Posterior Approach for Harvesting Vascularized Fibular Grafts: A Comprehensive Surgical Guide
Key Takeaway
The posterior approach for harvesting a vascularized fibular graft is a highly specialized orthopedic procedure requiring meticulous dissection. This technique utilizes the interval between the peroneus longus and soleus muscles to safely isolate the fibula and its peroneal vascular pedicle. Proper patient positioning, precise extraperiosteal dissection, and careful protection of the superficial peroneal nerve are critical to ensuring graft viability and minimizing donor-site morbidity.
INTRODUCTION TO VASCULARIZED FIBULAR GRAFTING
The free vascularized fibular graft (FVFG) remains one of the most versatile and biomechanically robust options in the armamentarium of the reconstructive orthopedic microsurgeon. Pioneered and refined by surgical luminaries such as Gilbert, Tamai et al., and Weiland, the posterior approach for harvesting the fibular graft provides unparalleled access to the fibular diaphysis and its vascular pedicle.
The fibula is uniquely suited for reconstructing massive segmental bone defects resulting from trauma, oncologic resection, or congenital pseudarthrosis. It offers up to 25 centimeters of dense, straight cortical bone that can withstand significant biomechanical loads once incorporated. Furthermore, its dual blood supply—via the endosteal nutrient artery and the periosteal segmental vessels derived from the peroneal artery—ensures robust osteocyte viability, rapid incorporation at the recipient site, and resistance to infection.
This masterclass delineates the posterior approach for harvesting a fibular graft, providing a rigorous, step-by-step academic guide tailored for orthopedic residents, microsurgical fellows, and practicing consultants.
SURGICAL ANATOMY AND BIOMECHANICS
A profound understanding of the lateral and posterior compartments of the leg is non-negotiable for safe graft harvest.
Osteology and Biomechanics
The fibula acts as a lateral strut for the lower extremity, serving primarily as a site for muscle attachment rather than axial weight-bearing. Only about 10% to 15% of the body's weight is transmitted through the fibula. However, the proximal and distal ends are biomechanically critical. The proximal fibula is integral to the stability of the posterolateral corner of the knee and houses the common peroneal nerve. The distal fibula forms the lateral malleolus, which is essential for the integrity of the ankle mortise.
Surgical Warning: To prevent catastrophic destabilization of the knee and ankle, a minimum of 6 to 8 centimeters of the proximal fibula and 6 to 8 centimeters of the distal fibula must be preserved during harvest. In pediatric patients, preserving the distal syndesmosis is critical to prevent progressive valgus deformity of the ankle.
Vascular Anatomy
The vascular basis of the FVFG is the peroneal artery and its venae comitantes. The peroneal artery arises from the tibioperoneal trunk and descends through the deep posterior compartment of the leg, lying medial to the fibula and deep to the flexor hallucis longus (FHL) muscle. It supplies the fibula via a primary nutrient artery (typically entering the middle third of the diaphysis) and multiple musculoperiosteal branches.
Neurologic Considerations
Two major nerves dictate the boundaries of the dissection:
1. Common Peroneal Nerve: Winds around the fibular neck proximally.
2. Superficial Peroneal Nerve: Courses within the lateral compartment, lying intimately against the fibula before piercing the crural fascia in the distal third of the leg.
PREOPERATIVE PLANNING AND INDICATIONS
Indications
- Segmental Bone Defects: Traumatic or post-infectious diaphyseal defects exceeding 6 centimeters.
- Oncologic Reconstruction: Following intercalary resection of primary bone sarcomas.
- Avascular Necrosis (AVN): Core decompression and vascularized fibular grafting for pre-collapse AVN of the femoral head.
- Congenital Deformities: Congenital pseudarthrosis of the tibia or radius.
Preoperative Imaging
Standard orthogonal radiographs of the tibia and fibula are mandatory to assess bone quality and rule out prior occult trauma.
Clinical Pearl: Preoperative angiography or Computed Tomography Angiography (CTA) of the lower extremities is highly recommended. The surgeon must confirm a patent three-vessel runoff to the foot. If the patient possesses a peroneal arteria magna (where the peroneal artery is the dominant supply to the foot due to hypoplastic anterior or posterior tibial arteries), harvesting the fibula with its pedicle is strictly contraindicated to avoid catastrophic foot ischemia.
PATIENT POSITIONING AND PREPARATION
Optimal positioning is critical to facilitate simultaneous access by two surgical teams (one at the donor site, one at the recipient site) and to allow gravity to assist in the retraction of the posterior musculature.
- Positioning: Place the patient in the supine position.
- Limb Orientation: Flex the donor extremity at the hip and the knee. Internally rotate the foot slightly to bring the posterolateral aspect of the leg into the operative field.
- Support: Place a large sandbag or a specialized gel bump under the ipsilateral buttock to maintain the internal rotation and stabilize the pelvis.
- Tourniquet: Apply a well-padded pneumatic tourniquet to the proximal thigh. During the initial portion of the dissection, the tourniquet is inflated to maintain a bloodless field, which is essential for identifying delicate intermuscular septa and the vascular pedicle.
STEP-BY-STEP SURGICAL TECHNIQUE: THE POSTERIOR APPROACH
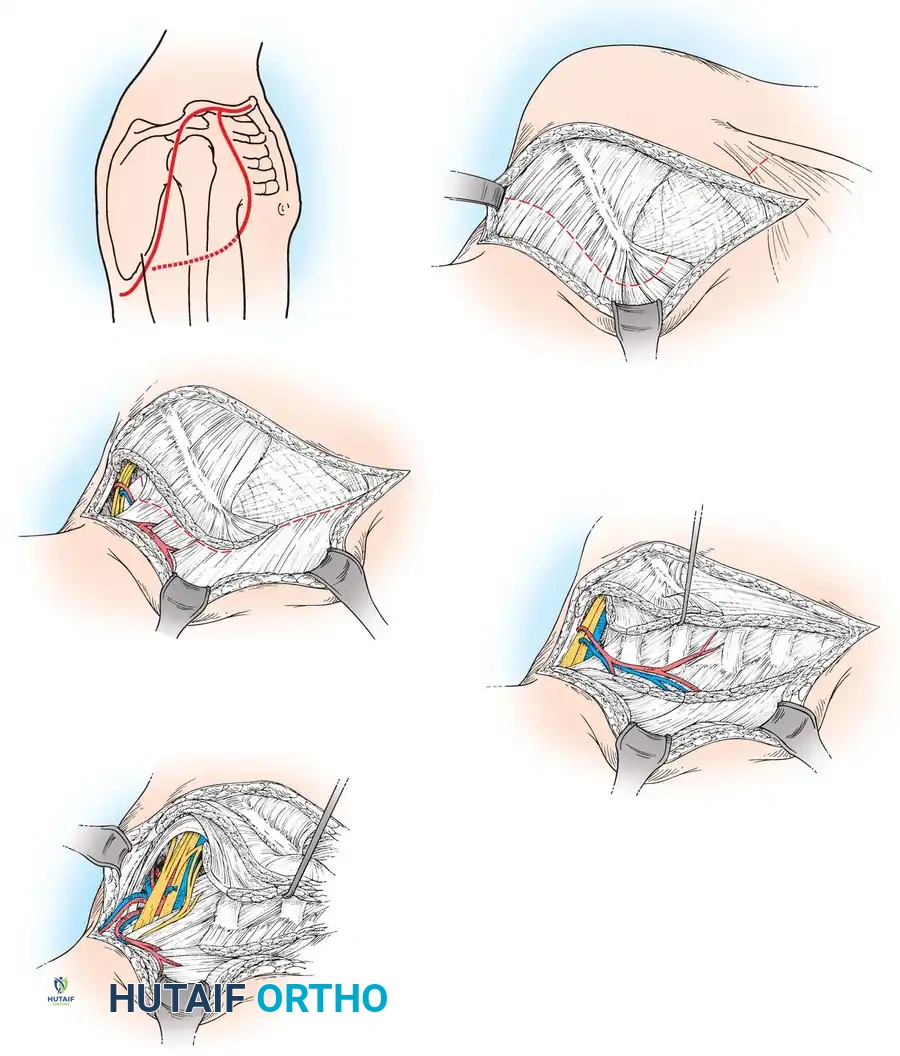
The posterior approach (often associated with the lateral decubitus or modified supine position) utilizes the internervous and intermuscular planes to safely isolate the fibula.
1. Incision and Superficial Dissection
- Make a longitudinal incision centered over the fibula along the lateral aspect of the leg.
- The incision should extend from the neck of the fibula proximally, coursing distally toward the lateral malleolus of the ankle.
- Incise the skin and subcutaneous tissues sharply down to the superficial crural fascia. Maintain meticulous hemostasis of the superficial venous network.
2. Developing the Intermuscular Interval
- Identify the interval between the peroneus longus muscle (lateral compartment) and the soleus muscle (superficial posterior compartment).
- Incise the aponeurosis longitudinally.
- Proceed with the dissection posterior to the peroneus longus muscle and anterior to the soleus muscle.
Clinical Pearl: In the proximal leg, the muscle bellies can be dense and the fascial planes indistinct. To ensure correct orientation, identify the peroneus longus tendon in the distal part of the incision where the anatomy is more defined, and trace the interval proximally.
3. Elevation of the Soleus Muscle
- Incise the fascia along the interval between the soleus muscle posteriorly and the peroneus longus muscle laterally.
- Begin in the distal portion of the wound. Using blunt dissection (such as a sweeping motion with a sponge or a blunt elevator), elevate the soleus muscle off the deep posterior compartment.
- Proceed proximally until the origin of the soleus muscle on the proximal fibula is encountered.
- Pedicle Identification: At this juncture, carefully inspect the area just deep to the soleus. The peroneal vessels (artery and venae comitantes) will be identified lying nearly in contact with the fibula.
- Once the pedicle is visually confirmed and protected, sharply incise the fibular origin of the soleus. This release allows for adequate posterior retraction of the soleus, providing wide exposure for the subsequent pedicle dissection.
4. Managing the Deep Posterior Compartment and FHL
- With the soleus retracted posteriorly, identify the interval between the peroneal muscles and the flexor hallucis longus (FHL) in the distal portion of the leg.
- Look for a thin line of adipose tissue just posterior to the peroneals; this serves as a reliable anatomical landmark for the interval.
- The FHL lies posterior to the peroneals and deep to the soleus, covering the posterolateral surface of the fibula.
- Crucial Anatomical Relationship: The peroneal vessels course within or deep to the flexor hallucis longus muscle. By maintaining the FHL over the vessels, the pedicle remains protected during the anterior dissection.
5. Extraperiosteal Dissection of the Peroneal Muscles
- Retract the peroneal muscles (longus and brevis) anteriorly.
- Sharply dissect the peroneal muscles off the lateral surface of the fibula in an extraperiosteal fashion. It is vital to leave the periosteum intact on the fibular graft to preserve the periosteal blood supply derived from the peroneal vessels.
Surgical Warning: During the anterior retraction and extraperiosteal dissection of the peroneal muscles, the surgeon must carefully identify and protect the superficial peroneal nerve. This nerve is closely applied to the fibula in the proximal and middle thirds of the wound before it pierces the fascia. Overzealous retraction or careless scalpel work here can result in permanent sensory loss over the dorsum of the foot and potential neuroma formation.
6. Fibular Osteotomies
- Determine the exact length of the graft required based on preoperative templating of the recipient site.
- Mark the osteotomy sites, ensuring a minimum of 6 to 8 cm of fibula is left intact proximally (to protect the common peroneal nerve and knee stability) and distally (to preserve the syndesmosis and ankle stability).
- Pass malleable retractors or right-angle retractors subperiosteally only at the specific sites of the osteotomies to protect the underlying deep structures.
- Perform the osteotomies using an oscillating saw or a Gigli saw. Copious saline irrigation must be used during the saw cuts to prevent thermal necrosis of the bone ends.
7. Pedicle Isolation and Graft Harvest
- Once the osteotomies are complete, place a bone hook in the medullary canal of the proximal end of the mobilized fibular segment and apply gentle lateral traction.
- This traction places the interosseous membrane on stretch. Sharply divide the interosseous membrane from distal to proximal, staying close to the fibula to avoid injuring the anterior tibial vessels.
- As the fibula is rotated outward, the peroneal pedicle is fully exposed.
- Trace the peroneal artery and venae comitantes proximally to their origin at the tibioperoneal trunk to maximize pedicle length.
- Deflate the tourniquet. Observe the graft for active bleeding from the medullary canal and periosteum, confirming robust perfusion.
- Once viability is confirmed and the recipient site is prepared, ligate the distal peroneal vessels, followed by the proximal vessels, and transfer the graft.
POSTOPERATIVE PROTOCOL AND DONOR SITE MANAGEMENT
Meticulous closure and postoperative care of the donor site are imperative to minimize morbidity.
Wound Closure
- Achieve absolute hemostasis using bipolar electrocautery.
- Insert a closed-suction drain into the deep posterior compartment bed to prevent hematoma formation, which could lead to compartment syndrome.
- Reapproximate the muscle fascia loosely. Do not close the fascia tightly, as the lateral and deep posterior compartments are highly susceptible to postoperative compartment syndrome.
- Close the subcutaneous tissue and skin in a standard layered fashion.
Rehabilitation and Weight-Bearing
- Immobilization: The donor leg is typically placed in a bulky Jones dressing or a posterior splint with the ankle in neutral dorsiflexion to prevent equinus contracture.
- Weight-Bearing: Patients are generally restricted to partial weight-bearing (toe-touch) on the donor leg for the first 4 to 6 weeks to allow the soft tissues to heal and to prevent stress fractures of the tibia, which now bears the full axial load.
- Physical Therapy: Early active and passive range of motion of the toes (especially the great toe, to prevent FHL tethering) and the knee is encouraged. Progressive strengthening of the peroneal muscles and ankle stabilizers begins at 6 weeks postoperatively.
COMPLICATIONS AND PITFALLS
While the posterior approach is highly reliable, surgeons must be vigilant regarding potential donor-site morbidities:
- Nerve Injury: The most common neurologic complication is neuropraxia or transection of the superficial peroneal nerve during anterior compartment retraction. Proximal dissection too close to the fibular head risks common peroneal nerve palsy, resulting in foot drop.
- Flexor Hallucis Longus Tethering: Scarring of the FHL muscle belly can lead to a flexion contracture of the great toe. Early mobilization is the best preventative measure.
- Ankle Instability and Valgus Deformity: Harvesting the fibula too distally compromises the syndesmosis. In pediatric patients, the distal fibula must be rigidly stabilized (often with a syndesmotic screw) if the harvest approaches the distal third, to prevent proximal migration of the lateral malleolus and subsequent valgus collapse of the ankle mortise.
- Compartment Syndrome: Postoperative bleeding into the tightly bound compartments of the leg can cause compartment syndrome. Leaving the fascial layers open or loosely approximated, combined with adequate closed-suction drainage, mitigates this risk.
CONCLUSION
The posterior approach for harvesting a vascularized fibular graft is a demanding but highly rewarding surgical technique. By mastering the intricate anatomy of the lateral and posterior compartments, respecting the intermuscular planes, and meticulously protecting the peroneal vascular pedicle and adjacent neural structures, the orthopedic microsurgeon can reliably harvest a robust osteocutaneous or osseous graft. Strict adherence to the biomechanical principles of preserving the proximal and distal fibular struts ensures that donor-site morbidity remains minimal, allowing patients to achieve optimal functional outcomes following complex reconstructive procedures.
You Might Also Like