Orthopedic MCQ Exam: Foot, Hip & Knee Practice Questions Part 88
Key Takeaway
This page offers Part 88 of an interactive orthopedic surgery board review quiz, specifically designed for orthopedic residents and surgeons preparing for OITE/AAOS/ABOS certification. It includes 50 high-yield MCQs, formatted like real exams, covering Foot, Hip, and Knee, with detailed explanations for comprehensive exam preparation.
Orthopedic MCQ Exam: Foot, Hip & Knee Practice Questions Part 88
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
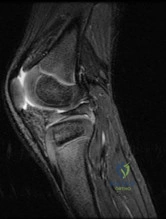
A 55-year-old female presents with acute knee pain after performing a deep squat. MRI demonstrates a complete radial tear of the medial meniscus posterior root.
Biomechanically, this injury pattern most closely mimics which of the following conditions?
Explanation
Question 2
A 65-year-old female undergoes primary total hip arthroplasty (THA) via a posterior approach. Post-operatively, she experiences recurrent anterior dislocations.
Which of the following component malpositions is the most likely cause of her anterior instability?
Explanation
Question 3
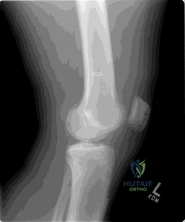
A 60-year-old male with long-standing, poorly controlled diabetes presents with a red, hot, and swollen left foot of 2 weeks duration. He denies any systemic symptoms or open wounds. Radiographs reveal fragmentation, periarticular debris, and subluxation at the tarsometatarsal joint.
What is the most appropriate initial management?

Explanation
Question 4
An 18-year-old female with recurrent patellar dislocations is scheduled for medial patellofemoral ligament (MPFL) reconstruction. Correct placement of the femoral tunnel is critical to ensure anisometry is minimized. Fluoroscopically, the correct femoral attachment (Schöttle point) is best identified by which of the following landmarks on a true lateral radiograph?
Explanation
Question 5
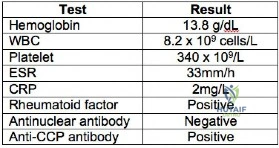
A 55-year-old female presents with medial ankle pain and a progressive flatfoot deformity. She cannot perform a single-leg heel raise. Passive correction of the hindfoot valgus is possible. Radiographs demonstrate a talonavicular uncoverage of 20% without arthritic changes.
Which of the following surgical procedures is most appropriate?
Explanation
Question 6
A 28-year-old male hockey player presents with chronic groin pain that worsens with deep hip flexion and internal rotation. A standing AP pelvis radiograph demonstrates a 'crossover sign'. A frog-leg lateral radiograph shows an alpha angle of 65 degrees.
Which of the following morphologies is predominantly present?
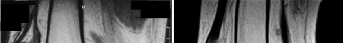
Explanation
Question 7
A 30-year-old male sustains an isolated posterior cruciate ligament (PCL) injury during a motor vehicle collision. On physical examination, the posterior drawer test is utilized to assess posterior tibial translation. At what degree of knee flexion is the PCL subjected to the highest in situ forces, making it the most reliable position for this test?
Explanation
Question 8
A 45-year-old active male presents with chronic dorsal foot pain localized to the first metatarsophalangeal (MTP) joint. Radiographs show dorsal osteophytes with mild to moderate joint space narrowing and preservation of the plantar joint space (Coughlin and Shurnas Grade 2).
Non-operative management has failed. Which surgical intervention is the most appropriate first-line treatment?
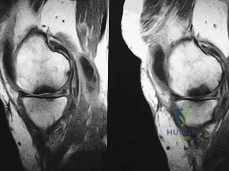
Explanation
Question 9
A 12-year-old obese male presents with left knee pain and a limp for 3 weeks. Examination reveals an antalgic gait. When the hip is passively flexed, it falls into obligatory external rotation.
What is the most appropriate definitive management for the left hip?
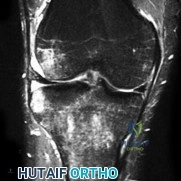
Explanation
Question 10
A 22-year-old female undergoes an anterior cruciate ligament (ACL) reconstruction. Post-operatively, she complains of a persistent lack of full knee extension. Imaging reveals that the graft is impinging against the intercondylar roof. What is the most likely technical error leading to this complication?
Explanation
Question 11
A 25-year-old professional soccer player sustains a fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal.
Given his athletic status, what is the recommended treatment to minimize nonunion risk and expedite return to play?
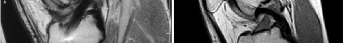
Explanation
Question 12
A 40-year-old female with systemic lupus erythematosus on chronic corticosteroids presents with progressive groin pain. MRI reveals a crescent sign in the anterosuperior aspect of the femoral head.
According to the Ficat and Arlet classification of osteonecrosis, what stage does this radiographic finding represent?
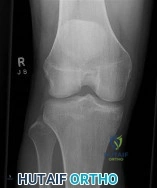
Explanation
Question 13
A 70-year-old male presents with global knee stiffness 6 months after a primary total knee arthroplasty (TKA). His range of motion is 15 to 70 degrees. Radiographs demonstrate appropriate component sizing, but the joint line has been elevated by 8 mm compared to the contralateral knee.
What is the most likely biomechanical consequence of elevating the joint line in TKA?
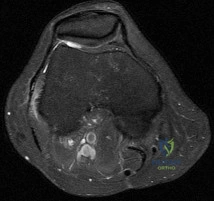
Explanation
Question 14
A 38-year-old recreational athlete sustains an acute Achilles tendon rupture. He opts for non-operative management utilizing an early functional rehabilitation protocol. Compared to traditional open surgical repair, what does high-level literature demonstrate regarding rerupture rates when early functional rehabilitation is strictly followed?
Explanation
Question 15
A 65-year-old female presents with intractable lateral hip pain and weakness in hip abduction. MRI confirms a severe abductor tendon tear. Anatomically, the gluteus minimus tendon primarily inserts onto which specific facet of the greater trochanter?
Explanation
Question 16
A 14-year-old male presents with knee pain and catching. Radiographs reveal a classic osteochondritis dissecans (OCD) lesion.
What is the most common anatomic location for an OCD lesion in the knee?
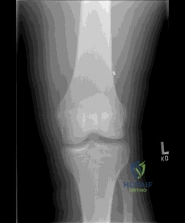
Explanation
Question 17
A 32-year-old male sustains a severe midfoot injury. Imaging shows a complete lateral displacement of the second through fifth metatarsals, while the first metatarsal remains in anatomic alignment with the medial cuneiform.
According to the Hardcastle and Myerson classification of Lisfranc injuries, this pattern is best described as:
Explanation
Question 18
A 78-year-old active female sustains a displaced femoral neck fracture (Garden IV). When counseling her on surgical options, comparing total hip arthroplasty (THA) to hemiarthroplasty, THA is associated with which of the following outcomes?
Explanation
Question 19
A 25-year-old male suffers a varus blow to his anteromedial knee while his foot is planted. Examination demonstrates increased external rotation of the tibia at 30 degrees of knee flexion compared to the uninjured side, but symmetrical tibial rotation at 90 degrees of flexion. Which structure is predominantly injured?
Explanation
Question 20
A 60-year-old male with end-stage post-traumatic ankle osteoarthritis is undergoing a tibiotalar arthrodesis.
What is the optimal position for the ankle fusion to maximize functional outcomes and gait?

Explanation
Question 21
A 65-year-old male is 3 months post-operative from a primary total hip arthroplasty (THA) via a posterior approach. He presents with a history of three posterior dislocations. Radiographs demonstrate a well-fixed acetabular component with 45 degrees of abduction and 20 degrees of anteversion. The femoral stem is stable but appears retroverted by 10 degrees. What is the most appropriate surgical intervention to definitively address this instability?
Explanation
Question 22
A 28-year-old male presents with right knee pain following a dashboard mechanism injury. On examination, the posterior drawer test is negative. The dial test demonstrates 15 degrees of increased external rotation at 30 degrees of knee flexion compared to the uninjured side. At 90 degrees of knee flexion, external rotation is symmetric bilaterally. Which of the following structures is most likely injured?
Explanation
Question 23
A 55-year-old female with poorly controlled type 2 diabetes mellitus presents with a warm, swollen, and erythematous left foot and ankle. She denies any systemic symptoms, fevers, or open wounds. White blood cell count and inflammatory markers are mildly elevated. Radiographs reveal fragmentation, periarticular debris, and subluxation of the tarsometatarsal joints.
Which of the following is the most appropriate initial management?

Explanation
Question 24
A 24-year-old male professional soccer player complains of chronic groin pain exacerbated by kicking. Physical examination reveals a positive impingement test (pain with flexion, adduction, and internal rotation). Radiographs display a "pistol-grip" deformity of the proximal femur and an alpha angle of 68 degrees. What is the primary pathoanatomy responsible for this condition?
Explanation
Question 25
A 70-year-old female is 5 years status post total knee arthroplasty (TKA). She complains of anterior knee pain and a "clunking" sensation when actively extending the knee from a flexed position. Physical examination reveals a palpable and audible clunk at roughly 35 degrees of knee flexion. Radiographs demonstrate a well-fixed posterior stabilized (PS) TKA with no evidence of loosening. What is the most likely diagnosis?
Explanation
Question 26
A 32-year-old male sustains a midfoot injury while playing football. Weight-bearing radiographs demonstrate a 3 mm diastasis between the medial and middle cuneiforms and a "fleck sign" in the first intermetatarsal space. Which ligament complex is primarily disrupted in this injury?
Explanation
Question 27
A 13-year-old obese male presents with insidious onset of left groin and knee pain. He walks with an externally rotated gait. When his left hip is passively flexed, it obligatory goes into external rotation. Radiographs confirm a stable slipped capital femoral epiphysis (SCFE). He undergoes in situ single-screw fixation. Which of the following is the most common long-term complication following successful fixation of this condition?
Explanation
Question 28
A 35-year-old female sustains a high-energy knee dislocation. On examination in the emergency department, the foot is cool with diminished pulses. An ankle-brachial index (ABI) is 0.7. A subsequent CT angiogram confirms a complete popliteal artery occlusion. What is the most appropriate sequence of surgical intervention?
Explanation
Question 29
A 42-year-old weekend athlete sustains an acute Achilles tendon rupture. He is managed nonoperatively with a functional rehabilitation protocol. Based on recent Level I evidence, which of the following statements is true regarding nonoperative functional rehabilitation compared to operative management?
Explanation
Question 30
A 45-year-old male on chronic corticosteroids for systemic lupus erythematosus presents with severe groin pain. Plain radiographs show a crescent sign, and MRI confirms Ficat Stage III avascular necrosis (AVN) of the femoral head involving 45% of the weight-bearing area. What is the most reliable definitive surgical treatment for this patient?

Explanation
Question 31
A 21-year-old male sustains a bucket-handle tear of the medial meniscus. The tear is located in the peripheral red-white zone. The surgeon elects to perform an arthroscopic repair using an inside-out technique for the posterior horn. During the passage of the sutures through the posterior medial joint capsule, which anatomic structure is at greatest risk of iatrogenic injury?
Explanation
Question 32
A 22-year-old collegiate football running back hyper-extends his great toe during a tackle. Examination reveals exquisite tenderness at the plantar aspect of the first metatarsophalangeal (MTP) joint, swelling, and ecchymosis. MRI demonstrates a complete disruption of the plantar plate and capsuloligamentous complex with proximal retraction of the sesamoids. What is the most appropriate management for this athlete?
Explanation
Question 33
A 68-year-old female presents with a grossly loose total hip arthroplasty and severe pelvic osteolysis. Preoperative evaluation suspects a pelvic discontinuity. Which of the following radiographic findings is the most reliable indicator of an ipsilateral pelvic discontinuity?
Explanation
Question 34
A 40-year-old male fell from a ladder 6 weeks ago. He presents now with an inability to actively extend his knee. Radiographs reveal patella alta and no fractures. MRI confirms a complete, chronically retracted patellar tendon rupture. If primary surgical repair is attempted, what adjunctive soft-tissue procedure is most likely required due to the chronicity of the injury?
Explanation
Question 35
A 50-year-old female complains of a painful bunion. Weight-bearing radiographs show a hallux valgus angle (HVA) of 38 degrees and an intermetatarsal angle (IMA) of 16 degrees. Clinical examination reveals no hypermobility of the first tarsometatarsal (TMT) joint and no evidence of degenerative joint disease. What is the most appropriate surgical intervention?
Explanation
Question 36
A 60-year-old male with a metal-on-metal (MoM) total hip arthroplasty presents with new-onset groin pain and a palpable anterior thigh mass. Serum cobalt and chromium levels are elevated. MRI demonstrates a large fluid collection and cystic pseudotumor around the hip.
What type of hypersensitivity reaction is primarily responsible for this adverse local tissue reaction (ALTR)?

Explanation
Question 37
A 25-year-old football player sustains a valgus blow to his right knee. Examination reveals pain along the medial joint line, 5 mm of medial opening at 30 degrees of knee flexion with a firm endpoint, and no opening at 0 degrees of flexion. MRI confirms an isolated tear of the superficial medial collateral ligament (MCL). What is the recommended treatment?
Explanation
Question 38
A 60-year-old female presents with a progressive, painful flatfoot deformity. She is unable to perform a single-leg heel raise on the affected side. Examination reveals a flexible pes planovalgus deformity. Radiographs demonstrate 40% talonavicular uncoverage but no significant degenerative joint disease. After failing 6 months of orthotics and bracing, which surgical procedure is most appropriate?
Explanation
Question 39
In a patient with a typical slipped capital femoral epiphysis (SCFE), what is the true anatomic displacement of the femoral metaphysis (femoral neck) relative to the epiphysis?
Explanation
Question 40
A 14-year-old male presents with vague knee pain and occasional catching. Radiographs reveal a 1.5 cm osteochondritis dissecans (OCD) lesion on the lateral aspect of the medial femoral condyle. MRI confirms the lesion is completely intact with no high T2 fluid signal behind the fragment. His distal femoral physes remain wide open. What is the initial treatment of choice?

Explanation
Question 41
A 68-year-old woman presents with recurrent posterior dislocations of her total hip arthroplasty. Radiographic evaluation demonstrates an acetabular component positioned at 45 degrees of inclination and 0 degrees of anteversion.
Which of the following is the most appropriate surgical intervention to prevent further posterior dislocation?

Explanation
Question 42
In ceramic-on-ceramic total hip arthroplasty, which of the following component malpositions is most strongly associated with the complication of squeaking?
Explanation
Question 43
During a posterior-stabilized (PS) total knee arthroplasty, trial reduction reveals that the knee is well-balanced in full extension but excessively tight in 90 degrees of flexion. Which of the following adjustments is the most appropriate next step?
Explanation
Question 44
A 24-year-old athlete sustains a midfoot injury. Weight-bearing radiographs demonstrate subtle widening between the medial and middle cuneiforms and a 'fleck sign' at the base of the second metatarsal. The torn ligament responsible for this pathognomonic sign connects which two structures?
Explanation
Question 45
A 55-year-old man presents with dorsal foot pain and limited dorsiflexion of his great toe. Radiographs show a dorsal osteophyte at the first metatarsophalangeal (MTP) joint with preservation of the plantar joint space. He has failed conservative management. What is the most appropriate surgical treatment?
Explanation
Question 46
Regarding the native anterior cruciate ligament (ACL), which of the following statements correctly describes the biomechanical function of its two distinct bundles?
Explanation
Question 47
A 32-year-old man sustains a completely displaced Pauwels type III femoral neck fracture in a motor vehicle accident.
Which of the following fixation constructs provides the most biomechanically stable fixation against the dominant vertical shear forces present in this fracture pattern?

Explanation
Question 48
During an ankle fracture-dislocation with suspected syndesmotic injury, it is critical to understand the stabilizing structures. Which of the following ligaments provides the greatest resistance to lateral displacement of the fibula?
Explanation
Question 49
A 60-year-old woman presents with isolated medial compartment knee osteoarthritis. Which of the following clinical or radiographic findings is a classic contraindication to performing a medial unicompartmental knee arthroplasty (UKA)?
Explanation
Question 50
A 28-year-old male hockey player presents with groin pain exacerbated by hip flexion and internal rotation. An AP pelvis radiograph demonstrates a 'crossover sign' and a 'prominent ischial spine sign.' These radiographic findings are most indicative of which of the following pathologies?
Explanation
Question 51
According to the Young-Burgess classification, an anteroposterior compression type II (APC-II) pelvic ring injury is characterized by the disruption of the symphysis pubis and which of the following posterior structures?
Explanation
Question 52
When comparing the open tibial inlay technique to the arthroscopic transtibial tunnel technique for posterior cruciate ligament (PCL) reconstruction, biomechanical and clinical outcome studies have demonstrated which of the following?
Explanation
Question 53
A 56-year-old man with long-standing, poorly controlled diabetes presents with a unilaterally warm, erythematous, and swollen foot for 3 weeks. Radiographs display marked osteopenia and periarticular fragmentation without signs of consolidation.
According to the Eichenholtz classification, what is the most appropriate initial management for this condition?

Explanation
Question 54
A 16-year-old female presents with recurrent lateral patellar dislocations. MRI evaluation of the knee demonstrates a tibial tubercle-trochlear groove (TT-TG) distance of 24 mm. In addition to a medial patellofemoral ligament (MPFL) reconstruction, which of the following procedures is most indicated to correct her underlying pathoanatomy?
Explanation
Question 55
Based on the 2018 International Consensus Meeting (ICM) on Periprosthetic Joint Infection criteria, which of the following synovial fluid profiles strongly supports the diagnosis of a chronic PJI following total hip arthroplasty?
Explanation
Question 56
A 40-year-old construction worker falls from a ladder and sustains an intra-articular calcaneus fracture.
Based on the Sanders classification, a coronal CT image showing two articular fragments (one primary fracture line) through the posterior facet is classified as:

Explanation
Question 57
A 22-year-old male sustains an acute knee dislocation resulting in disruption of the ACL, PCL, and the posterolateral corner (Schenck KD III-L). Which of the following physical exam findings must be carefully evaluated due to its high incidence in this specific injury pattern?
Explanation
Question 58
A 45-year-old female presents with severe end-stage osteoarthritis secondary to developmental dysplasia of the hip (DDH). Radiographs demonstrate complete dislocation of the femoral head with proximal migration greater than 100% of the femoral head height (Crowe IV).
During total hip arthroplasty, the acetabular component is placed at the level of the true acetabulum. Which of the following is the most appropriate technique to safely reduce the hip and minimize the risk of sciatic nerve palsy?

Explanation
Question 59
A 48-year-old male runner complains of chronic posterior heel pain that worsens with activity. MRI confirms insertional Achilles tendinopathy with a large retrocalcaneal exostosis (Haglund's deformity) and calcification within the tendon insertion. During surgical debridement, 60% of the Achilles tendon insertion is detached to remove the diseased tissue and bone. What is the most appropriate next step in surgical management?
Explanation
Question 60
A 70-year-old man with severe osteoarthritis of the right hip walks with a cane. To maximally decrease the joint reaction force across his right hip, in which hand should he hold the cane and what is the primary biomechanical reason?
Explanation
Question 61
A 12-year-old boy presents with left hip pain and an acutely worsening limp. Radiographs confirm a severe, unstable slipped capital femoral epiphysis (SCFE) of the left hip. The right hip is radiographically normal and asymptomatic. Which of the following is the strongest universally accepted indication for prophylactic in situ pinning of the contralateral asymptomatic hip?
Explanation
Question 62
A 24-year-old male sustains an isolated posterior cruciate ligament (PCL) tibial avulsion fracture. Surgical fixation is planned via an open posteromedial approach (Burks and Schaffer). Which internervous or intermuscular interval is utilized in this specific surgical approach?
Explanation
Question 63
A 22-year-old professional football player sustains a severe hyperextension injury to his first metatarsophalangeal (MTP) joint. Clinical examination reveals significant ecchymosis and gross instability. MRI confirms a complete rupture of the plantar plate with proximal migration of the sesamoids. What is the most appropriate management for this injury?
Explanation
Question 64
A 55-year-old female with a metal-on-metal total hip arthroplasty presents with new-onset groin pain and a palpable anterior mass 5 years postoperatively. Radiographs show a well-fixed implant. A MARS MRI reveals a large cystic lesion.
What is the classic histologic finding associated with this specific complication?

Explanation
Question 65
A 45-year-old active female presents with isolated lateral compartment knee osteoarthritis and an anatomic valgus alignment of 12 degrees. A lateral opening-wedge distal femoral osteotomy is planned. Compared to a medial closing-wedge osteotomy, what is a primary biomechanical or surgical advantage of the lateral opening-wedge technique?
Explanation
Question 66
A 35-year-old construction worker falls from a roof, sustaining an intra-articular calcaneal fracture.
The Sanders classification is utilized to grade this injury. This classification system is based on the number and location of fracture lines through which anatomic structure on the coronal CT scan?

Explanation
Question 67
A 28-year-old male hockey player presents with anterior groin pain worsened by hip flexion, adduction, and internal rotation. Radiographs reveal a "pistol grip" deformity of the proximal femur. An alpha angle is measured on the lateral radiograph to quantify the cam lesion. In the context of Femoroacetabular Impingement (FAI), an alpha angle greater than what value is traditionally considered the threshold for abnormal?
Explanation
Question 68
During a medial patellofemoral ligament (MPFL) reconstruction for recurrent patellar instability, accurate placement of the femoral tunnel is critical to ensure proper graft isometry. According to Schottle's point, where should the optimal femoral attachment be positioned on a true lateral radiograph?
Explanation
Question 69
A 22-year-old collegiate basketball player sustains a Zone 2 fracture of the proximal fifth metatarsal (true Jones fracture). He is treated with intramedullary screw fixation. To optimize biomechanical stability and reduce the risk of nonunion, which of the following screw characteristics is highly recommended?
Explanation
Question 70
A 65-year-old male is undergoing a total hip arthroplasty (THA). He has a history of severe heterotopic ossification (Brooker Class IV) following a previous contralateral THA. Which of the following prophylactic regimens is most appropriate and supported by the highest level of evidence?
Explanation
Question 71
A 60-year-old male with isolated medial compartment knee osteoarthritis is evaluated for a unicompartmental knee arthroplasty (UKA).
According to classical indications, which of the following is considered a primary contraindication to performing a medial UKA?

Explanation
Question 72
A 56-year-old male with uncontrolled type II diabetes presents with an acute, warm, swollen right foot. Radiographs reveal fragmentation, osteopenia, and subluxation exclusively involving the talonavicular and calcaneocuboid joints. The tarsometatarsal joints are entirely spared. According to the Brodsky anatomic classification of Charcot neuroarthropathy, what type of injury is this?
Explanation
Question 73
Ceramic-on-ceramic (CoC) bearing surfaces in total hip arthroplasty offer extremely low volumetric wear rates. However, they are associated with unique complications not seen in other bearing couples. Which of the following is a recognized and unique complication of CoC bearings?
Explanation
Question 74
A 52-year-old male undergoes MRI of the knee after a deep squatting injury, which reveals a complete posterior medial meniscal root tear. Biomechanical studies have demonstrated that a complete tear of the medial meniscus posterior root is mechanically equivalent to which of the following conditions regarding tibiofemoral contact pressures?
Explanation
Question 75
The Lisfranc ligament complex is critical for maintaining the stability of the midfoot. Which of the following accurately describes the anatomic attachments of the primary Lisfranc ligament?
Explanation
Question 76
A 32-year-old female in her third trimester of pregnancy presents with the insidious onset of severe left groin pain. She has no history of trauma. Radiographs show focal, severe osteopenia of the left femoral head and neck with a preserved joint space. MRI reveals diffuse bone marrow edema in the femoral head and neck without subchondral collapse.
What is the most likely diagnosis and appropriate initial management?

Explanation
Question 77
The posterior cruciate ligament (PCL) provides primary restraint against posterior tibial translation. It is composed of two main functional bundles. During knee range of motion, how do the tension patterns of these bundles behave?
Explanation
Question 78
A 26-year-old male sustains a pronation-external rotation ankle fracture with syndesmotic disruption. He undergoes open reduction internal fixation, including the placement of two solid 3.5 mm trans-syndesmotic screws. According to current prospective literature, what is the recommendation regarding the routine removal of these syndesmotic screws prior to initiating weight-bearing?
Explanation
Question 79
A 40-year-old male sustained a traumatic posterior hip dislocation 2 years ago. He now presents with worsening groin pain.
Radiographs demonstrate a sclerotic femoral head with a clear subchondral lucent line (crescent sign), but the articular surface has not collapsed. According to the Ficat and Arlet classification for avascular necrosis, what stage is this disease?

Explanation
Question 80
A 42-year-old male undergoes a medial opening-wedge high tibial osteotomy (HTO) for medial compartment osteoarthritis with a varus deformity. During the procedure, the osteotomy gap is opened equally at the anterior and posterior cortex with a rectangular distractor. What is the most likely consequence of this maneuver on the sagittal profile of the proximal tibia?
Explanation
Question 81
A 28-year-old male sustains a knee injury during a soccer match. On physical examination, the dial test reveals 15 degrees of increased external rotation on the injured side compared to the normal side when tested at 30 degrees of knee flexion. When tested at 90 degrees of knee flexion, the external rotation is symmetric between both knees. Which of the following is the most likely diagnosis?
Explanation
Question 82
A 65-year-old male who underwent a primary total hip arthroplasty 5 years ago presents with persistent groin pain. Workup reveals elevated serum cobalt levels and a pseudotumor on MRI, consistent with trunnionosis. Which of the following factors is biomechanically most associated with an increased risk of mechanically assisted crevice corrosion at the head-neck junction?
Explanation
Question 83
A 15-year-old boy with Charcot-Marie-Tooth disease presents with a progressive cavovarus foot deformity. On examination, his hindfoot varus corrects to neutral when standing on a Coleman block, indicating a flexible hindfoot driven by forefoot pathology. Overactivity of which of the following tendons is the primary deforming force driving his plantarflexed first ray?
Explanation
Question 84
A 22-year-old female undergoes a medial patellofemoral ligament (MPFL) reconstruction for recurrent patellar instability. Postoperatively, she complains of a severe loss of knee flexion, and examination reveals a tight graft in deeper degrees of flexion. Which of the following femoral tunnel malpositions is the most likely cause of this complication?
Explanation
Question 85
A 40-year-old male with a history of high-dose corticosteroid use presents with insidious onset groin pain. MRI of the hip reveals a subchondral crescentic lesion with a "double-line sign" on T2-weighted imaging. The inner hyperintense line of this classic sign represents which of the following?
Explanation
Question 86
During a primary total knee arthroplasty using a measured resection technique, the trial components are placed. The surgeon notes that the joint is well-balanced and symmetric in full extension, but the flexion gap is unacceptably tight. Which of the following is the most appropriate intraoperative step to balance the knee?
Explanation
Question 87
A 26-year-old male athlete presents with deep anterior groin pain exacerbated by hip flexion and internal rotation. Radiographs demonstrate a pistol-grip deformity and an alpha angle of 65 degrees. During hip arthroscopy for this condition, where is the most common anatomic location of articular cartilage damage?
Explanation
Question 88
A 38-year-old male undergoes percutaneous repair of an acute Achilles tendon rupture. During the passage of sutures in the proximal stump, the surgeon must be particularly careful to avoid injury to a nerve. Which nerve is most at risk, and what is its typical anatomical relationship to the Achilles tendon in this region?
Explanation
Question 89
A 30-year-old male presents to the trauma bay with a visibly deformed knee after a motorcycle collision. Radiographs confirm a multi-ligamentous knee dislocation (KD-III). After prompt closed reduction, the patient's Ankle-Brachial Index (ABI) is calculated to be 0.85, though distal pulses are palpable. What is the most appropriate next step in management?
Explanation
Question 90
A 78-year-old osteoporotic female falls and sustains a reverse obliquity intertrochanteric femur fracture (AO/OTA 31-A3). Which of the following fixation constructs is biomechanically optimal and associated with the lowest failure rate for this specific fracture pattern?
Explanation
Question 91
A 62-year-old male complains of severe first metatarsophalangeal (MTP) joint pain present throughout the entire arc of motion. Radiographs show complete obliteration of the joint space, extensive dorsal and lateral osteophytes, and subchondral cystic changes. He has failed rigid-soled shoe modifications. What is the gold-standard surgical treatment?
Explanation
Question 92
A 12-year-old gymnast complains of poorly localized knee pain. Radiographs demonstrate a well-circumscribed osteochondral defect with a stable subchondral bone fragment. In juvenile osteochondritis dissecans (JOCD) of the knee, what is the most common anatomical location of the lesion?
Explanation
Question 93
A 12-year-old boy presents with right-sided groin pain and an externally rotated leg. Radiographs confirm a unilateral slipped capital femoral epiphysis (SCFE). Which of the following conditions constitutes the strongest absolute indication for prophylactic in situ pinning of the asymptomatic contralateral hip?
Explanation
Question 94
A 55-year-old female presents with Stage IIb adult acquired flatfoot deformity, demonstrating a flexible hindfoot valgus and greater than 40% talonavicular uncoverage on AP weight-bearing radiographs. In addition to a flexor digitorum longus (FDL) transfer and medial displacement calcaneal osteotomy, which procedure is specifically indicated to address her profound forefoot abduction?
Explanation
Question 95
A 6-year-old girl is evaluated for a painless "snapping" sensation in her lateral knee with extension. MRI confirms a Wrisberg-variant discoid lateral meniscus. By definition, this specific meniscal variant lacks which of the following normal posterior stabilizing attachments?
Explanation
Question 96
A 45-year-old male sustains a severe pelvic ring injury after a crush accident. Radiographs reveal an anteroposterior compression (APC) injury. According to the Young-Burgess classification, which finding differentiates an APC III injury from an APC II injury?
Explanation
Question 97
A 32-year-old female sustains a Hawkins Type II fracture of the talar neck after a fall from a height. The surgeon counsels her on the significant risk of avascular necrosis (AVN). Which artery provides the primary, most abundant blood supply to the talar body that is typically disrupted in displaced talar neck fractures?
Explanation
Question 98
During a primary total knee arthroplasty, a surgeon accidentally sets the tibial component with 15 degrees of excessive internal rotation relative to the tibial tubercle. Which of the following complications is most directly caused by this rotational malalignment?
Explanation
None
