Beyond Winging: Scapulothoracic Arthrodesis for the Scapula Surface
Key Takeaway
Learn more about Beyond Winging: Scapulothoracic Arthrodesis for the Scapula Surface and how to manage it. Scapular winging is a debilitating condition characterized by impaired articulation of the scapula with the rib cage, leading to pain and upper extremity dysfunction. This can result from nerve injuries, muscle weakness, or bony abnormalities affecting the smooth movement of the scapula's surface over the thorax. Treatments vary from soft tissue transfers to scapulothoracic arthrodesis for persistent or severe cases.
Introduction and Epidemiology
Refractory disorders of the scapulothoracic articulation have been reported to result in debilitating pain and profound upper extremity dysfunction that frequently require complex surgical management. The most common clinical presentation, scapular winging, was first reported in the published literature in 1723, and several distinct etiologies for scapular winging have been documented extensively since that time.

Historically, soft tissue operations, such as pectoralis major tendon transfers or Eden-Lange procedures, have demonstrated reported success in stabilizing the dyskinetic scapula in appropriately selected patients. These dynamic transfers aim to restore the force couples necessary for synchronous periscapular motion. Despite successful clinical outcomes in many primary cases, a distinct population of patients experience recurrent symptomatic scapular winging even after technically sound pectoralis major or minor transfers.

Several authors report that scapulothoracic arthrodesis is the definitive treatment of choice for these failed muscle transfers. For failed pectoralis transfer, profound facioscapulohumeral dystrophy, or significant irreducible fixed winging, scapulothoracic arthrodesis serves as a highly successful salvage operation. By rigidly fixing the scapula to the posterior thoracic cage, surgeons can provide a stable fulcrum for the glenohumeral joint, thereby restoring forward elevation and abduction driven by the deltoid and intact rotator cuff musculature, while simultaneously eliminating the painful crepitus and fatigue associated with severe scapulothoracic dyskinesia.
Surgical Anatomy and Biomechanics
The scapula is uniquely positioned over the posterolateral aspect of the rib cage, typically overlying ribs one through seven in the resting anatomic position. It is suspended from the axial skeleton anteriorly by the clavicle via the acromioclavicular and sternoclavicular joints. This complex osseous and ligamentous suspension system plays an indispensable role in positioning the upper extremity in space for proper kinematic function.

The lateral aspect of the scapula includes the glenoid fossa for articulation with the humeral head. The scapula itself provides an attachment for 16 separate muscles, which function synergistically to maintain it in functional positions during dynamic upper extremity tasks. It articulates on the thoracic cavity, allowing for a complex combination of motions including elevation and depression, protraction and retraction, medial and lateral rotation, and anterior and posterior tilting.

A thin, specialized bursal layer separates the anterior concave surface of the scapula from the underlying convex ribs. The primary bursae include the supraserratus bursa, located between the subscapularis and the serratus anterior, and the infraserratus bursa, located between the serratus anterior and the posterolateral chest wall. Hypertrophy or fibrotic changes within these bursal spaces frequently contribute to the pathogenesis of snapping scapula syndrome.

Biomechanically, the scapulothoracic articulation is responsible for approximately one-third of total shoulder elevation. The normal scapulohumeral rhythm dictates a 2 to 1 ratio of glenohumeral to scapulothoracic motion during active arm elevation. When performing a scapulothoracic arthrodesis, this dynamic contribution is intentionally obliterated. Consequently, the patient must rely entirely on the glenohumeral joint for post-operative elevation. A stable, arthrodesed scapula provides a fixed origin for the deltoid and rotator cuff, allowing these muscles to generate maximum torque across the glenohumeral joint.

Pathogenesis and Clinical Evaluation
Dysfunction of the scapulothoracic articulation has been well documented in the peer-reviewed literature, with the most common manifestation being symptomatic scapular winging. Traumatic injuries to the serratus anterior muscle or its innervation, the long thoracic nerve, have been frequently reported to cause symptomatic medial winging. The long thoracic nerve is particularly vulnerable to traction injuries or direct compression due to its long, superficial course along the lateral chest wall.

Atraumatic etiologies also represent a significant portion of scapular dysfunction. Conditions such as neuralgic amyotrophy (Parsonage-Turner syndrome), poliomyelitis, and muscular dystrophies—most notably facioscapulohumeral muscular dystrophy (FSHD)—can produce profoundly disabling scapular winging. In FSHD, progressive fatty infiltration and atrophy of the periscapular musculature lead to a loss of the stabilizing force couples, rendering dynamic tendon transfers ineffective and making arthrodesis the primary surgical indication.

Intolerable winging has also been demonstrated in association with structural bony abnormalities, including rib or scapular osteochondromas, malunited scapular fractures, and highly restrictive soft tissue lesions such as muscle contractures or severe scapulothoracic bursitis. Furthermore, recent literature highlights a significant incidence of scapular winging secondary to primary glenohumeral joint lesions, such as massive rotator cuff tears and multidirectional instability, where the dyskinesia is a compensatory mechanism rather than a primary neurologic deficit.

Patients presenting with scapulothoracic disorders typically complain of debilitating periscapular pain, profound shoulder fatigue, and noticeable cosmetic deformity. Physical examination must focus on the resting posture of the scapula as well as its dynamic position. Both scapulae should be observed and palpated while the arms are actively elevated in the sagittal and coronal planes, and while the patient performs a wall push-up to unmask subtle serratus anterior weakness. Neurologic deficits should be meticulously documented, and electromyography (EMG) is often utilized to confirm the specific pattern of denervation.
Indications and Contraindications
Most patients who present with symptomatic scapular winging, scapulothoracic pain, or crepitus respond to nonoperative measures, including targeted physical therapy focusing on periscapular strengthening, nonsteroidal anti-inflammatory medications, and judicious corticosteroid injections into the scapulothoracic bursa. However, a subset of this patient population experiences complex scapulothoracic dysfunction refractory to all conservative modalities.

The decision to proceed with scapulothoracic arthrodesis requires careful patient selection. The procedure is typically reserved as a salvage operation. Primary indications include progressive muscular dystrophies (such as FSHD) where dynamic transfers are biologically destined to fail due to progressive myopathy. Secondary indications include failed prior dynamic transfers (e.g., failed pectoralis major transfer for long thoracic nerve palsy) and severe, irreducible fixed winging secondary to brachial plexus injuries where no local donor muscles are available.

Contraindications include active infection, severe medical comorbidities precluding prolonged general anesthesia, and poor bone stock (such as severe osteoporosis) that would preclude rigid hardware fixation. A relative contraindication is the absence of a functional glenohumeral joint; because arthrodesis eliminates scapulothoracic motion, the patient must possess an intact rotator cuff and deltoid, as well as a congruent glenohumeral joint, to achieve meaningful post-operative upper extremity elevation.
| Clinical Scenario | Operative Indication for Arthrodesis | Non-Operative / Alternative Management |
|---|---|---|
| Facioscapulohumeral Dystrophy (FSHD) | Severe winging, inability to forward elevate >90°, intact deltoid/cuff | Mild weakness, preserved compensatory motion |
| Long Thoracic Nerve Palsy | Failed prior pectoralis major transfer, fixed irreducible deformity | Observation (up to 18-24 months), Primary dynamic tendon transfer |
| Spinal Accessory Nerve Palsy | Failed Eden-Lange procedure, chronic severe pain | Primary Eden-Lange transfer, targeted physical therapy |
| Snapping Scapula Syndrome | Refractory to all conservative care AND failed arthroscopic bursectomy/resection | Corticosteroid injections, postural rehabilitation |
| Severe Brachial Plexus Injury | Lack of local donor muscles for transfer, need for stable fulcrum | Primary nerve grafting/transfers if identified early |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential for a successful scapulothoracic arthrodesis. Standard radiographic evaluation should include true anteroposterior, scapular Y, and axillary views of the shoulder, as well as dedicated orthogonal views of the scapula and a chest radiograph to assess rib architecture. Advanced imaging, specifically a fine-cut computed tomography (CT) scan with 3D reconstruction, is highly recommended to evaluate the bone stock of the medial scapular border and the underlying ribs, particularly in patients with chronic deformities or prior surgical interventions.

Pulmonary function tests (PFTs) should be considered in patients with underlying respiratory conditions or severe muscular dystrophy, as restricting the mobility of the thoracic cage via arthrodesis can cause a mild but permanent decrease in forced vital capacity (FVC).

Patient positioning is a critical step in the surgical workflow. The patient is typically placed in the prone position on a radiolucent Jackson table with chest rolls to allow for unencumbered thoracic excursion during ventilation. The operative arm must be draped free to allow the surgeon to manipulate the upper extremity and assess the position of the scapula dynamically during the reduction and fixation phases.

Careful padding of all bony prominences is mandatory. The anesthesiologist must be aware of the surgical plan, as the use of muscle relaxants should be minimized during the initial dissection if intraoperative nerve monitoring is utilized, though profound relaxation is often helpful during the reduction of a chronically retracted scapula.
Detailed Surgical Approach and Technique
Incision and Superficial Dissection
The surgical approach begins with a longitudinal parascapular incision placed approximately 2 to 3 centimeters medial to the medial border of the scapula. This incision typically extends from the level of the scapular spine down to the inferior angle.

Subcutaneous flaps are elevated to expose the trapezius muscle. Depending on the remaining muscle bulk (which may be severely atrophic in FSHD), the trapezius is either split in line with its fibers or elevated off the medial border of the scapula. The rhomboid major and minor muscles are subsequently identified and detached from their insertions on the medial scapular border. This provides direct access to the subscapularis muscle on the anterior surface of the scapula.

Preparation of the Fusion Bed
To achieve a robust arthrodesis, meticulous preparation of the osseous fusion beds is required. The subscapularis muscle is elevated subperiosteally off the medial 3 to 4 centimeters of the anterior scapular surface.

Attention is then turned to the thoracic cage. The surgeon must identify the optimal ribs for fixation, which are typically ribs three, four, and five, or ribs four, five, and six, depending on the patient's specific anatomy and the planned resting height of the scapula. The periosteum over the outer cortex of the selected ribs is carefully incised and reflected.

A high-speed spherical burr is utilized to aggressively decorticate the anterior undersurface of the medial scapula and the corresponding outer cortices of the selected ribs until bleeding cancellous bone is encountered. Copious irrigation is utilized to prevent thermal necrosis of the bone. Autologous bone graft, typically harvested from the posterior superior iliac spine (PSIS), or high-quality allograft combined with demineralized bone matrix (DBM), is packed into the decorticated intervals to promote osteogenesis.

Scapular Positioning and Reduction
Determining the precise position for scapular fusion is arguably the most critical step of the procedure, as it directly dictates the patient's postoperative functional range of motion. The consensus in the orthopedic literature recommends positioning the scapula in approximately 15 to 20 degrees of external rotation, 15 to 20 degrees of abduction, and ensuring the medial border is parallel to the spinous processes at a distance of approximately 5 to 7 centimeters from the midline.

The arm should be manipulated intraoperatively to ensure that in this fused position, the patient will have the ability to bring their hand to their mouth (requiring functional forward flexion) and reach their back pocket. Temporary fixation with heavy Kirschner wires or reduction clamps can hold the scapula in this optimal alignment while the permanent fixation constructs are applied.
Fixation Strategies
Historically, fixation was achieved using heavy non-absorbable sutures or stainless steel wires passed through drill holes in the scapula and circumferentially around the ribs. When passing wires or cables around the ribs, the surgeon must stay strictly subperiosteal to avoid injury to the intercostal neurovascular bundle, which runs along the inferior costal groove, and to prevent inadvertent pleural puncture leading to pneumothorax.

Modern techniques increasingly favor the use of multifilament titanium cables or rigid plate fixation. Reconstruction plates can be contoured to bridge the medial border of the scapula directly to the underlying ribs. Plate fixation offers superior biomechanical rigidity compared to wire constructs, potentially decreasing the rate of pseudarthrosis and allowing for earlier mobilization. Regardless of the chosen hardware, the construct must compress the decorticated scapular surface firmly against the decorticated ribs. Following fixation, the detached periscapular musculature is meticulously repaired over the hardware to provide soft tissue coverage and minimize hardware prominence.
Complications and Management
Scapulothoracic arthrodesis is a major structural reconstruction and carries a significant risk profile. Intraoperative complications require immediate recognition and management. The most critical intraoperative risk is pneumothorax resulting from pleural violation during rib exposure or cable passage. A routine postoperative chest radiograph in the post-anesthesia care unit (PACU) is mandatory for all patients undergoing this procedure.

Postoperative complications include hardware failure, pseudarthrosis (nonunion), persistent pain, and pulmonary restriction. Because the scapula is subjected to significant cantilever forces from the weight of the arm, hardware breakage (particularly wire failure) is a known complication if the fusion mass does not consolidate rapidly. Nonunion rates have historically been reported between 10% and 20%, often requiring revision bone grafting and enhanced rigid fixation.

| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Pneumothorax | 5% - 10% | Strict subperiosteal dissection on ribs; use blunt passers. Management: Thoracostomy tube if symptomatic or >20% volume. |
| Pseudarthrosis (Nonunion) | 10% - 20% | Aggressive decortication, generous autograft use, rigid plate/cable fixation. Salvage: Revision arthrodesis with iliac crest graft. |
| Hardware Prominence / Failure | 15% - 25% | Meticulous closure of rhomboids/trapezius over hardware; avoid monofilament wire. Salvage: Hardware removal after solid fusion is confirmed via CT. |
| Pleural Effusion | 5% - 15% | Careful hemostasis. Management: Usually self-limiting; thoracentesis if hemodynamically significant or causing respiratory distress. |
| Intercostal Neuralgia | 5% - 10% | Avoid placing cables directly over the inferior rib border. Management: Gabapentinoids, intercostal nerve blocks, eventual hardware removal. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol following scapulothoracic arthrodesis must balance the need for rigid immobilization to achieve osseous union with the goal of preventing severe glenohumeral adhesive capsulitis.
Immediately postoperatively, the upper extremity is immobilized in a custom abduction orthosis or a rigid sling with an abduction pillow. This immobilization is strictly maintained for 6 to 8 weeks to minimize sheer forces across the scapulothoracic interface. During this initial phase, active and passive range of motion of the elbow, wrist, and hand are encouraged to prevent distal stiffness. Pendulum exercises for the glenohumeral joint may be initiated at 3 to 4 weeks under the strict guidance of a physical therapist, ensuring no active elevation or periscapular muscle contraction occurs.

Radiographic evaluation is typically performed at 6 weeks, 12 weeks, and 6 months postoperatively. Once clinical and radiographic signs of early consolidation are present (usually around 8 weeks), the immobilization device is discontinued, and a progressive active-assisted range of motion program is initiated. Patients must be extensively counseled pre
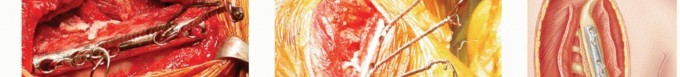
Clinical & Radiographic Imaging

























You Might Also Like
