Orthopedic Board Review MCQs (2026 Edition) - Part 1

Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Orthopedic Board Review MCQs (2026 Edition) - Part 1
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 68-year-old male presents with incapacitating low back pain and significant postural changes. Standing X-rays reveal a severe thoracolumbar kyphoscoliosis with a positive sagittal vertical axis (SVA) of +10 cm and a pelvic incidence (PI) of 60 degrees. The patient has undergone prior L3-S1 fusion. Revision surgery is planned.
Considering modern spinopelvic parameters, what is the MOST critical sagittal parameter to restore for optimal long-term outcomes and pain relief in this patient?

Explanation
Question 2
A 72-year-old patient undergoes revision total knee arthroplasty due to persistent pain and effusion 18 months post-primary surgery. Preoperative workup showed ESR 45 mm/hr, CRP 3.2 mg/dL. Knee aspiration yielded 12,000 WBCs with 85% neutrophils. Intraoperatively, tissue cultures are sent. Synovial fluid for alpha-defensin is also sent, yielding a positive result. Given these findings, what is the MOST appropriate next diagnostic step to confirm or refute a diagnosis of periprosthetic joint infection (PJI)?
Explanation
Question 3
A 35-year-old male sustains a high-energy pelvic injury after a motor vehicle collision, presenting with hemodynamic instability. Initial resuscitation includes two liters of crystalloid and two units of packed red blood cells. A physical exam reveals a shortened and externally rotated left lower extremity. Pelvic X-rays and CT scan demonstrate a Young-Burgess LC-III pattern injury with a symphyseal disruption, bilateral sacral fractures, and evidence of significant retroperitoneal hematoma.
What is the MOST appropriate immediate surgical management strategy?
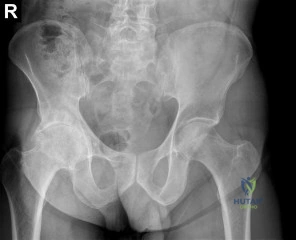
Explanation
Question 4
A 28-year-old professional athlete presents with a symptomatic 2.5 cm full-thickness chondral defect on the femoral condyle following an acute twisting injury. Previous microfracture surgery 6 months ago failed to provide lasting relief. MRI confirms the defect. The patient is keen on returning to high-level sports. Considering advanced biologic augmentation techniques, which option represents the MOST evidence-supported next-step treatment approach for superior hyaline-like cartilage repair in a young, active patient?
Explanation
Question 5
A 12-year-old child with cerebral palsy (GMFCS level V) develops a progressive thoracolumbar scoliosis exceeding 60 degrees, leading to significant sitting imbalance, worsening pain, and recurrent respiratory infections. The patient has severe spasticity and a history of gastric reflux. Surgical correction is planned. What is the MOST critical consideration in the preoperative evaluation and planning for this patient, beyond standard scoliosis workup?
Explanation
Question 6
A 58-year-old female with a history of breast cancer presents with severe, localized pain in her right humerus. X-rays reveal a lytic lesion in the proximal humerus with cortical destruction extending greater than 50%. She is ambulatory but guards her arm significantly. The Mirels' score is calculated to be 10.
What is the MOST appropriate management strategy?
Explanation
Question 7
A 62-year-old diabetic patient presents with a warm, swollen, red, and painful midfoot. Plain radiographs show subtle osteopenia, joint subluxation, and fragmentation of the midfoot bones, consistent with early Charcot neuroarthropathy. There are no skin breaks or signs of infection. What is the MOST critical initial step in management to prevent further progression and deformity?
Explanation
Question 8
A 45-year-old patient develops severe pain, swelling, skin discoloration, and allodynia in her left hand and wrist three weeks after a distal radius fracture. Radiographs show no hardware issues or signs of infection. Nerve conduction studies are normal. Based on the clinical presentation, Complex Regional Pain Syndrome (CRPS) Type I is suspected.
What is the MOST appropriate initial management strategy?

Explanation
Question 9
A 75-year-old female undergoes a reverse total shoulder arthroplasty (RTSA) for rotator cuff tear arthropathy. Six months postoperatively, she presents with persistent shoulder pain, weakness, and a positive 'drop arm' sign. X-rays show no signs of loosening or infection. Physical examination reveals impaired active external rotation. What is the MOST likely cause of her persistent symptoms and functional deficit?
Explanation
Question 10
A 78-year-old patient with a history of recurrent hip dislocations following a primary total hip arthroplasty (THA) is being considered for revision surgery. The patient has significant cognitive impairment and poor compliance with hip precautions. Which of the following bearing surface configurations would provide the BEST stability against future dislocations, while balancing wear characteristics?
Explanation
Question 11
A 28-year-old male sustains a vertically oriented Pauwels type III femoral neck fracture in a motorcycle collision.
Which fixation construct offers the greatest biomechanical stability against shear forces for this specific fracture pattern?
Explanation
Question 12
A 65-year-old female presents with progressive groin pain and a palpable mass 8 years after a metal-on-metal total hip arthroplasty. Aspiration yields sterile, cloudy fluid. MRI demonstrates a solid and cystic periarticular mass. Which of the following histological findings is most characteristic of this condition?
Explanation
Question 13
A 12-year-old obese boy presents with right hip pain and a limp. Radiographs confirm a stable severe right slipped capital femoral epiphysis (SCFE) with a Southwick slip angle of 65 degrees.
What is the strongest primary indication for prophylactic in situ pinning of the contralateral, asymptomatic hip?

Explanation
Question 14
A 15-year-old male presents with a painful mass around his right knee. Radiographs reveal a mixed lytic and sclerotic lesion in the distal femoral metaphysis with a 'sunburst' periosteal reaction. Biopsy confirms high-grade intramedullary osteosarcoma. Which of the following genetic alterations is most frequently associated with the pathogenesis of this tumor?
Explanation
Question 15
A 72-year-old male with degenerative cervical myelopathy is scheduled for a posterior cervical laminectomy and fusion. Preoperatively, he exhibits a modified Japanese Orthopaedic Association (mJOA) score of 12. Which of the following preoperative MRI findings correlates most strongly with a poor neurological recovery following decompression?
Explanation
Question 16
A 21-year-old female soccer player undergoes primary anterior cruciate ligament (ACL) reconstruction using a bone-patellar tendon-bone autograft. Six months postoperatively, she complains of anterior knee pain and a hard block to terminal knee extension at 10 degrees of flexion. What is the most likely surgical etiology of this complication?
Explanation
Question 17
A 12-year-old obese male presents with 3 weeks of left groin pain and a limp. Exam shows obligate external rotation with hip flexion. Radiographs confirm a stable left slipped capital femoral epiphysis (SCFE). Which of the following is the most appropriate absolute indication for prophylactic pinning of the contralateral asymptomatic hip?
Explanation
Question 18
A 6-year-old boy sustains a severe supracondylar humerus fracture resulting in a pink, pulseless hand. Closed reduction and percutaneous pinning are performed expeditiously. Postoperatively, the hand remains pink and capillary refill is less than 2 seconds, but the radial pulse remains completely absent. What is the most appropriate next step in management?
Explanation
Question 19
A 35-year-old male presents with a hypotensive APC-III pelvic ring disruption following a severe crush injury.
Despite initial massive transfusion protocols and appropriate application of a pelvic binder, he remains hemodynamically unstable. What is the most common anatomical source of massive hemorrhage in this specific fracture pattern?

Explanation
Question 20
A 55-year-old male with severe cervical myelopathy due to ossification of the posterior longitudinal ligament (OPLL) from C3-C6 presents for surgical evaluation. MRI and lateral radiographs show a fixed kyphotic alignment. The OPLL mass crosses the K-line (K-line negative). What is the most appropriate surgical strategy?
Explanation
Question 21
A 24-year-old female presents with a slow-growing, painful mass in her foot. MRI demonstrates a soft tissue mass with heterogeneous enhancement. Biopsy reveals a biphasic tumor with both epithelial and spindle cell components. Which of the following chromosomal translocations is highly specific to this diagnosis?
Explanation
Question 22
During a posterior-stabilized total knee arthroplasty, the surgeon notes that the knee is symmetric and stable in extension, but overly tight in flexion, causing the trial femoral component to lift off anteriorly. What is the most appropriate step to balance the knee?
Explanation
Question 23
A 32-year-old male sustains a vertically oriented femoral neck fracture (Pauwels type III). Open reduction and internal fixation is performed. Which of the following fixation constructs provides the greatest biomechanical stability for this specific fracture pattern?
Explanation
Question 24
A 6-year-old child presents with a pulseless, pink hand following a fall from monkey bars. Radiographs show a Garland III posterolaterally displaced supracondylar humerus fracture.
What is the most likely concomitant neurologic deficit?
Explanation
Question 25
A 45-year-old manual laborer presents with chronic dorsal wrist pain. Radiographs reveal advanced radiocarpal arthritis sparing the radiolunate joint, but with proximal migration of the capitate and capitolunate arthritis. He is diagnosed with Scapholunate Advanced Collapse (SLAC) Stage III. What is the most appropriate surgical treatment?
Explanation
Question 26
Denosumab is increasingly used as a targeted medical therapy for the treatment of giant cell tumor of bone. By which specific mechanism does this monoclonal antibody halt tumor progression?
Explanation
Question 27
A 45-year-old male is involved in a severe motor vehicle collision. Pelvic radiographs demonstrate an acetabular fracture with a positive 'gull sign' on the AP view. What does this specific radiographic finding indicate?
Explanation
Question 28
A 62-year-old female presents with persistent groin pain 6 years after a primary total hip arthroplasty using a metal-on-polyethylene bearing. Laboratory tests reveal a serum cobalt level of 12 ppb and a chromium level of 2 ppb. A MARS MRI shows a thick-walled cystic mass communicating with the joint. What is the most likely source of this patient's pathology?
Explanation
Question 29
A 12-year-old boy with a BMI of 32 presents with right knee pain and an obligate external rotation of the hip during passive flexion. Radiographs confirm a severe, stable slipped capital femoral epiphysis (SCFE). Prophylactic pinning of the contralateral, asymptomatic hip is most strongly indicated if the patient has a history of which of the following?
Explanation
Question 30
A 25-year-old athlete sustains a multi-ligament knee injury. Physical examination reveals a negative posterior drawer test but a dial test that shows 20 degrees of increased external rotation at 30 degrees of flexion, which reduces to symmetric rotation at 90 degrees of flexion compared to the uninjured side. Which structure or combination of structures is most likely injured?
Explanation
Question 31
A 60-year-old Asian male presents with progressive bilateral hand dexterity loss and a wide-based gait. Cervical CT demonstrates continuous ossification of the posterior longitudinal ligament (OPLL) from C3 to C6.
The 'K-line' connects the midpoints of the spinal canal at C2 and C7 on a neutral sagittal image. In this patient, the OPLL mass crosses the K-line (K-line negative). What is the surgical implication of this finding?
Explanation
Question 32
A 55-year-old female presents with a sudden inability to actively flex the interphalangeal joint of her right thumb, 8 months after undergoing open reduction and internal fixation of a distal radius fracture with a volar locking plate.
What technical error during the initial surgery most likely caused this complication?

Explanation
Question 33
A 42-year-old female presents with a destructive, lytic lesion in the proximal humerus with cortical breakthrough. Biopsy reveals malignant, pleomorphic spindle cells producing unmineralized osteoid. Which of the following is the most important prognostic factor for overall survival in a patient with this diagnosis without systemic metastasis on initial staging?
Explanation
Question 34
In the manufacturing of ultra-high molecular weight polyethylene (UHMWPE) for total joint arthroplasty, highly cross-linked polyethylene is utilized to reduce volumetric wear. However, the cross-linking process introduces free radicals. Which secondary process is most commonly used to extinguish these free radicals and prevent long-term oxidative degradation?
Explanation
Question 35
A 6-year-old boy sustains a supracondylar humerus fracture with complete posterior displacement. Initially, he has an absent radial pulse but the hand is warm and pink. Closed reduction and percutaneous pinning are performed. Post-reduction, the radial pulse remains non-palpable, but capillary refill in the fingers remains brisk (<2 seconds). What is the most appropriate next step in management?
Explanation
Question 36
A 35-year-old male sustains an isolated, closed, mid-diaphyseal femur fracture. He is optimized and scheduled for an antegrade intramedullary nailing utilizing a trochanteric entry portal. To minimize the risk of a varus malalignment during nail insertion, where should the optimal starting point be located on the AP radiograph?
Explanation
None
