Full Question & Answer Text (for Search Engines)
Question 1:
A 15-year-old male presents with right knee pain and a palpable mass. Radiographs reveal a sunburst periosteal reaction in the distal femur. Biopsy confirms the production of malignant osteoid. The patient's family history is significant for a soft-tissue sarcoma in his father and early-onset breast cancer in his aunt. A mutation in which of the following genes is most likely associated with this patient's underlying condition?
Options:
Correct Answer: TP53
Explanation:
The patient's family history is highly suggestive of Li-Fraumeni syndrome, an autosomal dominant disorder caused by a germline mutation in the TP53 tumor suppressor gene. This syndrome classically predisposes individuals to a spectrum of malignancies, notably osteosarcoma, breast cancer, brain tumors, leukemia, and soft-tissue sarcomas. While RB1 mutations (familial retinoblastoma) also predispose to osteosarcoma, the family history of early-onset breast cancer and soft-tissue sarcoma strongly points to a TP53 mutation.
Question 2:
A 12-year-old boy presents with progressive diaphyseal tibial pain, fevers, and an elevated ESR. Radiographs show a permeative lytic lesion with an 'onion-skin' periosteal reaction. Histopathology demonstrates sheets of uniform small round blue cells. Cytogenetic analysis is most likely to reveal which of the following translocations?
Options:
- t(X;18)
- t(11;22)
- t(2;13)
- t(12;16)
- t(9;22)
Correct Answer: t(11;22)
Explanation:
The clinical, radiographic, and histologic presentation is classic for Ewing sarcoma. Over 85% of Ewing sarcomas are characterized by the t(11;22)(q24;q12) translocation, which results in the EWSR1-FLI1 fusion gene. t(X;18) is associated with synovial sarcoma, t(2;13) with alveolar rhabdomyosarcoma, t(12;16) with myxoid liposarcoma, and t(9;22) with CML (Philadelphia chromosome) and some forms of ALL.
Question 3:
A 32-year-old female presents with a painful, eccentrically located, purely lytic lesion in the proximal tibial epiphysis extending into the metaphysis. Biopsy reveals numerous multinucleated giant cells in a background of mononuclear stromal cells. For unresectable cases or to facilitate joint preservation, a targeted biologic agent can be used. What is the mechanism of action of this agent?
Options:
- Inhibition of vascular endothelial growth factor (VEGF)
- Tyrosine kinase inhibition
- Monoclonal antibody against RANK ligand (RANKL)
- Inhibition of colony-stimulating factor 1 receptor (CSF1R)
- Inhibition of the mTOR pathway
Correct Answer: Monoclonal antibody against RANK ligand (RANKL)
Explanation:
The diagnosis is Giant Cell Tumor (GCT) of bone. Denosumab is a fully human monoclonal antibody that binds to and inhibits RANKL, preventing the activation of the RANK receptor on the surface of osteoclast precursors and multinucleated giant cells. This arrests the osteoclast-like giant cell formation, leading to tumor necrosis and woven bone formation, making it highly effective for locally advanced or unresectable GCTs. CSF1R inhibitors (like Pexidartinib) are used for tenosynovial giant cell tumors (PVNS).
Question 4:
A 45-year-old man presents with chronic hip pain. Radiographs reveal a purely lytic lesion in the proximal femoral epiphysis. Biopsy demonstrates sheets of cells with abundant clear cytoplasm, distinct cytoplasmic membranes, and central nuclei scattered among hyaline cartilage. Woven bone formation is also noted. Which of the following is the most likely diagnosis?
Options:
- Chondroblastoma
- Clear cell chondrosarcoma
- Metastatic renal cell carcinoma
- Osteoblastoma
- Giant cell tumor of bone
Correct Answer: Clear cell chondrosarcoma
Explanation:
Clear cell chondrosarcoma is a rare, low-grade malignant cartilage tumor that characteristically involves the epiphysis of long bones (most commonly the proximal femur or humerus) in adults (usually 30-50 years old). The presence of clear cells and variable woven bone production is classic. While chondroblastoma also occurs in the epiphysis and may contain areas resembling clear cells, it typically affects skeletally immature patients and exhibits 'chicken-wire' calcification.
Question 5:
A 10-year-old girl is evaluated for multiple bony prominences around her knees and wrists. Radiographs confirm multiple osteochondromas. Genetic testing reveals a mutation in the EXT1 gene. This mutation directly disrupts the biosynthesis of which of the following macromolecules?
Options:
- Hyaluronic acid
- Heparan sulfate
- Chondroitin sulfate
- Keratan sulfate
- Type II collagen
Correct Answer: Heparan sulfate
Explanation:
Multiple hereditary exostoses (MHE) is an autosomal dominant condition caused by mutations in the EXT1 or EXT2 genes. These genes encode glycosyltransferases essential for the polymerization and biosynthesis of heparan sulfate. The resulting deficiency in heparan sulfate proteoglycans disrupts normal Indian hedgehog (Ihh) signaling at the growth plate, leading to the formation of osteochondromas.
Question 6:
A 9-year-old girl presents with a prominent limp and an apparent leg length discrepancy. Radiographs reveal a ground-glass appearance in the proximal femur with a 'shepherd's crook' deformity. Physical examination shows irregular, large pigmented skin patches with rough borders. What is the underlying molecular pathogenesis of this patient's bone lesions?
Options:
- Loss of function mutation in the NF1 gene
- Activating mutation in the GNAS gene causing persistent cAMP production
- Mutation in the FGFR3 gene resulting in constitutively active tyrosine kinase
- Defect in the CBFA1/RUNX2 transcription factor
- Inactivating mutation in the SQSTM1 gene
Correct Answer: Activating mutation in the GNAS gene causing persistent cAMP production
Explanation:
The clinical picture describes McCune-Albright syndrome, defined by the triad of polyostotic fibrous dysplasia, 'coast of Maine' café-au-lait spots, and endocrinopathies (like precocious puberty). Fibrous dysplasia is caused by a somatic activating mutation in the GNAS gene, which encodes the alpha subunit of the stimulatory G protein (Gs). This leads to constitutively active adenylate cyclase, resulting in elevated intracellular cAMP and subsequent abnormal osteoblast differentiation.
Question 7:
A 28-year-old female presents with a slowly enlarging, painless mass at the posterior aspect of her distal thigh. Radiographs reveal a heavily ossified, broad-based mass attached to the posterior cortex of the distal metaphysis of the femur. A radiolucent cleft is visible between portions of the mass and the underlying cortex. Cytogenetic analysis of the tumor is most likely to show amplification of which of the following genes?
Options:
- c-MYC
- HER2
- MDM2
- EWSR1
- RUNX2
Correct Answer: MDM2
Explanation:
The clinical and radiographic presentation is classic for a parosteal osteosarcoma, a low-grade surface osteosarcoma typically arising from the posterior aspect of the distal femur. The 'string sign' (radiolucent cleft) is characteristic. These tumors consistently show supernumerary ring chromosomes containing amplified sequences of 12q13-15, which include the MDM2 and CDK4 genes. Amplification of MDM2 leads to degradation of the p53 tumor suppressor protein.
Question 8:
A 24-year-old male presents with a dull ache in his left lower leg. Radiographs demonstrate a multi-loculated, expansile, eccentric lytic lesion in the anterior cortex of the tibial diaphysis. Biopsy reveals a biphasic tumor consisting of epithelial cells forming nests and tubular structures embedded in a fibrous stroma. Immunohistochemistry is expected to be strongly positive for which of the following markers?
Options:
- S-100
- Cytokeratin
- Vimentin only
- CD99
- Smooth muscle actin (SMA)
Correct Answer: Cytokeratin
Explanation:
The presentation is classic for adamantinoma, a rare, low-grade malignant primary bone tumor with a striking predilection for the anterior tibial diaphysis. Histologically, it is a biphasic tumor characterized by islands of epithelial cells within a fibrous stroma. The epithelial component characteristically stains positive for cytokeratins (like AE1/AE3) and EMA. CD99 is associated with Ewing sarcoma, and S-100 with neural or cartilaginous tumors.
Question 9:
A 62-year-old man presents with progressive constipation and saddle anesthesia. MRI of the pelvis reveals a large, lobulated, locally destructive mass replacing the sacrum. Histopathological examination shows cords of cells with abundant vacuolated cytoplasm in a myxoid background. Which immunohistochemical marker is highly specific for confirming the origin of this tumor?
Options:
- Chromogranin
- Desmin
- Brachyury
- CD34
- S-100
Correct Answer: Brachyury
Explanation:
The clinical presentation and histology (physaliferous cells with vacuolated cytoplasm) are characteristic of a chordoma, a locally aggressive malignant tumor arising from notochord remnants. While chordomas often stain positive for S-100, cytokeratins, and EMA, nuclear expression of brachyury (a transcription factor vital for notochord development) is highly sensitive and specific for distinguishing chordoma from other clear cell or myxoid tumors (like chondrosarcoma).
Question 10:
A 25-year-old male presents with a slowly growing soft tissue mass deep in the thigh near the knee joint. Radiographs show a soft tissue density with eccentric stippled calcifications. Biopsy demonstrates a biphasic spindle-cell and epithelial proliferation. Which of the following genetic alterations is diagnostic for this mass?
Options:
- t(11;22)(q24;q12)
- t(X;18)(p11;q11)
- t(12;16)(q13;p11)
- t(2;13)(q35;q14)
- t(9;22)(q22;q12)
Correct Answer: t(X;18)(p11;q11)
Explanation:
Synovial sarcoma is characterized by the t(X;18)(p11;q11) translocation, which creates the SYT-SSX (SS18-SSX) fusion gene. It often occurs in young adults near large joints (especially the knee), though rarely involves the joint space itself. Up to 30% display calcifications on plain radiographs. Histologically, it can be biphasic (spindle and epithelial components) or monophasic (spindle cells only).
Question 11:
A 6-year-old boy presents with back pain. Radiographs reveal 'vertebra plana' of T8. A CT-guided biopsy is performed. The lesion contains numerous histiocytes with folded, clefted nuclei (coffee-bean shape) accompanied by eosinophils. Electron microscopy reveals racket-shaped intracytoplasmic organelles. The neoplastic cells are most likely to express which of the following immunophenotypes?
Options:
- CD1a (+), Langerin (+), S100 (+)
- CD68 (+), CD163 (+), CD1a (-)
- Cytokeratin (+), EMA (+), Brachyury (+)
- CD99 (+), FLI-1 (+), NKX2.2 (+)
- CD34 (+), STAT6 (+), S100 (-)
Correct Answer: CD1a (+), Langerin (+), S100 (+)
Explanation:
The clinical presentation (vertebra plana in a child) and histologic findings (coffee-bean nuclei, eosinophils, Birbeck granules on EM) are diagnostic of Langerhans Cell Histiocytosis (LCH). The characteristic immunophenotype for LCH cells is positive for S100, CD1a, and Langerin (CD207). CD68/CD163 positivity without CD1a suggests a non-Langerhans histiocytosis. CD99/FLI-1 is indicative of Ewing sarcoma.
Question 12:
A 22-year-old female presents with multiple painless, hard nodules on her hands. Examination reveals several bluish, soft, compressible nodules on her forearm and hand. Radiographs show multiple central lytic lesions with stippled calcifications within the phalanges. This patient is at a significantly increased risk for developing which of the following malignancies?
Options:
- Osteosarcoma
- Chondrosarcoma
- Angiosarcoma
- Ewing sarcoma
- Multiple myeloma
Correct Answer: Chondrosarcoma
Explanation:
The patient has Maffucci syndrome, characterized by the presence of multiple enchondromas (Ollier disease) combined with soft tissue hemangiomas (the bluish, compressible nodules). Patients with Maffucci syndrome carry a high risk (up to 100% in some series) of malignant transformation of an enchondroma into a secondary chondrosarcoma. They also have an increased risk of visceral malignancies, but chondrosarcoma is the most prominent skeletal risk. These syndromes are associated with somatic mosaic mutations in IDH1 or IDH2.
Question 13:
A 19-year-old male complains of right thigh pain that is worse at night and dramatically improves with ibuprofen. Radiographs demonstrate a 1-cm radiolucent nidus surrounded by dense cortical sclerosis in the femoral diaphysis. Which of the following is true regarding the histopathology and pathophysiology of this lesion?
Options:
- The nidus is avascular and necrotic.
- It is histologically distinct from an osteoblastoma.
- The lesion produces high levels of prostaglandins.
- Malignant transformation to osteosarcoma is common if left untreated.
- The peripheral sclerotic bone contains the highest concentration of nerve fibers.
Correct Answer: The lesion produces high levels of prostaglandins.
Explanation:
Osteoid osteoma is a benign bone-forming tumor characterized by a small (<1.5-2 cm) radiolucent nidus surrounded by reactive sclerosis. The nidus contains an interlacing network of osteoid trabeculae and highly vascularized stroma. It produces high levels of prostaglandins (especially PGE2), which mediate the intense pain and intense localized inflammatory response. NSAIDs block this production, providing dramatic relief. Histologically, it is identical to osteoblastoma (differentiated primarily by size >2cm). The nidus, not the sclerotic rim, contains abundant unmyelinated nerve fibers.
Question 14:
A 14-year-old girl presents with knee pain. MRI reveals an eccentric, expansile metaphyseal lesion in the proximal tibia with multiple fluid-fluid levels. Biopsy reveals blood-filled spaces separated by fibrous septa lacking an endothelial lining. Recent molecular studies indicate that primary forms of this lesion are true neoplasms driven by a specific genetic rearrangement. Which gene is most commonly rearranged in this condition?
Options:
Correct Answer: USP6
Explanation:
The lesion described is an aneurysmal bone cyst (ABC). While historically considered a reactive process, molecular analysis has shown that primary ABCs are true neoplasms characterized by translocations involving the USP6 gene (most commonly t(16;17)(q22;p13) producing a CDH11-USP6 fusion). This leads to USP6 upregulation, driving matrix metalloproteinase production and cystic changes. GNAS is seen in fibrous dysplasia; EXT1 in MHE; MDM2 in parosteal osteosarcoma/atypical lipomatous tumors; IDH1 in enchondromas/chondrosarcomas.
Question 15:
A 68-year-old man presents with dull low back pain and anemia. A technetium-99m bone scan is largely unremarkable, but subsequent radiographs reveal numerous discrete, 'punched-out' lytic lesions in the skull, spine, and pelvis. Which of the following best explains the false-negative finding on the bone scan?
Options:
- The lesions predominantly contain woven bone rather than lamellar bone.
- The tumor directly inhibits osteoblast function, preventing radiotracer uptake.
- The patient has underlying severe osteoporosis precluding tracer binding.
- Technetium-99m primarily binds to areas of hypervascularity, which is absent here.
- The tumor secretes a substance that competitively binds the radiotracer.
Correct Answer: The tumor directly inhibits osteoblast function, preventing radiotracer uptake.
Explanation:
The patient's presentation (anemia, back pain, punched-out lytic lesions, cold bone scan) is classic for Multiple Myeloma. A technetium-99m (Tc-99m) bone scan relies on osteoblastic activity (bone formation) to incorporate the radiotracer. Multiple myeloma cells secrete inhibitors of osteoblast differentiation (such as DKK1 and sFRP2), leading to purely lytic lesions with essentially no reactive new bone formation. Consequently, bone scans are classically falsely negative in myeloma. A skeletal survey or whole-body low-dose CT/MRI is preferred.
Question 16:
A 72-year-old man presents with progressive hearing loss and increasing hat size. His serum alkaline phosphatase is markedly elevated, but calcium and phosphate levels are normal. Biopsy of a bowing tibial lesion reveals a mosaic pattern of lamellar bone with prominent cement lines. Which of the following treatments is the first-line pharmacologic therapy for symptomatic disease in this patient?
Options:
- Teriparatide
- Denosumab
- Zoledronic acid
- Raloxifene
- Calcitonin
Correct Answer: Zoledronic acid
Explanation:
The presentation is classic for Paget's disease of bone (osteitis deformans). The hallmark histological finding is the 'mosaic' or 'jigsaw puzzle' pattern of lamellar bone caused by disorganized osteoclastic and osteoblastic activity. First-line medical therapy for symptomatic Paget's disease consists of nitrogen-containing bisphosphonates, such as intravenous zoledronic acid, which potently inhibit osteoclast-mediated bone resorption.
Question 17:
A 16-year-old boy presents with rapid swelling and pain in his distal femur. MRI reveals an expansile, destructive, predominantly cystic mass with multiple fluid-fluid levels. Based on imaging alone, it closely mimics an aneurysmal bone cyst (ABC). Which of the following histopathological findings differentiates this lesion from a primary ABC?
Options:
- The presence of multinucleated giant cells
- Blood-filled spaces lacking endothelial lining
- Highly pleomorphic cells producing delicate lace-like osteoid within the septa
- A thick rim of reactive lamellar bone surrounding the cyst
- Translocation involving the USP6 gene
Correct Answer: Highly pleomorphic cells producing delicate lace-like osteoid within the septa
Explanation:
The lesion describes a telangiectatic osteosarcoma, a highly malignant variant of osteosarcoma that classically mimics an ABC radiographically and macroscopically (both have large blood-filled spaces and fluid-fluid levels). The critical differentiating feature on histopathology is the presence of highly atypical, pleomorphic sarcomatous cells producing malignant osteoid within the septae separating the cystic spaces. Primary ABCs lack this cytological atypia and malignant osteoid.
Question 18:
A 15-year-old male presents with chronic knee pain. Radiographs reveal a sharply demarcated, 2-cm lytic lesion in the distal femoral epiphysis with a thin sclerotic rim. Histological examination shows mononuclear cells with grooved (coffee-bean) nuclei and scattered multinucleated giant cells. A fine, 'chicken-wire' pattern of pericellular calcification is present. What is the standard treatment for this lesion?
Options:
- Wide en bloc resection
- Neoadjuvant chemotherapy followed by limb salvage surgery
- Extended curettage and bone grafting
- Radiation therapy alone
- Indomethacin therapy and observation
Correct Answer: Extended curettage and bone grafting
Explanation:
The clinical and histological findings (epiphyseal location in a skeletally immature patient, grooved nuclei, chicken-wire calcification) are diagnostic of a chondroblastoma. It is a benign but locally aggressive cartilage tumor. Standard treatment is extended (aggressive) intralesional curettage (often with high-speed burr and chemical adjuvants like phenol or cryotherapy) followed by bone grafting or PMMA cementing to prevent local recurrence while preserving joint function.
Question 19:
A 35-year-old female presents with chronic, painless swelling of the right knee. Aspiration yields dark brown, non-clotting fluid. MRI demonstrates a large, nodular intra-articular soft tissue mass with marked 'blooming artifact' on gradient-echo sequences. This condition is driven by a translocation that results in the overexpression of which of the following?
Options:
- Vascular Endothelial Growth Factor (VEGF)
- Colony Stimulating Factor 1 (CSF1)
- Fibroblast Growth Factor Receptor (FGFR)
- Epidermal Growth Factor Receptor (EGFR)
- Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL)
Correct Answer: Colony Stimulating Factor 1 (CSF1)
Explanation:
The clinical picture and MRI findings (blooming artifact representing hemosiderin deposition) are characteristic of Pigmented Villonodular Synovitis (PVNS), now more accurately termed diffuse tenosynovial giant cell tumor (TGCT). The pathogenesis involves a specific translocation t(1;2) resulting in the fusion of the COL6A3 promoter to the CSF1 gene. This leads to the overexpression and secretion of CSF1 by a small minority of neoplastic cells, which then recruits a massive non-neoplastic inflammatory infiltrate of macrophages expressing the CSF1 receptor. Systemic therapy with CSF1R inhibitors (e.g., pexidartinib) targets this mechanism.
Question 20:
A 5-year-old boy presents with anterior bowing of the tibia. Radiographs show a multi-loculated, entirely intracortical lytic lesion along the anterior tibial diaphysis. Biopsy reveals a fibro-osseous lesion with trabeculae of woven bone rimmed by active osteoblasts. Immunohistochemical stains reveal scattered individual cytokeratin-positive cells. What is the most appropriate management for this lesion if it is asymptomatic?
Options:
- Immediate wide local excision to prevent malignant transformation
- Amputation due to aggressive local invasion
- Observation with serial radiographs
- Neoadjuvant chemotherapy followed by resection
- Curettage and autologous bone grafting immediately
Correct Answer: Observation with serial radiographs
Explanation:
The diagnosis is osteofibrous dysplasia (OFD) of the tibia (Campanacci disease). It occurs almost exclusively in the anterior cortex of the tibia in children <10 years old. Histologically, it features woven bone rimmed by active osteoblasts (unlike fibrous dysplasia, which lacks osteoblastic rimming). A key feature is the presence of scattered cytokeratin-positive cells. OFD shares clinical and histological overlap with adamantinoma but behaves benignly. Asymptomatic lesions are observed, as they often stabilize or spontaneously regress after skeletal maturity. Surgery is reserved for severe deformity or risk of fracture, and is generally delayed until after skeletal maturity due to a high recurrence rate if excised early.
Question 21:
A 32-year-old male presents with chronic, dull anterior shin pain. Radiographs demonstrate an eccentric, multi-loculated, "soap-bubble" osteolytic lesion in the anterior tibial diaphysis. Biopsy reveals a biphasic tumor characterized by nests of basaloid cells surrounded by a bland fibrous stroma. Immunohistochemistry is strongly positive for cytokeratin and epithelial membrane antigen (EMA). Which of the following is the most likely diagnosis?
Options:
- Osteofibrous dysplasia
- Adamantinoma
- Ewing sarcoma
- Chondromyxoid fibroma
- Synovial sarcoma
Correct Answer: Adamantinoma
Explanation:
The clinical presentation and histology are classic for adamantinoma. Adamantinoma is a rare, low-grade malignant bone tumor that almost exclusively occurs in the anterior diaphyseal cortex of the tibia. Histologically, it is a biphasic tumor consisting of epithelial cells (which stain positively for cytokeratin and EMA) interspersed in an osteofibrous stroma. Osteofibrous dysplasia (OFD) occurs in a similar location but typically in the first decade of life and lacks the prominent epithelial nests seen in adamantinoma (though OFD can have scattered cytokeratin-positive cells, it is not grossly biphasic). Standard treatment for adamantinoma is wide en bloc resection, as it is relatively radioresistant and chemoresistant.
Question 22:
A 45-year-old male presents with persistent right hip pain. Radiographs demonstrate a well-defined, expansile, lytic lesion in the proximal femoral epiphysis. Biopsy shows large cells with abundant clear cytoplasm, distinct cytoplasmic membranes, and centrally located nuclei, admixed with areas of conventional hyaline cartilage. Which of the following is the most accurate statement regarding this condition?
Options:
- It typically presents as a diaphyseal lesion in young children.
- It has a distinct predilection for the epiphysis of long bones.
- It is best managed with primary external beam radiation therapy.
- A characteristic t(X;18) chromosomal translocation is pathognomonic.
- It represents the malignant transformation of a pre-existing chondroblastoma.
Correct Answer: It has a distinct predilection for the epiphysis of long bones.
Explanation:
The diagnosis is clear cell chondrosarcoma. This is a rare, low-grade variant of chondrosarcoma that is unique among malignant bone tumors because it has a strong predilection for the epiphyses of long bones (most commonly the proximal femur and proximal humerus) in adults (typically 30-50 years old). This distinguishes it from conventional chondrosarcoma (which is usually metaphyseal/diaphyseal) and chondroblastoma (which is epiphyseal but typically occurs in skeletally immature patients). Wide surgical resection is the treatment of choice. t(X;18) is seen in synovial sarcoma. It is distinct from chondroblastoma and does not arise from it.
Question 23:
A 48-year-old female with a known history of polyostotic fibrous dysplasia presents with a painless, slow-growing soft tissue mass in her right thigh. MRI reveals a well-circumscribed intramuscular mass exhibiting high T2 signal and heterogeneous contrast enhancement. A biopsy confirms an intramuscular myxoma. What is the underlying genetic mutation associated with this specific syndrome?
Options:
- Loss-of-function mutation in the PTEN gene
- Missense mutation in the GNAS gene
- Inactivating mutation in EXT1
- Deletion of the NF1 gene
- Loss of heterozygosity in RB1
Correct Answer: Missense mutation in the GNAS gene
Explanation:
The patient's presentation of polyostotic fibrous dysplasia combined with intramuscular myxomas is diagnostic of Mazabraud syndrome. Like isolated fibrous dysplasia and McCune-Albright syndrome, Mazabraud syndrome is caused by an activating post-zygotic missense mutation in the GNAS gene (specifically at the Arg201 codon). This mutation leads to constitutive activation of the Gs-alpha protein and downstream overproduction of cAMP, which disrupts normal osteoblast differentiation and promotes the formation of fibro-osseous lesions and myxomas.
Question 24:
A 14-year-old girl presents with multiple asymmetric cartilaginous bone lesions leading to limb length discrepancy, along with several bluish soft-tissue nodules on her hands and feet. A biopsy of a soft-tissue nodule reveals a spindle cell hemangioma. Which of the following statements is true regarding her condition compared to a patient with multiple enchondromas alone (Ollier disease)?
Options:
- She has a significantly higher risk of developing non-mesenchymal malignancies, such as astrocytoma or ovarian carcinoma.
- Her condition is inherited in an autosomal dominant pattern with high penetrance.
- She has a lower lifetime risk of malignant transformation to chondrosarcoma.
- Her condition is characterized by a pathognomonic t(11;22) chromosomal translocation.
- She is more likely to experience spontaneous resolution of her bone lesions after skeletal maturity.
Correct Answer: She has a significantly higher risk of developing non-mesenchymal malignancies, such as astrocytoma or ovarian carcinoma.
Explanation:
The patient has Maffucci syndrome, characterized by multiple enchondromas and soft tissue hemangiomas (often spindle cell hemangiomas). While both Ollier disease (enchondromatosis alone) and Maffucci syndrome carry a high risk of malignant transformation to chondrosarcoma (estimated up to 25-30% for Ollier and closer to 100% lifetime risk for Maffucci), Maffucci syndrome is uniquely associated with a high risk of developing secondary non-mesenchymal malignancies, such as astrocytomas, gastrointestinal carcinomas, and ovarian tumors. Both disorders are caused by somatic mosaic mutations in IDH1 or IDH2, not inherited autosomal dominant mutations.
Question 25:
A 30-year-old female presents with a massive, unresectable giant cell tumor of bone (GCTB) located in her sacrum. Her oncologist initiates treatment with denosumab. Which of the following best describes the cellular mechanism of action of this targeted therapy?
Options:
- It binds to the RANK receptor expressed on the surface of neoplastic multinucleated giant cells, inducing apoptosis.
- It binds to RANKL expressed by the neoplastic mononuclear stromal cells, preventing the activation of osteoclast-like giant cells.
- It directly inhibits vascular endothelial growth factor (VEGF), depriving the highly vascular tumor of its blood supply.
- It internalizes into osteoclasts and disrupts the mevalonate pathway by inhibiting farnesyl pyrophosphate synthase.
- It acts as a recombinant osteoprotegerin (OPG) analog, binding directly to the Wnt receptor.
Correct Answer: It binds to RANKL expressed by the neoplastic mononuclear stromal cells, preventing the activation of osteoclast-like giant cells.
Explanation:
Giant cell tumor of bone (GCTB) is characterized by neoplastic mononuclear stromal cells and reactive, non-neoplastic multinucleated giant cells (which resemble osteoclasts). The neoplastic mononuclear cells overexpress RANK Ligand (RANKL). This RANKL binds to the RANK receptor on the reactive giant cells, leading to their activation and subsequent massive bone osteolysis. Denosumab is a fully human monoclonal antibody that specifically binds to and neutralizes RANKL (expressed by the mononuclear cells), thereby preventing the recruitment and activation of the bone-destroying giant cells. Choice D describes the mechanism of nitrogen-containing bisphosphonates.
Question 26:
A 12-year-old boy presents with an expansile, lytic, multi-cystic lesion in the distal femoral metaphysis. MRI demonstrates multiple fluid-fluid levels within the lesion. A core needle biopsy confirms a primary aneurysmal bone cyst (ABC). Which of the following molecular alterations is most characteristic and diagnostic of a primary aneurysmal bone cyst?
Options:
- USP6 gene rearrangement [t(16;17)]
- GNAS missense mutation
- MDM2 and CDK4 amplification
- t(X;18) chromosomal translocation
- BRAF V600E somatic mutation
Correct Answer: USP6 gene rearrangement [t(16;17)]
Explanation:
Primary Aneurysmal Bone Cysts (ABCs) are now recognized as genuine neoplasms rather than purely reactive lesions. They are driven by a characteristic recurrent chromosomal translocation, t(16;17)(q22;p13), which results in the upregulation of the USP6 gene (ubiquitin-specific protease 6). This helps distinguish primary ABCs from secondary ABCs, which can arise in the setting of other tumors (e.g., giant cell tumor, osteoblastoma, chondroblastoma) and lack the USP6 rearrangement. GNAS is seen in fibrous dysplasia; MDM2 in atypical lipomatous tumors and parosteal osteosarcoma; t(X;18) in synovial sarcoma; and BRAF V600E in Langerhans Cell Histiocytosis.
Question 27:
A 25-year-old male undergoes curettage of a locally aggressive lytic lesion in the mandible. Histological examination reveals an abundant collagenous stroma containing uniform, spindled fibroblasts with no cytologic atypia, pleomorphism, or necrosis. Immunohistochemistry demonstrates abnormal nuclear accumulation of beta-catenin. What is the most likely diagnosis?
Options:
- Desmoplastic fibroma
- Fibrous dysplasia
- Non-ossifying fibroma
- Low-grade central osteosarcoma
- Chondromyxoid fibroma
Correct Answer: Desmoplastic fibroma
Explanation:
Desmoplastic fibroma is a rare, locally aggressive, benign primary bone tumor that is considered the intraosseous equivalent of extra-abdominal soft-tissue desmoid tumors (desmoid-type fibromatosis). Like soft tissue desmoid tumors, desmoplastic fibromas of bone frequently harbor mutations in the CTNNB1 gene or APC gene, leading to the abnormal nuclear accumulation of beta-catenin. Histologically, it features bland fibroblasts separated by abundant collagen without atypia or matrix calcification. Treatment involves wide local excision due to the high risk of local recurrence with curettage alone.
Question 28:
A 50-year-old male presents with generalized progressive muscle weakness, diffuse bone pain, and multiple pseudo-fractures visible on radiographs. Laboratory studies reveal severe hypophosphatemia, decreased 1,25-dihydroxyvitamin D, and normal serum calcium levels. A total body DOTATATE PET/CT reveals a small, highly avid soft tissue mass in the plantar aspect of the left foot. Surgical resection of this mass will most likely demonstrate a neoplasm secreting which of the following?
Options:
- Parathyroid hormone (PTH)
- Parathyroid hormone-related peptide (PTHrP)
- Fibroblast Growth Factor 23 (FGF23)
- 1,25-dihydroxyvitamin D
- Calcitonin
Correct Answer: Fibroblast Growth Factor 23 (FGF23)
Explanation:
The patient's presentation is pathognomonic for Tumor-Induced Osteomalacia (TIO), also known as oncogenic osteomalacia. TIO is a paraneoplastic syndrome typically caused by a small, benign, indolent mesenchymal tumor (Phosphaturic Mesenchymal Tumor, or PMT) that secretes Fibroblast Growth Factor 23 (FGF23). FGF23 acts on the kidneys to inhibit phosphate reabsorption (causing phosphaturia and hypophosphatemia) and inhibits 1-alpha-hydroxylase (reducing active vitamin D synthesis). Complete surgical resection of the offending tumor typically results in a rapid and complete reversal of the biochemical and clinical abnormalities.
Question 29:
A 35-year-old female presents with a 2-year history of chronic lower back pain and new-onset saddle anesthesia. Imaging reveals a well-circumscribed, lytic mass within the sacrum causing cortical expansion. Biopsy shows cuboidal to columnar cells arranged radially around myxoid vascular cores. Which of the following is the most likely diagnosis?
Options:
- Chordoma
- Chondrosarcoma
- Giant cell tumor of bone
- Myxopapillary ependymoma
- Schwannoma
Correct Answer: Myxopapillary ependymoma
Explanation:
The description of "cells arranged radially around myxoid vascular cores" characterizes perivascular pseudorosettes, which are the histologic hallmark of a myxopapillary ependymoma. This is a crucial differential diagnosis for sacral and sacrococcygeal masses. While chordoma is the most common primary malignant tumor of the sacrum, its classic histology features cords of vacuolated "physaliferous" cells in a myxoid stroma, not perivascular pseudorosettes. Myxopapillary ependymomas arise from the filum terminale and can present as primary sacral bone lesions through direct extension or primary intraosseous development.
Question 30:
A 62-year-old male presents with a pathologic fracture of the proximal femur. Radiographs show an aggressive lytic lesion with cortical destruction superimposed on a background of intralesional stippled and "popcorn" calcifications. Biopsy demonstrates a sharp, distinct histologic transition between a low-grade hyaline cartilage tumor and a high-grade, non-chondrogenic pleomorphic spindle cell sarcoma. Which of the following best characterizes the clinical behavior of this specific lesion?
Options:
- Excellent long-term survival with neoadjuvant multi-agent chemotherapy alone.
- Dismal prognosis, with a very high likelihood of early hematogenous metastasis to the lungs.
- Typically arises only in patients with Multiple Hereditary Exostoses (MHE).
- Best managed definitively with intralesional curettage and cementation.
- Lymph node metastasis is its primary and most common route of systemic spread.
Correct Answer: Dismal prognosis, with a very high likelihood of early hematogenous metastasis to the lungs.
Explanation:
The clinical and histologic description represents a dedifferentiated chondrosarcoma. This tumor is defined by the coexistence of a well-differentiated, low-grade cartilage tumor abruptly adjacent to a high-grade, non-cartilaginous sarcoma (e.g., osteosarcoma, undifferentiated pleomorphic sarcoma). Dedifferentiated chondrosarcoma is highly aggressive and carries a dismal prognosis, with a 5-year survival rate often reported below 15-20%, primarily due to early and rapid hematogenous dissemination to the lungs. Chemotherapy is generally ineffective for the low-grade chondroid component, though it is sometimes attempted for the high-grade component. Wide surgical resection is required.
Question 31:
A 55-year-old male undergoes en bloc resection of a clival tumor. Histopathology reveals lobulated architecture containing characteristic physaliferous cells with abundant, bubbly, vacuolated cytoplasm embedded in a myxoid stroma. Which of the following immunohistochemical markers is most highly specific for confirming this diagnosis and distinguishing it from a chondrosarcoma?
Options:
- S100 protein
- Cytokeratin
- Brachyury
- CD99
- Epithelial Membrane Antigen (EMA)
Correct Answer: Brachyury
Explanation:
The lesion described is a chordoma, characterized histologically by physaliferous (bubbly) cells. Differentiating chordoma from chondrosarcoma can sometimes be challenging, particularly in the skull base and spine. Both can be positive for S100. However, Brachyury (a transcription factor crucial for notochord development) is highly sensitive and specific for chordoma and is negative in chondrosarcomas. Chordomas are also typically positive for epithelial markers (Cytokeratin and EMA), whereas conventional chondrosarcomas are negative, but Brachyury is considered the definitive confirmatory marker.
Question 32:
A 28-year-old female presents with a painless, hard, fixed mass on the posterior aspect of her distal thigh. Radiographs demonstrate a dense, heavily ossified, lobulated mass originating from the posterior cortex of the distal femur. A distinct radiolucent cleft (the "string sign") separates a portion of the tumor from the underlying diaphyseal cortex. What is the most characteristic genetic aberration associated with this primary bone tumor?
Options:
- MDM2 and CDK4 amplification
- EWSR1-FLI1 fusion
- H3F3A mutation
- EXT1 or EXT2 loss of function
- TP53 mutation alone
Correct Answer: MDM2 and CDK4 amplification
Explanation:
The clinical presentation, location (posterior distal femur), and radiographic "string sign" are classic for parosteal osteosarcoma, a low-grade surface osteosarcoma. Molecularly, parosteal osteosarcomas (like low-grade central osteosarcomas and atypical lipomatous tumors) are characterized by supernumerary ring chromosomes containing amplifications of the 12q13-15 region, which prominently houses the MDM2 and CDK4 genes. MDM2 is an antagonist of the p53 tumor suppressor. Identifying MDM2 amplification via FISH is highly useful in distinguishing parosteal osteosarcoma from reactive lesions like myositis ossificans.
Question 33:
A 14-year-old boy presents with a destructive diaphyseal lesion in his left fibula associated with a prominent "onion-skin" periosteal reaction. A core biopsy reveals sheets of small, uniform, round blue cells with scant cytoplasm that are diffusely positive for CD99 (MIC2). While the EWSR1-FLI1 fusion via t(11;22) is the most common translocation driving this disease, which of the following represents the second most common fusion gene variant found in this tumor?
Options:
- EWSR1-ERG t(21;22)
- SYT-SSX t(X;18)
- ETV6-NTRK3 t(12;15)
- PAX3-FOXO1 t(2;13)
- FUS-DDIT3 t(12;16)
Correct Answer: EWSR1-ERG t(21;22)
Explanation:
The patient has Ewing sarcoma. Approximately 85-90% of Ewing sarcomas harbor the classic t(11;22)(q24;q12) translocation, resulting in the EWSR1-FLI1 fusion protein. The second most common variant, present in about 5-10% of cases, is t(21;22)(q22;q12), which results in the EWSR1-ERG fusion. SYT-SSX is found in synovial sarcoma; ETV6-NTRK3 in infantile fibrosarcoma (and congenital mesoblastic nephroma); PAX3-FOXO1 in alveolar rhabdomyosarcoma; and FUS-DDIT3 in myxoid liposarcoma.
Question 34:
A 32-year-old male presents with a slowly enlarging, deep soft tissue mass near the knee joint. He reports intermittent pain for the past 18 months. Radiographs reveal a soft tissue mass with eccentric stippled calcifications. Biopsy demonstrates a biphasic pattern consisting of sheets of uniform spindle cells intertwined with epithelial-like glandular structures. Which cytogenetic abnormality is diagnostic for this tumor?
Options:
- t(9;22)(q22;q12)
- t(X;18)(p11;q11)
- t(2;13)(q35;q14)
- t(11;22)(q24;q12)
- t(12;16)(q13;p11)
Correct Answer: t(X;18)(p11;q11)
Explanation:
The clinical history, radiographic evidence of calcification (seen in ~30% of cases), and biphasic histology are classic for synovial sarcoma. Synovial sarcoma is uniquely characterized by the balanced reciprocal translocation t(X;18)(p11;q11), leading to the fusion of the SS18 (formerly SYT) gene on chromosome 18 with one of the SSX genes (SSX1, SSX2, or SSX4) on the X chromosome. Despite its name, synovial sarcoma rarely arises directly from the synovium of a joint, but rather from adjacent deep soft tissues.
Question 35:
A 40-year-old male with a history of multiple café-au-lait macules and axillary freckling presents with a rapidly enlarging, painful mass in his proximal thigh. He has a known history of a long-standing plexiform neurofibroma at this exact site. Core needle biopsy reveals a high-grade spindle cell sarcoma. Loss of function of which of the following proteins is directly implicated in the pathogenesis of this patient's underlying genetic syndrome and subsequent malignant transformation?
Options:
- Merlin, leading to hyperactivation of mTOR
- Neurofibromin, leading to hyperactivation of the RAS pathway
- APC, leading to beta-catenin accumulation
- p53, leading to failure of apoptosis
- RB1, leading to uncontrolled cell cycle progression
Correct Answer: Neurofibromin, leading to hyperactivation of the RAS pathway
Explanation:
The patient's clinical signs (café-au-lait macules, axillary freckling, plexiform neurofibroma) indicate Neurofibromatosis type 1 (NF1). Patients with NF1 have up to a 10% lifetime risk of a plexiform neurofibroma undergoing malignant transformation into a Malignant Peripheral Nerve Sheath Tumor (MPNST), as described here. NF1 is caused by a mutation in the NF1 gene, which encodes the protein neurofibromin. Neurofibromin is a GTPase-activating protein (GAP) that negatively regulates the RAS signaling pathway. Loss of neurofibromin leads to unopposed, hyperactive RAS signaling, promoting tumorigenesis.
Question 36:
A 45-year-old male presents with bone pain and is found to have multifocal lytic bone lesions in the lower extremity. A biopsy shows cords and nests of epithelioid cells set in a myxohyaline stroma. Many cells contain intracytoplasmic vacuoles that resemble primitive vascular lumens, some containing erythrocytes. The tumor cells are strongly positive for CD31 and ERG. Molecular testing reveals a WWTR1-CAMTA1 gene fusion. Which of the following is the most likely diagnosis?
Options:
- Angiosarcoma
- Epithelioid sarcoma
- Epithelioid hemangioendothelioma
- Metastatic renal cell carcinoma
- Adamantinoma
Correct Answer: Epithelioid hemangioendothelioma
Explanation:
The clinical, histologic, and molecular findings are diagnostic of Epithelioid Hemangioendothelioma (EHE) of bone. EHE is a rare vascular tumor of intermediate to malignant potential. It frequently presents with multifocal bone involvement. Histologically, it features epithelioid cells with distinctive intracytoplasmic lumina ("blister cells") in a myxohyaline stroma. It expresses endothelial markers like CD31, CD34, and ERG. The hallmark molecular alteration is the t(1;3)(p36;q25) translocation, resulting in the WWTR1-CAMTA1 fusion gene, which is highly specific for EHE and differentiates it from angiosarcoma or epithelioid sarcoma.
Question 37:
A 22-year-old male complains of chronic, mild left knee pain. Imaging reveals an eccentric, well-defined, lytic lesion in the proximal tibial metaphysis with a scalloped, sclerotic margin. Histological examination of curettage material displays a lobular architecture featuring a hypocellular myxochondroid center containing stellate cells and a hypercellular periphery containing spindle cells and occasional multinucleated giant cells. What is the most appropriate initial treatment for this lesion?
Options:
- Observation and serial radiographs
- Intralesional curettage with high-speed burring and bone grafting
- Wide en bloc resection with massive allograft reconstruction
- Primary radiation therapy
- Neoadjuvant chemotherapy followed by wide resection
Correct Answer: Intralesional curettage with high-speed burring and bone grafting
Explanation:
The clinical presentation and classic "zonal" histology (hypocellular center with stellate cells and hypercellular periphery) describe a Chondromyxoid Fibroma (CMF), a rare benign cartilaginous bone tumor. Because it is a benign but locally aggressive lesion (Campanacci stage 2 or 3), observation is inadequate. The standard of care is intralesional extended curettage (utilizing a high-speed burr or adjuvants like phenol/argon beam) followed by bone grafting or cementation. Wide en bloc resection is rarely indicated unless the lesion is massive, recurrent, or involves an expendable bone (e.g., proximal fibula).
Question 38:
A 7-year-old boy presents with a painful lytic lesion in the skull and a separate localized lytic lesion in the clavicle. A biopsy of the clavicular lesion reveals sheets of mononuclear cells with characteristic grooved "coffee bean" nuclei intermingled with numerous eosinophils. Immunohistochemistry shows the cells are positive for CD1a and Langerin (CD207). Which of the following specific genetic mutations is most frequently identified in the pathogenesis of this disease?
Options:
- EXT1 nonsense mutation
- KRAS activating mutation
- BRAF V600E point mutation
- GNAS missense mutation
- IDH1 point mutation
Correct Answer: BRAF V600E point mutation
Explanation:
The patient has Langerhans Cell Histiocytosis (LCH), supported by the typical lytic bone lesions, histology (eosinophils and cells with folded/grooved nuclei), and diagnostic immunomarkers (CD1a and Langerin). It is now established that LCH is a clonal neoplastic disorder of myeloid-derived dendritic cells. Approximately 50-60% of LCH cases harbor the BRAF V600E activating mutation, leading to constitutive activation of the MAPK/ERK signaling pathway. This has important therapeutic implications, as BRAF inhibitors (e.g., vemurafenib) can be used in severe, multi-system, or refractory cases.
Question 39:
A 65-year-old male is newly diagnosed with multiple myeloma presenting with diffuse osteolytic bone lesions. The pathogenesis of these purely lytic lesions is related to a profound uncoupling of bone remodeling, featuring both osteoclast activation and severe osteoblast inhibition. Overexpression of which of the following molecules by the neoplastic plasma cells is primarily responsible for the direct inhibition of osteoblastic bone formation?
Options:
- Sclerostin
- Osteoprotegerin (OPG)
- Receptor activator of nuclear factor kappa-B ligand (RANKL)
- Dickkopf-1 (DKK1)
- Fibroblast Growth Factor 2 (FGF2)
Correct Answer: Dickkopf-1 (DKK1)
Explanation:
Multiple myeloma bone disease is uniquely characterized by purely lytic lesions with essentially no osteoblastic response (hence why bone scans are often negative). The neoplastic plasma cells induce this by upregulating RANKL and downregulating OPG to massively stimulate osteoclasts. Concurrently, they secrete Dickkopf-1 (DKK1) and soluble Frizzled-related protein 2 (sFRP-2). DKK1 is a potent soluble inhibitor of the Wnt/beta-catenin signaling pathway. Inhibition of the Wnt pathway directly blocks the differentiation of mesenchymal stem cells into osteoblasts, thereby preventing bone formation.
Question 40:
A 38-year-old female presents with recurrent, massive knee swelling, stiffness, and pain. MRI demonstrates a large joint effusion and extensive nodular synovial proliferation that shows distinctly low signal intensity on both T1- and T2-weighted images due to hemosiderin deposition. Recent advances in systemic targeted therapy for advanced, unresectable forms of this specific disease are designed to inhibit which of the following pathways?
Options:
- Vascular Endothelial Growth Factor Receptor (VEGFR)
- Epidermal Growth Factor Receptor (EGFR)
- Colony-stimulating factor 1 receptor (CSF1R)
- Platelet-derived growth factor receptor (PDGFR)
- Human epidermal growth factor receptor 2 (HER2)
Correct Answer: Colony-stimulating factor 1 receptor (CSF1R)
Explanation:
The clinical presentation and MRI findings (hemosiderin causing blooming/low signal on T1/T2) are classic for Pigmented Villonodular Synovitis (PVNS), currently termed diffuse Tenosynovial Giant Cell Tumor (TGCT). The pathogenesis of TGCT involves a specific genetic translocation—most commonly t(1;2)(p13;q37)—that leads to the overexpression of Colony-Stimulating Factor 1 (CSF1) by a small clone of neoplastic synovial cells. This overexpressed CSF1 acts as a chemoattractant, massively recruiting CSF1R-expressing macrophages, which form the bulk of the tumor mass. Pexidartinib, a targeted CSF1R inhibitor, is FDA-approved for adults with symptomatic, advanced TGCT not amenable to improvement with surgery.
Question 41:
A 35-year-old male presents with chronic, dull pain in his left hip. Radiographs demonstrate a radiolucent lesion located within the proximal femoral epiphysis. A biopsy is performed, and histologic examination reveals lobules of cells with distinct cell membranes and abundant clear cytoplasm, interspersed with woven bone and areas of chondroid matrix. What is the most likely diagnosis?
Options:
- Chondroblastoma
- Clear cell chondrosarcoma
- Giant cell tumor of bone
- Osteosarcoma
- Ewing sarcoma
Correct Answer: Clear cell chondrosarcoma
Explanation:
The clinical presentation and histology are classic for clear cell chondrosarcoma. This is a rare, low-grade malignant cartilaginous tumor that characteristically arises in the epiphysis of long bones (most commonly the proximal femur or humerus) in adults (typically 3rd to 5th decades). Histologically, it is defined by cells with abundant clear cytoplasm (due to glycogen) and distinct cell membranes, admixed with woven bone and hyaline cartilage. While chondroblastoma also occurs in the epiphysis, it typically affects skeletally immature patients and shows 'chicken-wire' calcification with mononuclear cells and osteoclast-like giant cells, lacking the distinct clear cells seen in clear cell chondrosarcoma.
Question 42:
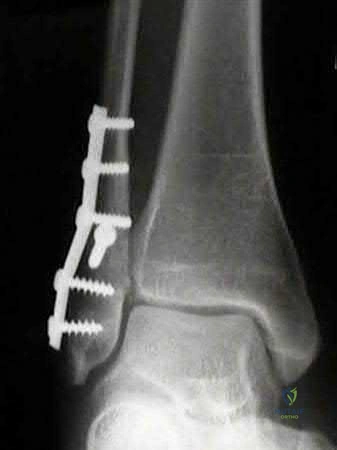
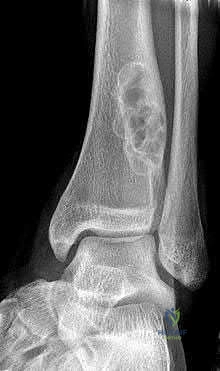
A 14-year-old girl presents with progressive pain and swelling over her proximal fibula. Radiographs demonstrate an expansile, multiloculated lytic lesion as seen in the representative radiograph. A core needle biopsy confirms a primary aneurysmal bone cyst (ABC). Which of the following genetic alterations is most characteristic of primary aneurysmal bone cysts?
Options:
- t(11;22) EWS-FLI1
- t(X;18) SYT-SSX
- t(16;17) CDH11-USP6
- GNAS1 mutation
- EXT1 mutation
Correct Answer: t(16;17) CDH11-USP6
Explanation:
Primary aneurysmal bone cysts (ABCs) are now recognized as true neoplasms driven by recurrent translocations, most commonly t(16;17)(q22;p13), which fuses the promoter region of the osteoblast cadherin 11 gene (CDH11) to the ubiquitin-specific protease 6 gene (USP6). This leads to USP6 upregulation. t(11;22) is seen in Ewing sarcoma. t(X;18) is seen in Synovial Sarcoma. GNAS1 mutations are associated with fibrous dysplasia. EXT1/EXT2 mutations are linked to multiple hereditary exostoses.
Question 43:
A 28-year-old female presents with a painless, slow-growing mass on the posterior aspect of her distal thigh. Radiographs reveal a densely mineralized, lobulated mass attached to the posterior cortex of the distal femur via a broad base. Biopsy reveals a low-grade spindle cell proliferation with well-formed woven bone trabeculae. Which of the following molecular alterations is most commonly associated with this tumor?
Options:
- MDM2 and CDK4 amplification
- TP53 mutation
- H3F3A mutation
- USP6 rearrangement
- FUS-CHOP fusion
Correct Answer: MDM2 and CDK4 amplification
Explanation:
The patient's presentation is classic for a parosteal osteosarcoma, a low-grade surface osteosarcoma that typically arises on the posterior aspect of the distal femur. Cytogenetically, parosteal osteosarcomas are characterized by supernumerary ring chromosomes containing amplified sequences of 12q13-15, which include the MDM2 and CDK4 genes. MDM2 inhibits p53, and CDK4 promotes cell cycle progression. TP53 mutations are more common in conventional high-grade osteosarcoma. H3F3A mutations are seen in giant cell tumors of bone and chondroblastomas. FUS-CHOP (FUS-DDIT3) is seen in myxoid liposarcoma.
Question 44:
A 30-year-old male presents with anterior tibial bowing and a persistent dull ache in his leg. Radiographs display a multilocular, 'soap-bubble' appearing lytic lesion in the anterior diaphysis of the tibia. Biopsy demonstrates nests of uniform epithelial cells surrounded by a spindle cell fibrous stroma. Immunohistochemistry shows strong positivity for cytokeratin. What is the most likely diagnosis?
Options:
- Osteofibrous dysplasia
- Adamantinoma
- Fibrous dysplasia
- Metastatic squamous cell carcinoma
- Chondromyxoid fibroma
Correct Answer: Adamantinoma
Explanation:
Adamantinoma is a rare, low-grade malignant bone tumor that almost exclusively occurs in the anterior diaphyseal cortex of the tibia. It has a biphasic histologic pattern consisting of epithelial cells and osteofibrous stroma. The epithelial nature of the cells is confirmed by positive immunostaining for cytokeratins (e.g., AE1/AE3). Osteofibrous dysplasia (OFD) occurs in the same location but typically in children under 10 years old; while OFD may have scattered cytokeratin-positive cells, it lacks the prominent epithelial nests seen in adamantinoma. Metastatic SCC would be extremely rare as a primary presentation in the tibial diaphysis of a 30-year-old and would show marked cytologic atypia.
Question 45:
A 60-year-old male presents with insidious onset of bowel and bladder dysfunction, accompanied by localized sacral pain. Imaging shows a large, destructive midline sacral mass. Histologic examination demonstrates cords of large cells with abundant vacuolated cytoplasm within a myxoid stroma. Which of the following immunohistochemical markers is highly sensitive and specific for the diagnosis of this neoplasm?
Options:
- Brachyury
- S100
- CD99
- Cytokeratin
- SATB2
Correct Answer: Brachyury
Explanation:
The clinical picture and presence of 'physaliferous' (bubbly/vacuolated) cells in a myxoid background are pathognomonic for chordoma, a primary bone tumor arising from notochordal remnants. Brachyury is a transcription factor required for notochordal development and is highly sensitive and specific for chordoma. While chordomas often co-express S100 and cytokeratins, these markers are not specific. CD99 is characteristic of Ewing sarcoma. SATB2 is a marker for osteoblastic differentiation (seen in osteosarcoma).
Question 46:
A 25-year-old male undergoes routine pelvic radiographs after a minor trauma. The films fortuitously reveal numerous 2 to 10 mm distinct sclerotic foci clustered near the joint spaces of the pelvis and proximal femurs. He is otherwise completely asymptomatic but mentions a history of connective tissue nevi (dermatofibrosis lenticularis disseminata). What gene mutation is established as the cause of this skeletal condition?
Options:
- LEMD3
- SQSTM1
- GNAS
- COL1A1
- EXT1
Correct Answer: LEMD3
Explanation:
The presentation is classic for osteopoikilosis ('spotted bone disease'), an asymptomatic, benign autosomal dominant sclerosing bone dysplasia characterized by numerous discrete bone islands clustered at the ends of long bones and pelvis. When accompanied by connective tissue nevi, it is termed Buschke-Ollendorff syndrome. This condition is caused by loss-of-function mutations in the LEMD3 gene. SQSTM1 is associated with Paget's disease of bone. GNAS is associated with Fibrous Dysplasia. COL1A1 is associated with Osteogenesis Imperfecta.
Question 47:
A 45-year-old male presents with a deep, painless intramuscular mass in the anterior thigh. Biopsy reveals a proliferation of small, uniform round-to-oval cells, a prominent plexiform capillary network resembling 'chicken-wire', and small mucin-filled lipoblasts in a myxoid background. Which chromosomal translocation is characteristic of this tumor?
Options:
- t(12;16)(q13;p11)
- t(X;18)(p11;q11)
- t(2;13)(q35;q14)
- t(9;22)(q22;q12)
- t(11;22)(q24;q12)
Correct Answer: t(12;16)(q13;p11)
Explanation:
The histology describes a myxoid liposarcoma, which is characterized by the t(12;16)(q13;p11) translocation resulting in the FUS-DDIT3 (formerly FUS-CHOP) fusion gene in over 90% of cases. t(X;18) is seen in synovial sarcoma. t(2;13) is characteristic of alveolar rhabdomyosarcoma. t(9;22) is seen in extraskeletal myxoid chondrosarcoma. t(11;22) is classic for Ewing sarcoma.
Question 48:
A 32-year-old female presents with a slow-growing, painful mass near her knee joint. MRI reveals a deep, well-circumscribed soft tissue mass adjacent to the joint capsule. Histopathology shows a biphasic tumor comprised of both spindle cells and epithelial-like glandular structures. Which of the following is true regarding this tumor?
Options:
- It originates directly from the synovial lining of the joint
- It is characterized by the t(X;18) chromosomal translocation
- It primarily affects patients over the age of 60
- Complete resistance to radiotherapy is the standard clinical behavior
- The primary treatment is intra-articular steroid injection
Correct Answer: It is characterized by the t(X;18) chromosomal translocation
Explanation:
The tumor is a synovial sarcoma. Despite its name, synovial sarcoma does NOT arise from synovium; it occurs near joints (most commonly the knee in young adults) but arises from multipotent mesenchymal cells. It is defined cytogenetically by the t(X;18)(p11;q11) translocation, which fuses the SS18 (formerly SYT) gene on chromosome 18 with one of the SSX genes on the X chromosome. It affects young adults (ages 15-40 primarily) and is typically treated with wide surgical excision, often combined with radiation therapy, to which it is generally responsive.
Question 49:
A 7-year-old boy presents with severe back pain. Radiographs reveal vertebra plana (flattening) of the T8 vertebral body. A CT-guided needle biopsy demonstrates a dense infiltrate of cells with folded, grooved nuclei intermixed with numerous eosinophils. If electron microscopy were performed on this biopsy specimen, it would most likely reveal which of the following pathognomonic structures?
Options:
- Weibel-Palade bodies
- Birbeck granules
- Russell bodies
- Howell-Jolly bodies
- Negri bodies
Correct Answer: Birbeck granules
Explanation:
The clinical scenario of vertebra plana in a young child combined with histology showing cells with grooved (coffee-bean) nuclei and eosinophils is diagnostic of Langerhans Cell Histiocytosis (Eosinophilic Granuloma). The pathogenic Langerhans cells are characterized ultrastructurally by Birbeck granules, which have a distinctive 'tennis-racket' shape on electron microscopy. Weibel-Palade bodies are found in endothelial cells. Russell bodies are inclusions in plasma cells. Howell-Jolly bodies are nuclear remnants in RBCs. Negri bodies are seen in rabies infection.
Question 50:
A 65-year-old male presents with a large, destructive, expansile lytic lesion of the proximal humerus with an impending fracture. A needle biopsy confirms metastatic clear cell carcinoma consistent with a renal primary. He is scheduled for a wide excision and endoprosthetic reconstruction. To minimize intraoperative complications, what is the most appropriate next step in management prior to surgery?
Options:
- Neoadjuvant radiation therapy
- Preoperative arterial embolization
- Neoadjuvant chemotherapy with doxorubicin
- Denosumab therapy for 6 months
- Intralesional steroid injection
Correct Answer: Preoperative arterial embolization
Explanation:
Renal cell carcinoma (RCC) and thyroid carcinoma metastases to bone are notoriously hypervascular. Surgical intervention without preoperative planning can lead to massive, life-threatening hemorrhage. Therefore, preoperative selective arterial embolization is strongly recommended (typically 24-48 hours before surgery) to reduce intraoperative blood loss. Radiation or systemic treatments do not provide the immediate hemostatic benefit required prior to impending fracture stabilization for RCC metastases.
Question 51:
A 55-year-old male presents with diffuse thigh pain. Radiographs show a permeative, poorly marginated lytic lesion in the femoral diaphysis with minimal periosteal reaction. MRI reveals extensive marrow replacement extending far beyond the cortical changes. A biopsy is performed, showing sheets of atypical lymphoid cells that stain positively for CD20 and CD45. Assuming there is no impending fracture, what is the mainstay of treatment for this condition?
Options:
- Wide surgical resection and endoprosthesis
- Preoperative embolization followed by curettage
- Chemotherapy and radiation therapy
- Denosumab and observation
- Radiofrequency ablation
Correct Answer: Chemotherapy and radiation therapy
Explanation:
The diagnosis is Primary Bone Lymphoma (PBL), most commonly diffuse large B-cell lymphoma (DLBCL), indicated by CD20 and CD45 (LCA) positivity. The hallmark of PBL treatment is that it is fundamentally a medical disease. The mainstay of treatment is systemic combination chemotherapy (e.g., R-CHOP) frequently combined with involved-field radiation therapy. Surgical intervention is contraindicated unless required for the stabilization of an impending or actual pathologic fracture.
Question 52:
A 15-year-old male presents with multiple asymmetric hard nodules on his hands and fingers, causing deformity. He also has several bluish, compressible soft tissue masses on his forearms. He has a known history of multiple enchondromas. Which of the following is the most accurate statement regarding his condition?
Options:
- It is inherited in an autosomal dominant pattern
- He has a nearly 100% risk of developing malignant transformation over his lifetime
- The condition is caused by a germline mutation in EXT1
- The soft tissue masses are neurofibromas
- Prophylactic amputation of affected digits is the standard of care
Correct Answer: He has a nearly 100% risk of developing malignant transformation over his lifetime
Explanation:
The patient has Maffucci syndrome, characterized by multiple enchondromas and soft tissue hemangiomas (bluish, compressible masses). Unlike Ollier disease (multiple enchondromas alone), Maffucci syndrome carries a drastically higher risk of malignant transformation. Nearly 100% of these patients will develop a malignancy in their lifetime, most commonly chondrosarcoma, but also highly frequent are astrocytomas, GI malignancies, and ovarian tumors. It is non-hereditary (sporadic mutations in IDH1/IDH2). EXT1 is associated with Multiple Hereditary Exostoses (osteochondromas).
Question 53:
An 80-year-old male presents with increasing head size, progressive hearing loss, and anterior bowing of his tibiae. Radiographs of the skull display a classic 'cotton wool' appearance. Laboratory testing reveals markedly elevated alkaline phosphatase but normal serum calcium and phosphorus. The underlying pathogenesis of this disease is most strongly associated with mutations in which of the following genes?
Options:
- SQSTM1
- COL1A1
- FGFR3
- RUNX2
- COMP
Correct Answer: SQSTM1
Explanation:
The clinical and radiographic findings are classic for Paget's disease of bone. Paget's disease is characterized by an initial phase of rampant osteoclastic bone resorption followed by disorganized osteoblastic bone formation (elevated ALP with normal calcium/phosphorus). Up to 40-50% of familial cases and 5-10% of sporadic cases of Paget's disease are associated with mutations in the SQSTM1 gene (sequestosome 1), which leads to increased osteoclast activation via the NF-kB pathway.
Question 54:
A 45-year-old asymptomatic female undergoes a lumbar spine MRI for mild mechanical back pain. An incidental finding at the L3 vertebral body is noted. The discrete lesion is hyperintense on both T1- and T2-weighted MRI sequences. A subsequent CT scan reveals a 'polka-dot' appearance in the axial plane and coarse vertical trabeculations in the sagittal plane. What is the most likely diagnosis?
Options:
- Metastatic breast carcinoma
- Vertebral hemangioma
- Multiple myeloma
- Chordoma
- Eosinophilic granuloma
Correct Answer: Vertebral hemangioma
Explanation:
The findings are pathognomonic for a vertebral hemangioma. Hemangiomas contain fat and vascular channels, which results in high signal intensity on both T1 and T2 MRI sequences. The compensatory thickening of the remaining vertical trabeculae gives the classic 'corduroy' or 'jail-bar' appearance on sagittal CT/plain film, and the 'polka-dot' appearance on axial CT. They are usually asymptomatic, benign incidental findings requiring no treatment.
Question 55:
A 22-year-old male presents with chronic mid-back pain. He describes the pain as a dull, constant ache that is not reliably relieved by NSAIDs. A CT scan of the thoracic spine shows a 3.5 cm expansile, radiolucent lesion with scattered matrix calcifications originating in the posterior elements of T10. Histology demonstrates interconnected trabeculae of woven bone lined by prominent, plump osteoblasts within a highly vascularized connective tissue stroma. What is the most likely diagnosis?
Options:
- Osteoid osteoma
- Osteoblastoma
- Aneurysmal bone cyst
- Chondroblastoma
- Giant cell tumor
Correct Answer: Osteoblastoma
Explanation:
The clinical presentation and histology describe an osteoblastoma. Histologically, osteoblastoma is very similar (often identical) to osteoid osteoma, displaying woven bone trabeculae rimmed by active osteoblasts. However, osteoblastomas are distinguished clinically and radiographically by their larger size (>2 cm), progressive growth, and propensity to cause pain that is typically NOT relieved by NSAIDs or aspirin (unlike the nocturnal pain of osteoid osteoma that responds dramatically to NSAIDs). They most commonly occur in the posterior elements of the spine.
Question 56:
A 35-year-old male presents with recurrent, spontaneous hemarthrosis and a boggy, painless swelling of the right knee. MRI demonstrates a villous, nodular intra-articular synovial mass. The mass exhibits a profound 'blooming artifact' on gradient-echo sequences. Which molecular alteration is the primary driver of this disease process?
Options:
- Overexpression of colony-stimulating factor 1 (CSF1)
- Amplification of MDM2
- Mutation in IDH1
- Translocation t(11;22)
- Mutation in GNAS
Correct Answer: Overexpression of colony-stimulating factor 1 (CSF1)
Explanation:
The clinical and MRI findings (specifically the 'blooming artifact' on gradient-echo MRI due to hemosiderin deposition) are characteristic of Pigmented Villonodular Synovitis (PVNS), now more accurately termed Tenosynovial Giant Cell Tumor (TGCT). The pathogenesis of TGCT involves a specific genetic translocation, t(1;2)(p13;q37), which fuses the COL6A3 gene to the CSF1 gene, leading to the overexpression of colony-stimulating factor 1 (CSF1). This attracts a massive non-neoplastic infiltrate of macrophages and multinucleated giant cells that form the bulk of the tumor mass. Pexidartinib, a CSF1R inhibitor, is an FDA-approved targeted therapy for this condition.
Question 57:
A 28-year-old female develops a rapidly enlarging, destructive lytic lesion in the distal femur. Biopsy confirms a Giant Cell Tumor of Bone (GCTB). Due to extensive joint involvement making joint-sparing resection impossible, medical therapy with Denosumab is initiated to downstage the tumor prior to surgery. What is the precise mechanism of action of Denosumab in the treatment of GCTB?
Options:
- It directly induces apoptosis of the neoplastic mononuclear stromal cells
- It is a monoclonal antibody that binds to RANKL, preventing activation of the giant cells
- It inhibits the tyrosine kinase activity of the CSF1 receptor
- It acts as an angiogenesis inhibitor via VEGF blockade
- It binds to estrogen receptors on giant cells, inhibiting proliferation
Correct Answer: It is a monoclonal antibody that binds to RANKL, preventing activation of the giant cells
Explanation:
Giant Cell Tumor of Bone (GCTB) consists of neoplastic mononuclear stromal cells that express high levels of RANK Ligand (RANKL). This RANKL recruits and activates reactive osteoclast-like multinucleated giant cells, which cause the massive bone destruction seen in the disease. Denosumab is a fully human monoclonal antibody that binds directly to RANKL, preventing it from interacting with the RANK receptor on the surface of osteoclast precursors and giant cells. This effectively halts osteolysis. It does not directly kill the neoplastic stromal cells.
Question 58:
A 5-year-old boy presents with progressive anterior bowing of the left tibia. Radiographs reveal a sharply marginated, radiolucent, intracortical lesion in the anterior diaphyseal cortex of the tibia with a sclerotic margin. Biopsy confirms woven bone trabeculae rimmed by prominent osteoblasts within a bland fibrous stroma. No epithelial nests are seen. What is the recommended initial management for this lesion, assuming no impending fracture?
Options:
- Wide excision and allograft reconstruction
- Intralesional curettage and bone grafting
- Observation and close clinical follow-up
- Neoadjuvant chemotherapy
- Immediate prophylactic intramedullary nailing
Correct Answer: Observation and close clinical follow-up
Explanation:
The clinical presentation is classic for Osteofibrous Dysplasia (Campanacci disease), an uncommon benign bone lesion almost exclusively found in the anterior cortex of the tibia in children under 10 years old. Histology shows bone trabeculae with prominent osteoblastic rimming (unlike fibrous dysplasia). Because the lesion generally halts progression or regresses after skeletal maturity, and because early surgical intervention carries a high rate of recurrence (and risk of pseudoarthrosis), the initial management of choice is observation. Surgery is reserved for severe progressive deformity or non-healing fractures, typically delayed until skeletal maturity if possible.
Question 59:
A 19-year-old male presents with persistent right pelvic pain. Radiographs show a large, aggressive-appearing lytic lesion in the right ilium with cortical breakthrough. Biopsy demonstrates a hypocellular proliferation of bland, benign-appearing spindle cells (fibroblasts) separated by abundant dense collagen bundles. No cytologic atypia, pleomorphism, or mitotic figures are observed. This rare primary bone tumor is considered the osseous counterpart of which of the following soft tissue lesions?
Options:
- Nodular fasciitis
- Desmoid tumor (aggressive fibromatosis)
- Fibrosarcoma
- Myxofibrosarcoma
- Elastofibroma
Correct Answer: Desmoid tumor (aggressive fibromatosis)
Explanation:
The histology and clinical behavior describe a desmoplastic fibroma of bone. This is a rare, locally aggressive, benign primary bone tumor characterized by dense collagenous tissue and bland spindle cells. It does not metastasize but causes significant local destruction. It is considered the exact intraosseous equivalent of a soft tissue desmoid tumor (aggressive fibromatosis). Like desmoid tumors, it requires wide surgical margins to prevent high rates of local recurrence.
Question 60:
A 65-year-old male presents with severe back pain and generalized fatigue. Radiographs demonstrate multiple 'punched-out' lytic lesions in the skull and pelvis. A bone marrow biopsy confirms 20% clonal plasma cells. According to the classic 'CRAB' criteria, which of the following findings is NOT an accepted criterion defining end-organ damage in symptomatic multiple myeloma?
Options:
- Hypercalcemia
- Renal insufficiency
- Anemia
- Osteolytic bone lesions
- Elevated alkaline phosphatase > 3x normal
Correct Answer: Elevated alkaline phosphatase > 3x normal
Explanation:
The CRAB criteria defining symptomatic multiple myeloma include: Calcium elevation (Hypercalcemia), Renal insufficiency, Anemia, and Bone abnormalities (lytic lesions, severe osteopenia, or pathologic fractures). Elevated alkaline phosphatase is NOT part of the CRAB criteria. In fact, a hallmark of multiple myeloma bone disease is the profound uncoupling of bone turnover: profound osteoclast activation with severe suppression of osteoblast activity. Consequently, alkaline phosphatase (an osteoblast marker) is typically normal in myeloma patients, unless there is a healing fracture.
Question 61:
A 25-year-old male presents with a long-standing history of anterior leg pain. Radiographs reveal an eccentrically located, multi-loculated, purely lytic lesion in the anterior tibial diaphysis. Biopsy demonstrates a biphasic tumor with nests of epithelial cells surrounded by a fibrous stroma. Immunohistochemistry is strongly positive for cytokeratin. What is the most likely diagnosis?
Options:
- Osteosarcoma
- Ewing Sarcoma
- Adamantinoma
- Osteofibrous Dysplasia
- Fibrous Dysplasia
Correct Answer: Adamantinoma
Explanation:
The clinical presentation and classic anterior tibial diaphyseal location are hallmark for adamantinoma. It is a low-grade malignant bone tumor. Histologically, it presents with an epithelial component that stains positive for cytokeratin, distinguishing it from osteofibrous dysplasia (which is often considered a benign precursor but lacks frank cytokeratin-positive epithelial nests on standard evaluation, though scattered positive cells may exist). Wide surgical resection is the treatment of choice.
Question 62:
A 45-year-old woman presents with progressive diffuse muscle weakness and bone pain over the past year. Laboratory studies reveal severe hypophosphatemia, normocalcemia, normal PTH levels, and markedly elevated alkaline phosphatase. Further workup identifies a small soft tissue mass in her thigh. Secretion of which of the following substances by this tumor is primarily responsible for her metabolic derangement?
Options:
- Parathyroid hormone (PTH)
- Fibroblast growth factor 23 (FGF-23)
- 1,25-dihydroxyvitamin D
- Calcitonin
- PTH-related peptide (PTHrP)
Correct Answer: Fibroblast growth factor 23 (FGF-23)
Explanation:
This clinical scenario describes tumor-induced osteomalacia (TIO), a paraneoplastic syndrome most commonly caused by a phosphaturic mesenchymal tumor. The tumor secretes Fibroblast Growth Factor 23 (FGF-23), which inhibits sodium-phosphate cotransporters in the proximal renal tubule (leading to phosphate wasting) and inhibits 1-alpha-hydroxylase (decreasing active vitamin D levels). Resection of the tumor usually cures the metabolic defect.
Question 63:
A 28-year-old male presents with a slowly enlarging soft tissue mass near his knee joint. MRI shows a heterogenous, well-circumscribed juxta-articular soft tissue mass that does not enter the joint space. Biopsy confirms a biphasic morphology with spindle cells and epithelial-like glandular structures. Which specific chromosomal translocation is diagnostic for this malignancy?
Options:
- t(11;22)(q24;q12)
- t(X;18)(p11;q11)
- t(12;16)(q13;p11)
- t(2;13)(q35;q14)
- t(12;22)(q13;q12)
Correct Answer: t(X;18)(p11;q11)
Explanation:
The vignette describes a synovial sarcoma, which frequently occurs as a juxta-articular mass in young adults (rarely strictly intra-articular). The pathognomonic genetic alteration is the t(X;18)(p11;q11) translocation, which results in the SYT-SSX fusion gene. t(11;22) is Ewing sarcoma, t(12;16) is myxoid liposarcoma, t(2;13) is alveolar rhabdomyosarcoma, and t(12;22) is clear cell sarcoma.
Question 64:
A 55-year-old male presents with bowel and bladder dysfunction and sacral pain. Imaging demonstrates a destructive midline sacral mass. Core needle biopsy reveals large, vacuolated cells with abundant bubbly cytoplasm arranged in cords and lobules within a myxoid stroma. Which of the following immunohistochemical markers is most highly sensitive and specific for confirming this diagnosis?
Options:
- Cytokeratin
- S-100
- Brachyury
- CD99
- Smooth muscle actin
Correct Answer: Brachyury
Explanation:
The clinical picture and presence of 'physaliferous' (bubbly) cells is characteristic of a chordoma, a tumor arising from notochordal remnants most commonly found in the sacrococcygeal region or spheno-occipital (clivus) region. While chordomas often express cytokeratin and S-100, the nuclear transcription factor brachyury is considered the most highly sensitive and specific diagnostic marker for notochordal differentiation.
Question 65:
A 6-year-old boy presents with back pain. Radiographs reveal a severe collapse of the T8 vertebral body, often termed 'vertebra plana.' Biopsy of the lesion demonstrates a prominent population of large cells with grooved nuclei mixed with eosinophils. Electron microscopy of these cells is most likely to reveal which of the following ultrastructural features?
Options:
- Weibel-Palade bodies
- Howell-Jolly bodies
- Birbeck granules
- Auer rods
- Heinz bodies
Correct Answer: Birbeck granules
Explanation:
The clinical and radiographic presentation of 'vertebra plana' in a young child combined with grooved nuclei and eosinophils on histology is diagnostic of Langerhans Cell Histiocytosis (Eosinophilic Granuloma). On electron microscopy, the diagnostic ultrastructural finding is Birbeck granules, which have a characteristic 'tennis racket' appearance. These cells also classically stain positive for CD1a and S-100.
Question 66:
A 16-year-old boy presents with severe right thigh pain that awakens him from sleep. The pain is consistently and rapidly relieved by taking ibuprofen. A CT scan demonstrates a well-circumscribed 8 mm radiolucent nidus surrounded by dense sclerotic bone in the proximal femur. The intense, nocturnal pain experienced by this patient is directly mediated by dramatically elevated local production of which of the following?
Options:
- Interleukin-1 (IL-1)
- Prostaglandin E2 (PGE2)
- Tumor Necrosis Factor-alpha (TNF-a)
- Substance P
- Bradykinin
Correct Answer: Prostaglandin E2 (PGE2)
Explanation:
The classic presentation of an osteoid osteoma includes nocturnal pain that is dramatically responsive to NSAIDs. This response occurs because the nidus of the osteoid osteoma produces high levels of Prostaglandin E2 (PGE2). Cyclooxygenase inhibitors (NSAIDs) block the production of PGE2, providing substantial pain relief.
Question 67:
A 32-year-old female presents with pain and swelling in her distal femur. Radiographs reveal an eccentrically placed lytic lesion extending into the epiphysis up to the subchondral bone. Biopsy confirms Giant Cell Tumor of bone (GCT). Medical therapy with Denosumab can be utilized in unresectable or recurrent cases. What is the precise mechanism of action of Denosumab in treating this lesion?
Options:
- Inhibiting Vascular Endothelial Growth Factor (VEGF)
- Inhibiting Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL)
- Stimulating osteoblast differentiation via Wnt signaling
- Inhibiting mammalian target of rapamycin (mTOR)
- Inhibiting tyrosine kinases associated with c-KIT
Correct Answer: Inhibiting Receptor Activator of Nuclear Factor Kappa-B Ligand (RANKL)
Explanation:
In Giant Cell Tumor of bone, the neoplastic cells are actually the mononuclear stromal cells, which express high levels of RANKL. The multinucleated giant cells are reactive, non-neoplastic osteoclasts expressing RANK. Denosumab is a monoclonal antibody that binds and inhibits RANKL, effectively halting the recruitment and activation of the bone-destroying giant cells, leading to tumor calcification and stabilization.
Question 68:
A slow-growing primary malignant bone tumor composed of abundant clear cytoplasm and chondroid matrix is diagnosed on core needle biopsy. Which of the following best describes the typical demographic and anatomical location for Clear Cell Chondrosarcoma?
Options:
- Diaphyseal lesion in a child (under 10 years)
- Metaphyseal lesion in an adolescent (10-20 years)
- Epiphyseal lesion in an older adult (30-50 years)
- Cortical lesion in a teenager
- Juxta-articular soft tissue mass in a young adult
Correct Answer: Epiphyseal lesion in an older adult (30-50 years)
Explanation:
Clear cell chondrosarcoma is a rare, low-grade malignant cartilaginous tumor. It is distinctive because it classically involves the epiphysis (often of the proximal femur or humerus) and typically occurs in older adults (third to fifth decade). It is frequently confused with chondroblastoma radiographically, but chondroblastoma usually occurs in skeletally immature patients (teens).
Question 69:
A 70-year-old male with a known history of advanced Paget's disease of bone presents with a sudden, rapid increase in pain and a progressively enlarging mass in his right hemipelvis over the last 2 months. You suspect a sarcomatous transformation. Historically, which of the following viral inclusions has been controversially linked to the underlying pathophysiology of his long-standing bone disease?
Options:
- Epstein-Barr virus
- Cytomegalovirus
- Paramyxovirus
- Adenovirus
- Parvovirus B19
Correct Answer: Paramyxovirus
Explanation:
Paget's disease has a known, albeit rare (approx. 1%), risk of malignant transformation, most commonly to osteosarcoma. The etiology of Paget's disease remains incompletely understood but involves a mix of genetics (SQSTM1 mutations) and potential viral factors. Intranuclear inclusion bodies resembling Paramyxovirus (specifically measles virus or respiratory syncytial virus nucleocapsids) have been observed in pagetic osteoclasts, leading to the viral hypothesis of its etiology.
Question 70:
A 55-year-old male presents with deep thigh pain. Radiographs show a permeative, destructive diaphyseal lesion in the femur with minimal periosteal reaction. MRI shows extensive marrow replacement. Biopsy yields a diagnosis of primary lymphoma of bone. The majority of primary bone lymphomas will stain strongly positive for which of the following cluster of differentiation (CD) markers?
Options:
- CD99
- CD1a
- CD20
- Cytokeratin
- S-100
Correct Answer: CD20
Explanation:
Primary lymphoma of bone is most commonly Diffuse Large B-cell Lymphoma (DLBCL). Therefore, the neoplastic cells will strongly express B-cell markers such as CD20, as well as the leukocyte common antigen CD45. CD99 is typically associated with Ewing Sarcoma (though it can occasionally be positive in lymphoblastic lymphomas, DLBCL is primarily CD20+). CD1a is a marker for Langerhans Cell Histiocytosis.
Question 71:
A 22-year-old male presents with a painful mass in his quadriceps muscle 4 weeks after suffering a blunt contusion during a football game. A biopsy is taken from the mass due to concerns for a soft tissue sarcoma. Which of the following histologic patterns is most characteristic of Myositis Ossificans and helps distinguish it from an extraskeletal osteosarcoma?
Options:
- Central maturation with peripheral immature woven bone
- Peripheral maturation with mature lamellar bone surrounding an immature cellular center
- Diffuse cellular atypia with irregular mitotic figures throughout
- Chondroid matrix forming a thick cap over mature trabecular bone
- Spindle cells forming a herring-bone pattern with minimal osteoid
Correct Answer: Peripheral maturation with mature lamellar bone surrounding an immature cellular center
Explanation:
Myositis ossificans classically demonstrates a 'zonal phenomenon' of maturation. The periphery of the lesion consists of mature, well-organized lamellar bone, while the central portion is composed of highly cellular, immature fibroblasts and woven bone. This is the exact opposite of osteosarcoma, which typically shows less mature, anaplastic cells and malignant osteoid at its growing periphery.
Question 72:
A patient with Maffucci syndrome is at an increased risk of multiple conditions compared to a patient with isolated Ollier disease. Which of the following clinical features and associated risks most accurately distinguish Maffucci syndrome from Ollier disease?
Options:
- Multiple enchondromas and café-au-lait spots
- Multiple enchondromas, soft tissue hemangiomas, and increased risk of gastrointestinal/ovarian malignancies
- Multiple osteochondromas and precocious puberty
- Fibrous dysplasia and intramuscular myxomas
- Enchondromatosis and bilateral acoustic neuromas
Correct Answer: Multiple enchondromas, soft tissue hemangiomas, and increased risk of gastrointestinal/ovarian malignancies
Explanation:
Maffucci syndrome is characterized by the presence of multiple enchondromas associated with soft tissue hemangiomas (often presenting as bluish nodules with phleboliths on X-ray). Patients with Maffucci syndrome have a high risk of malignant transformation to chondrosarcoma (up to 100% in some series) and an increased risk of visceral malignancies, including astrocytomas, and GI or ovarian cancers. Ollier disease consists of multiple enchondromas without the hemangiomas.
Question 73:
A 40-year-old asymptomatic female undergoes a lumbar spine MRI for mild lower back pain. An incidental lesion is found in the L3 vertebral body. On plain radiographs, this lesion has a coarse, vertically striated 'corduroy' appearance. What are the expected signal characteristics of this lesion on a non-contrast MRI?
Options:
- Low T1, High T2 signal
- High T1, High T2 signal
- Low T1, Low T2 signal
- High T1, Low T2 signal
- Intermediate T1, Intermediate T2 signal
Correct Answer: High T1, High T2 signal
Explanation:
The lesion described is a vertebral hemangioma, characterized by prominent vertical trabeculae appearing as 'corduroy' on plain film or 'polka dots' on axial CT. Due to their high adipose (fat) content, benign intraosseous hemangiomas characteristically demonstrate high signal intensity on both T1-weighted and T2-weighted MRI sequences.
Question 74:
A 35-year-old female presents with a painless mass on the posterior aspect of her distal thigh. Radiographs demonstrate a dense, lobulated, heavily ossified mass attached to the posterior cortex of the distal femur on a broad stalk, with no medullary involvement. A core biopsy confirms a low-grade malignant spindle cell stroma with well-formed woven bone trabeculae. Amplification of which of the following gene pairs is a pathognomonic molecular feature of this tumor?
Options:
- TP53 and RB1
- MDM2 and CDK4
- c-MYC and N-MYC
- EWSR1 and FLI1
- GNAS and EXT1
Correct Answer: MDM2 and CDK4
Explanation:
This is a classic presentation of parosteal osteosarcoma, a low-grade surface osteosarcoma most commonly arising on the posterior distal femur. It is characterized molecularly by ring chromosomes and supernumerary ring chromosomes containing amplification of the 12q13-15 region, which houses the MDM2 and CDK4 genes.
Question 75:
A 65-year-old male with a known history of metastatic clear cell Renal Cell Carcinoma (RCC) presents with an impending pathologic fracture of his right proximal femur. A prophylactic stabilization surgery is planned. Which of the following preoperative interventions is most critical to reduce perioperative mortality and morbidity?
Options:
- Preoperative radiation therapy
- Immediate prophylactic intramedullary nailing
- Preoperative angiographic embolization
- Initiation of bisphosphonates 4 weeks prior to surgery
- Neoadjuvant multi-agent chemotherapy
Correct Answer: Preoperative angiographic embolization
Explanation:
Metastatic renal cell carcinoma (as well as metastatic thyroid cancer) lesions to bone are notoriously hypervascular. Surgical intervention without prior intervention can lead to massive, life-threatening intraoperative hemorrhage. Preoperative selective angiographic embolization (typically 24-48 hours before surgery) is a critical step in managing these specific metastatic lesions to minimize surgical blood loss.
Question 76:
Aneurysmal bone cysts (ABCs) were historically considered entirely reactive lesions but are now recognized to have a primary neoplastic pathogenesis in many cases. Primary ABCs are most commonly driven by a recurrent chromosomal translocation resulting in the upregulation of which of the following genes?
Options:
- Translocation t(11;22) EWSR1-FLI1
- Rearrangement of the USP6 gene at 17p13
- Activating mutation of the GNAS gene
- Mutation in the EXT1 or EXT2 genes
- MDM2 amplification
Correct Answer: Rearrangement of the USP6 gene at 17p13
Explanation:
Primary Aneurysmal Bone Cysts (ABCs) are neoplastic and characterized by a recurrent t(16;17) translocation that results in fusion of the promoter region of the CDH11 gene with the coding sequence of the USP6 gene. This leads to transcriptional upregulation of USP6, which drives the formation of the cyst. This genetic finding separates primary ABCs from secondary ABC-like changes found in other tumors (e.g., giant cell tumor, chondroblastoma).
Question 77:
A 14-year-old girl is evaluated for a progressive deformity of her proximal femur. Radiographs show a purely lytic lesion in the metadiaphysis with a classic 'ground-glass' matrix and a 'shepherd's crook' varus deformity. Which of the following genetic alterations is responsible for the pathogenesis of this condition?
Options:
- EXT1 mutation
- USP6 rearrangement
- GNAS activating mutation
- TP53 deletion
- RB1 loss of heterozygosity
Correct Answer: GNAS activating mutation
Explanation:
The clinical and radiographic description is classic for Fibrous Dysplasia (ground glass matrix, shepherd's crook deformity). Fibrous dysplasia is caused by a somatic activating missense mutation in the GNAS gene (specifically at the Arg201 codon), which encodes the alpha subunit of the Gs stimulatory protein. This leads to constitutive activation of adenylate cyclase and excessive intracellular cAMP, preventing proper maturation of osteoblasts.
Question 78:
A 9-year-old boy presents with a pathologic fracture through a well-circumscribed, centrally located radiolucent lesion in the proximal humerus metaphysis. A cortical fragment is seen resting at the dependent portion of the lucency ('fallen leaf' sign). Which of the following best describes the accepted pathophysiology driving the expansion of this lesion?
Options:
- Abnormal proliferation of monoclonal plasma cells
- Venous outflow obstruction leading to elevated intra-cystic fluid pressure and prostaglandins
- A traumatic arteriovenous fistula within the metaphysis
- Overexpression of RANKL by neoplastic mononuclear cells
- Failure of osteoclast formation at the physis
Correct Answer: Venous outflow obstruction leading to elevated intra-cystic fluid pressure and prostaglandins
Explanation:
The vignette describes a Unicameral Bone Cyst (UBC) or Simple Bone Cyst. The pathophysiology of UBCs is widely believed to be caused by a focal venous outflow obstruction within the bone, leading to elevated intra-cystic pressures. The accumulated fluid has been found to have high levels of prostaglandins, interleukins, and other bone-resorbing factors that drive continuous cyst expansion.
Question 79:
A 21-year-old male presents with chronic, dull back pain. Radiographs and CT show a 3.5 cm expansile, radiolucent mass with central ossification involving the posterior elements of the L4 vertebra. Which of the following features differentiates this diagnosis (Osteoblastoma) from an Osteoid Osteoma?
Options:
- Size <1.5 cm and nocturnal pain completely relieved by NSAIDs
- Epiphyseal location and "chicken wire" calcification
- Size >2.0 cm and progressive dull aching pain not completely relieved by NSAIDs
- Permeative diaphyseal destruction with an "onion skin" periosteal reaction
- Purely lytic metaphyseal lesion with a "fallen leaf" sign
Correct Answer: Size >2.0 cm and progressive dull aching pain not completely relieved by NSAIDs
Explanation:
Osteoblastoma and osteoid osteoma are histologically very similar (forming woven bone trabeculae lined by prominent osteoblasts). However, osteoblastoma is distinguished clinically and radiographically: it is larger (defined as >2 cm, whereas osteoid osteoma is <1.5-2 cm), often found in the spine (posterior elements), and produces a dull, aching pain that is generally NOT completely relieved by NSAIDs, unlike the classic nocturnal NSAID-responsive pain of an osteoid osteoma.
Question 80:
A 28-year-old female presents with a deep-seated soft tissue mass in her foot. A biopsy is obtained and demonstrates nests of pale spindle cells separated by fibrous septae. The tumor stains positive for S-100 and HMB-45. This lesion, historically known as 'melanoma of soft parts,' is characterized by which of the following cytogenetic abnormalities?
Options:
- t(11;22) EWSR1-FLI1
- t(X;18) SYT-SSX
- t(12;22) EWSR1-ATF1
- t(2;13) PAX3-FOXO1
- t(9;22) BCR-ABL
Correct Answer: t(12;22) EWSR1-ATF1
Explanation:
Clear Cell Sarcoma of soft tissue is often called 'melanoma of soft parts' due to its melanin production and positive staining for neural crest/melanocytic markers (S-100, HMB-45, Melan-A). Unlike true cutaneous melanoma, it is defined by a characteristic reciprocal translocation t(12;22)(q13;q12), which results in the EWSR1-ATF1 fusion transcript.
Question 81:
A 28-year-old female presents with a painless mass on the posterior aspect of her distal thigh. Radiographs demonstrate a dense, lobulated, ossified mass attached to the posterior cortex of the distal femur by a broad base, with a visible radiolucent 'string sign' separating part of the tumor from the cortex. Histologic examination reveals well-differentiated spindle cells with minimal atypia embedded in a fibrous stroma, interspersed with well-formed woven bone trabeculae. Which of the following genetic amplifications is diagnostic for this condition?
Options:
- MDM2
- USP6
- H3F3A
- EXT1
- GNAS
Correct Answer: MDM2
Explanation:
The clinical, radiographic, and histologic descriptions are classic for parosteal osteosarcoma. This is a low-grade surface osteosarcoma typically located on the posterior distal femur. The 'string sign' represents a radiolucent cleft between the tumor and the underlying cortex. Parosteal osteosarcoma is characterized by the amplification of MDM2 and CDK4 genes on chromosome 12q13-15. USP6 is associated with Aneurysmal Bone Cysts; H3F3A with Giant Cell Tumors of bone and Chondroblastoma; EXT1 with Osteochondromas; and GNAS with Fibrous Dysplasia.
Question 82:
A 14-year-old boy presents with multiple unilateral cartilaginous bone tumors and multiple soft tissue hemangiomas exhibiting phleboliths on radiographs. He is diagnosed with a rare non-hereditary congenital disorder. What is the most likely gene mutation associated with this syndrome?
Options:
- EXT1 or EXT2
- IDH1 or IDH2
- PTEN
- GNAS
- APC
Correct Answer: IDH1 or IDH2
Explanation:
The patient has Maffucci syndrome, characterized by multiple enchondromas and soft tissue hemangiomas (distinguishing it from Ollier disease, which is multiple enchondromas alone). Both Ollier disease and Maffucci syndrome are associated with somatic mosaic mutations in the IDH1 or IDH2 genes. The risk of malignant transformation (most commonly to secondary chondrosarcoma) is nearly 100% over the patient's lifetime in Maffucci syndrome, and up to 30% in Ollier disease. EXT mutations cause Multiple Hereditary Exostoses (MHE).
Question 83:
A 45-year-old male presents with chronic hip pain. Radiographs reveal a secondary well-defined, slightly expansile lytic lesion in the epiphysis of the proximal femur. Biopsy reveals uniform cells with central nuclei and abundant vacuolated clear cytoplasm, distinctly clear cell borders, scattered multinucleated giant cells, and reactive bone formation. Which of the following is the most likely diagnosis?
Options:
- Chondroblastoma
- Clear cell chondrosarcoma
- Giant cell tumor of bone
- Metastatic renal cell carcinoma
- Osteoblastoma
Correct Answer: Clear cell chondrosarcoma
Explanation:
Clear cell chondrosarcoma is a rare, low-grade variant of chondrosarcoma that characteristically occurs in the epiphysis of long bones, especially the proximal femur or humerus, in adults (typically 30-50 years old). Histologically, it features cells with abundant clear cytoplasm and distinct boundaries. While chondroblastoma also occurs in the epiphysis and contains giant cells, it typically affects skeletally immature patients (teens). Clear cell chondrosarcoma requires wide surgical resection.
Question 84:
A 35-year-old female undergoes targeted medical therapy for a recurrent, diffuse, destructive intra-articular mass in her knee that is no longer amenable to surgical resection. Histology previously confirmed Pigmented Villonodular Synovitis (PVNS), also known as Tenosynovial Giant Cell Tumor. What is the primary molecular target of the FDA-approved systemic therapy (e.g., Pexidartinib) for this condition?
Options:
- RANKL
- CSF1R
- BRAF
- mTOR
- VEGF
Correct Answer: CSF1R
Explanation:
Tenosynovial Giant Cell Tumor (PVNS) is driven by a chromosomal translocation t(1;2)(p13;q37) fusing COL6A3 to CSF1. This results in an overexpression of Colony-Stimulating Factor 1 (CSF1), which attracts macrophages expressing the CSF1 receptor (CSF1R) that make up the bulk of the tumor mass. Pexidartinib is a highly selective CSF1R inhibitor approved for adults with symptomatic TGCT associated with severe morbidity or functional limitation not amenable to improvement with surgery.
Question 85:
A 25-year-old male presents with anterior lower leg pain. Radiographs show a well-circumscribed, multiloculated, expansile osteolytic lesion in the anterior diaphysis of the tibia. A biopsy demonstrates a biphasic pattern consisting of epithelial cells forming nests and tubular structures, surrounded by bland fibrous spindle cells. The epithelial cells stain strongly positive for cytokeratin. What is the recommended surgical management for this pathology?
Options:
- Intralesional curettage with local adjuvants
- Wide surgical resection
- Primary radiation therapy
- Neoadjuvant chemotherapy followed by wide resection
- Immediate above-knee amputation
Correct Answer: Wide surgical resection
Explanation:
The clinical and histologic findings describe Adamantinoma, a rare, low-grade malignant bone tumor that almost exclusively occurs in the anterior diaphysis of the tibia. The biphasic histology (epithelial and fibrous components) and cytokeratin positivity are pathognomonic. Because it is a low-grade malignancy that does not respond reliably to radiation or chemotherapy, the standard of care is wide surgical resection (often requiring segmental defect reconstruction). Intralesional curettage has an unacceptably high recurrence rate.
Question 86:
A 45-year-old female with a known history of polyostotic fibrous dysplasia presents with a progressively enlarging, painless mass in her quadriceps muscle. A core needle biopsy of the soft tissue mass reveals bland, stellate-to-spindle-shaped cells in an abundant hypovascular, mucopolysaccharide-rich myxoid stroma. What is the most likely diagnosis for the soft tissue mass in the context of her underlying skeletal condition?
Options:
- Myxofibrosarcoma
- Intramuscular myxoma
- Plexiform neurofibroma
- Desmoid tumor
- Liposarcoma
Correct Answer: Intramuscular myxoma
Explanation:
The patient has Mazabraud syndrome, which is characterized by the association of fibrous dysplasia (usually polyostotic) and one or more intramuscular myxomas. The histology describes a benign intramuscular myxoma, which classically presents as an avascular, hypocellular mass with abundant myxoid stroma. Both the fibrous dysplasia and the myxomas in this syndrome share a somatic activating mutation in the GNAS gene.
Question 87:
A 58-year-old male presents with bowel and bladder dysfunction and sacral pain. Imaging reveals a large, destructive, midline mass in the sacrum. Biopsy demonstrates cords and lobules of large cells with abundant, vacuolated, bubbly cytoplasm set in a myxoid stroma. Which of the following immunohistochemical markers is highly sensitive and specific for the diagnosis of this tumor?
Options:
- Cytokeratin
- Brachyury
- S100
- CD99
- SATB2
Correct Answer: Brachyury
Explanation:
The vignette describes a Chordoma, a locally aggressive malignancy arising from remnants of the embryonic notochord. The cells with bubbly cytoplasm are 'physaliferous' cells. Brachyury, a transcription factor essential for notochordal development, is a highly sensitive and specific nuclear immunohistochemical marker for chordoma, reliably distinguishing it from chondrosarcoma. While chordomas also co-express cytokeratin and S100, these are not highly specific.
Question 88:
A 30-year-old male with an unresectable Giant Cell Tumor (GCT) of the sacrum is treated with Denosumab. Which of the following histologic changes is most commonly observed in the tumor tissue after several months of this targeted therapy?
Options:
- Extensive necrosis and apoptosis of the neoplastic mononuclear stromal cells
- Depletion of multinucleated osteoclast-like giant cells and massive deposition of dense woven bone
- Widespread myxoid degeneration with cyst formation
- Transformation into a predominantly chondroid matrix
- Spindle cell sarcomatous transformation as a direct effect of the drug
Correct Answer: Depletion of multinucleated osteoclast-like giant cells and massive deposition of dense woven bone
Explanation:
Denosumab is a monoclonal antibody against RANKL. In GCT of bone, the neoplastic mononuclear stromal cells express RANKL, which recruits and activates the reactive multinucleated osteoclast-like giant cells. By blocking RANKL, Denosumab rapidly eliminates the giant cells. The remaining neoplastic stromal cells subsequently produce abundant dense fibro-osseous tissue (woven bone), which causes the dramatic radiographic sclerosis seen after treatment. Denosumab does not typically kill the neoplastic stromal cells themselves.
Question 89:
A 14-year-old boy is diagnosed with Ewing Sarcoma of the ilium. Cytogenetics confirm a t(11;22) translocation resulting in the EWS-FLI1 fusion protein. At the time of diagnosis, which of the following represents the most significant adverse prognostic factor for overall survival?
Options:
- Age older than 10 years
- Pelvic location of the primary tumor
- Tumor size greater than 8 cm
- Presence of clinically detectable metastatic disease
- Elevated serum lactate dehydrogenase (LDH)
Correct Answer: Presence of clinically detectable metastatic disease
Explanation:
While older age, large tumor size, elevated LDH, and pelvic location (axial skeleton) are all poor prognostic factors in Ewing Sarcoma, the presence of metastatic disease at the time of diagnosis is consistently the most powerful and significant adverse prognostic factor for overall survival. Patients with localized disease have a long-term survival rate of ~70-75%, whereas those with metastatic disease at presentation have a survival rate of <30%.
Question 90:
A 62-year-old male with known metastatic clear cell renal cell carcinoma presents with progressive thigh pain and a substantial, lytic lesion in the proximal femur with an impending pathologic fracture. Prophylactic stabilization with an intramedullary nail is planned. What is the most critical adjunctive procedure to perform 24-48 hours prior to surgical intervention?
Options:
- Postoperative radiation therapy simulation
- Administration of neoadjuvant systemic immunotherapy
- Preoperative selective arterial embolization of the lesion
- Intravenous bisphosphonate infusion to harden the cortex
- Prophylactic stabilization of the contralateral asymptomatic femur
Correct Answer: Preoperative selective arterial embolization of the lesion
Explanation:
Metastatic lesions from renal cell carcinoma (RCC) and thyroid carcinoma are notoriously hypervascular. Surgical intervention, such as curettage or intramedullary nailing, carries a high risk of massive, life-threatening hemorrhage. Preoperative selective arterial embolization is strongly recommended 24-48 hours prior to surgery to minimize intraoperative blood loss.
Question 91:
A 50-year-old male presents with polyneuropathy, generalized edema, new-onset diabetes mellitus, and skin hyperpigmentation. A skeletal survey demonstrates multiple osteosclerotic lesions rather than typical 'punched-out' lytic lesions. This specific constellation of clinical findings is most classically associated with which underlying pathology?
Options:
- Monoclonal plasma cell proliferative disorder
- Metastatic breast carcinoma
- Metastatic prostate carcinoma
- Langerhans cell histiocytosis
- Eosinophilic granulomatosis
Correct Answer: Monoclonal plasma cell proliferative disorder
Explanation:
The vignette describes POEMS syndrome (Polyneuropathy, Organomegaly, Endocrinopathy, Monoclonal gammopathy, and Skin changes). POEMS syndrome is uniquely associated with a variant of plasma cell dyscrasia (monoclonal plasma cell proliferative disorder), most notably osteosclerotic myeloma, where the bone lesions are sclerotic rather than the classic lytic lesions seen in standard multiple myeloma.
Question 92:
A 35-year-old male presents with multi-centric, well-defined osteolytic lesions distributed throughout the bones of his right lower extremity (femur, tibia, and talus). Biopsy of the tibial lesion reveals interconnecting cords and nests of plump, epithelioid cells with intracytoplasmic vacuoles containing erythrocytes, strongly positive for CD31 and ERG. What is the most likely diagnosis?
Options:
- Metastatic melanoma
- Epithelioid hemangioendothelioma
- Enchondromatosis (Ollier disease)
- Kaposi sarcoma
- Bacillary angiomatosis
Correct Answer: Epithelioid hemangioendothelioma
Explanation:
Epithelioid hemangioendothelioma is a low-to-intermediate grade vascular tumor. A classic and highly characteristic presentation of vascular tumors of bone (like hemangioma, hemangioendothelioma, or angiosarcoma) is regional multicentricity—multiple lesions clustering within the bones of a single anatomic region or extremity. Histologically, it forms vascular channels lined by plump epithelioid endothelial cells, which are positive for vascular markers like CD31, CD34, and ERG.
Question 93:
An 18-year-old male presents with severe, progressive back pain that worsens at night and is dramatically relieved by naproxen. He has recently developed a painful scoliosis. CT imaging identifies a 1.0 cm radiolucent nidus surrounded by dense reactive sclerosis in the right posterior elements of the T8 vertebra. Regarding the resultant spinal deformity, which statement is most accurate?
Options:
- The lesion is typically located on the concavity of the scoliotic curve.
- The lesion is typically located on the convexity of the scoliotic curve.
- The lesion is typically located at the exact apex of the convexity.
- The curvature varies randomly and shows no consistent relationship to the lesion side.
- The resultant scoliosis is always non-structural and purely compensatory for leg length inequality.
Correct Answer: The lesion is typically located on the concavity of the scoliotic curve.
Explanation:
The patient has an osteoid osteoma of the spine. When an osteoid osteoma arises in the spine, it predominantly affects the posterior elements (lamina, pedicle). The severe pain causes asymmetric muscle spasm, leading to a scoliotic deformity. Classically, the resulting curve is rigid, and the tumor nidus is found on the concavity of the curve due to the intense local muscle spasm.
Question 94:
A 9-year-old boy sustains a proximal humerus fracture after a minor fall. Radiographs demonstrate a fracture through a large, centrally located, radiolucent lesion in the metaphysis that mildly expands the bone. A small fragment of cortical bone is visible resting at the dependent (bottom) portion of the radiolucent cavity. What is this characteristic radiographic sign called?
Options:
- Sunburst sign
- Fallen leaf sign
- Shepherd's crook deformity
- Corduroy sign
- Blade of grass sign
Correct Answer: Fallen leaf sign
Explanation:
The 'fallen leaf' or 'fallen fragment' sign is pathognomonic for a Simple Bone Cyst (Unicameral Bone Cyst). Because the cyst is fluid-filled and lacks a solid matrix, a fractured fragment of cortex can fall freely through the fluid to rest at the dependent portion of the cavity. If the cyst were a solid tumor (like an enchondroma or fibrous dysplasia), the fragment would remain suspended in place.
Question 95:
A 72-year-old male presents with increasing hat size, hearing loss, and anterior bowing of his tibiae. Laboratory studies show markedly elevated serum alkaline phosphatase with normal calcium and phosphorus. Histologic evaluation of a bone biopsy shows a 'mosaic' pattern of lamellar bone with prominent cement lines. The dysregulated osteoclasts central to this disease's pathogenesis have been hypothesized to be linked to an earlier infection with which viral family?
Options:
- Herpesviridae
- Parvoviridae
- Paramyxoviridae
- Retroviridae
- Papillomaviridae
Correct Answer: Paramyxoviridae
Explanation:
The patient has Paget's disease of bone, which is driven by hyperactive, giant multinucleated osteoclasts. Ultrastructural studies (electron microscopy) of pagetic osteoclasts have revealed nuclear inclusion bodies resembling the nucleocapsids of paramyxoviruses (such as the measles virus or respiratory syncytial virus), leading to the hypothesis that a slow viral infection plays a role in the etiology of Paget's disease, alongside genetic factors like SQSTM1 mutations.
Question 96:
A 45-year-old male presents with chronic knee pain and a sensation of multiple loose bodies 'catching' in the joint. Radiographs show dozens of uniformly sized, calcified nodules confined to the joint space. A synovial biopsy confirms primary synovial chondromatosis. Which of the following best represents the approximate lifetime risk of malignant transformation of this primary condition to chondrosarcoma?
Options:
- Less than 1%
- 5%
- 15%
- 25%
- 50%
Correct Answer: 5%
Explanation:
Primary synovial chondromatosis is a benign neoplastic process of the synovium resulting in multiple intra-articular cartilaginous loose bodies. Although benign, it has a well-documented risk of malignant transformation into secondary synovial chondrosarcoma. The universally cited textbook rate for this malignant transformation is approximately 5%.
Question 97:
A 16-year-old female presents with knee pain. MRI reveals a rapidly expanding, eccentric, purely lytic lesion in the distal femur metaphysis demonstrating multiple fluid-fluid levels. A core biopsy confirms the diagnosis of a primary Aneurysmal Bone Cyst (ABC). The pathogenesis of a primary ABC is most strongly driven by a recurrent chromosomal translocation resulting in the upregulation of which gene?
Options:
Correct Answer: USP6
Explanation:
Primary Aneurysmal Bone Cysts (ABCs) are genuine neoplasms (not just reactive phenomena) driven by recurrent translocations, most commonly t(16;17)(q22;p13), which places the USP6 gene promoter under the control of highly active promoters like CDH11. This leads to the upregulation of USP6. MDM2 is associated with atypical lipomatous tumors and parosteal osteosarcoma; H3F3A with giant cell tumors; EXT1 with osteochondromas; and EWS with Ewing Sarcoma.
Question 98:
A 60-year-old male presents with a permeative, destructive lesion in the diaphyseal marrow cavity of his femur. Biopsy reveals sheets of large, atypical lymphoid cells with prominent nucleoli. The cells strongly express CD20 and CD45, and lack CD99 expression. Which of the following special stains will most characteristically demonstrate a network of fibers wrapping around individual tumor cells, aiding in differentiating this entity from Ewing sarcoma?
Options:
- Periodic Acid-Schiff (PAS)
- Reticulin stain
- Fontana-Masson
- Congo Red
- Masson Trichrome
Correct Answer: Reticulin stain
Explanation:
Primary bone lymphoma (typically Diffuse Large B-Cell Lymphoma, expressing CD20/CD45) can radiographically and histologically mimic Ewing sarcoma. Ewing sarcoma expresses CD99 and is strongly PAS positive (due to intracellular glycogen). A defining histologic feature visible on special stains is that reticulin fibers surround *individual* tumor cells in lymphoma, whereas in Ewing sarcoma (and other carcinomas), reticulin fibers surround *nests* or clusters of cells, rather than individual cells.
Question 99:
A 5-year-old boy presents with painless anterior bowing of the tibia. Radiographs demonstrate a multiloculated, expansile, osteolytic lesion confined to the anterior cortex of the tibial diaphysis. Biopsy reveals fibrous tissue interspersed with trabeculae of woven bone ringed by plump osteoblasts, consistent with Osteofibrous Dysplasia (Campanacci disease). What is the primary reason that wide resection or very close observation is mandated for this condition?
Options:
- It has a near 100% risk of pathological fracture requiring prophylactic nailing.
- It is strongly associated with Neurofibromatosis Type 1 (NF1).
- It shares a close histogenetic relationship with, and may coexist with or progress to, Adamantinoma.
- It carries a high risk of rapid, fatal lung metastasis.
- It undergoes spontaneous malignant transformation to osteosarcoma during adolescence.
Correct Answer: It shares a close histogenetic relationship with, and may coexist with or progress to, Adamantinoma.
Explanation:
Osteofibrous dysplasia (OFD) is a rare fibro-osseous lesion of childhood that predominantly affects the anterior cortex of the tibia. It is critically important because it is considered a precursor to, or part of a spectrum with, Adamantinoma. Because small foci of adamantinoma may coexist within a lesion that is otherwise indistinguishable from OFD, biopsy requires extensive sampling, and some authorities recommend wide resection for larger lesions to avoid missing a diagnosis of adamantinoma.
Question 100:
A 22-year-old female presents with a bone tumor on the anterior surface of the mid-tibial diaphysis. The surgeon is differentiating between parosteal osteosarcoma and periosteal osteosarcoma. Which of the following characteristics is most strictly associated with periosteal osteosarcoma compared to parosteal osteosarcoma?
Options:
- It is typically a low-grade, predominantly fibro-osseous lesion.
- It is an intermediate-grade lesion with a predominantly chondroblastic matrix.
- It typically occurs on the posterior aspect of the distal femur.
- It has a significantly lower risk of metastasis.
- It is characterized molecularly by consistent MDM2 and CDK4 amplification.
Correct Answer: It is an intermediate-grade lesion with a predominantly chondroblastic matrix.
Explanation:
Periosteal osteosarcoma is an intermediate-grade surface osteosarcoma that typically arises on the anterior surface of the tibial diaphysis and has a predominantly chondroblastic matrix. In contrast, parosteal osteosarcoma is a low-grade surface tumor that typically arises on the posterior aspect of the distal femur metaphysis, has a predominantly fibro-osseous matrix, and is defined by MDM2/CDK4 amplification. Periosteal osteosarcoma has a higher risk of metastasis than parosteal, but lower than conventional intramedullary osteosarcoma.