and lunate.
Surgical Warning: The dorsal aspect of the corticocancellous graft must sit perfectly flush with, or slightly recessed below, the level of the dorsal radius. A proud graft will inevitably impede the glide of the extensor tendons, leading to severe tenosynovitis or attritional tendon rupture.
6. Rigid Internal Fixation
* Stabilize the graft and the radiolunate joint using rigid internal fixation. The Saffar technique recommends two compression screws: one passed through the graft into the palmar surface of the radius, and the second through the graft into the palmar aspect of the lunate.
* Alternative Fixation: A low-profile dorsal spanning plate or memory-compression staples can be highly effective.
* Contraindication: Kirschner wire fixation alone is strictly not recommended due to the lack of dynamic compression and high rates of nonunion.
7. Addressing the DRUJ
* Perform any additional procedures necessary to treat concurrent DRUJ pathological processes (e.g., ulnar shortening, Darrach, or Suave-Kapandji procedures) before final closure.
Postoperative Care Protocol
- Days 0-4: Apply a bulky volar splint in neutral position to control edema and protect the fixation.
- Day 4 to Union: Replace the splint with a rigid short-arm cast. Cast immobilization is strictly maintained until radiographic evidence of solid bony union is observed (typically 6 to 8 weeks).
- Rehabilitation Phase: Once union is confirmed and the cast is removed, initiate progressive range-of-motion (ROM) and strengthening exercises daily for the subsequent 2 months, focusing on midcarpal flexion/extension and forearm rotation.
PROXIMAL ROW CARPECTOMY (PRC) AS A SALVAGE OPTION
Proximal row carpectomy is a motion-preserving procedure that involves the excision of the scaphoid, lunate, and triquetrum, allowing the capitate to articulate directly with the lunate fossa of the radius.
While highly effective for SLAC/SNAC wrists, PRC has limited indications for the salvage of distal radial malunions.
Indications and Strict Contraindications
In the unusual case where the cartilage of the proximal capitate and the lunate facet of the radius are completely intact, and degenerative arthritis is strictly limited to the radial side of the wrist (e.g., scaphoid fossa), PRC is a viable option.
Surgical Pitfall: PRC is absolutely contraindicated in patients with a step-off or incongruity between the scaphoid and lunate fossae of the distal radius. It is also contraindicated if there is any destruction of the articular cartilage of the lunate facet, as the capitate will rapidly degenerate against a compromised radial surface.
For patients with heavy functional demands where PRC is contraindicated, total wrist arthrodesis is preferred. Total wrist arthroplasty remains a salvage procedure restricted exclusively to low-demand, elderly patients.
DISTAL RADIOULNAR JOINT (DRUJ) INCONGRUITY AND ARTHROSIS
Dysfunction of the DRUJ is a frequent source of persistent, debilitating complaints following distal radial malunions. Characteristic symptoms include ulnar-sided wrist pain, significantly decreased forearm rotation (supination/pronation), decreased grip strength, and subjective instability.
These symptoms can be caused by:
1. Malunion of fractures extending into the sigmoid notch.
2. Chronic injuries to the triangular fibrocartilage complex (TFCC).
3. Palmarly displaced malunions of ulnar styloid fractures.
4. Extra-articular radial deformities altering DRUJ kinematics.
Management of Positive Ulnar Variance
Positive ulnar variance—protrusion of the ulna distal to its normal articulation with the ulnar notch of the radius—causes consequent impingement on the carpus (Ulnar Impaction Syndrome). This is commonly caused by malunited Colles fractures, radial nonunions, or premature cessation of distal radial physeal growth.
This length discrepancy can be surgically managed in one of three ways:
1. Restoration of Radial Length: Via distal radius corrective osteotomy.
2. Ulnar Shortening: Via diaphyseal osteotomy.
3. Ablative Resection: Partial (hemiresection arthroplasty) or complete (Darrach procedure) resection of the distal ulna.
Joint-Preserving Procedures
Joint-preserving procedures afford a more anatomical reconstruction and better preservation of joint kinematics. Preservation of the DRUJ is highly recommended when the joint can be congruously reduced and arthritic changes are minimal.
Ulnar Shortening Osteotomy:
An ulnar shortening osteotomy alone is indicated if:
* The radial deformity is not severe (< 10 degrees of abnormal angulation in the frontal and sagittal planes).
* There is unacceptable positive ulnar variance.
* The DRUJ is reducible.
In addition to restoring joint congruity and unloading the ulnar side of the wrist, diaphyseal ulnar shortening effectively tightens the ulnocarpal ligaments and the TFCC, thereby stabilizing the distal ulna.
Distal Radial Osteotomy:
If the radial deformity is unacceptable (>10 degrees angulation), a distal radial osteotomy alone frequently realigns the DRUJ, especially if the initial radial shortening is 6 mm or less. If positive ulnar variance persists after the radius is corrected, a concurrent ulnar shortening procedure can be performed.
Pediatric Considerations: Distal Radial Growth Arrest
If the discrepancy in length is the result of an abnormality or premature cessation of growth of the distal radial physis, the ulna becomes relatively lengthened and will impinge heavily on the carpus.
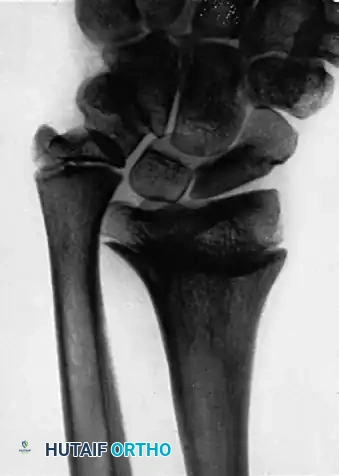
(Above: Disproportion in length of radius and ulna secondary to injury of the distal radial physis, demonstrating severe positive ulnar variance and carpal impingement.)
In growing children, the stability provided by the distal ulna and its ligaments must be preserved. Therefore, instead of resecting the distal ulna and its physis (which would arrest ulnar growth entirely and destroy the TFCC attachments), a segment of the ulnar shaft should be resected. This shortens the ulna enough to allow its head to articulate congruously with the ulnar notch of the radius while preserving the distal growth plate.
If the child is approaching skeletal maturity and prevention of further growth of the distal ulna is desirable, the resection may include the distal ulnar physis (e.g., a Milch cuff resection).
Ablative Procedures for the DRUJ
If pain in the DRUJ persists after joint-preserving procedures, or if severe arthrosis is present at the sigmoid notch, an ablative procedure is indicated.
Usually, a segment is removed approximately 2.5 cm proximal to the head of the ulna, ensuring it is long enough to correct the discrepancy in length of the two bones and prevent painful radioulnar impingement during pronation.
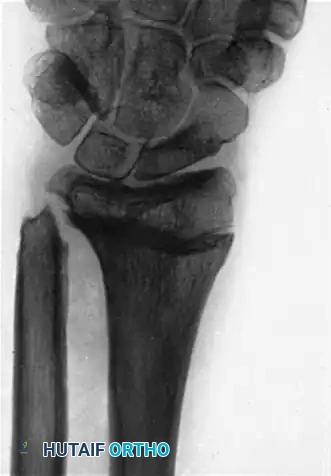
(Above: Postoperative radiograph after resection of the distal end of the ulna. Note the clearance achieved to decompress the ulnocarpal articulation.)
While the Darrach procedure (complete resection of the distal ulna) is effective for pain relief in low-demand patients, it carries a high risk of postoperative ulnar stump instability and radioulnar convergence. In higher-demand patients requiring ablation, the Sauvé-Kapandji procedure (DRUJ arthrodesis with proximal ulnar pseudoarthrosis) or hemiresection interposition arthroplasty are generally preferred to maintain the ligamentous sling of the ulnar carpus.
COMPLICATIONS AND PITFALLS
Surgeons performing radiolunate arthrodesis and DRUJ reconstructions must be vigilant regarding several high-risk complications:
- Nonunion of the Arthrodesis: The radiolunate joint has a small surface area. Failure to achieve bleeding subchondral bone, inadequate bone grafting, or the use of non-compressive fixation (K-wires alone) significantly increases nonunion rates.
- Extensor Tendon Rupture: As emphasized, dorsal hardware or proud bone grafts will cause attritional rupture of the extensor digitorum communis or EPL. Meticulous dorsal contouring and retinacular repair are mandatory.
- Persistent Ulnar-Sided Pain: Failure to adequately address positive ulnar variance during radiocarpal reconstruction will leave the patient with debilitating ulnar impaction syndrome. Always assess DRUJ kinematics intraoperatively after the radiolunate fusion is provisionally fixed.
- Ulnar Stump Impingement: Following a Darrach procedure, excessive resection of the ulna can lead to dynamic convergence of the ulnar stump against the radius during heavy lifting, necessitating secondary stabilization procedures.
