Orthopedic Surgery MCQs: Trauma, Shoulder & Elbow Board Review | Part 83
Key Takeaway
This page offers Part 83 of a comprehensive Orthopedic Surgery Board Review, featuring 50 high-yield MCQs. Designed for orthopedic residents and surgeons, it simulates OITE/AAOS exams with clinical scenarios, detailed explanations, and two interactive learning modes to enhance board certification preparation.
Orthopedic Surgery MCQs: Trauma, Shoulder & Elbow Board Review | Part 83
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 45-year-old bodybuilder feels a sudden 'pop' in his antecubital fossa while lifting weights and presents with weakness in supination. A distal biceps tendon rupture is diagnosed, and surgical repair via a single-incision anterior approach is planned. What is the most common iatrogenic nerve injury associated with this specific surgical approach?
Explanation
Question 2
A 35-year-old woman sustains a terrible triad injury of the elbow. Intraoperatively, the coronoid fracture is secured with a lasso technique, the radial head is replaced, and the lateral ulnar collateral ligament (LUCL) is primarily repaired to its anatomic footprint on the lateral epicondyle. Upon fluoroscopic stress testing, the elbow readily dislocates at 30 degrees of extension.
What is the next most appropriate step in surgical management?

Explanation
Question 3
A 68-year-old osteoporotic female undergoes open reduction and internal fixation of a 3-part proximal humerus fracture using a locked plate construct. Postoperative follow-up at 6 weeks reveals varus collapse of the humeral head and superior screw cut-out into the glenohumeral joint. To minimize the risk of this specific complication, which of the following surgical maneuvers is most critical during the index procedure?
Explanation
Question 4
A 25-year-old male sustains a midshaft clavicle fracture from a bicycle crash. He prefers non-operative management. Which of the following radiographic fracture characteristics is most strongly associated with a higher risk of nonunion if treated non-operatively?
Explanation
Question 5
A 32-year-old competitive powerlifter experiences a sudden tearing sensation in his anterior chest wall while performing a heavy bench press. Examination reveals a palpable defect and loss of the normal anterior axillary fold contour. MRI confirms a complete rupture of the pectoralis major tendon. Which portion of the muscle is most commonly injured in this mechanism, and what is its normal anatomic insertion relative to the other head?
Explanation
Question 6
A 40-year-old male is involved in a high-speed motor vehicle collision and sustains multiple injuries, including an isolated fracture of the scapula. Which of the following isolated fracture patterns is an absolute indication for open reduction and internal fixation?
Explanation
Question 7
A 40-year-old female presents with acute elbow pain after a fall. Radiographs demonstrate a coronal shear fracture of the distal humerus.
Advanced imaging reveals that the fracture includes the capitellum and extends medially to involve the lateral aspect of the trochlea, but leaves the lateral epicondyle intact. According to the Bryan and Morrey classification modified by McKee, what type of fracture is this?
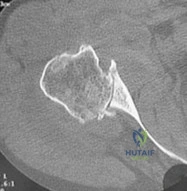
Explanation
Question 8
An 82-year-old low-demand nursing home resident sustains an isolated, displaced, transverse olecranon fracture after a ground-level fall. Due to severe medical comorbidities, non-operative management with early mobilization is chosen. Based on current literature, what is the most likely functional outcome and complication profile for this patient?
Explanation
Question 9
A 35-year-old male sustains a closed, spiral fracture of the distal third of the humeral shaft (Holstein-Lewis fracture) following an arm-wrestling match. On initial examination in the emergency department, he exhibits an inability to extend his wrist and fingers, with loss of sensation over the dorsal first web space. What is the most appropriate initial management?
Explanation
Question 10
A 28-year-old male cyclist falls directly onto his right shoulder. Clinical examination and radiographs confirm a Type III acromioclavicular (AC) joint dislocation. He is counseled on operative versus non-operative treatment. According to the current orthopedic literature, what is the expected outcome if he chooses non-operative management compared to surgical reconstruction?
Explanation
Question 11
A 42-year-old male presents to the emergency department after a seizure. He complains of right shoulder pain and an inability to externally rotate the arm. Radiographs reveal a posterior shoulder dislocation.
A CT scan is obtained after closed reduction and demonstrates an anteromedial impaction fracture of the humeral head (reverse Hill-Sachs lesion) involving 25% of the articular surface. Which of the following is the most appropriate surgical treatment?
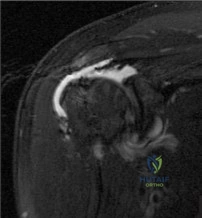
Explanation
Question 12
A 30-year-old female undergoes open reduction and internal fixation for a displaced Mason type II radial head fracture that caused a mechanical block to forearm rotation. To avoid impingement of the hardware on the proximal radioulnar joint during pronation and supination, the plate must be placed within the radial head 'safe zone'. Which of the following accurately describes this anatomic safe zone?
Explanation
Question 13
A 45-year-old polytrauma patient presents with an ipsilateral midshaft clavicle fracture and a displaced scapular neck fracture (floating shoulder). The surgeon considers operative fixation of the scapula rather than the clavicle alone. Which of the following radiographic findings is a primary indication for surgical fixation of the scapular fracture in this scenario?
Explanation
Question 14
A 26-year-old male sustains an elbow dislocation that is reduced in the emergency department.
A subsequent CT scan reveals an isolated fracture of the anteromedial facet of the coronoid process. What specific mechanism of injury and associated ligamentous disruption is most characteristic of this particular fracture pattern?
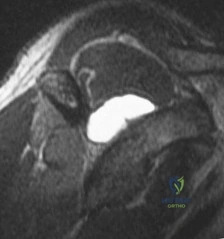
Explanation
Question 15
A 19-year-old collegiate football player sustains a direct blow to the anteromedial aspect of his shoulder. He presents to the trauma bay with severe pain, a feeling of fullness in his neck, dysphagia, and mild stridor. Imaging confirms a posterior sternoclavicular (SC) joint dislocation. A closed reduction in the operating room under general anesthesia is planned. Which surgical specialist must be immediately available on standby during the reduction?
Explanation
Question 16
A 48-year-old male presents with acute weakness in elbow extension after attempting a heavy overhead triceps extension. MRI confirms a complete avulsion of the distal triceps tendon from the olecranon. During surgical repair using a transosseous cruciate technique, understanding the anatomic footprint is crucial. What is the most accurate description of the triceps tendon insertion on the olecranon to guide anatomic repair?
Explanation
Question 17
A 6-year-old boy falls off the monkey bars. Radiographs demonstrate an anterior bowing (plastic deformation) of the ulnar shaft and an anterior dislocation of the radial head. According to the Bado classification, what type of Monteggia lesion is this, and what is the preferred initial management?
Explanation
Question 18
A 45-year-old female who smokes 1 pack of cigarettes a day presents 9 months after sustaining a midshaft humerus fracture that was treated non-operatively in a functional brace. She reports persistent pain and gross motion at the fracture site. Radiographs demonstrate smooth, sclerotic fracture ends with no bridging callus. Which of the following represents the gold standard surgical management for this condition?
Explanation
Question 19
A 65-year-old female sustains an AO/OTA 13-C3 comminuted intra-articular fracture of the distal humerus. The surgeon elects to perform an olecranon osteotomy for optimal articular visualization during open reduction and internal fixation. To maximize stability and minimize the risk of subsequent osteotomy nonunion, what is the preferred geometry and location of the osteotomy?
Explanation
Question 20
A 55-year-old man presents with a complex elbow injury following a fall from a height. Radiographs demonstrate a comminuted fracture of the olecranon. The distal radius and ulna, along with the radial head and coronoid, are displaced anteriorly relative to the distal humerus. However, the proximal radioulnar joint (PRUJ) remains anatomically congruent. What is the key pathomechanical feature of this 'trans-olecranon fracture-dislocation' that distinguishes it from an anterior Monteggia fracture-dislocation?
Explanation
Question 21
A 42-year-old male sustains a closed, isolated scapula fracture in an MVC. Non-operative management is generally indicated for most scapula fractures; however, surgical fixation is recommended when certain criteria are met. Which of the following radiographic parameters is a widely accepted indication for open reduction and internal fixation of the scapula?
Explanation
Question 22
A 42-year-old male presents with a traumatic elbow injury. Radiographs and CT scan reveal a fracture of the anteromedial facet of the coronoid process. On examination, the elbow demonstrates instability when a varus stress is applied. Which of the following ligamentous structures is almost invariably disrupted in this specific injury pattern?
Explanation
Question 23
A 55-year-old female sustains a completely displaced, comminuted midshaft clavicle fracture. She opts for non-operative management. Which of the following radiographic or demographic factors is most strongly predictive of nonunion in this patient?
Explanation
Question 24
Historically, the arcuate artery (a branch of the anterior humeral circumflex artery) was thought to provide the main blood supply to the humeral head. However, recent quantitative cadaveric studies have demonstrated that the principal blood supply to the humeral head is derived from which of the following vessels?
Explanation
Question 25
A surgeon plans to repair a retracted distal biceps tendon rupture using a two-incision (modified Boyd-Anderson) approach. This approach was historically developed to minimize the risk to the posterior interosseous nerve (PIN). However, compared to the single-incision anterior approach, the two-incision technique carries a higher risk of which of the following complications?
Explanation
Question 26
A 35-year-old male with a history of poorly controlled seizures presents with a locked internal rotation deformity of his right shoulder. A CT scan confirms a posterior shoulder dislocation with an impaction fracture of the anterior humeral head (reverse Hill-Sachs lesion) involving 35% of the articular surface. The dislocation is <3 weeks old. What is the most appropriate surgical management?
Explanation
Question 27
A 22-year-old male presents to the emergency department after a high-speed motor vehicle collision. He complains of chest pain, shortness of breath, and pain in the right medial clavicle region. Examination shows a posterior sternoclavicular dislocation. What is the most appropriate next step in management?
Explanation
Question 28
A 40-year-old patient sustains a severely comminuted fracture of the scapular body after falling from a roof. Measurement of the glenopolar angle (GPA) is obtained to evaluate the need for surgical intervention. What is the normal range of the GPA, and at what threshold is surgical fixation generally recommended?
Explanation
Question 29
A 30-year-old male weightlifter felt a sudden "tearing" sensation in his chest while performing a heavy bench press. Examination reveals loss of the anterior axillary fold contour and weakness in internal rotation. Operative repair of the pectoralis major is planned. Which anatomical statement correctly describes the insertion of the most commonly ruptured portion of this muscle?
Explanation
Question 30
A 28-year-old manual laborer requires surgical reconstruction for a chronic Type III acromioclavicular (AC) joint separation. The reconstruction will target the coracoclavicular (CC) ligaments. Which of the following best describes the anatomical orientation of the native CC ligaments?
Explanation
Question 31
A 45-year-old female presents with a highly comminuted radial head fracture, acute wrist pain, and distal radioulnar joint (DRUJ) instability. A diagnosis of an Essex-Lopresti injury is made. If the radial head is simply excised and not replaced, what is the most likely biomechanical consequence?
Explanation
Question 32
A 34-year-old female presents with elbow pain after a fall. Radiographs and CT demonstrate a coronal shear fracture of the capitellum that extends medially to include the majority of the trochlea, with a separate comminuted fracture of the posterior trochlea. According to the Dubberley classification, what is the most appropriate surgical approach for open reduction and internal fixation of this Type 3B injury?
Explanation
Question 33
A 17-year-old male sustains a direct blow to the medial chest wall during a football game. He presents with severe chest pain, shortness of breath, and dysphagia. Examination reveals a palpable depression at the medial end of the clavicle. What is the most appropriate next step in management?

Explanation
Question 34
A 28-year-old sustains a closed, isolated midshaft transverse humerus fracture after a direct blow. On initial examination in the emergency department, he is noted to have a complete absence of wrist extension, finger extension, and decreased sensation over the dorsal first web space. What is the most appropriate initial management for this neurologic finding?
Explanation
Question 35
A 24-year-old cyclist sustains a highly displaced midshaft clavicle fracture. Which of the following is considered an absolute indication for acute open reduction and internal fixation?
Explanation
Question 36
During the surgical reconstruction of a "terrible triad" injury of the elbow, the surgeon follows a standard protocol to restore elbow stability. After addressing the deep articular structures, which of the following represents the most appropriate sequence of repair?
Explanation
Question 37
A 32-year-old male sustains an elbow injury. CT reveals a fracture of the anteromedial facet of the coronoid. Examination shows instability when the elbow is subjected to a varus stress in flexion. Which of the following ligamentous structures is almost universally injured in this specific fracture pattern?
Explanation
None
