PRINCIPLES OF TREATMENT IN HAND TRAUMA
The fundamental objective in the management of metacarpal and phalangeal fractures is the rapid restoration of functional anatomy while minimizing iatrogenic injury to the delicate soft-tissue envelope. For the vast majority of closed fractures involving the metacarpals and phalanges, conservative management—comprising closed manipulation, proper splinting in the intrinsic-plus (position of function), and early protected motion—produces excellent functional outcomes.
However, the hand is an unforgiving anatomical region where even minor skeletal malalignments can lead to profound functional deficits, such as digital overlapping, loss of grip strength, and severe joint contractures. When conservative measures fail to achieve or maintain an acceptable reduction, operative intervention becomes mandatory. The decision to proceed with closed reduction and percutaneous pinning (CRPP) or open reduction and internal fixation (ORIF) requires meticulous clinical judgment, a deep understanding of hand biomechanics, and precise surgical execution.
Clinical Pearl: The soft-tissue envelope of the hand dictates the timing and nature of surgical intervention. Percutaneous pinning should be attempted early, before profound edema obliterates external anatomical landmarks. Conversely, if the soft-tissue envelope is massively swollen, a deliberate delay in open fixation of 7 to 10 days is often warranted to allow the edema to subside, thereby reducing the risk of wound dehiscence and deep infection. If necessary, the extremity should be strictly elevated for 24 to 48 hours prior to reduction and pinning.
Indications for Operative Fixation
Surgical stabilization—whether via percutaneous K-wires, interfragmentary screws, or plate osteosynthesis—is strictly indicated in the following clinical scenarios:
- Displaced Intra-articular Fractures: When a fracture involves a significant portion of the articular surface (typically >25% or with >1mm step-off), exact anatomical reduction is paramount to restore smooth joint kinematics and prevent early-onset post-traumatic osteoarthritis.
- Major Ligamentous or Tendinous Avulsions: Fractures that represent the bony avulsion of critical stabilizing structures (e.g., bony mallet finger with subluxation, or massive collateral ligament avulsions) require fixation to restore the tension band effect of the musculotendinous unit.
- Irreducible Fractures: When a fracture is so severely displaced that the interposition of tendons, volar plate, or other soft tissues prevents realignment by closed manipulation.
- Multiple Fractures (Polytrauma of the Hand): When multiple metacarpal or phalangeal fractures are present, the hand loses its structural architectural framework and cannot be held in the position of function without internal fixation.
- Open Fractures: Internal fixation provides rigid skeletal stability, which is a prerequisite for soft-tissue healing. It allows for aggressive postoperative wound care, repeated debridement, and dressing changes without the risk of losing fracture reduction.
Surgical Warning: Severely comminuted closed fractures of the phalangeal shafts should generally not be opened. The periosteal stripping required to expose multiple tiny fragments often devascularizes the bone, leading to nonunion, and creates massive scar tissue that binds the extensor mechanism. In these cases, limited percutaneous pinning or external fixation is the treatment of choice.
CLINICAL EVALUATION OF ROTATIONAL ALIGNMENT
Rotational malalignment is the most commonly missed deformity in hand fractures and is poorly visualized on standard anteroposterior and lateral radiographs. A rotational deformity of merely 5 degrees at the metacarpal base can result in 1.5 cm of digital overlap at the fingertips, severely impairing the patient's ability to form a tight fist.
Clinical assessment of rotation must be performed meticulously. During flexion, all digits should point toward the scaphoid tubercle.
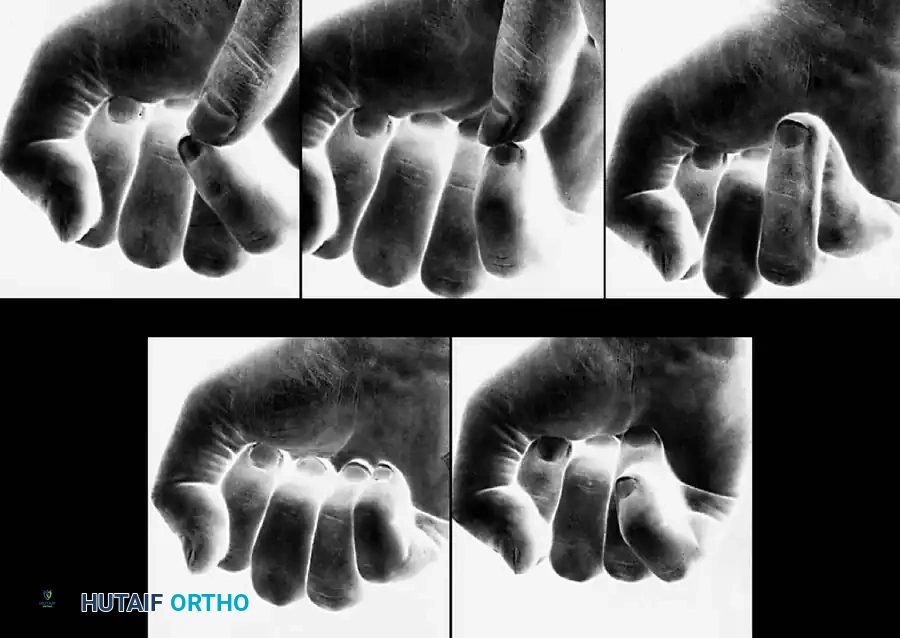
Figure 64-3: Assessment of Rotational Deformity in the Little Finger.
A, Note the alignment of a normal little finger during flexion. B, A normal little finger can be passively manipulated to overlap the ring finger. With incomplete flexion, this overlap may be falsely perceived as a rotational deformity. C, Rotation of the little finger at the carpometacarpal (CMC) joint may be accentuated by passive assistance. D, From the normal alignment of the little finger, true external rotation is impossible. E, Incomplete flexion of the ring finger may simulate a rotational deformity because it tends to overlap the little finger.
During surgical fixation, rotational alignment must be verified repeatedly. The hand must be taken through a passive range of motion, flexing the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and distal interphalangeal (DIP) joints fully. The injured digit must be compared with the adjacent uninjured fingers before definitive rotational control is locked in with implants.
MANAGEMENT OF DISLOCATIONS
Most simple dislocations of the PIP and DIP joints can be managed readily by closed manipulation, reduction, and early protected function. Many are self-reduced by the patient at the scene of the injury. Following reduction, "buddy taping" the injured digit to an adjacent stable finger generally provides an excellent functional result while allowing early active motion to prevent stiffness.
However, the surgeon must maintain a high index of suspicion for associated ligamentous incompetence or tendon avulsions. Operative intervention for dislocations is required in the following specific conditions:
- Unstable Carpometacarpal (CMC) Dislocations: Particularly of the thumb or the ulnar digits, where closed reduction cannot be maintained due to the deforming forces of the extrinsic tendons.
- Thumb MCP Dislocations with Complete UCL Rupture: A Stener lesion (where the adductor aponeurosis becomes interposed between the ruptured ulnar collateral ligament and its insertion) prevents healing and mandates open repair.
- Complex Dislocations: Where a tendon, volar plate, or sesamoid is trapped within the joint space, rendering the dislocation irreducible by closed manipulative maneuvers.
- Old, Undiagnosed Dislocations: Where soft-tissue contracture and fibrosis necessitate open release and reduction.
- "Buttonhole" (Boutonnière) Dislocations: Where the head of the proximal phalanx herniates through a rent in the extensor mechanism.
OPEN FRACTURES AND DISLOCATIONS
The management of open hand trauma demands a systematic, aggressive approach to prevent deep space infection and osteomyelitis.
Irrigation, Debridement, and Skeletal Stabilization
In open fractures and dislocations, the initial step is meticulous surgical debridement and copious pulsatile or gravity irrigation. Once the wound is surgically clean, the fractures must be reduced and stabilized. Rigid stabilization is critical; it allows finger motion as soon as soft-tissue healing permits and facilitates wound inspection without loss of fracture alignment.
If the hand is severely traumatized, additional surgical incisions are usually unnecessary to expose the fracture; the traumatic wound itself, if appropriately extended, provides adequate access. Fractures should be fixed under direct vision or percutaneously to restore the normal architectural columns of the hand.
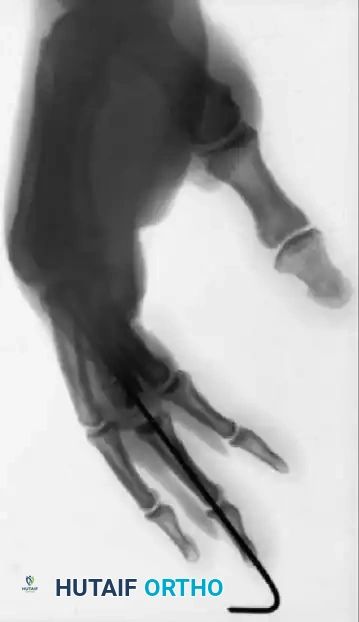

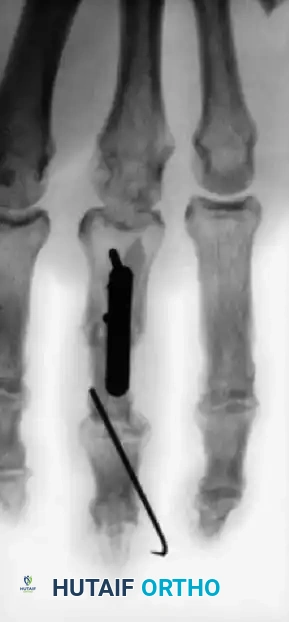
Figure 64-4: Massive Trauma and Reconstructive Efforts.
A and B, Severe open fractures of the right hand demonstrating loss of the distal end of the middle phalanx and a painful, partially amputated small finger. C and D, Innovative reconstructive salvage: The proximal phalanx of the painful and stiff small finger was harvested and utilized as a structural bone graft to restore the articular column and length of the middle finger.
Segmental Bone Loss and Soft Tissue Coverage
In cases of massive trauma with segmental defects of the tubular bones, immediate definitive bone grafting is contraindicated due to infection risk. Instead, temporary spacers—often fashioned from heavy Kirschner wire bent into the shape of a "U"—can be inserted to maintain length and prevent soft-tissue collapse while the wound heals.
Judgment is paramount in determining wound closure. If there is any doubt regarding the adequacy of debridement or the viability of the tissues, the wound must be left open for repeat debridement and irrigation at 48 hours. Closing a compromised wound under tension is disastrous; the inevitable postoperative edema within the first 48 hours will strangulate the skin edges, leading to full-thickness necrosis.
The ultimate goal is to achieve definitive wound closure or coverage within the first 4 to 5 days, before aggressive granulation tissue forms and fibrotic contractures develop. Exposed tendons devoid of their paratenon or synovial sheath will rapidly desiccate and necrose without appropriate vascularized coverage (e.g., local rotational flaps or cross-finger flaps).
Antibiotic Protocols
Routine culturing of acute open hand injuries in the emergency department is no longer recommended unless there is evidence of gross, prolonged contamination (e.g., farm injuries, aquatic environments). While recent literature emphasizes that vigorous irrigation and sharp debridement are the most critical factors in preventing infection, prophylactic intravenous antibiotics remain the standard of care. They are especially vital when essential tissues have borderline viability or when microscopic contamination likely remains despite thorough debridement.
BASIC BONE TECHNIQUES AND IMPLANT SELECTION
The modern orthopedic surgeon has access to a vast array of devices for the internal and external fixation of hand fractures. Considerable clinical judgment is required to select the specific device that provides the best opportunity for the restoration of normal function while minimizing soft-tissue morbidity.
Pitfall: Ill-advised plating of the tubular bones of the phalanges is a common source of iatrogenic complication. The extensor mechanism glides mere millimeters above the periosteum; bulky plates can cause severe tendon adhesions, extensor lag, tendon ruptures, and skin sloughs. Plating should be reserved for specific indications, such as multiple metacarpal shaft fractures or complex peri-articular injuries where absolute stability is required.
Kirschner Wire (K-wire) Fixation
Rarely is more fixation needed than that afforded by Kirschner wires combined with external splinting. K-wires (typically 0.035 or 0.045 inches in diameter) are versatile, require minimal soft-tissue stripping, and can be placed percutaneously.
K-wires should be sharpened on both ends. This allows the surgeon to drill the wire antegrade through the fracture site and out the distal cortex/skin, reduce the fracture, and then drill the wire retrograde back across the fracture site into the proximal fragment.
Certain unstable fracture patterns benefit from augmenting K-wires with tension band wiring or 90/90 intraosseous wiring. This converts tensile distraction forces at the dorsal cortex into dynamic compression forces at the volar cortex during active flexion.
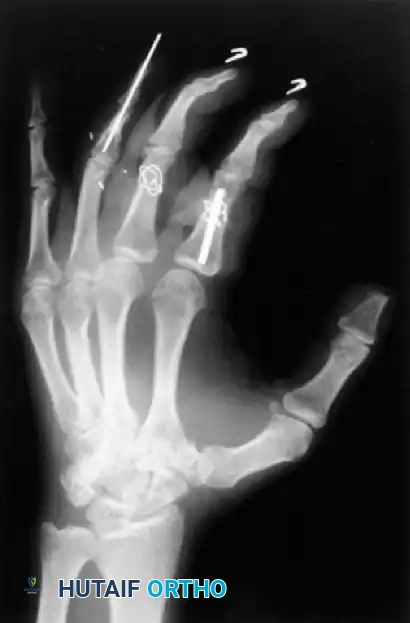
Figure 64-5: Advanced Wiring Techniques.
Various techniques employed to manage middle phalangeal fractures during a complex multidigit replantation. Note the combination of an intramedullary Kirschner wire rod with supplemental wiring in the index finger, and intraosseous wiring alone in the middle finger, both achieving excellent rotational control.
Interfragmentary Screw Fixation
Unstable, long oblique, or spiral fractures of the metacarpals and proximal phalanges are often best treated with interfragmentary lag screw fixation alone. The fracture length must be at least twice the diameter of the bone to accommodate two or more screws safely. This technique provides absolute stability and dynamic compression, allowing for immediate active range of motion without the need for bulky plates.
External Fixation
External fixators are highly useful for highly comminuted intra-articular fractures (e.g., pilon fractures of the PIP joint) utilizing the principles of ligamentotaxis, or for severe open fractures with bone loss. However, the surgeon must be cautious, as external fixator pins can impinge on the sagittal bands, lateral bands, or collateral ligaments, severely interfering with postoperative function.
Surgical Instrumentation
Except for dedicated minifragment plate and screw sets or specialized external fixator frames, very little heavy equipment is required for hand trauma. The same delicate instruments used for soft-tissue handling are employed for bone manipulation. A straight Kocher clamp or a pointed reduction towel clip is usually sufficient to provisionally reduce a metacarpal shaft fracture. For smaller phalangeal fragments, a fine hemostat is ideal for holding the reduction prior to provisional K-wire fixation. Because the bones of the hand are small and fragile, dental instruments, small rasps, and micro-bone cutters are highly useful adjuncts on the sterile field.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The success of operative hand fracture management relies as much on postoperative rehabilitation as it does on surgical execution.
- Immobilization: Immediately postoperatively, the hand should be immobilized in a bulky, non-compressive dressing with a volar plaster splint. The hand must be placed in the "intrinsic-plus" position: the wrist extended 20 to 30 degrees, the MCP joints flexed 70 to 90 degrees, and the PIP/DIP joints in full extension. This position maintains the collateral ligaments of the MCP joints at their maximal length (preventing extension contractures) and prevents volar plate contractures at the PIP joints.
- Elevation: Strict elevation above the level of the heart is mandatory for the first 48 to 72 hours to mitigate edema, which is the primary enemy of hand function.
- Early Active Motion: If rigid internal fixation (e.g., lag screws or plates) was achieved, early active motion under the guidance of a certified hand therapist should commence within 3 to 5 days. If K-wires were used, motion may be delayed or restricted to protected arcs until early clinical union is evident (typically 3 to 4 weeks), at which point the pins are removed in the clinic and aggressive rehabilitation begins.
