In Situ Decompression of the Ulnar Nerve: Open and Endoscopic Techniques
Key Takeaway
In situ decompression of the ulnar nerve is a highly effective surgical intervention for cubital tunnel syndrome. This procedure involves releasing Osborne’s ligament and the aponeurosis of the flexor carpi ulnaris while leaving the nerve undisturbed in its native bed. Both open and endoscopic techniques yield excellent outcomes, provided meticulous care is taken to protect the medial antebrachial cutaneous nerve and iatrogenic subluxation is avoided.
Introduction to Cubital Tunnel Syndrome and Ulnar Nerve Decompression
Cubital tunnel syndrome is the second most common compression neuropathy of the upper extremity, surpassed only by carpal tunnel syndrome. It results from compression, traction, or friction of the ulnar nerve as it traverses the medial aspect of the elbow. While conservative management—such as nighttime extension splinting and activity modification—is the first line of treatment for mild cases, surgical intervention is indicated for patients with progressive motor weakness, severe sensory deficits, or refractory symptoms.
Historically, anterior transposition of the ulnar nerve (subcutaneous, intramuscular, or submuscular) was considered the gold standard. However, contemporary orthopedic literature heavily supports in situ decompression as the primary surgical intervention for idiopathic cubital tunnel syndrome without preoperative nerve subluxation. In situ decompression offers equivalent clinical outcomes to transposition but with significantly lower complication rates, reduced operative time, and faster postoperative rehabilitation.
This comprehensive guide details the surgical anatomy, indications, and step-by-step techniques for both open and endoscopic in situ decompression of the ulnar nerve.
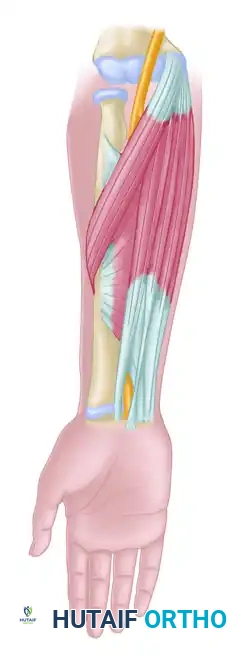
Relevant Surgical Anatomy and Biomechanics
A profound understanding of the medial elbow anatomy is paramount to performing a safe and complete decompression. The ulnar nerve can be compressed at five primary anatomical sites around the elbow.
The Five Sites of Ulnar Nerve Compression
- The Arcade of Struthers: A fascial band extending from the medial head of the triceps to the medial intermuscular septum, located approximately 8 cm proximal to the medial epicondyle. Present in roughly 70% of the population.
- The Medial Intermuscular Septum: The nerve pierces the septum to transition from the anterior to the posterior compartment of the arm.
- The Medial Epicondyle: Hypertrophy, osteophytes, or valgus deformity can cause direct osseous compression or increased traction.
- The Cubital Tunnel (Osborne’s Ligament): The true cubital tunnel is roofed by Osborne’s ligament (the cubital tunnel retinaculum), a fascial band bridging the medial epicondyle and the olecranon. The floor is formed by the medial collateral ligament (MCL) and the joint capsule.
- The Deep Flexor Pronator Aponeurosis: The fascial arcade between the humeral and ulnar heads of the flexor carpi ulnaris (FCU).
Biomechanics of the Cubital Tunnel
During elbow flexion, the geometry of the cubital tunnel changes dramatically. The distance between the medial epicondyle and the olecranon increases, drawing Osborne’s ligament taut. Simultaneously, the medial head of the triceps pushes the ulnar nerve medially, and the MCL bulges medially. This combination decreases the cross-sectional area of the cubital tunnel by up to 55%, leading to a multifold increase in extraneural and intraneural pressure.
The Medial Antebrachial Cutaneous (MABC) Nerve
The MABC nerve provides sensation to the medial aspect of the forearm. Its posterior branch is highly variable but typically crosses the operative field from anterior to posterior, approximately 2 to 3 cm distal to the medial epicondyle.
⚠️ Surgical Warning: MABC Nerve Injury
Iatrogenic injury to the posterior branch of the MABC nerve is the most common complication of open ulnar nerve surgery. Transection or entrapment in scar tissue can lead to a painful neuroma, which is often more debilitating for the patient than the original cubital tunnel syndrome. Meticulous superficial dissection is mandatory.
Indications and Patient Selection
Proper patient selection is the cornerstone of successful in situ decompression.
Indications for In Situ Decompression
- Mild to moderate idiopathic cubital tunnel syndrome refractory to conservative management (typically 3–6 months).
- Positive electrodiagnostic studies (EMG/NCS) demonstrating focal slowing or conduction block across the elbow.
- Absence of preoperative ulnar nerve subluxation or dislocation during dynamic elbow flexion.
Contraindications to In Situ Decompression
- Preoperative Nerve Subluxation: A nerve that snaps over the medial epicondyle requires an anterior transposition to prevent friction neuritis.
- Severe Valgus Deformity (Tardy Ulnar Palsy): Increased carrying angle places excessive traction on the nerve, necessitating transposition.
- Throwing Athletes: Overhead athletes (e.g., baseball pitchers) often have underlying MCL insufficiency or valgus extension overload; transposition is generally preferred.
- Post-Traumatic Cubital Tunnel Syndrome: Bony architectural distortion usually requires transposition.
Preoperative Preparation and Positioning
- Anesthesia: The procedure can be performed under general anesthesia, regional anesthesia (supraclavicular or axillary block), or even wide-awake local anesthesia no tourniquet (WALANT), depending on surgeon and patient preference.
- Positioning: The patient is placed supine on the operating table. The operative arm is positioned on a radiolucent hand table.
- Arm Position: The shoulder is abducted to 90 degrees and externally rotated. The elbow is flexed to approximately 45 to 90 degrees to bring the medial epicondyle and olecranon into clear view.
- Tourniquet: A non-sterile tourniquet is applied high on the brachium. Exsanguination is performed with an Esmarch bandage, and the tourniquet is inflated to 250 mmHg (or 100 mmHg above systolic blood pressure).
Open In Situ Decompression: Step-by-Step Surgical Technique
The open in situ decompression remains the workhorse procedure for cubital tunnel syndrome. It is highly effective, reproducible, and requires no specialized equipment.
1. Incision and Superficial Dissection
With the elbow flexed and the arm abducted and externally rotated, identify the medial epicondyle and the tip of the olecranon. Make a 3- to 5-cm longitudinal incision along the course of the ulnar nerve, centered exactly halfway between the medial epicondyle and the olecranon.
Spread the subcutaneous tissues longitudinally using tenotomy scissors. Develop the avascular plane overlying the deep fascia.
2. Identification and Protection of the MABC Nerve
Take extreme care to avoid damaging the medial antebrachial cutaneous (MABC) nerve. The posterior branches of the MABC lie superficially along the fascia, usually crossing the operative field about 3 cm distal to the medial epicondyle.
💡 Clinical Pearl: Retraction Technique
Use right-angle retractors (such as Senn or Ragnell retractors) to carefully elevate the subcutaneous tissue and the undivided cutaneous nerves off the deep fascia. Never use self-retaining retractors (like a Weitlaner) in the superficial subcutaneous layer, as the sharp prongs can easily crush or sever unseen MABC branches.
3. Fascial Release and Decompression
Identify the thickened fascia bridging the medial epicondyle and the olecranon—this is Osborne’s ligament.
- Proximal Release: Incise Osborne's ligament and continue the fascial release proximally over the ulnar nerve for a distance of 8 to 9 cm. Follow the nerve up to the medial intermuscular septum and the Arcade of Struthers. Ensure there are no proximal fascial bands tethering the nerve.
- Distal Release: Continue the incision distally, dividing both the deep and superficial fascia between the two heads (humeral and ulnar) of the flexor carpi ulnaris (FCU). The distal release should extend until the nerve dives freely into the anterior compartment of the forearm.
🛑 Pitfall: Iatrogenic Subluxation
Leave the ulnar nerve completely undisturbed in its native soft tissue bed. Do not circumferentially dissect the nerve or elevate it from the floor of the cubital tunnel. Excessive mobilization disrupts the segmental vascular supply (vasa nervorum) and destabilizes the nerve, leading to iatrogenic anterior subluxation.
4. Dynamic Assessment
Once the decompression is complete, reinspect the entire visible length of the nerve carefully for any remaining areas of compression.
Release the retractors and passively flex and extend the elbow through a full range of motion. Observe the ulnar nerve closely. Make absolutely certain that the nerve does not subluxate or dislocate anteriorly across the medial epicondyle during terminal flexion.
If subluxation occurs: The in situ decompression must be abandoned, and a formal anterior transposition (subcutaneous or submuscular) is strongly recommended to prevent postoperative friction neuritis.
5. Closure
Deflate the tourniquet prior to closure to obtain careful and meticulous hemostasis. Bipolar electrocautery should be used sparingly and strictly away from the nerve to prevent thermal injury.
Close the subcutaneous tissue with interrupted absorbable sutures (e.g., 3-0 or 4-0 Vicryl) to eliminate dead space. Close the skin with a running subcuticular suture or interrupted nylon sutures. Apply a soft, bulky compressive dressing.
Endoscopic Decompression of the Ulnar Nerve
Endoscopic decompression of the ulnar nerve at the elbow was first described by Tsai in 1999 and has since grown significantly in popularity among upper extremity specialists.
Rationale and Evidence
The primary goal of the endoscopic technique is to achieve the same extensive proximal and distal release as an open procedure but through a much smaller incision.
The reported advantages of endoscopic decompression include:
* A smaller skin incision (typically 1.5 to 2 cm).
* Less soft tissue dissection and disruption of the vascular bed.
* Decreased incidence of incisional tenderness.
* Enhanced visualization and protection of the medial antebrachial cutaneous (MABC) nerve branches.
The clinical outcomes of endoscopic decompression have been shown to be highly comparable to open in situ decompression. A notable nonrandomized level III study reported a 60% (9 of 15) patient satisfaction rate with open in situ decompression compared with a 79% (15 of 19) satisfaction rate in the endoscopic group. While some surgeons have no experience with this technique, those who adopt it often cite faster early return to work and reduced scar hypersensitivity.
Endoscopic Surgical Technique Overview
- Portal Placement: A 1.5- to 2-cm transverse or longitudinal incision is made directly over the cubital tunnel, slightly proximal to the medial epicondyle.
- Superficial Dissection: The subcutaneous tissue is bluntly spread to identify the deep fascia and the ulnar nerve. The MABC branches are identified and swept away from the portal site.
- Cannula Insertion: A specialized slotted cannula or a clear endoscopic retractor system is introduced over the ulnar nerve, first directed proximally.
- Proximal Release: Under direct endoscopic visualization (using a 30-degree, 4.0-mm endoscope), the fascia overlying the nerve, including the medial intermuscular septum and the Arcade of Struthers, is divided using endoscopic scissors or a retrograde knife.
- Distal Release: The cannula is then redirected distally. Osborne’s ligament and the aponeurosis between the two heads of the FCU are visualized and divided.
- Dynamic Testing: Just as in the open technique, the endoscope is removed, and the elbow is taken through a full range of motion to ensure the nerve remains stable in its bed and does not subluxate.
💡 Clinical Pearl: The Learning Curve
Endoscopic ulnar nerve decompression has a steep learning curve. Surgeons transitioning to this technique must maintain a low threshold for converting to an open procedure if visualization is compromised, if bleeding obscures the camera, or if there is any doubt regarding the completeness of the release.
Complications and Avoidance
While in situ decompression is generally a safe procedure, complications can occur and must be actively mitigated.
- Incomplete Decompression: The most common cause of persistent postoperative symptoms. This usually results from a failure to release the distal FCU aponeurosis or the proximal medial intermuscular septum. An 8 to 9 cm proximal release and a thorough distal release are mandatory.
- MABC Neuroma: As previously emphasized, injury to the MABC nerve causes severe, burning medial elbow pain. Avoid transverse incisions and avoid blind placement of self-retaining retractors.
- Iatrogenic Nerve Instability: Caused by over-dissection of the nerve from its bed. If the nerve subluxates intraoperatively, convert to a transposition.
- Hematoma Formation: The cubital tunnel is a highly vascular area. Always deflate the tourniquet and achieve meticulous hemostasis before closure. A postoperative hematoma can lead to perineural fibrosis and recurrent compression.
- Infection: Superficial surgical site infections are rare but should be treated promptly with oral antibiotics. Deep infections may require surgical irrigation and debridement.
Postoperative Rehabilitation Protocol
The postoperative protocol for in situ decompression (both open and endoscopic) is designed to promote nerve gliding and prevent perineural adhesions.
- Immediate Postoperative Phase (Days 0-7): A soft, bulky dressing is applied in the operating room. Unlike anterior transposition, which often requires a period of immobilization in a splint, in situ decompression allows for immediate elbow motion. Patients are encouraged to perform active range of motion (AROM) exercises for the fingers, wrist, and elbow as tolerated to prevent neural adhesions.
- Suture Removal (Days 10-14): The bulky dressing is removed, and sutures are taken out. Patients may begin showering normally.
- Intermediate Phase (Weeks 2-4): Patients are instructed to perform nerve gliding exercises. Light activities of daily living (ADLs) are permitted. Heavy lifting, forceful gripping, and repetitive elbow flexion are restricted.
- Return to Activity (Weeks 4-6): Progressive strengthening is initiated. Most patients can return to unrestricted activities, including heavy manual labor and sports, by 6 weeks postoperatively, provided they have regained full, painless range of motion and baseline strength.
Conclusion
In situ decompression of the ulnar nerve is a highly reliable, evidence-based surgical intervention for cubital tunnel syndrome. By meticulously releasing the compressive fascial structures—from the Arcade of Struthers proximally to the FCU aponeurosis distally—surgeons can achieve excellent clinical outcomes. Whether utilizing the traditional open approach or the minimally invasive endoscopic technique, the fundamental principles remain the same: protect the medial antebrachial cutaneous nerve, ensure a complete fascial release, leave the ulnar nerve undisturbed in its native bed, and verify dynamic stability prior to closure. Adherence to these principles minimizes complications and maximizes the potential for full neurologic recovery.
You Might Also Like