Bowler's Thumb: Comprehensive Management of Ulnar Digital Nerve Fibrosis
Key Takeaway
Bowler's Thumb, or perineural fibrosis of the ulnar digital nerve, results from repetitive compression during bowling. This guide details its pathophysiology, clinical presentation, and diagnostic criteria. It outlines conservative management and advanced surgical techniques, including neurolysis and dorsal nerve transfer, for refractory cases, ensuring optimal patient outcomes and return to sport.
Introduction to Bowler's Thumb
Bowler's Thumb, also known as a traumatic perineural fibroma or neuroma of the ulnar proper digital nerve of the thumb, is a distinct clinical entity characterized by localized perineural fibrosis. This condition arises from chronic, repetitive microtrauma to the nerve, typically observed in individuals engaged in activities that involve sustained or forceful gripping with specific thumb positioning, most notably bowling. The resultant fibrous thickening around the nerve leads to a constellation of neuropathic symptoms, significantly impacting hand function and quality of life for affected individuals.
Etiology and Epidemiology
The primary etiology of Bowler's Thumb is repetitive mechanical compression and shear forces applied to the ulnar aspect of the thumb's metacarpophalangeal (MCP) joint and proximal phalanx. In bowling, this occurs as the thumb is repeatedly inserted into and extracted from the bowling ball's thumbhole. The edge of the thumbhole, particularly if ill-fitting or with sharp edges, acts as a fulcrum, causing direct pressure and friction on the ulnar digital nerve.
- Repetitive Trauma: The condition is almost exclusively seen in avid bowlers, particularly those who bowl several times a week or engage in high-volume play.
- Thumbhole Fit: An improperly sized or shaped thumbhole is a significant contributing factor. A tight thumbhole can cause excessive compression, while a loose one may lead to increased friction and shear as the thumb shifts.
- Bowling Technique: Certain gripping techniques or ball release mechanics can exacerbate nerve irritation.
- Other Activities: While less common, similar conditions have been reported in individuals involved in other activities requiring repetitive thumb compression, such as certain industrial tasks or specific sports.
The exact incidence is not well-documented, but it is recognized as an occupational hazard for professional and amateur bowlers. It typically affects the dominant hand, though bilateral involvement is possible.
Relevant Anatomy and Biomechanics
A thorough understanding of the anatomy of the thumb's digital nerves and the biomechanics of bowling is crucial for diagnosing and managing Bowler's Thumb.
Anatomy of the Ulnar Proper Digital Nerve of the Thumb
The thumb receives sensory innervation from both the radial and median nerves. The ulnar proper digital nerve of the thumb typically originates from the median nerve, specifically from the first common palmar digital nerve, which then divides into the radial proper digital nerve of the index finger and the ulnar proper digital nerve of the thumb. Less commonly, it can be a branch of the ulnar nerve.
- Course: This nerve runs along the ulnar side of the thumb, superficial to the flexor pollicis longus tendon sheath, and deep to the skin and subcutaneous tissue. It provides sensation to the ulnar aspect of the thumb pulp and distal phalanx.
- Vulnerability: Its superficial course, particularly around the MCP joint and proximal phalanx, makes it susceptible to external compression and trauma.
- Variations: Anatomical variations in nerve branching patterns exist, which can influence the precise location of injury and clinical presentation.

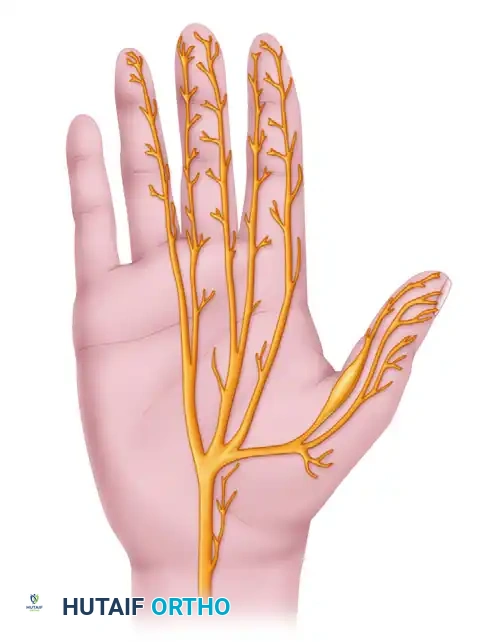
Figure 76-23: Distal sensory branches of the median nerve in the hand, illustrating the typical location of perineural fibrosis affecting the proper ulnar digital nerve of the thumb.
Biomechanics of Bowling and Nerve Compression
The act of bowling involves a complex sequence of movements, with the thumb playing a critical role in gripping and releasing the ball.
- Grip Phase: As the bowler grips the ball, the thumb is inserted into the thumbhole. The ulnar aspect of the thumb, particularly the skin and subcutaneous tissue overlying the ulnar proper digital nerve, is pressed against the edge of the thumbhole.
- Swing Phase: During the backswing and downswing, the thumb maintains its position, often under significant pressure, to control the ball.
- Release Phase: The most critical phase for nerve irritation. As the ball is released, the thumb is rapidly extracted from the thumbhole. This rapid withdrawal can cause shear forces and friction against the nerve, especially if the thumbhole is tight or has an irregular edge. Repeated cycles of compression, friction, and shear lead to chronic irritation.
Pathophysiology: Perineural Fibrosis
The repetitive microtrauma to the ulnar proper digital nerve of the thumb initiates an inflammatory response. This chronic inflammation leads to the proliferation of fibroblasts and collagen deposition around the nerve fascicles, resulting in perineural fibrosis. This fibrous tissue encases the nerve, causing:
- Mechanical Compression: The thickened fibrous sheath constricts the nerve, impairing axonal transport and blood supply.
- Increased Sensitivity: The fibrotic tissue itself can become a source of pain, and the compressed nerve becomes hypersensitive to mechanical stimuli.
- Neuroma Formation: In severe or prolonged cases, the nerve may develop a true traumatic neuroma, a disorganized proliferation of nerve tissue and scar, which is exquisitely tender.
This process is analogous to other entrapment neuropathies but is unique in its localized, external traumatic origin.
Clinical Presentation
Patients typically present with a characteristic set of symptoms and signs.
Symptoms
- Pain: Localized pain on the ulnar side of the thumb, often described as burning, aching, or sharp. Pain is exacerbated by bowling or activities involving similar thumb compression.
- Paresthesias: Tingling, numbness, or "pins and needles" sensation in the distribution of the ulnar proper digital nerve of the thumb, typically affecting the ulnar pulp and distal phalanx.
- Hyperesthesia/Dysesthesia: Increased sensitivity or abnormal, unpleasant sensations to light touch in the affected area.
- Weakness (Rare): Motor weakness is uncommon as this is a purely sensory nerve. However, severe pain may lead to grip weakness due to guarding.
Signs
- Palpable Mass: A key diagnostic finding is a palpable, firm, and exquisitely tender lump on the ulnar side of the thumb, usually at the level of the MCP joint or proximal phalanx. This lump represents the perineural fibrosis or neuroma.
- Tinel's Sign: Percussion over the palpable mass or along the course of the nerve typically elicits radiating pain or paresthesias distally into the thumb pulp.
- Skin Atrophy: In chronic, severe cases, distal skin atrophy or trophic changes may be observed in the affected sensory distribution, indicating prolonged nerve compromise.
- Sensory Deficit: Diminished light touch or two-point discrimination may be present in the ulnar pulp of the thumb.
Clinical Pearl: The presence of a palpable, tender mass combined with neuropathic symptoms in an active bowler is highly suggestive of Bowler's Thumb.
Differential Diagnosis
It is important to differentiate Bowler's Thumb from other conditions causing thumb pain or neuropathy.
- De Quervain's Tenosynovitis: Pain at the radial styloid, positive Finkelstein's test.
- Basal Thumb Arthritis (CMC Joint Arthritis): Pain at the base of the thumb, positive grind test, often associated with crepitus and deformity.
- Trigger Thumb: Pain and catching/locking of the thumb during flexion/extension, palpable nodule in the A1 pulley.
- Ganglion Cyst: Soft, mobile, non-tender mass, usually dorsal.
- Foreign Body Reaction: History of penetrating injury, localized inflammation.
- Other Neuropathies: More proximal nerve entrapments (e.g., carpal tunnel syndrome, pronator syndrome) would have a broader sensory distribution.
- Soft Tissue Tumors: Lipomas, fibromas, or other benign tumors can present as a mass, but typically lack the specific neuropathic symptoms and tenderness of Bowler's Thumb.
Diagnostic Workup
Diagnosis is primarily clinical, supported by imaging in equivocal cases.
Clinical Examination
- History: Detailed history of bowling frequency, technique, ball fit, and symptom onset/progression.
- Inspection: Look for skin changes, swelling, or atrophy.
- Palpation: Carefully palpate the ulnar aspect of the thumb for a tender mass.
- Neurological Examination: Assess sensation (light touch, two-point discrimination) and elicit Tinel's sign.
Imaging Studies
- Ultrasound (US): High-resolution ultrasound is an excellent non-invasive tool. It can visualize the thickened, hypoechoic perineural fibrosis or neuroma, differentiate it from other soft tissue masses, and assess its relationship to surrounding structures. Dynamic ultrasound during thumb movement can sometimes demonstrate nerve compression.
- Magnetic Resonance Imaging (MRI): MRI can provide detailed anatomical information, showing the nerve thickening and surrounding inflammatory changes. It is particularly useful for ruling out other soft tissue pathologies or if the diagnosis remains unclear after ultrasound.
- Nerve Conduction Studies (NCS) and Electromyography (EMG): While not routinely necessary for diagnosis, NCS may show slowed conduction velocity or reduced amplitude across the affected segment of the digital nerve, confirming axonal damage or demyelination. EMG is generally not indicated as it is a sensory nerve lesion.
Non-Operative Management
Conservative management is the first line of treatment, especially in early or mild cases. The goal is to reduce nerve irritation and allow for healing.
- Activity Modification and Rest:
- Cessation of Bowling: The most crucial step. Complete rest from bowling or any activity that exacerbates symptoms is essential.
- Modification of Bowling Technique: If returning to bowling, adjustments to grip, thumbhole size, and release technique are paramount. A larger, beveled thumbhole or a thumb insert (e.g., a "thumb slug") can reduce friction and pressure.
- Protective Measures:
- Padding/Shielding: Custom-molded thermoplastic splints or protective padding (e.g., silicone gel pads, moleskin) applied to the ulnar aspect of the thumb can cushion the nerve from direct pressure.
- Taping: Athletic tape can provide some protection and reduce skin friction.
- Anti-inflammatory Medications:
- NSAIDs: Oral non-steroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation.
- Topical Agents: Topical NSAID creams or patches may provide localized relief.
- Physical Therapy:
- Desensitization: Gentle massage and desensitization techniques for hyperesthetic areas.
- Nerve Glides: Exercises to promote nerve mobility, though their efficacy for localized perineural fibrosis is limited.
- Corticosteroid Injections:
- Indications: For persistent symptoms despite other conservative measures.
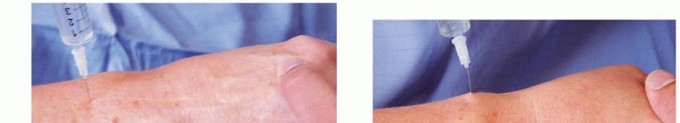
- Technique: A small volume of corticosteroid (e.g., triamcinolone) mixed with a local anesthetic can be injected carefully around (but not into) the nerve at the site of maximal tenderness.
- Caution: Repeated injections carry risks of skin atrophy, fat necrosis, and potential nerve injury. Ultrasound guidance is recommended to ensure accurate placement and avoid direct nerve injection.
Surgical Warning: Direct injection into the nerve can cause permanent damage. Always aspirate before injecting and consider ultrasound guidance.
Operative Management
Surgical intervention is considered for patients with persistent, debilitating symptoms despite a comprehensive trial of non-operative management (typically 3-6 months). The primary goal is to decompress the nerve and remove the fibrotic tissue.
Indications for Surgery
- Failure of conservative management for at least 3-6 months.
- Persistent, severe pain, paresthesias, or hyperesthesia significantly impacting daily activities or ability to bowl.
- Presence of a clearly defined, tender, palpable neuroma or extensive perineural fibrosis confirmed by imaging.
- Progressive neurological deficit (e.g., increasing sensory loss, trophic changes).
Contraindications
- Unwillingness or inability to comply with postoperative rehabilitation.
- Active infection in the surgical field.
- Uncontrolled systemic medical conditions that preclude safe surgery.
- Symptoms amenable to further conservative measures.
Preoperative Planning
- Detailed Clinical Assessment: Reconfirm diagnosis, localize the lesion precisely.
- Imaging Review: Review ultrasound or MRI to understand the extent of fibrosis and relationship to adjacent structures.
- Patient Counseling: Discuss realistic expectations, potential complications (e.g., persistent numbness, recurrence, scar tenderness), and the need for postoperative rehabilitation and activity modification.
- Anesthesia: Regional anesthesia (e.g., axillary block) or local anesthesia with sedation is typically preferred. A tourniquet is used for a bloodless field.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Arm Table: The affected arm is abducted and placed on a hand table, ensuring comfortable positioning for the surgeon and assistant.
- Tourniquet: A pneumatic tourniquet is applied to the upper arm.
Surgical Approach: Neurolysis and Dorsal Transfer
The surgical procedure involves careful exploration of the ulnar proper digital nerve of the thumb, neurolysis to release the nerve from the surrounding fibrosis, and potentially a dorsal transfer to reposition the nerve away from the area of compression.
Step-by-Step Surgical Technique
-
Incision:
- A longitudinal incision is made along the ulnar aspect of the thumb, centered over the palpable mass and the anticipated course of the ulnar proper digital nerve. The incision should be curvilinear or slightly zigzag to avoid contracture.
- The incision typically extends from the base of the proximal phalanx to just distal to the MCP joint.
-
Surgical Warning: Avoid placing the incision directly over the area of maximal pressure from the bowling ball, as this can lead to painful scar formation. A slightly more dorsal or palmar approach may be considered depending on the exact location of the neuroma.
-
Dissection:
- Careful dissection is performed through the subcutaneous tissue. The digital nerve is superficial in this area.
- Identify and protect the neurovascular bundle. The ulnar proper digital nerve of the thumb is typically found superficial to the flexor pollicis longus tendon sheath.
-
Clinical Pearl: Use loupe magnification (2.5x to 4.5x) for precise identification and protection of the delicate nerve structures.
-
Nerve Identification and Exposure:
- Once the nerve is identified, trace it proximally and distally to fully expose the extent of the perineural fibrosis or neuroma.
- The affected segment will appear thickened, firm, and often discolored compared to the normal nerve.
- The image provided illustrates the general course of the digital nerves in the hand, with a clear swelling on the ulnar digital nerve of the thumb, indicating the typical location of the pathology.

Figure 76-23: Distal sensory branches of the median nerve in the hand and location of perineural fibrosis of proper ulnar digital nerve of thumb are shown.
-
Neurolysis:
- Perform an external neurolysis, carefully incising and excising the dense fibrous tissue surrounding the nerve.
- The goal is to free the nerve completely from its constricting scar tissue, allowing it to glide freely.
- If a true neuroma-in-continuity is present, meticulous internal neurolysis (fascicular dissection) may be considered, but this carries a higher risk of nerve damage and is generally reserved for experienced surgeons.
-
Surgical Warning: Exercise extreme caution during neurolysis to avoid damaging the nerve fascicles. Use fine instruments and microsurgical techniques.
-
Dorsal Transfer of the Nerve (Optional but Recommended):
- After adequate neurolysis, the nerve is often mobilized and transposed dorsally. This repositions the nerve away from the high-pressure zone on the ulnar-palmar aspect of the thumb, where it was previously compressed by the bowling ball.
- Create a new, more dorsal subcutaneous bed for the nerve.
- Ensure the nerve lies in a tension-free position in its new bed. This step is crucial to prevent recurrence of compression.
-
Wound Closure:
- Achieve meticulous hemostasis.
- Close the subcutaneous tissue with fine absorbable sutures to minimize dead space.
- Close the skin with fine non-absorbable sutures (e.g., 5-0 or 6-0 nylon) or staples.
- Apply a small, dry, compression dressing.
Postoperative Protocol
Postoperative care is critical for optimal recovery and prevention of recurrence.
Immediate Postoperative Period (Days 0-7)
- Dressing: The compression dressing is typically removed after 48 hours.
- Elevation: Keep the hand elevated to minimize swelling.
- Pain Management: Oral analgesics as needed.
- Early Mobilization: Gentle active range of motion exercises for the thumb and fingers are encouraged to prevent stiffness, provided the nerve is protected. Avoid forceful gripping.
Early Rehabilitation (Weeks 1-6)
- Suture Removal: Sutures are removed at 10 to 14 days.
- Wound Care: Keep the incision clean and dry.
- Scar Management: Begin scar massage and desensitization techniques once the wound is healed to prevent hypersensitivity and adhesions. Silicone gel sheets can be beneficial.
- Gradual Mobilization: Continue gentle active and passive range of motion exercises for the thumb.
- Nerve Glides: Introduce gentle nerve gliding exercises to promote nerve mobility and prevent adhesions.
- Protection: Continue to protect the thumb from direct pressure or trauma. A custom-made protective splint may be used during activities.
Advanced Rehabilitation (Weeks 6-12+)
- Strengthening: Gradually introduce grip strengthening exercises.
- Functional Activities: Progress to light functional activities, avoiding repetitive thumb compression.
- Return to Sport:
- Return to bowling is highly individualized and should be gradual.
- Typically, patients can consider returning to bowling no earlier than 3 months post-surgery, and often longer.
- Crucially, the patient must address the underlying cause: ensure proper thumbhole fit, consider using a thumb insert, and modify bowling technique to minimize nerve irritation.
- A protective thumb shield or splint may be necessary during bowling activities.
Pitfall: Premature return to bowling or failure to address the causative biomechanical factors (e.g., ill-fitting thumbhole) significantly increases the risk of recurrence.
Potential Complications
While generally safe, surgical intervention for Bowler's Thumb carries potential risks:
- Persistent Symptoms: Incomplete neurolysis or severe, irreversible nerve damage can lead to ongoing pain, numbness, or hyperesthesia.
- Recurrence: If the nerve is not adequately decompressed or if the patient returns to the same causative activity without modification, fibrosis can recur.
- Scar Tenderness/Hypersensitivity: Incision site pain or hypersensitivity, especially if the scar is in a high-pressure area.
- Infection: As with any surgical procedure.
- Hematoma: Bleeding and blood collection under the skin.
- Nerve Damage: Direct injury to the nerve during dissection or neurolysis, leading to permanent sensory loss or neuroma formation.
- Stiffness: Adhesions or prolonged immobilization can lead to joint stiffness.
Prognosis
The prognosis for Bowler's Thumb following appropriate management is generally good, especially with early diagnosis and adherence to conservative measures. For those requiring surgery, neurolysis with dorsal nerve transfer typically provides significant relief of symptoms and allows for a return to activities, including bowling, provided the causative factors are addressed. Patient education regarding activity modification and protective measures is paramount for long-term success and prevention of recurrence.
You Might Also Like