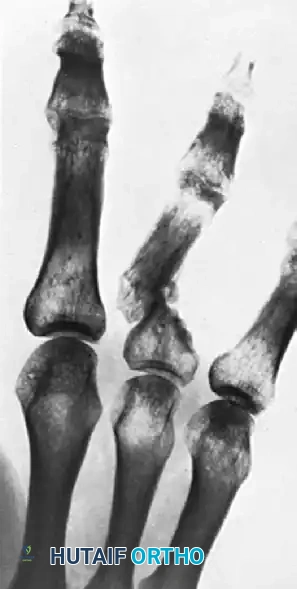
Thumb MCP Joint Collateral Ligament Reconstruction: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for a masterclass on chronic thumb MCP joint collateral ligament reconstruction. We'll meticulously detail surgical anatomy, patient positioning, and step-by-step execution for UCL and RCL tears using tendon grafts. Learn critical pearls, avoid pitfalls, and understand comprehensive postoperative management to restore stability and function to the thumb.
Introduction and Pathogenesis
Chronic instability of the thumb metacarpophalangeal (MCP) joint primarily involves the ulnar collateral ligament (UCL) and, less frequently, the radial collateral ligament (RCL). This pathology typically arises from unrecognized, untreated, or inadequately managed acute ligamentous disruptions. Less commonly, chronic repetitive microtrauma leads to progressive attenuation and eventual incompetence of the ligamentous complex.
The pathogenesis of UCL injuries classically involves forceful hyperabduction and extension of the thumb, often occurring during a fall onto an outstretched hand with the thumb abducted (e.g., "skier's thumb" or "gamekeeper's thumb"). This mechanism places extreme valgus stress on the MCP joint, leading to avulsion of the UCL from its insertion at the base of the proximal phalanx, midsubstance rupture, or avulsion from the metacarpal origin. Chronic UCL instability generally stems from four primary clinical scenarios:
1. Failure to diagnose an acute, complete ligamentous rupture.
2. Failure to identify a Stener lesion, leading to futile nonoperative management.
3. Inadequate immobilization of an acute tear lacking a Stener lesion.
4. Progressive ligamentous attenuation secondary to repetitive occupational or athletic trauma.
Conversely, RCL tears result from forceful ulnar deviation and extension of the MCP joint. Proximal and distal avulsions occur with relatively equal frequency, whereas intrasubstance tears remain rare. Chronic RCL instability is most often due to missed diagnoses or the historical tendency of clinicians to manage radial-sided injuries less aggressively than their ulnar counterparts.
Regardless of the side injured, complete disruption of the collateral ligament complex results in rotatory subluxation of the MCP joint. When one collateral ligament is rendered incompetent while the other remains intact, the base of the proximal phalanx translates volarly on the injured side, rotating around the longitudinal axis of the intact ligament. This volar translation creates a prominent dorsal metacarpal head on the injured side, altering joint kinematics and leading to asymmetric articular wear.
Surgical Anatomy and Biomechanics
A profound understanding of thumb MCP joint anatomy is a prerequisite for successful ligamentous reconstruction. The joint exhibits biomechanical characteristics of both a condyloid (ellipsoid) and a ginglymus (hinge) articulation. The metacarpal head is asymmetric; the radial condyle is taller in the dorsovolar dimension compared to the ulnar condyle, which dictates the complex tracking of the proximal phalanx during flexion and extension.
The Ligamentous Complex
The collateral ligament complex on both the radial and ulnar sides consists of two distinct anatomical structures:
* Proper Collateral Ligament (PCL): Originates from the dorsal-proximal fossae of the metacarpal head and passes obliquely to insert on the volar third of the base of the proximal phalanx. The PCL is tight in MCP joint flexion and lax in extension. It is the primary restraint to varus/valgus stress when the joint is flexed.
* Accessory Collateral Ligament (ACL): Originates contiguous with, but slightly volar to, the PCL. It extends obliquely to insert onto the volar plate and the sesamoid bones. The ACL is tight in MCP joint extension and lax in flexion.
A complete ligamentous rupture, by biomechanical definition, requires the disruption of both the proper and accessory collateral ligaments.
The Aponeurotic Anatomy and the Stener Lesion
The dynamic stabilizers of the thumb MCP joint include the adductor and abductor aponeuroses.
* Adductor Aponeurosis (Ulnar side): An extension of the adductor pollicis tendon, contributing oblique fibers to the extensor mechanism.
* Abductor Aponeurosis (Radial side): An extension of the abductor pollicis brevis tendon, which is notably wider than the adductor aponeurosis.
The anatomical relationship between the UCL and the adductor aponeurosis is the basis for the Stener lesion. When the proximal phalanx forcefully deviates radially (typically >70 degrees), the UCL avulses from its distal insertion. As the phalanx rebounds to a neutral posture, the proximal stump of the UCL can become superficial and proximal to the adductor aponeurosis. The aponeurosis acts as an interposing mechanical barrier between the ruptured ligament and its anatomical footprint, precluding spontaneous healing and necessitating surgical intervention.
Because the abductor aponeurosis on the radial side is substantially wider, the ends of a torn RCL typically remain deep to the aponeurosis. Therefore, a Stener-equivalent lesion on the radial side is an anatomical rarity.
Neurovascular Considerations
The dorsoulnar and dorsoradial digital nerves, terminal branches of the superficial sensory branch of the radial nerve, invariably cross the operative field. They lie in the subcutaneous plane immediately superficial to the adductor and abductor aponeuroses. Iatrogenic injury or forceful retraction of these nerves during exposure can result in debilitating neurapraxia, neuroma formation, or hypesthesia over the dorsal thumb.
Natural History and Clinical Presentation
Uncorrected chronic collateral ligament instability leads to a predictable cascade of functional deficits. Patients experience progressive weakness in pinch and grip strength due to the loss of the thumb as a stable post. For example, UCL incompetence severely diminishes the thumb's ability to provide counter-pressure against the index finger during key pinch. RCL instability frequently manifests as pain during torsional loads, such as turning a key or unscrewing a jar lid.
Over time, the chronic rotatory subluxation and incongruity of the joint lead to asymmetric cartilage wear and posttraumatic osteoarthritis. Once advanced arthrosis develops, joint reconstruction is contraindicated, and arthrodesis becomes the salvage procedure of choice.
Patient History and Physical Findings
The clinical evaluation begins with a detailed history, focusing on remote trauma, insidious onset of pain with grasp/pinch, and occupational demands.
Physical examination requires meticulous observation and palpation:
* Resting Posture: Chronic incompetence often presents with a static angulated or rotated resting posture. Chronic RCL instability frequently exhibits a visible dorsal prominence on the radial aspect of the metacarpal head.
* Palpation: Tenderness is localized to the injured collateral ligament footprint. A palpable, tender soft-tissue mass on the ulnar aspect of the metacarpal head is pathognomonic for a Stener lesion.
* Stress Testing: The definitive clinical test. The joint is stressed in both full extension (testing the ACL and volar plate) and 30 degrees of flexion (isolating the PCL).
* Diagnostic criteria for complete rupture include 30 to 35 degrees of absolute laxity when stressed in extension, or >15 degrees of asymmetric laxity compared to the contralateral uninjured thumb when stressed in 30 degrees of flexion.
* The End Point: The absence of a firm, discrete end point during valgus/varus stress is highly specific for a complete ligamentous disruption.
* Assessment for Arthrosis: The joint must be axially loaded while passively moved through flexion, extension, and radioulnar deviation. Crepitus or deep joint pain suggests underlying osteoarthritis, which dictates a shift in the surgical algorithm toward arthrodesis.
Imaging and Diagnostic Studies
Standard radiographic evaluation includes posteroanterior (PA), lateral, and oblique views of bilateral thumbs.
* Plain Radiographs: Essential to rule out avulsion fractures, metacarpal head fractures, or base of proximal phalanx fractures. The lateral view is critical for identifying volar subluxation of the proximal phalanx, which indicates extension of the collateral ligament tear into the dorsal capsule.
* Stress Radiographs: While historically recommended to document the degree of joint opening, most experienced hand surgeons rely on clinical stress testing. Stress views may be obtained primarily for medicolegal or academic documentation.
* Advanced Imaging (MRI/Ultrasound): While highly sensitive for identifying acute Stener lesions, advanced imaging is rarely indicated in the setting of chronic instability. The chronicity of the injury and the established clinical laxity already dictate the need for surgical reconstruction; identifying a Stener lesion preoperatively will not alter the surgical approach (tendon graft reconstruction).
* Arthroscopy: The role of MCP joint arthroscopy remains investigational. While it offers excellent visualization of articular cartilage and ligamentous remnants, arthroscopic reconstruction techniques are technically demanding and have not yet demonstrated reproducible superiority over open techniques.
Differential Diagnosis
When evaluating a patient for chronic thumb MCP instability, the surgeon must consider:
* Fracture of the thumb metacarpal head or the base of the proximal phalanx.
* Chronic synovitis of the MCP joint (e.g., inflammatory arthropathies).
* Chronic partial tear (Grade II) of the UCL or RCL.
* Primary or posttraumatic MCP joint arthrosis.
Indications and Contraindications for Surgery
Indications
The primary indication for ligamentous reconstruction is persistent pain and symptomatic instability of the MCP joint that has failed a dedicated course of nonoperative management (thermoplastic splinting, NSAIDs, judicious corticosteroid injections). While instability alone is considered a "soft" indication, prophylactic reconstruction to prevent asymmetric articular wear and subsequent osteoarthritis is a valid biomechanical rationale, provided the patient accepts the rigorous postoperative rehabilitation requirements.
Contraindications
- Osteoarthritis: Significant chondromalacia or established arthrosis is an absolute contraindication to soft-tissue reconstruction. Stabilizing an arthritic joint will paradoxically increase contact pressures and exacerbate pain, ultimately requiring conversion to an arthrodesis.
- Multidirectional Instability: Suggests global capsuloligamentous incompetence.
- Fixed Subluxation: Reconstructing a fixed deformity requires extensive capsular releases, which often results in iatrogenic multidirectional instability or rapid recurrence of the deformity.
Note on Chronicity: Traditional surgical dogma suggests that ligaments torn for more than 6 weeks cannot be primarily repaired. However, if the native ligament remnant remains supple and can be mobilized to its anatomic footprint without excessive tension, delayed primary repair may be attempted. If the tissue is contracted, fibrotic, or deficient, free tendon graft reconstruction is mandatory.
Preoperative Planning and Patient Positioning
During the preoperative clinic visit, the surgeon must assess for the presence of the palmaris longus (PL) tendon, which serves as the primary graft source. The patient is asked to actively oppose all five digits while simultaneously flexing the wrist against resistance to visualize and palpate the PL tendon at the volar wrist.
The patient is positioned supine on the operating table. The operative arm is extended onto a radiolucent hand table at an angle slightly less than 90 degrees to the torso. A pneumatic upper arm tourniquet is utilized for hemostasis. Examination under anesthesia (EUA) is performed prior to incision to confirm the degree of laxity without patient guarding.
Surgical Technique: Ulnar Collateral Ligament Reconstruction (Tendon Graft)
Exposure and Joint Preparation
A lazy S or chevron-shaped incision is centered over the ulnar midaxial line of the MCP joint.
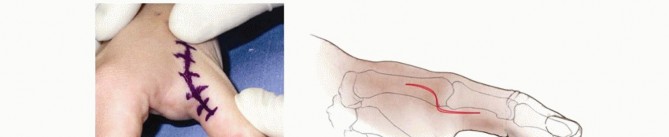
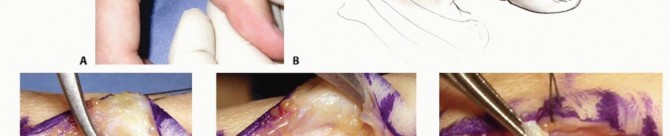
Full-thickness skin flaps are elevated and retracted using 4-0 silk stay sutures. Meticulous blunt dissection is required to identify and protect the terminal branches of the dorsoulnar sensory nerve, which invariably traverse the operative field.
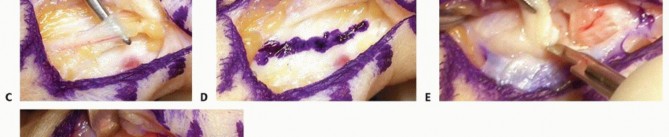
The adductor aponeurosis is identified. In chronic cases, it is often thickened and fibrotic. If a Stener lesion is present, the proximal stump of the UCL may be visible superficial to the aponeurosis. The aponeurosis is incised longitudinally, leaving a 2-mm dorsal cuff of tissue to facilitate robust repair during closure.

The underlying remnants of the UCL are inspected. If the tissue is inadequate for direct repair, the fibrotic remnants are excised to expose the ulnar aspect of the metacarpal head and the base of the proximal phalanx. The MCP joint is gently "booked open" to inspect the articular surfaces. Mild chondromalacia is acceptable, but widespread eburnation dictates immediate conversion to MCP arthrodesis.
Osseous Preparation
Bone tunnels must be created to anatomically route the tendon graft.
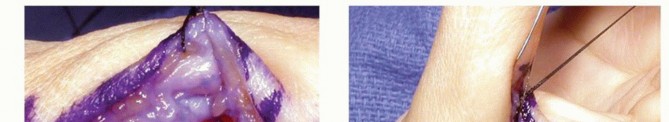
For the proximal phalanx (viewing a right thumb en face), holes are placed at the 7 o'clock and 11 o'clock positions. Using handheld gouges or a small burr, the holes are directed at a 45-degree angle to converge within the medullary canal, creating a continuous V-shaped bone tunnel. A critical surgical pearl is to ensure an adequate cortical bone bridge remains between the holes to prevent iatrogenic fracture during graft tensioning. A 28-gauge stainless steel wire (or a 0-polypropylene suture loop) is pre-bent and passed through the tunnel to serve as a shuttle relay for the graft.
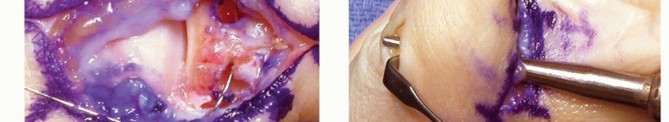
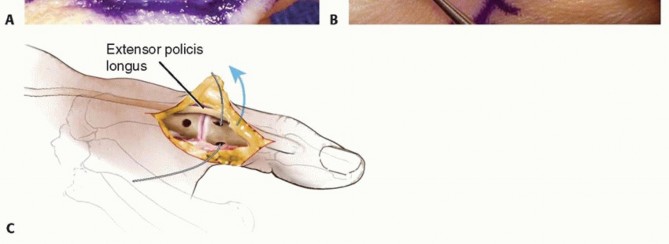
Next, a single large bone tunnel is created in the metacarpal neck. Starting at the anatomic footprint of the UCL origin on the ulnar metacarpal head, a gouge is directed obliquely from distal-ulnar to proximal-radial, exiting the radial cortex. A small 1-cm counter-incision is made radially over the exiting gouge to retrieve the graft. A second 28-gauge wire is placed through this trans-metacarpal tunnel.
Prior to graft passage, a 0.045-inch double-arm Kirschner wire (K-wire) is preset into the metacarpal head. It is driven retrograde through the radial cortex and withdrawn until the tip sits just deep to the articular cartilage, ready to transfix the joint later in the procedure.
Tendon Graft Harvest and Passage
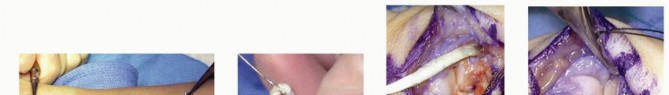
The palmaris longus tendon is harvested using either two small transverse volar incisions or a standard tendon stripper. Extreme care is taken to protect the median nerve, which lies deep and slightly radial to the PL.
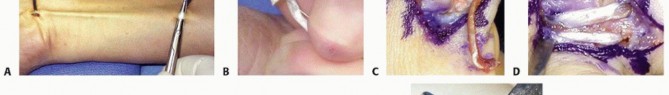
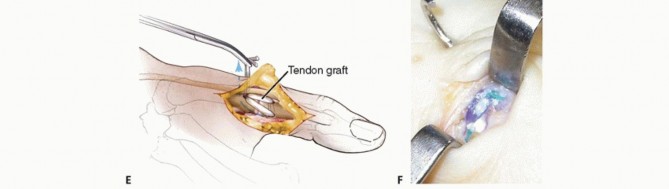
The harvested graft is moistened with saline. One end of the graft is secured to the volar limb of the proximal phalangeal wire loop. Using a combination of longitudinal traction and a gentle circular motion, the graft is shuttled into the volar hole and out the dorsal hole of the proximal phalanx.
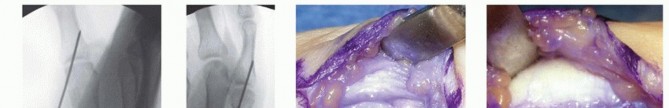
Once the graft is centered in the proximal phalanx, both free ends are captured by the ulnar limb of the metacarpal wire loop. Both limbs of the graft are then simultaneously shuttled through the metacarpal bone tunnel, exiting on the radial side of the metacarpal neck.
Tensioning, Fixation, and Closure
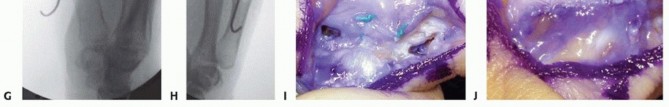
Appropriate tensioning is the most critical step of the reconstruction. Tension is set by pulling both limbs of the graft radially while simultaneously applying a radially directed stress to the proximal phalanx (reducing the joint). The joint is taken through a range of motion to ensure it is neither over-constrained (limiting flexion) nor under-constrained (allowing laxity).
Once optimal tension is achieved, the two ends of the graft are tied into a knot over the radial metacarpal cortex. This knot is rigidly secured to the adjacent radial periosteum using multiple 3-0 braided nonabsorbable mattress sutures. Alternatively, a suture anchor can be placed adjacent to the radial tunnel exit to secure the graft.
The joint is held in anatomic reduction, and the preset 0.045-inch K-wire is driven antegrade across the MCP joint into the proximal phalanx to temporarily neutralize shear forces. The pin is bent and cut outside the skin. For augmented stability, the graft is sutured to any remaining native collateral ligament tissue on the ulnar side. The adductor aponeurosis is meticulously repaired with 5-0 absorbable suture, ensuring it glides independently of the underlying reconstructed ligament. The skin is closed with 4-0 subcuticular or 5-0 interrupted sutures, and a forearm-based thumb spica splint is applied.
Surgical Technique: Radial Collateral Ligament Reconstruction (Tendon Graft)
The principles for RCL reconstruction mirror those of UCL reconstruction, with anatomical modifications specific to the radial side.
Exposure and Joint Preparation

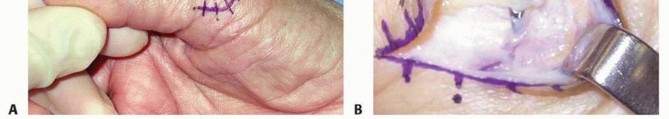
A lazy S incision is utilized over the radial aspect of the MCP joint. The dorsal radial sensory nerve branches are identified and meticulously protected. The broad abductor aponeurosis is incised longitudinally. In chronic RCL tears, the ligament is often densely adherent to the aponeurosis. The fibrotic RCL remnants are excised, and the joint is inspected for arthrosis.
Osseous Preparation and Graft Passage

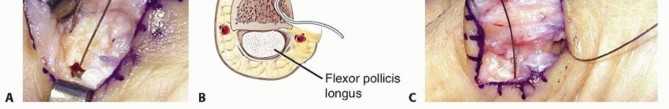
For the proximal phalanx (viewing a right thumb laterally), the converging bone tunnels are created at the 1 o'clock and 5 o'clock positions.
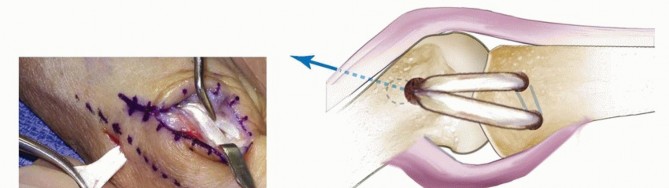
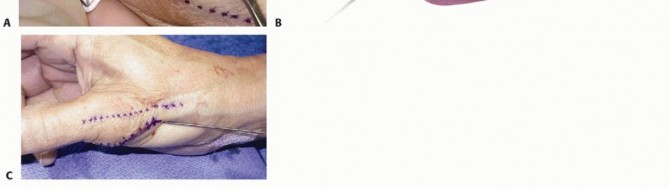
The metacarpal bone tunnel is initiated at the RCL anatomic footprint on the radial metacarpal head and directed obliquely to exit on the ulnar cortex. The PL tendon graft is shuttled through the proximal phalanx, and both ends are passed from radial to ulnar through the metacarpal tunnel. Tensioning is performed while applying ulnar stress to the joint. The graft is knotted and secured on the ulnar cortex, the joint is transfixed with a K-wire, and the abductor aponeurosis is repaired.
Surgical Pearls and Pitfalls
- Nerve Management: Excessive traction on the superficial radial nerve branches is the most common cause of postoperative morbidity. Dysesthesia or neuroma formation can be more debilitating than the original instability. Use gentle, static retraction.
- Bone Tunnel Creation: Handheld gouges provide superior tactile feedback compared to power drills. Power drills risk thermal necrosis of the bone and can inadvertently wrap up adjacent soft tissues if a drill guide is not meticulously used.
- Preserving the Bone Bridge: The most catastrophic intraoperative complication is fracturing the cortical bridge between the proximal phalangeal holes. To prevent this, ensure the holes are spaced adequately apart. When pulling the wire/graft through the tunnel, apply traction parallel to the axis of the tunnel with a twisting motion. Pulling perpendicular to the tunnel places immense shear stress on the cortical bridge. If the bridge fractures, the surgeon must pivot to suture anchors or transosseous periosteal routing.
- Graft Tensioning: Over-tensioning results in a stiff, painful joint. Under-tensioning results in failure of the procedure. Always test ROM and stability prior to final knot fixation.
- Wire Handling: Never wrap the passing wire manually around your fingers; the required force can easily lacerate the surgeon's gloves and skin. Always use a heavy hemostat to grasp and pull the wire.
Postoperative Rehabilitation Protocols
Rigorous adherence to postoperative rehabilitation is paramount.
* Weeks 0-6: The thumb is continuously immobilized in a forearm-based thumb spica cast or rigid splint. The interphalangeal (IP) joint is left free to prevent distal stiffness.
* Week 6: The cast and the transarticular K-wire are removed in the clinic. A custom-molded thermoplastic short opponens splint is fabricated. Active and active-assisted ROM exercises for MCP flexion and extension are initiated (12 repetitions, 4 times daily). Lateral stress must be strictly avoided.
* Weeks 8-12: The thermoplastic splint is weaned for daily activities but retained for strenuous tasks. Light strengthening with therapy putty begins.
* Weeks 12-16: Formal pinch and grip strengthening protocols are initiated.
* Week 16: Return to full, unrestricted athletic and occupational activities.
Clinical Outcomes and Complications
Tendon graft reconstruction for chronic collateral ligament instability yields highly predictable and satisfactory results, closely mirroring outcomes of acute primary repair.
* Range of Motion: Patients typically regain approximately 80% of native MCP joint motion and 94% of IP joint motion compared to the contralateral uninjured side. RCL reconstructions tend to be slightly stiffer, recovering roughly 60% of native MCP motion.
* Strength: Key pinch strength returns to >90% (averaging 95%), and grip strength normalizes to >100% of the unoperated thumb.
* Pain and Function: Nearly 70% of patients report zero pain at final follow-up, with the remainder noting only mild, intermittent discomfort. Functional limitations are minimal to nonexistent in nearly 90% of cohorts. Reconstructions performed on joints without pre-existing arthrosis rarely require late revision or arthrodesis.
Complications:
* Transient Hypesthesia: Common due to nerve retraction; typically resolves spontaneously within 6 to 12 weeks.
* Joint Stiffness: Usually secondary to over-tensioning of the graft or prolonged immobilization.
* Recurrent Laxity: Can occur from under-tensioning, premature aggressive rehabilitation (e.g., initiating key pinch exercises before 12 weeks), or failure of graft incorporation.
* Intraoperative Cortical Fracture: Managed with alternative fixation strategies (anchors) as discussed in the pitfalls section.
References and Suggested Readings
References
You Might Also Like