Subungual Melanoma and Nail Bed Lesions: Comprehensive Surgical Management
Key Takeaway
Subungual melanoma is a rare but aggressive malignancy of the nail apparatus, often misdiagnosed as a subungual hematoma or onychomycosis. Early recognition of clinical markers, such as Hutchinson’s sign, is critical. Definitive orthopedic management typically requires proximal amputation at the metatarsophalangeal joint. This guide details the diagnostic workup, surgical anatomy, amputation techniques, and the excision of differential lesions like glomus tumors using an L-shaped full-thickness flap.
Introduction to Subungual Melanoma
The orthopaedic surgeon is seldom the first clinician to evaluate a patient with a subungual melanoma; however, the responsibility of definitive surgical management and oncologic staging often falls within their purview. To overlook this diagnosis—or to omit it from the differential of a chronic, atypical nail bed lesion—can lead to catastrophic prognostic consequences. A delay in the treatment of acral lentiginous melanoma directly correlates with increased Breslow depth, higher rates of lymphatic metastasis, and significantly worse overall survival outcomes.
Subungual melanomas account for only 2% to 3% of all cutaneous melanomas. However, their demographic distribution is highly specific: they are disproportionately more common in individuals of Asian or African descent. In these populations, the overall incidence of melanoma at other anatomical sites is markedly lower, making acral and subungual presentations the predominant phenotype.
Clinical Pearl: Any new, unexplained pigmented lesion in the nail apparatus of a patient of Asian or African descent must be considered subungual melanoma until proven otherwise via histopathologic examination.
Clinical Presentation and Diagnostic Evaluation
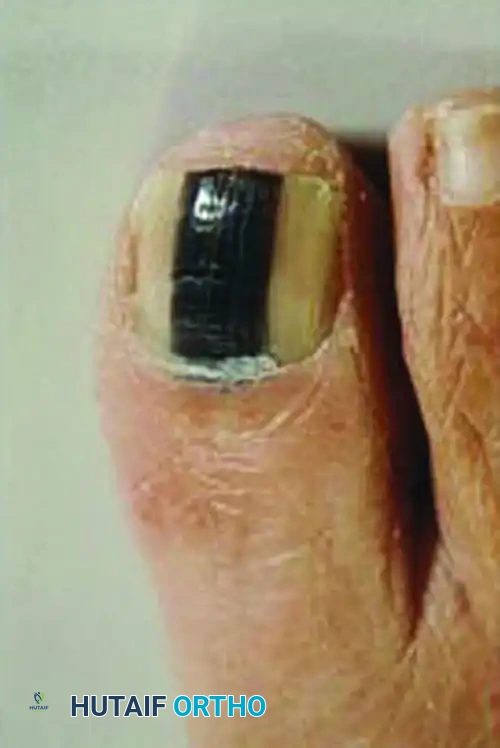
Subungual melanomas typically present as painless, longitudinal black or brown discolorations under the nail plate, a condition known as melanonychia striata. However, the clinical presentation can be highly variable. A significant subset of these tumors is amelanotic (lacking pigment), presenting as chronic paronychia, pyogenic granuloma-like masses, or non-healing nail bed ulcerations. Furthermore, the lesion may or may not involve structural changes to the nail plate itself, such as splitting, dystrophy, or complete avulsion.
Differentiating Melanoma from Benign Pathology
The primary differential diagnoses for a pigmented subungual lesion include subungual hematoma, onychomycosis, melanocytic nevi, and glomus tumors. Distinguishing a malignancy from these benign entities requires meticulous clinical observation.
Warning Signs of Subungual Melanoma:
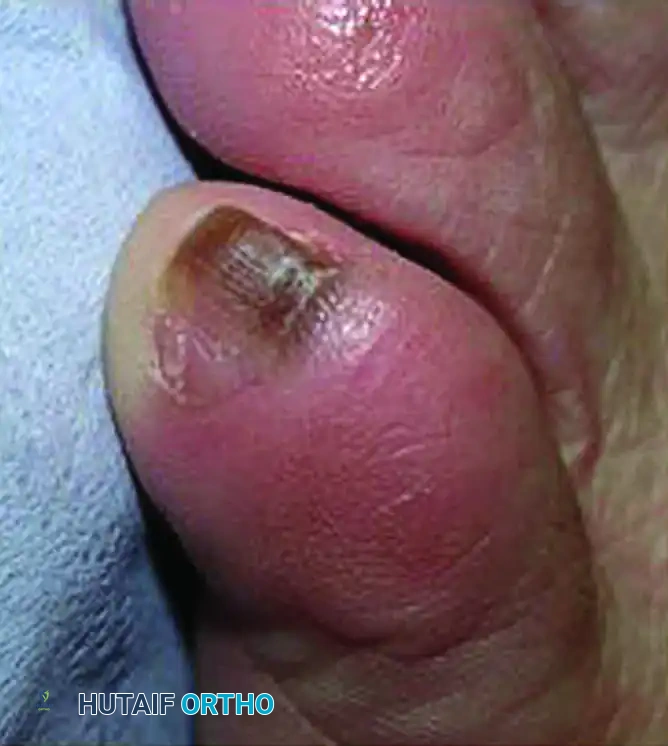
* Hutchinson’s Sign: This is the pathognomonic periungual extension of brown or black pigment from the nail bed and matrix onto the proximal or lateral nail folds. Its presence is highly indicative of advanced subungual melanoma.
* Lack of Distal Migration: Unlike a subungual hematoma, which will migrate distally as the nail plate grows (approximately 1 mm per month in toes), the pigmentation of a melanoma originates in the matrix and remains fixed or expands proximally.
* Band Width and Variation: A pigmented band wider than 3 mm, or one that exhibits variegated shades of brown and black with blurred borders, is highly suspicious.
Clinical presentation of a subungual melanoma demonstrating Hutchinson’s sign, characterized by the extension of dark pigmentation into the proximal nail fold and surrounding eponychium.
Biopsy Principles
When clinical suspicion is raised, a definitive tissue diagnosis is mandatory before proceeding with radical surgical resection.
* Matrix Biopsy: Because the melanocytes responsible for the lesion reside in the germinal matrix, a full-thickness longitudinal incisional biopsy or a punch biopsy of the matrix is required.
* Avoid Shave Biopsies: Superficial shave biopsies of the nail bed are frequently non-diagnostic and may fail to capture the true Breslow depth of the lesion, which is the most critical factor in determining the level of surgical amputation.
Surgical Anatomy and Biomechanics of the Nail Apparatus
A profound understanding of the perionychial anatomy is essential for both diagnostic biopsies and the surgical management of differential lesions.
- The Germinal Matrix: Located proximally beneath the eponychium, this highly cellular layer is responsible for 90% of nail plate generation. Melanomas typically originate here.
- The Sterile Matrix: Extending from the lunula to the hyponychium, this layer provides adherence for the nail plate.
- Vascular Supply: The nail apparatus is supplied by the terminal branches of the proper plantar digital arteries, which form a rich anastomotic arcade within the distal phalanx.
- Biomechanics of the Hallux: The great toe plays a critical role in the terminal stance phase of the gait cycle, bearing approximately 50% of body weight during toe-off. Amputations proximal to the interphalangeal (IP) joint significantly alter foot biomechanics, reducing push-off power and increasing load transfer to the lesser metatarsal heads.
Surgical Management: Subungual Melanoma
Once the diagnosis and staging (including Sentinel Lymph Node Biopsy for lesions >0.8mm thick or with ulceration) are finalized, the definitive surgical treatment is amputation. Historically, radical amputations were favored, but contemporary oncologic principles advocate for joint-sparing or functional amputations when negative margins can be assured.
For invasive subungual melanoma of the hallux, the standard of care remains a proximal amputation at the metatarsophalangeal (MTP) joint or the proximal metatarsal, depending on the proximal extent of the disease.
Step-by-Step Technique: First Metatarsophalangeal Joint Disarticulation
1. Positioning and Anesthesia:
The patient is placed supine on a radiolucent operating table. General or regional anesthesia (popliteal block) is administered. A pneumatic thigh or calf tourniquet is applied to ensure a bloodless surgical field.
2. Incision Design:
A racquet-shaped incision is utilized. The handle of the racquet begins dorsally over the distal third of the first metatarsal. The incision diverges to encircle the base of the proximal phalanx, preserving a slightly longer plantar flap to ensure robust soft-tissue coverage over the metatarsal head.
3. Dissection and Neurovascular Management:
* The incision is deepened through the dermis and subcutaneous tissue.
* The dorsal digital veins are identified, ligated, and transected.
* The medial and lateral plantar proper digital nerves are identified. They must be drawn distally, transected sharply under tension, and allowed to retract deep into the intrinsic musculature to prevent painful stump neuromas.
* The digital arteries are clamped, ligated with 3-0 absorbable suture, and divided.
4. Tendon Management:
* The Extensor Hallucis Longus (EHL) and Extensor Hallucis Brevis (EHB) tendons are identified dorsally, transected, and allowed to retract.
* The Flexor Hallucis Longus (FHL) is identified plantarly, transected, and allowed to retract.
Surgical Warning: Do not suture the EHL to the FHL over the metatarsal head. This historical practice restricts the excursion of the FHL, potentially causing a flexion contracture of the lesser toes (due to the Master Knot of Henry interconnections).
5. Joint Disarticulation:
* A dorsal capsulotomy of the first MTP joint is performed.
* The collateral ligaments are released from the base of the proximal phalanx.
* The plantar plate and sesamoid complex are evaluated. In oncologic resections for melanoma, if the deep margins are clear, the sesamoids may be left in situ within the plantar plate to preserve the weight-bearing mechanics of the first metatarsal head. If margins are narrow, the sesamoids are excised en bloc with the digit.
6. Closure:
* The articular cartilage of the metatarsal head is typically left intact, as it provides a smooth, avascular barrier that resists infection and limits bony overgrowth.
* The robust plantar flap is rotated dorsally.
* The deep subcutaneous layers are closed with 3-0 absorbable sutures, and the skin is approximated with 4-0 non-absorbable nylon using interrupted horizontal mattress sutures to minimize tension on the wound edges.
Differential Diagnosis Surgical Excision: The Glomus Tumor
While subungual melanoma is painless and pigmented, the orthopaedic surgeon will frequently encounter patients presenting with exquisitely painful, sometimes bluish, subungual masses. These are often glomus tumors—benign hamartomas of the neuromyoarterial glomus body.
Because glomus tumors reside deep within the epithelial bed or matrix, their removal requires a specialized, tissue-sparing approach to prevent postoperative nail dystrophy. The L-shaped full-thickness flap is the preferred technique for complete excision while preserving the germinal matrix.
Step-by-Step Technique: L-Shaped Full-Thickness Flap for Glomus Tumor
1. Preparation:
A digital block is performed using 1% plain lidocaine. A sterile digital tourniquet (Penrose drain) is applied to the base of the toe to provide a bloodless field, which is critical for identifying these small (often 2-5 mm) vascular tumors.
2. Flap Design and Incision:
An L-shaped incision is designed over the proximal nail fold. The transverse limb runs parallel to the eponychium, and the longitudinal limb extends proximally along the lateral or medial border of the nail fold, depending on the tumor's location.
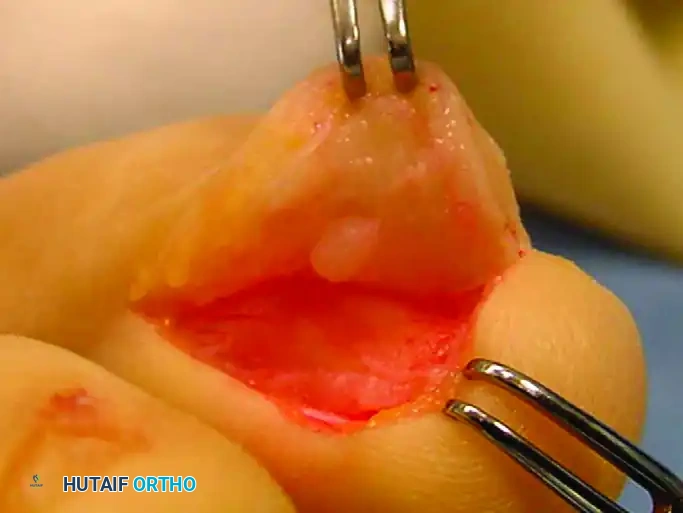
Elevation of the L-shaped full-thickness flap, exposing the underlying proximal nail matrix and the pathology residing within the epithelial bed.
3. Elevation of the Nail Matrix:
The full-thickness flap, consisting of skin and subcutaneous tissue, is carefully elevated off the underlying extensor tendon expansion and the proximal germinal matrix. The proximal portion of the nail plate may be partially avulsed or elevated in continuity with the matrix to expose the tumor bed.
Direct visualization of the glomus tumor embedded within the epithelial bed underneath the elevated flap. Meticulous hemostasis is required to identify the encapsulated lesion.
4. Tumor Excision:
The glomus tumor typically appears as a well-encapsulated, bluish-red nodule. Using microsurgical instruments or tenotomy scissors, the tumor is marginally excised. It is imperative to remove the entire capsule to prevent recurrence, which is a common complication of incomplete excision.
5. Matrix Repair and Closure:
* If the germinal matrix was incised to access the tumor, it must be meticulously repaired using 6-0 or 7-0 absorbable sutures (e.g., polyglactin or chromic gut) on a spatulated needle. Perfect approximation prevents postoperative nail splitting or pterygium formation.
* The L-shaped flap is then repositioned.
* The skin is closed using 4-0 or 5-0 non-absorbable sutures.
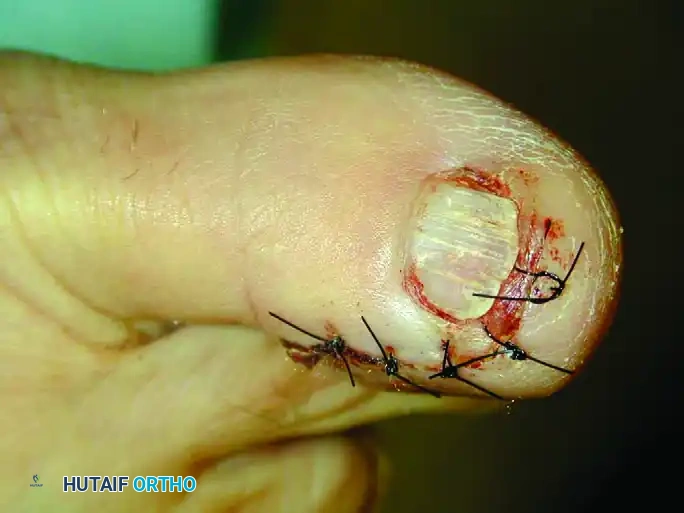
Postoperative photograph demonstrating the anatomical closure of the L-shaped flap. The nail plate is preserved where possible to act as a biologic splint for the healing matrix.
Postoperative Protocols and Rehabilitation
Following MTP Disarticulation (Melanoma)
- Wound Care: The surgical site is dressed with non-adherent gauze and a bulky, compressive dressing. Sutures are typically removed at 3 weeks, as acral skin heals slower than other regions.
- Weight-Bearing: The patient is placed in a rigid postoperative shoe and restricted to heel-touch weight-bearing for the first 2 to 3 weeks to prevent dehiscence of the plantar flap.
- Prosthetics and Orthotics: Once the stump is fully healed, a custom orthosis with a Morton’s extension or a toe filler is prescribed to prevent the migration of adjacent toes and to assist with push-off during the terminal stance phase of gait.
- Oncologic Surveillance: The patient must be followed closely by a multidisciplinary oncology team. Routine surveillance includes clinical lymph node examinations, dermatologic skin checks, and serial imaging (PET-CT or MRI) based on the initial staging.
Following Glomus Tumor Excision
- Wound Care: A non-adherent dressing is applied. The digital tourniquet must be removed prior to dressing application to ensure vascular perfusion returns.
- Weight-Bearing: Weight-bearing as tolerated in a stiff-soled surgical shoe is permitted immediately.
- Suture Removal: Skin sutures are removed at 10 to 14 days.
- Nail Regrowth: Patients must be counseled that the nail may shed postoperatively and that a new, fully formed nail plate will take 9 to 12 months to grow completely from the matrix to the hyponychium.
Complications and Surgical Pitfalls
- Misdiagnosis of Melanoma: The most devastating pitfall is treating a subungual melanoma as a benign hematoma or fungal infection. Any subungual pigmentation that does not migrate distally, involves the periungual skin (Hutchinson's sign), or occurs in a high-risk demographic must be biopsied.
- Inadequate Oncologic Margins: Attempting a distal interphalangeal (DIP) joint amputation for a melanoma that extends proximally into the matrix often results in positive margins. Proximal MTP disarticulation is the safest oncologic choice for invasive lesions.
- Stump Neuroma: Failure to place the digital nerves under tension before transection during amputation will result in a superficial neuroma, rendering the patient unable to bear weight on the forefoot.
- Nail Dystrophy: During glomus tumor excision, rough handling or failure to precisely repair the germinal matrix will result in permanent, cosmetically displeasing nail dystrophy, splitting, or complete loss of adherence.
📚 Medical References
Fig. 84-31 Hutchinson sign. Band of pigmented tissue associated with subungual melanoma. (From Tomczak RL: Embryology of the nail unit. In Myerson MS, ed: Foot and ankle disorders, Philadelphia, 2000, Saunders; courtesy of Elvin Zook, MD.)
🔪 Surgical Technique 84-14
• Excise the tumor (which usually is well encapsulated) with a small knife or curet.
• Release the tourniquet, control bleeding with bipolar electrocautery, and close the wound in one layer with nylon interrupted suture.
Kuru I, Sualp T, Ferit D, et al: Factors affecting recurrence rate of ingrown toenail treated with marginal toenail ablation, Foot Ankle Int 25:410, 2004.](https://pubmed.ncbi.nlm.nih.gov/?term=subungual%20melanoma.%20%28From%20Tomczak%20RL%3A%20Embryology%20of%20the%20nail%20unit.%20In%20Myerson%20MS%2C%20ed%3A%20Foot%20and%20ankle%20disorders%2C%20Philadelphia%2C%202000%2C%20Saunders%3B%20courtesy%20of%20Elvin%20Zook%2C%20MD.%29%5D%28/media/hutaifortho/hutaifortho-references-p4791-a4fcbb.webp%29%0A%0A%2AFig.%2084-31%20Hutchinson%20sign.%20Band%20of%20pigmented%20tissue%20associated%20with%20subungual%20melanoma.%20%28From%20Tomczak%20RL%3A%20Embryology%20of%20the%20nail%20unit.%20In%20Myerson%20MS%2C%20ed%3A%20Foot%20and%20ankle%20disorders%2C%20Philadelphia%2C%202000%2C%20Saunders%3B%20courtesy%20of%20Elvin%20Zook%2C%20MD.%29%2A%0A%0A%3E%20%23%23%23%20%F0%9F%94%AA%20Surgical%20Technique%2084-14%0A%0A%E2%80%A2%20Excise%20the%20tumor%20%28which%20usually%20is%20well%20encapsulated%29%20with%20a%20small%20knife%20or%20curet.%0A%0A%E2%80%A2%20Release%20the%20tourniquet%2C%20control%20bleeding%20with%20bipolar%20electrocautery%2C%20and%20close%20the%20wound%20in%20one%20layer%20with%20nylon%20interrupted%20suture.%0A%0AKuru%20I%2C%20Sualp%20T%2C%20Ferit%20D%2C%20et%20al%3A%20Factors%20affecting%20recurrence%20rate%20of%20ingrown%20toenail%20treated%20with%20marginal%20toenail%20ablation%2C%20Foot%20Ankle%20Int%2025%3A410%2C%202004.)
- Lapidus PW: Complete and permanent removal of toe nail in onychogryphosis and subungual osteoma, Am J Surg 19:92, 1933.
- Lewis BL: Microscopic studies of fetal and mature nail and surrounding soft tissue, Arch Dermatol Syphilol 70:732, 1954.
- Lloyd-Davies RW, Brill GC: The aetiology and out-patient management of ingrowing toe-nails, Br J Surg 50:592, 1963.
- Lokiec F, Ezra E, Krasin E, et al: A simple and effi cient surgical technique for
You Might Also Like