Surgical Approach to the Median Nerve: Extensile Exposures, Techniques, and Clinical Outcomes
Key Takeaway
The surgical approach to the median nerve requires meticulous dissection through the arm, antecubital fossa, and forearm. By navigating critical anatomical landmarks such as the lacertus fibrosus and the pronator teres, surgeons can safely expose the nerve for repair or decompression. This guide details the extensile exposures, alternative Z-lengthening techniques, and critical timelines for delayed neurorrhaphy to optimize both motor and sensory recovery.
Introduction and Surgical Philosophy
The median nerve is often referred to as the "eye of the hand" due to its critical role in providing sensory innervation to the palmar aspect of the thumb, index, long, and radial half of the ring fingers. While motor recovery of the extrinsic flexors and intrinsic thenar musculature is paramount following nerve injury, a hand devoid of median nerve sensory supply is functionally severely compromised, lacking the stereognosis required for fine motor manipulation.
Approaching the median nerve requires a comprehensive understanding of its complex anatomical course from the brachial plexus down to the carpal tunnel. The surgical exposure must be extensile, allowing for proximal and distal extension without compromising the vascular supply to the nerve or creating debilitating flexion contractures across the antecubital fossa or wrist creases. This masterclass details the definitive surgical approaches to the median nerve, encompassing standard exposures, alternative Z-lengthening techniques for complex reconstructions, and the critical timelines governing delayed neurorrhaphy.
Applied Surgical Anatomy
A profound three-dimensional understanding of the median nerve's anatomical relationships is mandatory for safe surgical exploration.
The Arm
The median nerve is formed by the confluence of the medial and lateral cords of the brachial plexus. In the proximal arm, it lies lateral to the brachial artery within the neurovascular bundle.
Surgical Pearl: The median nerve gives off absolutely no motor or sensory branches in the upper arm. Any branches encountered in this region belong to the musculocutaneous or ulnar nerves, or represent high anatomical variants (e.g., Martin-Gruber anastomoses).
At the junction of the middle and distal thirds of the arm, the median nerve crosses to the medial side of the brachial artery. It usually courses posteriorly to the artery, although occasionally it may pass anteriorly.
The Elbow and Proximal Forearm
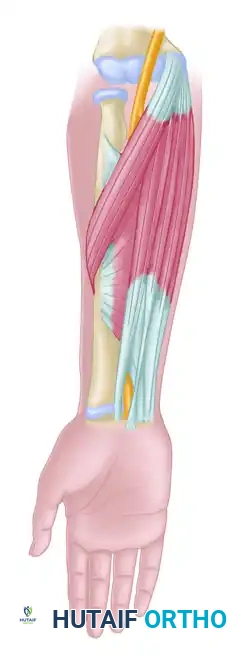
As the nerve approaches the elbow, it enters the antecubital fossa medial to the brachial artery and the biceps tendon. It passes beneath the lacertus fibrosus (bicipital aponeurosis), which forms a rigid fascial roof over the nerve.
Immediately distal to the lacertus fibrosus, the nerve dives between the superficial and deep heads of the pronator teres. It is in this region that the nerve begins to arborize:
* Pronator Teres: Usually receives two branches (one to the superficial head, one to the deep head).
* Flexor Carpi Radialis (FCR) & Palmaris Longus (PL): Receive several branches.
* Flexor Digitorum Sublimis (FDS) & Flexor Digitorum Profundus (FDP): Receive one primary branch each in the proximal forearm.
The Anterior Interosseous Nerve (AIN)
The AIN is a critical motor branch that emerges from the posteromedial aspect of the median nerve immediately after it passes through the two heads of the pronator teres. It courses distally along the interosseous membrane to supply:
1. Flexor pollicis longus (FPL)
2. The radial half of the flexor digitorum profundus (FDP to the index and long fingers)
3. Pronator quadratus
The Distal Forearm and Wrist
After exiting the pronator teres, the median nerve continues distally beneath the fascial arch of the flexor digitorum sublimis (FDS), resting on the epimysium of the flexor digitorum profundus (FDP). As it approaches the wrist, it becomes progressively more superficial. It emerges from beneath the FDS and lies directly beneath the tendon of the flexor carpi radialis (FCR). At the level of the proximal wrist crease, it is easily identified in the interval between the FCR and the palmaris longus tendons.
Preoperative Planning and Patient Positioning
- Positioning: The patient is placed supine with the operative upper extremity extended on a radiolucent hand table.
- Tourniquet: A sterile pneumatic tourniquet is applied high on the brachium. Exsanguination is performed with an Esmarch bandage, and the tourniquet is inflated to 250 mmHg (or 100 mmHg above systolic blood pressure).
- Magnification: Loupe magnification (3.5x to 4.5x) is standard for the approach, while an operating microscope is required for interfascicular neurolysis or neurorrhaphy.
- Instrumentation: A standard orthopedic soft tissue tray, supplemented with micro-instruments (jeweler's forceps, micro-scissors, vessel loops) and a nerve stimulator.
Surgical Approach to the Median Nerve
The exposure of the median nerve can be tailored to the specific zone of injury, but the incision is designed to be fully extensile from the axilla to the palm.
1. Incision and Superficial Dissection
To expose the median nerve in the arm and at the elbow, utilize the same fundamental approach as that for the ulnar nerve, but modify the trajectory to avoid crossing the flexion creases of the antecubital fossa perpendicularly.
- Arm: Begin the incision along the medial border of the biceps brachii.
- Elbow: As the incision reaches the medial epicondyle, curve it obliquely across the volar aspect of the forearm. Never cross the antecubital crease at a right angle, as this will inevitably lead to a hypertrophic scar and a severe flexion contracture.
- Forearm: Continue the incision distally over the anatomical course of the nerve.
- Wrist: In approaching the wrist, curve the incision toward the radial side.
- Note: If simultaneous exploration of both the median and ulnar nerves is indicated, curve the incision toward the ulnar side instead.
- Hand: As the flexor creases of the wrist are reached, return the incision along one of the creases to the midline of the wrist. If the nerve must be explored distal to the carpal tunnel, extend the incision distally along the thenar crease, avoiding the palmar cutaneous branch of the median nerve.
2. Deep Dissection in the Arm
Deepen the incision through the subcutaneous tissue and superficial fascia. To accomplish adequate exposure at the elbow, undermine the skin flaps widely.
In the arm, identify the medial intermuscular septum. Retract the brachial artery and its accompanying venae comitantes medially. The median nerve will be exposed on the lateral aspect of the neurovascular bundle in the proximal arm, crossing to the medial side as it descends toward the elbow. Use vessel loops to gently mobilize the nerve, preserving its segmental vasa nervorum.
3. Deep Dissection at the Elbow (Technique 62-19)
At the elbow, the nerve is tethered by the lacertus fibrosus.
- Expose the nerve by sharply incising the transverse fibers of the lacertus fibrosus at its attachment to the deep fascia over the pronator-flexor muscle group.
- Dissect the fascia radially from this group of muscles.
- Incise the fascia distally and radially along the proximal border of the pronator teres.
- Continue the fascial incision distally across the pronator teres muscle belly and along the medial side of the flexor carpi radialis.
- The pronator teres can now be widely mobilized and separated from the FCR. This permits easy exposure of the nerve as it dives between the pronator heads and significantly facilitates tension-free closure later.
4. Deep Dissection in the Forearm
Expose the nerve where it emerges from beneath the fibrous arch of the flexor digitorum sublimis.
To trace the nerve proximally into the deep forearm:
1. Retract the flexor carpi radialis laterally.
2. Retract the pronator teres proximally and medially.
3. Carefully separate the muscle fibers of the flexor digitorum sublimis.
4. By sequentially retracting these structures, the median nerve can be exposed over its entire course through the middle third of the forearm.
Surgical Warning: When dissecting the nerve as it exits the pronator teres, exercise extreme caution to identify and protect the Anterior Interosseous Nerve (AIN), which branches posteromedially. Iatrogenic injury to the AIN will result in devastating loss of thumb interphalangeal and index distal interphalangeal joint flexion.
Alternative Exposure: The Z-Lengthening Technique
In cases of severe trauma, extensive scarring, or when a massive neuroma requires resection and grafting, the standard retraction of the pronator teres and FDS may not provide sufficient visualization. In these complex scenarios, an alternative, highly extensile method is required.
Instead of merely retracting the muscles, the surgeon can systematically divide them to open the forearm like a book.
- Identify the radial origin of the flexor digitorum sublimis. Cut this origin in line with the course of the median nerve.
- Identify the insertion of the pronator teres on the lateral radius. Sever the pronator teres using a formal Z-shaped incision near its tendinous insertion.
- This Z-lengthening allows for massive exposure of the deep forearm and permits anatomical repair of the muscle during closure without excessive tension.

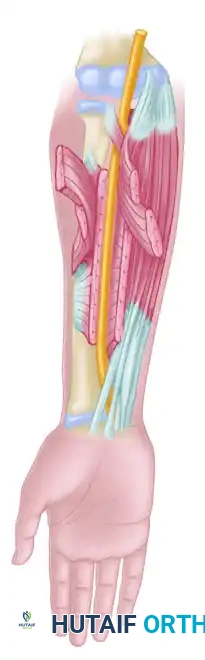
Figure: Alternative method of exposing the median nerve throughout the forearm. Note the Z-incision through the pronator teres, the incision through the radial origin of the flexor digitorum sublimis, and the exposure of the deep ulnar head of the pronator teres relative to the median nerve.
Nerve Transposition
If a large gap is present following neuroma resection, transposition of the median nerve may be required to gain length for a tension-free neurorrhaphy. Dissection of the deep ulnar head of the pronator teres and the strategic placement of the flexor carpi radialis deep to the median nerve may make mobilization and transposition of the nerve to a more superficial, subcutaneous position easier, effectively shortening its anatomical path across the elbow joint.
Postoperative Care and Rehabilitation
Postoperative management is dictated by the nature of the nerve repair. If a primary neurorrhaphy or interfascicular grafting was performed:
* Immobilization: The limb is immobilized in a long-arm posterior splint. The elbow is placed in 90 degrees of flexion, and the wrist is placed in neutral to slight flexion (20 degrees) to minimize tension on the repair site.
* Duration: Absolute immobilization is maintained for 3 to 4 weeks to allow for initial axonal crossing of the repair site.
* Mobilization: After 4 weeks, the splint is transitioned to a hinged brace, and a graduated active range of motion protocol is initiated. Extension is increased by 10 to 15 degrees per week.
* Sensory Re-education: Once advancing Tinel's signs reach the palm, formal sensory re-education programs are initiated by occupational therapy to maximize cortical remapping and stereognosis.
Clinical Outcomes of Median Nerve Suture
The prognosis following median nerve repair is highly dependent on the patient's age, the mechanism of injury, the level of the lesion, and the delay to surgery.
Motor recovery is undeniably crucial; however, it must be reiterated that a hand without median nerve sensory supply is almost useless. Even with the best possible sensory recovery, the patient will likely experience some permanent difficulty with fine stereognosis.
Statistical Outcomes Under Favorable Circumstances:
* Sensory Recovery: Approximately 50% of patients undergoing median nerve suture recover sensitivity to pain and touch, alongside some functional degree of stereognosis.
* Extrinsic Motor Recovery: About 90% of patients recover a useful degree of motor function in the long flexors of the forearm (FPL, FDP, FDS).
* Intrinsic Motor Recovery (High Lesions): When the lesion is in the upper arm, a much smaller number—perhaps one-third (33%)—obtain useful recovery in the thenar intrinsic muscles.
* Intrinsic Motor Recovery (Low Lesions): In more distal lesions (e.g., wrist level), about two-thirds (66%) attain useful thenar motor recovery.
* Overall Success Rates: Modern microsurgical literature reports between 82% and 90% good-to-fair motor recovery, and up to 97% protective sensory recovery after primary repair or interfascicular grafting.
The Critical Limit of Delay for Neurorrhaphy
Time is muscle, and in the context of peripheral nerve surgery, time is also the survival of the motor endplate. The timing of surgical intervention is the single most critical modifiable factor in median nerve reconstruction.
Motor Recovery Limits
Motor recovery in the intrinsic muscles of the hand generally does not occur if nerve suture is delayed beyond:
* 9 months in high lesions (arm/proximal elbow).
* 12 months in low lesions (distal forearm/wrist).
Zachary's landmark studies established strict parameters for expected motor return. He found that useful motor recovery cannot be expected after delays of:
* 9 months in lesions above the pronator teres.
* 32 months in lesions below the flexor pollicis longus.
Sensory Recovery Limits
Sensory end-organs (Meissner's and Pacinian corpuscles) are slightly more resilient to prolonged denervation than motor endplates, but they still possess a definitive biological clock.
* Useful sensory recovery only rarely occurs after 9 months in high lesions or 12 months in low ones.
* However, in exceptional cases, protective sensation may occur even when suture has been delayed up to 2 years.
* Zachary's Sensory Limits (Adults): The critical period of delay for sensory return in adults seems to be 12 months in lesions above the pronator teres, or 9 months in lesions below the flexor pollicis longus.
* Pediatric Exception: Sensory return in children is significantly more robust and is possible after much longer delays due to enhanced neuroplasticity.
Clinical Pitfall: Inasmuch as sensory recovery is absolutely vital for hand function, a second operation (such as exploration, neurolysis, or revision grafting) may be strictly indicated if sensation does not return at the expected time based on the calculated rate of axonal regeneration (1 mm/day). Revision surgery is often the only way that protective sensation can ultimately be regained if the primary repair fails.
You Might Also Like

