Operative Management of Monteggia and Distal Humerus Nonunions

Key Takeaway
Long-standing nonunions of the proximal ulna associated with radial head dislocations (Monteggia fractures) present complex reconstructive challenges. Surgical management typically involves resection of the dislocated radial head rather than attempted reduction, combined with rigid internal fixation of the ulna using compression plating or intramedullary nailing, supplemented by autologous iliac crest bone grafting. Distal humeral nonunions require meticulous rigid fixation, ulnar nerve neurolysis, and structural grafting to prioritize bone healing over immediate motion.
NONUNION OF THE PROXIMAL THIRD OF THE ULNA WITH DISLOCATION OF THE RADIAL HEAD (MONTEGGIA FRACTURE)
The management of long-standing nonunions of the proximal third of the ulna associated with chronic dislocation of the radial head—the classic missed or failed Monteggia fracture-dislocation—represents a formidable challenge in reconstructive orthopaedic surgery. The proximal ulna dictates the anatomic length and alignment of the forearm; thus, an ununited, deformed ulna invariably leads to persistent radiocapitellar instability, restricted forearm rotation, and debilitating elbow pain.
In chronic, long-standing instances of this pathology, the radiocapitellar joint undergoes irreversible morphologic changes. The radial head becomes hypertrophic or deformed, the capitellum loses its congruent articular cartilage, and the annular ligament is replaced by dense fibrotic scar tissue. Consequently, no attempt is made to reduce the chronic radial head dislocation. Forcible reduction in this setting leads to severe loss of motion, radiocapitellar arthritis, and high rates of re-dislocation. Instead, the surgical strategy mandates resection of the radial head and as much of the radial neck as necessary to restore unhindered forearm pronation and supination, coupled with aggressive reconstruction of the ulnar pseudarthrosis.
Surgical Pearl: The primary goal in chronic Monteggia nonunions is the restoration of ulnar length and stable internal fixation. The radial head is a secondary stabilizer of the elbow; in the presence of a chronic dislocation with a competent medial ulnar collateral ligament (MUCL), radial head excision is well tolerated and reliably restores forearm rotation.
Preoperative Planning and Biomechanics
Preoperative evaluation must include orthogonal radiographs of the elbow and forearm. Computed tomography (CT) is highly recommended to assess the exact morphology of the ulnar nonunion, the presence of segmental bone loss, and the degree of sclerosis at the fracture margins.
Biomechanically, the proximal ulna is subjected to significant bending and torsional forces. A nonunion in this region is typically atrophic or oligotrophic due to the poor soft-tissue envelope and the inherent instability of the initial injury. Therefore, achieving union requires both absolute mechanical stability (via rigid internal fixation) and biological augmentation (via autologous bone grafting).
Surgical Technique: Step-by-Step
1. Patient Positioning and Approach
The patient is positioned supine with the affected arm draped free on a radiolucent hand table. A sterile tourniquet is applied high on the arm. A modified Boyd approach or separate incisions (a posterolateral Kocher approach for the radial head and a posterior approach for the ulna) may be utilized. The posterior approach to the ulna utilizes the internervous plane between the extensor carpi ulnaris (posterior interosseous nerve) and the flexor carpi ulnaris (ulnar nerve).
2. Radial Head Resection
The radiocapitellar joint is accessed. The dislocated, often deformed radial head is identified. A retractor is carefully placed to protect the posterior interosseous nerve (PIN), which may be distorted due to the chronic dislocation. The radial head and a portion of the neck are resected using an oscillating saw. The level of resection should be just proximal to the bicipital tuberosity to preserve the insertion of the biceps brachii.

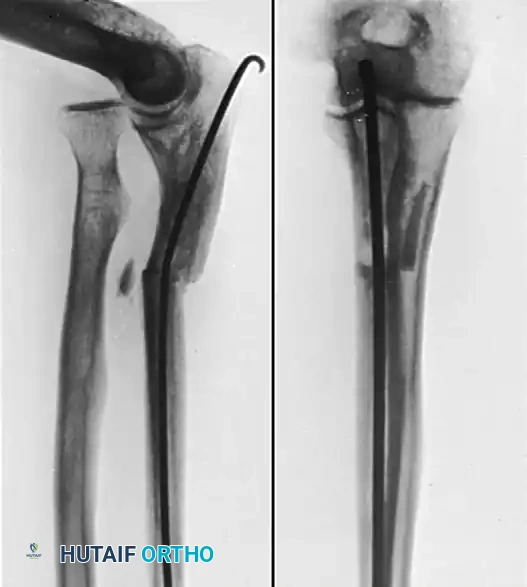
Figure A: Radiographic demonstration of a chronic nonunion of the ulna following radial head excision. Note the sclerotic margins and the retained wire/suture material from previous failed interventions.
3. Preparation of the Ulnar Nonunion
Attention is then directed to the ulnar nonunion. The pseudarthrosis is taken down meticulously. All intervening fibrous tissue is excised, and the sclerotic bone ends are decorticated using a high-speed burr or osteotomes until punctate bleeding (the "paprika sign") is observed, indicating healthy, vascularized bone. If an angular deformity exists, the ulnar ends must be mobilized and realigned to restore the anatomic bow of the proximal ulna.
4. Internal Fixation and Bone Grafting
The fragments of the ulna are fixed with either a rigid compression plate (typically a 3.5-mm dynamic compression plate or locking compression plate) or a locked intramedullary nail, depending on the fracture morphology and surgeon preference.
* Plate Fixation: If plating is chosen, a minimum of six cortices of fixation proximal and distal to the nonunion is required. Compression should be achieved across the nonunion site if the fracture pattern allows.
* Intramedullary Nailing: In cases of poor bone quality or specific segmental defects, a locked forearm nail can provide excellent load-sharing biomechanics.
Once rigid fixation is achieved, copious autologous iliac crest bone grafts (cancellous or tricortical, depending on the presence of a structural defect) are placed circumferentially around the nonunion site to provide osteoinductive and osteoconductive stimuli.
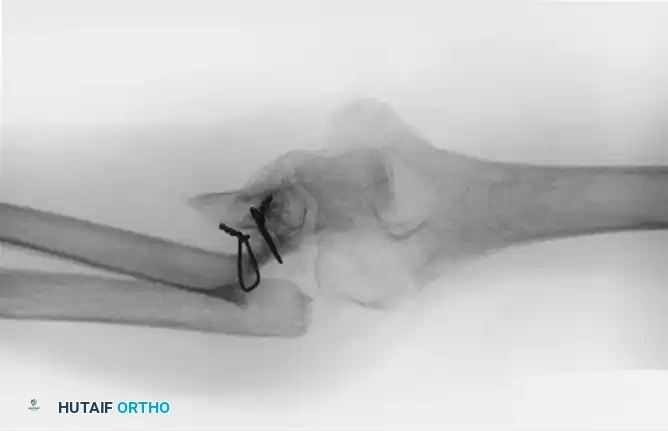
Figure B: Proximal ulnar fracture nonunion successfully treated with a locked forearm intramedullary nail and a tricortical iliac crest bone graft to bridge the defect and restore ulnar length.
Postoperative Protocol
Postoperatively, the arm is placed in a well-padded posterior splint at 90 degrees of elbow flexion for 10 to 14 days to allow soft-tissue healing. Following suture removal, active and active-assisted range of motion (ROM) of the elbow and forearm is initiated. Weight-bearing and heavy lifting are strictly prohibited until radiographic evidence of bridging callus is observed, typically between 8 and 12 weeks.
NONUNIONS OF BOTH FOREARM BONES
When treating nonunions involving both the radius and the ulna, the surgical complexity increases exponentially. The forearm functions as a complex joint ring; thus, the anatomic relationship between the radius and ulna must be perfectly restored to salvage pronation and supination.
When resecting the sclerotic ends of the fragments, the surgeon must stay within the permissible amount of bone resection (typically less than 1-2 cm) to avoid severe shortening of the forearm, which would slacken the interosseous membrane and destabilize the distal radioulnar joint (DRUJ). If resection exceeds this permissible amount, structural intercalary bone grafting (such as a tricortical iliac crest graft or a free vascularized fibular graft) becomes mandatory to restore length. Both bones must be rigidly fixed with 3.5-mm compression plates, and autologous cancellous bone grafting is routinely applied to both nonunion sites.
DISTAL HUMERUS NONUNIONS
Nonunions of the distal humerus are profoundly debilitating, severely compromising the function of the entire upper extremity. Poor initial fracture fixation is the major reason for nonunion in the supracondylar area. The distal humerus is subjected to massive torsional and bending forces during elbow flexion and extension, and inadequate plate constructs or early aggressive mobilization often lead to hardware failure and subsequent pseudarthrosis.
While many patients treated for distal humeral fracture nonunions can expect eventual union with appropriate revision surgery, most will have residual morbidity, including permanent stiffness, weakness, and chronic pain. Patients with nonunions extending distally into the ulnar trochlear region fare worse than others, despite eventual union of the fracture, due to the disruption of the articular surface and the profound scarring of the elbow capsule.
Surgical Warning: Bone healing takes absolute precedence over motion when attempting to unite a distal humeral nonunion. The surgeon must not compromise the rigidity of the fixation in an attempt to allow early aggressive rehabilitation. Restoration of motion can be addressed after union has been achieved via physical therapy, dynamic splints, and delayed capsular releases as needed.
Surgical Management Strategies
The standard of care for aseptic distal humeral nonunions involves open reduction, rigid internal fixation, bone grafting, release of joint contractures, and meticulous management of the ulnar nerve.
1. Internal Fixation and Bone Grafting
For distal humeral nonunions, Sanders and Sackett recommended rigid internal fixation with a plate and screws combined with a bone graft. The current gold standard involves orthogonal (90-90) or parallel dual plating techniques using pre-contoured locking plates. The nonunion site is aggressively debrided, and the medullary canals are opened. Autologous cancellous bone graft from the iliac crest is packed into the defect. If there is medial column comminution, a structural graft may be required to prevent varus collapse.
Mitsunagase, Bryan, and Linscheid demonstrated the efficacy of this approach, obtaining union in 25 of 32 patients treated by open reduction, internal fixation, and bone grafting of the nonunion. Union of the fractures resulted in significant relief of pain and good functional motion of the elbow. However, the complexity of these cases is highlighted by their complication rate: six patients required secondary procedures for repeat bone grafting or revision of the fixation device.
2. Management of the Ulnar Nerve
The ulnar nerve is at extreme risk during both the initial injury and the reconstructive procedure. Ulnar nerve transposition or neurolysis is performed for almost all distal humeral nonunions. If a previous transposition is symptomatic or encased in scar tissue, a meticulous microscopic neurolysis is required. The nerve must be handled with vessel loops and protected throughout the procedure to prevent iatrogenic traction neuropraxia.
3. Advanced Reconstruction and Salvage Procedures
In cases of massive bone loss or in elderly patients with poor bone stock, standard ORIF may be destined to fail.
- Free Vascularized Bone Grafts: Beredjiklian et al. utilized free vascularized bone grafts (typically from the fibula) in patients with segmental bone loss in nonunions of the distal humerus. They reserve this highly technically demanding technique for younger, high-demand patients with segmental bone loss for which conventional fixation and non-vascularized bone grafting are inappropriate, and when a total elbow replacement would yield a poor long-term outcome due to lifting restrictions.
- Total Elbow Arthroplasty (TEA): In the series by Mitsunagase et al., seven patients were treated by total elbow arthroplasty, and two required reoperation for loose humeral components. TEA is strictly considered a salvage procedure. It is highly effective for pain relief and immediate stability in elderly, low-demand patients (typically over 65 years of age) with profound intra-articular nonunions where joint reconstruction is impossible. However, the lifetime 5-lb lifting restriction makes it unsuitable for young, active individuals.
Management of Infected Nonunions
Infected nonunions of the distal humerus represent the most severe end of the spectrum. The presence of osteomyelitis precludes immediate internal fixation. These complex cases are best treated with a staged approach:
1. Stage 1: Complete removal of all retained hardware, aggressive surgical débridement of all devascularized and infected bone and soft tissue, capsulectomy, and ulnar nerve transposition or neurolysis. An antibiotic-impregnated cement spacer is often placed to sterilize the bed and maintain the soft-tissue envelope.
2. Stage 2: Once the infection is eradicated (confirmed by normal inflammatory markers and negative cultures), bone grafting is performed when appropriate, and stability is achieved via the application of a ring fixator (Ilizarov frame). The ring fixator provides excellent stability, allows for compression across the nonunion site, and permits access for wound care without the risk of placing large metallic implants into a previously infected bed.
Postoperative Rehabilitation
The postoperative protocol for distal humeral nonunions is dictated by the stability of the fixation. Because bone healing is the paramount goal, the elbow is often immobilized in a splint or a hinged brace locked at 90 degrees for the first 2 to 4 weeks. Once early callus is visible, gentle active-assisted ROM is permitted. Aggressive passive stretching is avoided to prevent hardware failure. If profound stiffness persists after solid bony union is achieved (typically at 6 to 9 months), the patient may be offered an open or arthroscopic capsular release to optimize final functional outcomes.
You Might Also Like