Orthopedic Basic Review | Dr Hutaif Basic Science Revie -...
14 Apr 2026
152 min read
87 Views

Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Orthopedic Basic Review | Dr Hutaif Basic Sci...
00:00
Start Quiz
Question 1High Yield
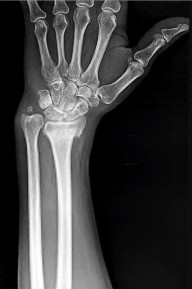
Figures 66a and 66b are the radiographs of a healthy 54-year-old right-hand-dominant man 3 months after he fell onto his outstretched left hand. He was initially treated with 8 weeks of closed reduction and casting. He reports ongoing ulnar-sided wrist pain, stiffness, and diminished function. An examination reveals a clinical sag deformity with a loss of radial length but no substantial swelling. The distal radius is nontender, and rotation is nearly full. Wrist motion is limited, with 55 degrees of flexion, 25 degrees of extension, and full digital motion. The most appropriate treatment is
Explanation
This patient has a substantial nascent malunion of his distal radius. Although a distal ulna excision would likely improve his ulnar-sided wrist pain, the Darrach procedure is more appropriate for older, somewhat less active individuals. In addition, the distal radius malunion is substantial, and it would be preferable to address the malunion given the major loss of radial length, inclination, and increased palmar tilt. The joint surface of the distal radius is uninvolved, and there is no evidence of arthrosis. It is preferable to osteotomize the distal radius sooner rather than later. Delayed osteotomy is often more difficult with more severe soft-tissue contractures, and improved results have been demonstrated following surgical treatment of nascent rather than mature distal radius malunions. Advantages include easier correction, no need for structural bone grafts, less overall total disability, and earlier return to work.
RECOMMENDED READINGS
30. Bilgin SS, Armangil M. Correction of nascent malunion of distal radius fractures. Acta Orthop Traumatol Turc. 2012;46(1):30-4. PubMed PMID: 22441449.
31. Jupiter JB, Ring D. A comparison of early and late reconstruction of malunited fractures of the distal end of the radius. J Bone Joint Surg Am. 1996 May;78(5):739-48. PubMed PMID: 8642031.
RECOMMENDED READINGS
30. Bilgin SS, Armangil M. Correction of nascent malunion of distal radius fractures. Acta Orthop Traumatol Turc. 2012;46(1):30-4. PubMed PMID: 22441449.
31. Jupiter JB, Ring D. A comparison of early and late reconstruction of malunited fractures of the distal end of the radius. J Bone Joint Surg Am. 1996 May;78(5):739-48. PubMed PMID: 8642031.
Question 2High Yield
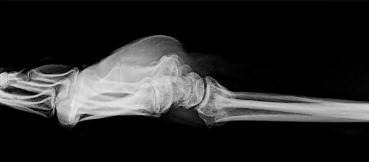
Figure 23 shows the radiograph of an elderly man who fell on his right arm. What is the most important determinate of a good outcome following this injury?
Explanation
Minimally displaced fractures of the proximal humerus have a good outcome if physical therapy is initiated within 2 weeks of the injury. Results are not affected by age, open reduction and internal fixation, or involvement of the greater tuberosity. Immobilization for longer than 3 weeks will often result in stiffness.
REFERENCES: Koval KJ, Gallagher MA, Marsicano JG, et al: Functional outcome after minimally displaced fractures of the proximal part of the humerus. J Bone Joint Surg Am 1997;79:203-207.
Hodgson SA, Mawson SJ, Stanley D: Rehabilitation after two-part fractures of the neck of the humerus. J Bone Joint Surg Br 2003;85:419-422.
REFERENCES: Koval KJ, Gallagher MA, Marsicano JG, et al: Functional outcome after minimally displaced fractures of the proximal part of the humerus. J Bone Joint Surg Am 1997;79:203-207.
Hodgson SA, Mawson SJ, Stanley D: Rehabilitation after two-part fractures of the neck of the humerus. J Bone Joint Surg Br 2003;85:419-422.
Question 3High Yield
Figures 2a through 2h
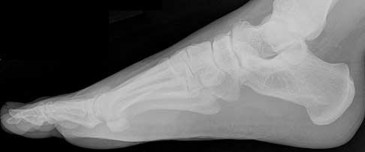
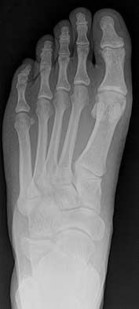
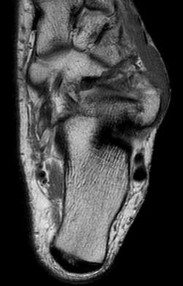
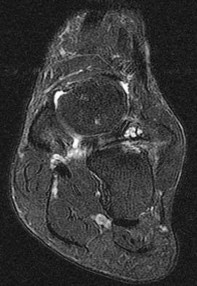
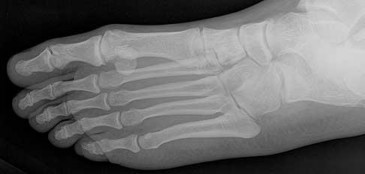
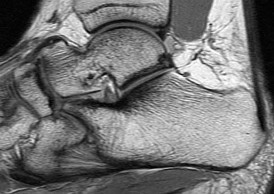
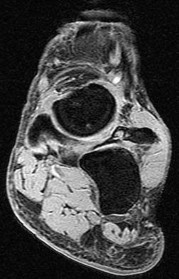
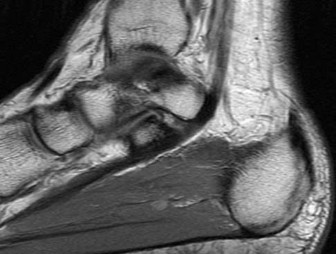
Explanation
- Calcaneonavicular (CN) coalition
Question 4High Yield
All of the following are true statements regarding compartment syndrome in the pediatric patient EXCEPT:
Explanation
Compartment syndrome can often be difficult to diagnosis in the pediatric patient. Mechanism of injury is not the best predictor of compartment syndrome development or diagnosis in pediatric patients. It is important to note that functional outcome following compartment syndrome in patients is inversely related to the duration of elevated tissue pressures before surgical fasciotomy.
Level 4 evidence by Bae et al reviewed 33 children with compartment syndrome. They found that all 10 compartment syndrome patients that had access to nurse or patient controlled analgesia (PCAs), during their initial evaluation, demonstrated an increasing requirement for pain medication.
Matsen et al reviewed 24 children with compartment syndrome with the most common causes being fracture, vascular injury, and tibial osteotomy. The study concluded that is imperative that a compartment syndrome be identified and treated as promptly as possible.
Level 4 evidence by Bae et al reviewed 33 children with compartment syndrome. They found that all 10 compartment syndrome patients that had access to nurse or patient controlled analgesia (PCAs), during their initial evaluation, demonstrated an increasing requirement for pain medication.
Matsen et al reviewed 24 children with compartment syndrome with the most common causes being fracture, vascular injury, and tibial osteotomy. The study concluded that is imperative that a compartment syndrome be identified and treated as promptly as possible.
Question 5High Yield
During the application of halo skeletal fixation, the most appropriate position for the placement of the anterior halo pins is approximately 1 cm above the superior orbital rim and
Explanation
Halo fixation is the most rigid form of cervical orthosis but complications can arise from improper placement of the fixation pins. A relatively safe zone for anterior pin placement is located 1 cm above and within the lateral third of the superior orbital rim. This position avoids the supraorbital and supratrochlear nerves over the medial one third of the orbit. The more lateral positions in the temporal fossa have very thin bone and can interfere with the muscles of mastication.
Question 6High Yield
Which of the following zones of the articular cartilage most likely seals the cartilage off from the immune system:
Explanation
The superficial zone has a number of important characteristics: Thinnest articular cartilage layer
Two layers:
Most superficial – fine collagen fibrils (lamina splendens)
Deep layer – flattened fibroblast-like chondrocytes (parallel to joint surface) Forms a cartilage skin
Important chemical properties:
High collagen and low proteoglycan concentration
Fibronectin and water concentrations are highest in this zone
Great tensile stiffness and strength
Seals off the cartilage from the immune system
Two layers:
Most superficial – fine collagen fibrils (lamina splendens)
Deep layer – flattened fibroblast-like chondrocytes (parallel to joint surface) Forms a cartilage skin
Important chemical properties:
High collagen and low proteoglycan concentration
Fibronectin and water concentrations are highest in this zone
Great tensile stiffness and strength
Seals off the cartilage from the immune system
Question 7High Yield
When compared with postoperative external beam radiation therapy for the treatment of soft-tissue sarcomas, preoperative radiation therapy is associated with which of the following?

Explanation
The next most appropriate step in management is to proceed with a biopsy of the most accessible site. This can be done
by the surgeon or by an interventional radiologist trained in core biopsy techniques. It is imperative to make a pathologic diagnosis prior to proceeding with any further medical, surgical, or radiation treatments. A histologic diagnosis at this point is the only way a medical oncologist can have a meaningful discussion with the patient about their disease, its natural history, and ultimately discuss treatment options and prognosis. Further imaging at this point only delays the time to histologic evaluation. Consideration of surgical stabilization can be delayed until a diagnosis is established and a multidisciplinary approach is initiated. This fracture can be treated at least temporarily with nonsurgical protected weight bearing with a walker or crutches.
Hospice may soon serve a useful role but a diagnosis must first be rendered and a limited life expectancy anticipated. Pre Res # 100 is 2
**MORE MCQS**
[ORTHO MCQS 011 FREE BANK 02](http://hutaifortho.com/878)
---
[ORTHO MCQS 011 FREE BANK](http://hutaifortho.com/877)
[Orthopedic MCQS online Hip and knee ADULT...](http://hutaifortho.com/876)
[ORTHOPEDIC MCQS OB 20 TRAUMA1](http://hutaifortho.com/875)
[ORTHOPEDIC MCQS OB 20 BASIC5](http://hutaifortho.com/874)
[ORTHOPEDIC MCQS OB 20 BASIC7](http://hutaifortho.com/873)
[ORTHOPEDIC MCQS OB 20 BASIC 6](http://hutaifortho.com/872)
[ORTHOPEDIC MCQS OB 20 BASIC 44](http://hutaifortho.com/871)
[ORTHOPEDIC MCQS OB 20 BASIC 4](http://hutaifortho.com/870)
[ORTHOPEDIC MCQS OB 20 BASIC 3](http://hutaifortho.com/869)
[ORTHOPEDIC MCQS OB 20 BASIC 2](http://hutaifortho.com/868)
[ORTHOPEDIC MCQS OB 20 BASIC 1](http://hutaifortho.com/867)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW4](http://hutaifortho.com/865)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW3](http://hutaifortho.com/864)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW 2](http://hutaifortho.com/863)
[1ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW](http://hutaifortho.com/862)
[ORTHOPEDIC MCQS BANK WITH ANSWER HIP 01](http://hutaifortho.com/861)
[ORTHOPEDIC MCQS BANK WITH ANSWER PEDS 01](http://hutaifortho.com/860)
[ORTHOPEDIC MCQS BANK WITH ANSWER SPORT 01](http://hutaifortho.com/859)
[ORTHOPEDIC MCQS BANK WITH
NATOMY 02](http://hutaifortho.com/858)
[ORTHOPEDIC MCQS BANK WITH ANSWER PATHOLOGY 02](http://hutaifortho.com/857)
[ORTHOPEDIC MCQS BANK WITH ANSWER SHOULDER 02](http://hutaifortho.com/856)
[ORTHOPEDIC MCQS WITH ANSWER FOOT 03](http://hutaifortho.com/855)
[ORTHOPEDIC MCQS WITH ANSWER SPINE 03](http://hutaifortho.com/854)
[ORTHOPEDIC MCQS WITH ANSWER TRAUMA 03](http://hutaifortho.com/853)
[ORTHOPEDIC MCQS WITH ANSWER HIP 04](http://hutaifortho.com/852)
[ORTHOPEDIC MCQS WITH ANSWER PEDS 04](http://hutaifortho.com/851)
[ORTHOPEDIC MCQS WITH ANSWER SPORT 04](http://hutaifortho.com/850)
[ORTHOPEDIC MCQS WITH ANSWER ANATOMY 05](http://hutaifortho.com/849)
[ORTHOPEDIC MCQS WITH ANSWER TUMOR/ONCOLOGY 05](http://hutaifortho.com/848)
[ORTHOPEDIC MCQS WITH ANSWER UPPER LIMB 05](http://hutaifortho.com/847)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE SPINE 06](http://hutaifortho.com/846)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE FOOT AND ANKLE...](http://hutaifortho.com/845)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE TRAUMA 06](http://hutaifortho.com/844)
[ORTHOPEDIC MCQS with Answers ONLINE BASIC 06](http://hutaifortho.com/843)
[ORTHOPEDIC MCQS ONLINE PEDIATRICS 07](http://hutaifortho.com/842)
[ORTHOPEDIC MCQS ONLINE HIP AND KNEE RECON 07](http://hutaifortho.com/841)
[ONLINE ORTHOPEDIC MCQS SPORT07](http://hutaifortho.com/840)
[ONLINE ORTHOPEDIC MCQS UPPER LIMB08](http://hutaifortho.com/839)
[ONLINE ORTHOPEDIC MCQS ONCOLOGY/TUMOR08](http://hutaifortho.com/838)
[ONLINE ORTHOPEDIC MCQS ANATOMY08](http://hutaifortho.com/837)
[ONLINE ORTHOPEDIC MCQS FOOT0 9](http://hutaifortho.com/836)
[ONLINE ORTHOPEDIC MCQS SPINE0 9](http://hutaifortho.com/835)
[ONLINE ORTHOPEDIC MCQS TRAUMA 9](http://hutaifortho.com/834)
[Orthopedic MCQS online sports Medicine](http://hutaifortho.com/833)
[Orthopedic MCQS online Shoulder and Elbow](http://hutaifortho.com/832)
[Orthopedic MCQS online Hip and knee](http://hutaifortho.com/831)
[online orthopedic mcqs](http://hutaifortho.com/830)
[Shoulder and elbow: Mcqs AND EMQS Answers](http://hutaifortho.com/766)
[Shoulder And Elbow: Questions Mcqs AND EMQS](http://hutaifortho.com/765)
[Hand and wrist: Answers MCQS EMQS](http://hutaifortho.com/764)
[Hand and wrist: MCQ AND EMQ Questions](http://hutaifortho.com/763)
[quize](http://hutaifortho.com/729)
[KEY POINTS](http://hutaifortho.com/727)
[MIND MAP](http://hutaifortho.com/726)
[action tree](http://hutaifortho.com/725)
[action2](http://hutaifortho.com/724)
[Action](http://hutaifortho.com/723)
[patient](http://hutaifortho.com/722)
[Bop](http://hutaifortho.com/721)
[New](http://hutaifortho.com/720)
[Trial](http://hutaifortho.com/714)
[Pupup](http://hutaifortho.com/713)
[SSEE](http://hutaifortho.com/704)
[SE](http://hutaifortho.com/703)
[2021 SHOULDER AND ELBOW MCQS FREE](http://hutaifortho.com/689)
[Pediatric Orthopaedic MCQS Self-Assessment...](http://hutaifortho.com/685)
[Self-Assessment Examination 2020 Adult Spine MCQS](http://hutaifortho.com/684)
[Foot and Ankle free MCQS2020 Online](http://hutaifortho.com/681)
[UPDATED ORTHOPEDIC MCQS](http://hutaifortho.com/680)
[FREE Orthopedics MCQS 2022 1951.-2000.](http://hutaifortho.com/677)
[FREE Orthopedics MCQS 2022 1901.-1950.](http://hutaifortho.com/676)
[FREE Orthopedics MCQS 2022 1851-1900.](http://hutaifortho.com/675)
[FREE Orthopedics MCQS 2022 1751-1850..](http://hutaifortho.com/674)
[FREE Orthopedics MCQS 2022 1751-1800..](http://hutaifortho.com/673)
[Foot and Ankle FREE ORTHOPEDICS MCQS Question 11](http://hutaifortho.com/672)
[FREE Orthopedics MCQS 2022 1701-1750.](http://hutaifortho.com/668)
[FREE Orthopedics MCQS 2022 1651-1700](http://hutaifortho.com/667)
[FREE Orthopedics MCQS 2022 1601-1650.](http://hutaifortho.com/666)
[ORTHOPEDIC MCQS FREE 2023](http://hutaifortho.com/665)
[FREE Orthopedics MCQS 2022 1551-1600](http://hutaifortho.com/664)
[FREE Orthopedics MCQS 2022 1501-1550](http://hutaifortho.com/663)
[FREE Orthopedics MCQS 2022 1451-1500](http://hutaifortho.com/662)
[FREE Orthopedics MCQS 2022 1401-1450](http://hutaifortho.com/661)
[FREE Orthopedics MCQS 2022 1351 -1400](http://hutaifortho.com/660)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1301-1350](http://hutaifortho.com/659)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1251-1300](http://hutaifortho.com/658)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1151-1200](http://hutaifortho.com/656)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1101 1150](http://hutaifortho.com/655)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ1051-1100](http://hutaifortho.com/654)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ1001-1051](http://hutaifortho.com/653)
[ORTHOPEDICS HYPERGUIDE MCQ 951-1000](http://hutaifortho.com/652)
[ORTHOPEDICS HYPERGUIDE MCQ 901-950](http://hutaifortho.com/651)
[ORTHOPEDICS HYPERGUIDE MCQ 851-900](http://hutaifortho.com/650)
[ORTHOPEDICS HYPERGUIDE MCQ 800-850](http://hutaifortho.com/649)
[ORTHOPEDICS HYPERGUIDE MCQ 751-800](http://hutaifortho.com/647)
[ORTHOPEDICS HYPERGUIDE MCQ 701-750](http://hutaifortho.com/646)
[ORTHOPEDICS HYPERGUIDE MCQ 651-700](http://hutaifortho.com/645)
[ORTHOPEDICS HYPERGUIDE MCQ 601-650](http://hutaifortho.com/644)
[ORTHOPEDICS HYPERGUIDE MCQ 551-600](http://hutaifortho.com/643)
[ORTHOPEDICS HYPERGUIDE MCQ 501-550](http://hutaifortho.com/642)
[ORTHOPEDICS HYPERGUIDE MCQ 451-500](http://hutaifortho.com/641)
[ORTHOPEDICS HYPERGUIDE MCQ 401-450](http://hutaifortho.com/640)
[ORTHOPEDICS HYPERGUIDE MCQ 351-400](http://hutaifortho.com/639)
[ORTHOPEDICS HYPERGUIDE MCQ 301-350](http://hutaifortho.com/638)
[ORTHOPEDICS HYPERGUIDE MCQ 251-300](http://hutaifortho.com/637)
[ORTHOPEDICS HYPERGUIDE MCQ 201-250](http://hutaifortho.com/636)
[ORTHOPEDICS HYPERGUIDE MCQ 151-200](http://hutaifortho.com/635)
[ORTHOPEDICS HYPERGUIDE MCQ 101-150](http://hutaifortho.com/634)
[FREE Orthopedics MCQS 2022 51-100](http://hutaifortho.com/633)
[Orthopedics Hyperguide MCQ 1-50](http://hutaifortho.com/631)
by the surgeon or by an interventional radiologist trained in core biopsy techniques. It is imperative to make a pathologic diagnosis prior to proceeding with any further medical, surgical, or radiation treatments. A histologic diagnosis at this point is the only way a medical oncologist can have a meaningful discussion with the patient about their disease, its natural history, and ultimately discuss treatment options and prognosis. Further imaging at this point only delays the time to histologic evaluation. Consideration of surgical stabilization can be delayed until a diagnosis is established and a multidisciplinary approach is initiated. This fracture can be treated at least temporarily with nonsurgical protected weight bearing with a walker or crutches.
Hospice may soon serve a useful role but a diagnosis must first be rendered and a limited life expectancy anticipated. Pre Res # 100 is 2
**MORE MCQS**
[ORTHO MCQS 011 FREE BANK 02](http://hutaifortho.com/878)
---
[ORTHO MCQS 011 FREE BANK](http://hutaifortho.com/877)
[Orthopedic MCQS online Hip and knee ADULT...](http://hutaifortho.com/876)
[ORTHOPEDIC MCQS OB 20 TRAUMA1](http://hutaifortho.com/875)
[ORTHOPEDIC MCQS OB 20 BASIC5](http://hutaifortho.com/874)
[ORTHOPEDIC MCQS OB 20 BASIC7](http://hutaifortho.com/873)
[ORTHOPEDIC MCQS OB 20 BASIC 6](http://hutaifortho.com/872)
[ORTHOPEDIC MCQS OB 20 BASIC 44](http://hutaifortho.com/871)
[ORTHOPEDIC MCQS OB 20 BASIC 4](http://hutaifortho.com/870)
[ORTHOPEDIC MCQS OB 20 BASIC 3](http://hutaifortho.com/869)
[ORTHOPEDIC MCQS OB 20 BASIC 2](http://hutaifortho.com/868)
[ORTHOPEDIC MCQS OB 20 BASIC 1](http://hutaifortho.com/867)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW4](http://hutaifortho.com/865)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW3](http://hutaifortho.com/864)
[ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW 2](http://hutaifortho.com/863)
[1ORTHOPEDIC MCQS OB 20 SHOULDER AND ELBOW](http://hutaifortho.com/862)
[ORTHOPEDIC MCQS BANK WITH ANSWER HIP 01](http://hutaifortho.com/861)
[ORTHOPEDIC MCQS BANK WITH ANSWER PEDS 01](http://hutaifortho.com/860)
[ORTHOPEDIC MCQS BANK WITH ANSWER SPORT 01](http://hutaifortho.com/859)
[ORTHOPEDIC MCQS BANK WITH
NATOMY 02](http://hutaifortho.com/858)
[ORTHOPEDIC MCQS BANK WITH ANSWER PATHOLOGY 02](http://hutaifortho.com/857)
[ORTHOPEDIC MCQS BANK WITH ANSWER SHOULDER 02](http://hutaifortho.com/856)
[ORTHOPEDIC MCQS WITH ANSWER FOOT 03](http://hutaifortho.com/855)
[ORTHOPEDIC MCQS WITH ANSWER SPINE 03](http://hutaifortho.com/854)
[ORTHOPEDIC MCQS WITH ANSWER TRAUMA 03](http://hutaifortho.com/853)
[ORTHOPEDIC MCQS WITH ANSWER HIP 04](http://hutaifortho.com/852)
[ORTHOPEDIC MCQS WITH ANSWER PEDS 04](http://hutaifortho.com/851)
[ORTHOPEDIC MCQS WITH ANSWER SPORT 04](http://hutaifortho.com/850)
[ORTHOPEDIC MCQS WITH ANSWER ANATOMY 05](http://hutaifortho.com/849)
[ORTHOPEDIC MCQS WITH ANSWER TUMOR/ONCOLOGY 05](http://hutaifortho.com/848)
[ORTHOPEDIC MCQS WITH ANSWER UPPER LIMB 05](http://hutaifortho.com/847)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE SPINE 06](http://hutaifortho.com/846)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE FOOT AND ANKLE...](http://hutaifortho.com/845)
[ORTHOPEDIC MCQS WITH ANSWERS ONLINE TRAUMA 06](http://hutaifortho.com/844)
[ORTHOPEDIC MCQS with Answers ONLINE BASIC 06](http://hutaifortho.com/843)
[ORTHOPEDIC MCQS ONLINE PEDIATRICS 07](http://hutaifortho.com/842)
[ORTHOPEDIC MCQS ONLINE HIP AND KNEE RECON 07](http://hutaifortho.com/841)
[ONLINE ORTHOPEDIC MCQS SPORT07](http://hutaifortho.com/840)
[ONLINE ORTHOPEDIC MCQS UPPER LIMB08](http://hutaifortho.com/839)
[ONLINE ORTHOPEDIC MCQS ONCOLOGY/TUMOR08](http://hutaifortho.com/838)
[ONLINE ORTHOPEDIC MCQS ANATOMY08](http://hutaifortho.com/837)
[ONLINE ORTHOPEDIC MCQS FOOT0 9](http://hutaifortho.com/836)
[ONLINE ORTHOPEDIC MCQS SPINE0 9](http://hutaifortho.com/835)
[ONLINE ORTHOPEDIC MCQS TRAUMA 9](http://hutaifortho.com/834)
[Orthopedic MCQS online sports Medicine](http://hutaifortho.com/833)
[Orthopedic MCQS online Shoulder and Elbow](http://hutaifortho.com/832)
[Orthopedic MCQS online Hip and knee](http://hutaifortho.com/831)
[online orthopedic mcqs](http://hutaifortho.com/830)
[Shoulder and elbow: Mcqs AND EMQS Answers](http://hutaifortho.com/766)
[Shoulder And Elbow: Questions Mcqs AND EMQS](http://hutaifortho.com/765)
[Hand and wrist: Answers MCQS EMQS](http://hutaifortho.com/764)
[Hand and wrist: MCQ AND EMQ Questions](http://hutaifortho.com/763)
[quize](http://hutaifortho.com/729)
[KEY POINTS](http://hutaifortho.com/727)
[MIND MAP](http://hutaifortho.com/726)
[action tree](http://hutaifortho.com/725)
[action2](http://hutaifortho.com/724)
[Action](http://hutaifortho.com/723)
[patient](http://hutaifortho.com/722)
[Bop](http://hutaifortho.com/721)
[New](http://hutaifortho.com/720)
[Trial](http://hutaifortho.com/714)
[Pupup](http://hutaifortho.com/713)
[SSEE](http://hutaifortho.com/704)
[SE](http://hutaifortho.com/703)
[2021 SHOULDER AND ELBOW MCQS FREE](http://hutaifortho.com/689)
[Pediatric Orthopaedic MCQS Self-Assessment...](http://hutaifortho.com/685)
[Self-Assessment Examination 2020 Adult Spine MCQS](http://hutaifortho.com/684)
[Foot and Ankle free MCQS2020 Online](http://hutaifortho.com/681)
[UPDATED ORTHOPEDIC MCQS](http://hutaifortho.com/680)
[FREE Orthopedics MCQS 2022 1951.-2000.](http://hutaifortho.com/677)
[FREE Orthopedics MCQS 2022 1901.-1950.](http://hutaifortho.com/676)
[FREE Orthopedics MCQS 2022 1851-1900.](http://hutaifortho.com/675)
[FREE Orthopedics MCQS 2022 1751-1850..](http://hutaifortho.com/674)
[FREE Orthopedics MCQS 2022 1751-1800..](http://hutaifortho.com/673)
[Foot and Ankle FREE ORTHOPEDICS MCQS Question 11](http://hutaifortho.com/672)
[FREE Orthopedics MCQS 2022 1701-1750.](http://hutaifortho.com/668)
[FREE Orthopedics MCQS 2022 1651-1700](http://hutaifortho.com/667)
[FREE Orthopedics MCQS 2022 1601-1650.](http://hutaifortho.com/666)
[ORTHOPEDIC MCQS FREE 2023](http://hutaifortho.com/665)
[FREE Orthopedics MCQS 2022 1551-1600](http://hutaifortho.com/664)
[FREE Orthopedics MCQS 2022 1501-1550](http://hutaifortho.com/663)
[FREE Orthopedics MCQS 2022 1451-1500](http://hutaifortho.com/662)
[FREE Orthopedics MCQS 2022 1401-1450](http://hutaifortho.com/661)
[FREE Orthopedics MCQS 2022 1351 -1400](http://hutaifortho.com/660)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1301-1350](http://hutaifortho.com/659)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1251-1300](http://hutaifortho.com/658)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1151-1200](http://hutaifortho.com/656)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ-1101 1150](http://hutaifortho.com/655)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ1051-1100](http://hutaifortho.com/654)
[ORTHOPEDICS HYPERGUIDE 2022 MCQ1001-1051](http://hutaifortho.com/653)
[ORTHOPEDICS HYPERGUIDE MCQ 951-1000](http://hutaifortho.com/652)
[ORTHOPEDICS HYPERGUIDE MCQ 901-950](http://hutaifortho.com/651)
[ORTHOPEDICS HYPERGUIDE MCQ 851-900](http://hutaifortho.com/650)
[ORTHOPEDICS HYPERGUIDE MCQ 800-850](http://hutaifortho.com/649)
[ORTHOPEDICS HYPERGUIDE MCQ 751-800](http://hutaifortho.com/647)
[ORTHOPEDICS HYPERGUIDE MCQ 701-750](http://hutaifortho.com/646)
[ORTHOPEDICS HYPERGUIDE MCQ 651-700](http://hutaifortho.com/645)
[ORTHOPEDICS HYPERGUIDE MCQ 601-650](http://hutaifortho.com/644)
[ORTHOPEDICS HYPERGUIDE MCQ 551-600](http://hutaifortho.com/643)
[ORTHOPEDICS HYPERGUIDE MCQ 501-550](http://hutaifortho.com/642)
[ORTHOPEDICS HYPERGUIDE MCQ 451-500](http://hutaifortho.com/641)
[ORTHOPEDICS HYPERGUIDE MCQ 401-450](http://hutaifortho.com/640)
[ORTHOPEDICS HYPERGUIDE MCQ 351-400](http://hutaifortho.com/639)
[ORTHOPEDICS HYPERGUIDE MCQ 301-350](http://hutaifortho.com/638)
[ORTHOPEDICS HYPERGUIDE MCQ 251-300](http://hutaifortho.com/637)
[ORTHOPEDICS HYPERGUIDE MCQ 201-250](http://hutaifortho.com/636)
[ORTHOPEDICS HYPERGUIDE MCQ 151-200](http://hutaifortho.com/635)
[ORTHOPEDICS HYPERGUIDE MCQ 101-150](http://hutaifortho.com/634)
[FREE Orthopedics MCQS 2022 51-100](http://hutaifortho.com/633)
[Orthopedics Hyperguide MCQ 1-50](http://hutaifortho.com/631)
Question 8High Yield
The patient fails nonsurgical treatment. What is the best next step?
Explanation
- CT scan
Question 9High Yield
What is the most common cause of rotator cuff injury in high school athletes?
Explanation
A large number of etiologies of rotator cuff injury have been proposed. Both intrinsic and extrinsic mechanisms have been suggested. In the young athlete the common underlying mechanism is overuse. Contributing factors include increased laxity, anatomic variation in the coracoacromial arch, and altered kinematics.
REFERENCES: Wilkins KE: Shoulder injuries: Epidemiology, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, pp 175-182.
Sher JS: Anatomy, biomechanics, and pathophysiology of rotator cuff disease, in Iannnotti JP, Williams GR (eds): Disorders of the Shoulder: Diagnosis and Management. Philadelphia, PA, Lippincott Williams and Wilkins, 1999, pp 3-30.
REFERENCES: Wilkins KE: Shoulder injuries: Epidemiology, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, pp 175-182.
Sher JS: Anatomy, biomechanics, and pathophysiology of rotator cuff disease, in Iannnotti JP, Williams GR (eds): Disorders of the Shoulder: Diagnosis and Management. Philadelphia, PA, Lippincott Williams and Wilkins, 1999, pp 3-30.
Question 10High Yield
The risk of nerve injury following revision total hip arthroplasty (THA) is approximately:
Explanation
Following primary THA, the incidence of nerve palsy is reported to be approximately 1.3%, but may be as high as 5.2% for primary THA performed for developmental dysplasia or dislocation. For revision surgery, the incidence may be as high as
7.60%
7.60%
Question 11High Yield
A 45-year-old woman has a painless thigh mass that is larger than 5 cm. What is the best next step?
Explanation
Masses exceeding 5 cm in size and any deep mass should be evaluated with MRI prior to biopsy or excision to ensure the most viable tissue is sampled and to minimize morbidity and complications from an improperly placed biopsy site. Examinations are unreliable when attempting to determine if a mass is a simple lipoma, and any large or deep mass should be considered a sarcoma until proven otherwise. PET/CT is a staging examination to evaluate for metastatic or multifocal disease. These are expensive tests that should not be ordered prior to MR imaging of the primary lesion. For patients that are unable to obtain an MRI, CT of the mass is the preferred imaging modality.
RECOMMENDED READINGS
11. [Gilbert NF, Cannon CP, Lin PP, Lewis VO. Soft-tissue sarcoma. J Am Acad Orthop Surg. 2009 Jan;17(1):40-7. Review. PubMed PMID: 19136426.](http://www.ncbi.nlm.nih.gov/pubmed/19136426)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19136426)
12. [Damron TA, Beauchamp CP, Rougraff BT, Ward WG Sr. Soft-tissue lumps and bumps. Instr Course Lect. 2004;53:625-37. Review. PubMed PMID: 15116652.](http://www.ncbi.nlm.nih.gov/pubmed/15116652)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15116652)
13. Simon MA. Diagnostic Strategies. In: Simon MA, Springfield D, eds. _Surgery for Bone and Soft Tissue Tumors_. Philadelphia, PA: Lippincott-Raven; 1998:21-30.
CLINICAL SITUATION FOR QUESTIONS 9 THROUGH 11
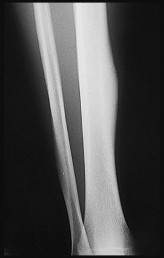
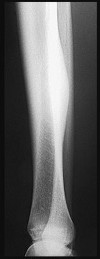
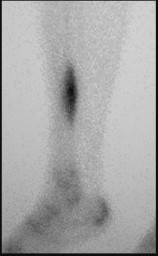
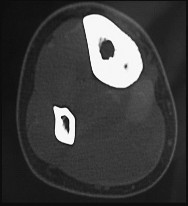
Figures 9a through 9d are the anteroposterior and lateral radiographs, CT scan, and technetium bone scan of a 12-year-old boy who has experienced 7 months of pain in his lower leg. The pain limits his ability to participate in sports and he is having difficulty sleeping. He is afebrile, and laboratory study findings including an erythrocyte sedimentation rate, C-reactive protein, and complete blood count are within normal limits.
RECOMMENDED READINGS
11. [Gilbert NF, Cannon CP, Lin PP, Lewis VO. Soft-tissue sarcoma. J Am Acad Orthop Surg. 2009 Jan;17(1):40-7. Review. PubMed PMID: 19136426.](http://www.ncbi.nlm.nih.gov/pubmed/19136426)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19136426)
12. [Damron TA, Beauchamp CP, Rougraff BT, Ward WG Sr. Soft-tissue lumps and bumps. Instr Course Lect. 2004;53:625-37. Review. PubMed PMID: 15116652.](http://www.ncbi.nlm.nih.gov/pubmed/15116652)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15116652)
13. Simon MA. Diagnostic Strategies. In: Simon MA, Springfield D, eds. _Surgery for Bone and Soft Tissue Tumors_. Philadelphia, PA: Lippincott-Raven; 1998:21-30.
CLINICAL SITUATION FOR QUESTIONS 9 THROUGH 11
Figures 9a through 9d are the anteroposterior and lateral radiographs, CT scan, and technetium bone scan of a 12-year-old boy who has experienced 7 months of pain in his lower leg. The pain limits his ability to participate in sports and he is having difficulty sleeping. He is afebrile, and laboratory study findings including an erythrocyte sedimentation rate, C-reactive protein, and complete blood count are within normal limits.
Question 12High Yield
..Figure 59 is the MRI scan of a 30-year-old fire fighter who dislocated his left shoulder during work activities. His shoulder was reduced in the emergency department. After 8 weeks of physical therapy, he continues to have apprehension when lifting and pushing the fire hose back into the truck. He has normal rotator cuff strength and a negative sulcus sign. What treatment option will allow this patient to return to work as soon as possible?
Explanation
- Posterior labral repair
CLINICAL SITUATION FOR QUESTIONS 60 AND 61
A 10-year-old left-hand-dominant baseball pitcher has had left elbow pain for 6 weeks. His pain primarily is located medially, and he states that it is worst during the late cocking/early acceleration phase of his pitch. Recently he noticed that he is not able to throw as fast as usual. He decreased his pitch count by half during the last 2 weeks without significant improvement in his symptoms. When he is not pitching, he does not have significant pain. Radiographs show widening of the medial epicondyle physis.
CLINICAL SITUATION FOR QUESTIONS 60 AND 61
A 10-year-old left-hand-dominant baseball pitcher has had left elbow pain for 6 weeks. His pain primarily is located medially, and he states that it is worst during the late cocking/early acceleration phase of his pitch. Recently he noticed that he is not able to throw as fast as usual. He decreased his pitch count by half during the last 2 weeks without significant improvement in his symptoms. When he is not pitching, he does not have significant pain. Radiographs show widening of the medial epicondyle physis.
Question 13High Yield
A 10-year-old girl has a midshaft both bone forearm fracture. After attempted closed reduction, alignment consists of bayonet apposition, 10° of malrotation, and 8° of volar angulation. Management should now consist of
Explanation
Acceptable alignment in both bone forearm fractures is related to age and location. In children younger than age 9 years, angulations of 15° and malrotation of 45° are acceptable. In children older than age 9 years, acceptable alignment is 10° of angulation and 30° of malrotation. Bayonet apposition is acceptable provided that the angular and rotational reductions are held within these guidelines. A long arm cast provides better control of deforming forces than a short arm cast.
REFERENCES: Do TT, Strub WM, Foad SL, et al: Reduction versus remodeling in pediatric distal forearm fractures: A preliminary cost analysis. J Pediatr Orthop B 2003;12:109-115.
Flynn JM: Pediatric forearm fractures: Decision making, surgical techniques, and complications. Instr Course Lect 2002;51:355-360.
Ring D, Waters PM, Hotchkiss RN, et al: Pediatric floating elbow. J Pediatr Orthop 2001;21:456-459.
Noonan KJ, Price CT: Forearm and distal radius fractures in children. J Am Acad Orthop Surg 1998;6:146-156.
REFERENCES: Do TT, Strub WM, Foad SL, et al: Reduction versus remodeling in pediatric distal forearm fractures: A preliminary cost analysis. J Pediatr Orthop B 2003;12:109-115.
Flynn JM: Pediatric forearm fractures: Decision making, surgical techniques, and complications. Instr Course Lect 2002;51:355-360.
Ring D, Waters PM, Hotchkiss RN, et al: Pediatric floating elbow. J Pediatr Orthop 2001;21:456-459.
Noonan KJ, Price CT: Forearm and distal radius fractures in children. J Am Acad Orthop Surg 1998;6:146-156.
Question 14High Yield
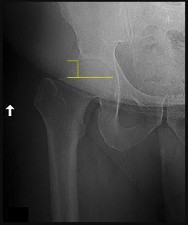
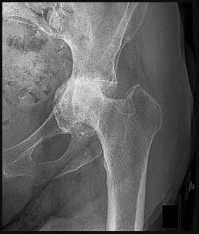
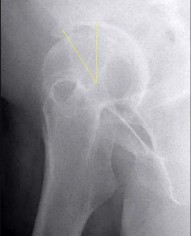
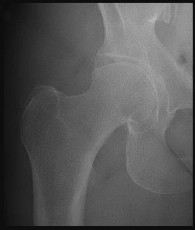
A 46-year-old male construction worker has right hip pain that has failed to respond to nonsurgical management. His body mass index (BMI) is 32, he is 6’2” tall, and he has no other medical comorbidities. AP and lateral radiographs of the right hip are shown in Figures 23a and 23b. The patient inquires about his suitability for metal-on-metal hip resurfacing. The patient should be educated that he is at higher risk for failure secondary to which of the following?
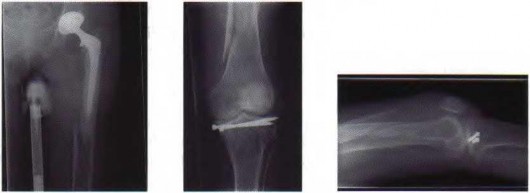
Explanation
This young patient has osteonecrosis of the femoral head with a large area of collapse.
The results of hip resurfacing arthroplasty have been reported to be best in young, male patients who are younger than 55 years of age with a diagnosis of osteoarthritis. Although some authors advocate metal- on-metal hip resurfacing as an option for patients with osteonecrosis of the femoral head, in this particular patient, given the size of the necrotic segment, he would be at higher risk for failure and a conventional total hip arthroplasty would be a more conservative option. As the acetabulum is resurfaced in metal- on-metal hip resurfacing, the secondary changes of the acetabulum are not an issue and his BMI is in an acceptable range for the procedure.
REFERENCES: Mont MA, Ragland PS, Etienne G, et al: Hip resurfacing arthroplasty. J Am Acad Orthop Surg 2006;14:454-463.
Revell MP, McBryde CW, Bhatnagar S, et al: Metal-on-metal hip resurfacing in osteonecrosis of the femoral head. J Bone Joint Surg Am 2006;88:98-103.
Buergi ML, Walter WL: Hip resurfacing arthroplasty: The Australian experience. J Arthroplasty 2007;22:61-65. Question 24
A 31-year-old woman had disabling right knee pain. An arthroscopic assessment reveals chondromalacia of both the lateral femoral condyle and tibial plateau. The standing femorotibial axis measures 10 degrees of valgus. The
optimum treatment of this condition should include
1. distal femoral varus osteotomy.
2. osteoarticular transplant to the lateral femoral condyle.
3. unicondylar arthroplasty.
4. high tibial osteotomy.
5. Fulkerson tibial tubercle transfer. PREFERRED RESPONSE: 1
DISCUSSION: The long-term outcome of a distal femoral varus osteotomy has been quite favorable and should remain the primary choice for this young active woman. Sharma and associates have shown that a 5-degree valgus malalignment has a five-fold chance of progressing at least one grade within 18 months, making a corrective osteotomy the most important surgical maneuver.
REFERENCES: Sharma L, Song J, Felson DT, et al: The role of knee alignment in disease progression and function decline in knee osteoarthritis. JAMA 2001 ;286:188-195.
Murray PB, Rand JA: Symptomatic valgus knee: The surgical options. J Am Acad Orthop Surg 1993; 1:19.
Figure 25a Figure 25b Figure 25c
The results of hip resurfacing arthroplasty have been reported to be best in young, male patients who are younger than 55 years of age with a diagnosis of osteoarthritis. Although some authors advocate metal- on-metal hip resurfacing as an option for patients with osteonecrosis of the femoral head, in this particular patient, given the size of the necrotic segment, he would be at higher risk for failure and a conventional total hip arthroplasty would be a more conservative option. As the acetabulum is resurfaced in metal- on-metal hip resurfacing, the secondary changes of the acetabulum are not an issue and his BMI is in an acceptable range for the procedure.
REFERENCES: Mont MA, Ragland PS, Etienne G, et al: Hip resurfacing arthroplasty. J Am Acad Orthop Surg 2006;14:454-463.
Revell MP, McBryde CW, Bhatnagar S, et al: Metal-on-metal hip resurfacing in osteonecrosis of the femoral head. J Bone Joint Surg Am 2006;88:98-103.
Buergi ML, Walter WL: Hip resurfacing arthroplasty: The Australian experience. J Arthroplasty 2007;22:61-65. Question 24
A 31-year-old woman had disabling right knee pain. An arthroscopic assessment reveals chondromalacia of both the lateral femoral condyle and tibial plateau. The standing femorotibial axis measures 10 degrees of valgus. The
optimum treatment of this condition should include
1. distal femoral varus osteotomy.
2. osteoarticular transplant to the lateral femoral condyle.
3. unicondylar arthroplasty.
4. high tibial osteotomy.
5. Fulkerson tibial tubercle transfer. PREFERRED RESPONSE: 1
DISCUSSION: The long-term outcome of a distal femoral varus osteotomy has been quite favorable and should remain the primary choice for this young active woman. Sharma and associates have shown that a 5-degree valgus malalignment has a five-fold chance of progressing at least one grade within 18 months, making a corrective osteotomy the most important surgical maneuver.
REFERENCES: Sharma L, Song J, Felson DT, et al: The role of knee alignment in disease progression and function decline in knee osteoarthritis. JAMA 2001 ;286:188-195.
Murray PB, Rand JA: Symptomatic valgus knee: The surgical options. J Am Acad Orthop Surg 1993; 1:19.
Figure 25a Figure 25b Figure 25c
Question 15High Yield
In patients undergoing elective hip or knee arthroplasty who are not at elevated risk (beyond the risk associated
with the surgery) for venous thromboembolism or bleeding, using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism was assigned what grade of recommendation by the 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty?
with the surgery) for venous thromboembolism or bleeding, using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism was assigned what grade of recommendation by the 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty?
Explanation
Using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism in patients undergoing elective hip or knee arthroplasty who are not at elevated risk beyond that of the surgery itself for venous thromboembolism or bleeding was given a moderate grade of
recommendation in the 2011 AAOS Clinical Practice Guideline referenced above.
recommendation in the 2011 AAOS Clinical Practice Guideline referenced above.
Question 16High Yield
Which of the following describes galvanic corrosion:
Explanation
Galvanic corrosion is caused by an electrochemical potential that is created between two metals that are located in a conductive environment, such as body fluids.
Examples of galvanic corrosion include: Screw heads and a plate
Femoral head screw and barrel of a dynamic hip screw
Interlocking screws and an intramedullary nail
Galvanic corrosion can also occur within a metal if there are impurities (intergranular corrosion).
The other responses refer to:
Fretting corrosion: Between the femoral head and tapered neck
C revice corrosion: Screw head and countersunk region of the acetabular component
Oxidative degradation: Delamination of high-density polyethylene
Oxidative degradation: Irradiation of high-density polytheylene in an ambient environment
C orrect Answer: At the interface between a plate and the screw heads
Examples of galvanic corrosion include: Screw heads and a plate
Femoral head screw and barrel of a dynamic hip screw
Interlocking screws and an intramedullary nail
Galvanic corrosion can also occur within a metal if there are impurities (intergranular corrosion).
The other responses refer to:
Fretting corrosion: Between the femoral head and tapered neck
C revice corrosion: Screw head and countersunk region of the acetabular component
Oxidative degradation: Delamination of high-density polyethylene
Oxidative degradation: Irradiation of high-density polytheylene in an ambient environment
C orrect Answer: At the interface between a plate and the screw heads
Question 17High Yield
Figures below depict the radiographs obtained from a 76-year-old woman with a painful total knee
arthroplasty. She describes an uneventful recovery with no wound-healing issues and was pain free for the first 10 years. Although reporting no trauma or inciting event, she now describes pain in the entire knee that is most severe with her first few steps. She has begun to notice night pain and, more recently, constant swelling. What is the most appropriate work-up at this time?
arthroplasty. She describes an uneventful recovery with no wound-healing issues and was pain free for the first 10 years. Although reporting no trauma or inciting event, she now describes pain in the entire knee that is most severe with her first few steps. She has begun to notice night pain and, more recently, constant swelling. What is the most appropriate work-up at this time?

Explanation
An evaluation of the painful total knee must be supported by an understanding of the potential etiologies of pain. They may include, aseptic loosening, infection, osteolysis, gap imbalance, referred pain, stiffness, and complex regional pain syndrome. In this case, the patient demonstrates start-up pain and had no prior history of infections. Her radiographs show subsidence of the tibia, indicating a loose prosthesis. Knowing that the prosthesis is already loose precludes the need for a bone scan. It is, however, important to rule out infection in this case; therefore, CRP and ESR testing is essential. Aspiration is also recommended when going into knee arthroplasty, and infection is a concern.
Question 18High Yield
Which of the following statements best describes labral tears in the hip?
Explanation
DISCUSSION: Labral and chondral lesions are observed within the anterosuperior quadrant of the acetabulum. Tearing of the labrum markedly reduces resistance to joint motion, leading to instability.
The most common associated lesions are chondral injuries. They can occur with or without abnormal bone morphology. The etiology for labral tears can be from traumatic and degenerative causes, structural abnormalities from femoroacetabular impingement, developmental abnormalities, and hip instability.
REFERENCES: Beck M, Kalhor M, Leunig M, et al: Hip morphology influences the pattern of damage to the acetabular cartilage: Femoroacetabular impingement as a cause of early osteoarthritis of the hip. J Bone Joint Surg Br 2005;87:1012-1018.
Ito K, Leunig M, Ganz R: Histopathologic features of the acetabular labrum in femoroacetabular impingement. Clin Orthop Relat Res 2004;429:262-271.
Crawford MJ, Dy CJ, Alexander JW, et al: The 2007 Frank Stinchfield Award. The biomechanics of the hip labrum and the stability of the hip. Clin Orthop Relat Res 2007;465:16-22.
DISCUSSION: Labral and chondral lesions are observed within the anterosuperior quadrant of the acetabulum. Tearing of the labrum markedly reduces resistance to joint motion, leading to instability.
The most common associated lesions are chondral injuries. They can occur with or without abnormal bone morphology. The etiology for labral tears can be from traumatic and degenerative causes, structural abnormalities from femoroacetabular impingement, developmental abnormalities, and hip instability.
REFERENCES: Beck M, Kalhor M, Leunig M, et al: Hip morphology influences the pattern of damage to the acetabular cartilage: Femoroacetabular impingement as a cause of early osteoarthritis of the hip. J Bone Joint Surg Br 2005;87:1012-1018.
Ito K, Leunig M, Ganz R: Histopathologic features of the acetabular labrum in femoroacetabular impingement. Clin Orthop Relat Res 2004;429:262-271.
Crawford MJ, Dy CJ, Alexander JW, et al: The 2007 Frank Stinchfield Award. The biomechanics of the hip labrum and the stability of the hip. Clin Orthop Relat Res 2007;465:16-22.
Question 19High Yield
Advantages of plain film radiograph in diagnosis and treatment of femoral acetabular impingement do NOT include:
Explanation
Plain film radiographs can successfully detect cam and pincer impingement and cartilage space narrowing, as well as allow quantified measurement of femoral head coverage. A magnetiCresonance arthrogram is necessary, however, to successfully visualize labral pathology.
Question 20High Yield
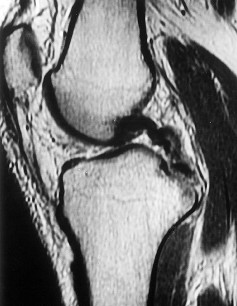
A 57-year-old man has had a 2-week history of neck pain. He has no history of radiating symptoms, and has no complaints of numbness or paresthesias. There was no trauma associated with the onset of the pain. Figure 1 shows the MRI scan initially obtained by his family physician. What should the patient be told regarding the prevalence of the MRI findings in his age group?

Explanation
■
The MRI findings reveal age-related degenerative changes in the cervical spine, which is a very common finding in the adult population. Boden and associates evaluated cervical spine MRI findings on 63 asymptomatic subjects and found that the prevalence of having at least one degenerative disk was approximately 57% in those older than age 40 years.
The MRI findings reveal age-related degenerative changes in the cervical spine, which is a very common finding in the adult population. Boden and associates evaluated cervical spine MRI findings on 63 asymptomatic subjects and found that the prevalence of having at least one degenerative disk was approximately 57% in those older than age 40 years.
Question 21High Yield
Figure 50 is the radiograph of a 19-year-old woman who injured her left knee while playing soccer 4 days ago. She was cutting to her right, was tackled on the inside of her left knee, and felt a pop. She has no history of prior injury to her knee. Which structure attaches at the site of the avulsion fracture?
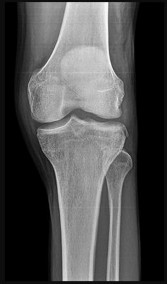
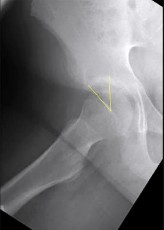
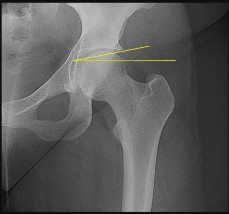
Explanation
The knee ALL is a fibrous band at the anterolateral aspect of the knee. It first was reported by Segond and also is known as the lateral capsular ligament, mid-third lateral capsular ligament, and anterior band of the lateral collateral ligament. It is thought to be injured with varus and internal rotation. It is associated with a torn anterior cruciate ligament 75% of the time and it is located in the third layer on the anterolateral side of the knee. It is 90% collagen I, with some collagen III and VI. The ALL originates at the lateral epicondyle between the lateral collateral ligament and popliteal tendon. It runs obliquely down and forward, inserting in the lateral meniscus and lateral aspect of the proximal tibia. Its role in rotational stability is debated but certainly worthy of consideration, especially in revision knee surgery.
The iliotibial band inserts on Gerdy’s tubercle. A portion of the ALL may insert on the lateral meniscus; however, a lateral meniscus tear is not directly associated with avulsion fractures. The fibular collateral ligament inserts on the fibular head.
RECOMMENDED READINGS
14. Macchi V, Porzionato A, Morra A, Stecco C, Tortorella C, Menegolo M, Grignon B, De Caro R. The anterolateral ligament of the knee: a radiologic and histotopographic study. Surg Radiol Anat. 2015 Oct
[17/. [Epub ahead of print] PubMed PMID: 26476833.](http://www.ncbi.nlm.nih.gov/pubmed/26476833)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26476833)
15. Kennedy MI, Claes S, Fuso FA, Williams BT, Goldsmith MT, Turnbull TL, Wijdicks CA, LaPrade RF. The Anterolateral Ligament: An Anatomic, Radiographic, and Biomechanical Analysis. Am J Sports Med. 2015 Jul;43(7):1606-15. doi: 10.1177/0363546515578253. Epub 2015 Apr 17. PubMed
[PMID: 25888590. ](http://www.ncbi.nlm.nih.gov/pubmed/25888590)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25888590)
RESPONSES FOR QUESTIONS 51 THROUGH 57
Figure 51 a- h
a b c
h
d
e
f
g
The iliotibial band inserts on Gerdy’s tubercle. A portion of the ALL may insert on the lateral meniscus; however, a lateral meniscus tear is not directly associated with avulsion fractures. The fibular collateral ligament inserts on the fibular head.
RECOMMENDED READINGS
14. Macchi V, Porzionato A, Morra A, Stecco C, Tortorella C, Menegolo M, Grignon B, De Caro R. The anterolateral ligament of the knee: a radiologic and histotopographic study. Surg Radiol Anat. 2015 Oct
[17/. [Epub ahead of print] PubMed PMID: 26476833.](http://www.ncbi.nlm.nih.gov/pubmed/26476833)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/26476833)
15. Kennedy MI, Claes S, Fuso FA, Williams BT, Goldsmith MT, Turnbull TL, Wijdicks CA, LaPrade RF. The Anterolateral Ligament: An Anatomic, Radiographic, and Biomechanical Analysis. Am J Sports Med. 2015 Jul;43(7):1606-15. doi: 10.1177/0363546515578253. Epub 2015 Apr 17. PubMed
[PMID: 25888590. ](http://www.ncbi.nlm.nih.gov/pubmed/25888590)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25888590)
RESPONSES FOR QUESTIONS 51 THROUGH 57
Figure 51 a- h
a b c
h
d
e
f
g
Question 22High Yield
A 47-year-old man has left-sided motor weakness in the extensor digitorum longus and extensor hallucis longus, sensory loss in the lateral calf and dorsal foot, and no discernible reflex loss.
Explanation
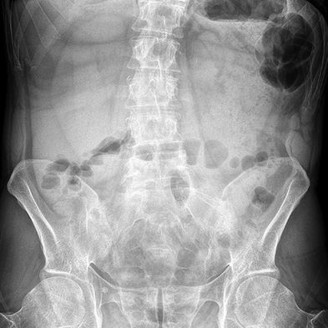
Figures 72a and 72b are the T1-weighted MR images of a disk bulge. Disk bulges are common in asymptomatic people and are not predictive of pathology. Figures 72c and 72d show T1 MR images of a far lateral disk herniation at the L4-L5 level. This would affect the exiting or L4 nerve root. Radicular symptoms would occur at the L4 level. Figures 72e and 72f show an annular tear at the L4-L5 level. This pathology is associated with discogenic low-back pain. Figures 72g and 72h show the T1 MR images of a central lateral disk herniation at the L4-L5 level. This would affect the traversing or L5 nerve root. Radicular symptoms would occur at the L5 level.
RECOMMENDED READINGS
1. [View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15990670)
2. Hoppenfeld S. Physical Exam of the Spine and Extremities. Stamford, CT: Appleton and Lange; 1995.
3. [Madigan L, Vaccaro AR, Spector LR, Milam RA. Management of symptomatic lumbar degenerative disk disease. J Am Acad Orthop Surg. 2009 Feb;17(2):102-11. Review. PubMed PMID: 19202123.](http://www.ncbi.nlm.nih.gov/pubmed/19202123)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19202123)
68
RESPONSES FOR QUESTIONS 76 THROUGH 82
For each MR image above, match the correct structure. The structure is labeled with a yellow dot.
RECOMMENDED READINGS
1. [View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15990670)
2. Hoppenfeld S. Physical Exam of the Spine and Extremities. Stamford, CT: Appleton and Lange; 1995.
3. [Madigan L, Vaccaro AR, Spector LR, Milam RA. Management of symptomatic lumbar degenerative disk disease. J Am Acad Orthop Surg. 2009 Feb;17(2):102-11. Review. PubMed PMID: 19202123.](http://www.ncbi.nlm.nih.gov/pubmed/19202123)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/19202123)
68
RESPONSES FOR QUESTIONS 76 THROUGH 82
For each MR image above, match the correct structure. The structure is labeled with a yellow dot.
Question 23High Yield
A 40-year-old man who is a manual laborer has had 3 years of worsening medial-sided left knee pain that has inhibited his ability to work. He reports undergoing a left subtotal medial meniscectomy 10 years ago. He has been treated with nonsteroidal anti-inflammatory drugs and two different corticosteroids, with the most recent injection given 1 month ago. Each injection provided him with a few weeks of pain control. His medical history is unremarkable, and he has smoked 20 cigarettes per day for the last 15 years. His BMI is 22. On examination, he has varus alignment of the involved leg and medial joint line tenderness and no lateral or patellofemoral pain. His knee range of motion is 3° shy of full extension to 130° of flexion. He has negative Lachman and posterior drawer test results. He demonstrates no lateral thrust with ambulation. The patient is offered a VPHTO. What aspect of his history will determine the most appropriate VPHTO technique?
Explanation
This patient has a classic presentation of postmeniscectomy medial compartment arthritis. The appropriate diagnostic study is weight-bearing radiographs to confirm the diagnosis. An MRI scan will reveal medial compartment arthritis but will not provide information about alignment. A CT scan would be appropriate to detect an occult fracture; however, this condition is not suspected in this clinical scenario. Ultrasonography can provide information about fluid collection around the knee or a deep vein thrombosis; however, these conditions also are not suspected in this clinical scenario. Because the patient has a correctable deformity (gaps 3 mm with valgus stress), and his symptoms are localized to the involved
compartment, a trial of a medial unloader brace is appropriate both diagnostically and therapeutically. If unloading the medial compartment resolves the patient’s symptoms, he would be an excellent candidate for an osteotomy. An MRI scan may be obtained to evaluate ligamentous integrity or to evaluate degenerative involvement of the lateral and patellofemoral compartment for presurgical planning of an osteotomy; however, the integrity of the medial meniscus has no clinical importance in a patient with severe medial compartment arthritis. A repeat corticosteroid injection is not indicated within 1 month of his last injection, and referral to pain management is not appropriate with other options available to help this patient. A VPHTO is the appropriate intervention considering the patient’s young age, high-functional occupation, examination, radiographic findings, and response to medial unloader bracing. A revision knee arthroscopy would be appropriate for a recurrent medial meniscus tear, but not appropriate in a patient with severe medial compartment arthritis. The patient’s young age and high functional requirements are contraindications to TKA. The presence of severe arthritis is a contraindication to medial meniscus transplant. The patient is a candidate for a VPHTO. The technical options include a medial opening-wedge or a lateral closing-wedge osteotomy. Both techniques have advantages and disadvantages; however, a medial opening-wedge osteotomy is contraindicated in a smoker because of concern for nonunion. As a result, current smoking history is the only factor listed that would influence the technique used. The history of prior arthroscopy has no relevance in the decision about which type of osteotomy is appropriate. Normal BMI is between 18.5 and 24.9, so this patient’s BMI is considered normal and would not affect the surgical technique (if this patient were obese, a lateral closing-wedge osteotomy would be considered, but this is controversial). His age of 40 years is an indication for HTO _but does not influence technique._
compartment, a trial of a medial unloader brace is appropriate both diagnostically and therapeutically. If unloading the medial compartment resolves the patient’s symptoms, he would be an excellent candidate for an osteotomy. An MRI scan may be obtained to evaluate ligamentous integrity or to evaluate degenerative involvement of the lateral and patellofemoral compartment for presurgical planning of an osteotomy; however, the integrity of the medial meniscus has no clinical importance in a patient with severe medial compartment arthritis. A repeat corticosteroid injection is not indicated within 1 month of his last injection, and referral to pain management is not appropriate with other options available to help this patient. A VPHTO is the appropriate intervention considering the patient’s young age, high-functional occupation, examination, radiographic findings, and response to medial unloader bracing. A revision knee arthroscopy would be appropriate for a recurrent medial meniscus tear, but not appropriate in a patient with severe medial compartment arthritis. The patient’s young age and high functional requirements are contraindications to TKA. The presence of severe arthritis is a contraindication to medial meniscus transplant. The patient is a candidate for a VPHTO. The technical options include a medial opening-wedge or a lateral closing-wedge osteotomy. Both techniques have advantages and disadvantages; however, a medial opening-wedge osteotomy is contraindicated in a smoker because of concern for nonunion. As a result, current smoking history is the only factor listed that would influence the technique used. The history of prior arthroscopy has no relevance in the decision about which type of osteotomy is appropriate. Normal BMI is between 18.5 and 24.9, so this patient’s BMI is considered normal and would not affect the surgical technique (if this patient were obese, a lateral closing-wedge osteotomy would be considered, but this is controversial). His age of 40 years is an indication for HTO _but does not influence technique._
Question 24High Yield
The patient ultimately undergoes rotationplasty. What is the most likely etiology of early limb loss after rotationplasty for sarcoma?
Explanation
- Vascular compromise_
Question 25High Yield
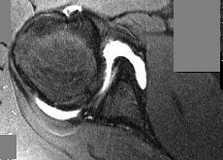
Figure 1 is the T2 axial MRI scan of a 21-year-old man who was injured while playing for his college football team. His pain was aggravated with blocking maneuvers and alleviated with rest, and he had to stop playing because of the pain. What examination maneuver most likely will reproduce his pain?
---
---
Explanation
This patient has a mechanism of injury and MRI scan consistent with a posterior labral tear and posterior instability. Flexion, adduction, and internal rotation produce a net posterior vector on the glenohumeral joint and should reproduce this patient's symptoms. Pain or instability with the arm elevated in the scapular plane describes an impingement sign. Pain or instability with the arm in external rotation and abduction describes the apprehension sign. Pain or instability with the arm in flexion and abduction is a _nonspecific finding._
Question 26High Yield
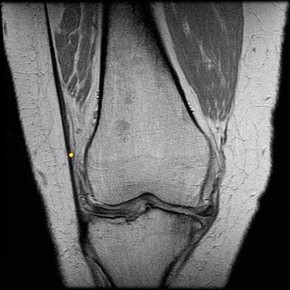
Figure 1 is the MR image of a 36-year-old athlete who is tackled from behind and falls forward onto his left knee. He has pain, swelling, and stiffness. Examination includes a moderate effusion, positive quadriceps active test, and normal Lachman test finding. Risk for vascular injury during transtibial drilling for reconstruction of this injury is increased by
---
---
Explanation
The clinical description and MR image point to an injury to the posterior cruciate ligament (PCL). This ligament is thought to be primarily composed of anterolateral and posteromedial bundles, with the former tightening in flexion and the latter in extension. Because of alterations in knee kinematics and increased varus alignment in PCL insufficiency, contact stresses and cartilage loads increase in the patellofemoral and medial compartments. Although good outcomes may be obtained with transtibial, open inlay, and arthroscopic inlay techniques, one major difference is the creation of the “killer-turn” during the transtibial approach. This sharp turn in the graft as it emerges from the tibia appears to lead to more pronounced attenuation and thinning of the graft during cyclic loading. The scenario describes a patient with chronic PCL and posterolateral corner (PLC) injury, as evidenced by the varus thrust and abnormal Dial test finding. A valgus-producing osteotomy may be effective, and, in fact, may be the only treatment necessary to address chronic PLC injury. Accordingly, an opening lateral osteotomy would not be appropriate. Of the remaining responses, an osteotomy that increases tibial slope would also address the PCL deficiency by reducing posterior tibial sag. Vascular injury is an uncommon, but potentially devastating, complication associated with PCL surgery and may occur regardless of the technique used. Numerous strategies have been described to reduce the risk, including use of a posteromedial accessory incision to allow finger retraction of the popliteal neurovascular bundle, oscillating drills to prevent excessive soft-tissue entanglement, and tapered (rather than square) drill bits that may minimize cut-out of sharp edges as drilling reaches the posterior tibial cortex. Knee extension lessens, rather than increases,
the distance between the posterior tibia and the neurovascular bundle and increases, not lessens, risk for _vascular injury._
the distance between the posterior tibia and the neurovascular bundle and increases, not lessens, risk for _vascular injury._
Question 27High Yield
A 45-year-old man sustained the injury shown in Figures 36a and 36b. The involved side is his dominantside. What is the most appropriate management?
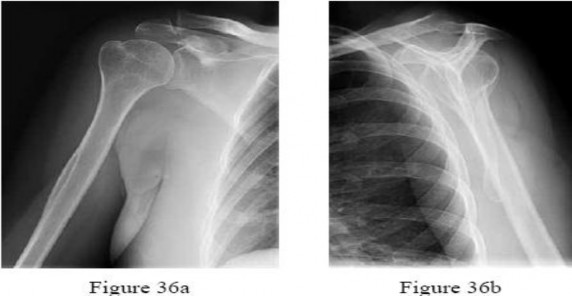
Explanation
No detailed explanation provided for this question.
Question 28High Yield
Which of the following structures is the most important restraint to posterior subluxation of the glenohumeral joint when positioned in 90 degrees of flexion and internal rotation?
Explanation
The posterior band of the inferior glenohumeral ligament is the most important restraint to posterior subluxation of the glenohumeral ligament with the shoulder in 90 degrees of flexion and internal rotation. With the shoulder in external rotation, the subscapularis is an important stabilizer to posterior subluxation. When the shoulder is in neutral rotation, the coracohumeral ligament is the primary stabilizer. The middle glenohumeral ligament functions primarily to resist anterior translation of the shoulder in the midrange of abduction. The supraspinatus muscle and tendon have relatively little contribution to anterior and posterior translation of the glenohumeral joint.
REFERENCES: Blasier RB, Soslowsky LJ, Malicky DM, Palmer ML: Posterior glenohumeral subluxation: Active and passive stabilization in a biomechanical model. J Bone Joint Surg Am 1997;79:433-440.
Flatow EL, Warner JI: Instability of the shoulder: Complex problems and failed repairs: Part I. Relevant biomechanics, multidirectional instability, and severe glenoid loss. Instr Course Lect 1998;47:97-112.
REFERENCES: Blasier RB, Soslowsky LJ, Malicky DM, Palmer ML: Posterior glenohumeral subluxation: Active and passive stabilization in a biomechanical model. J Bone Joint Surg Am 1997;79:433-440.
Flatow EL, Warner JI: Instability of the shoulder: Complex problems and failed repairs: Part I. Relevant biomechanics, multidirectional instability, and severe glenoid loss. Instr Course Lect 1998;47:97-112.
Question 29High Yield
Clinical characteristics of patients who are ideal for a nonsurgical treatment trial (instead of surgery) include
Explanation
- absence of neurologic deficits and MSSA infection.
Question 30High Yield
A
B C
D E
Figures 45a through 45c are the MR images of a 22-year-old woman who has had 6 months of ankle pain related to activities of daily living. She recently completed a course of cast immobilization and protected weight bearing without symptom resolution. Figures 45d and 45e are the intraoperative arthroscopy images after minimal probing. What is the most appropriate treatment?
B C
D E
Figures 45a through 45c are the MR images of a 22-year-old woman who has had 6 months of ankle pain related to activities of daily living. She recently completed a course of cast immobilization and protected weight bearing without symptom resolution. Figures 45d and 45e are the intraoperative arthroscopy images after minimal probing. What is the most appropriate treatment?
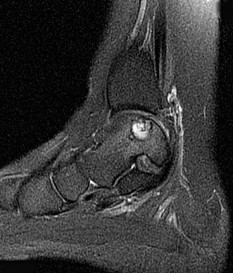
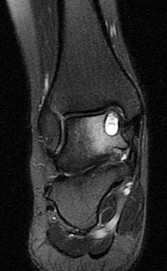
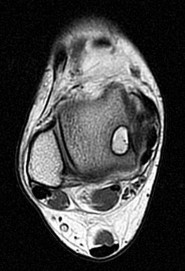
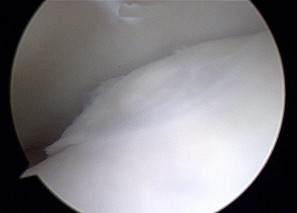
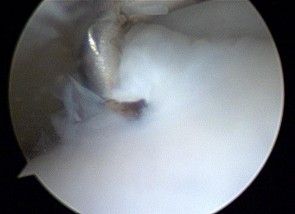
Explanation
The MR images reveal a large cystic medial talar dome osteochondral lesion (OCL) in a patient who has failed nonsurgical treatment. Ankle fusion is inappropriate because the patient has an otherwise normal ankle. Arthroscopic debridement and drilling are appropriate for smaller (< 1.5 cm sq) noncystic lesions. Retrograde drilling and bone grafting is an option in the treatment of cystic OCL if the cartilage surface is intact; however, intraoperative arthroscopy images show that this patient's cartilage surface is unstable. Osteochondral allografts and autografts are effective in the treatment of large cystic talar dome OCLs but are not appropriate for the initial surgical treatment of smaller lesions like this one.
RECOMMENDED READINGS
Hannon CP, Smyth NA, Murawski CD, Savage-Elliott I, Deyer TW, Calder JD, Kennedy JG. Osteochondral lesions of the talus: aspects of current management. Bone Joint J. 2014 Feb;96-B(2):164-71. doi: 10.1302/0301-620X.96B2.31637. Review. PubMed PMID:
[24493179/. ](http://www.ncbi.nlm.nih.gov/pubmed/24493179)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24493179)
[Easley ME, Latt LD, Santangelo JR, Merian-Genast M, Nunley JA 2nd. Osteochondral lesions of the talus. J Am Acad Orthop Surg. 2010 Oct;18(10):616-30. Review. PubMed PMID: 20889951. ](http://www.ncbi.nlm.nih.gov/pubmed/20889951)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20889951)
RECOMMENDED READINGS
Hannon CP, Smyth NA, Murawski CD, Savage-Elliott I, Deyer TW, Calder JD, Kennedy JG. Osteochondral lesions of the talus: aspects of current management. Bone Joint J. 2014 Feb;96-B(2):164-71. doi: 10.1302/0301-620X.96B2.31637. Review. PubMed PMID:
[24493179/. ](http://www.ncbi.nlm.nih.gov/pubmed/24493179)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24493179)
[Easley ME, Latt LD, Santangelo JR, Merian-Genast M, Nunley JA 2nd. Osteochondral lesions of the talus. J Am Acad Orthop Surg. 2010 Oct;18(10):616-30. Review. PubMed PMID: 20889951. ](http://www.ncbi.nlm.nih.gov/pubmed/20889951)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20889951)
Question 31High Yield
A 22-year-old skier reports painful range of motion in the left thumb after falling forward on his outstretched hand while holding his ski pole. Examination of the left thumb reveals increased AP laxity and 45° of valgus laxity at the metacarpophalangeal (MCP) joint. Examination of the right thumb shows 25° of valgus laxity at the MCP joint. Radiographs are normal. Management should consist of**
Explanation
The patient has a complete tear of the ulnar collateral ligament as defined by MCP joint laxity of greater than 30° (or 15° greater laxity compared with the opposite side). Primary repair is the treatment of choice because displacement of the ligament superficial to the adductor aponeurosis (Stener lesion) must be corrected. Any volar plate injury can be addressed during repair of the ulnar collateral ligament.
REFERENCE: Heyman P: Injuries to the ulnar collateral ligament of the thumb metacarpophalangeal joint. J Am Acad Orthop Surg 1997;5:224-229.
REFERENCE: Heyman P: Injuries to the ulnar collateral ligament of the thumb metacarpophalangeal joint. J Am Acad Orthop Surg 1997;5:224-229.
Question 32High Yield
A 6-year-old boy is being treated for acute hematogeneous osteomyelitis of the distal femur with intravenous antibiotics. The best method to determine the success or failure of initial treatment is by serial evaluations of which of the following studies?
Explanation
**38 • American Academy of Orthopaedic Surgeons**
DISCUSSION: Successful antibiotic treatment of acute osteomyelitis should lead to a rapid decline in the CRP. The CRP is the most sensitive study to follow the treatment of osteomyelitis. The CRP should decline after 48 to 72 hours of appropriate treatment. CBC and ESR are helpful in initial evaluation and diagnosis, but remain abnormal in the early phase of treatment regardless of response. Imaging studies are useful for surgical planning or secondarily if the CRP remains elevated.
REFERENCES: Unkila-Kallio L. Kallio MJ, Eskola J, et al: Serum C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in acute hematogenous osteomyelitis of children. Pediatrics 1994;93:59-62.
Herring JA(ed): Tachdjian’s Pediatric Orthopaedics, ed 4. Philadelphia. PA. WB Saunders, 2008, pp 2090-2100.
**38 • American Academy of Orthopaedic Surgeons**
DISCUSSION: Successful antibiotic treatment of acute osteomyelitis should lead to a rapid decline in the CRP. The CRP is the most sensitive study to follow the treatment of osteomyelitis. The CRP should decline after 48 to 72 hours of appropriate treatment. CBC and ESR are helpful in initial evaluation and diagnosis, but remain abnormal in the early phase of treatment regardless of response. Imaging studies are useful for surgical planning or secondarily if the CRP remains elevated.
REFERENCES: Unkila-Kallio L. Kallio MJ, Eskola J, et al: Serum C-reactive protein, erythrocyte sedimentation rate, and white blood cell count in acute hematogenous osteomyelitis of children. Pediatrics 1994;93:59-62.
Herring JA(ed): Tachdjian’s Pediatric Orthopaedics, ed 4. Philadelphia. PA. WB Saunders, 2008, pp 2090-2100.
Question 33High Yield
A 23-year-old woman was a restrained driver in a motor vehicle collision yesterday. She develops neck pain and goes to her primary care physician due to no improvement in degree of pain. She has no neurological deficits or radicular arm pain. Workup is negative for fracture. What is the best treatment for her injury shown in Figure 1?

Explanation
■
The patient has sustained a whiplash injury, which is a soft-tissue injury to the cervical spine. Her radiographs reveal loss of cervical lordosis secondary to muscle spasm. Various treatment options have been studied, ranging from aggressive physical therapy to immobilization. Early mobilization has been shown to provide the best treatment.
The patient has sustained a whiplash injury, which is a soft-tissue injury to the cervical spine. Her radiographs reveal loss of cervical lordosis secondary to muscle spasm. Various treatment options have been studied, ranging from aggressive physical therapy to immobilization. Early mobilization has been shown to provide the best treatment.
Question 34High Yield
Figures 98a and 98b are the radiograph and biopsy specimen of a 20-year-old man who is being evaluated for the first time for foot pain. Treatment should include
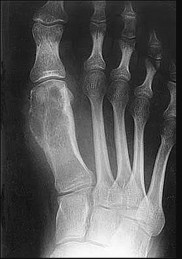
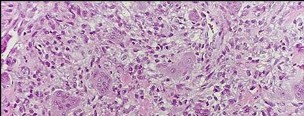
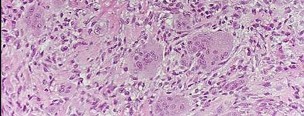
Explanation
This pathology is most consistent with giant-cell tumor. Note the presence of multinucleated cells and stroma of spindlelike cells with pale staining cytoplasm and nuclei. Giant-cell tumors typically occur in patients ages 20 to 40. Common sites include the epiphysis of the distal femur or proximal tibia (50% of the time). Although it is a benign lesion, giant-cell tumors have a tendency for bone destruction, recurrence, and, rarely, metastasis. The initial treatment of choice is curettage with grafting or cementation. For recurrent or stage III tumors, wide excision may be necessary. Chemotherapy or radiation therapy are not indicated as initial treatment, especially if this is an isolated primary lesion.
RECOMMENDED READINGS
106. [Turcotte RE. Giant cell tumor of bone. Orthop Clin North Am. 2006 Jan;37(1):35-51. Review. PubMed PMID: 16311110.](http://www.ncbi.nlm.nih.gov/pubmed/16311110)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16311110)
107. [Eckardt JJ, Grogan TJ. Giant cell tumor of bone. Clin Orthop Relat Res. 1986 Mar;(204):45-58. Review. PubMed PMID: 3514036.](http://www.ncbi.nlm.nih.gov/pubmed/3514036)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3514036)
RECOMMENDED READINGS
106. [Turcotte RE. Giant cell tumor of bone. Orthop Clin North Am. 2006 Jan;37(1):35-51. Review. PubMed PMID: 16311110.](http://www.ncbi.nlm.nih.gov/pubmed/16311110)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/16311110)
107. [Eckardt JJ, Grogan TJ. Giant cell tumor of bone. Clin Orthop Relat Res. 1986 Mar;(204):45-58. Review. PubMed PMID: 3514036.](http://www.ncbi.nlm.nih.gov/pubmed/3514036)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/3514036)
Question 35High Yield
The cystic lesion shown on the MR images in Figures 46a through 46c should cause denervation changes in which muscle?
A B
A B
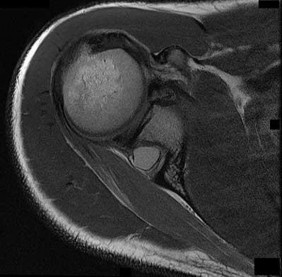
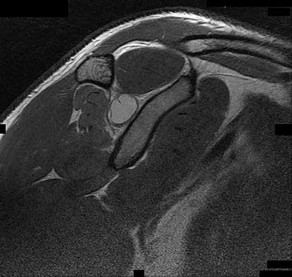
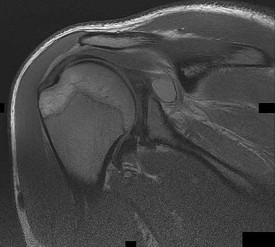
Explanation
The cystic lesion is shown in an area adjacent to the spinoglenoid notch. A space-occupying lesion in this area has the potential to compress the suprascapular nerve as it passes through the spinoglenoid notch to innervate the infraspinatus. Compression of the nerve can cause denervation and atrophy of the infraspinatus muscle. The supraspinatus is innervated by the suprascapular nerve proximal to the compressive lesions and will not undergo atrophy. The subscapularis and the teres major are innervated by the subscapular nerve.
RECOMMENDED READINGS
1. Getz CL, Ramsey ML, Williams GR. Paralabral cysts of the shoulder. In: Galatz LM, ed. Orthopaedic Knowledge Update: Shoulder and Elbow 3. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2008:339-344.
2. [Takagishi K, Saitoh A, Tonegawa M, Ikeda T, Itoman M. Isolated paralysis of the infraspinatus muscle. J Bone Joint Surg Br. 1994 Jul;76(4):584-7. PubMed PMID: 8027145.](http://www.ncbi.nlm.nih.gov/pubmed/8027145)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8027145)
RECOMMENDED READINGS
1. Getz CL, Ramsey ML, Williams GR. Paralabral cysts of the shoulder. In: Galatz LM, ed. Orthopaedic Knowledge Update: Shoulder and Elbow 3. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2008:339-344.
2. [Takagishi K, Saitoh A, Tonegawa M, Ikeda T, Itoman M. Isolated paralysis of the infraspinatus muscle. J Bone Joint Surg Br. 1994 Jul;76(4):584-7. PubMed PMID: 8027145.](http://www.ncbi.nlm.nih.gov/pubmed/8027145)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8027145)
Question 36High Yield
A 27-year-old female sustains injuries to the left femur and ipsilateral tibia shown in Figures A and B following an ATV accident. Her injury severity score (ISS) is 27 for her musculoskeletal and abdominal injuries. Her left limb is neurovascularly intact and there are no signs of compartment syndrome. What is the most appropriate definitive management?
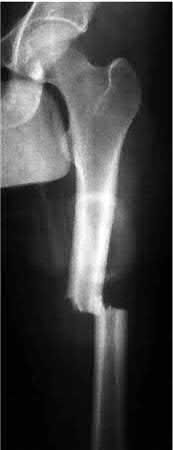
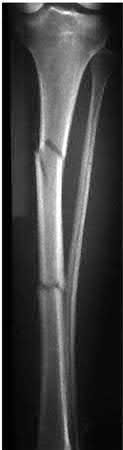
Explanation
Polytrauma patients with ipsilateral femoral and tibial fractures (floating knee injuries) often require aggressive hemodynamic resuscitation and immediate stabilization via external fixation following tenets of damage-control orthopaedics. However, goals for definitive management of these fractures include obtaining anatomic alignment, early joint range of motion, and early weightbearing. If the floating knee injury is an isolated injury and the patient is hemodynamically stable then immediate intramedullary nailing of the tibia and femur is acceptable. Of the choices listed, intramedullary nailing of both the femoral and the tibial fracture is the optimal form of fixation for these transverse fractures. The technique of antegrade intramedullary nailing of both the femur and the tibia has been well described. Retrograde femoral nails and antegrade tibial nails can be advantageous because it allows simultaneous surgical setup for both the femoral and the tibial fracture.
Question 37High Yield
A 60-year-old man who underwent left partial knee arthroplasty 6 months earlier was doing well until he
experienced left knee pain and swelling for 4 weeks following a dental procedure. The left knee aspirate was bloody, with a white blood cell count of 8,000 and 70% neutrophils. Culture grew group B Streptococcus (Granulicatella adiacens), and serologies were elevated, with an erythrocyte sedimentation rate of 55 mm/h (reference range: 0 to 20 mm/h) and a C-reactive protein level of 24 mg/L (reference range: 0.08 to 3.1 mg/L). What is the best next step?
experienced left knee pain and swelling for 4 weeks following a dental procedure. The left knee aspirate was bloody, with a white blood cell count of 8,000 and 70% neutrophils. Culture grew group B Streptococcus (Granulicatella adiacens), and serologies were elevated, with an erythrocyte sedimentation rate of 55 mm/h (reference range: 0 to 20 mm/h) and a C-reactive protein level of 24 mg/L (reference range: 0.08 to 3.1 mg/L). What is the best next step?











































Explanation
This complication is best addressed with either a single-stage or two-stage total knee arthroplasty. A recent report suggests that a single-stage arthroplasty can be effective, although many surgeons would perform a two-stage procedure with an articulating or static spacer. Arthroscopic would be non-effective, especially given 4 weeks of symptoms. Resection arthroplasty without a spacer would leave an unstable and poorly functioning extremity. Knee fusion should be used as a salvage procedure.
**below show** **the** **radiographs,** **and** **the** **CT** **obtained** **from** **a** **58-year-old** **woman** **who** **underwent**
**cementless** **left** **total** **hip** **arthroplasty.** **Nine** **months** **after** **surgery,** **she** **continued** **to** **have** **groin** **pain** **when actively** **flexing** **her** **hip.** **She** **has** **trouble** **walking** **up** **stairs** **and** **getting** **out** **of** **her** **car.** **A** **course** **of appropriate** **nonsurgical** **treatment** **failed.** **What** **is** **the** **next** **step** **in** **definitive** **treatment?**
A. **Acetabular** **component** **revision**
B. **Femoral** **component** **revision**
C. **Acetabular** **liner** **exchange**
D. Trochanteric bursectomy
Submit Answer
**Question 9**
**What** **factor** **is** **associated** **with** **a** **high** **risk** **of** **developing** **pseudotumors** **after** **metal-on-metal** **hip**
**resurfacing?**
A. **Large-diameter** **components**
B. **Age** **40** **or** **older** **for** **men**
C. **Age** **40** **or** **younger** **for** **women**
D. Diagnosis of primary osteoarthritis
**CORRECT ANSWER: C DISCUSSION:**
The recent experience of a large clinical cohort revealed the most likely risk factors as being female gender, age younger than 40, small components, and a diagnosis of hip dysplasia causing osteoarthritis. Failure was least likely among men and after procedures involving larger components. These data have prompted some authors to caution against using metal-on-metal hip resurfacing in women and to primarily target candidates who are men younger than age 50. Small components may be more prone to failure because of malpositioning and edge loading, which have been noted to be more common in dysplasia cases.
**Question 10**
**Figures** **below** **show** **the** **radiographs,** **MRI,** **and** **MR** **arthrogram** **obtained** **from** **a** **25-year-old** **collegiate**
**soccer** **player** **who** **has** **new-onset** **left** **groin** **pain.** **He** **played** **competitive** **soccer** **from** **a** **young** **age** **and** **has competed** **or** **practiced** **5** **to** **6** **times** **per** **week** **since** **the** **age** **of** **10.** **He** **denies** **any** **specific** **hip** **injury** **that necessitated** **treatment,** **but** **his** **trainer** **contends** **that** **he** **had** **a** **groin** **pull.** **He** **reports** **groin** **pain** **with** **passive flexion** **and** **internal** **rotation** **of** **the** **left** **hip,** **and** **his** **hip** **has** **less** **internal** **rotation** **than** **his** **asymptomatic right** **hip.** **He** **is** **otherwise** **healthy.When** **counseling** **patients** **who** **have** **a** **cam** **deformity,** **the** **orthopaedic surgeon** **should** **note** **that**
A. **osteoarthritis** **of** **the** **hip** **is** **likely** **to** **occur** **later** **in** **life.**
B. **correction** **prevents** **later** **development** **of** **osteoarthritis.**
C. **most** **acetabular** **tears** **are** **symptomatic,** **and** **surgical** **treatment** **will** **be** **necessary.**
D. this is an inherited deformity.
**CORRECT ANSWER: A DISCUSSION:**
Multiple studies have confirmed that cam or pincer anatomy is commonly present in asymptomatic hips. According to a large systematic review, cam deformities are present in approximately one-third of asymptomatic hips in young adults, and the proportion is higher than 50% in the subgroup of athletes. Ganz and associates proposed that femoral acetabular impingement is the root cause of osteoarthritis in most nontraumatic, nondysplastic hips, and functional improvement with surgical correction of the deformity has been demonstrated. Despite the link between cam deformity and hip osteoarthritis, a corresponding link between the correction of the deformity and prevention of osteoarthritis has never been proven. The results of cam deformity correction, typically including repair of the degenerative labral tear, are much poorer when substantial joint space loss is present. A typical joint space cutoff of 2 mm or less is used to recommend against hip preservation surgery.
**Question 11**
Figures below demonstrate the radiographs obtained from a 63-year-old man who had right total hip
arthroplasty (THA) 4 months ago. Progressive stiffness began 2 months after surgery, and he now reports pain only after prolonged physical activity. His examination reveals a normal gait and painless range of motion with flexion of 70°, extension of 0°, internal rotation of 20°, external rotation of 20°, abduction of 10°, and adduction of 10°. His erythrocyte sedimentation rate and C-reactive protein level are within defined limits. Physical therapy has produced no benefit. What is the most appropriate next step?
A. 25 mg of indomethacin 3 times daily for 6 weeks
B. 1 dose of irradiation at 800 Gy
C. Surgical excision of heterotopic ossification (HO)
D. Reevaluation in 6 months
**CORRECT ANSWER: D DISCUSSION:**
This patient presents with HO 4 months after undergoing THA. Symptomatic HO may complicate nearly
7% of primary THA cases. Improvement in pain is expected within 6 months, and most patients will not need surgical treatment. Surgical excision may be warranted for symptomatic patients after full maturation of the HO, usually 6 to 18 months after the surgery. Patients can be followed with repeated serum alkaline phosphatase levels, which are elevated initially and should return to normal upon maturation of the HO. Alternatively, a bone scan can show decreased activity after the HO has matured. Twenty-five milligrams of indomethacin 3 times daily for 6 weeks or 1 dose of irradiation at 700 to 800 Gy is effective in the prevention of HO but not for the treatment of established HO.
**Question 12**
**A** **55-year-old** **man** **is** **about** **to** **undergo** **right** **total** **hip** **arthroplasty.** **A** **preoperative** **AP** **pelvis** **radiograph**
**is** **shown** **in** **Figure** **below.** **The** **final** **acetabular** **component** **and** **polyethylene** **liner** **are** **implanted.** **With** **the broach** **in** **place,** **the** **surgeon** **trials** **a** **standard** **offset** **neck** **and** **neutral** **length** **femoral** **head.** **The** **leg** **lengths are** **approximately** **equal,** **but** **the** **hip** **is** **unstable.** **What** **is** **the** **best** **next** **step?**
A. **Choosing** **a** **longer** **femoral** **head** **and** **accepting** **a** **resulting** **leg-length** **discrepancy**
B. **Trialing** **a** **lateralized** **femoral** **neck** **component**
C. **Removing** **the** **acetabular** **liner** **and** **implanting** **an** **offset** **liner** **instead**
D. Performing a trochanteric osteotomy with advancement
**CORRECT ANSWER: B**
DISCUSSION:
The radiograph shows that this patient has a high offset varus femoral morphology of both hips. Preoperative templating would identify this, and the surgeon should choose an implant system that has extended offset options to help match the native anatomy and biomechanics and minimize the risk of instability. Trialing a high offset neck, rather than a standard offset neck, is the next most appropriate step. Depending on the design of the implant system, this step can be accomplished by direct medialization of the femoral head, which would not affect leg length, or by lowering the neck angle, which would affect the leg length and would require a longer femoral head, because the leg lengths had previously been equal. Placement of a longer femoral head would likely improve hip stability but would also make the leg length uneven, which is a common cause of dissatisfaction after total hip arthroplasty. An offset acetabular liner also increases the leg length and does not correct the issue, which is on the femoral side. Trochanteric
advancement is sometimes used as a treatment for instability but would be inappropriate as the next step in this setting.
**Question 13**
**During** **total** **hip** **arthroplasty,** **what** **characteristic** **of** **irradiated** **(10** **Mrad)** **and** **subsequently** **melted** **highly**
**cross-linked** **polyethylene** **should** **provide** **a** **more** **wear-resistant** **construct** **than** **traditional** **gamma- irradiated** **(2.5-4** **Mrad)-in-air** **polyethylene** **mated** **with** **the** **same** **head?**
A. **Resistance** **to** **adhesive** **wear** B. **Resistance** **to** **abrasive** **wear** C. **Resistance** **to** **fatigue** **wear**
D. Resistance to creep
**CORRECT ANSWER: B**
DISCUSSION:
Highly cross-linked polyethylene makes material resistant to adhesive wear. Abrasive wear from third bodies does not decrease wear. The fatigue strength of such material is inferior to that of traditional polyethylene, and its resistance to creep is the same, if not lower, than that of traditional polyethylene.
**Question 14**
**When** **compared** **with** **patients** **having** **a** **body** **mass** **index** **(BMI)** **lower** **than** **35,** **patients** **with** **a** **BMI**
**above** **40** **who** **undergo** **primary** **total** **hip** **arthroplasty** **(THA)** **and** **total** **knee** **arthroplasty** **(TKA)** **are likely** **to** **have**
A. **smaller** **incisions.**
B. **more** **wound** **complications.**
C. **fewer** **30-day** **and** **90-day** **readmissions.**
D. lower rates of patient satisfaction.
**CORRECT ANSWER: B**
DISCUSSION:
The obesity epidemic is increasing, and the number of patients with a BMI higher than 35 undergoing THA and TKA also is growing. Controversy exists over the optimal BMI cutoff and the ability to perform joint replacements safely in patients who are morbidly obese. Several clinical series and national database analyses have shown that morbidly obese patients undergoing THA or TKA are at increased risk for wound complications as well as 30-day and 90-day readmissions. These patients’ incisions are typically larger because of the size of the soft-tissue envelope. Although the clinical scores following successful THA or TKA often are lower than the scores of controls, the overall changes in clinical function and satisfaction are equivalent in nonobese and obese patients.
**Question 15**
**An** **otherwise** **healthy** **76-year-old** **woman** **has** **pain** **2** **years** **after** **total** **hip** **arthroplasty.** **The** **clinical**
**photograph** **in** **Figures** **below** **demonstrates** **her** **skin** **envelope,** **and** **associated** **radiograph.** **Her** **C-reactive protein** **level** **is** **normal,** **and** **her** **erythrocyte** **sedimentation** **rate** **is** **mildly** **elevated.** **The** **white** **blood** **cell count** **is** **normal.** **Hip** **aspiration** **attempted** **under** **fluoroscopy** **generates** **no** **fluid.** **What** **is** **the** **best** **definitive treatment?**
A. **Repeat** **left** **hip** **aspiration**
B. **Initiation** **of** **a** **wound** **care** **consult** **and** **oral** **antibiotics**
C. **Irrigation** **and** **debridement** **with** **closure** **of** **the** **dehisced** **wound,** **performance** **of** **a** **liner** **exchange, and** **administration** **of** **intravenous** **antibiotics**
D. **Debridement** **of** **the** **wound,** **explant** **of** **the** **total** **hip,** **placement** **of** **a** **spacer,** **and** **administration** **of**
intravenous antibiotics
**CORRECT ANSWER: D**
DISCUSSION:
This patient clearly has a chronically infected total hip arthroplasty, indicated by the open, draining sinus, as well as trochanteric bone resorption on radiographs, and two years of pain. Recently, specific guidelines have been published to better help the clinician define infection. Repeating the hip aspiration is unnecessary, because infection is already evident. Initiating a wound care consult would not address the underlying infection. The determination whether to retain the components or perform a two-stage exchange is based more on the acuity of infection. In this particular case, the patient is chronically infected. Irrigation and debridement with a liner exchange and retention of the components are reserved for the acute setting.
**Question 16**
Figures below show the radiographs obtained from a 90-year-old woman who is seen in the emergency
department after a fall from a height. She has right hip and thigh pain and is unable to bear weight. Based on this patient's history and imaging, what is the best next step?
A. Hip revision and implantation of a proximal femoral replacement
B. Hip revision and implantation of a tapered fluted stem
C. Open reduction and internal fixation with a locked plate and allograft struts
D. Erythrocyte sedimentation rate and C-reactive protein laboratory studies
**CORRECT ANSWER: D**
DISCUSSION:
Periprosthetic fracture is the third most common reason (after loosening and infection) for revision surgery after total hip arthroplasty (THA). Late periprosthetic fracture risk is 0.4% to 1.1% after primary
THA and 2.1% to 4% after revision THA. Risk factors for periprosthetic fracture include age over 70 years, decreasing bone mass, and loosening of implants and osteolysis. The risk of concomitant infection in the presence of a periprosthetic fracture is 11%, according to Chevillotte and associates. Obtaining presurgical aspiration or intrasurgical tissue for culture is recommended if concomitant infection is suspected.
**Question 17**
**Figure** **below** **shows** **the** **radiograph** **obtained** **from** **a** **73-year-old** **woman** **who** **returns** **status** **post** **total** **hip**
**arthroplasty** **14** **years** **earlier.** **She** **denies** **pain** **and** **has** **no** **discomfort** **on** **examination.** **She** **then** **undergoes revision** **total** **hip** **arthroplasty** **with** **head** **and** **liner** **exchange** **and** **bone** **grafting.** **After** **a** **physical** **therapy session** **two** **days** **after** **surgical** **intervention,** **she** **develops** **inability** **to** **dorsiflex** **the** **foot** **while** **she** **is** **sitting in** **a** **chair.** **The** **initial** **treatment** **should** **consist** **of**
A. **lying** **completely** **supine** **in** **bed.**
B. **remaining** **seated** **and** **placing** **the** **postsurgical** **leg** **on** **a** **stool.**
C. **transferring** **back** **to** **bed** **with** **the** **head** **of** **the** **bed** **no** **lower** **than** **60°.**
D. transferring back to bed with the head of the bed level and the surgical knee flexed.
**CORRECT ANSWER: D**
DISCUSSION:
Gamma irradiation produces free radicals. Although these free radicals can form cross-links with other polyethylene chains, the free radicals can also form a bond with oxygen, resulting in early oxidation. Gamma irradiation in air produces the highest risk for oxidized polyethylene, resulting in the highest risk for wear, delamination, and subsequent osteolysis. This patient demonstrates severe periarticular osteolysis. When she is asymptomatic, this suggests the acetabular and femoral components remain well fixed to the bone. Consequently, she can be treated by removing the wear generator (polyethylene exchange), along with bone grafting of the osteolytic defect. Considering the extensive amount of osteolysis indefinite observation would not be appropriate. A foot drop develops 2 days after surgery. As a result, it can be assumed that the nerve was not injured directly during the surgical procedure. Although MRI or CT may be indicated to identify an evolving hematoma, the immediate concern is to minimize pressure on the sciatic nerve. Tension on the nerve can be reduced by flexing the surgical knee and positioning the bed flat.
**Question 18**
**Figure** **below** **depicts** **the** **radiograph** **obtained** **from** **a** **52-year-old** **woman** **who** **has** **leg-length** **inequality**
**and** **chronic,** **activity-related** **buttock** **discomfort.** **This** **problem** **has** **been** **lifelong,** **but** **it** **is** **getting** **worse and** **increasingly** **causing** **back** **pain.** **What** **is** **the** **best** **current** **technique** **for** **total** **hip** **arthroplasty?**
A. **High** **hip** **center**
B. **Anatomic** **hip** **center** **with** **trochanteric** **osteotomy** **and** **progressive** **femoral** **shortening**
C. **Anatomic** **hip** **center** **with** **subtrochanteric** **shortening** **osteotomy**
D. Iliofemoral lengthening followed by an anatomic hip center
**CORRECT ANSWER: C**
DISCUSSION:
A high hip center is not recommended for Crowe type IV hips because of the lack of acetabular bone and altered hip biomechanics. An anatomic center is a better option but necessitates a technique to address the tight soft-tissue envelope. A trochanteric osteotomy with progressive femoral shortening has been described but can be prone to trochanter nonunion. Iliofemoral lengthening prior to surgery has been described but may not be tolerated by all patients. A shortening subtrochanteric osteotomy avoids trochanter nonunion and allows adjustment of femoral anteversion. Fixation of the osteotomy can include a stem with distal rotational control, plate fixation, a step versus oblique cut, or strut grafts.
**Question 19**
**Figures** **1** **through** **5** **show** **the** **radiographs,** **MRI,** **and** **MR** **arthrogram** **obtained** **from** **a** **25-year-old**
**collegiate** **soccer** **player** **who** **has** **new-onset** **left** **groin** **pain.** **He** **played** **competitive** **soccer** **from** **a** **young age** **and** **has** **competed** **or** **practiced** **5** **to** **6** **times** **per** **week** **since** **the** **age** **of** **10.** **He** **denies** **any** **specific** **hip injury** **that** **necessitated** **treatment,** **but** **his** **trainer** **contends** **that** **he** **had** **a** **groin** **pull.** **He** **reports** **groin** **pain**
**with** **passive** **flexion** **and** **internal** **rotation** **of** **the** **left** **hip,** **and** **his** **hip** **has** **less** **internal** **rotation** **than** **his asymptomatic** **right** **hip.** **He** **is** **otherwise** **healthy.** **Approximately** **what** **percentage** **of** **asymptomatic**
**athletes** **have** **cam** **deformities** **of** **the** **hip?**
A. **5%**
B. **10%**
C. **25%**
D. At least 50%
**CORRECT ANSWER: D**
DISCUSSION:
Multiple studies have confirmed that cam or pincer anatomy is commonly present in asymptomatic hips. According to a large systematic review, cam deformities are present in approximately one-third of asymptomatic hips in young adults, and the proportion is higher than 50% in the subgroup of athletes. Ganz and associates proposed that femoral acetabular impingement is the root cause of osteoarthritis in most nontraumatic, nondysplastic hips, and functional improvement with surgical correction of the deformity has been demonstrated. Despite the link between cam deformity and hip osteoarthritis, a corresponding link between the correction of the deformity and prevention of osteoarthritis has never been proven. The results of cam deformity correction, typically including repair of the degenerative labral tear, are much poorer when substantial joint space loss is present. A typical joint space cutoff of 2 mm or less is used to recommend against hip preservation surgery.
**Question 20**
**A** **59-year-old** **active** **woman** **undergoes** **elective** **total** **hip** **replacement** **in** **which** **a** **posterior** **approach** **is**
**used.** **She** **has** **minimal** **pain** **and** **is** **discharged** **to** **home** **2** **days** **after** **surgery.** **Four** **weeks** **later,** **she dislocates** **her** **hip** **while** **shaving** **her** **legs.** **She** **undergoes** **a** **closed** **reduction** **in** **the** **emergency** **department. Postreduction** **radiographs** **show** **a** **reduced** **hip** **with** **well-fixed** **components** **in** **satisfactory** **alignment. What** **is** **the** **most** **appropriate** **management** **of** **this** **condition** **from** **this** **point** **forward?**
A. **Observation** **and** **patient** **education** **regarding** **hip** **dislocation** **precautions**
B. **Revision** **to** **a** **larger-diameter** **femoral** **head**
C. **Revision** **to** **a** **constrained** **acetabular** **component**
D. Application of a hip orthosis for 3 months
**CORRECT ANSWER: A**
DISCUSSION:
First-time early dislocations are often treated successfully without revision surgery, especially when no component malalignment is present. In this clinical scenario, it appears the patient would benefit from better education about dislocation precautions. Hip orthoses are of questionable benefit unless the patient is cognitively impaired. Revision surgery can be successful but is usually reserved for patients with recurrent dislocations.
**Question 21**
A 62-year-old active man returns for routine follow-up 16 years after hip replacement. He has no hip pain.
Radiographs reveal a well-circumscribed osteolytic lesion around a single acetabular screw. All hip components are perfectly positioned. Comparison radiographs obtained 6 months later show an increase in the size of the osteolytic lesion. CT depicts a well-described lesion that is 3 cm at its largest diameter and is localized around one screw hole with an eccentric femoral head. What treatment is appropriate, assuming that well-fixed cementless total hip components are in place?
A. Revision of the polyethylene liner, removal of the screw, and debridement of the osteolytic lesion with or without bone grafting
B. Revision of the acetabular component to a newer design without screws
C. Removal of the screw, revision of the polyethylene liner, and stem cell injection into the lytic lesion
D. Removal of the offending screw from the metal socket and placement of a new polyethylene liner in the existing socket
**CORRECT ANSWER: A**
DISCUSSION:
Given a well-fixed acetabular metal shell and a localized osteolytic lesion, good outcomes can be expected from liner revision in this clinical scenario with retention of the metal socket, assuming no damage to the components or other unexpected findings arise during revision surgery. Here, complete cup revision is not warranted, considering the appropriate implant position. Beaulé and associates reviewed 83 consecutive patients (90 hips) in whom a well-fixed acetabular component was retained in a clinical scenario such as the one described. No hip showed recurrence or expansion of periacetabular osteolytic lesions. If the metal cup is unstable, acetabular component revision may be indicated.
**Question 22**
Figure 1 shows the radiograph obtained from a 78-year-old woman who has a recent history of increasing
thigh pain 12 years after undergoing total hip arthroplasty. Figure 2 depicts the radiograph obtained after she fell and was unable to ambulate. What is the most appropriate treatment?
A. Application of a femoral cable plate
B. Application of cerclage-wired double allograft femoral struts
C. Femoral revision with an uncemented long stem
D. Femoral revision with a cemented long-stem prosthesis
**CORRECT ANSWER: C**
DISCUSSION:
The surgical treatment of periprosthetic fractures of total hip replacement with a loose implant and progressive bone loss is associated with a high complication rate. The recent literature would favor the use of long "Wagner-type" stems, which have a long distal taper that may optimally engage the remaining femoral shaft isthmus. Plating options are problematic, because the intramedullary stem limits the ability to use screws with the plate. Using long distally fixed stems circumvents this problem by enhancing
fracture healing and creating a long-term prosthetic solution in these most difficult cases.
**Question 23**
**Early** **postoperative** **infections** **following** **primary** **total** **hip** **arthroplasty** **are** **most** **likely** **caused** **by** **which**
**organism?**
A. **Staphylococcus** **epidermidis**
B. **Streptococcus** **viridans**
C. **Propionibacterium** **acnes**
D. Staphylococcus aureus
**CORRECT ANSWER: D**
DISCUSSION:
_S aureus_ is the most common organism cultured in early (fewer than 4 weeks postoperative) periprosthetic infections. Methicillin-resistant _S aureus_ is becoming a more common pathogen in certain patient populations. B hemolytic _Streptococcus_ and some gram-negative infections can also be found in early postoperative infections. _S epidermidis_ , _S viridans_ , and _P acnes_ are more commonly found in late (more
than 4 weeks postoperative) infections.
**Question 24**
**A** **healthy,** **active** **72-year-old** **man** **trips** **and** **falls,** **landing** **on** **his** **left** **hip** **10** **weeks** **after** **an** **uncomplicated**
**left** **primary** **uncemented** **total** **hip** **replacement.** **A** **radiograph** **taken** **6** **weeks** **after** **surgery** **and** **before** **the fall** **is** **shown** **in** **Figure** **1.** **A** **radiograph** **taken** **after** **the** **fall** **is** **shown** **in** **Figure** **2.** **He** **is** **unable** **to** **bear weight** **and** **is** **brought** **to** **the** **emergency** **department.** **Examination** **reveals** **a** **slightly** **shortened** **left** **lower extremity** **and** **some** **mild** **ecchymosis** **just** **distal** **to** **the** **left** **greater** **trochanteric** **region,** **but** **his** **skin** **is** **intact, without** **abrasions** **or** **lacerations.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Open** **reduction** **and** **cerclage** **fixation** **of** **the** **fracture**
B. **Open** **reduction** **and** **revision** **of** **the** **femoral** **implant** **to** **a** **long** **cemented** **stem**
C. **Open** **reduction** **and** **revision** **of** **the** **femoral** **implant** **to** **a** **long** **fluted** **and** **tapered** **uncemented stem**
D. Application of balanced traction followed by surgery after the ecchymosis has resolved
**CORRECT ANSWER: D**
DISCUSSION:
This patient has a periprosthetic femoral fracture with a loose femoral stem and normal femoral bone stock, representing a Vancouver type B2 fracture. The most appropriate treatment is fixation of the fracture, along with revision of the stem. Considering his age, bone quality, and activity level, a longer uncemented stem is most predictable. Although a cylindrical stem may also be used, the fluted stem option is the only uncemented choice listed and is the most appropriate option. A cemented stem is a poorer choice because it is difficult to keep the cement out of the fracture site, which would pose a risk for nonunion at the fracture. Also, overall poorer results have been associated with long cemented stems in healthy, active people. Surgery does not need to be delayed to allow the ecchymosis to resolve, and simple open reduction and fixation does not address the loose stem.
**Question 25**
**A** **70-year-old** **man** **undergoes** **removal** **of** **an** **infected** **total** **hip** **arthroplasty** **(THA)** **and** **insertion** **of** **an**
**articulating** **antibiotic-loaded** **spacer** **to** **treat** **a** **deep** **periprosthetic** **hip** **infection.** **While** **in** **a** **nursing** **home receiving** **intravenous** **antibiotics** **3** **weeks** **after** **surgery,** **the** **patient** **trips** **and** **falls.** **Examination** **reveals swelling** **in** **the** **mid** **and** **distal** **thigh,** **intact** **skin** **and** **neurovascular** **structures,** **and** **severe** **pain** **with** **knee**
**or** **hip** **movement.** **Radiographs** **of** **the** **femur** **are** **shown** **in** **Figures** **1** **through** **4.** **What** **is** **the** **most appropriate** **treatment** **for** **the** **fracture** **below** **the** **implant?**
A. **Balanced** **traction** **to** **address** **concern** **for** **persistent** **infection** **with** **reoperation**
B. **Open** **reduction** **and** **internal** **fixation** **of** **the** **fracture** **with** **a** **lateral** **plate** **and** **screws**
C. **Removal** **of** **the** **articulating** **spacer** **and** **revision** **to** **a** **longer-stem** **antibiotic-loaded** **articulating spacer**
D. **Removal** **of** **the** **articulating** **spacer** **and** **reimplantation** **using** **a** **long-stem** **fluted** **uncemented** **hip replacement**
**CORRECT ANSWER: B**
DISCUSSION:
This patient has a type C periprosthetic femoral fracture. The articulating spacer is not involved in the fracture, which is well distal to the implant. The most appropriate treatment is open reduction and internal fixation of the fracture. Traction is not appropriate for this fracture because the injury can be treated surgically despite the history of previous hip infection. Traction would also be needed for at least 5 weeks and would delay the surgical treatment of the periprosthetic fracture until the time of second-stage revision THA. The fracture is fairly distal, and revision to a longer antibiotic-loaded implant or uncemented stem is not suitable for this fracture pattern, because it extends well past the isthmus. A femoral stem in the distal fragment would provide little stability for the fracture. Removal of the articulating spacer and reimplantation using a long-stem fluted uncemented hip replacement is not appropriate, because it would be premature to reimplant the man's hip while he is still receiving treatment for a deep hip infection.
**Question 26**
**Figures** **1** **and** **2** **demonstrate** **the** **radiographs** **obtained** **from** **a** **35-year-old** **woman** **with** **end-stage**
**debilitating** **osteoarthritis** **of** **the** **right** **hip.** **She** **is** **contemplating** **total** **hip** **arthroplasty** **(THA).** **She** **has** **a history** **of** **right** **hip** **dysplasia** **and** **underwent** **hip** **osteotomy** **as** **an** **adolescent.** **Over** **the** **years,** **nonsurgical treatment,** **including** **weight** **loss,** **activity** **modifications,** **and** **intra-articular** **injections,** **has** **failed.** **Her infection** **work-up** **reveals** **laboratory** **findings** **within** **defined** **limits.** **Which** **bearing** **surface** **is contraindicated** **for** **this** **patient?**
A. **Ceramic-on-ceramic**
B. **Ceramic-on-highly** **cross-linked** **polyethylene** **(HXPE)**
C. **Metal-on-HXPE**
D. Metal-on-metal
**CORRECT ANSWER: D**
DISCUSSION:
THA has proven durable and reliable for pain relief and improving function for patients with end-stage arthritis. Appropriate bearing selection is critical to minimize wear and hip complications. A metal-on- metal articulation is associated with excellent wear rates in vitro. With its capacity to offer a low wear rate with large femoral heads, it is an attractive bearing choice for THA. However, local soft-tissue reactions, pseudotumors, and potential systemic reactions including renal failure, cardiomyopathy, carcinogenesis, and potential teratogenesis with potential transfer of metal ions across the placental barrier make metal-on-metal bearings less desirable and relatively contraindicated for younger women of child- bearing age. The workup of a painful metal-on-metal hip arthroplasty necessitates a systematic approach. Several algorithms have been proposed. Routine laboratory studies including sedimentation rate, CRP, and serum cobalt and chromium ion levels should be obtained for all patients with pain. Advanced imaging including MARS MRI should be performed to evaluate for the presence of fluid collections, pseudotumors, and abductor mechanism destruction. Infection can coexist with metal-on-metal reactions, so, when indicated (if the CRP level is elevated), a hip arthrocentesis should be obtained. However, in this setting, a manual cell count and differential should be obtained because an automated cell counter may provide falsely elevated cell counts. The results of revision surgery for a failed metal-on-metal hip prosthesis can be variable. The amount of local tissue destruction and the integrity of the hip abductor mechanism can greatly influence outcomes. Instability is the most common complication following revision of failed metal-on-metal hip replacements.
**Question 27**
**Figures** **below** **show** **the** **radiograph** **and** **the** **MRI** **scan** **obtained** **from** **a** **37-year-old** **woman** **with** **a** **2-month**
**history** **of** **left** **hip** **pain.** **Which** **presurgical** **factor** **is** **most** **commonly** **associated** **with** **a** **poor** **outcome** **after a** **hip** **joint** **salvage** **procedure?**
A. **Age** **older** **than** **40** **years**
B. **Body** **mass** **index** **higher** **than** **30**
C. **Tönnis** **grade** **of** **2** **or** **higher**
D. Outer bridge grade of III or IV
**CORRECT ANSWER: C**
DISCUSSION:
MRI reveals an anterior labral tear, and the radiograph shows minimal arthritis with possible dysplasia. The most common location of pain in patients with a labral tear is the groin, and the most common physical finding is a positive impingement test result. Pain during sitting, clicking, and buttock pain are frequently described by patients with a labral tear, but these symptoms are less common than groin pain. A positive posterior impingement test finding is more common in patients with a posterior labral tear. Although age over 40 years and a body mass index higher than 30 can adversely affect clinical outcomes after joint preservation procedures such as PAO, hip arthroscopy, and femoral acetabular impingement surgery, the presence of hip arthritis on presurgical radiographs is the most commonly mentioned cause of failed hip joint preservation surgery. Tönnis grade is a radiographic measure of hip arthritis. A higher Outerbridge score is associated with more frequent poor outcomes after hip arthroscopy; however, the
Outerbridge cartilage score is determined by direct visualization at the time of surgery. The Outerbridge
score cannot be determined presurgically.
**Question 28**
Figure below shows the radiograph obtained from a 68-year-old man who fell 3 weeks after undergoing a
successful left primary total hip arthroplasty. He is experiencing a substantial increase in pain and an inability to bear weight. What is an appropriate treatment plan?
A. Open reduction and internal fixation (ORIF) of the fracture
B. Removal of the current stem, femur ORIF, and insertion of a longer revision stem
C. Femur ORIF with cables and strut graft, leaving the current stem in situ
D. Femur ORIF combined with reimplantation of the primary component
**CORRECT ANSWER: B**
DISCUSSION:
The fracture has occurred around the stem, representing a Vancouver type B fracture, and the stem is clearly loose, making it a type B2 fracture. The appropriate treatment is removal of the loose in situ stem; ORIF of the femur using cerclage wires, cables, or a plate; and insertion of a longer revision stem such as a tapered fluted modular titanium or fully porous coated cylindrical stem to bypass the fracture. All of the other options are incorrect, because they represent inappropriate treatment options for a Vancouver type B2 fracture.
**Question 29**
**What** **factor** **is** **associated** **with** **a** **higher** **risk** **of** **dislocation** **after** **total** **hip** **arthroplasty?**
A. **Male** **gender**
B. **Previous** **hip** **surgery**
C. **A** **direct** **lateral** **surgical** **approach**
D. Metal-on-metal bearing surfaces
**CORRECT ANSWER: B**
DISCUSSION:
Dislocation after total hip arthroplasty is a multifactorial problem. Numerous risk factors may act independently or cumulatively to increase the risk of this complication. Previous hip surgery of any kind is associated with a twofold increased risk for dislocation. Other risk factors include female gender, impaired mental status, inflammatory arthritis, and older age. Numerous studies have shown a lower dislocation rate with a direct lateral approach, although surgical techniques such as capsular repair have
significantly lowered the incidence of dislocation after using the posterior approach. Metal-on-metal bearings have been associated with other complications such as adverse tissue reactions but are often used with larger-diameter bearings, which pose a lower risk of dislocation.
**Question 30**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **19-year-old** **woman** **with** **a** **3-year** **history** **of**
**progressive** **hip** **pain** **in** **the** **left** **groin** **with** **activity,** **which** **is** **unresponsive** **to** **activity** **modification** **and physical** **therapy.** **Examination** **reveals** **normal** **range** **of** **motion,** **with** **pain** **on** **anterior** **impingement** **testing. What** **treatment** **is** **associated** **with** **the** **best** **long-term** **results?**
A. **Hip** **arthroscopy** **with** **labral** **repair** B. **Reverse** **periacetabular** **osteotomy** C. **Varus** **rotational** **osteotomy**
D. Open surgical dislocation with rim trimming
**CORRECT ANSWER: B**
DISCUSSION:
This patient has symptomatic femoroacetabular impingement as well as clinical and radiographic signs of acetabular retroversion, including a cross-over sign, ischial spine sign, and posterior wall sign bilaterally. Good midterm to long-term outcomes have been reported with reverse (anteverting) Bernese periacetabular osteotomy (PAO). In patients with less retroversion, open or arthroscopic rim trimming with labral refixation have shown good short-term results, but longer-term results have yet to be fully delineated. Isolated hip arthroscopy and labral repair would not be indicated without addressing the retroversion deformity. Femoral varus rotational osteotomy plays no role in the treatment of this pathology. Open surgical dislocation with rim trimming could be considered in patients with less deformity, but some studies have shown inferior long-term results compared with reverse PAO.
**Question 31**
**Figure** **below** **depicts** **the** **radiograph** **obtained** **from** **a** **30-year-old** **woman** **who** **began** **having** **more** **right**
**than** **left** **hip** **pain** **during** **a** **recent** **pregnancy.** **Physical** **examination** **reveals** **increased** **range** **of** **motion** **with positive** **flexion** **abduction** **and** **external** **rotation** **and** **flexion** **adduction** **and** **internal** **rotation** **as** **well** **as** **pain with** **external** **logroll.** **Assessment** **of** **Figure** **below** **reveals**
A. **classic** **dysplasia** **with** **volume** **deficient** **acetabula.**
B. **acetabular** **retroversion** **with** **positive** **crossover** **signs** **and** **ischial** **spine** **signs.**
C. **no** **substantial** **dysplasia,** **with** **normal** **acetabular** **volume** **and** **anteversion.**
D. inadequate radiographic evidence to assess for hip dysplasia.
**CORRECT ANSWER: D**
DISCUSSION:
Studies have demonstrated that pelvic inclination can dramatically affect the interpretation of radiographs in the dysplastic hip, with 9° of increased pelvic inclination leading to the presence of crossover signs and posterior wall signs. A distance of 30 mm to 50 mm from the sacrococcygeal junction to the pubis is often used to assess the adequacy of pelvic inclination on radiographs, although Siebenrock and associates determined the mean difference to be 32 mm in men and 47 mm in women. In this patient, the pelvic inclination is dramatically increased, leading to overestimation of acetabular retroversion.
**Question 32**
In patients with Crowe types III and IV developmental dysplasia of the hip with high hip centers, acetabular
reconstruction often requires lowering the acetabular component into the native acetabulum. In doing so, considerable risk for limb lengthening beyond 4 cm exists, making the hip difficult to reduce and raising the risk for nerve injury. Which technique is used to overcome this problem?
A. Subtrochanteric osteotomy with femoral shortening
B. An offset femoral component
C. A lateralized liner
D. Extended trochanteric osteotomy
**CORRECT ANSWER: A**
DISCUSSION:
When substantial lengthening of a dysplastic hip will occur because a high dislocation is relocated into a considerably lower acetabulum, a femoral shortening may be necessary to reduce the hip and avoid a stretch injury to the sciatic nerve. No other choice specifically addresses the need for femoral shortening, and high offset stems and lateralized liners may exacerbate the problem if used alone and without femoral shortening.
**Question 33**
Figures 1 through 3 show the radiograph and MR arthrograms obtained from a 25-year-old woman who has
had right groin pain since joining the military 4 years ago. She has undergone treatment with NSAIDs, physical therapy, and activity modification. Examination reveals positive flexion abduction and external rotation, a positive external log roll, and increased range of motion. What is the most appropriate treatment?
A. Viscosupplementation of the right hip
B. Hip arthroscopy with labral repair
C. Periacetabular osteotomy
D. Total hip arthroplasty
**CORRECT ANSWER: C**
DISCUSSION:
This patient has symptomatic hip dysplasia that has been recalcitrant to nonsurgical management. Radiographs reveal an upsloping sourcil (acetabular index of 18) and a lateral center edge angle of 14, with posterior uncovering. The MR arthrogram shows no definitive evidence of a labral tear. Appropriate surgical management would include periacetabular osteotomy. Viscosupplementation in the hip is controversial in the treatment of osteoarthritis and plays no role in the treatment of dysplasia. Hip arthroscopy with labral repair is controversial in mild hip dysplasia, with studies demonstrating between
60% and 77% good and excellent results, inferior to the results for hip arthroscopy in a femoroacetabular impingement cohort. In moderate to severe dysplasia, hip arthroscopy is not recommended. Because the acetabular cartilage is well maintained, total hip arthroplasty would not be recommended in this young and active patient.
**Question 34**
**Figures** **1** **and** **2** **show** **the** **radiographs** **obtained** **from** **a** **68-year-old** **morbidly** **obese** **man** **who** **underwent**
**left** **total** **hip** **replacement** **7** **years** **ago** **and** **did** **well,** **with** **no** **symptoms** **prior** **to** **the** **current** **presentation. He** **recently** **rose** **from** **a** **seated** **position** **and** **felt** **a** **pop** **in** **the** **hip,** **with** **immediate** **pain** **and** **inability** **to** **bear weight.** **Any** **pressure** **on** **the** **left** **foot** **now** **produces** **a** **painful,** **grinding** **sensation** **with** **loss** **of** **left** **hip stability.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **of** **the** **acetabular** **implant** **to** **a** **constrained** **bearing** **with** **modular** **exchange** **of** **the femoral** **head** **and** **neck**
B. **Revision** **of** **the** **acetabular** **and** **femoral** **implants**
C. **Retention** **of** **the** **acetabular** **implant** **with** **modular** **exchange** **of** **the** **femoral** **head** **and** **neck**
D. Revision of the femoral component alone with a new ceramic head
**CORRECT ANSWER: B**
DISCUSSION:
The modular femoral stem has fractured. Changing the liner to a constrained design is not warranted at this time based on the information provided. Revision of the acetabular implant is appropriate because of the potential for damage to the existing cup from metal debris and femoral implant contact and to convert from a metal-on-metal articulation. Nonsurgical management would not provide pain relief or improvement; revision of the total hip arthroplasty is recommended. The implant failed in a short time, and retention of the femoral stem is not recommended because of the concern for failure with only a neck exchange. A dual-mobility bearing may be a good option if the surgeon plans to retain the acetabular component. Extended trochanteric osteotomy is a useful technique for the removal of a well-fixed femoral implant. In this patient, femoral stem removal without
osteotomy would be difficult due to the fracture of the implant’s femoral neck and the
inability to gain purchase for extraction.
**Question 35**
**A** **63-year-old** **woman** **had** **a** **primary** **total** **hip** **arthroplasty** **7** **years** **ago** **that** **included** **a** **proximally** **coated titanium** **stem,** **a** **cobalt** **alloy** **femoral** **head,** **a** **titanium** **hemispherical** **acetabular** **component,** **and** **a polyethylene** **liner.** **She** **did** **well** **for** **4** **years** **but** **has** **now** **had** **two** **dislocations** **and** **reports** **pain** **and weakness** **around** **the** **left** **hip.** **She** **denies** **any** **fevers,** **chills,** **or** **constitutional** **symptoms.** **On** **examination, the** **patient** **walks** **well** **without** **any** **signs** **of** **an** **antalgic** **or** **Trendelenburg** **gait.** **Her** **abductor** **mechanism demonstrates** **good** **strength.** **Her** **erythrocyte** **sedimentation** **rate** **and** **C-reactive** **protein** **level** **are** **normal. On** **radiographs,** **all** **components** **appear** **well** **fixed** **and** **in** **good** **alignment.** **What** **is** **the** **most** **appropriate treatment** **at** **this** **time?**
A. **Physical** **therapy** **to** **improve** **hip** **stability**
B. **Use** **of** **an** **abduction** **brace** **to** **limit** **the** **patient’s** **range** **of** **motion**
C. **Conversion** **to** **a** **constrained** **acetabular** **liner**
D. Cobalt and chromium serum metal ion level testing
**CORRECT ANSWER: D**
DISCUSSION:
Trunnionosis is a recently recognized complication following total hip arthroplasty and can occur when a cobalt alloy femoral head is used on a titanium alloy or cobalt alloy femoral stem. Patients often present with pain or swelling around the hip but at times can present with instability. Certain femoral stem designs have been associated with increased reports of trunnionosis. In a patient with a cobalt alloy femoral head who presents with instability, swelling, and weakness around the hip, the potential for trunnionosis and
an adverse local tissue reaction should be considered.
**Question 36**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **68-year** **old** **man** **with** **progressively** **worsening** **right**
**side** **hip** **pain** **over** **the** **last** **8** **months.** **He** **is** **6** **feet** **tall,** **with** **a** **BMI** **of** **51** **kg/m** 2 **and** **reports** **that** **his** **index total** **hip** **arthroplasty** **was** **performed** **8** **years** **ago.** **The** **preoperative** **work-up** **includes** **negative** **infectious laboratory** **results.** **What** **is** **the** **most** **appropriate** **surgical** **plan** **for** **revision** **of** **the** **femoral** **component** **in this** **patient?**
A. **Superior** **approach** **with** **trochanteric** **slide**
B. **Direct** **anterior** **approach** **with** **a** **chevron** **modification** **of** **the** **standard** **greater** **trochanteric osteotomy**
C. **Lateral** **approach** **with** **a** **partial** **greater** **trochanter** **osteotomy**
D. Posterolateral approach with an extended trochanteric osteotomy
**CORRECT ANSWER: D**
DISCUSSION:
Submit Answer
The patient’s radiographs demonstrate varus femoral remodeling around a broken cylindrical, distally fixed femoral stem. Proximal femoral remodeling around loose or fractured stems occurs in 21% to 42% of femoral revisions, based on the definitions outlined by Foran and associates. In definition 1, varus femoral remodeling occurs when the template falls within 2 mm of the endosteal cortex of the metaphysis on templating with a diaphyseal engaging stem. In definition 2, varus femoral remodeling = when the template crosses the lateral femoral cortex proximally. Based on the templating or drawing a line from the isthmus proximally along the lateral cortex, implantation of a straight stem would perforate the cortex proximally, indicating varus femoral remodeling. An extended trochanteric osteotomy would aid in the removal of the well-fixed distal segment and enable the safe insertion of the new femoral component. The approach is not the concern in this case, because extended trochanteric osteotomies have been described from the posterior and direct lateral approaches with excellent outcomes and union rates. The key is that the extended osteotomy is necessary and not a trochanteric slide or standard (shorter or incomplete trochanteric) osteotomy. These types would not provide access to the well-fixed distal stem, nor would they afford a straight tube in which to insert a new femoral component.
**Question 37**
**Figures** **1** **and** **2** **show** **the** **radiograph** **and** **CT** **obtained** **from** **a** **78-year-old** **woman** **who** **underwent** **right**
**total** **hip** **replacement** **in** **1995.** **She** **initially** **did** **well** **with** **no** **pain.** **She** **was** **last** **seen** **7** **years** **ago** **and** **was having** **mild** **hip** **pain** **at** **that** **time.** **She** **was** **found** **to** **have** **a** **supra-acetabular** **cyst** **on** **radiographs.** **She** **has had** **severe** **right** **hip** **pain** **for** **the** **past** **9** **months** **while** **using** **a** **walker** **for** **ambulation.** **The** **initial** **blood work** **reveals** **an** **estimated** **erythrocyte** **sedimentation** **rate** **of** **32** **mm/hr,** **a** **C-reactive** **protein** **level** **of** **0.5 mg/L,** **a** **serum** **cobalt** **level** **of** **0.4** **µg/L,** **and** **a** **serum** **chromium** **level** **of** **0.6** **µg/L.** **Right** **hip** **aspiration** **is performed,** **revealing** **a** **white** **blood** **cell** **count** **of** **139,** **52%** **neutrophils,** **and** **a** **negative** **leukocyte** **esterase test.** **What** **is** **the** **best** **next** **step?**
A. **Acetabular** **revision,** **with** **placement** **of** **a** **custom** **triflange** **acetabular** **component** **and** **femoral head** **exchange**
B. **Removal** **of** **the** **femoral** **and** **acetabular** **components** **and** **placement** **of** **an** **antibiotic** **spacer,** **with** **6 weeks** **of** **intravenous** **antibiotics**
C. **Head** **and** **liner** **exchange** **and** **retention** **of** **the** **femoral** **and** **acetabular** **implants** **with** **acetabular bone** **grafting**
D. Nonsurgical management with the initiation of bisphosphonates and referral to pain management
**CORRECT ANSWER: A**
DISCUSSION:
The hip replacement was performed in 1995, during the period when the previous generation of polyethylene was utilized. This polyethylene was subjected to irradiation in air, with subsequent oxidation and consequent osteolysis after implantation. The mechanism of osteolysis begins with the uptake of polyethylene particles by macrophages, which then initiate an inflammatory cascade and the release of osteolytic factors. This cycle continues, with eventual implant loosening and failure. The imaging shows significant osteolysis and raises concern for pelvic discontinuity and acetabular implant failure. The surgical treatment consists of acetabular reconstruction. In this patient, concern exists for discontinuity based on the substantial amount of bone loss and nonsupportive anterior and posterior columns. This scenario requires complex acetabular revision using a custom triflange device, distraction with a jumbo acetabular component, or placement of a porous metal cup/cage construct with augmentation. The laboratory values are not consistent with infection or failure due to metal debris.
**Question 38**
**Figure** **below** **shows** **a** **cross-table** **lateral** **radiograph** **obtained** **from** **a** **healthy** **56-year-old** **woman** **with**
**recurrent** **hip** **dislocations** **6** **months** **after** **total** **hip** **arthroplasty** **performed** **through** **a** **posterolateral approach.** **Each** **dislocation** **occurred** **when** **she** **was** **bending** **over** **to** **put** **her** **shoes** **on** **or** **pick** **something up.** **She** **has** **dislocated** **four** **times** **and** **has** **had** **no** **pain** **between** **dislocations.** **Abductor** **strength** **is** **5** **out** **of**
**5.** **The** **infection** **work-up** **is** **negative.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **of** **the** **acetabulum** **and** **evaluation** **of** **the** **femoral** **stem**
B. **Conversion** **to** **a** **constrained** **liner**
C. **Gluteus** **medius** **repair** **and** **application** **of** **a** **hip** **abductor** **brace**
D. Revision to an elevated acetabular polyethylene liner
**CORRECT ANSWER: A**
DISCUSSION:
The cross-table lateral radiograph shows that the patient has decreased acetabular anteversion. She is likely impinging on her cup in flexion and levering the femoral component posteriorly. Given a well-fixed and well-aligned femoral component and a negative infection work-up, the preferred treatment is to revise the acetabulum with a goal of increasing acetabular anteversion to avoid prosthetic impingement. Conversion to a constrained or elevated rim liner is suboptimal in this setting, because the problem is impingement. Indications for a constrained liner are neuromuscular compromise, abductor deficiency, or instability despite well-fixed and well-placed components. Given her 5 of 5 abductor strength, gluteus
medius repair is not indicated.
**Question 39**
Figures below show the radiographs obtained from a 75-year-old woman who underwent right total hip
arthroplasty in 2009. She did well until last month, when a right posterior hip dislocation occurred after she fell from her bed to the floor. Successful closed reduction was performed. She sustained two more posterior dislocations requiring closed reduction under anesthesia. The surgical report from the index arthroplasty notes a 54-mm monoblock acetabular component with a 28-mm inner diameter compression molded polyethylene and a high offset neck cementless stem with a +8-mm length, 28-mm head. What is the best next step?
A. Hip spica cast placement
B. Acetabular revision arthroplasty
C. Resection arthroplasty
D. Femoral head revision to a 28-mm diameter, +10-mm length head
**CORRECT ANSWER: B**
DISCUSSION:
This patient has demonstrated recurrent instability, and her current implants lack the modularity to upsize and improve the head-neck ratio and range to impingement. Given the monoblock acetabular component and a +7-mm neck length, the best option is revision to a large-diameter femoral head or dual-mobility component. Placement of a hip spica cast and resection arthroplasty are unreasonable. Revision to a longer ball length likely would not solve this recurrent instability pattern.
**Question 40**
**According** **to** **Musculoskeletal** **Infection** **Society** **(MSIS)** **guidelines,** **which** **set** **of** **patient** **laboratory** **study**
**results** **fits** **the** **definition** **of** **chronic** **prosthetic** **joint** **infection?**
A. **Erythrocyte** **sedimentation** **rate** **(ESR)** **50** **mm/hr,** **C-reactive** **protein** **(CRP)** **8** **mg/L,** **joint aspiration** **white** **blood** **cell** **(WBC)** **count** **542,** **62%** **neutrophils,** **and** **positive** **leukocyte** **esterase**
B. **ESR** **42** **mm/hr,** **CRP** **12** **mg/L,** **joint** **aspiration** **WBC** **count** **3,540,** **72%** **neutrophils,** **and** **positive leukocyte** **esterase**
C. **ESR** **20** **mm/hr,** **CRP** **15** **mg/L,** **joint** **aspiration** **WBC** **count** **4,135,** **54%** **neutrophils,** **and** **negative**
**leukocyte** **esterase**
D. **ESR** **25** **mm/hr,** **CRP** **7** **mg/L,** **joint** **aspiration** **WBC** **count** **252,** **82%** **neutrophils,** **and** **negative leukocyte** **esterase**
**CORRECT ANSWER: B**
DISCUSSION:
The MSIS definition of periprosthetic joint infection was updated in 2014 with two major and six minor criteria. The presence of one major criterion or three minor criteria is diagnostic for infection. The major criteria are two positive cultures with the same organism or a draining sinus tract. The current MSIS minor criteria are 1) an elevated ESR (more than 30 mm/hr) and CRP level (more than 10 mg/L), 2) an elevated synovial WBC count (more than 3,000 cells per/microliter), 3) an elevated synovial fluid polymorphonuclear count (more than 80%), 4) a positive histological analysis of periprosthetic tissue, and 5) a single positive culture.
**Question 41**
Figures below show the AP and lateral radiographs obtained from a 54-year-old woman who has worsening
groin pain 18 months after a primary left total hip arthroplasty. The pain is worst when climbing stairs, when rising from a seated position, and during resisted hip flexion. Her pain improved early after surgery but did
not completely resolve. Her C-reactive protein and erythrocyte sedimentation rate results of less than 1 mg/dL
and 10 mm/hr, respectively, were obtained in the office. What is the best next step?
A. MRI with MARS of the left hip
B. Revision of the left acetabular component
C. Intra-articular ultrasound-guided left hip injection
D. Physical therapy for the left hip
**CORRECT ANSWER: B**
DISCUSSION:
Iliopsoas impingement is a potential cause of persistent groin pain after a total hip arthroplasty. This patient’s history gives groin pain with resisted hip flexion and during activities that require this level of function. The radiographs depict an acetabular component with substantial retroversion. Typical options for the management of iliopsoas tendon impingement include injections, tenotomy, and acetabular revision. Recently, Chalmers and associates reported more predictable groin pain resolution with 8 mm or more of anterior acetabular component when overhang was revised. The radiographs clearly show more retroversion, with a cup prominence of more than 8 mm anteriorly. MRI with MARS could potentially help in the diagnosis of this impingement but would not help in management (option A). An ultrasound- guided injection would need to be administered into the iliopsoas tendon sheath to be of help and, in this case, would likely be performed for diagnostic purposes due to the extreme anterior overhang (option C). Option D would be useful for mild cases of iliopsoas impingement but likely would not help much in this more extreme case.
**Question 42**
**Figure** **1** **shows** **the** **radiograph** **obtained** **from** **a** **67-year-old** **man** **recently** **diagnosed** **with** **osteoarthritis,** **8**
**years** **after** **receiving** **a** **left** **metal-on-metal** **total** **hip** **arthroplasty** **(THA).** **The** **acetabular** **component** **has** **a modular** **cobalt** **alloy** **acetabular** **liner.** **The** **patient** **states** **that** **he** **did** **very** **well** **postoperatively,** **but** **for** **the last** **6** **months** **has** **noted** **worsening** **pain** **and** **swelling** **in** **his** **left** **hip.** **Serum** **metal** **ion** **testing** **reveals** **a chromium** **level** **of** **12.4** **ng/mL,** **compared** **with** **a** **normal** **level** **of** **less** **than** **0.3** **ng/mL,** **and** **a** **cobalt** **level of** **11.8** **ng/mL,** **compared** **with** **a** **normal** **level** **less** **than** **0.7** **ng/mL.** **An** **MRI** **with** **metal** **artefact** **reduction sequence** **(MARS)** **was** **performed** **and** **is** **shown** **in** **Figure** **2.** **What** **is** **the** **most** **appropriate** **management** **at this** **time?**
A. **Annual** **monitoring** **of** **serum** **metal** **ion** **levels**
B. **Repeated** **MRI** **with** **MARS** **in** **6** **months**
C. **Conversion** **of** **the** **THA** **to** **a** **cobalt** **alloy** **femoral** **head** **and** **polyethylene** **bearing**
D. **Conversion** **of** **the** **THA** **to** **a** **ceramic** **femoral** **head** **with** **an** **inner** **titanium** **sleeve** **and polyethylene** **bearing**
**CORRECT ANSWER: D**
DISCUSSION:
Metal-on-metal THA was initially introduced in the 1990s, with the proposed advantages of decreased wear and improved stability. However, catastrophic adverse local tissue reactions associated with their use has raised numerous concerns. The work-up of a patient with a prior metal-on-metal total hip arthroplasty involves a thorough history and physical examination; blood analysis, including the erythrocyte sedimentation rate, C-reactive protein, and metal ion levels; and secondary imaging, including ultrasonography, CT, and MRI. In a patient with clinical symptoms, elevated metal ion levels, and a large fluid collection seen on MRI, the most appropriate treatment would be removal of the metal-on-metal bearing. Given the presence of an adverse reaction involving cobalt and chromium, a revision ceramic head may be most appropriate to avoid the potential of trunnion-associated corrosion.
**Question 43**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **76-year-old** **woman** **with** **a** **painful** **total** **knee**
**arthroplasty.** **She** **describes** **an** **uneventful** **recovery** **with** **no** **wound-healing** **issues** **and** **was** **pain** **free** **for the** **first** **10** **years.** **Although** **reporting** **no** **trauma** **or** **inciting** **event,** **she** **now** **describes** **pain** **in** **the** **entire knee** **that** **is** **most** **severe** **with** **her** **first** **few** **steps.** **She** **has** **begun** **to** **notice** **night** **pain** **and,** **more** **recently, constant** **swelling.** **What** **is** **the** **most** **appropriate** **work-up** **at** **this** **time?**
A. **Knee** **aspiration** **with** **cell** **count/cultures,** **C-reactive** **protein** **(CRP)** **level,** **erythrocyte sedimentation** **rate** **(ESR),** **CT**
B. **Knee** **aspiration** **with** **cell** **count/cultures,** **CRP,** **ESR**
C. **Fresh-frozen** **specimen** **at** **the** **time** **of** **revision** **knee** **arthroplasty** **only**
D. Technetium-99m bone scan, knee aspiration with cell count/cultures
**CORRECT ANSWER: B**
DISCUSSION:
An evaluation of the painful total knee must be supported by an understanding of the potential etiologies of pain. They may include, aseptic loosening, infection, osteolysis, gap imbalance, referred pain, stiffness, and complex regional pain syndrome. In this case, the patient demonstrates start-up pain and had no prior history of infections. Her radiographs show subsidence of the tibia, indicating a loose prosthesis. Knowing that the prosthesis is already loose precludes the need for a bone scan. It is, however, important to rule out infection in this case; therefore, CRP and ESR testing is essential. Aspiration is also recommended when going into knee arthroplasty, and infection is a concern.
**Question 44**
**The** **direct** **anterior** **(Smith-Peterson)** **approach** **to** **hip** **arthroplasty** **is** **most** **commonly** **associated** **with**
**injury** **to** **what** **nerve?**
A. **Lateral** **femoral** **cutaneous**
B. **Sciatic**
C. **Pudendal**
D. Superior gluteal
**CORRECT ANSWER: A**
---
DISCUSSION:
Some authors have reported the incidence of lateral femoral cutaneous nerve neuropraxia following hip arthroplasty with the direct anterior approach to be near 80%, but resolution of the sensory deficits has been observed in most patients over time. Femoral nerve palsy has been reported to occur in .64% to 2.3% direct lateral (Hardinge) and anterolateral (Watson-Jones) approaches, and the superior gluteal nerve may be injured with proximal extension of the abductor muscular dissection. The posterior approach has been reported to be associated with sciatic nerve injury, especially in cases of dysplasia. Pudendal nerve injury has not been reported with the anterior, anterolateral, direct lateral, or posterior approaches to hip
arthroplasty. It has been reported following hip arthroscopy and the use of a traction table, however.
**Question 45**
**A** **55-year-old** **woman** **is** **referred** **for** **evaluation** **of** **a** **painful** **knee** **replacement.** **She** **underwent** **total** **knee**
**arthroplasty** **(TKA)** **more** **than** **1** **year** **ago** **without** **perioperative** **complications** **but** **has** **had** **consistent** **pain since** **the** **surgery.** **The** **patient’s** **preoperative** **radiographs** **and** **postoperative** **radiographs** **are** **shown** **in Figures** **below.** **Examination** **reveals** **medial** **laxity** **during** **valgus** **stress** **testing** **and** **range** **of** **motion** **of** **0° to** **70°.** **Her** **erythrocyte** **sedimentation** **rate** **and** **C-reactive** **protein** **level** **are** **normal.** **What** **is** **the** **best** **next step?**
A. **Unloader** **brace**
B. **Distal** **femoral** **osteotomy**
C. **Open** **arthrofibrosis** **debridement** **with** **lateral** **ligament** **balancing** **and** **polyethylene** **exchange**
D. Revision TKA of both the femoral and tibial components
**CORRECT ANSWER: D**
DISCUSSION:
The radiographs show substantial valgus malalignment of the femoral component, with lateral mechanical axis deviation. Clinically, by examination she displays instability and stiffness as a result. Revision knee replacement is appropriate and should consist of total revision to stemmed femoral and tibial components with a varus-valgus constrained insert, given the likely attenuation of the medial collateral ligament. Open debridement with ligament balancing and polyethylene exchange do not address the underlying cause and are inappropriate. Distal femoral osteotomy is not useful in the setting of previous total knee replacement.
Nonsurgical treatment with an unloader brace would be ineffective in correcting the alignment.
**Question 46**
**A** **45-year-old** **man** **has** **a** **draining** **sinus** **and** **recurrent** **infection** **of** **his** **right** **total** **knee** **arthroplasty.** **He** **has**
**had** **two** **prior** **revision** **surgeries** **after** **the** **primary** **procedure** **and** **three** **other** **surgeries** **before** **his** **initial replacement,** **including** **a** **proximal** **tibial** **osteotomy** **and** **subsequent** **hardware** **removal.** **On** **clinical examination,** **he** **has** **a** **draining** **sinus** **in** **the** **mid** **portion** **of** **his** **surgical** **scar** **and** **a** **range** **of** **motion** **of** **5°** **to**
**85°.** **AP** **and** **lateral** **radiographs** **of** **the** **right** **knee** **are** **shown** **in** **Figures** **below.** **During** **surgery,** **the** **femoral component** **is** **found** **to** **be** **grossly** **loose,** **but** **the** **tibial** **component** **is** **well** **fixed.** **What** **is** **the** **most appropriate** **extensile** **approach** **that** **would** **provide** **adequate** **exposure** **and** **aid** **in** **tibial** **component extraction?**
A. **Extended** **medial** **parapatellar** **approach**
B. **Quadriceps** **snip**
C. **Extended** **tibial** **tubercle** **osteotomy**
D. Medial epicondyle osteotomy
CORRECT ANSWER: C
DISCUSSION:
Extended tibial tubercle osteotomy is an extensile approach to revision total knee arthroplasty that affords excellent exposure and can facilitate removal of tibial sleeves and cones. This patient has had multiple surgeries, including a proximal tibial osteotomy, as well as poor range of motion, patella baja, and a well- fixed metaphyseal sleeve component. Classically, an extended tibial tubercle osteotomy provides outstanding exposure for component removal in the setting of prior high tibial osteotomy and patella baja. For this patient, it is important to recognize the patella baja on the radiographs, as well as the tibial sleeve. In many of these cases the osteotomy provides access to the sleeve to help with extraction, because the stem will not pull through the sleeve or detach from the tray to allow visualization of the sleeve. The extended medial parapatellar approach is just a long medial approach that typically yields good exposure
but would not help with the patella baja or extraction of the tibial sleeve. The quadriceps snip would give good exposure to the knee but would not aid in tibial component removal. Lastly, the medial epicondyle osteotomy could help with exposure and tensioning of the medial complex of the knee but would not help
with tibial component extraction.
**Question 47**
**A** **58-year-old** **woman** **underwent** **a** **left** **total** **knee** **arthroplasty** **6** **years** **ago.** **She** **initially** **did** **well** **after**
**surgery** **but** **sustained** **a** **fall** **2** **months** **ago** **while** **at** **work.** **She** **now** **describes** **left** **knee** **pain** **and** **instability and** **an** **inability** **to** **straighten** **her** **knee** **since** **the** **fall.** **She** **has** **been** **using** **a** **hinged** **knee** **brace,** **which provides** **partial** **support.** **On** **examination,** **she** **has** **passive** **range** **of** **motion** **of** **0°** **to** **115°** **and** **active** **range of** **motion** **of** **80°** **to** **-115°.** **Her** **radiographs** **are** **shown** **in** **Figures** **below.** **What** **is** **the** **best** **option** **for** **the restoration** **of** **her** **function?**
A. **Revision** **total** **knee** **arthroplasty** **with** **placement** **of** **a** **hinge** **constrained** **device**
B. **Patellar** **tendon** **repair** **with** **nonabsorbable** **suture** **and** **patellar** **resurfacing**
C. **Hinged** **knee** **brace** **with** **drop** **lock** **design** **to** **restore** **stability** **during** **ambulation**
D. **Extensor** **mechanism** **reconstruction** **using** **synthetic** **mesh** **or** **allograft**
**CORRECT ANSWER: D**
---
DISCUSSION:
The patient has an extensor mechanism disruption with patellar tendon rupture. This injury is treated with extensor mechanism reconstruction in the setting of previous total knee arthroplasty. There is a reported high failure rate with attempted repair. Revision to hinge knee arthroplasty would provide implant stability but would not restore the extensor mechanism. The patient is relatively young and is working, so reconstruction would offer better long-term function than a drop lock brace, which can be better used in low-functioning patients with this type of injury. Extensor mechanism reconstruction historically has been accomplished with allograft material, but a novel technique using synthetic mesh also has proved successful in treating this difficult problem.
**Question 48**
**Figures** **below** **show** **the** **radiographs,** **and** **the** **CT** **obtained** **from** **a** **58-year-old** **woman** **who** **underwent**
**cementless** **left** **total** **hip** **arthroplasty.** **Nine** **months** **after** **surgery,** **she** **continued** **to** **have** **groin** **pain** **when actively** **flexing** **her** **hip.** **She** **has** **trouble** **walking** **up** **stairs** **and** **getting** **out** **of** **her** **car.**
What is the most likely diagnosis?
A. **Trochanteric** **bursitis**
B. **Femoral** **component** **loosening**
C. **Iliopsoas** **tendonitis**
D. Acetabular component loosening
**CORRECT ANSWER: C**
---
DISCUSSION:
Groin pain after total hip replacement has a number of possible causes, and an exact diagnosis may remain elusive in some patients. Infection should be ruled out with laboratory studies and, if indicated, diagnostic aspiration of the hip joint. Implant loosening should be evaluated by plain radiograph and bone scan, if indicated. Synovitis resulting from wear debris should be considered in patients with polyethylene liners who experience late-onset symptoms or in any patient with a metal-on-metal bearing. This patient's symptoms are classic for iliopsoas tendonitis. Physical examination usually reveals pain and weakness with resisted hip flexion. A cross-table lateral radiograph and CT show that the anterior edge of the acetabulum protrudes beyond the anterior wall, thereby acting as a source of iliopsoas tendon irritation. In such cases, acetabular component revision and repositioning are indicated. Fluoroscope-guided iliopsoas cortisone injection can help to establish the diagnosis and relieve groin pain. If the acetabular component is well positioned, then iliopsoas tenotomy should be considered.
**Question 49**
**A** **72-year-old** **woman** **is** **scheduled** **to** **undergo** **right** **total** **hip** **arthroplasty.** **Her** **preoperative** **radiograph**
**is** **shown** **in** **Figure** **below.** **To** **avoid** **increasing** **this** **patient’s** **combined** **offset** **while** **maintaining** **her** **leg**
length, what is the most appropriate surgical plan?
A. **Lateralize** **the** **acetabular** **component,** **use** **a** **low** **offset** **femoral** **component,** **and** **make** **a** **shorter neck** **cut**
B. **Medialize** **the** **acetabular** **component,** **use** **a** **low** **offset** **femoral** **component,** **and** **make** **a** **longer neck** **cut**
C. **Lateralize** **the** **acetabular** **component,** **use** **a** **high** **offset** **femoral** **component,** **and** **make** **a** **shorter neck** **cut**
D. **Medialize** **the** **acetabular** **component,** **use** **a** **high** **offset** **femoral** **component,** **and** **make** **a** **longer neck** **cut**
**CORRECT ANSWER: B**
---
DISCUSSION:
The management of patients with proximal femoral deformity can be difficult. Appropriate implant selection and preoperative templating are critical. In this patient, it would be difficult to avoid increasing the combined offset by too much, which could contribute to the overtensioning of the soft tissues and trochanteric pain. By medializing the acetabular component (decreasing the combined offset), using a low offset femoral component or a cemented component placed more valgus (decreasing the combined offset), and making a longer neck cut (to avoid shortening of the lower extremity), restoration of the patient’s native offset and leg length can be achieved.
**Question 50**
Figures below demonstrate the radiographs obtained from a 56-year-old man with a 3-year history of right
groin pain. A comprehensive nonsurgical program has failed, and the patient would like to proceed with total hip arthroplasty. He is seen by a pain management specialist and is currently taking 40 mg of sustained-release morphine twice daily with oxycodone 10 mg 2 to 3 times a day for severe pain. What is the recommended course of action regarding his chronic narcotic use?
A. Increase his current opioid medication regimen prior to and after surgery as needed to control his pain.
B. Decrease his preoperative opioid use, and work with his pain management physician to decrease his postoperative opioid requirement.
C. Avoid using narcotics in the perioperative period to prevent overdose, and use acetaminophen only for pain control.
D. Stop all his opioids 5 days before surgery, and place the patient on a morphine pain control pump postoperatively with a basal rate.
**CORRECT ANSWER: B**
DISCUSSION:
Chronic opioid consumption prior to total joint arthroplasty has been associated with increased pain after surgery, increased opioid requirements, a slower recovery and longer hospital stay, and higher 90-day postoperative complications compared with patients not on chronic opioids preoperatively. Based on this information, Nguyen and associates performed a study in three patient groups that included 1) chronic opioid users who underwent no preoperative intervention, 2) chronic opioid users who were weaned down to 50% of their prior opioid regimen, and 3) patients who were not chronic opioid users. The authors found that the reduction of preoperative opioid use improved postoperative function, pain, and recovery and that the weaned group performed more like the opioid naive group than the chronic opioid user
group. Increasing opioid use prior to surgery in this patient would make it more difficult to control pain after surgery. Stopping all of his opioids just prior to surgery would place the patient at substantial risk for opioid withdrawal and is not recommended. Avoiding the use of all narcotics and using only acetaminophen postoperatively is very unlikely to provide appropriate pain relief in a chronic opioid user. The recommendation based on the provided literature is to decrease the patient's narcotic use prior to
surgery.
**Question 51**
**A** **72-year-old** **patient** **fell** **3** **weeks** **after** **undergoing** **a** **total** **hip** **arthroplasty** **using** **cementless** **fixation** **of**
**the** **femoral** **component.** **She** **sustained** **a** **comminuted** **Vancouver** **type** **B-2** **fracture** **with** **displacement** **of the** **calcar** **fragment.** **What** **is** **the** **best** **treatment** **option?**
A. **Revision** **using** **a** **proximal** **femoral** **replacement** **prosthesis**
B. **Revision** **using** **a** **diaphyseal** **engaging** **femoral** **prosthesis** **along** **with** **cerclage** **fixation**
C. **Open** **reduction** **internal** **fixation** **using** **a** **locking** **plate** **with** **strut** **graft**
D. Protected weight bearing with abduction bracing
**CORRECT ANSWER: B**
DISCUSSION:
The patient has an acute postoperative fracture of the proximal femur with subsidence. It is also common that the stem retroverts relative to the femur. It is most often seen in proximally porous coated stems within 90 days of surgery, one paper found it to occur 0.7% of the time in modern implants. There is always a debate whether this is a missed intraoperative fracture, or a new fracture that has resulted from an event of increased hoop stresses. Removal of the primary stem, placement of a diaphyseal engaging
stem (most frequently a tapered-fluted stem), and cabling of the fracture is the most successful treatment.
**Question 52**
**What** **is** **the** **most** **important** **preoperative** **factor** **predicting** **conversion** **to** **total** **hip** **arthroplasty** **after**
**arthroscopic** **surgery** **of** **the** **hip?**
A. **Age** **over** **60** **years**
B. **Morbid** **obesity**
C. **Diagnosis** **of** **osteoarthritis**
D. Tobacco use
**CORRECT ANSWER: B**
DISCUSSION:
---
The authors cited in the references examined large databases to determine the risk factors for conversion to total hip arthroplasty after arthroscopic surgery of the hip. In the study by Kester and associates, obesity had an odds ratio (OR) of 5.6 for conversion to hip arthroplasty, whereas age over 60 years had an OR of
3.4, osteoarthritis had an OR of 2.4, and tobacco use had an OR of 1.9.
**Question 53**
A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected
to undergo total hip arthroplasty. Her son recently learned he has factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
A. Type of surgery, age, and BMI
B. Type of surgery, hypercholesterolemia, and age
C. Age, BMI, and hypercholesterolemia
D. BMI, type of surgery, and hypercholesterolemia
**CORRECT ANSWER: A**
DISCUSSION:
Risk stratification is one of the most critical clinical evaluations to undertake before performing total joint arthroplasty. Many factors have been identified that increase the risk for venous thromboembolism (VTE) The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and
hormone replacement therapy. Hypercholesterolemia is not a risk factor for thromboembolic disease.
**Question 54**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **76-year-old** **woman** **who** **comes** **to** **the** **emergency**
**department** **after** **experiencing** **a** **fall.** **She** **is** **an** **unassisted** **community** **ambulator** **with** **a** **history** **of** **right** **hip pain.** **What** **is** **the** **most** **appropriate** **surgical** **treatment** **for** **this** **fracture?**
A. **Cemented** **unipolar** **hemiarthroplasty** B. **Cemented** **bipolar** **hemiarthroplasty** C. **Total** **hip** **replacement**
D. Open reduction and internal fixation
**CORRECT ANSWER: C**
DISCUSSION:
This patient has pre-existing right hip osteoarthritis. The most correct option for the treatment of this active patient is a right total hip arthroplasty. Hemiarthroplasty would not address the patient's pain from osteoarthritis, and open reduction and internal fixation would not fix the femoral head issue or the
osteoarthritis.
**Question 55**
**Figures** **below** **show** **the** **clinical** **photograph** **and** **radiograph** **obtained** **from** **a** **62-year-old** **man** **who** **has**
**deformity** **and** **pain** **1** **year** **after** **primary** **total** **hip** **arthroplasty.** **What** **is** **the** **reason** **for** **the** **observed deformity?**
A. **A** **Vancouver** **type** **B1** **fracture**
B. **Residual** **leg-length** **discrepancy**
C. **Loosening** **and** **subsidence** **of** **the** **femoral** **stem** **into** **anteversion**
D. Loosening and subsidence of the femoral stem into retroversion
**CORRECT ANSWER: D**
DISCUSSION:
Figure 1 reveals an external rotation deformity of the right lower extremity. This deformity can have numerous causes, including extra-articular deformity. Figure 2 reveals a loose, subsided femoral component. Femoral stems typically subside into retroversion due to proximal femoral biomechanics, which cause a compensatory external rotation deformity. The combined findings from both images suggest an external rotation deformity most likely related to subsidence into retroversion.
**Question 56**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **an** **86-year-old-woman** **who** **has** **had** **chronic** **left** **hip**
**pain** **for** **several** **years.** **She** **now** **uses** **a** **walker** **and** **a** **wheelchair** **for** **ambulation.** **She** **is** **medically** **healthy. What** **is** **the** **most** **appropriate** **surgical** **intervention?**
A. **Cemented** **left** **total** **hip** **arthroplasty** **(THA)**
B. **Cementless** **left** **THA** **with** **a** **proximally** **porous** **coated** **femoral** **stem**
C. **Hybrid** **left** **THA**
D. Cementless left THA with a diaphyseal engaging conical femoral stem
**CORRECT ANSWER: C**
DISCUSSION:
This 86-year-old woman has poor bone quality and osteoarthritis of the left hip. Her lateral radiograph confirms Dorr type C bone quality. A hybrid left THA with a cemented femoral stem would be the treatment of choice.
**Question 57**
**Figure** **below** **shows** **the** **radiograph** **obtained** **from** **a** **76-year-old** **woman** **who** **has** **sharp** **pain** **in** **her** **groin,**
**thigh,** **and** **buttocks** **that** **worsens** **with** **activity.** **She** **has** **been** **dealing** **with** **this** **pain** **for** **more** **than** **a** **year but** **is** **otherwise** **healthy.** **Recently,** **she** **has** **begun** **to** **notice** **night** **pain.** **The** **pain** **no** **longer** **responds** **to NSAIDs.** **She** **would** **like** **to** **be** **able** **to** **dance** **at** **her** **daughter's** **wedding** **in** **4** **months** **and** **wonders** **how** **best**
**to** **proceed.** **What** **is** **the** **best** **next** **step?**
A. **Radiograph-guided** **steroid** **injection** **followed** **by** **total** **hip** **arthroplasty** **6** **weeks** **later**
B. **Total** **hip** **arthroplasty**
C. **Physical** **therapy**
D. Referral back to her spine surgeon
**CORRECT ANSWER: C**
DISCUSSION:
The next best course of action is total hip arthroplasty. The patient is an otherwise healthy woman requesting pain relief and expresses a desire to be dancing in 4 months. She has had more than 6 months of symptoms that are classic hip osteoarthritis symptoms, with pain in the groin and thigh. Severe osteoarthritis is seen in the radiograph as well. NSAIDs are no longer working. Given the objective findings, the subjective reports, and the duration of symptoms, this patient merits surgery. Consideration for steroid injection is reasonable, but given her desire to be dancing in 4 months, an injection would increase her risk of infection if total hip arthroplasty were to be performed within 3 months of the
injection.
**Question 58**
**A** **68-year-old** **woman** **underwent** **an** **uncemented** **medial/lateral** **tapered** **femoral** **placement** **during** **a** **total**
**hip** **arthroplasty.** **The** **orthopaedic** **surgeon** **noticed** **a** **nondisplaced** **vertical** **fracture** **in** **the** **calcar** **region** **of the** **femoral** **neck** **during** **final** **implant** **insertion.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Removal** **of** **the** **press-fit** **implant** **and** **cementing** **of** **the** **same** **femoral** **stem**
B. **Removal** **of** **the** **uncemented** **femoral** **component** **and** **placement** **of** **a** **revision** **modular** **taper- fluted** **femoral** **stem**
C. **Removal** **of** **the** **implant,** **placement** **of** **a** **cerclage** **wire** **around** **the** **femoral** **neck** **above** **the** **lesser trochanter,** **and** **reinsertion** **of** **the** **implant**
D. Final seating of the uncemented femoral component without additional measures
**CORRECT ANSWER: C**
DISCUSSION:
The recognized treatment for a proximal periprosthetic fracture is to first identify the extent and then optimize the correction of the fracture. Several studies indicate that proximal cerclage wiring is adequate to create "barrel hoop" stability of the proximal femur. Braided cables offer superior stability compared with twisted wires or Luque wires. Finally, the appropriate postoperative treatment is protected
weight bearing for 6 weeks, with periodic radiographs taken at 2-week intervals. Other options such as
cementing the femoral stem and using a revision arthroplasty device are indicated for unstable fractures.
**Question 59**
**Injury** **to** **the** **popliteal** **artery** **during** **total** **knee** **arthroplasty** **(TKA)** **is** **most** **likely** **to** **occur** **when** **placing** **a**
**sharp** **retractor**
A. **directly** **posterior** **to** **the** **posterior** **cruciate** **ligament** **(PCL).**
B. **posteromedial** **to** **the** **PCL.**
C. **posterolateral** **to** **the** **PCL.**
D. in the posteromedial corner of the knee.
**CORRECT ANSWER: C**
DISCUSSION:
Vascular complications during TKA are rare but do occur. Traditionally, it was taught that the popliteal artery was situated posterior to the PCL; however, more recent anatomic dissections have demonstrated that this artery is usually located posterolateral to the PCL.
**Question 60**
**A** **70-year-old** **woman** **has** **a** **3-year** **history** **of** **gradually** **increasing** **diffuse** **and** **global** **right** **knee** **pain.** **Her**
**main** **issues** **are** **difficulty** **with** **stairs,** **stiffness** **with** **prolonged** **sitting,** **and** **swelling.** **She** **has** **taken** **NSAIDs and** **has** **received** **intra-articular** **steroid** **injections,** **all** **with** **decreasing** **efficacy.** **Her** **right** **knee** **examination reveals** **a** **range** **of** **motion** **of** **15°** **to** **80°** **with** **a** **fixed** **deformity** **to** **varus** **and** **valgus** **stress.** **Her** **symptoms are** **no** **longer** **manageable** **nonsurgically.** **Radiographs** **reveal** **a** **30-degree** **mechanical** **axis** **deformity. When** **using** **the** **measured** **resection** **technique** **during** **total** **knee** **arthroplasty** **(TKA),** **the** **best** **way** **to** **avoid femoral** **malrotation** **is** **to** **reference** **the**
A. **anteroposterior** **axis.**
B. **tibial** **intramedullary** **axis.**
C. **posterior** **condylar** **axis.**
D. femoral intramedullary axis.
**CORRECT ANSWER: A**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point, can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking
or instability, which is a common complication associated with primary TKA.
**Question 61**
**A** **70-year-old** **woman** **has** **a** **3-year** **history** **of** **gradually** **increasing** **diffuse** **and** **global** **right** **knee** **pain.** **Her**
**main** **issues** **are** **difficulty** **with** **stairs,** **stiffness** **with** **prolonged** **sitting,** **and** **swelling.** **She** **has** **taken** **NSAIDs and** **has** **received** **intra-articular** **steroid** **injections,** **all** **with** **decreasing** **efficacy.** **Her** **right** **knee** **examination reveals** **a** **range** **of** **motion** **of** **15°** **to** **80°** **with** **a** **fixed** **deformity** **to** **varus** **and** **valgus** **stress.** **Her** **symptoms are** **no** **longer** **manageable** **nonsurgically.** **Radiographs** **reveal** **a** **30-degree** **mechanical** **axis** **deformity. The** **deformity** **shown** **in** **Figure** **below** **is** **predominantly** **associated** **with**
A. **a** **hypoplastic** **lateral** **femoral** **condyle.**
B. **a** **contracted** **medial** **collateral** **ligament.**
C. **an** **excessive** **proximal** **tibial** **slope.**
D. trochlear dysplasia.
**CORRECT ANSWER: A**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point, can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking
or instability, which is a common complication associated with primary TKA.
**Question 62**
**Figures** **below** **show** **the** **radiographs,** **and** **the** **MRIs** **obtained** **from** **a** **32-year-old** **man** **with** **worsening** **left**
**knee** **pain.** **A** **3-foot** **hip-to-ankle** **radiograph** **shows** **a** **13-degree** **varus** **knee** **deformity.** **The** **patient sustained** **a** **major** **left** **knee** **injury** **5** **years** **ago** **and** **a** **confirmed** **complete** **anterior** **cruciate** **ligament** **(ACL) tear.** **He** **managed** **this** **injury** **nonsurgically** **with** **a** **functional** **brace** **but** **experienced** **worsening** **pain.** **He was** **seen** **by** **an** **orthopaedic** **surgeon** **18** **months** **ago,** **and** **a** **medial** **meniscus** **tear** **was** **diagnosed;** **the** **tear was** **treated** **with** **an** **arthroscopic** **partial** **medial** **meniscectomy.** **Since** **then,** **his** **knee** **has** **been** **giving** **way more** **often,** **and** **he** **no** **longer** **feels** **safe** **working** **on** **a** **pitched** **roof.** **The** **patient** **received** **6** **months** **of** **formal physical** **therapy** **and** **was** **fitted** **for** **a** **new** **functional** **ACL** **brace,** **but** **he** **still** **has** **pain** **and** **instability.** **He believes** **he** **has** **exhausted** **his** **nonsurgical** **options** **and** **would** **like** **to** **undergo** **surgery.** **What** **is** **the** **most appropriate** **treatment** **at** **this** **time?**
A. **ACL** **reconstruction** **and** **subsequent** **proximal** **tibial** **osteotomy**
B. **ACL** **reconstruction** **alone**
C. **Distal** **femoral** **osteotomy** **with** **simultaneous** **ACL** **reconstruction**
D. Proximal tibial osteotomy with subsequent ACL reconstruction
**CORRECT ANSWER: D**
DISCUSSION:
Proximal tibial osteotomy is the most appropriate intervention to correct varus malalignment and to reduce stress on the ACL. In some cases, proximal tibial osteotomy alone may address both pain and instability, but if instability persists, particularly in the setting in which instability can be dangerous, subsequent ACL reconstruction can further stabilize the knee with less stress on the graft after the correction of malalignment. Varus alignment places increased stress on the native or reconstructed ACL. ACL reconstruction should be performed only at the same time as or following proximal tibial osteotomy to correct alignment in the setting of varus malalignment. It is not appropriate to perform ACL reconstruction prior to proximal tibial osteotomy in this setting. Distal femoral osteotomy is not indicated to correct varus malalignment. Varus alignment places increased stress on the native or reconstructed ACL, and ACL
reconstruction alone is not indicated for this patient.
**Question 63**
**When** **balancing** **gaps** **in** **the** **coronal** **plane,** **what** **structure** **preferentially** **impacts** **the** **flexion** **space** **more**
**than** **the** **extension** **space?**
A. **Iliotibial** **band**
B. **Popliteus** **tendon**
C. **Lateral** **collateral** **ligament**
D. **Lateral** **head** **of** **the** **gastrocnemius**
**CORRECT ANSWER: B**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point,
can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking or instability, which is a common complication associated with primary TKA.
**Question 64**
**A** **45-year-old** **woman** **has** **severe** **anterior** **knee** **pain.** **Her** **radiographs** **indicate** **end-stage** **patellofemoral**
**compartment** **osteoarthritis.** **The** **tibiofemoral** **compartments** **are** **preserved.** **Extensive** **nonsurgical treatment** **has** **failed** **to** **provide** **relief,** **and** **she** **is** **offered** **patellofemoral** **arthroplasty** **(PFA).** **What** **is** **the most** **common** **long-term** **mode** **of** **failure** **for** **PFA** **using** **an** **implant** **with** **an** **onlay** **prosthesis** **design?**
A. **Infection**
B. **Patellar** **instability**
C. **Aseptic** **loosening**
D. Progression of tibiofemoral arthritis
**CORRECT ANSWER: D**
DISCUSSION:
Contemporary onlay-design trochlear prostheses in PFA replace the entire anterior trochlear surface. Previous inlay designs were inset within the native trochlea and carried a higher risk of catching and patellar instability, particularly in patients with trochlear dysplasia; they also generally have higher failure rates. The current most common mode of failure is progression of arthritis throughout the knee, in some series as high as 25% at 15 years. Aseptic loosening, particularly of cemented implants, is less common. Infection is an uncommon long-term complication. Patients considering PFA should be advised of the risk of arthritis progression. Many authors routinely obtain a preoperative MRI to assess the status of the tibiofemoral compartments.
**Question 65**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **79-year-old** **woman** **who** **has** **been** **experiencing**
**increasing** **tibial** **pain** **10** **years** **after** **undergoing** **revision** **total** **knee** **arthroplasty.** **No** **evidence** **of** **infection is** **seen.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Retain** **the** **components,** **and** **implant** **a** **tibial** **strut** **allograft.**
B. **Revise** **the** **tibial** **component** **with** **a** **metaphyseal** **cone** **and** **metaphyseal** **uncemented** **stem.**
C. **Revise** **the** **tibial** **component** **with** **a** **metaphyseal** **cone** **and** **a** **press-fit** **diaphyseal-engaging** **stem.**
D. Revise the tibial component with a long cemented diaphyseal-engaging stem.
**CORRECT ANSWER: C**
DISCUSSION:
---
Stems are available for cemented and press-fit implantation. To be effective, press-fit stems should engage the diaphysis, as shown in Figures 3 and 4. They also assist in obtaining correct limb alignment. Short metaphyseal-engaging stems are associated with failure rates that range between 16% and 29%. Cemented stems may be shorter than press-fit stems, because they do not have to engage the diaphysis. Short, fully cemented stems offer the advantage of metaphyseal fixation. Hybrid stem fixation makes use of the metaphysis for cement fixation with metaphyseal cones or sleeves and diaphyseal-engaging press-fit stems.
**Question 66**
**A** **70-year-old** **man** **reports** **symptomatic** **medial** **knee** **pain** **that** **has** **become** **progressively** **worse** **during**
**the** **past** **year.** **MRI** **reveals** **a** **complex,** **posterior** **horn** **medial** **meniscus** **tear** **with** **associated** **medial** **lateral and** **patellofemoral** **cartilage** **defects.** **Radiographs** **reveal** **medial** **joint** **space** **narrowing** **and** **osteophytes** **in the** **other** **compartments.** **What** **treatment** **is** **most** **likely** **to** **provide** **long-term,** **durable** **relief** **of** **symptoms?**
A. **High** **tibial** **osteotomy**
B. **Total** **knee** **replacement**
C. **Unicondylar** **knee** **replacement**
D. Arthroscopic partial meniscectomy
**CORRECT ANSWER: B**
DISCUSSION:
Total knee replacement is a well-established surgery for diffuse, symptomatic osteoarthritis of the knee joint, and its efficacy has been shown in many studies. According to the 2008 AAOS Clinical Practice Guideline, Treatment of Osteoarthritis of the Knee, arthroscopy in the setting of existing osteoarthritis is efficacious for relieving the signs and symptoms of a torn meniscus but not for osteoarthritis. Likewise, in young and active patients, clinical outcomes show improvement after realignment osteotomy for single- compartment osteoarthritis. Unicondylar knee replacement is not indicated for tricompartmental disease
of the knee.
**Question 67**
**A** **58-year-old** **man** **with** **insulin-dependent** **diabetes** **mellitus** **underwent** **primary** **total** **knee** **arthroplasty**
**(TKA).** **A** **full-thickness** **skin** **slough** **measuring** **3** **cm** **by** **4** **cm** **developed,** **with** **postsurgical** **exposure** **of the** **patellar** **tendon.** **No** **change** **is** **observed** **in** **the** **appearance** **of** **the** **wound** **after** **2** **weeks** **of** **wet-to-dry dressing** **changes.** **What** **is** **the** **best** **next** **treatment** **step** **for** **the** **soft-tissue** **defect?**
A. **Continued** **dressing** **changes**
B. **Split-thickness** **skin** **graft** C. **Full-thickness** **skin** **graft** D. **Local** **rotational** **flap**
**CORRECT ANSWER: D**
DISCUSSION:
If wound healing does not occur and deep soft tissues such as the patellar tendon are exposed following TKA, local rotational flap is the procedure of choice. The procedure should be performed relatively early after the recognition of a soft-tissue wound-healing problem. In the setting of TKA, the gastrocnemius muscle is an excellent source of flaps for wound coverage of the proximal tibia.
**Question 68**
**A** **77-year-old** **man** **who** **underwent** **right** **total** **knee** **replacement** **surgery** **2** **and** **a** **half** **years** **ago** **has** **had knee** **pain** **since** **surgery.** **The** **pain** **is** **diffuse,** **constant,** **and** **made** **worse** **with** **activity.** **He** **notes** **warmth and** **swelling** **in** **his** **knee.** **Examination** **shows** **a** **well-healed** **incision,** **no** **erythema,** **moderate** **warmth, synovitis,** **and** **an** **effusion.** **The** **knee** **is** **stable,** **and** **has** **an** **arc** **of** **flexion** **between** **3°** **and** **120°.** **Radiographs show** **well-fixed** **and** **well-aligned** **implants.** **What** **is** **the** **most** **appropriate** **initial** **treatment?**
A. **Knee** **aspiration** **for** **culture**
B. **CT** **of** **the** **knee** **to** **assess** **implant** **rotation**
C. **Indium-111** **leukocyte/technetium-99m** **sulfur** **colloid** **scan** **of** **the** **knee**
D. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) laboratory studies
**CORRECT ANSWER: D**
DISCUSSION:
This patient's history and physical findings are concerning for deep infection. Inflammatory markers, including ESR and CRP, should be obtained first. If the levels are elevated, knee aspiration should be performed for the synovial cell count and culture. A bone scan is not indicated in an initial investigation for deep infection; it is rarely helpful and is not cost effective. CT to assess implant rotation is an appropriate investigation for knee pain when the clinical scenario is not suspicious for a deep infection
and when infection has been excluded.
**Question 69**
**A** **61-year-old** **man** **with** **a** **body** **mass** **index** **of** **31** **had** **a** **6-month** **gradual** **onset** **of** **right** **medial** **knee** **pain.**
**Examination** **revealed** **a** **small** **effusion,** **stable** **ligaments,** **a** **normally** **tracking** **patella,** **and** **mild** **medial joint** **line** **tenderness.** **Standing** **radiographs** **show** **mild** **medial** **joint** **space** **narrowing.** **Effective** **treatment at** **this** **stage** **of** **early** **medial** **compartmental** **osteoarthritis** **includes**
A. **glucosamine** **1,500** **mg/day** **and** **chondroitin** **sulfate** **800** **mg/day.**
B. **weight** **loss** **through** **dietary** **management** **and** **low-impact** **aerobic** **exercises.**
C. **arthroscopic** **debridement** **and** **lavage.**
D. a valgus-directing brace.
**CORRECT ANSWER: B**
DISCUSSION:
According to the 2008 AAOS Clinical Practice Guideline, Treatment of Osteoarthritis of the Knee (Nonarthroplasty), level 1 evidence confirms that weight loss and exercise benefit patients with knee osteoarthritis. The other responses have either inclusive evidence (a valgus-directing brace) or no evidence to support their use (glucosamine 1,500 mg/day and chondroitin sulfate 800 mg/day as well as
arthroscopic debridement and lavage).
**Question 70**
**In** **patients** **with** **Crowe** **types** **III** **and** **IV** **developmental** **dysplasia** **of** **the** **hip** **with** **high** **hip** **centers,**
**acetabular** **reconstruction** **often** **requires** **lowering** **the** **acetabular** **component** **into** **the** **native** **acetabulum. In** **doing** **so,** **considerable** **risk** **for** **limb** **lengthening** **beyond** **4** **cm** **exists,** **making** **the** **hip** **difficult** **to** **reduce and** **raising** **the** **risk** **for** **nerve** **injury.** **Which** **technique** **is** **used** **to** **overcome** **this** **problem?**
A. **Subtrochanteric** **osteotomy** **with** **femoral** **shortening**
B. **An** **offset** **femoral** **component**
C. **A** **lateralized** **liner**
D. **Extended** **trochanteric** **osteotomy**
**CORRECT ANSWER: A**
DISCUSSION:
---
When substantial lengthening of a dysplastic hip will occur because a high dislocation is relocated into a considerably lower acetabulum, a femoral shortening may be necessary to reduce the hip and avoid a stretch injury to the sciatic nerve. No other choice specifically addresses the need for femoral shortening, and high offset stems and lateralized liners may exacerbate the problem if used alone and without femoral shortening.
**Question 71**
What factor is considered one of the early changes in osteoarthritic cartilage?
A. Decreased water content
B. Increased proteoglycan content
C. Decreased loading of the solid matrix
D. Increased cartilage tissue permeability
**CORRECT ANSWER: D**
DISCUSSION:
The normal regulation of a cartilage surface is a delicate balance of degradation and synthesis. When this normal regulation of the cartilage is disturbed, a proinflammatory state tips the cellular pathway in the direction of degradation. The proinflammatory state upregulates the production of cytokines and proteolytic enzymes, specifically matrix metalloproteinases. These enzymes attack the proteoglycan content of the cartilage, leading to an overall reduction in the proteoglycan content. This reduction in content leads to increased permeability of the cartilage substrate. With increased permeability, water is able to move into the cartilage itself, thereby increasing the overall water content within the cartilage in an arthritic state. Finally, because of the increased permeability and increased water content, the overall load or pressure placed on the underlying solid matrix is increased. Increased water content, decreased proteoglycan content, and an increased load on the solid matrix are typical of an osteoarthritic process within normal cartilage. Therefore, the only correct option is that the cartilage has an increased amount
of permeability in osteoarthritis.
**Question 72**
**A** **47-year-old** **obese** **man** **with** **a** **body** **mass** **index** **of** **42** **comes** **into** **the** **office** **with** **left** **knee** **pain** **1** **year**
**after** **undergoing** **an** **uncomplicated** **left** **medial** **unicompartmental** **knee** **arthroplasty** **(UKA).** **Radiographs show** **a** **loose** **tibial** **component** **in** **varus.** **What** **is** **the** **most** **appropriate** **next** **step** **to** **treat** **this** **failed construct?**
A. **Aspiration** **of** **joint** **fluid** **to** **obtain** **a** **cell** **count**
B. **Revision** **of** **the** **UKA** **using** **primary** **total** **knee** **arthroplasty** **(TKA)** **components**
C. **Revision** **of** **the** **UKA** **using** **a** **revision** **TKA** **with** **augments**
D. Procurement of the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) level
**CORRECT ANSWER: D**
DISCUSSION:
This patient likely is experiencing failure of the UKA secondary to poor patient selection. In this young, heavy man, the component likely loosened due to the ongoing varus alignment of the knee and his elevated
weight. Despite this likely scenario, the next step is determining whether an infection is the cause of his pain. Prior to obtaining an aspiration, the surgeon can order ESR and CRP studies to determine whether aspiration is warranted. If the laboratory studies are unremarkable, the surgeon likely can forgo the
aspiration and proceed to a revision TKA with possible augments on standby.
**Question 73**
Figure below shows the standing AP radiograph obtained from a 55-year-old man who has a 5-year history of
daily left knee medial joint line pain with weight-bearing activities. He denies night pain or symptoms of instability. On examination, his range of motion is 0° to 140°. He has a mild, fully correctable varus deformity and a negative Lachman test result. Nonsurgical treatment has failed. What is the UKA survivorship for a 55- year-old patient, compared with the survivorship for total knee arthroplasty?
A. Equal at 10 years B. Lower at 10 years C. Higher at 10 years
D. Not known when using a mobile-bearing UKA
**CORRECT ANSWER: B**
DISCUSSION:
A patient with medial compartment arthritis and a correctable varus deformity with no clinical or examination findings of knee instability most likely has an intact anterior cruciate ligament (ACL). The pattern of medial compartment osteoarthritis most commonly associated with an intact ACL is that of anteromedial osteoarthritis. An incompetent ACL is commonly associated with a fixed varus deformity and radiographic signs of posteromedial wear. An incompetent ACL is a relative contraindication to a mobile-bearing UKA. When evaluating patients for a mobile-bearing UKA, a stress radiograph aids the orthopaedic surgeon in determining the correction of the varus deformity and assessing the lateral compartment. An inability to fully correct the deformity or narrowing of the lateral compartment with valgus stress should influence the surgeon against UKA. Joint registries across the world have shown decreased survivorship associated with TKA and UKA in men compared with other age groups, but survivorship is lower for UKA than for TKA. No studies to date have shown any differences in survivorship between fixed-bearing and mobile-bearing UKAs. The complication that is unique to mobile-bearing UKA is bearing spinout, which occurs in less than 1% of mobile-bearing UKA procedures. In vivo and in vitro polyethylene wear in mobile-bearing UKA are low. Arthritis may progress
faster in patients with mobile-bearing UKAs than in those with fixed-bearing UKAs.
**Question 74**
**A** **57-year-old** **woman** **experiences** **pain** **1** **year** **after** **total** **knee** **arthroplasty** **(TKA).** **She** **reports** **sharp**
**anterior** **pain** **and** **a** **painful** **catching** **sensation** **that** **is** **aggravated** **by** **rising** **from** **a** **chair** **or** **climbing** **stairs. Physical** **examination** **reveals** **a** **mild** **effusion** **and** **a** **range** **of** **motion** **of** **2°** **to** **130°,** **with** **patellar** **crepitus.**
**The** **symptoms** **are** **reproduced** **by** **resisted** **knee** **extension.** **Radiographs** **show** **a** **well-aligned** **posterior- stabilized** **TKA** **without** **evidence** **of** **component** **loosening.** **What** **is** **the** **most** **likely** **cause** **of** **this** **patient's pain?**
A. **Patellar** **clunk** **syndrome**
B. **Flexion** **gap** **instability**
C. **Polyethylene** **wear**
D. Femoral component malrotation
**CORRECT ANSWER: A**
DISCUSSION:
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
**Question 75**
**In** **total** **knee** **arthroplasty,** **in** **vitro** **testing** **has** **shown** **that** **cross-linking** **can** **diminish** **the** **rate** **of**
**polyethylene** **wear** **by** **30%** **to** **80%.** **What** **other** **change** **in** **material** **properties** **is** **possible** **when polyethylene** **is** **highly** **cross-linked?**
A. **Increased** **ductility**
B. **Increased** **wettability**
C. **Diminished** **fatigue** **strength**
D. Decreased resistance to abrasive wear
**CORRECT ANSWER: C**
DISCUSSION:
The most important concern regarding highly cross-linked polyethylene relates to decreased mechanical properties. Cross-linking results in reduced ductility, tensile strength, and fatigue crack propagation resistance. These problems have not been shown to cause implant failure in the most recent clinical trials, but they remain the most important mechanical issues associated with current material processing methods.
**Question 76**
**A** **70-year-old** **woman** **who** **underwent** **total** **knee** **replacement** **18** **months** **ago** **has** **had** **3** **weeks** **of** **moderate**
**drainage** **from** **a** **previously** **healed** **wound.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Vacuum-assisted** **wound** **closure** **dressing**
B. **Intravenous** **antibiotics** **for** **6** **weeks,** **followed** **by** **long-term** **oral** **antibiotic** **administration**
C. **Irrigation** **and** **debridement,** **followed** **by** **polyethylene** **exchange**
D. Two-stage debridement and reconstruction
**CORRECT ANSWER: D**
DISCUSSION:
This situation represents a definitively and chronically infected knee replacement. Antibiotic therapy alone might suppress the infection but would not eradicate it. Debridement and polyethylene exchange would be appropriate treatment for an early postoperative infection. The treatment of choice is to perform a two-stage debridement and reconstruction. Although not among the listed choices, an aspiration or culture could be done presurgically and might help clinicians identify the best antibiotics to treat the condition. Antibiotic selection would not affect the need for the two-stage reconstruction, however.
**Question 77**
During a posterior cruciate ligament (PCL)-retaining total knee arthroplasty, a critical principle to remember
is to
A. accurately tension the PCL.
B. use bony resection to adjust the joint line.
C. maintain a small amount of residual deformity.
D. use intraoperative fluoroscopy to ensure femoral roll back.
**CORRECT ANSWER: A**
DISCUSSION:
Maintenance of the joint line and accurately tensioning the PCL are critical in the proper execution of a PCL-retaining total knee arthroplasty. Appropriate tension helps ensure femoral rollback and avoid stiffness or instability. Raising the joint line to help ensure full extension should be avoided in cruciate- retaining knees, because doing so creates an unfavorable kinematic environment. The three important principles of surgical technique needed to maintain appropriate tensioning of the PCL include 1) choosing the proper femur size to reproduce the native femoral anterior/posterior dimension, 2) reproducing the joint line by resecting as much tibia from the healthy side as will be replaced by the smallest thickness of the tibial component and, 3) ensuring that full extension is achieved by soft-tissue releases and not by taking additional distal femur, as may be done in a posterior stabilized approach. Another important principle is to re-create the natural degree of the patient’s posterior tibial slope to avoid tightness in
flexion.
**Question 78**
**Figures** **below** **depict** **the** **AP** **and** **lateral** **radiographs** **obtained** **from** **a** **64-year-old** **man** **with** **long-standing**
**right** **knee** **osteoarthritis** **and** **pain** **that** **is** **unresponsive** **to** **nonsurgical** **treatment.** **The** **patient** **undergoes navigated** **cruciate-retaining** **right** **total** **knee** **arthroplasty.** **After** **surgery,** **this** **patient** **continues** **to experience** **pain** **and** **swelling** **of** **the** **knee** **with** **recurrent** **effusions.** **He** **returns** **to** **the** **office** **reporting continued** **pain** **2** **years** **after** **surgery.** **He** **describes** **instability,** **particularly** **when** **descending** **stairs.** **On examination,** **range** **of** **motion** **of** **0°** **to** **120°** **is** **observed,** **with** **no** **extensor** **lag.** **Slope** **of** **the** **tibial** **component is** **7°.** **The** **knee** **is** **stable** **to** **varus** **and** **valgus** **stress** **in** **extension,** **but** **flexion** **instability** **is** **present** **in** **both the** **anterior-posterior** **direction** **and** **the** **varus-valgus** **direction.** **Bracing** **leads** **to** **a** **slight** **decrease** **in symptoms** **but** **is** **not** **well** **tolerated.** **Isokinetic** **testing** **demonstrates** **decreased** **knee** **extension** **velocity** **at**
**mid** **push.** **Radiographs** **demonstrate** **well-aligned** **and** **fixed** **knee** **implants.** **An** **infection** **work-up** **is negative.** **What** **is** **the** **most** **appropriate** **surgical** **intervention** **at** **this** **time?**
A. **Tibial** **polyethylene** **exchange**
B. **Revision** **of** **the** **femoral** **and** **tibial** **components** **and** **conversion** **to** **a** **posterior** **stabilized** **insert**
C. **Revision** **of** **the** **femoral** **and** **tibial** **components** **to** **a** **constrained** **rotating** **hinge** **prosthesis**
D. **Isolated** **femoral** **component** **revision** **and** **upsizing** **of** **the** **femoral** **implant** **with** **a** **new** **posterior cruciate** **ligament** **(PCL)-retaining** **polyethylene** **insert**
**CORRECT ANSWER: B**
DISCUSSION:
The patient’s symptoms at follow-up—pain, swelling, and difficulty descending stairs—suggest knee flexion instability. Considering his history, an incompetent PCL must be considered. Revision of the knee to a posterior stabilized or nonlinked constrained condylar implant (depending on the condition of the ligaments) likely is needed to address his symptoms. The difference in extension stability and flexion stability makes polyethylene exchange a poor option. A constrained rotating hinge design is not necessary. Repeat use of a PCL-retaining insert is not recommended. Tibial and femoral revision both are required. Correction of excessive slope will be attained with tibial revision, femoral component revision is required to convert to a PCL-substituting design. There is also an opportunity to increase posterior condylar offset if needed.
**Question 79**
**Figure** **below** **shows** **the** **standing** **AP** **radiograph** **obtained** **from** **a** **55-year-old** **man** **who** **has** **a** **5-year** **history**
**of** **daily** **left** **knee** **medial** **joint** **line** **pain** **with** **weight-bearing** **activities.** **He** **denies** **night** **pain** **or** **symptoms of** **instability.** **On** **examination,** **his** **range** **of** **motion** **is** **0°** **to** **140°.** **He** **has** **a** **mild,** **fully** **correctable** **varus deformity** **and** **a** **negative** **Lachman** **test** **result.** **Nonsurgical** **treatment** **has** **failed.** **Unicompartmental** **knee arthroplasty** **(UKA)** **is** **discussed** **with** **the** **patient.** **The** **most** **appropriate** **next** **radiographic** **evaluation should** **be**
**A.** **MRI** **of** **the** **left** **knee** **to** **evaluate** **the** **lateral** **compartment.**
**B.** **a** **CT** **arthrogram** **to** **evaluate** **the** **status** **of** **the** **medial** **and** **lateral** **meniscus. C.** **a** **stress** **radiograph** **to** **evaluate** **correction** **of** **the** **varus** **deformity.**
D. a sunrise view to determine the status of the patellofemoral joint.
**CORRECT ANSWER: C**
DISCUSSION:
A patient with medial compartment arthritis and a correctable varus deformity with no clinical or examination findings of knee instability most likely has an intact anterior cruciate ligament (ACL). The pattern of medial compartment osteoarthritis most commonly associated with an intact ACL is that of anteromedial osteoarthritis. An incompetent ACL is commonly associated with a fixed varus deformity and radiographic signs of posteromedial wear. An incompetent ACL is a relative contraindication to a mobile-bearing UKA. When evaluating patients for a mobile-bearing UKA, a stress radiograph aids the orthopaedic surgeon in determining the correction of the varus deformity and assessing the lateral compartment. An inability to fully correct the deformity or narrowing of the lateral compartment with valgus stress should influence the surgeon against UKA. Joint registries across the world have shown decreased survivorship associated with TKA and UKA in men compared with other age groups, but survivorship is lower for UKA than for TKA. No studies to date have shown any differences in survivorship between fixed-bearing and mobile-bearing UKAs. The complication that is unique to mobile-bearing UKA is bearing spinout, which occurs in less than 1% of mobile-bearing UKA procedures. In vivo and in vitro polyethylene wear in mobile-bearing UKA are low. Arthritis may progress
faster in patients with mobile-bearing UKAs than in those with fixed-bearing UKAs.
**Question 80**
**Compared** **with** **retention** **of** **the** **native** **patella** **in** **primary** **total** **knee** **arthroplasty,** **routine** **patellar**
**resurfacing** **is** **associated** **with**
A. **no** **patellar** **complications.**
B. **an** **increased** **occurrence** **of** **anterior** **knee** **pain.**
C. **a** **reduced** **patellar** **fracture** **rate.**
D. a reduced risk for revision surgery.
**CORRECT ANSWER: D**
DISCUSSION:
Despite concerns regarding fracture, osteonecrosis, and patellar clunk, the routine retention of the native patella during primary total knee replacement is associated with a 20% to 30% increased revision risk in
large joint registries. In addition, the retention of the native patella results in a 5.7% revision surgery rate
in patients with anterior knee pain.
**Question 81**
**A** **surgeon** **prepares** **a** **medial** **gastrocnemius** **rotational** **flap** **to** **cover** **a** **medial** **proximal** **tibia** **defect** **at** **the**
**time** **of** **revision** **knee** **replacement** **surgery.** **To** **optimize** **coverage,** **the** **surgeon** **must** **optimally** **mobilize which** **artery?**
A. **Profunda** **femoris** B. **Middle** **genicular** C. **Medial** **sural**
D. Inferior medial genicular
**CORRECT ANSWER: C**
DISCUSSION:
The medial sural arteries vascularize the gastrocnemius, plantaris, and soleus muscles proximally. These arteries arise from the popliteal artery. If this artery is not adequately mobilized, a gastrocnemius soleus flap can be devascularized.
**Question 82**
Figures below represent the radiographs obtained from a 37-year-old man with severe right knee pain. He has
a history of prior tibial osteotomy for adolescent tibia vara but notes residual bowing of his legs. On examination, he is 5'8" tall and weighs 322 pounds. He has a waddling gait with a bilateral varus thrust and
20° varus deformity of both legs. His right knee range of motion is 0° to 120° with a fixed varus deformity. What is the best next step?
A. Total knee arthroplasty with standard components
B. Correction of tibial deformity with osteotomy and nonsurgical management of the osteoarthritis
C. Arthrodesis with a long antegrade nail
D. Total knee arthroplasty with a constrained device
**CORRECT ANSWER: D**
DISCUSSION:
This patient has severe, uncorrectable varus deformity and pain from end-stage osteoarthritis secondary to prior adolescent tibia vara. Although he is young to consider arthroplasty, this option is likely to give him the most functional limb, compared with arthrodesis with a long antegrade nail. During arthroplasty surgery, his knee will likely require extensive medial release to achieve anatomic limb alignment. Standard components in total knee arthroplasty likely would result in lateral instability, so this option is
not the best answer. The best choice is total knee arthroplasty with a constrained device, which adds
constraint to the knee to provide balance.
**Question 83**
**An** **85-year-old** **obese** **woman** **has** **left** **knee** **pain.** **She** **had** **surgery** **5** **years** **ago** **for** **a** **patellar** **nonunion** **after**
**total** **knee** **arthroplasty** **that** **was** **complicated** **by** **infection,** **which** **was** **treated** **with** **implant** **removal** **and patellectomy.** **She** **has** **not** **been** **ambulatory** **since** **then.** **She** **states** **she** **is** **no** **longer** **on** **antibiotics.** **She** **has moderate** **pain,** **but** **her** **primary** **problem** **is** **instability** **of** **the** **knee.** **She** **has** **a** **40°** **extensor** **lag.** **Darkening of** **the** **skin** **is** **present** **distal** **to** **the** **incision** **consistent** **with** **venous** **stasis** **changes.** **The** **erythrocyte sedimentation** **rate** **is** **12** **mm/h** **(reference** **range** **0** **to** **20** **mm/h)** **and** **her** **C-reactive** **protein** **level** **is** **1.0** **mg/L**
**(reference** **range** **0.08** **to** **3.1** **mg/L).** **Left** **knee** **aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **800** **and** **20%**
**neutrophils.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **total** **knee** **arthroplasty** **with** **primary** **quadriceps** **tendon** **repair**
B. **Hinged** **knee** **arthroplasty** **with** **full** **extensor** **mechanism** **allograft**
C. **Arthrotomy** **with** **debridement** **and** **antegrade** **knee** **arthrodesis** **nailing**
D. Two-stage revision knee arthroplasty and quadriceps repair with Achilles allograft
**CORRECT ANSWER: C**
DISCUSSION:
This patient is elderly, obese, and nonambulatory and has a chronic quadriceps tendon rupture after infected total knee arthroplasty. Her potential for ambulation after revision total knee arthroplasty is very low. Primary repair of the tendon is unlikely to be successful, even with augmentation, so revision total knee arthroplasty with primary quadriceps tendon repair and two-stage revision knee arthroplasty and quadricep repair with Achilles allograft are not the best management techniques. Extensor mechanism allograft could be done but would have a high failure rate in a patient of this size. No sign of infection is seen, based on laboratory studies, so a two-stage procedure is not necessary. The best management although not optimal, would be treatment in a drop-lock brace. Arthrodesis is also an option, but would have a high complication rate, and in a patient that is nonambulatory, a fused knee would be increasingly
difficult with activities of daily living and mobility.
**Question 84**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **53-year-old** **man** **who** **has** **had** **swelling** **in** **his** **right**
**knee** **for** **2** **years,** **with** **minimal** **pain.** **He** **did** **not** **note** **an** **injury** **to** **the** **knee** **but** **has** **been** **unable** **to ambulate** **without** **crutches** **during** **this** **period.** **His** **past** **history** **is** **unremarkable,** **and** **he** **denies** **a** **history**
**of** **diabetes** **or** **back** **problems.** **The** **social** **history** **reveals** **that** **he** **emigrated** **from** **China,** **and** **he** **works** **at** **a desk** **job.** **Physical** **examination** **shows** **a** **healthy** **man** **in** **no** **acute** **distress.** **Range** **of** **motion** **of** **the** **right knee** **is** **5°** **to** **120°** **actively** **and** **0°** **to** **120°** **passively,** **without** **pain.** **Sensation** **is** **decreased** **on** **the** **bottom of** **both** **feet,** **but** **otherwise** **the** **neurologic** **examination** **is** **unremarkable.** **Laboratory** **testing** **reveals** **a positive** **rapid** **plasma** **reagin** **(RPR)** **test.** **What** **is** **the** **best** **next** **step?**
A. **Open** **reduction** **and** **internal** **fixation**
B. **Hinged** **total** **knee** **arthroplasty**
C. **Arthrodesis** **using** **an** **intramedullary** **nail**
D. Irrigation and debridement with spacer placement
**CORRECT ANSWER: B**
DISCUSSION:
This patient has a neuropathic knee caused by neurosyphilis, as shown by the joint destruction on the radiographs, with a lack of pain and a positive RPR test. He has a low-demand job and would be best treated with a hinged knee arthroplasty to provide stability for his knee.
**Question 85**
**At** **the** **time** **of** **revision** **knee** **arthroplasty,** **a** **surgeon** **performs** **a** **rectus** **snip** **to** **gain** **exposure** **to** **the** **knee.**
**When** **compared** **with** **a** **standard** **parapatellar** **approach,** **what** **is** **the** **expected** **outcome?**
A. **Improvement** **in** **range** **of** **motion**
B. **Reduction** **in** **range** **of** **motion**
C. **Increase** **in** **extensor** **mechanism** **lag**
D. No differences in motion and strength
**CORRECT ANSWER: D**
DISCUSSION:
Rectus snip during total knee arthroplasty has no effect on motion or strength at long-term follow-up. It has not been associated with extensor mechanism lag.
**Question 86**
**Hip** **pain** **of** **1-month** **duration** **has** **developed** **in** **a** **72-year-old** **man** **with** **a** **previous** **total** **hip** **arthroplasty.**
**He** **underwent** **dental** **work** **6** **weeks** **ago.** **Aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **more** **than** **6,000 cells/μL** **(reference** **range** **4,500** **to** **11,000** **cells/μL)** **and** **the** **presence** **of** **gram-positive** **cocci** **in** **clusters** **on Gram** **stain.** **The** **orthopaedic** **surgeon** **recommends** **urgent** **debridement** **and** **irrigation.** **Fixation** **of** **the components** **is** **judged** **to** **be** **stable,** **and** **the** **surgeon** **elects** **to** **retain** **the** **implants.** **The** **patient** **has** **a** **final culture** **that** **reveals** **methicillin-resistant** _Staphylococcus aureus_**(MRSA).** **If** **the** **attending** **physician recommends** **the** **two-stage** **protocol,** **including** **the** **use** **of** **an** **antibiotic-cement** **spacer,** **what** **is** **the** **most likely** **prognosis** **for** **this** **patient?**
A. **Better** **functional** **outcome** **than** **that** **associated** **with** **infections** **from** **sensitive** **organisms**
B. **Same** **functional** **outcome** **as** **that** **associated** **with** **infections** **from** **sensitive** **organisms**
C. **Same** **prognosis** **for** **eradication** **of** **infection** **as** **that** **associated** **with** **infections** **from** **sensitive organisms**
D. **Poorer** **prognosis** **for** **eradication** **of** **infection** **than** **that** **associated** **with** **infection** **from** **sensitive organisms**
**CORRECT ANSWER: D**
DISCUSSION:
The patient has a late infection of at least 4 weeks symptomatic duration that most likely is hematogenous in etiology. This infection is not an acute hematogenous infection that can successfully be treated with irrigation and debridement. Retention of the implants with debridement and irrigation alone has been associated with a poor prognosis. In a recent study, the success rate was only 44% in a series of 104 patients at a mean 5.7-year follow-up. In one study of 50 infections attributable to MRSA or methicillin- resistant _Staphylococcus epidermidis_ organisms treated with a two-stage protocol, the failure rate was
21%. Patients who experienced successful infection treatment had lower functional outcome measures using the Western Ontario and McMaster Universities Osteoarthritis Index, the University of California
Los Angeles Activity Score, and the 12-item Oxford Knee Score, however.
**Question 87**
**An** **80-year-old** **African** **American** **woman** **who** **lives** **in** **a** **large** **city** **is** **scheduled** **for** **total** **hip** **arthroplasty**
**to** **address** **primary** **osteoarthritis.** **Part** **of** **the** **presurgical** **protocol** **includes** **nasal** **swab** **screening** **to** **assess for** **methicillin-resistant** _Staphylococcus aureus_**(MRSA)** **colonization.** **Which** **demographic** **factor** **places this** **patient** **at** **highest** **risk** **for** **a** **positive** **result?**
A. **Gender**
B. **Age**
C. **Race**
D. Environment
**CORRECT ANSWER: C**
DISCUSSION:
Demographic factors are associated with increased risk for MRSA colonization, so it is important to identify vulnerable patients. Female gender and advanced age reduce the risk for colonization, whereas African American race increases this risk. Urban environments do not influence MRSA colonization.
**Question 88**
**Hip** **pain** **of** **1-month** **duration** **has** **developed** **in** **a** **72-year-old** **man** **with** **a** **previous** **total** **hip** **arthroplasty. He** **underwent** **dental** **work** **6** **weeks** **ago.** **Aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **more** **than** **6,000**
**cells/μL** **(reference** **range** **4,500** **to** **11,000** **cells/μL)** **and** **the** **presence** **of** **gram-positive** **cocci** **in** **clusters** **on Gram** **stain.** **The** **orthopaedic** **surgeon** **recommends** **urgent** **debridement** **and** **irrigation.** **Fixation** **of** **the components** **is** **judged** **to** **be** **stable,** **and** **the** **surgeon** **elects** **to** **retain** **the** **implants.** **What** **is** **this** **patient's**
**prognosis** **for** **infection** **resolution?**
A. **Good** **because** **it** **is** **a** **gram-positive** **organism**
B. **Good** **because** **it** **is** **an** **acute** **infection**
C. **Poor** **because** **it** **is** **a** **gram-positive** **organism**
D. Poor because it is a late infection
**CORRECT ANSWER: D**
DISCUSSION:
---
The patient has a late infection of at least 4 weeks symptomatic duration that most likely is hematogenous in etiology. This infection is not an acute hematogenous infection that can successfully be treated with irrigation and debridement. Retention of the implants with debridement and irrigation alone has been associated with a poor prognosis. In a recent study, the success rate was only 44% in a series of 104 patients at a mean 5.7-year follow-up. In one study of 50 infections attributable to MRSA or methicillin- resistant _Staphylococcus epidermidis_ organisms treated with a two-stage protocol, the failure rate was
21%. Patients who experienced successful infection treatment had lower functional outcome measures using the Western Ontario and McMaster Universities Osteoarthritis Index, the University of California Los Angeles Activity Score, and the 12-item Oxford Knee Score, however.
**Question 89**
**A** **40-year-old** **man** **with** **a** **history** **of** **Legg-Calve-Perthes** **disease** **underwent** **a** **right** **hip** **resurfacing** **3** **years**
**ago** **with** **no** **perioperative** **complications.** **Hip** **pain** **has** **developed** **gradually** **during** **the** **last** **4** **months. Radiographs** **show** **no** **evidence** **of** **fixation** **loosening** **or** **any** **adverse** **changes** **at** **the** **femoral** **neck.** **No periarticular** **osteolysis** **is** **evident.** **What** **is** **the** **most** **appropriate** **management** **of** **this** **condition?**
A. **Continue** **to** **observe** **with** **repeat** **radiographs** **in** **6** **months** B. **Fluoroscopic-guided** **iliopsoas** **tendon** **cortisone** **injection** C. **Hip** **aspiration**
D. Serum cobalt and chromium levels and metal-reduction MRI scan
**CORRECT ANSWER: D**
DISCUSSION:
Controversy persists over what exactly is the best approach to managing patients with metal-on-metal (MOM) hip arthroplasties. All patients with painful MOM hip arthroplasties should be examined for fixation loosening, wear/osteolysis, and infection—no differently than patients without MOM hip arthroplasties. It is recommended to obtain serum trace element levels. If the levels are high, cross- sectional imaging should be obtained to determine whether any pseudotumor or tissue necrosis is present around the hip arthroplasty. Hip aspiration should be considered if concern for infection exists. Adverse tissue reaction has been identified to occur around MOM hip arthroplasties. The predominant histologic feature is tissue necrosis with infiltration of lymphocytes and plasma cells.
**Question 90**
In patients undergoing elective hip or knee arthroplasty who are not at elevated risk (beyond the risk associated
with the surgery) for venous thromboembolism or bleeding, using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism was assigned what grade of recommendation by the 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty?
A. Strong
B. Moderate
C. Limited
D. Inconclusive
**CORRECT ANSWER: B**
DISCUSSION:
Using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism in patients undergoing elective hip or knee arthroplasty who are not at elevated risk beyond that of the surgery itself for venous thromboembolism or bleeding was given a moderate grade of
recommendation in the 2011 AAOS Clinical Practice Guideline referenced above.
**Question 91**
**A** **40-year-old** **man** **with** **a** **history** **of** **Legg-Calve-Perthes** **disease** **underwent** **a** **right** **hip** **resurfacing** **3** **years**
**ago** **with** **no** **perioperative** **complications.** **Hip** **pain** **has** **developed** **gradually** **during** **the** **last** **4** **months. Radiographs** **show** **no** **evidence** **of** **fixation** **loosening** **or** **any** **adverse** **changes** **at** **the** **femoral** **neck.** **No periarticular** **osteolysis** **is** **evident.** **A** **large** **intra-articular** **and** **intrapelvic** **pseudotumor** **has** **developed. What** **predominant** **histological** **feature(s)** **is/are** **present** **in** **such** **a** **lesion?**
A. **Polymorphonuclear** **leukocytes**
B. **Extracellular** **metal-wear** **debris**
C. **Cement** **particles** **within** **the** **macrophages**
D. Lymphocytes and plasma cells
**CORRECT ANSWER: D**
DISCUSSION:
Controversy persists over what exactly is the best approach to managing patients with metal-on-metal (MOM) hip arthroplasties. All patients with painful MOM hip arthroplasties should be examined for fixation loosening, wear/osteolysis, and infection—no differently than patients without MOM hip arthroplasties. It is recommended to obtain serum trace element levels. If the levels are high, cross- sectional imaging should be obtained to determine whether any pseudotumor or tissue necrosis is present around the hip arthroplasty. Hip aspiration should be considered if concern for infection exists. Adverse tissue reaction has been identified to occur around MOM hip arthroplasties. The predominant histologic
feature is tissue necrosis with infiltration of lymphocytes and plasma cells.
**Question 92**
**A** **57-year-old** **woman** **experiences** **pain** **1** **year** **after** **total** **knee** **arthroplasty** **(TKA).** **She** **reports** **sharp**
**anterior** **pain** **and** **a** **painful** **catching** **sensation** **that** **is** **aggravated** **by** **rising** **from** **a** **chair** **or** **climbing** **stairs. Physical** **examination** **reveals** **a** **mild** **effusion** **and** **a** **range** **of** **motion** **of** **2°** **to** **130°,** **with** **patellar** **crepitus. The** **symptoms** **are** **reproduced** **by** **resisted** **knee** **extension.** **Radiographs** **show** **a** **well-aligned** **posterior- stabilized** **TKA** **without** **evidence** **of** **component** **loosening.** **What** **is** **the** **recommended** **treatment** **for** **this patient?**
A. **Physical** **therapy**
B. **Arthroscopic** **synovectomy**
C. **Tibial** **insert** **revision**
D. Femoral component revision
**CORRECT ANSWER: B**
DISCUSSION:
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor
mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
**Question 93**
Which modality has the broadest application for the reduction of postsurgical transfusion?
A. Regional anesthesia
B. Tranexamic acid (TXA) administration
C. Reduced transfusion trigger
D. Hypotensive anesthesia
**CORRECT ANSWER: B**
DISCUSSION:
TXA is easy to administer, inexpensive, and safe for virtually all patients. Multiple studies have demonstrated transfusion rates lower than 3% for total knee arthroplasty and lower than 10% for total hip arthroplasty. Regional and hypotensive anesthesia effectively reduce transfusion; however, they cannot be used in as wide a range of patients as can TXA. A reduced transfusion trigger must be considered along
with patient symptoms when determining the need for transfusion.
**Question 94**
**When** **do** **most** **symptomatic** **thromboembolic** **events** **occur** **after** **total** **joint** **arthroplasty?**
A. **On** **the** **day** **of** **surgery**
B. **Within** **the** **first** **week** **after** **surgery**
C. **Between** **1** **week** **and** **6** **weeks** **after** **surgery**
D. More than 3 months after surgery
**CORRECT ANSWER: C**
DISCUSSION:
Most clinical venous thromboembolism events occur between the second and sixth weeks after surgery. It is estimated that 10% of patients are readmitted to the hospital within the first 3 months after total hip or knee arthroplasties. Most pulmonary events on the day of surgery are related to fat embolism or cardiac events.
**Question 95**
**When** **comparing** **arthroscopic** **lavage** **and** **knee** **debridement** **with** **placebo** **in** **patients** **with** **chronic**
**symptomatic** **osteoarthritis,** **what** **outcome** **has** **been** **demonstrated?**
A. **Reliable** **and** **durable** **pain** **relief**
B. **No** **significant** **benefit** **for** **chronic** **osteoarthritis**
C. **Up** **to** **75%** **pain** **relief** **for** **2** **months,** **then** **variable** **response**
D. Three-month measurable pain relief, followed by recurrence
**CORRECT ANSWER: B**
DISCUSSION:
Excluding a diagnosis of meniscal tear, loose body, or mechanical derangement, treating knee osteoarthritis of indeterminate cause with arthroscopic lavage and debridement has been found to provide no discernable benefit to offset the risk of surgery. The effects of arthroscopy have not been clinically significant in the vast majority of patient-oriented outcomes measures for pain and function at multiple
times between 1 week and 2 years after surgery.
**Question 96**
**Figure** **below** **shows** **the** **abdominal** **radiograph** **obtained** **from** **a** **70-year-old** **woman** **who** **experiences**
**nausea** **and** **abdominal** **tightness** **48** **hours** **following** **left** **total** **knee** **arthroplasty** **performed** **under** **general anesthesia.** **She** **received** **24** **hours** **of** **cefazolin** **antibiotic** **prophylaxis** **and** **a** **patient-controlled** **analgesia narcotic** **pump** **for** **pain** **management.** **She** **has** **been** **receiving** **warfarin** **for** **thromboembolic** **prophylaxis. Her** **severe** **abdominal** **distension** **and** **markedly** **decreased** **bowel** **sounds** **are** **most** **likely** **secondary** **to** **the administration** **of**
A. **general** **anesthesia.**
B. **antibiotics.**
C. **warfarin.**
D. narcotics.
**CORRECT ANSWER: D**
DISCUSSION:
The radiograph reveals severe intestinal dilatation, which has occurred as the result of acute colonic pseudo-obstruction and is associated with excessive narcotic administration following total joint arthroplasty. Anesthetic type, antibiotic administration, and warfarin have not been associated with this obstruction. Electrolyte imbalances such as hypokalemia have been associated with postsurgical acute colonic pseudo-obstruction.
**Question 97**
**Venous** **thromboembolism** **may** **occur** **after** **total** **joint** **arthroplasty.** **The** **risk** **of** **this** **complication** **is**
**elevated** **in** **patients** **with**
A. **a** **BMI** **lower** **than** **30.**
B. **diabetes** **mellitus,** **with** **a** **hemoglobin** **A1c** **test** **result** **less** **than** **7.**
C. **tranexamic** **acid** **use.**
D. metabolic syndrome.
**CORRECT ANSWER: D**
DISCUSSION:
Obesity, a prior history of venous thromboembolism, and metabolic syndrome have all been associated with an increased risk of thromboembolism. A recent meta-analysis showed that diabetes had no significant relationship with venous thromboembolism following hip or knee arthroplasty. Tranexamic acid is an antifibrinolytic agent that has been shown to reduce blood loss substantially following hip and knee arthroplasty. It has also been shown to be safe in patients with severe medial comorbidities and a prior history of venous thromboembolism.
**Question 98**
**A** **70-year** **old** **woman** **undergoes** **revision** **total** **knee** **arthroplasty** **for** **tibial** **component** **aseptic** **loosening.**
**She** **is** **concerned** **about** **recurrent** **loosening,** **and** **tibial** **stem** **fixation** **options** **during** **revision** **are** **reviewed. Figure** **below** **displays** **a** **radiograph** **of** **the** **revision** **technique** **used** **for** **this** **patient.** **What** **is** **the** **incidence of** **intraoperative** **tibial** **shaft** **fracture** **that** **is** **associated** **with** **this** **type** **of** **revision** **surgery?**
A. **0%** **to** **1%** **with** **press-fit** **tibial** **stems** B. **3%** **to** **5%** **with** **press-fit** **tibial** **stems** C. **3%** **to** **5%** **with** **cemented** **tibial** **stems**
D. More than 5% with press-fit tibial stems
**CORRECT ANSWER: B**
DISCUSSION:
Using press-fit tibial stems during a hybrid revision total knee arthroplasty is associated with a 3% to 5% incidence of intraoperative tibial shaft fracture. Diaphyseal fixation of press-fit stems has the advantage of setting component alignment, dispersing forces on the proximal tibia, and offers excellent clinical results. The disadvantages include proximal and distal tibia anatomic mismatch and tibial shaft fracture. Cipriano and associates reported a tibial shaft fracture incidence of 4.9% in a series of 420 consecutive
knee revisions. All fractures healed with nonsurgical management, and none led to implant loosening. In this patient, it is important to recognize on the radiograph that this technique is a hybrid method of revision total knee arthroplasty, with cementation along the tibial tray and metaphysis and with press-fit fixation of the diaphyseal engaging stem. Then, it is important to know the risk and management of intraoperative diaphyseal tibial fractures. Cemented tibial stems are associated with a low rate of intraoperative fracture, because the implant is typically undersized to allow for an appropriate cement mantle. Option C is incorrect, because this revision is not cemented. Option A underestimates the incidence of fracture,
whereas D overestimates the rate of fracture.
**Question 99**
Figures below depict the radiographs obtained from a 60-year-old man with instability and pain 1 year after
primary right total knee arthroplasty. He states that he had surgery on two occasions for a tendon rupture that was repaired with sutures but that his knee popped again, and now the leg is unable to hold his weight. On examination, he is in no acute distress. His height is 6'3", and he weighs 240 pounds. He is ambulatory with crutches. Range of motion of the right knee is 50° to 120° actively and 0° to 120° passively. More than 10° of varus/valgus laxity and more than 5 mm of anteroposterior drawer are present. A palpable defect is observed in the tissue just proximal to the patella. The incision is well healed. The erythrocyte sedimentation rate is 46 mm/h (reference range 0 to 20 mm/h) and the C-reactive protein level is 2.04 mg/L (reference range 0.08 to
3.1 mg/L). Aspiration of the right knee reveals hazy yellow fluid with a white blood cell count of 120 and 1%
neutrophils. No growth of organisms is seen on routine culture. What is the best next step?
A. Revision total knee arthroplasty with extensor mechanism allograft
B. Revision total knee arthroplasty with liner change and primary quadriceps repair
C. Resection knee arthroplasty and arthrodesis with antegrade nail
D. Two-stage revision total knee arthroplasty with extensor mechanism allograft
**CORRECT ANSWER: A**
DISCUSSION:
This patient has a chronic quadriceps tendon rupture after total knee arthroplasty. Two previous primary repair attempts have failed, which is not surprising based on the poor results of primary repair reported in the literature. The patient also has an unstable knee and will require revision of some or all of the prosthesis to achieve a stable knee. Revision total knee arthroplasty with extensor mechanism allograft allows an allograft reconstruction of the ruptured quadriceps tendon. The other option is to utilize a synthetic mesh extensor mechanism reconstruction. These are likely to have the best result in this situation. Revision total knee arthroplasty with liner change and primary quadriceps repair is not the best form of management, because it involves a third attempt at primary tendon repair, which will likely fail again. Resection knee arthroplasty and arthrodesis with antegrade nail is a possible option but is not the best, because it would likely make driving and other daily activities difficult. Two-stage revision total
knee arthroplasty with extensor mechanism allograft is not the best option because the laboratory results
show no signs of infection, so a single-stage procedure is preferred.
**Question 100**
**A** **60-year-old** **man** **who** **underwent** **left** **partial** **knee** **arthroplasty** **6** **months** **earlier** **was** **doing** **well** **until** **he**
**experienced** **left** **knee** **pain** **and** **swelling** **for** **4** **weeks** **following** **a** **dental** **procedure.** **The** **left** **knee** **aspirate was** **bloody,** **with** **a** **white** **blood** **cell** **count** **of** **8,000** **and** **70%** **neutrophils.** **Culture** **grew** **group** **B Streptococcus** **(**_Granulicatella adiacens_**),** **and** **serologies** **were** **elevated,** **with** **an** **erythrocyte** **sedimentation rate** **of** **55** **mm/h** **(reference** **range:** **0** **to** **20** **mm/h)** **and** **a** **C-reactive** **protein** **level** **of** **24** **mg/L** **(reference range:** **0.08** **to** **3.1** **mg/L).** **What** **is** **the** **best** **next** **step?**
A. **Arthroscopic** **debridement**
B. **Two-stage** **total** **knee** **revision** **arthroplasty**
C. **Resection** **arthroplasty** **without** **an** **antibiotic** **impregnated** **cement** **spacer**
D. Knee fusion
**CORRECT ANSWER: B**
DISCUSSION:
This complication is best addressed with either a single-stage or two-stage total knee arthroplasty. A recent report suggests that a single-stage arthroplasty can be effective, although many surgeons would perform a two-stage procedure with an articulating or static spacer. Arthroscopic would be non-effective, especially given 4 weeks of symptoms. Resection arthroplasty without a spacer would leave an unstable _and poorly functioning extremity. Knee fusion should be used as a salvage procedure._
**_[**ERGUIDE MCQ 401-450**](http://hutaifortho.com/640)_**
---
**_[**ORTHOPEDICS HYPERGUIDE MCQ 351-400**](http://hutaifortho.com/639)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 301-350**](http://hutaifortho.com/638)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 251-300**](http://hutaifortho.com/637)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 201-250**](http://hutaifortho.com/636)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 151-200**](http://hutaifortho.com/635)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 101-150**](http://hutaifortho.com/634)_**
**_[**FREE Orthopedics MCQS 2022 51-100**](http://hutaifortho.com/633)_**
**_[**Orthopedics Hyperguide MCQ 1-50**](http://hutaifortho.com/631)_**
**below show** **the** **radiographs,** **and** **the** **CT** **obtained** **from** **a** **58-year-old** **woman** **who** **underwent**
**cementless** **left** **total** **hip** **arthroplasty.** **Nine** **months** **after** **surgery,** **she** **continued** **to** **have** **groin** **pain** **when actively** **flexing** **her** **hip.** **She** **has** **trouble** **walking** **up** **stairs** **and** **getting** **out** **of** **her** **car.** **A** **course** **of appropriate** **nonsurgical** **treatment** **failed.** **What** **is** **the** **next** **step** **in** **definitive** **treatment?**
A. **Acetabular** **component** **revision**
B. **Femoral** **component** **revision**
C. **Acetabular** **liner** **exchange**
D. Trochanteric bursectomy
Submit Answer
**Question 9**
**What** **factor** **is** **associated** **with** **a** **high** **risk** **of** **developing** **pseudotumors** **after** **metal-on-metal** **hip**
**resurfacing?**
A. **Large-diameter** **components**
B. **Age** **40** **or** **older** **for** **men**
C. **Age** **40** **or** **younger** **for** **women**
D. Diagnosis of primary osteoarthritis
**CORRECT ANSWER: C DISCUSSION:**
The recent experience of a large clinical cohort revealed the most likely risk factors as being female gender, age younger than 40, small components, and a diagnosis of hip dysplasia causing osteoarthritis. Failure was least likely among men and after procedures involving larger components. These data have prompted some authors to caution against using metal-on-metal hip resurfacing in women and to primarily target candidates who are men younger than age 50. Small components may be more prone to failure because of malpositioning and edge loading, which have been noted to be more common in dysplasia cases.
**Question 10**
**Figures** **below** **show** **the** **radiographs,** **MRI,** **and** **MR** **arthrogram** **obtained** **from** **a** **25-year-old** **collegiate**
**soccer** **player** **who** **has** **new-onset** **left** **groin** **pain.** **He** **played** **competitive** **soccer** **from** **a** **young** **age** **and** **has competed** **or** **practiced** **5** **to** **6** **times** **per** **week** **since** **the** **age** **of** **10.** **He** **denies** **any** **specific** **hip** **injury** **that necessitated** **treatment,** **but** **his** **trainer** **contends** **that** **he** **had** **a** **groin** **pull.** **He** **reports** **groin** **pain** **with** **passive flexion** **and** **internal** **rotation** **of** **the** **left** **hip,** **and** **his** **hip** **has** **less** **internal** **rotation** **than** **his** **asymptomatic right** **hip.** **He** **is** **otherwise** **healthy.When** **counseling** **patients** **who** **have** **a** **cam** **deformity,** **the** **orthopaedic surgeon** **should** **note** **that**
A. **osteoarthritis** **of** **the** **hip** **is** **likely** **to** **occur** **later** **in** **life.**
B. **correction** **prevents** **later** **development** **of** **osteoarthritis.**
C. **most** **acetabular** **tears** **are** **symptomatic,** **and** **surgical** **treatment** **will** **be** **necessary.**
D. this is an inherited deformity.
**CORRECT ANSWER: A DISCUSSION:**
Multiple studies have confirmed that cam or pincer anatomy is commonly present in asymptomatic hips. According to a large systematic review, cam deformities are present in approximately one-third of asymptomatic hips in young adults, and the proportion is higher than 50% in the subgroup of athletes. Ganz and associates proposed that femoral acetabular impingement is the root cause of osteoarthritis in most nontraumatic, nondysplastic hips, and functional improvement with surgical correction of the deformity has been demonstrated. Despite the link between cam deformity and hip osteoarthritis, a corresponding link between the correction of the deformity and prevention of osteoarthritis has never been proven. The results of cam deformity correction, typically including repair of the degenerative labral tear, are much poorer when substantial joint space loss is present. A typical joint space cutoff of 2 mm or less is used to recommend against hip preservation surgery.
**Question 11**
Figures below demonstrate the radiographs obtained from a 63-year-old man who had right total hip
arthroplasty (THA) 4 months ago. Progressive stiffness began 2 months after surgery, and he now reports pain only after prolonged physical activity. His examination reveals a normal gait and painless range of motion with flexion of 70°, extension of 0°, internal rotation of 20°, external rotation of 20°, abduction of 10°, and adduction of 10°. His erythrocyte sedimentation rate and C-reactive protein level are within defined limits. Physical therapy has produced no benefit. What is the most appropriate next step?
A. 25 mg of indomethacin 3 times daily for 6 weeks
B. 1 dose of irradiation at 800 Gy
C. Surgical excision of heterotopic ossification (HO)
D. Reevaluation in 6 months
**CORRECT ANSWER: D DISCUSSION:**
This patient presents with HO 4 months after undergoing THA. Symptomatic HO may complicate nearly
7% of primary THA cases. Improvement in pain is expected within 6 months, and most patients will not need surgical treatment. Surgical excision may be warranted for symptomatic patients after full maturation of the HO, usually 6 to 18 months after the surgery. Patients can be followed with repeated serum alkaline phosphatase levels, which are elevated initially and should return to normal upon maturation of the HO. Alternatively, a bone scan can show decreased activity after the HO has matured. Twenty-five milligrams of indomethacin 3 times daily for 6 weeks or 1 dose of irradiation at 700 to 800 Gy is effective in the prevention of HO but not for the treatment of established HO.
**Question 12**
**A** **55-year-old** **man** **is** **about** **to** **undergo** **right** **total** **hip** **arthroplasty.** **A** **preoperative** **AP** **pelvis** **radiograph**
**is** **shown** **in** **Figure** **below.** **The** **final** **acetabular** **component** **and** **polyethylene** **liner** **are** **implanted.** **With** **the broach** **in** **place,** **the** **surgeon** **trials** **a** **standard** **offset** **neck** **and** **neutral** **length** **femoral** **head.** **The** **leg** **lengths are** **approximately** **equal,** **but** **the** **hip** **is** **unstable.** **What** **is** **the** **best** **next** **step?**
A. **Choosing** **a** **longer** **femoral** **head** **and** **accepting** **a** **resulting** **leg-length** **discrepancy**
B. **Trialing** **a** **lateralized** **femoral** **neck** **component**
C. **Removing** **the** **acetabular** **liner** **and** **implanting** **an** **offset** **liner** **instead**
D. Performing a trochanteric osteotomy with advancement
**CORRECT ANSWER: B**
DISCUSSION:
The radiograph shows that this patient has a high offset varus femoral morphology of both hips. Preoperative templating would identify this, and the surgeon should choose an implant system that has extended offset options to help match the native anatomy and biomechanics and minimize the risk of instability. Trialing a high offset neck, rather than a standard offset neck, is the next most appropriate step. Depending on the design of the implant system, this step can be accomplished by direct medialization of the femoral head, which would not affect leg length, or by lowering the neck angle, which would affect the leg length and would require a longer femoral head, because the leg lengths had previously been equal. Placement of a longer femoral head would likely improve hip stability but would also make the leg length uneven, which is a common cause of dissatisfaction after total hip arthroplasty. An offset acetabular liner also increases the leg length and does not correct the issue, which is on the femoral side. Trochanteric
advancement is sometimes used as a treatment for instability but would be inappropriate as the next step in this setting.
**Question 13**
**During** **total** **hip** **arthroplasty,** **what** **characteristic** **of** **irradiated** **(10** **Mrad)** **and** **subsequently** **melted** **highly**
**cross-linked** **polyethylene** **should** **provide** **a** **more** **wear-resistant** **construct** **than** **traditional** **gamma- irradiated** **(2.5-4** **Mrad)-in-air** **polyethylene** **mated** **with** **the** **same** **head?**
A. **Resistance** **to** **adhesive** **wear** B. **Resistance** **to** **abrasive** **wear** C. **Resistance** **to** **fatigue** **wear**
D. Resistance to creep
**CORRECT ANSWER: B**
DISCUSSION:
Highly cross-linked polyethylene makes material resistant to adhesive wear. Abrasive wear from third bodies does not decrease wear. The fatigue strength of such material is inferior to that of traditional polyethylene, and its resistance to creep is the same, if not lower, than that of traditional polyethylene.
**Question 14**
**When** **compared** **with** **patients** **having** **a** **body** **mass** **index** **(BMI)** **lower** **than** **35,** **patients** **with** **a** **BMI**
**above** **40** **who** **undergo** **primary** **total** **hip** **arthroplasty** **(THA)** **and** **total** **knee** **arthroplasty** **(TKA)** **are likely** **to** **have**
A. **smaller** **incisions.**
B. **more** **wound** **complications.**
C. **fewer** **30-day** **and** **90-day** **readmissions.**
D. lower rates of patient satisfaction.
**CORRECT ANSWER: B**
DISCUSSION:
The obesity epidemic is increasing, and the number of patients with a BMI higher than 35 undergoing THA and TKA also is growing. Controversy exists over the optimal BMI cutoff and the ability to perform joint replacements safely in patients who are morbidly obese. Several clinical series and national database analyses have shown that morbidly obese patients undergoing THA or TKA are at increased risk for wound complications as well as 30-day and 90-day readmissions. These patients’ incisions are typically larger because of the size of the soft-tissue envelope. Although the clinical scores following successful THA or TKA often are lower than the scores of controls, the overall changes in clinical function and satisfaction are equivalent in nonobese and obese patients.
**Question 15**
**An** **otherwise** **healthy** **76-year-old** **woman** **has** **pain** **2** **years** **after** **total** **hip** **arthroplasty.** **The** **clinical**
**photograph** **in** **Figures** **below** **demonstrates** **her** **skin** **envelope,** **and** **associated** **radiograph.** **Her** **C-reactive protein** **level** **is** **normal,** **and** **her** **erythrocyte** **sedimentation** **rate** **is** **mildly** **elevated.** **The** **white** **blood** **cell count** **is** **normal.** **Hip** **aspiration** **attempted** **under** **fluoroscopy** **generates** **no** **fluid.** **What** **is** **the** **best** **definitive treatment?**
A. **Repeat** **left** **hip** **aspiration**
B. **Initiation** **of** **a** **wound** **care** **consult** **and** **oral** **antibiotics**
C. **Irrigation** **and** **debridement** **with** **closure** **of** **the** **dehisced** **wound,** **performance** **of** **a** **liner** **exchange, and** **administration** **of** **intravenous** **antibiotics**
D. **Debridement** **of** **the** **wound,** **explant** **of** **the** **total** **hip,** **placement** **of** **a** **spacer,** **and** **administration** **of**
intravenous antibiotics
**CORRECT ANSWER: D**
DISCUSSION:
This patient clearly has a chronically infected total hip arthroplasty, indicated by the open, draining sinus, as well as trochanteric bone resorption on radiographs, and two years of pain. Recently, specific guidelines have been published to better help the clinician define infection. Repeating the hip aspiration is unnecessary, because infection is already evident. Initiating a wound care consult would not address the underlying infection. The determination whether to retain the components or perform a two-stage exchange is based more on the acuity of infection. In this particular case, the patient is chronically infected. Irrigation and debridement with a liner exchange and retention of the components are reserved for the acute setting.
**Question 16**
Figures below show the radiographs obtained from a 90-year-old woman who is seen in the emergency
department after a fall from a height. She has right hip and thigh pain and is unable to bear weight. Based on this patient's history and imaging, what is the best next step?
A. Hip revision and implantation of a proximal femoral replacement
B. Hip revision and implantation of a tapered fluted stem
C. Open reduction and internal fixation with a locked plate and allograft struts
D. Erythrocyte sedimentation rate and C-reactive protein laboratory studies
**CORRECT ANSWER: D**
DISCUSSION:
Periprosthetic fracture is the third most common reason (after loosening and infection) for revision surgery after total hip arthroplasty (THA). Late periprosthetic fracture risk is 0.4% to 1.1% after primary
THA and 2.1% to 4% after revision THA. Risk factors for periprosthetic fracture include age over 70 years, decreasing bone mass, and loosening of implants and osteolysis. The risk of concomitant infection in the presence of a periprosthetic fracture is 11%, according to Chevillotte and associates. Obtaining presurgical aspiration or intrasurgical tissue for culture is recommended if concomitant infection is suspected.
**Question 17**
**Figure** **below** **shows** **the** **radiograph** **obtained** **from** **a** **73-year-old** **woman** **who** **returns** **status** **post** **total** **hip**
**arthroplasty** **14** **years** **earlier.** **She** **denies** **pain** **and** **has** **no** **discomfort** **on** **examination.** **She** **then** **undergoes revision** **total** **hip** **arthroplasty** **with** **head** **and** **liner** **exchange** **and** **bone** **grafting.** **After** **a** **physical** **therapy session** **two** **days** **after** **surgical** **intervention,** **she** **develops** **inability** **to** **dorsiflex** **the** **foot** **while** **she** **is** **sitting in** **a** **chair.** **The** **initial** **treatment** **should** **consist** **of**
A. **lying** **completely** **supine** **in** **bed.**
B. **remaining** **seated** **and** **placing** **the** **postsurgical** **leg** **on** **a** **stool.**
C. **transferring** **back** **to** **bed** **with** **the** **head** **of** **the** **bed** **no** **lower** **than** **60°.**
D. transferring back to bed with the head of the bed level and the surgical knee flexed.
**CORRECT ANSWER: D**
DISCUSSION:
Gamma irradiation produces free radicals. Although these free radicals can form cross-links with other polyethylene chains, the free radicals can also form a bond with oxygen, resulting in early oxidation. Gamma irradiation in air produces the highest risk for oxidized polyethylene, resulting in the highest risk for wear, delamination, and subsequent osteolysis. This patient demonstrates severe periarticular osteolysis. When she is asymptomatic, this suggests the acetabular and femoral components remain well fixed to the bone. Consequently, she can be treated by removing the wear generator (polyethylene exchange), along with bone grafting of the osteolytic defect. Considering the extensive amount of osteolysis indefinite observation would not be appropriate. A foot drop develops 2 days after surgery. As a result, it can be assumed that the nerve was not injured directly during the surgical procedure. Although MRI or CT may be indicated to identify an evolving hematoma, the immediate concern is to minimize pressure on the sciatic nerve. Tension on the nerve can be reduced by flexing the surgical knee and positioning the bed flat.
**Question 18**
**Figure** **below** **depicts** **the** **radiograph** **obtained** **from** **a** **52-year-old** **woman** **who** **has** **leg-length** **inequality**
**and** **chronic,** **activity-related** **buttock** **discomfort.** **This** **problem** **has** **been** **lifelong,** **but** **it** **is** **getting** **worse and** **increasingly** **causing** **back** **pain.** **What** **is** **the** **best** **current** **technique** **for** **total** **hip** **arthroplasty?**
A. **High** **hip** **center**
B. **Anatomic** **hip** **center** **with** **trochanteric** **osteotomy** **and** **progressive** **femoral** **shortening**
C. **Anatomic** **hip** **center** **with** **subtrochanteric** **shortening** **osteotomy**
D. Iliofemoral lengthening followed by an anatomic hip center
**CORRECT ANSWER: C**
DISCUSSION:
A high hip center is not recommended for Crowe type IV hips because of the lack of acetabular bone and altered hip biomechanics. An anatomic center is a better option but necessitates a technique to address the tight soft-tissue envelope. A trochanteric osteotomy with progressive femoral shortening has been described but can be prone to trochanter nonunion. Iliofemoral lengthening prior to surgery has been described but may not be tolerated by all patients. A shortening subtrochanteric osteotomy avoids trochanter nonunion and allows adjustment of femoral anteversion. Fixation of the osteotomy can include a stem with distal rotational control, plate fixation, a step versus oblique cut, or strut grafts.
**Question 19**
**Figures** **1** **through** **5** **show** **the** **radiographs,** **MRI,** **and** **MR** **arthrogram** **obtained** **from** **a** **25-year-old**
**collegiate** **soccer** **player** **who** **has** **new-onset** **left** **groin** **pain.** **He** **played** **competitive** **soccer** **from** **a** **young age** **and** **has** **competed** **or** **practiced** **5** **to** **6** **times** **per** **week** **since** **the** **age** **of** **10.** **He** **denies** **any** **specific** **hip injury** **that** **necessitated** **treatment,** **but** **his** **trainer** **contends** **that** **he** **had** **a** **groin** **pull.** **He** **reports** **groin** **pain**
**with** **passive** **flexion** **and** **internal** **rotation** **of** **the** **left** **hip,** **and** **his** **hip** **has** **less** **internal** **rotation** **than** **his asymptomatic** **right** **hip.** **He** **is** **otherwise** **healthy.** **Approximately** **what** **percentage** **of** **asymptomatic**
**athletes** **have** **cam** **deformities** **of** **the** **hip?**
A. **5%**
B. **10%**
C. **25%**
D. At least 50%
**CORRECT ANSWER: D**
DISCUSSION:
Multiple studies have confirmed that cam or pincer anatomy is commonly present in asymptomatic hips. According to a large systematic review, cam deformities are present in approximately one-third of asymptomatic hips in young adults, and the proportion is higher than 50% in the subgroup of athletes. Ganz and associates proposed that femoral acetabular impingement is the root cause of osteoarthritis in most nontraumatic, nondysplastic hips, and functional improvement with surgical correction of the deformity has been demonstrated. Despite the link between cam deformity and hip osteoarthritis, a corresponding link between the correction of the deformity and prevention of osteoarthritis has never been proven. The results of cam deformity correction, typically including repair of the degenerative labral tear, are much poorer when substantial joint space loss is present. A typical joint space cutoff of 2 mm or less is used to recommend against hip preservation surgery.
**Question 20**
**A** **59-year-old** **active** **woman** **undergoes** **elective** **total** **hip** **replacement** **in** **which** **a** **posterior** **approach** **is**
**used.** **She** **has** **minimal** **pain** **and** **is** **discharged** **to** **home** **2** **days** **after** **surgery.** **Four** **weeks** **later,** **she dislocates** **her** **hip** **while** **shaving** **her** **legs.** **She** **undergoes** **a** **closed** **reduction** **in** **the** **emergency** **department. Postreduction** **radiographs** **show** **a** **reduced** **hip** **with** **well-fixed** **components** **in** **satisfactory** **alignment. What** **is** **the** **most** **appropriate** **management** **of** **this** **condition** **from** **this** **point** **forward?**
A. **Observation** **and** **patient** **education** **regarding** **hip** **dislocation** **precautions**
B. **Revision** **to** **a** **larger-diameter** **femoral** **head**
C. **Revision** **to** **a** **constrained** **acetabular** **component**
D. Application of a hip orthosis for 3 months
**CORRECT ANSWER: A**
DISCUSSION:
First-time early dislocations are often treated successfully without revision surgery, especially when no component malalignment is present. In this clinical scenario, it appears the patient would benefit from better education about dislocation precautions. Hip orthoses are of questionable benefit unless the patient is cognitively impaired. Revision surgery can be successful but is usually reserved for patients with recurrent dislocations.
**Question 21**
A 62-year-old active man returns for routine follow-up 16 years after hip replacement. He has no hip pain.
Radiographs reveal a well-circumscribed osteolytic lesion around a single acetabular screw. All hip components are perfectly positioned. Comparison radiographs obtained 6 months later show an increase in the size of the osteolytic lesion. CT depicts a well-described lesion that is 3 cm at its largest diameter and is localized around one screw hole with an eccentric femoral head. What treatment is appropriate, assuming that well-fixed cementless total hip components are in place?
A. Revision of the polyethylene liner, removal of the screw, and debridement of the osteolytic lesion with or without bone grafting
B. Revision of the acetabular component to a newer design without screws
C. Removal of the screw, revision of the polyethylene liner, and stem cell injection into the lytic lesion
D. Removal of the offending screw from the metal socket and placement of a new polyethylene liner in the existing socket
**CORRECT ANSWER: A**
DISCUSSION:
Given a well-fixed acetabular metal shell and a localized osteolytic lesion, good outcomes can be expected from liner revision in this clinical scenario with retention of the metal socket, assuming no damage to the components or other unexpected findings arise during revision surgery. Here, complete cup revision is not warranted, considering the appropriate implant position. Beaulé and associates reviewed 83 consecutive patients (90 hips) in whom a well-fixed acetabular component was retained in a clinical scenario such as the one described. No hip showed recurrence or expansion of periacetabular osteolytic lesions. If the metal cup is unstable, acetabular component revision may be indicated.
**Question 22**
Figure 1 shows the radiograph obtained from a 78-year-old woman who has a recent history of increasing
thigh pain 12 years after undergoing total hip arthroplasty. Figure 2 depicts the radiograph obtained after she fell and was unable to ambulate. What is the most appropriate treatment?
A. Application of a femoral cable plate
B. Application of cerclage-wired double allograft femoral struts
C. Femoral revision with an uncemented long stem
D. Femoral revision with a cemented long-stem prosthesis
**CORRECT ANSWER: C**
DISCUSSION:
The surgical treatment of periprosthetic fractures of total hip replacement with a loose implant and progressive bone loss is associated with a high complication rate. The recent literature would favor the use of long "Wagner-type" stems, which have a long distal taper that may optimally engage the remaining femoral shaft isthmus. Plating options are problematic, because the intramedullary stem limits the ability to use screws with the plate. Using long distally fixed stems circumvents this problem by enhancing
fracture healing and creating a long-term prosthetic solution in these most difficult cases.
**Question 23**
**Early** **postoperative** **infections** **following** **primary** **total** **hip** **arthroplasty** **are** **most** **likely** **caused** **by** **which**
**organism?**
A. **Staphylococcus** **epidermidis**
B. **Streptococcus** **viridans**
C. **Propionibacterium** **acnes**
D. Staphylococcus aureus
**CORRECT ANSWER: D**
DISCUSSION:
_S aureus_ is the most common organism cultured in early (fewer than 4 weeks postoperative) periprosthetic infections. Methicillin-resistant _S aureus_ is becoming a more common pathogen in certain patient populations. B hemolytic _Streptococcus_ and some gram-negative infections can also be found in early postoperative infections. _S epidermidis_ , _S viridans_ , and _P acnes_ are more commonly found in late (more
than 4 weeks postoperative) infections.
**Question 24**
**A** **healthy,** **active** **72-year-old** **man** **trips** **and** **falls,** **landing** **on** **his** **left** **hip** **10** **weeks** **after** **an** **uncomplicated**
**left** **primary** **uncemented** **total** **hip** **replacement.** **A** **radiograph** **taken** **6** **weeks** **after** **surgery** **and** **before** **the fall** **is** **shown** **in** **Figure** **1.** **A** **radiograph** **taken** **after** **the** **fall** **is** **shown** **in** **Figure** **2.** **He** **is** **unable** **to** **bear weight** **and** **is** **brought** **to** **the** **emergency** **department.** **Examination** **reveals** **a** **slightly** **shortened** **left** **lower extremity** **and** **some** **mild** **ecchymosis** **just** **distal** **to** **the** **left** **greater** **trochanteric** **region,** **but** **his** **skin** **is** **intact, without** **abrasions** **or** **lacerations.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Open** **reduction** **and** **cerclage** **fixation** **of** **the** **fracture**
B. **Open** **reduction** **and** **revision** **of** **the** **femoral** **implant** **to** **a** **long** **cemented** **stem**
C. **Open** **reduction** **and** **revision** **of** **the** **femoral** **implant** **to** **a** **long** **fluted** **and** **tapered** **uncemented stem**
D. Application of balanced traction followed by surgery after the ecchymosis has resolved
**CORRECT ANSWER: D**
DISCUSSION:
This patient has a periprosthetic femoral fracture with a loose femoral stem and normal femoral bone stock, representing a Vancouver type B2 fracture. The most appropriate treatment is fixation of the fracture, along with revision of the stem. Considering his age, bone quality, and activity level, a longer uncemented stem is most predictable. Although a cylindrical stem may also be used, the fluted stem option is the only uncemented choice listed and is the most appropriate option. A cemented stem is a poorer choice because it is difficult to keep the cement out of the fracture site, which would pose a risk for nonunion at the fracture. Also, overall poorer results have been associated with long cemented stems in healthy, active people. Surgery does not need to be delayed to allow the ecchymosis to resolve, and simple open reduction and fixation does not address the loose stem.
**Question 25**
**A** **70-year-old** **man** **undergoes** **removal** **of** **an** **infected** **total** **hip** **arthroplasty** **(THA)** **and** **insertion** **of** **an**
**articulating** **antibiotic-loaded** **spacer** **to** **treat** **a** **deep** **periprosthetic** **hip** **infection.** **While** **in** **a** **nursing** **home receiving** **intravenous** **antibiotics** **3** **weeks** **after** **surgery,** **the** **patient** **trips** **and** **falls.** **Examination** **reveals swelling** **in** **the** **mid** **and** **distal** **thigh,** **intact** **skin** **and** **neurovascular** **structures,** **and** **severe** **pain** **with** **knee**
**or** **hip** **movement.** **Radiographs** **of** **the** **femur** **are** **shown** **in** **Figures** **1** **through** **4.** **What** **is** **the** **most appropriate** **treatment** **for** **the** **fracture** **below** **the** **implant?**
A. **Balanced** **traction** **to** **address** **concern** **for** **persistent** **infection** **with** **reoperation**
B. **Open** **reduction** **and** **internal** **fixation** **of** **the** **fracture** **with** **a** **lateral** **plate** **and** **screws**
C. **Removal** **of** **the** **articulating** **spacer** **and** **revision** **to** **a** **longer-stem** **antibiotic-loaded** **articulating spacer**
D. **Removal** **of** **the** **articulating** **spacer** **and** **reimplantation** **using** **a** **long-stem** **fluted** **uncemented** **hip replacement**
**CORRECT ANSWER: B**
DISCUSSION:
This patient has a type C periprosthetic femoral fracture. The articulating spacer is not involved in the fracture, which is well distal to the implant. The most appropriate treatment is open reduction and internal fixation of the fracture. Traction is not appropriate for this fracture because the injury can be treated surgically despite the history of previous hip infection. Traction would also be needed for at least 5 weeks and would delay the surgical treatment of the periprosthetic fracture until the time of second-stage revision THA. The fracture is fairly distal, and revision to a longer antibiotic-loaded implant or uncemented stem is not suitable for this fracture pattern, because it extends well past the isthmus. A femoral stem in the distal fragment would provide little stability for the fracture. Removal of the articulating spacer and reimplantation using a long-stem fluted uncemented hip replacement is not appropriate, because it would be premature to reimplant the man's hip while he is still receiving treatment for a deep hip infection.
**Question 26**
**Figures** **1** **and** **2** **demonstrate** **the** **radiographs** **obtained** **from** **a** **35-year-old** **woman** **with** **end-stage**
**debilitating** **osteoarthritis** **of** **the** **right** **hip.** **She** **is** **contemplating** **total** **hip** **arthroplasty** **(THA).** **She** **has** **a history** **of** **right** **hip** **dysplasia** **and** **underwent** **hip** **osteotomy** **as** **an** **adolescent.** **Over** **the** **years,** **nonsurgical treatment,** **including** **weight** **loss,** **activity** **modifications,** **and** **intra-articular** **injections,** **has** **failed.** **Her infection** **work-up** **reveals** **laboratory** **findings** **within** **defined** **limits.** **Which** **bearing** **surface** **is contraindicated** **for** **this** **patient?**
A. **Ceramic-on-ceramic**
B. **Ceramic-on-highly** **cross-linked** **polyethylene** **(HXPE)**
C. **Metal-on-HXPE**
D. Metal-on-metal
**CORRECT ANSWER: D**
DISCUSSION:
THA has proven durable and reliable for pain relief and improving function for patients with end-stage arthritis. Appropriate bearing selection is critical to minimize wear and hip complications. A metal-on- metal articulation is associated with excellent wear rates in vitro. With its capacity to offer a low wear rate with large femoral heads, it is an attractive bearing choice for THA. However, local soft-tissue reactions, pseudotumors, and potential systemic reactions including renal failure, cardiomyopathy, carcinogenesis, and potential teratogenesis with potential transfer of metal ions across the placental barrier make metal-on-metal bearings less desirable and relatively contraindicated for younger women of child- bearing age. The workup of a painful metal-on-metal hip arthroplasty necessitates a systematic approach. Several algorithms have been proposed. Routine laboratory studies including sedimentation rate, CRP, and serum cobalt and chromium ion levels should be obtained for all patients with pain. Advanced imaging including MARS MRI should be performed to evaluate for the presence of fluid collections, pseudotumors, and abductor mechanism destruction. Infection can coexist with metal-on-metal reactions, so, when indicated (if the CRP level is elevated), a hip arthrocentesis should be obtained. However, in this setting, a manual cell count and differential should be obtained because an automated cell counter may provide falsely elevated cell counts. The results of revision surgery for a failed metal-on-metal hip prosthesis can be variable. The amount of local tissue destruction and the integrity of the hip abductor mechanism can greatly influence outcomes. Instability is the most common complication following revision of failed metal-on-metal hip replacements.
**Question 27**
**Figures** **below** **show** **the** **radiograph** **and** **the** **MRI** **scan** **obtained** **from** **a** **37-year-old** **woman** **with** **a** **2-month**
**history** **of** **left** **hip** **pain.** **Which** **presurgical** **factor** **is** **most** **commonly** **associated** **with** **a** **poor** **outcome** **after a** **hip** **joint** **salvage** **procedure?**
A. **Age** **older** **than** **40** **years**
B. **Body** **mass** **index** **higher** **than** **30**
C. **Tönnis** **grade** **of** **2** **or** **higher**
D. Outer bridge grade of III or IV
**CORRECT ANSWER: C**
DISCUSSION:
MRI reveals an anterior labral tear, and the radiograph shows minimal arthritis with possible dysplasia. The most common location of pain in patients with a labral tear is the groin, and the most common physical finding is a positive impingement test result. Pain during sitting, clicking, and buttock pain are frequently described by patients with a labral tear, but these symptoms are less common than groin pain. A positive posterior impingement test finding is more common in patients with a posterior labral tear. Although age over 40 years and a body mass index higher than 30 can adversely affect clinical outcomes after joint preservation procedures such as PAO, hip arthroscopy, and femoral acetabular impingement surgery, the presence of hip arthritis on presurgical radiographs is the most commonly mentioned cause of failed hip joint preservation surgery. Tönnis grade is a radiographic measure of hip arthritis. A higher Outerbridge score is associated with more frequent poor outcomes after hip arthroscopy; however, the
Outerbridge cartilage score is determined by direct visualization at the time of surgery. The Outerbridge
score cannot be determined presurgically.
**Question 28**
Figure below shows the radiograph obtained from a 68-year-old man who fell 3 weeks after undergoing a
successful left primary total hip arthroplasty. He is experiencing a substantial increase in pain and an inability to bear weight. What is an appropriate treatment plan?
A. Open reduction and internal fixation (ORIF) of the fracture
B. Removal of the current stem, femur ORIF, and insertion of a longer revision stem
C. Femur ORIF with cables and strut graft, leaving the current stem in situ
D. Femur ORIF combined with reimplantation of the primary component
**CORRECT ANSWER: B**
DISCUSSION:
The fracture has occurred around the stem, representing a Vancouver type B fracture, and the stem is clearly loose, making it a type B2 fracture. The appropriate treatment is removal of the loose in situ stem; ORIF of the femur using cerclage wires, cables, or a plate; and insertion of a longer revision stem such as a tapered fluted modular titanium or fully porous coated cylindrical stem to bypass the fracture. All of the other options are incorrect, because they represent inappropriate treatment options for a Vancouver type B2 fracture.
**Question 29**
**What** **factor** **is** **associated** **with** **a** **higher** **risk** **of** **dislocation** **after** **total** **hip** **arthroplasty?**
A. **Male** **gender**
B. **Previous** **hip** **surgery**
C. **A** **direct** **lateral** **surgical** **approach**
D. Metal-on-metal bearing surfaces
**CORRECT ANSWER: B**
DISCUSSION:
Dislocation after total hip arthroplasty is a multifactorial problem. Numerous risk factors may act independently or cumulatively to increase the risk of this complication. Previous hip surgery of any kind is associated with a twofold increased risk for dislocation. Other risk factors include female gender, impaired mental status, inflammatory arthritis, and older age. Numerous studies have shown a lower dislocation rate with a direct lateral approach, although surgical techniques such as capsular repair have
significantly lowered the incidence of dislocation after using the posterior approach. Metal-on-metal bearings have been associated with other complications such as adverse tissue reactions but are often used with larger-diameter bearings, which pose a lower risk of dislocation.
**Question 30**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **19-year-old** **woman** **with** **a** **3-year** **history** **of**
**progressive** **hip** **pain** **in** **the** **left** **groin** **with** **activity,** **which** **is** **unresponsive** **to** **activity** **modification** **and physical** **therapy.** **Examination** **reveals** **normal** **range** **of** **motion,** **with** **pain** **on** **anterior** **impingement** **testing. What** **treatment** **is** **associated** **with** **the** **best** **long-term** **results?**
A. **Hip** **arthroscopy** **with** **labral** **repair** B. **Reverse** **periacetabular** **osteotomy** C. **Varus** **rotational** **osteotomy**
D. Open surgical dislocation with rim trimming
**CORRECT ANSWER: B**
DISCUSSION:
This patient has symptomatic femoroacetabular impingement as well as clinical and radiographic signs of acetabular retroversion, including a cross-over sign, ischial spine sign, and posterior wall sign bilaterally. Good midterm to long-term outcomes have been reported with reverse (anteverting) Bernese periacetabular osteotomy (PAO). In patients with less retroversion, open or arthroscopic rim trimming with labral refixation have shown good short-term results, but longer-term results have yet to be fully delineated. Isolated hip arthroscopy and labral repair would not be indicated without addressing the retroversion deformity. Femoral varus rotational osteotomy plays no role in the treatment of this pathology. Open surgical dislocation with rim trimming could be considered in patients with less deformity, but some studies have shown inferior long-term results compared with reverse PAO.
**Question 31**
**Figure** **below** **depicts** **the** **radiograph** **obtained** **from** **a** **30-year-old** **woman** **who** **began** **having** **more** **right**
**than** **left** **hip** **pain** **during** **a** **recent** **pregnancy.** **Physical** **examination** **reveals** **increased** **range** **of** **motion** **with positive** **flexion** **abduction** **and** **external** **rotation** **and** **flexion** **adduction** **and** **internal** **rotation** **as** **well** **as** **pain with** **external** **logroll.** **Assessment** **of** **Figure** **below** **reveals**
A. **classic** **dysplasia** **with** **volume** **deficient** **acetabula.**
B. **acetabular** **retroversion** **with** **positive** **crossover** **signs** **and** **ischial** **spine** **signs.**
C. **no** **substantial** **dysplasia,** **with** **normal** **acetabular** **volume** **and** **anteversion.**
D. inadequate radiographic evidence to assess for hip dysplasia.
**CORRECT ANSWER: D**
DISCUSSION:
Studies have demonstrated that pelvic inclination can dramatically affect the interpretation of radiographs in the dysplastic hip, with 9° of increased pelvic inclination leading to the presence of crossover signs and posterior wall signs. A distance of 30 mm to 50 mm from the sacrococcygeal junction to the pubis is often used to assess the adequacy of pelvic inclination on radiographs, although Siebenrock and associates determined the mean difference to be 32 mm in men and 47 mm in women. In this patient, the pelvic inclination is dramatically increased, leading to overestimation of acetabular retroversion.
**Question 32**
In patients with Crowe types III and IV developmental dysplasia of the hip with high hip centers, acetabular
reconstruction often requires lowering the acetabular component into the native acetabulum. In doing so, considerable risk for limb lengthening beyond 4 cm exists, making the hip difficult to reduce and raising the risk for nerve injury. Which technique is used to overcome this problem?
A. Subtrochanteric osteotomy with femoral shortening
B. An offset femoral component
C. A lateralized liner
D. Extended trochanteric osteotomy
**CORRECT ANSWER: A**
DISCUSSION:
When substantial lengthening of a dysplastic hip will occur because a high dislocation is relocated into a considerably lower acetabulum, a femoral shortening may be necessary to reduce the hip and avoid a stretch injury to the sciatic nerve. No other choice specifically addresses the need for femoral shortening, and high offset stems and lateralized liners may exacerbate the problem if used alone and without femoral shortening.
**Question 33**
Figures 1 through 3 show the radiograph and MR arthrograms obtained from a 25-year-old woman who has
had right groin pain since joining the military 4 years ago. She has undergone treatment with NSAIDs, physical therapy, and activity modification. Examination reveals positive flexion abduction and external rotation, a positive external log roll, and increased range of motion. What is the most appropriate treatment?
A. Viscosupplementation of the right hip
B. Hip arthroscopy with labral repair
C. Periacetabular osteotomy
D. Total hip arthroplasty
**CORRECT ANSWER: C**
DISCUSSION:
This patient has symptomatic hip dysplasia that has been recalcitrant to nonsurgical management. Radiographs reveal an upsloping sourcil (acetabular index of 18) and a lateral center edge angle of 14, with posterior uncovering. The MR arthrogram shows no definitive evidence of a labral tear. Appropriate surgical management would include periacetabular osteotomy. Viscosupplementation in the hip is controversial in the treatment of osteoarthritis and plays no role in the treatment of dysplasia. Hip arthroscopy with labral repair is controversial in mild hip dysplasia, with studies demonstrating between
60% and 77% good and excellent results, inferior to the results for hip arthroscopy in a femoroacetabular impingement cohort. In moderate to severe dysplasia, hip arthroscopy is not recommended. Because the acetabular cartilage is well maintained, total hip arthroplasty would not be recommended in this young and active patient.
**Question 34**
**Figures** **1** **and** **2** **show** **the** **radiographs** **obtained** **from** **a** **68-year-old** **morbidly** **obese** **man** **who** **underwent**
**left** **total** **hip** **replacement** **7** **years** **ago** **and** **did** **well,** **with** **no** **symptoms** **prior** **to** **the** **current** **presentation. He** **recently** **rose** **from** **a** **seated** **position** **and** **felt** **a** **pop** **in** **the** **hip,** **with** **immediate** **pain** **and** **inability** **to** **bear weight.** **Any** **pressure** **on** **the** **left** **foot** **now** **produces** **a** **painful,** **grinding** **sensation** **with** **loss** **of** **left** **hip stability.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **of** **the** **acetabular** **implant** **to** **a** **constrained** **bearing** **with** **modular** **exchange** **of** **the femoral** **head** **and** **neck**
B. **Revision** **of** **the** **acetabular** **and** **femoral** **implants**
C. **Retention** **of** **the** **acetabular** **implant** **with** **modular** **exchange** **of** **the** **femoral** **head** **and** **neck**
D. Revision of the femoral component alone with a new ceramic head
**CORRECT ANSWER: B**
DISCUSSION:
The modular femoral stem has fractured. Changing the liner to a constrained design is not warranted at this time based on the information provided. Revision of the acetabular implant is appropriate because of the potential for damage to the existing cup from metal debris and femoral implant contact and to convert from a metal-on-metal articulation. Nonsurgical management would not provide pain relief or improvement; revision of the total hip arthroplasty is recommended. The implant failed in a short time, and retention of the femoral stem is not recommended because of the concern for failure with only a neck exchange. A dual-mobility bearing may be a good option if the surgeon plans to retain the acetabular component. Extended trochanteric osteotomy is a useful technique for the removal of a well-fixed femoral implant. In this patient, femoral stem removal without
osteotomy would be difficult due to the fracture of the implant’s femoral neck and the
inability to gain purchase for extraction.
**Question 35**
**A** **63-year-old** **woman** **had** **a** **primary** **total** **hip** **arthroplasty** **7** **years** **ago** **that** **included** **a** **proximally** **coated titanium** **stem,** **a** **cobalt** **alloy** **femoral** **head,** **a** **titanium** **hemispherical** **acetabular** **component,** **and** **a polyethylene** **liner.** **She** **did** **well** **for** **4** **years** **but** **has** **now** **had** **two** **dislocations** **and** **reports** **pain** **and weakness** **around** **the** **left** **hip.** **She** **denies** **any** **fevers,** **chills,** **or** **constitutional** **symptoms.** **On** **examination, the** **patient** **walks** **well** **without** **any** **signs** **of** **an** **antalgic** **or** **Trendelenburg** **gait.** **Her** **abductor** **mechanism demonstrates** **good** **strength.** **Her** **erythrocyte** **sedimentation** **rate** **and** **C-reactive** **protein** **level** **are** **normal. On** **radiographs,** **all** **components** **appear** **well** **fixed** **and** **in** **good** **alignment.** **What** **is** **the** **most** **appropriate treatment** **at** **this** **time?**
A. **Physical** **therapy** **to** **improve** **hip** **stability**
B. **Use** **of** **an** **abduction** **brace** **to** **limit** **the** **patient’s** **range** **of** **motion**
C. **Conversion** **to** **a** **constrained** **acetabular** **liner**
D. Cobalt and chromium serum metal ion level testing
**CORRECT ANSWER: D**
DISCUSSION:
Trunnionosis is a recently recognized complication following total hip arthroplasty and can occur when a cobalt alloy femoral head is used on a titanium alloy or cobalt alloy femoral stem. Patients often present with pain or swelling around the hip but at times can present with instability. Certain femoral stem designs have been associated with increased reports of trunnionosis. In a patient with a cobalt alloy femoral head who presents with instability, swelling, and weakness around the hip, the potential for trunnionosis and
an adverse local tissue reaction should be considered.
**Question 36**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **68-year** **old** **man** **with** **progressively** **worsening** **right**
**side** **hip** **pain** **over** **the** **last** **8** **months.** **He** **is** **6** **feet** **tall,** **with** **a** **BMI** **of** **51** **kg/m** 2 **and** **reports** **that** **his** **index total** **hip** **arthroplasty** **was** **performed** **8** **years** **ago.** **The** **preoperative** **work-up** **includes** **negative** **infectious laboratory** **results.** **What** **is** **the** **most** **appropriate** **surgical** **plan** **for** **revision** **of** **the** **femoral** **component** **in this** **patient?**
A. **Superior** **approach** **with** **trochanteric** **slide**
B. **Direct** **anterior** **approach** **with** **a** **chevron** **modification** **of** **the** **standard** **greater** **trochanteric osteotomy**
C. **Lateral** **approach** **with** **a** **partial** **greater** **trochanter** **osteotomy**
D. Posterolateral approach with an extended trochanteric osteotomy
**CORRECT ANSWER: D**
DISCUSSION:
Submit Answer
The patient’s radiographs demonstrate varus femoral remodeling around a broken cylindrical, distally fixed femoral stem. Proximal femoral remodeling around loose or fractured stems occurs in 21% to 42% of femoral revisions, based on the definitions outlined by Foran and associates. In definition 1, varus femoral remodeling occurs when the template falls within 2 mm of the endosteal cortex of the metaphysis on templating with a diaphyseal engaging stem. In definition 2, varus femoral remodeling = when the template crosses the lateral femoral cortex proximally. Based on the templating or drawing a line from the isthmus proximally along the lateral cortex, implantation of a straight stem would perforate the cortex proximally, indicating varus femoral remodeling. An extended trochanteric osteotomy would aid in the removal of the well-fixed distal segment and enable the safe insertion of the new femoral component. The approach is not the concern in this case, because extended trochanteric osteotomies have been described from the posterior and direct lateral approaches with excellent outcomes and union rates. The key is that the extended osteotomy is necessary and not a trochanteric slide or standard (shorter or incomplete trochanteric) osteotomy. These types would not provide access to the well-fixed distal stem, nor would they afford a straight tube in which to insert a new femoral component.
**Question 37**
**Figures** **1** **and** **2** **show** **the** **radiograph** **and** **CT** **obtained** **from** **a** **78-year-old** **woman** **who** **underwent** **right**
**total** **hip** **replacement** **in** **1995.** **She** **initially** **did** **well** **with** **no** **pain.** **She** **was** **last** **seen** **7** **years** **ago** **and** **was having** **mild** **hip** **pain** **at** **that** **time.** **She** **was** **found** **to** **have** **a** **supra-acetabular** **cyst** **on** **radiographs.** **She** **has had** **severe** **right** **hip** **pain** **for** **the** **past** **9** **months** **while** **using** **a** **walker** **for** **ambulation.** **The** **initial** **blood work** **reveals** **an** **estimated** **erythrocyte** **sedimentation** **rate** **of** **32** **mm/hr,** **a** **C-reactive** **protein** **level** **of** **0.5 mg/L,** **a** **serum** **cobalt** **level** **of** **0.4** **µg/L,** **and** **a** **serum** **chromium** **level** **of** **0.6** **µg/L.** **Right** **hip** **aspiration** **is performed,** **revealing** **a** **white** **blood** **cell** **count** **of** **139,** **52%** **neutrophils,** **and** **a** **negative** **leukocyte** **esterase test.** **What** **is** **the** **best** **next** **step?**
A. **Acetabular** **revision,** **with** **placement** **of** **a** **custom** **triflange** **acetabular** **component** **and** **femoral head** **exchange**
B. **Removal** **of** **the** **femoral** **and** **acetabular** **components** **and** **placement** **of** **an** **antibiotic** **spacer,** **with** **6 weeks** **of** **intravenous** **antibiotics**
C. **Head** **and** **liner** **exchange** **and** **retention** **of** **the** **femoral** **and** **acetabular** **implants** **with** **acetabular bone** **grafting**
D. Nonsurgical management with the initiation of bisphosphonates and referral to pain management
**CORRECT ANSWER: A**
DISCUSSION:
The hip replacement was performed in 1995, during the period when the previous generation of polyethylene was utilized. This polyethylene was subjected to irradiation in air, with subsequent oxidation and consequent osteolysis after implantation. The mechanism of osteolysis begins with the uptake of polyethylene particles by macrophages, which then initiate an inflammatory cascade and the release of osteolytic factors. This cycle continues, with eventual implant loosening and failure. The imaging shows significant osteolysis and raises concern for pelvic discontinuity and acetabular implant failure. The surgical treatment consists of acetabular reconstruction. In this patient, concern exists for discontinuity based on the substantial amount of bone loss and nonsupportive anterior and posterior columns. This scenario requires complex acetabular revision using a custom triflange device, distraction with a jumbo acetabular component, or placement of a porous metal cup/cage construct with augmentation. The laboratory values are not consistent with infection or failure due to metal debris.
**Question 38**
**Figure** **below** **shows** **a** **cross-table** **lateral** **radiograph** **obtained** **from** **a** **healthy** **56-year-old** **woman** **with**
**recurrent** **hip** **dislocations** **6** **months** **after** **total** **hip** **arthroplasty** **performed** **through** **a** **posterolateral approach.** **Each** **dislocation** **occurred** **when** **she** **was** **bending** **over** **to** **put** **her** **shoes** **on** **or** **pick** **something up.** **She** **has** **dislocated** **four** **times** **and** **has** **had** **no** **pain** **between** **dislocations.** **Abductor** **strength** **is** **5** **out** **of**
**5.** **The** **infection** **work-up** **is** **negative.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **of** **the** **acetabulum** **and** **evaluation** **of** **the** **femoral** **stem**
B. **Conversion** **to** **a** **constrained** **liner**
C. **Gluteus** **medius** **repair** **and** **application** **of** **a** **hip** **abductor** **brace**
D. Revision to an elevated acetabular polyethylene liner
**CORRECT ANSWER: A**
DISCUSSION:
The cross-table lateral radiograph shows that the patient has decreased acetabular anteversion. She is likely impinging on her cup in flexion and levering the femoral component posteriorly. Given a well-fixed and well-aligned femoral component and a negative infection work-up, the preferred treatment is to revise the acetabulum with a goal of increasing acetabular anteversion to avoid prosthetic impingement. Conversion to a constrained or elevated rim liner is suboptimal in this setting, because the problem is impingement. Indications for a constrained liner are neuromuscular compromise, abductor deficiency, or instability despite well-fixed and well-placed components. Given her 5 of 5 abductor strength, gluteus
medius repair is not indicated.
**Question 39**
Figures below show the radiographs obtained from a 75-year-old woman who underwent right total hip
arthroplasty in 2009. She did well until last month, when a right posterior hip dislocation occurred after she fell from her bed to the floor. Successful closed reduction was performed. She sustained two more posterior dislocations requiring closed reduction under anesthesia. The surgical report from the index arthroplasty notes a 54-mm monoblock acetabular component with a 28-mm inner diameter compression molded polyethylene and a high offset neck cementless stem with a +8-mm length, 28-mm head. What is the best next step?
A. Hip spica cast placement
B. Acetabular revision arthroplasty
C. Resection arthroplasty
D. Femoral head revision to a 28-mm diameter, +10-mm length head
**CORRECT ANSWER: B**
DISCUSSION:
This patient has demonstrated recurrent instability, and her current implants lack the modularity to upsize and improve the head-neck ratio and range to impingement. Given the monoblock acetabular component and a +7-mm neck length, the best option is revision to a large-diameter femoral head or dual-mobility component. Placement of a hip spica cast and resection arthroplasty are unreasonable. Revision to a longer ball length likely would not solve this recurrent instability pattern.
**Question 40**
**According** **to** **Musculoskeletal** **Infection** **Society** **(MSIS)** **guidelines,** **which** **set** **of** **patient** **laboratory** **study**
**results** **fits** **the** **definition** **of** **chronic** **prosthetic** **joint** **infection?**
A. **Erythrocyte** **sedimentation** **rate** **(ESR)** **50** **mm/hr,** **C-reactive** **protein** **(CRP)** **8** **mg/L,** **joint aspiration** **white** **blood** **cell** **(WBC)** **count** **542,** **62%** **neutrophils,** **and** **positive** **leukocyte** **esterase**
B. **ESR** **42** **mm/hr,** **CRP** **12** **mg/L,** **joint** **aspiration** **WBC** **count** **3,540,** **72%** **neutrophils,** **and** **positive leukocyte** **esterase**
C. **ESR** **20** **mm/hr,** **CRP** **15** **mg/L,** **joint** **aspiration** **WBC** **count** **4,135,** **54%** **neutrophils,** **and** **negative**
**leukocyte** **esterase**
D. **ESR** **25** **mm/hr,** **CRP** **7** **mg/L,** **joint** **aspiration** **WBC** **count** **252,** **82%** **neutrophils,** **and** **negative leukocyte** **esterase**
**CORRECT ANSWER: B**
DISCUSSION:
The MSIS definition of periprosthetic joint infection was updated in 2014 with two major and six minor criteria. The presence of one major criterion or three minor criteria is diagnostic for infection. The major criteria are two positive cultures with the same organism or a draining sinus tract. The current MSIS minor criteria are 1) an elevated ESR (more than 30 mm/hr) and CRP level (more than 10 mg/L), 2) an elevated synovial WBC count (more than 3,000 cells per/microliter), 3) an elevated synovial fluid polymorphonuclear count (more than 80%), 4) a positive histological analysis of periprosthetic tissue, and 5) a single positive culture.
**Question 41**
Figures below show the AP and lateral radiographs obtained from a 54-year-old woman who has worsening
groin pain 18 months after a primary left total hip arthroplasty. The pain is worst when climbing stairs, when rising from a seated position, and during resisted hip flexion. Her pain improved early after surgery but did
not completely resolve. Her C-reactive protein and erythrocyte sedimentation rate results of less than 1 mg/dL
and 10 mm/hr, respectively, were obtained in the office. What is the best next step?
A. MRI with MARS of the left hip
B. Revision of the left acetabular component
C. Intra-articular ultrasound-guided left hip injection
D. Physical therapy for the left hip
**CORRECT ANSWER: B**
DISCUSSION:
Iliopsoas impingement is a potential cause of persistent groin pain after a total hip arthroplasty. This patient’s history gives groin pain with resisted hip flexion and during activities that require this level of function. The radiographs depict an acetabular component with substantial retroversion. Typical options for the management of iliopsoas tendon impingement include injections, tenotomy, and acetabular revision. Recently, Chalmers and associates reported more predictable groin pain resolution with 8 mm or more of anterior acetabular component when overhang was revised. The radiographs clearly show more retroversion, with a cup prominence of more than 8 mm anteriorly. MRI with MARS could potentially help in the diagnosis of this impingement but would not help in management (option A). An ultrasound- guided injection would need to be administered into the iliopsoas tendon sheath to be of help and, in this case, would likely be performed for diagnostic purposes due to the extreme anterior overhang (option C). Option D would be useful for mild cases of iliopsoas impingement but likely would not help much in this more extreme case.
**Question 42**
**Figure** **1** **shows** **the** **radiograph** **obtained** **from** **a** **67-year-old** **man** **recently** **diagnosed** **with** **osteoarthritis,** **8**
**years** **after** **receiving** **a** **left** **metal-on-metal** **total** **hip** **arthroplasty** **(THA).** **The** **acetabular** **component** **has** **a modular** **cobalt** **alloy** **acetabular** **liner.** **The** **patient** **states** **that** **he** **did** **very** **well** **postoperatively,** **but** **for** **the last** **6** **months** **has** **noted** **worsening** **pain** **and** **swelling** **in** **his** **left** **hip.** **Serum** **metal** **ion** **testing** **reveals** **a chromium** **level** **of** **12.4** **ng/mL,** **compared** **with** **a** **normal** **level** **of** **less** **than** **0.3** **ng/mL,** **and** **a** **cobalt** **level of** **11.8** **ng/mL,** **compared** **with** **a** **normal** **level** **less** **than** **0.7** **ng/mL.** **An** **MRI** **with** **metal** **artefact** **reduction sequence** **(MARS)** **was** **performed** **and** **is** **shown** **in** **Figure** **2.** **What** **is** **the** **most** **appropriate** **management** **at this** **time?**
A. **Annual** **monitoring** **of** **serum** **metal** **ion** **levels**
B. **Repeated** **MRI** **with** **MARS** **in** **6** **months**
C. **Conversion** **of** **the** **THA** **to** **a** **cobalt** **alloy** **femoral** **head** **and** **polyethylene** **bearing**
D. **Conversion** **of** **the** **THA** **to** **a** **ceramic** **femoral** **head** **with** **an** **inner** **titanium** **sleeve** **and polyethylene** **bearing**
**CORRECT ANSWER: D**
DISCUSSION:
Metal-on-metal THA was initially introduced in the 1990s, with the proposed advantages of decreased wear and improved stability. However, catastrophic adverse local tissue reactions associated with their use has raised numerous concerns. The work-up of a patient with a prior metal-on-metal total hip arthroplasty involves a thorough history and physical examination; blood analysis, including the erythrocyte sedimentation rate, C-reactive protein, and metal ion levels; and secondary imaging, including ultrasonography, CT, and MRI. In a patient with clinical symptoms, elevated metal ion levels, and a large fluid collection seen on MRI, the most appropriate treatment would be removal of the metal-on-metal bearing. Given the presence of an adverse reaction involving cobalt and chromium, a revision ceramic head may be most appropriate to avoid the potential of trunnion-associated corrosion.
**Question 43**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **76-year-old** **woman** **with** **a** **painful** **total** **knee**
**arthroplasty.** **She** **describes** **an** **uneventful** **recovery** **with** **no** **wound-healing** **issues** **and** **was** **pain** **free** **for the** **first** **10** **years.** **Although** **reporting** **no** **trauma** **or** **inciting** **event,** **she** **now** **describes** **pain** **in** **the** **entire knee** **that** **is** **most** **severe** **with** **her** **first** **few** **steps.** **She** **has** **begun** **to** **notice** **night** **pain** **and,** **more** **recently, constant** **swelling.** **What** **is** **the** **most** **appropriate** **work-up** **at** **this** **time?**
A. **Knee** **aspiration** **with** **cell** **count/cultures,** **C-reactive** **protein** **(CRP)** **level,** **erythrocyte sedimentation** **rate** **(ESR),** **CT**
B. **Knee** **aspiration** **with** **cell** **count/cultures,** **CRP,** **ESR**
C. **Fresh-frozen** **specimen** **at** **the** **time** **of** **revision** **knee** **arthroplasty** **only**
D. Technetium-99m bone scan, knee aspiration with cell count/cultures
**CORRECT ANSWER: B**
DISCUSSION:
An evaluation of the painful total knee must be supported by an understanding of the potential etiologies of pain. They may include, aseptic loosening, infection, osteolysis, gap imbalance, referred pain, stiffness, and complex regional pain syndrome. In this case, the patient demonstrates start-up pain and had no prior history of infections. Her radiographs show subsidence of the tibia, indicating a loose prosthesis. Knowing that the prosthesis is already loose precludes the need for a bone scan. It is, however, important to rule out infection in this case; therefore, CRP and ESR testing is essential. Aspiration is also recommended when going into knee arthroplasty, and infection is a concern.
**Question 44**
**The** **direct** **anterior** **(Smith-Peterson)** **approach** **to** **hip** **arthroplasty** **is** **most** **commonly** **associated** **with**
**injury** **to** **what** **nerve?**
A. **Lateral** **femoral** **cutaneous**
B. **Sciatic**
C. **Pudendal**
D. Superior gluteal
**CORRECT ANSWER: A**
---
DISCUSSION:
Some authors have reported the incidence of lateral femoral cutaneous nerve neuropraxia following hip arthroplasty with the direct anterior approach to be near 80%, but resolution of the sensory deficits has been observed in most patients over time. Femoral nerve palsy has been reported to occur in .64% to 2.3% direct lateral (Hardinge) and anterolateral (Watson-Jones) approaches, and the superior gluteal nerve may be injured with proximal extension of the abductor muscular dissection. The posterior approach has been reported to be associated with sciatic nerve injury, especially in cases of dysplasia. Pudendal nerve injury has not been reported with the anterior, anterolateral, direct lateral, or posterior approaches to hip
arthroplasty. It has been reported following hip arthroscopy and the use of a traction table, however.
**Question 45**
**A** **55-year-old** **woman** **is** **referred** **for** **evaluation** **of** **a** **painful** **knee** **replacement.** **She** **underwent** **total** **knee**
**arthroplasty** **(TKA)** **more** **than** **1** **year** **ago** **without** **perioperative** **complications** **but** **has** **had** **consistent** **pain since** **the** **surgery.** **The** **patient’s** **preoperative** **radiographs** **and** **postoperative** **radiographs** **are** **shown** **in Figures** **below.** **Examination** **reveals** **medial** **laxity** **during** **valgus** **stress** **testing** **and** **range** **of** **motion** **of** **0° to** **70°.** **Her** **erythrocyte** **sedimentation** **rate** **and** **C-reactive** **protein** **level** **are** **normal.** **What** **is** **the** **best** **next step?**
A. **Unloader** **brace**
B. **Distal** **femoral** **osteotomy**
C. **Open** **arthrofibrosis** **debridement** **with** **lateral** **ligament** **balancing** **and** **polyethylene** **exchange**
D. Revision TKA of both the femoral and tibial components
**CORRECT ANSWER: D**
DISCUSSION:
The radiographs show substantial valgus malalignment of the femoral component, with lateral mechanical axis deviation. Clinically, by examination she displays instability and stiffness as a result. Revision knee replacement is appropriate and should consist of total revision to stemmed femoral and tibial components with a varus-valgus constrained insert, given the likely attenuation of the medial collateral ligament. Open debridement with ligament balancing and polyethylene exchange do not address the underlying cause and are inappropriate. Distal femoral osteotomy is not useful in the setting of previous total knee replacement.
Nonsurgical treatment with an unloader brace would be ineffective in correcting the alignment.
**Question 46**
**A** **45-year-old** **man** **has** **a** **draining** **sinus** **and** **recurrent** **infection** **of** **his** **right** **total** **knee** **arthroplasty.** **He** **has**
**had** **two** **prior** **revision** **surgeries** **after** **the** **primary** **procedure** **and** **three** **other** **surgeries** **before** **his** **initial replacement,** **including** **a** **proximal** **tibial** **osteotomy** **and** **subsequent** **hardware** **removal.** **On** **clinical examination,** **he** **has** **a** **draining** **sinus** **in** **the** **mid** **portion** **of** **his** **surgical** **scar** **and** **a** **range** **of** **motion** **of** **5°** **to**
**85°.** **AP** **and** **lateral** **radiographs** **of** **the** **right** **knee** **are** **shown** **in** **Figures** **below.** **During** **surgery,** **the** **femoral component** **is** **found** **to** **be** **grossly** **loose,** **but** **the** **tibial** **component** **is** **well** **fixed.** **What** **is** **the** **most appropriate** **extensile** **approach** **that** **would** **provide** **adequate** **exposure** **and** **aid** **in** **tibial** **component extraction?**
A. **Extended** **medial** **parapatellar** **approach**
B. **Quadriceps** **snip**
C. **Extended** **tibial** **tubercle** **osteotomy**
D. Medial epicondyle osteotomy
CORRECT ANSWER: C
DISCUSSION:
Extended tibial tubercle osteotomy is an extensile approach to revision total knee arthroplasty that affords excellent exposure and can facilitate removal of tibial sleeves and cones. This patient has had multiple surgeries, including a proximal tibial osteotomy, as well as poor range of motion, patella baja, and a well- fixed metaphyseal sleeve component. Classically, an extended tibial tubercle osteotomy provides outstanding exposure for component removal in the setting of prior high tibial osteotomy and patella baja. For this patient, it is important to recognize the patella baja on the radiographs, as well as the tibial sleeve. In many of these cases the osteotomy provides access to the sleeve to help with extraction, because the stem will not pull through the sleeve or detach from the tray to allow visualization of the sleeve. The extended medial parapatellar approach is just a long medial approach that typically yields good exposure
but would not help with the patella baja or extraction of the tibial sleeve. The quadriceps snip would give good exposure to the knee but would not aid in tibial component removal. Lastly, the medial epicondyle osteotomy could help with exposure and tensioning of the medial complex of the knee but would not help
with tibial component extraction.
**Question 47**
**A** **58-year-old** **woman** **underwent** **a** **left** **total** **knee** **arthroplasty** **6** **years** **ago.** **She** **initially** **did** **well** **after**
**surgery** **but** **sustained** **a** **fall** **2** **months** **ago** **while** **at** **work.** **She** **now** **describes** **left** **knee** **pain** **and** **instability and** **an** **inability** **to** **straighten** **her** **knee** **since** **the** **fall.** **She** **has** **been** **using** **a** **hinged** **knee** **brace,** **which provides** **partial** **support.** **On** **examination,** **she** **has** **passive** **range** **of** **motion** **of** **0°** **to** **115°** **and** **active** **range of** **motion** **of** **80°** **to** **-115°.** **Her** **radiographs** **are** **shown** **in** **Figures** **below.** **What** **is** **the** **best** **option** **for** **the restoration** **of** **her** **function?**
A. **Revision** **total** **knee** **arthroplasty** **with** **placement** **of** **a** **hinge** **constrained** **device**
B. **Patellar** **tendon** **repair** **with** **nonabsorbable** **suture** **and** **patellar** **resurfacing**
C. **Hinged** **knee** **brace** **with** **drop** **lock** **design** **to** **restore** **stability** **during** **ambulation**
D. **Extensor** **mechanism** **reconstruction** **using** **synthetic** **mesh** **or** **allograft**
**CORRECT ANSWER: D**
---
DISCUSSION:
The patient has an extensor mechanism disruption with patellar tendon rupture. This injury is treated with extensor mechanism reconstruction in the setting of previous total knee arthroplasty. There is a reported high failure rate with attempted repair. Revision to hinge knee arthroplasty would provide implant stability but would not restore the extensor mechanism. The patient is relatively young and is working, so reconstruction would offer better long-term function than a drop lock brace, which can be better used in low-functioning patients with this type of injury. Extensor mechanism reconstruction historically has been accomplished with allograft material, but a novel technique using synthetic mesh also has proved successful in treating this difficult problem.
**Question 48**
**Figures** **below** **show** **the** **radiographs,** **and** **the** **CT** **obtained** **from** **a** **58-year-old** **woman** **who** **underwent**
**cementless** **left** **total** **hip** **arthroplasty.** **Nine** **months** **after** **surgery,** **she** **continued** **to** **have** **groin** **pain** **when actively** **flexing** **her** **hip.** **She** **has** **trouble** **walking** **up** **stairs** **and** **getting** **out** **of** **her** **car.**
What is the most likely diagnosis?
A. **Trochanteric** **bursitis**
B. **Femoral** **component** **loosening**
C. **Iliopsoas** **tendonitis**
D. Acetabular component loosening
**CORRECT ANSWER: C**
---
DISCUSSION:
Groin pain after total hip replacement has a number of possible causes, and an exact diagnosis may remain elusive in some patients. Infection should be ruled out with laboratory studies and, if indicated, diagnostic aspiration of the hip joint. Implant loosening should be evaluated by plain radiograph and bone scan, if indicated. Synovitis resulting from wear debris should be considered in patients with polyethylene liners who experience late-onset symptoms or in any patient with a metal-on-metal bearing. This patient's symptoms are classic for iliopsoas tendonitis. Physical examination usually reveals pain and weakness with resisted hip flexion. A cross-table lateral radiograph and CT show that the anterior edge of the acetabulum protrudes beyond the anterior wall, thereby acting as a source of iliopsoas tendon irritation. In such cases, acetabular component revision and repositioning are indicated. Fluoroscope-guided iliopsoas cortisone injection can help to establish the diagnosis and relieve groin pain. If the acetabular component is well positioned, then iliopsoas tenotomy should be considered.
**Question 49**
**A** **72-year-old** **woman** **is** **scheduled** **to** **undergo** **right** **total** **hip** **arthroplasty.** **Her** **preoperative** **radiograph**
**is** **shown** **in** **Figure** **below.** **To** **avoid** **increasing** **this** **patient’s** **combined** **offset** **while** **maintaining** **her** **leg**
length, what is the most appropriate surgical plan?
A. **Lateralize** **the** **acetabular** **component,** **use** **a** **low** **offset** **femoral** **component,** **and** **make** **a** **shorter neck** **cut**
B. **Medialize** **the** **acetabular** **component,** **use** **a** **low** **offset** **femoral** **component,** **and** **make** **a** **longer neck** **cut**
C. **Lateralize** **the** **acetabular** **component,** **use** **a** **high** **offset** **femoral** **component,** **and** **make** **a** **shorter neck** **cut**
D. **Medialize** **the** **acetabular** **component,** **use** **a** **high** **offset** **femoral** **component,** **and** **make** **a** **longer neck** **cut**
**CORRECT ANSWER: B**
---
DISCUSSION:
The management of patients with proximal femoral deformity can be difficult. Appropriate implant selection and preoperative templating are critical. In this patient, it would be difficult to avoid increasing the combined offset by too much, which could contribute to the overtensioning of the soft tissues and trochanteric pain. By medializing the acetabular component (decreasing the combined offset), using a low offset femoral component or a cemented component placed more valgus (decreasing the combined offset), and making a longer neck cut (to avoid shortening of the lower extremity), restoration of the patient’s native offset and leg length can be achieved.
**Question 50**
Figures below demonstrate the radiographs obtained from a 56-year-old man with a 3-year history of right
groin pain. A comprehensive nonsurgical program has failed, and the patient would like to proceed with total hip arthroplasty. He is seen by a pain management specialist and is currently taking 40 mg of sustained-release morphine twice daily with oxycodone 10 mg 2 to 3 times a day for severe pain. What is the recommended course of action regarding his chronic narcotic use?
A. Increase his current opioid medication regimen prior to and after surgery as needed to control his pain.
B. Decrease his preoperative opioid use, and work with his pain management physician to decrease his postoperative opioid requirement.
C. Avoid using narcotics in the perioperative period to prevent overdose, and use acetaminophen only for pain control.
D. Stop all his opioids 5 days before surgery, and place the patient on a morphine pain control pump postoperatively with a basal rate.
**CORRECT ANSWER: B**
DISCUSSION:
Chronic opioid consumption prior to total joint arthroplasty has been associated with increased pain after surgery, increased opioid requirements, a slower recovery and longer hospital stay, and higher 90-day postoperative complications compared with patients not on chronic opioids preoperatively. Based on this information, Nguyen and associates performed a study in three patient groups that included 1) chronic opioid users who underwent no preoperative intervention, 2) chronic opioid users who were weaned down to 50% of their prior opioid regimen, and 3) patients who were not chronic opioid users. The authors found that the reduction of preoperative opioid use improved postoperative function, pain, and recovery and that the weaned group performed more like the opioid naive group than the chronic opioid user
group. Increasing opioid use prior to surgery in this patient would make it more difficult to control pain after surgery. Stopping all of his opioids just prior to surgery would place the patient at substantial risk for opioid withdrawal and is not recommended. Avoiding the use of all narcotics and using only acetaminophen postoperatively is very unlikely to provide appropriate pain relief in a chronic opioid user. The recommendation based on the provided literature is to decrease the patient's narcotic use prior to
surgery.
**Question 51**
**A** **72-year-old** **patient** **fell** **3** **weeks** **after** **undergoing** **a** **total** **hip** **arthroplasty** **using** **cementless** **fixation** **of**
**the** **femoral** **component.** **She** **sustained** **a** **comminuted** **Vancouver** **type** **B-2** **fracture** **with** **displacement** **of the** **calcar** **fragment.** **What** **is** **the** **best** **treatment** **option?**
A. **Revision** **using** **a** **proximal** **femoral** **replacement** **prosthesis**
B. **Revision** **using** **a** **diaphyseal** **engaging** **femoral** **prosthesis** **along** **with** **cerclage** **fixation**
C. **Open** **reduction** **internal** **fixation** **using** **a** **locking** **plate** **with** **strut** **graft**
D. Protected weight bearing with abduction bracing
**CORRECT ANSWER: B**
DISCUSSION:
The patient has an acute postoperative fracture of the proximal femur with subsidence. It is also common that the stem retroverts relative to the femur. It is most often seen in proximally porous coated stems within 90 days of surgery, one paper found it to occur 0.7% of the time in modern implants. There is always a debate whether this is a missed intraoperative fracture, or a new fracture that has resulted from an event of increased hoop stresses. Removal of the primary stem, placement of a diaphyseal engaging
stem (most frequently a tapered-fluted stem), and cabling of the fracture is the most successful treatment.
**Question 52**
**What** **is** **the** **most** **important** **preoperative** **factor** **predicting** **conversion** **to** **total** **hip** **arthroplasty** **after**
**arthroscopic** **surgery** **of** **the** **hip?**
A. **Age** **over** **60** **years**
B. **Morbid** **obesity**
C. **Diagnosis** **of** **osteoarthritis**
D. Tobacco use
**CORRECT ANSWER: B**
DISCUSSION:
---
The authors cited in the references examined large databases to determine the risk factors for conversion to total hip arthroplasty after arthroscopic surgery of the hip. In the study by Kester and associates, obesity had an odds ratio (OR) of 5.6 for conversion to hip arthroplasty, whereas age over 60 years had an OR of
3.4, osteoarthritis had an OR of 2.4, and tobacco use had an OR of 1.9.
**Question 53**
A 70-year-old woman with a body mass index (BMI) of 34 and a history of hypercholesterolemia has elected
to undergo total hip arthroplasty. Her son recently learned he has factor V Leiden following an episode of pulmonary embolism. What are this patient's risk factors for thromboembolic disease?
A. Type of surgery, age, and BMI
B. Type of surgery, hypercholesterolemia, and age
C. Age, BMI, and hypercholesterolemia
D. BMI, type of surgery, and hypercholesterolemia
**CORRECT ANSWER: A**
DISCUSSION:
Risk stratification is one of the most critical clinical evaluations to undertake before performing total joint arthroplasty. Many factors have been identified that increase the risk for venous thromboembolism (VTE) The major factors include previous VTE, obesity, type of surgery (such as total joint arthroplasty), hypercoagulable states, myocardial infarction, congestive heart failure, family history of VTE, and
hormone replacement therapy. Hypercholesterolemia is not a risk factor for thromboembolic disease.
**Question 54**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **76-year-old** **woman** **who** **comes** **to** **the** **emergency**
**department** **after** **experiencing** **a** **fall.** **She** **is** **an** **unassisted** **community** **ambulator** **with** **a** **history** **of** **right** **hip pain.** **What** **is** **the** **most** **appropriate** **surgical** **treatment** **for** **this** **fracture?**
A. **Cemented** **unipolar** **hemiarthroplasty** B. **Cemented** **bipolar** **hemiarthroplasty** C. **Total** **hip** **replacement**
D. Open reduction and internal fixation
**CORRECT ANSWER: C**
DISCUSSION:
This patient has pre-existing right hip osteoarthritis. The most correct option for the treatment of this active patient is a right total hip arthroplasty. Hemiarthroplasty would not address the patient's pain from osteoarthritis, and open reduction and internal fixation would not fix the femoral head issue or the
osteoarthritis.
**Question 55**
**Figures** **below** **show** **the** **clinical** **photograph** **and** **radiograph** **obtained** **from** **a** **62-year-old** **man** **who** **has**
**deformity** **and** **pain** **1** **year** **after** **primary** **total** **hip** **arthroplasty.** **What** **is** **the** **reason** **for** **the** **observed deformity?**
A. **A** **Vancouver** **type** **B1** **fracture**
B. **Residual** **leg-length** **discrepancy**
C. **Loosening** **and** **subsidence** **of** **the** **femoral** **stem** **into** **anteversion**
D. Loosening and subsidence of the femoral stem into retroversion
**CORRECT ANSWER: D**
DISCUSSION:
Figure 1 reveals an external rotation deformity of the right lower extremity. This deformity can have numerous causes, including extra-articular deformity. Figure 2 reveals a loose, subsided femoral component. Femoral stems typically subside into retroversion due to proximal femoral biomechanics, which cause a compensatory external rotation deformity. The combined findings from both images suggest an external rotation deformity most likely related to subsidence into retroversion.
**Question 56**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **an** **86-year-old-woman** **who** **has** **had** **chronic** **left** **hip**
**pain** **for** **several** **years.** **She** **now** **uses** **a** **walker** **and** **a** **wheelchair** **for** **ambulation.** **She** **is** **medically** **healthy. What** **is** **the** **most** **appropriate** **surgical** **intervention?**
A. **Cemented** **left** **total** **hip** **arthroplasty** **(THA)**
B. **Cementless** **left** **THA** **with** **a** **proximally** **porous** **coated** **femoral** **stem**
C. **Hybrid** **left** **THA**
D. Cementless left THA with a diaphyseal engaging conical femoral stem
**CORRECT ANSWER: C**
DISCUSSION:
This 86-year-old woman has poor bone quality and osteoarthritis of the left hip. Her lateral radiograph confirms Dorr type C bone quality. A hybrid left THA with a cemented femoral stem would be the treatment of choice.
**Question 57**
**Figure** **below** **shows** **the** **radiograph** **obtained** **from** **a** **76-year-old** **woman** **who** **has** **sharp** **pain** **in** **her** **groin,**
**thigh,** **and** **buttocks** **that** **worsens** **with** **activity.** **She** **has** **been** **dealing** **with** **this** **pain** **for** **more** **than** **a** **year but** **is** **otherwise** **healthy.** **Recently,** **she** **has** **begun** **to** **notice** **night** **pain.** **The** **pain** **no** **longer** **responds** **to NSAIDs.** **She** **would** **like** **to** **be** **able** **to** **dance** **at** **her** **daughter's** **wedding** **in** **4** **months** **and** **wonders** **how** **best**
**to** **proceed.** **What** **is** **the** **best** **next** **step?**
A. **Radiograph-guided** **steroid** **injection** **followed** **by** **total** **hip** **arthroplasty** **6** **weeks** **later**
B. **Total** **hip** **arthroplasty**
C. **Physical** **therapy**
D. Referral back to her spine surgeon
**CORRECT ANSWER: C**
DISCUSSION:
The next best course of action is total hip arthroplasty. The patient is an otherwise healthy woman requesting pain relief and expresses a desire to be dancing in 4 months. She has had more than 6 months of symptoms that are classic hip osteoarthritis symptoms, with pain in the groin and thigh. Severe osteoarthritis is seen in the radiograph as well. NSAIDs are no longer working. Given the objective findings, the subjective reports, and the duration of symptoms, this patient merits surgery. Consideration for steroid injection is reasonable, but given her desire to be dancing in 4 months, an injection would increase her risk of infection if total hip arthroplasty were to be performed within 3 months of the
injection.
**Question 58**
**A** **68-year-old** **woman** **underwent** **an** **uncemented** **medial/lateral** **tapered** **femoral** **placement** **during** **a** **total**
**hip** **arthroplasty.** **The** **orthopaedic** **surgeon** **noticed** **a** **nondisplaced** **vertical** **fracture** **in** **the** **calcar** **region** **of the** **femoral** **neck** **during** **final** **implant** **insertion.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Removal** **of** **the** **press-fit** **implant** **and** **cementing** **of** **the** **same** **femoral** **stem**
B. **Removal** **of** **the** **uncemented** **femoral** **component** **and** **placement** **of** **a** **revision** **modular** **taper- fluted** **femoral** **stem**
C. **Removal** **of** **the** **implant,** **placement** **of** **a** **cerclage** **wire** **around** **the** **femoral** **neck** **above** **the** **lesser trochanter,** **and** **reinsertion** **of** **the** **implant**
D. Final seating of the uncemented femoral component without additional measures
**CORRECT ANSWER: C**
DISCUSSION:
The recognized treatment for a proximal periprosthetic fracture is to first identify the extent and then optimize the correction of the fracture. Several studies indicate that proximal cerclage wiring is adequate to create "barrel hoop" stability of the proximal femur. Braided cables offer superior stability compared with twisted wires or Luque wires. Finally, the appropriate postoperative treatment is protected
weight bearing for 6 weeks, with periodic radiographs taken at 2-week intervals. Other options such as
cementing the femoral stem and using a revision arthroplasty device are indicated for unstable fractures.
**Question 59**
**Injury** **to** **the** **popliteal** **artery** **during** **total** **knee** **arthroplasty** **(TKA)** **is** **most** **likely** **to** **occur** **when** **placing** **a**
**sharp** **retractor**
A. **directly** **posterior** **to** **the** **posterior** **cruciate** **ligament** **(PCL).**
B. **posteromedial** **to** **the** **PCL.**
C. **posterolateral** **to** **the** **PCL.**
D. in the posteromedial corner of the knee.
**CORRECT ANSWER: C**
DISCUSSION:
Vascular complications during TKA are rare but do occur. Traditionally, it was taught that the popliteal artery was situated posterior to the PCL; however, more recent anatomic dissections have demonstrated that this artery is usually located posterolateral to the PCL.
**Question 60**
**A** **70-year-old** **woman** **has** **a** **3-year** **history** **of** **gradually** **increasing** **diffuse** **and** **global** **right** **knee** **pain.** **Her**
**main** **issues** **are** **difficulty** **with** **stairs,** **stiffness** **with** **prolonged** **sitting,** **and** **swelling.** **She** **has** **taken** **NSAIDs and** **has** **received** **intra-articular** **steroid** **injections,** **all** **with** **decreasing** **efficacy.** **Her** **right** **knee** **examination reveals** **a** **range** **of** **motion** **of** **15°** **to** **80°** **with** **a** **fixed** **deformity** **to** **varus** **and** **valgus** **stress.** **Her** **symptoms are** **no** **longer** **manageable** **nonsurgically.** **Radiographs** **reveal** **a** **30-degree** **mechanical** **axis** **deformity. When** **using** **the** **measured** **resection** **technique** **during** **total** **knee** **arthroplasty** **(TKA),** **the** **best** **way** **to** **avoid femoral** **malrotation** **is** **to** **reference** **the**
A. **anteroposterior** **axis.**
B. **tibial** **intramedullary** **axis.**
C. **posterior** **condylar** **axis.**
D. femoral intramedullary axis.
**CORRECT ANSWER: A**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point, can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking
or instability, which is a common complication associated with primary TKA.
**Question 61**
**A** **70-year-old** **woman** **has** **a** **3-year** **history** **of** **gradually** **increasing** **diffuse** **and** **global** **right** **knee** **pain.** **Her**
**main** **issues** **are** **difficulty** **with** **stairs,** **stiffness** **with** **prolonged** **sitting,** **and** **swelling.** **She** **has** **taken** **NSAIDs and** **has** **received** **intra-articular** **steroid** **injections,** **all** **with** **decreasing** **efficacy.** **Her** **right** **knee** **examination reveals** **a** **range** **of** **motion** **of** **15°** **to** **80°** **with** **a** **fixed** **deformity** **to** **varus** **and** **valgus** **stress.** **Her** **symptoms are** **no** **longer** **manageable** **nonsurgically.** **Radiographs** **reveal** **a** **30-degree** **mechanical** **axis** **deformity. The** **deformity** **shown** **in** **Figure** **below** **is** **predominantly** **associated** **with**
A. **a** **hypoplastic** **lateral** **femoral** **condyle.**
B. **a** **contracted** **medial** **collateral** **ligament.**
C. **an** **excessive** **proximal** **tibial** **slope.**
D. trochlear dysplasia.
**CORRECT ANSWER: A**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point, can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking
or instability, which is a common complication associated with primary TKA.
**Question 62**
**Figures** **below** **show** **the** **radiographs,** **and** **the** **MRIs** **obtained** **from** **a** **32-year-old** **man** **with** **worsening** **left**
**knee** **pain.** **A** **3-foot** **hip-to-ankle** **radiograph** **shows** **a** **13-degree** **varus** **knee** **deformity.** **The** **patient sustained** **a** **major** **left** **knee** **injury** **5** **years** **ago** **and** **a** **confirmed** **complete** **anterior** **cruciate** **ligament** **(ACL) tear.** **He** **managed** **this** **injury** **nonsurgically** **with** **a** **functional** **brace** **but** **experienced** **worsening** **pain.** **He was** **seen** **by** **an** **orthopaedic** **surgeon** **18** **months** **ago,** **and** **a** **medial** **meniscus** **tear** **was** **diagnosed;** **the** **tear was** **treated** **with** **an** **arthroscopic** **partial** **medial** **meniscectomy.** **Since** **then,** **his** **knee** **has** **been** **giving** **way more** **often,** **and** **he** **no** **longer** **feels** **safe** **working** **on** **a** **pitched** **roof.** **The** **patient** **received** **6** **months** **of** **formal physical** **therapy** **and** **was** **fitted** **for** **a** **new** **functional** **ACL** **brace,** **but** **he** **still** **has** **pain** **and** **instability.** **He believes** **he** **has** **exhausted** **his** **nonsurgical** **options** **and** **would** **like** **to** **undergo** **surgery.** **What** **is** **the** **most appropriate** **treatment** **at** **this** **time?**
A. **ACL** **reconstruction** **and** **subsequent** **proximal** **tibial** **osteotomy**
B. **ACL** **reconstruction** **alone**
C. **Distal** **femoral** **osteotomy** **with** **simultaneous** **ACL** **reconstruction**
D. Proximal tibial osteotomy with subsequent ACL reconstruction
**CORRECT ANSWER: D**
DISCUSSION:
Proximal tibial osteotomy is the most appropriate intervention to correct varus malalignment and to reduce stress on the ACL. In some cases, proximal tibial osteotomy alone may address both pain and instability, but if instability persists, particularly in the setting in which instability can be dangerous, subsequent ACL reconstruction can further stabilize the knee with less stress on the graft after the correction of malalignment. Varus alignment places increased stress on the native or reconstructed ACL. ACL reconstruction should be performed only at the same time as or following proximal tibial osteotomy to correct alignment in the setting of varus malalignment. It is not appropriate to perform ACL reconstruction prior to proximal tibial osteotomy in this setting. Distal femoral osteotomy is not indicated to correct varus malalignment. Varus alignment places increased stress on the native or reconstructed ACL, and ACL
reconstruction alone is not indicated for this patient.
**Question 63**
**When** **balancing** **gaps** **in** **the** **coronal** **plane,** **what** **structure** **preferentially** **impacts** **the** **flexion** **space** **more**
**than** **the** **extension** **space?**
A. **Iliotibial** **band**
B. **Popliteus** **tendon**
C. **Lateral** **collateral** **ligament**
D. **Lateral** **head** **of** **the** **gastrocnemius**
**CORRECT ANSWER: B**
DISCUSSION:
In the setting of valgus deformities, TKA poses different challenges than those encountered when varus deformities are present. Most valgus alignment is attributable to a deformity of the distal femur rather than of the proximal tibia, as seen in varus knees. One of the major anatomical differences is a hypoplastic lateral femoral condyle which, when not recognized and used as a rotational reference point,
can lead to internal rotation of the femoral component. This malrotation in turn leads to patellofemoral maltracking or instability, which is a common complication associated with primary TKA.
**Question 64**
**A** **45-year-old** **woman** **has** **severe** **anterior** **knee** **pain.** **Her** **radiographs** **indicate** **end-stage** **patellofemoral**
**compartment** **osteoarthritis.** **The** **tibiofemoral** **compartments** **are** **preserved.** **Extensive** **nonsurgical treatment** **has** **failed** **to** **provide** **relief,** **and** **she** **is** **offered** **patellofemoral** **arthroplasty** **(PFA).** **What** **is** **the most** **common** **long-term** **mode** **of** **failure** **for** **PFA** **using** **an** **implant** **with** **an** **onlay** **prosthesis** **design?**
A. **Infection**
B. **Patellar** **instability**
C. **Aseptic** **loosening**
D. Progression of tibiofemoral arthritis
**CORRECT ANSWER: D**
DISCUSSION:
Contemporary onlay-design trochlear prostheses in PFA replace the entire anterior trochlear surface. Previous inlay designs were inset within the native trochlea and carried a higher risk of catching and patellar instability, particularly in patients with trochlear dysplasia; they also generally have higher failure rates. The current most common mode of failure is progression of arthritis throughout the knee, in some series as high as 25% at 15 years. Aseptic loosening, particularly of cemented implants, is less common. Infection is an uncommon long-term complication. Patients considering PFA should be advised of the risk of arthritis progression. Many authors routinely obtain a preoperative MRI to assess the status of the tibiofemoral compartments.
**Question 65**
**Figures** **below** **show** **the** **radiographs** **obtained** **from** **a** **79-year-old** **woman** **who** **has** **been** **experiencing**
**increasing** **tibial** **pain** **10** **years** **after** **undergoing** **revision** **total** **knee** **arthroplasty.** **No** **evidence** **of** **infection is** **seen.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Retain** **the** **components,** **and** **implant** **a** **tibial** **strut** **allograft.**
B. **Revise** **the** **tibial** **component** **with** **a** **metaphyseal** **cone** **and** **metaphyseal** **uncemented** **stem.**
C. **Revise** **the** **tibial** **component** **with** **a** **metaphyseal** **cone** **and** **a** **press-fit** **diaphyseal-engaging** **stem.**
D. Revise the tibial component with a long cemented diaphyseal-engaging stem.
**CORRECT ANSWER: C**
DISCUSSION:
---
Stems are available for cemented and press-fit implantation. To be effective, press-fit stems should engage the diaphysis, as shown in Figures 3 and 4. They also assist in obtaining correct limb alignment. Short metaphyseal-engaging stems are associated with failure rates that range between 16% and 29%. Cemented stems may be shorter than press-fit stems, because they do not have to engage the diaphysis. Short, fully cemented stems offer the advantage of metaphyseal fixation. Hybrid stem fixation makes use of the metaphysis for cement fixation with metaphyseal cones or sleeves and diaphyseal-engaging press-fit stems.
**Question 66**
**A** **70-year-old** **man** **reports** **symptomatic** **medial** **knee** **pain** **that** **has** **become** **progressively** **worse** **during**
**the** **past** **year.** **MRI** **reveals** **a** **complex,** **posterior** **horn** **medial** **meniscus** **tear** **with** **associated** **medial** **lateral and** **patellofemoral** **cartilage** **defects.** **Radiographs** **reveal** **medial** **joint** **space** **narrowing** **and** **osteophytes** **in the** **other** **compartments.** **What** **treatment** **is** **most** **likely** **to** **provide** **long-term,** **durable** **relief** **of** **symptoms?**
A. **High** **tibial** **osteotomy**
B. **Total** **knee** **replacement**
C. **Unicondylar** **knee** **replacement**
D. Arthroscopic partial meniscectomy
**CORRECT ANSWER: B**
DISCUSSION:
Total knee replacement is a well-established surgery for diffuse, symptomatic osteoarthritis of the knee joint, and its efficacy has been shown in many studies. According to the 2008 AAOS Clinical Practice Guideline, Treatment of Osteoarthritis of the Knee, arthroscopy in the setting of existing osteoarthritis is efficacious for relieving the signs and symptoms of a torn meniscus but not for osteoarthritis. Likewise, in young and active patients, clinical outcomes show improvement after realignment osteotomy for single- compartment osteoarthritis. Unicondylar knee replacement is not indicated for tricompartmental disease
of the knee.
**Question 67**
**A** **58-year-old** **man** **with** **insulin-dependent** **diabetes** **mellitus** **underwent** **primary** **total** **knee** **arthroplasty**
**(TKA).** **A** **full-thickness** **skin** **slough** **measuring** **3** **cm** **by** **4** **cm** **developed,** **with** **postsurgical** **exposure** **of the** **patellar** **tendon.** **No** **change** **is** **observed** **in** **the** **appearance** **of** **the** **wound** **after** **2** **weeks** **of** **wet-to-dry dressing** **changes.** **What** **is** **the** **best** **next** **treatment** **step** **for** **the** **soft-tissue** **defect?**
A. **Continued** **dressing** **changes**
B. **Split-thickness** **skin** **graft** C. **Full-thickness** **skin** **graft** D. **Local** **rotational** **flap**
**CORRECT ANSWER: D**
DISCUSSION:
If wound healing does not occur and deep soft tissues such as the patellar tendon are exposed following TKA, local rotational flap is the procedure of choice. The procedure should be performed relatively early after the recognition of a soft-tissue wound-healing problem. In the setting of TKA, the gastrocnemius muscle is an excellent source of flaps for wound coverage of the proximal tibia.
**Question 68**
**A** **77-year-old** **man** **who** **underwent** **right** **total** **knee** **replacement** **surgery** **2** **and** **a** **half** **years** **ago** **has** **had knee** **pain** **since** **surgery.** **The** **pain** **is** **diffuse,** **constant,** **and** **made** **worse** **with** **activity.** **He** **notes** **warmth and** **swelling** **in** **his** **knee.** **Examination** **shows** **a** **well-healed** **incision,** **no** **erythema,** **moderate** **warmth, synovitis,** **and** **an** **effusion.** **The** **knee** **is** **stable,** **and** **has** **an** **arc** **of** **flexion** **between** **3°** **and** **120°.** **Radiographs show** **well-fixed** **and** **well-aligned** **implants.** **What** **is** **the** **most** **appropriate** **initial** **treatment?**
A. **Knee** **aspiration** **for** **culture**
B. **CT** **of** **the** **knee** **to** **assess** **implant** **rotation**
C. **Indium-111** **leukocyte/technetium-99m** **sulfur** **colloid** **scan** **of** **the** **knee**
D. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) laboratory studies
**CORRECT ANSWER: D**
DISCUSSION:
This patient's history and physical findings are concerning for deep infection. Inflammatory markers, including ESR and CRP, should be obtained first. If the levels are elevated, knee aspiration should be performed for the synovial cell count and culture. A bone scan is not indicated in an initial investigation for deep infection; it is rarely helpful and is not cost effective. CT to assess implant rotation is an appropriate investigation for knee pain when the clinical scenario is not suspicious for a deep infection
and when infection has been excluded.
**Question 69**
**A** **61-year-old** **man** **with** **a** **body** **mass** **index** **of** **31** **had** **a** **6-month** **gradual** **onset** **of** **right** **medial** **knee** **pain.**
**Examination** **revealed** **a** **small** **effusion,** **stable** **ligaments,** **a** **normally** **tracking** **patella,** **and** **mild** **medial joint** **line** **tenderness.** **Standing** **radiographs** **show** **mild** **medial** **joint** **space** **narrowing.** **Effective** **treatment at** **this** **stage** **of** **early** **medial** **compartmental** **osteoarthritis** **includes**
A. **glucosamine** **1,500** **mg/day** **and** **chondroitin** **sulfate** **800** **mg/day.**
B. **weight** **loss** **through** **dietary** **management** **and** **low-impact** **aerobic** **exercises.**
C. **arthroscopic** **debridement** **and** **lavage.**
D. a valgus-directing brace.
**CORRECT ANSWER: B**
DISCUSSION:
According to the 2008 AAOS Clinical Practice Guideline, Treatment of Osteoarthritis of the Knee (Nonarthroplasty), level 1 evidence confirms that weight loss and exercise benefit patients with knee osteoarthritis. The other responses have either inclusive evidence (a valgus-directing brace) or no evidence to support their use (glucosamine 1,500 mg/day and chondroitin sulfate 800 mg/day as well as
arthroscopic debridement and lavage).
**Question 70**
**In** **patients** **with** **Crowe** **types** **III** **and** **IV** **developmental** **dysplasia** **of** **the** **hip** **with** **high** **hip** **centers,**
**acetabular** **reconstruction** **often** **requires** **lowering** **the** **acetabular** **component** **into** **the** **native** **acetabulum. In** **doing** **so,** **considerable** **risk** **for** **limb** **lengthening** **beyond** **4** **cm** **exists,** **making** **the** **hip** **difficult** **to** **reduce and** **raising** **the** **risk** **for** **nerve** **injury.** **Which** **technique** **is** **used** **to** **overcome** **this** **problem?**
A. **Subtrochanteric** **osteotomy** **with** **femoral** **shortening**
B. **An** **offset** **femoral** **component**
C. **A** **lateralized** **liner**
D. **Extended** **trochanteric** **osteotomy**
**CORRECT ANSWER: A**
DISCUSSION:
---
When substantial lengthening of a dysplastic hip will occur because a high dislocation is relocated into a considerably lower acetabulum, a femoral shortening may be necessary to reduce the hip and avoid a stretch injury to the sciatic nerve. No other choice specifically addresses the need for femoral shortening, and high offset stems and lateralized liners may exacerbate the problem if used alone and without femoral shortening.
**Question 71**
What factor is considered one of the early changes in osteoarthritic cartilage?
A. Decreased water content
B. Increased proteoglycan content
C. Decreased loading of the solid matrix
D. Increased cartilage tissue permeability
**CORRECT ANSWER: D**
DISCUSSION:
The normal regulation of a cartilage surface is a delicate balance of degradation and synthesis. When this normal regulation of the cartilage is disturbed, a proinflammatory state tips the cellular pathway in the direction of degradation. The proinflammatory state upregulates the production of cytokines and proteolytic enzymes, specifically matrix metalloproteinases. These enzymes attack the proteoglycan content of the cartilage, leading to an overall reduction in the proteoglycan content. This reduction in content leads to increased permeability of the cartilage substrate. With increased permeability, water is able to move into the cartilage itself, thereby increasing the overall water content within the cartilage in an arthritic state. Finally, because of the increased permeability and increased water content, the overall load or pressure placed on the underlying solid matrix is increased. Increased water content, decreased proteoglycan content, and an increased load on the solid matrix are typical of an osteoarthritic process within normal cartilage. Therefore, the only correct option is that the cartilage has an increased amount
of permeability in osteoarthritis.
**Question 72**
**A** **47-year-old** **obese** **man** **with** **a** **body** **mass** **index** **of** **42** **comes** **into** **the** **office** **with** **left** **knee** **pain** **1** **year**
**after** **undergoing** **an** **uncomplicated** **left** **medial** **unicompartmental** **knee** **arthroplasty** **(UKA).** **Radiographs show** **a** **loose** **tibial** **component** **in** **varus.** **What** **is** **the** **most** **appropriate** **next** **step** **to** **treat** **this** **failed construct?**
A. **Aspiration** **of** **joint** **fluid** **to** **obtain** **a** **cell** **count**
B. **Revision** **of** **the** **UKA** **using** **primary** **total** **knee** **arthroplasty** **(TKA)** **components**
C. **Revision** **of** **the** **UKA** **using** **a** **revision** **TKA** **with** **augments**
D. Procurement of the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) level
**CORRECT ANSWER: D**
DISCUSSION:
This patient likely is experiencing failure of the UKA secondary to poor patient selection. In this young, heavy man, the component likely loosened due to the ongoing varus alignment of the knee and his elevated
weight. Despite this likely scenario, the next step is determining whether an infection is the cause of his pain. Prior to obtaining an aspiration, the surgeon can order ESR and CRP studies to determine whether aspiration is warranted. If the laboratory studies are unremarkable, the surgeon likely can forgo the
aspiration and proceed to a revision TKA with possible augments on standby.
**Question 73**
Figure below shows the standing AP radiograph obtained from a 55-year-old man who has a 5-year history of
daily left knee medial joint line pain with weight-bearing activities. He denies night pain or symptoms of instability. On examination, his range of motion is 0° to 140°. He has a mild, fully correctable varus deformity and a negative Lachman test result. Nonsurgical treatment has failed. What is the UKA survivorship for a 55- year-old patient, compared with the survivorship for total knee arthroplasty?
A. Equal at 10 years B. Lower at 10 years C. Higher at 10 years
D. Not known when using a mobile-bearing UKA
**CORRECT ANSWER: B**
DISCUSSION:
A patient with medial compartment arthritis and a correctable varus deformity with no clinical or examination findings of knee instability most likely has an intact anterior cruciate ligament (ACL). The pattern of medial compartment osteoarthritis most commonly associated with an intact ACL is that of anteromedial osteoarthritis. An incompetent ACL is commonly associated with a fixed varus deformity and radiographic signs of posteromedial wear. An incompetent ACL is a relative contraindication to a mobile-bearing UKA. When evaluating patients for a mobile-bearing UKA, a stress radiograph aids the orthopaedic surgeon in determining the correction of the varus deformity and assessing the lateral compartment. An inability to fully correct the deformity or narrowing of the lateral compartment with valgus stress should influence the surgeon against UKA. Joint registries across the world have shown decreased survivorship associated with TKA and UKA in men compared with other age groups, but survivorship is lower for UKA than for TKA. No studies to date have shown any differences in survivorship between fixed-bearing and mobile-bearing UKAs. The complication that is unique to mobile-bearing UKA is bearing spinout, which occurs in less than 1% of mobile-bearing UKA procedures. In vivo and in vitro polyethylene wear in mobile-bearing UKA are low. Arthritis may progress
faster in patients with mobile-bearing UKAs than in those with fixed-bearing UKAs.
**Question 74**
**A** **57-year-old** **woman** **experiences** **pain** **1** **year** **after** **total** **knee** **arthroplasty** **(TKA).** **She** **reports** **sharp**
**anterior** **pain** **and** **a** **painful** **catching** **sensation** **that** **is** **aggravated** **by** **rising** **from** **a** **chair** **or** **climbing** **stairs. Physical** **examination** **reveals** **a** **mild** **effusion** **and** **a** **range** **of** **motion** **of** **2°** **to** **130°,** **with** **patellar** **crepitus.**
**The** **symptoms** **are** **reproduced** **by** **resisted** **knee** **extension.** **Radiographs** **show** **a** **well-aligned** **posterior- stabilized** **TKA** **without** **evidence** **of** **component** **loosening.** **What** **is** **the** **most** **likely** **cause** **of** **this** **patient's pain?**
A. **Patellar** **clunk** **syndrome**
B. **Flexion** **gap** **instability**
C. **Polyethylene** **wear**
D. Femoral component malrotation
**CORRECT ANSWER: A**
DISCUSSION:
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
**Question 75**
**In** **total** **knee** **arthroplasty,** **in** **vitro** **testing** **has** **shown** **that** **cross-linking** **can** **diminish** **the** **rate** **of**
**polyethylene** **wear** **by** **30%** **to** **80%.** **What** **other** **change** **in** **material** **properties** **is** **possible** **when polyethylene** **is** **highly** **cross-linked?**
A. **Increased** **ductility**
B. **Increased** **wettability**
C. **Diminished** **fatigue** **strength**
D. Decreased resistance to abrasive wear
**CORRECT ANSWER: C**
DISCUSSION:
The most important concern regarding highly cross-linked polyethylene relates to decreased mechanical properties. Cross-linking results in reduced ductility, tensile strength, and fatigue crack propagation resistance. These problems have not been shown to cause implant failure in the most recent clinical trials, but they remain the most important mechanical issues associated with current material processing methods.
**Question 76**
**A** **70-year-old** **woman** **who** **underwent** **total** **knee** **replacement** **18** **months** **ago** **has** **had** **3** **weeks** **of** **moderate**
**drainage** **from** **a** **previously** **healed** **wound.** **What** **is** **the** **most** **appropriate** **treatment?**
A. **Vacuum-assisted** **wound** **closure** **dressing**
B. **Intravenous** **antibiotics** **for** **6** **weeks,** **followed** **by** **long-term** **oral** **antibiotic** **administration**
C. **Irrigation** **and** **debridement,** **followed** **by** **polyethylene** **exchange**
D. Two-stage debridement and reconstruction
**CORRECT ANSWER: D**
DISCUSSION:
This situation represents a definitively and chronically infected knee replacement. Antibiotic therapy alone might suppress the infection but would not eradicate it. Debridement and polyethylene exchange would be appropriate treatment for an early postoperative infection. The treatment of choice is to perform a two-stage debridement and reconstruction. Although not among the listed choices, an aspiration or culture could be done presurgically and might help clinicians identify the best antibiotics to treat the condition. Antibiotic selection would not affect the need for the two-stage reconstruction, however.
**Question 77**
During a posterior cruciate ligament (PCL)-retaining total knee arthroplasty, a critical principle to remember
is to
A. accurately tension the PCL.
B. use bony resection to adjust the joint line.
C. maintain a small amount of residual deformity.
D. use intraoperative fluoroscopy to ensure femoral roll back.
**CORRECT ANSWER: A**
DISCUSSION:
Maintenance of the joint line and accurately tensioning the PCL are critical in the proper execution of a PCL-retaining total knee arthroplasty. Appropriate tension helps ensure femoral rollback and avoid stiffness or instability. Raising the joint line to help ensure full extension should be avoided in cruciate- retaining knees, because doing so creates an unfavorable kinematic environment. The three important principles of surgical technique needed to maintain appropriate tensioning of the PCL include 1) choosing the proper femur size to reproduce the native femoral anterior/posterior dimension, 2) reproducing the joint line by resecting as much tibia from the healthy side as will be replaced by the smallest thickness of the tibial component and, 3) ensuring that full extension is achieved by soft-tissue releases and not by taking additional distal femur, as may be done in a posterior stabilized approach. Another important principle is to re-create the natural degree of the patient’s posterior tibial slope to avoid tightness in
flexion.
**Question 78**
**Figures** **below** **depict** **the** **AP** **and** **lateral** **radiographs** **obtained** **from** **a** **64-year-old** **man** **with** **long-standing**
**right** **knee** **osteoarthritis** **and** **pain** **that** **is** **unresponsive** **to** **nonsurgical** **treatment.** **The** **patient** **undergoes navigated** **cruciate-retaining** **right** **total** **knee** **arthroplasty.** **After** **surgery,** **this** **patient** **continues** **to experience** **pain** **and** **swelling** **of** **the** **knee** **with** **recurrent** **effusions.** **He** **returns** **to** **the** **office** **reporting continued** **pain** **2** **years** **after** **surgery.** **He** **describes** **instability,** **particularly** **when** **descending** **stairs.** **On examination,** **range** **of** **motion** **of** **0°** **to** **120°** **is** **observed,** **with** **no** **extensor** **lag.** **Slope** **of** **the** **tibial** **component is** **7°.** **The** **knee** **is** **stable** **to** **varus** **and** **valgus** **stress** **in** **extension,** **but** **flexion** **instability** **is** **present** **in** **both the** **anterior-posterior** **direction** **and** **the** **varus-valgus** **direction.** **Bracing** **leads** **to** **a** **slight** **decrease** **in symptoms** **but** **is** **not** **well** **tolerated.** **Isokinetic** **testing** **demonstrates** **decreased** **knee** **extension** **velocity** **at**
**mid** **push.** **Radiographs** **demonstrate** **well-aligned** **and** **fixed** **knee** **implants.** **An** **infection** **work-up** **is negative.** **What** **is** **the** **most** **appropriate** **surgical** **intervention** **at** **this** **time?**
A. **Tibial** **polyethylene** **exchange**
B. **Revision** **of** **the** **femoral** **and** **tibial** **components** **and** **conversion** **to** **a** **posterior** **stabilized** **insert**
C. **Revision** **of** **the** **femoral** **and** **tibial** **components** **to** **a** **constrained** **rotating** **hinge** **prosthesis**
D. **Isolated** **femoral** **component** **revision** **and** **upsizing** **of** **the** **femoral** **implant** **with** **a** **new** **posterior cruciate** **ligament** **(PCL)-retaining** **polyethylene** **insert**
**CORRECT ANSWER: B**
DISCUSSION:
The patient’s symptoms at follow-up—pain, swelling, and difficulty descending stairs—suggest knee flexion instability. Considering his history, an incompetent PCL must be considered. Revision of the knee to a posterior stabilized or nonlinked constrained condylar implant (depending on the condition of the ligaments) likely is needed to address his symptoms. The difference in extension stability and flexion stability makes polyethylene exchange a poor option. A constrained rotating hinge design is not necessary. Repeat use of a PCL-retaining insert is not recommended. Tibial and femoral revision both are required. Correction of excessive slope will be attained with tibial revision, femoral component revision is required to convert to a PCL-substituting design. There is also an opportunity to increase posterior condylar offset if needed.
**Question 79**
**Figure** **below** **shows** **the** **standing** **AP** **radiograph** **obtained** **from** **a** **55-year-old** **man** **who** **has** **a** **5-year** **history**
**of** **daily** **left** **knee** **medial** **joint** **line** **pain** **with** **weight-bearing** **activities.** **He** **denies** **night** **pain** **or** **symptoms of** **instability.** **On** **examination,** **his** **range** **of** **motion** **is** **0°** **to** **140°.** **He** **has** **a** **mild,** **fully** **correctable** **varus deformity** **and** **a** **negative** **Lachman** **test** **result.** **Nonsurgical** **treatment** **has** **failed.** **Unicompartmental** **knee arthroplasty** **(UKA)** **is** **discussed** **with** **the** **patient.** **The** **most** **appropriate** **next** **radiographic** **evaluation should** **be**
**A.** **MRI** **of** **the** **left** **knee** **to** **evaluate** **the** **lateral** **compartment.**
**B.** **a** **CT** **arthrogram** **to** **evaluate** **the** **status** **of** **the** **medial** **and** **lateral** **meniscus. C.** **a** **stress** **radiograph** **to** **evaluate** **correction** **of** **the** **varus** **deformity.**
D. a sunrise view to determine the status of the patellofemoral joint.
**CORRECT ANSWER: C**
DISCUSSION:
A patient with medial compartment arthritis and a correctable varus deformity with no clinical or examination findings of knee instability most likely has an intact anterior cruciate ligament (ACL). The pattern of medial compartment osteoarthritis most commonly associated with an intact ACL is that of anteromedial osteoarthritis. An incompetent ACL is commonly associated with a fixed varus deformity and radiographic signs of posteromedial wear. An incompetent ACL is a relative contraindication to a mobile-bearing UKA. When evaluating patients for a mobile-bearing UKA, a stress radiograph aids the orthopaedic surgeon in determining the correction of the varus deformity and assessing the lateral compartment. An inability to fully correct the deformity or narrowing of the lateral compartment with valgus stress should influence the surgeon against UKA. Joint registries across the world have shown decreased survivorship associated with TKA and UKA in men compared with other age groups, but survivorship is lower for UKA than for TKA. No studies to date have shown any differences in survivorship between fixed-bearing and mobile-bearing UKAs. The complication that is unique to mobile-bearing UKA is bearing spinout, which occurs in less than 1% of mobile-bearing UKA procedures. In vivo and in vitro polyethylene wear in mobile-bearing UKA are low. Arthritis may progress
faster in patients with mobile-bearing UKAs than in those with fixed-bearing UKAs.
**Question 80**
**Compared** **with** **retention** **of** **the** **native** **patella** **in** **primary** **total** **knee** **arthroplasty,** **routine** **patellar**
**resurfacing** **is** **associated** **with**
A. **no** **patellar** **complications.**
B. **an** **increased** **occurrence** **of** **anterior** **knee** **pain.**
C. **a** **reduced** **patellar** **fracture** **rate.**
D. a reduced risk for revision surgery.
**CORRECT ANSWER: D**
DISCUSSION:
Despite concerns regarding fracture, osteonecrosis, and patellar clunk, the routine retention of the native patella during primary total knee replacement is associated with a 20% to 30% increased revision risk in
large joint registries. In addition, the retention of the native patella results in a 5.7% revision surgery rate
in patients with anterior knee pain.
**Question 81**
**A** **surgeon** **prepares** **a** **medial** **gastrocnemius** **rotational** **flap** **to** **cover** **a** **medial** **proximal** **tibia** **defect** **at** **the**
**time** **of** **revision** **knee** **replacement** **surgery.** **To** **optimize** **coverage,** **the** **surgeon** **must** **optimally** **mobilize which** **artery?**
A. **Profunda** **femoris** B. **Middle** **genicular** C. **Medial** **sural**
D. Inferior medial genicular
**CORRECT ANSWER: C**
DISCUSSION:
The medial sural arteries vascularize the gastrocnemius, plantaris, and soleus muscles proximally. These arteries arise from the popliteal artery. If this artery is not adequately mobilized, a gastrocnemius soleus flap can be devascularized.
**Question 82**
Figures below represent the radiographs obtained from a 37-year-old man with severe right knee pain. He has
a history of prior tibial osteotomy for adolescent tibia vara but notes residual bowing of his legs. On examination, he is 5'8" tall and weighs 322 pounds. He has a waddling gait with a bilateral varus thrust and
20° varus deformity of both legs. His right knee range of motion is 0° to 120° with a fixed varus deformity. What is the best next step?
A. Total knee arthroplasty with standard components
B. Correction of tibial deformity with osteotomy and nonsurgical management of the osteoarthritis
C. Arthrodesis with a long antegrade nail
D. Total knee arthroplasty with a constrained device
**CORRECT ANSWER: D**
DISCUSSION:
This patient has severe, uncorrectable varus deformity and pain from end-stage osteoarthritis secondary to prior adolescent tibia vara. Although he is young to consider arthroplasty, this option is likely to give him the most functional limb, compared with arthrodesis with a long antegrade nail. During arthroplasty surgery, his knee will likely require extensive medial release to achieve anatomic limb alignment. Standard components in total knee arthroplasty likely would result in lateral instability, so this option is
not the best answer. The best choice is total knee arthroplasty with a constrained device, which adds
constraint to the knee to provide balance.
**Question 83**
**An** **85-year-old** **obese** **woman** **has** **left** **knee** **pain.** **She** **had** **surgery** **5** **years** **ago** **for** **a** **patellar** **nonunion** **after**
**total** **knee** **arthroplasty** **that** **was** **complicated** **by** **infection,** **which** **was** **treated** **with** **implant** **removal** **and patellectomy.** **She** **has** **not** **been** **ambulatory** **since** **then.** **She** **states** **she** **is** **no** **longer** **on** **antibiotics.** **She** **has moderate** **pain,** **but** **her** **primary** **problem** **is** **instability** **of** **the** **knee.** **She** **has** **a** **40°** **extensor** **lag.** **Darkening of** **the** **skin** **is** **present** **distal** **to** **the** **incision** **consistent** **with** **venous** **stasis** **changes.** **The** **erythrocyte sedimentation** **rate** **is** **12** **mm/h** **(reference** **range** **0** **to** **20** **mm/h)** **and** **her** **C-reactive** **protein** **level** **is** **1.0** **mg/L**
**(reference** **range** **0.08** **to** **3.1** **mg/L).** **Left** **knee** **aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **800** **and** **20%**
**neutrophils.** **What** **is** **the** **best** **next** **step?**
A. **Revision** **total** **knee** **arthroplasty** **with** **primary** **quadriceps** **tendon** **repair**
B. **Hinged** **knee** **arthroplasty** **with** **full** **extensor** **mechanism** **allograft**
C. **Arthrotomy** **with** **debridement** **and** **antegrade** **knee** **arthrodesis** **nailing**
D. Two-stage revision knee arthroplasty and quadriceps repair with Achilles allograft
**CORRECT ANSWER: C**
DISCUSSION:
This patient is elderly, obese, and nonambulatory and has a chronic quadriceps tendon rupture after infected total knee arthroplasty. Her potential for ambulation after revision total knee arthroplasty is very low. Primary repair of the tendon is unlikely to be successful, even with augmentation, so revision total knee arthroplasty with primary quadriceps tendon repair and two-stage revision knee arthroplasty and quadricep repair with Achilles allograft are not the best management techniques. Extensor mechanism allograft could be done but would have a high failure rate in a patient of this size. No sign of infection is seen, based on laboratory studies, so a two-stage procedure is not necessary. The best management although not optimal, would be treatment in a drop-lock brace. Arthrodesis is also an option, but would have a high complication rate, and in a patient that is nonambulatory, a fused knee would be increasingly
difficult with activities of daily living and mobility.
**Question 84**
**Figures** **below** **depict** **the** **radiographs** **obtained** **from** **a** **53-year-old** **man** **who** **has** **had** **swelling** **in** **his** **right**
**knee** **for** **2** **years,** **with** **minimal** **pain.** **He** **did** **not** **note** **an** **injury** **to** **the** **knee** **but** **has** **been** **unable** **to ambulate** **without** **crutches** **during** **this** **period.** **His** **past** **history** **is** **unremarkable,** **and** **he** **denies** **a** **history**
**of** **diabetes** **or** **back** **problems.** **The** **social** **history** **reveals** **that** **he** **emigrated** **from** **China,** **and** **he** **works** **at** **a desk** **job.** **Physical** **examination** **shows** **a** **healthy** **man** **in** **no** **acute** **distress.** **Range** **of** **motion** **of** **the** **right knee** **is** **5°** **to** **120°** **actively** **and** **0°** **to** **120°** **passively,** **without** **pain.** **Sensation** **is** **decreased** **on** **the** **bottom of** **both** **feet,** **but** **otherwise** **the** **neurologic** **examination** **is** **unremarkable.** **Laboratory** **testing** **reveals** **a positive** **rapid** **plasma** **reagin** **(RPR)** **test.** **What** **is** **the** **best** **next** **step?**
A. **Open** **reduction** **and** **internal** **fixation**
B. **Hinged** **total** **knee** **arthroplasty**
C. **Arthrodesis** **using** **an** **intramedullary** **nail**
D. Irrigation and debridement with spacer placement
**CORRECT ANSWER: B**
DISCUSSION:
This patient has a neuropathic knee caused by neurosyphilis, as shown by the joint destruction on the radiographs, with a lack of pain and a positive RPR test. He has a low-demand job and would be best treated with a hinged knee arthroplasty to provide stability for his knee.
**Question 85**
**At** **the** **time** **of** **revision** **knee** **arthroplasty,** **a** **surgeon** **performs** **a** **rectus** **snip** **to** **gain** **exposure** **to** **the** **knee.**
**When** **compared** **with** **a** **standard** **parapatellar** **approach,** **what** **is** **the** **expected** **outcome?**
A. **Improvement** **in** **range** **of** **motion**
B. **Reduction** **in** **range** **of** **motion**
C. **Increase** **in** **extensor** **mechanism** **lag**
D. No differences in motion and strength
**CORRECT ANSWER: D**
DISCUSSION:
Rectus snip during total knee arthroplasty has no effect on motion or strength at long-term follow-up. It has not been associated with extensor mechanism lag.
**Question 86**
**Hip** **pain** **of** **1-month** **duration** **has** **developed** **in** **a** **72-year-old** **man** **with** **a** **previous** **total** **hip** **arthroplasty.**
**He** **underwent** **dental** **work** **6** **weeks** **ago.** **Aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **more** **than** **6,000 cells/μL** **(reference** **range** **4,500** **to** **11,000** **cells/μL)** **and** **the** **presence** **of** **gram-positive** **cocci** **in** **clusters** **on Gram** **stain.** **The** **orthopaedic** **surgeon** **recommends** **urgent** **debridement** **and** **irrigation.** **Fixation** **of** **the components** **is** **judged** **to** **be** **stable,** **and** **the** **surgeon** **elects** **to** **retain** **the** **implants.** **The** **patient** **has** **a** **final culture** **that** **reveals** **methicillin-resistant** _Staphylococcus aureus_**(MRSA).** **If** **the** **attending** **physician recommends** **the** **two-stage** **protocol,** **including** **the** **use** **of** **an** **antibiotic-cement** **spacer,** **what** **is** **the** **most likely** **prognosis** **for** **this** **patient?**
A. **Better** **functional** **outcome** **than** **that** **associated** **with** **infections** **from** **sensitive** **organisms**
B. **Same** **functional** **outcome** **as** **that** **associated** **with** **infections** **from** **sensitive** **organisms**
C. **Same** **prognosis** **for** **eradication** **of** **infection** **as** **that** **associated** **with** **infections** **from** **sensitive organisms**
D. **Poorer** **prognosis** **for** **eradication** **of** **infection** **than** **that** **associated** **with** **infection** **from** **sensitive organisms**
**CORRECT ANSWER: D**
DISCUSSION:
The patient has a late infection of at least 4 weeks symptomatic duration that most likely is hematogenous in etiology. This infection is not an acute hematogenous infection that can successfully be treated with irrigation and debridement. Retention of the implants with debridement and irrigation alone has been associated with a poor prognosis. In a recent study, the success rate was only 44% in a series of 104 patients at a mean 5.7-year follow-up. In one study of 50 infections attributable to MRSA or methicillin- resistant _Staphylococcus epidermidis_ organisms treated with a two-stage protocol, the failure rate was
21%. Patients who experienced successful infection treatment had lower functional outcome measures using the Western Ontario and McMaster Universities Osteoarthritis Index, the University of California
Los Angeles Activity Score, and the 12-item Oxford Knee Score, however.
**Question 87**
**An** **80-year-old** **African** **American** **woman** **who** **lives** **in** **a** **large** **city** **is** **scheduled** **for** **total** **hip** **arthroplasty**
**to** **address** **primary** **osteoarthritis.** **Part** **of** **the** **presurgical** **protocol** **includes** **nasal** **swab** **screening** **to** **assess for** **methicillin-resistant** _Staphylococcus aureus_**(MRSA)** **colonization.** **Which** **demographic** **factor** **places this** **patient** **at** **highest** **risk** **for** **a** **positive** **result?**
A. **Gender**
B. **Age**
C. **Race**
D. Environment
**CORRECT ANSWER: C**
DISCUSSION:
Demographic factors are associated with increased risk for MRSA colonization, so it is important to identify vulnerable patients. Female gender and advanced age reduce the risk for colonization, whereas African American race increases this risk. Urban environments do not influence MRSA colonization.
**Question 88**
**Hip** **pain** **of** **1-month** **duration** **has** **developed** **in** **a** **72-year-old** **man** **with** **a** **previous** **total** **hip** **arthroplasty. He** **underwent** **dental** **work** **6** **weeks** **ago.** **Aspiration** **shows** **a** **white** **blood** **cell** **count** **of** **more** **than** **6,000**
**cells/μL** **(reference** **range** **4,500** **to** **11,000** **cells/μL)** **and** **the** **presence** **of** **gram-positive** **cocci** **in** **clusters** **on Gram** **stain.** **The** **orthopaedic** **surgeon** **recommends** **urgent** **debridement** **and** **irrigation.** **Fixation** **of** **the components** **is** **judged** **to** **be** **stable,** **and** **the** **surgeon** **elects** **to** **retain** **the** **implants.** **What** **is** **this** **patient's**
**prognosis** **for** **infection** **resolution?**
A. **Good** **because** **it** **is** **a** **gram-positive** **organism**
B. **Good** **because** **it** **is** **an** **acute** **infection**
C. **Poor** **because** **it** **is** **a** **gram-positive** **organism**
D. Poor because it is a late infection
**CORRECT ANSWER: D**
DISCUSSION:
---
The patient has a late infection of at least 4 weeks symptomatic duration that most likely is hematogenous in etiology. This infection is not an acute hematogenous infection that can successfully be treated with irrigation and debridement. Retention of the implants with debridement and irrigation alone has been associated with a poor prognosis. In a recent study, the success rate was only 44% in a series of 104 patients at a mean 5.7-year follow-up. In one study of 50 infections attributable to MRSA or methicillin- resistant _Staphylococcus epidermidis_ organisms treated with a two-stage protocol, the failure rate was
21%. Patients who experienced successful infection treatment had lower functional outcome measures using the Western Ontario and McMaster Universities Osteoarthritis Index, the University of California Los Angeles Activity Score, and the 12-item Oxford Knee Score, however.
**Question 89**
**A** **40-year-old** **man** **with** **a** **history** **of** **Legg-Calve-Perthes** **disease** **underwent** **a** **right** **hip** **resurfacing** **3** **years**
**ago** **with** **no** **perioperative** **complications.** **Hip** **pain** **has** **developed** **gradually** **during** **the** **last** **4** **months. Radiographs** **show** **no** **evidence** **of** **fixation** **loosening** **or** **any** **adverse** **changes** **at** **the** **femoral** **neck.** **No periarticular** **osteolysis** **is** **evident.** **What** **is** **the** **most** **appropriate** **management** **of** **this** **condition?**
A. **Continue** **to** **observe** **with** **repeat** **radiographs** **in** **6** **months** B. **Fluoroscopic-guided** **iliopsoas** **tendon** **cortisone** **injection** C. **Hip** **aspiration**
D. Serum cobalt and chromium levels and metal-reduction MRI scan
**CORRECT ANSWER: D**
DISCUSSION:
Controversy persists over what exactly is the best approach to managing patients with metal-on-metal (MOM) hip arthroplasties. All patients with painful MOM hip arthroplasties should be examined for fixation loosening, wear/osteolysis, and infection—no differently than patients without MOM hip arthroplasties. It is recommended to obtain serum trace element levels. If the levels are high, cross- sectional imaging should be obtained to determine whether any pseudotumor or tissue necrosis is present around the hip arthroplasty. Hip aspiration should be considered if concern for infection exists. Adverse tissue reaction has been identified to occur around MOM hip arthroplasties. The predominant histologic feature is tissue necrosis with infiltration of lymphocytes and plasma cells.
**Question 90**
In patients undergoing elective hip or knee arthroplasty who are not at elevated risk (beyond the risk associated
with the surgery) for venous thromboembolism or bleeding, using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism was assigned what grade of recommendation by the 2011 AAOS Clinical Practice Guideline, Preventing Venous Thromboembolic Disease in Patients Undergoing Elective Hip and Knee Arthroplasty?
A. Strong
B. Moderate
C. Limited
D. Inconclusive
**CORRECT ANSWER: B**
DISCUSSION:
Using pharmacologic agents and/or mechanical compressive devices for the prevention of venous thromboembolism in patients undergoing elective hip or knee arthroplasty who are not at elevated risk beyond that of the surgery itself for venous thromboembolism or bleeding was given a moderate grade of
recommendation in the 2011 AAOS Clinical Practice Guideline referenced above.
**Question 91**
**A** **40-year-old** **man** **with** **a** **history** **of** **Legg-Calve-Perthes** **disease** **underwent** **a** **right** **hip** **resurfacing** **3** **years**
**ago** **with** **no** **perioperative** **complications.** **Hip** **pain** **has** **developed** **gradually** **during** **the** **last** **4** **months. Radiographs** **show** **no** **evidence** **of** **fixation** **loosening** **or** **any** **adverse** **changes** **at** **the** **femoral** **neck.** **No periarticular** **osteolysis** **is** **evident.** **A** **large** **intra-articular** **and** **intrapelvic** **pseudotumor** **has** **developed. What** **predominant** **histological** **feature(s)** **is/are** **present** **in** **such** **a** **lesion?**
A. **Polymorphonuclear** **leukocytes**
B. **Extracellular** **metal-wear** **debris**
C. **Cement** **particles** **within** **the** **macrophages**
D. Lymphocytes and plasma cells
**CORRECT ANSWER: D**
DISCUSSION:
Controversy persists over what exactly is the best approach to managing patients with metal-on-metal (MOM) hip arthroplasties. All patients with painful MOM hip arthroplasties should be examined for fixation loosening, wear/osteolysis, and infection—no differently than patients without MOM hip arthroplasties. It is recommended to obtain serum trace element levels. If the levels are high, cross- sectional imaging should be obtained to determine whether any pseudotumor or tissue necrosis is present around the hip arthroplasty. Hip aspiration should be considered if concern for infection exists. Adverse tissue reaction has been identified to occur around MOM hip arthroplasties. The predominant histologic
feature is tissue necrosis with infiltration of lymphocytes and plasma cells.
**Question 92**
**A** **57-year-old** **woman** **experiences** **pain** **1** **year** **after** **total** **knee** **arthroplasty** **(TKA).** **She** **reports** **sharp**
**anterior** **pain** **and** **a** **painful** **catching** **sensation** **that** **is** **aggravated** **by** **rising** **from** **a** **chair** **or** **climbing** **stairs. Physical** **examination** **reveals** **a** **mild** **effusion** **and** **a** **range** **of** **motion** **of** **2°** **to** **130°,** **with** **patellar** **crepitus. The** **symptoms** **are** **reproduced** **by** **resisted** **knee** **extension.** **Radiographs** **show** **a** **well-aligned** **posterior- stabilized** **TKA** **without** **evidence** **of** **component** **loosening.** **What** **is** **the** **recommended** **treatment** **for** **this patient?**
A. **Physical** **therapy**
B. **Arthroscopic** **synovectomy**
C. **Tibial** **insert** **revision**
D. Femoral component revision
**CORRECT ANSWER: B**
DISCUSSION:
Patellar clunk syndrome is caused by the development of a fibrous nodule on the posterior aspect of the quadriceps tendon at its insertion into the patella. It causes a painful catching sensation when the extensor
mechanism traverses over the trochlear notch as the knee extends from 45° of flexion to 30° from full extension. It characteristically occurs in posterior stabilized total knee arthroplasties and appears to be related to femoral component design. The syndrome can usually be prevented by excising the residual synovial fold just proximal to the patella. Flexion gap instability can also cause a painful total knee arthroplasty but is less common in posterior stabilized implants. Femoral component malrotation can cause pain attributable to a flexion gap imbalance or patellar tracking problems. Polyethylene wear would be unlikely after just 1 year. Patellar clunk syndrome can usually be addressed successfully with arthroscopic synovectomy. Recurrence is uncommon. Physical therapy may help to strengthen the quadriceps following synovectomy but would not resolve the clunk syndrome symptoms. Femoral or tibial insert revision is not indicated if patellar clunk syndrome is the only problem resulting in a painful
total knee arthroplasty.
**Question 93**
Which modality has the broadest application for the reduction of postsurgical transfusion?
A. Regional anesthesia
B. Tranexamic acid (TXA) administration
C. Reduced transfusion trigger
D. Hypotensive anesthesia
**CORRECT ANSWER: B**
DISCUSSION:
TXA is easy to administer, inexpensive, and safe for virtually all patients. Multiple studies have demonstrated transfusion rates lower than 3% for total knee arthroplasty and lower than 10% for total hip arthroplasty. Regional and hypotensive anesthesia effectively reduce transfusion; however, they cannot be used in as wide a range of patients as can TXA. A reduced transfusion trigger must be considered along
with patient symptoms when determining the need for transfusion.
**Question 94**
**When** **do** **most** **symptomatic** **thromboembolic** **events** **occur** **after** **total** **joint** **arthroplasty?**
A. **On** **the** **day** **of** **surgery**
B. **Within** **the** **first** **week** **after** **surgery**
C. **Between** **1** **week** **and** **6** **weeks** **after** **surgery**
D. More than 3 months after surgery
**CORRECT ANSWER: C**
DISCUSSION:
Most clinical venous thromboembolism events occur between the second and sixth weeks after surgery. It is estimated that 10% of patients are readmitted to the hospital within the first 3 months after total hip or knee arthroplasties. Most pulmonary events on the day of surgery are related to fat embolism or cardiac events.
**Question 95**
**When** **comparing** **arthroscopic** **lavage** **and** **knee** **debridement** **with** **placebo** **in** **patients** **with** **chronic**
**symptomatic** **osteoarthritis,** **what** **outcome** **has** **been** **demonstrated?**
A. **Reliable** **and** **durable** **pain** **relief**
B. **No** **significant** **benefit** **for** **chronic** **osteoarthritis**
C. **Up** **to** **75%** **pain** **relief** **for** **2** **months,** **then** **variable** **response**
D. Three-month measurable pain relief, followed by recurrence
**CORRECT ANSWER: B**
DISCUSSION:
Excluding a diagnosis of meniscal tear, loose body, or mechanical derangement, treating knee osteoarthritis of indeterminate cause with arthroscopic lavage and debridement has been found to provide no discernable benefit to offset the risk of surgery. The effects of arthroscopy have not been clinically significant in the vast majority of patient-oriented outcomes measures for pain and function at multiple
times between 1 week and 2 years after surgery.
**Question 96**
**Figure** **below** **shows** **the** **abdominal** **radiograph** **obtained** **from** **a** **70-year-old** **woman** **who** **experiences**
**nausea** **and** **abdominal** **tightness** **48** **hours** **following** **left** **total** **knee** **arthroplasty** **performed** **under** **general anesthesia.** **She** **received** **24** **hours** **of** **cefazolin** **antibiotic** **prophylaxis** **and** **a** **patient-controlled** **analgesia narcotic** **pump** **for** **pain** **management.** **She** **has** **been** **receiving** **warfarin** **for** **thromboembolic** **prophylaxis. Her** **severe** **abdominal** **distension** **and** **markedly** **decreased** **bowel** **sounds** **are** **most** **likely** **secondary** **to** **the administration** **of**
A. **general** **anesthesia.**
B. **antibiotics.**
C. **warfarin.**
D. narcotics.
**CORRECT ANSWER: D**
DISCUSSION:
The radiograph reveals severe intestinal dilatation, which has occurred as the result of acute colonic pseudo-obstruction and is associated with excessive narcotic administration following total joint arthroplasty. Anesthetic type, antibiotic administration, and warfarin have not been associated with this obstruction. Electrolyte imbalances such as hypokalemia have been associated with postsurgical acute colonic pseudo-obstruction.
**Question 97**
**Venous** **thromboembolism** **may** **occur** **after** **total** **joint** **arthroplasty.** **The** **risk** **of** **this** **complication** **is**
**elevated** **in** **patients** **with**
A. **a** **BMI** **lower** **than** **30.**
B. **diabetes** **mellitus,** **with** **a** **hemoglobin** **A1c** **test** **result** **less** **than** **7.**
C. **tranexamic** **acid** **use.**
D. metabolic syndrome.
**CORRECT ANSWER: D**
DISCUSSION:
Obesity, a prior history of venous thromboembolism, and metabolic syndrome have all been associated with an increased risk of thromboembolism. A recent meta-analysis showed that diabetes had no significant relationship with venous thromboembolism following hip or knee arthroplasty. Tranexamic acid is an antifibrinolytic agent that has been shown to reduce blood loss substantially following hip and knee arthroplasty. It has also been shown to be safe in patients with severe medial comorbidities and a prior history of venous thromboembolism.
**Question 98**
**A** **70-year** **old** **woman** **undergoes** **revision** **total** **knee** **arthroplasty** **for** **tibial** **component** **aseptic** **loosening.**
**She** **is** **concerned** **about** **recurrent** **loosening,** **and** **tibial** **stem** **fixation** **options** **during** **revision** **are** **reviewed. Figure** **below** **displays** **a** **radiograph** **of** **the** **revision** **technique** **used** **for** **this** **patient.** **What** **is** **the** **incidence of** **intraoperative** **tibial** **shaft** **fracture** **that** **is** **associated** **with** **this** **type** **of** **revision** **surgery?**
A. **0%** **to** **1%** **with** **press-fit** **tibial** **stems** B. **3%** **to** **5%** **with** **press-fit** **tibial** **stems** C. **3%** **to** **5%** **with** **cemented** **tibial** **stems**
D. More than 5% with press-fit tibial stems
**CORRECT ANSWER: B**
DISCUSSION:
Using press-fit tibial stems during a hybrid revision total knee arthroplasty is associated with a 3% to 5% incidence of intraoperative tibial shaft fracture. Diaphyseal fixation of press-fit stems has the advantage of setting component alignment, dispersing forces on the proximal tibia, and offers excellent clinical results. The disadvantages include proximal and distal tibia anatomic mismatch and tibial shaft fracture. Cipriano and associates reported a tibial shaft fracture incidence of 4.9% in a series of 420 consecutive
knee revisions. All fractures healed with nonsurgical management, and none led to implant loosening. In this patient, it is important to recognize on the radiograph that this technique is a hybrid method of revision total knee arthroplasty, with cementation along the tibial tray and metaphysis and with press-fit fixation of the diaphyseal engaging stem. Then, it is important to know the risk and management of intraoperative diaphyseal tibial fractures. Cemented tibial stems are associated with a low rate of intraoperative fracture, because the implant is typically undersized to allow for an appropriate cement mantle. Option C is incorrect, because this revision is not cemented. Option A underestimates the incidence of fracture,
whereas D overestimates the rate of fracture.
**Question 99**
Figures below depict the radiographs obtained from a 60-year-old man with instability and pain 1 year after
primary right total knee arthroplasty. He states that he had surgery on two occasions for a tendon rupture that was repaired with sutures but that his knee popped again, and now the leg is unable to hold his weight. On examination, he is in no acute distress. His height is 6'3", and he weighs 240 pounds. He is ambulatory with crutches. Range of motion of the right knee is 50° to 120° actively and 0° to 120° passively. More than 10° of varus/valgus laxity and more than 5 mm of anteroposterior drawer are present. A palpable defect is observed in the tissue just proximal to the patella. The incision is well healed. The erythrocyte sedimentation rate is 46 mm/h (reference range 0 to 20 mm/h) and the C-reactive protein level is 2.04 mg/L (reference range 0.08 to
3.1 mg/L). Aspiration of the right knee reveals hazy yellow fluid with a white blood cell count of 120 and 1%
neutrophils. No growth of organisms is seen on routine culture. What is the best next step?
A. Revision total knee arthroplasty with extensor mechanism allograft
B. Revision total knee arthroplasty with liner change and primary quadriceps repair
C. Resection knee arthroplasty and arthrodesis with antegrade nail
D. Two-stage revision total knee arthroplasty with extensor mechanism allograft
**CORRECT ANSWER: A**
DISCUSSION:
This patient has a chronic quadriceps tendon rupture after total knee arthroplasty. Two previous primary repair attempts have failed, which is not surprising based on the poor results of primary repair reported in the literature. The patient also has an unstable knee and will require revision of some or all of the prosthesis to achieve a stable knee. Revision total knee arthroplasty with extensor mechanism allograft allows an allograft reconstruction of the ruptured quadriceps tendon. The other option is to utilize a synthetic mesh extensor mechanism reconstruction. These are likely to have the best result in this situation. Revision total knee arthroplasty with liner change and primary quadriceps repair is not the best form of management, because it involves a third attempt at primary tendon repair, which will likely fail again. Resection knee arthroplasty and arthrodesis with antegrade nail is a possible option but is not the best, because it would likely make driving and other daily activities difficult. Two-stage revision total
knee arthroplasty with extensor mechanism allograft is not the best option because the laboratory results
show no signs of infection, so a single-stage procedure is preferred.
**Question 100**
**A** **60-year-old** **man** **who** **underwent** **left** **partial** **knee** **arthroplasty** **6** **months** **earlier** **was** **doing** **well** **until** **he**
**experienced** **left** **knee** **pain** **and** **swelling** **for** **4** **weeks** **following** **a** **dental** **procedure.** **The** **left** **knee** **aspirate was** **bloody,** **with** **a** **white** **blood** **cell** **count** **of** **8,000** **and** **70%** **neutrophils.** **Culture** **grew** **group** **B Streptococcus** **(**_Granulicatella adiacens_**),** **and** **serologies** **were** **elevated,** **with** **an** **erythrocyte** **sedimentation rate** **of** **55** **mm/h** **(reference** **range:** **0** **to** **20** **mm/h)** **and** **a** **C-reactive** **protein** **level** **of** **24** **mg/L** **(reference range:** **0.08** **to** **3.1** **mg/L).** **What** **is** **the** **best** **next** **step?**
A. **Arthroscopic** **debridement**
B. **Two-stage** **total** **knee** **revision** **arthroplasty**
C. **Resection** **arthroplasty** **without** **an** **antibiotic** **impregnated** **cement** **spacer**
D. Knee fusion
**CORRECT ANSWER: B**
DISCUSSION:
This complication is best addressed with either a single-stage or two-stage total knee arthroplasty. A recent report suggests that a single-stage arthroplasty can be effective, although many surgeons would perform a two-stage procedure with an articulating or static spacer. Arthroscopic would be non-effective, especially given 4 weeks of symptoms. Resection arthroplasty without a spacer would leave an unstable _and poorly functioning extremity. Knee fusion should be used as a salvage procedure._
**_[**ERGUIDE MCQ 401-450**](http://hutaifortho.com/640)_**
---
**_[**ORTHOPEDICS HYPERGUIDE MCQ 351-400**](http://hutaifortho.com/639)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 301-350**](http://hutaifortho.com/638)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 251-300**](http://hutaifortho.com/637)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 201-250**](http://hutaifortho.com/636)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 151-200**](http://hutaifortho.com/635)_**
**_[**ORTHOPEDICS HYPERGUIDE MCQ 101-150**](http://hutaifortho.com/634)_**
**_[**FREE Orthopedics MCQS 2022 51-100**](http://hutaifortho.com/633)_**
**_[**Orthopedics Hyperguide MCQ 1-50**](http://hutaifortho.com/631)_**
Question 38High Yield
During the loading response of the foot through a gait cycle, what muscle activity restrains the rapid plantar flexion of the foot?
Explanation
■
The loading response of the foot and ankle during the gait cycle is the time segment that spans from the initial floor contact with the heel to the forefoot contact on the floor. During the loading response of the ankle and foot, in response to the rapid loading of the body weight on the heel lever, the foot is promptly driven to the floor. Intense, eccentric activity of the pretibial muscles (tibialis anterior and long toe extensors) generates an opposing dorsiflexor moment to decelerate this event, making forefoot contact a quiet event. Concentric activity of the pretibial muscles happens during the swing phase of the foot where ankle and foot is dorsiflexed to facilitate floor clearance and limb progression.
Eccentric contracture of the gastrocnemius-soleus muscle provides control of the ankle`s simultaneous progression and stability during the mid stance into the first half of terminal stance phase of the gait cycle. During this phase, soleus activity is the dominant decelerating force compared with gastrocnemius muscle, and their combined activity helps to control the forward progression of the limb by increasing dorsiflexion of the tibia over the articular surface of the talus. During the early pre-swing phase of the gait, activity of gastrocnemius-soleus muscle diminishes, but the ankle continues to plantar flex. Ultrasonography studies suggest that the abrupt burst of plantar flexor power during this period is elastic recoil of the Achilles tendon following quick release of the previously tense soleus and gastrocnemius. This allows the forces of the plantar flexor muscles to prepare the trailing limb for swing.
The loading response of the foot and ankle during the gait cycle is the time segment that spans from the initial floor contact with the heel to the forefoot contact on the floor. During the loading response of the ankle and foot, in response to the rapid loading of the body weight on the heel lever, the foot is promptly driven to the floor. Intense, eccentric activity of the pretibial muscles (tibialis anterior and long toe extensors) generates an opposing dorsiflexor moment to decelerate this event, making forefoot contact a quiet event. Concentric activity of the pretibial muscles happens during the swing phase of the foot where ankle and foot is dorsiflexed to facilitate floor clearance and limb progression.
Eccentric contracture of the gastrocnemius-soleus muscle provides control of the ankle`s simultaneous progression and stability during the mid stance into the first half of terminal stance phase of the gait cycle. During this phase, soleus activity is the dominant decelerating force compared with gastrocnemius muscle, and their combined activity helps to control the forward progression of the limb by increasing dorsiflexion of the tibia over the articular surface of the talus. During the early pre-swing phase of the gait, activity of gastrocnemius-soleus muscle diminishes, but the ankle continues to plantar flex. Ultrasonography studies suggest that the abrupt burst of plantar flexor power during this period is elastic recoil of the Achilles tendon following quick release of the previously tense soleus and gastrocnemius. This allows the forces of the plantar flexor muscles to prepare the trailing limb for swing.
Question 39High Yield
A 25-year-old man sustains a left brachial plexus injury from a fall while rock climbing. Examination reveals poor intrinsic function of the hand, ptosis, and miosis. He is able to abduct and forward flex his shoulder with full strength. This combination of physical findings is most suggestive of what pattern of nerve injury?
Explanation
A preganglionic lesion occurs proximal to the spinal foramen, whereas a postganglionic lesion occurs distal to the spinal foramen in the root, trunk, division, cord, or branches of the brachial plexus. The Horner sign, which is characterized by miosis, ptosis, anhydrosis, and enophthalmos, results from an injury to the sympathetic ganglion, which lies in close proximity to the T1 root level. The presence of a Horner sign is highly suggestive of a T1 preganglionic injury. Other physical examination indicators of a preganglionic injury include atrophy of the parascapular muscles (injury to the dorsal rami of the cervical spinal nerve roots), winged scapula (injury to the long thoracic nerve) and hemidiaphragmatic paralysis (phrenic nerve injury). The lack of intrinsic hand function in this patient is also suggestive of an injury at the level of C8-T1. Preservation of shoulder abduction and forward flexion would not typically be seen with an injury to the C5-C6 roots or the upper trunk.
Question 40High Yield
Figures 58a through 58c are the radiograph, MR image, and sagittal CT scan of a 13-year-old boy with a 5-month history of a left hip injury. He has no current pain, but substantial, progressive limitations in hip flexion are present. What is the most likely diagnosis?
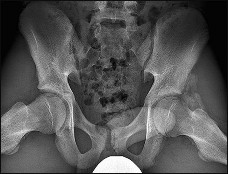
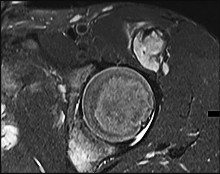
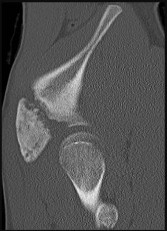
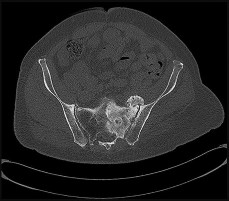
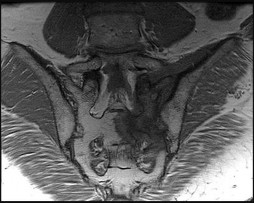
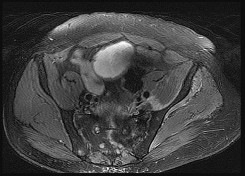
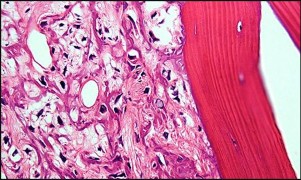
Explanation
This patient has a mineralized mass in the soft tissues in the rectus femoris origin. The clinical history favors an avulsion injury with subsequent myositis ossificans, and the imaging is consistent with an ossified soft-tissue mass. Extraskeletal osteosarcoma is a rare soft-tissue sarcoma and is generally seen in adults. Chondrosarcoma is also generally seen in adults and would have a more chondroid matrix as opposed to mature-looking bone on a CT scan. Pelvic osteosarcoma could have this appearance on radiograph, but the CT scan and MR image confirm this is a soft-tissue process with mature mineralization.
RECOMMENDED READINGS
13. Tyler P, Saifuddin A. The imaging of myositis ossificans. Semin Musculoskelet Radiol. 2010 Jun;14(2):201-16. doi: 10.1055/s-0030-1253161. Epub 2010 May 18. Review. PubMed PMID:
[20486028/. ](http://www.ncbi.nlm.nih.gov/pubmed/20486028)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20486028)
14. [Colman MW, Lozano-Calderon S, Raskin KA, Hornicek FJ, Gebhardt M. Non-neoplastic soft tissue masses that mimic sarcoma. Orthop Clin North Am. 2014 Apr;45(2):245-55. doi: 10.1016/j.ocl.2013.12.006. Epub 2014 Feb 1. Review. ](http://www.ncbi.nlm.nih.gov/pubmed/24684918)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24684918)
CLINICAL SITUATION FOR QUESTIONS 59 THROUGH 61
Figures 59a through 59d are the CT scans and biopsy specimen of a 68-year-old man with progressive radicular symptoms in his left lower extremity. Four years previously he underwent treatment of colorectal cancer with surgery, chemotherapy, and radiotherapy.
RECOMMENDED READINGS
13. Tyler P, Saifuddin A. The imaging of myositis ossificans. Semin Musculoskelet Radiol. 2010 Jun;14(2):201-16. doi: 10.1055/s-0030-1253161. Epub 2010 May 18. Review. PubMed PMID:
[20486028/. ](http://www.ncbi.nlm.nih.gov/pubmed/20486028)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20486028)
14. [Colman MW, Lozano-Calderon S, Raskin KA, Hornicek FJ, Gebhardt M. Non-neoplastic soft tissue masses that mimic sarcoma. Orthop Clin North Am. 2014 Apr;45(2):245-55. doi: 10.1016/j.ocl.2013.12.006. Epub 2014 Feb 1. Review. ](http://www.ncbi.nlm.nih.gov/pubmed/24684918)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/24684918)
CLINICAL SITUATION FOR QUESTIONS 59 THROUGH 61
Figures 59a through 59d are the CT scans and biopsy specimen of a 68-year-old man with progressive radicular symptoms in his left lower extremity. Four years previously he underwent treatment of colorectal cancer with surgery, chemotherapy, and radiotherapy.
Question 41High Yield
What are the five major compartments of the foot?
Explanation
The five major compartments of the foot are medial, lateral, central, interosseous, and calcaneal. There is no dorsal compartment in the foot.
REFERENCES: Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 262-264.
Shereff MJ: Compartment syndromes of the foot. Instr Course Lect 1990;39:127-132.
REFERENCES: Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 262-264.
Shereff MJ: Compartment syndromes of the foot. Instr Course Lect 1990;39:127-132.
Question 42High Yield
An obese 62-year-old man (BMI 38) who underwent a cementless total hip arthroplasty 14 months ago fell from a ladder and is now unable to bear weight on the extremity. A radiograph from his 3-month visit is shown in Figure 77a and a radiograph from the time of the injury is shown in Figure 77b. Appropriate management includes which
of the following?
of the following?
Explanation
The patient has a Vancouver type B1 fracture of the femur with a well-fixed femoral component. When comparing the two radiographs, the proximal femoral component position has not changed and remodeling is seen around the component. Nonsurgical management is associated with the complications of extended recumbency. As the femoral component is well-fixed, revision of the femoral component is not necessary.
REFERENCES: Masri BA, Meek RM, Duncan CP: Periprosthetic fractures evaluation and treatment. Clin Orthop Relat Res 2004;420:80-95.
Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 475-503.
Ricci WM, Bolhofner BR, Lofitus T, et al: Indirect reduction and plate fixation, without grafting, for
periprosthetic femoral shaft fractures about a stable intramedullary implant. J Bone Joint Surg Am 2005;87:2240-2245.
REFERENCES: Masri BA, Meek RM, Duncan CP: Periprosthetic fractures evaluation and treatment. Clin Orthop Relat Res 2004;420:80-95.
Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 475-503.
Ricci WM, Bolhofner BR, Lofitus T, et al: Indirect reduction and plate fixation, without grafting, for
periprosthetic femoral shaft fractures about a stable intramedullary implant. J Bone Joint Surg Am 2005;87:2240-2245.
Question 43High Yield
A complication associated with using the Morrey approach (triceps reflecting) to implant a semiconstrained total elbow arthroplasty is
Explanation
DISCUSSION:
Numerous approaches can be used to implant a total elbow arthroplasty. The Morrey approach identifies, transposes, and protects the ulnar nerve, and then subperiosteally reflects the triceps off the ulna. The sleeve of tissue is very thin distally, and the triceps need to be meticulously repaired at the time of closure. Implant dislocation and malposition are less likely with an extensile approach, and dislocation is unlikely with a semiconstrained implant. The development of heterotopic ossification is unrelated to the surgical approach
used for elbow arthroplasty.
DISCUSSION:
Numerous approaches can be used to implant a total elbow arthroplasty. The Morrey approach identifies, transposes, and protects the ulnar nerve, and then subperiosteally reflects the triceps off the ulna. The sleeve of tissue is very thin distally, and the triceps need to be meticulously repaired at the time of closure. Implant dislocation and malposition are less likely with an extensile approach, and dislocation is unlikely with a semiconstrained implant. The development of heterotopic ossification is unrelated to the surgical approach
used for elbow arthroplasty.
Question 44High Yield
When comparing the direct anterior approach with the posterolateral surgical approach, the direct anterior approach is associated with
Explanation
The direct anterior approach in primary total hip arthroplasty (THA) has continued to gain in popularity. Prior investigations have shown patients do very well following a direct anterior THA with excellent rates of recovery and clinical outcomes. However, the potential for femoral-sided complications, including femoral component subsidence and fracture, may be increased via the direct anterior approach versus a posterolateral surgical approach.
Question 45High Yield
A 45-year-old man has a grade 4 hallux rigidus secondary to a turf toe sustained as a football player in high school. He is an avid golfer and plays tennis on occasion. His activities are severely limited because of pain in his great toe and nonsurgical management has failed to provide relief. His goal is to be pain free, continue with his activities, and require no further orthopaedic care in the future. What is the best
treatment option for this patient?
treatment option for this patient?
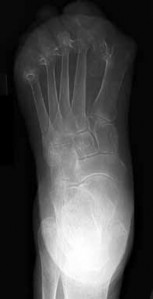
Explanation
There has been some research about interpositional grafting, whether autologous or allograft, but there is no convincing evidence at this point that there is a better functional outcome than with a great toe MTP fusion. A Keller procedure is not indicated for a young, active person. A joint replacement of the great toe similarly has not proven to be a reliable option for younger, active people.Cheilectomy will not provide reliable pain relief in grade 4 arthrosis of the first MTP joint.
---
---
Question 46High Yield
Which of the following categories of slipped capital femoral epiphysis (SC FE) is associated with the highest risk of a grade III
slip:
slip:
Explanation
A grade III slip refers to more than 50% displacement of the epiphysis. Renal failure is associated with the highest risk (43%) of progressing to a grade III slip. Fortunately, these slips are usually stable.
Question 47High Yield
A disadvantage associated with presurgical (vs postsurgical) radiation therapy for soft-tissue sarcoma is a
Explanation
Radiation therapy is used for soft-tissue sarcoma treatment to facilitate resection of tumors that are close to adjacent structures and to diminish risk for local recurrence. The disadvantages of radiation therapy for soft-tissue sarcoma include patient inconvenience, risk for secondary malignancy, and higher wound complication rates. The advantages of presurgical (neoadjuvant) radiation therapy include a smaller radiation field, formation of a “pseudocapsule” to facilitate a planned close-margin resection, tumor shrinkage, and lower local recurrence rates. The main disadvantage of presurgical radiation therapy is the much higher risk for wound healing complications (as demonstrated in numerous studies).
RECOMMENDED READINGS
7. [O'Sullivan B, Davis AM, Turcotte R, Bell R, Catton C, Chabot P, Wunder J, Kandel R, Goddard K, Sadura A, Pater J, Zee B. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: a randomised trial. Lancet. 2002 Jun 29;359(9325):2235-41. ](http://www.ncbi.nlm.nih.gov/pubmed/12103287)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/12103287)
8. [Zagars GK, Ballo MT, Pisters PW, Pollock RE, Patel SR, Benjamin RS. Preoperative vs. postoperative radiation therapy for soft tissue sarcoma: a retrospective comparative evaluation of disease outcome. Int J Radiat Oncol Biol Phys. 2003 Jun 1;56(2):482-8. ](http://www.ncbi.nlm.nih.gov/pubmed/12738324)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/12738324)
9. [Peat BG, Bell RS, Davis A, O'Sullivan B, Mahoney J, Manktelow RT, Bowen V, Catton C, Fornasier VL, Langer F. Wound-healing complications after soft-tissue sarcoma surgery. Plast Reconstr Surg. 1994 Apr;93(5):980-7. PubMed PMID: 8134491. ](http://www.ncbi.nlm.nih.gov/pubmed/8134491)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8134491)
RECOMMENDED READINGS
7. [O'Sullivan B, Davis AM, Turcotte R, Bell R, Catton C, Chabot P, Wunder J, Kandel R, Goddard K, Sadura A, Pater J, Zee B. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: a randomised trial. Lancet. 2002 Jun 29;359(9325):2235-41. ](http://www.ncbi.nlm.nih.gov/pubmed/12103287)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/12103287)
8. [Zagars GK, Ballo MT, Pisters PW, Pollock RE, Patel SR, Benjamin RS. Preoperative vs. postoperative radiation therapy for soft tissue sarcoma: a retrospective comparative evaluation of disease outcome. Int J Radiat Oncol Biol Phys. 2003 Jun 1;56(2):482-8. ](http://www.ncbi.nlm.nih.gov/pubmed/12738324)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/12738324)
9. [Peat BG, Bell RS, Davis A, O'Sullivan B, Mahoney J, Manktelow RT, Bowen V, Catton C, Fornasier VL, Langer F. Wound-healing complications after soft-tissue sarcoma surgery. Plast Reconstr Surg. 1994 Apr;93(5):980-7. PubMed PMID: 8134491. ](http://www.ncbi.nlm.nih.gov/pubmed/8134491)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8134491)
Question 48High Yield
A 77-year-old man with diabetes mellitus has had a nonhealing Wagner grade I ulcer under the medial sesamoid for the past 3 months. He smokes tobacco regularly. He has undergone several debridements and total contact casting. Examination reveals no palpable pulses. He has no erythema or purulence, and he is afebrile. Radiographs reveal no abnormalities. What is the best initial diagnostic test to help determine why the ulcer has failed to heal?**
Explanation
The best initial test for this patient is to assess the vascular supply to the foot. An elderly smoker with diabetes mellitus has a high risk of peripheral vascular disease. Decreased weight bearing has not been successful. Although a bone scan might be helpful, it would take secondary consideration to the patient’s vascular supply, especially in the absence of any acute infection. Monofilament testing would help diagnosis neuropathy, which is a root cause behind the ulcer forming, but does not prevent it from healing. The Thompson’s test is used to diagnosis an Achilles tendon rupture.
REFERENCE: Brodsky JW: Evaluation of the diabetic foot. Instr Course Lect 1999;48:289-303.
REFERENCE: Brodsky JW: Evaluation of the diabetic foot. Instr Course Lect 1999;48:289-303.
Question 49High Yield
What is the most common complication associated with scalene regional anesthesia for shoulder procedures?
Explanation
Failure of the scalene block, necessitating general anesthesia or the immediate administration of narcotic medications, is the most common complication, occurring in 3% to 18% of patients. Cardiac arrest or cardiovascular collapse has been reported in anecdotal occurrences. Seizure that is the result of intravascular injection of local anesthetic is a rare complication, with an incidence reported of 0% to 6%. Neurologic complications, including laryngeal and phrenic nerve injuries, are rare although parathesias lasting up to 2 weeks have been reported in up to 3% of patients.
REFERENCES: Weber SC, Jain R: Scalene regional anesthesia for shoulder surgery in a community setting: An assessment of risk. J Bone Joint Surg Am 2002;84:775-779.
Conn RA, Colfield RH, Byer DE, Lindstromberg JW: Interscalene block anesthesia for shoulder surgery. Clin Orthop 1987;216:94-98.
REFERENCES: Weber SC, Jain R: Scalene regional anesthesia for shoulder surgery in a community setting: An assessment of risk. J Bone Joint Surg Am 2002;84:775-779.
Conn RA, Colfield RH, Byer DE, Lindstromberg JW: Interscalene block anesthesia for shoulder surgery. Clin Orthop 1987;216:94-98.
Question 50High Yield
Injuries to what two structures would result in a “floating shoulder"?
Explanation
The superior shoulder suspensory complex (SSSC) is a bone and soft-tissue ring secured to the trunk by superior and inferior bony struts, from which the upper extremity is suspended. The ring is composed of the glenoid process, coracoid process, coracoclavicular ligaments, distal clavicle, acromioclavicular joint, and acromial process. Double lesions of the SSSC are referred to as “floating shoulder” injuries, as in this case in which the injury involves a fractured scapular neck and ipsilateral clavicle fracture. Ipsilateral acromioclavicular dislocation and coracoid fracture is a less common double disruption of the SSSC. Although several case studies have been published on surgical and nonsurgical management of these injuries, no study provides measurable surgical indications beyond the simple presence of the double lesion. This is often referred to as an unstable shoulder girdle.
47
47
You Might Also Like

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon