Operative Management of Mammalian Bite Injuries to the Hand and Upper Extremity
Key Takeaway
Mammalian bite injuries to the hand, particularly human clenched-fist injuries, represent surgical emergencies due to the high risk of deep space infection, septic arthritis, and osteomyelitis. Successful management dictates a high index of suspicion, meticulous surgical debridement, copious irrigation, and targeted antimicrobial therapy. This guide details the pathoanatomy, microbiology, and step-by-step operative protocols required to prevent devastating functional morbidity following human, canine, and feline bite wounds.
INTRODUCTION TO MAMMALIAN BITE INJURIES
Mammalian bite injuries to the hand and upper extremity are common clinical entities that possess a disproportionately high potential for devastating functional morbidity. The unique anatomy of the hand—characterized by superficial joints, delicate extensor mechanisms, and complex synovial sheaths—renders it exceptionally vulnerable to deep space infections following penetrating trauma.
Bite wounds are inherently contaminated with complex, polymicrobial oral flora. When these organisms are inoculated into the relatively avascular spaces of the hand (such as joint capsules or tendon sheaths), rapid bacterial proliferation ensues. The management of these injuries requires a rigorous, evidence-based approach, combining prompt surgical intervention, meticulous debridement, and targeted antimicrobial therapy. This comprehensive guide delineates the pathoanatomy, microbiology, and operative management of human, canine, and feline bite injuries.
HUMAN BITE INJURIES
Human bite injuries are generally categorized into two distinct mechanisms: inadvertent (accidental) bites and intentional (violent) strikes.
- Inadvertent Bites: These are relatively innocent injuries involving nail-biting, accidental dental contact during sports, or minor occupational exposures (e.g., dental professionals). They typically present as superficial abrasions or minor lacerations.
- Intentional Bites and Clenched-Fist Injuries (CFIs): Often referred to as "fight bites," these occur when a closed fist strikes an opponent's tooth. This mechanism accounts for the majority of severe human bite infections. Other intentional injuries include full-thickness bite amputations (e.g., of digits or ears) sustained during violent altercations.
Pathoanatomy and Biomechanics of the Clenched-Fist Injury
The clenched-fist injury (CFI) is the most treacherous of all mammalian bites. The injury typically occurs over the metacarpophalangeal (MCP) joint—most commonly the third or fourth digit.
CLINICAL PEARL: The biomechanics of the CFI dictate its pathophysiology. At the moment of impact, the MCP joint is in maximal flexion. The opponent's tooth penetrates the skin, the stretched extensor tendon (or sagittal band), and the dorsal joint capsule, inoculating the articular space with oral flora. When the patient subsequently extends the fingers, the tissue layers glide proximally and distally, misaligning the puncture tracts. This creates a one-way valve that seals the virulent bacteria within the joint space, creating an anaerobic environment primed for rapid sepsis.
Microbiology of Human Bites
Human saliva contains over 600 species of bacteria, with concentrations reaching $10^8$ organisms per milliliter. Infections are almost universally polymicrobial, involving both aerobes and anaerobes.
* Eikenella corrodens: A fastidious, gram-negative, facultative anaerobe present in up to 30% of human bite infections. It acts synergistically with other organisms to cause severe tissue destruction. Crucially, E. corrodens is typically resistant to first-generation cephalosporins, macrolides, and clindamycin.
* Staphylococcus aureus: The most common gram-positive aerobe isolated.
* Streptococcus species: Including S. viridans and S. pyogenes.
* Anaerobes: Peptostreptococcus, Bacteroides, and Fusobacterium species.
Clinical Evaluation
Patients with CFIs often provide a deceptive history due to embarrassment or legal concerns, attributing the wound to a fall or a crush injury. Any laceration over the dorsal MCP joint must be treated as a human bite until proven otherwise.
- Physical Examination: Assess for erythema, edema, purulent drainage, and lymphangitis. Evaluate the extensor mechanism for lag. Crucially, examine the wound with the patient's hand in the exact position of injury (full fist flexion) to visualize the true extent of the capsular penetration.
- Radiographic Evaluation: Standard posteroanterior, lateral, and oblique radiographs of the hand are mandatory. The surgeon must actively rule out metacarpal neck/head fractures, cortical violations, and retained foreign bodies (e.g., radiopaque tooth fragments).
Surgical Management and Indications
The timing of presentation dictates the clinical approach.
Early Presentation (< 24 Hours)
Patients presenting within 24 hours of injury typically do not exhibit overt signs of sepsis. However, conservative management is fraught with peril.
* Protocol: Formal joint exploration, swabbing for aerobic and anaerobic cultures (with specific requests to the laboratory to isolate E. corrodens), thorough irrigation, and prophylactic antibiotic therapy.
* Disposition: While some surgeons advocate for mandatory hospital admission for all human bites, reliable patients with early, uninfected wounds may be managed with aggressive emergency department debridement, intravenous antibiotics, and close outpatient observation (24-hour follow-up).
Delayed Presentation (> 24 Hours)
Patients presenting after 24 hours frequently exhibit established septic arthritis, tenosynovitis, or deep space abscesses.
* Protocol: These patients require emergent operative intervention in the operating room. Open joint drainage, extensive debridement, and copious irrigation are mandatory.
* Disposition: Hospital admission for continuous intravenous antibiotic therapy and elevation is required.
Operative Technique: The Clenched-Fist Injury
- Anesthesia and Positioning: The procedure is performed under regional anesthesia (brachial plexus block) or general anesthesia. A proximal arm tourniquet is utilized to ensure a bloodless field.
- Incision and Exposure: Do not rely on the traumatic puncture wound. Extend the wound longitudinally or via a lazy-S incision over the involved MCP joint.
- Tendon Inspection: Retract the skin flaps. Inspect the extensor tendon. The finger must be passively flexed to recreate the position of injury, bringing the tendon laceration into view.
- Arthrotomy and Debridement: If the joint capsule is violated, extend the arthrotomy longitudinally. Excise all necrotic, macerated, and devitalized tissue. Remove any retained tooth fragments or foreign debris.
- Irrigation: Perform high-volume, low-pressure irrigation of the joint space and tendon sheath using a minimum of 3 liters of normal saline.
- Wound Closure: Never primarily close a human bite wound. The joint capsule, extensor tendon, and skin must be left open to allow for continuous drainage and secondary healing (or delayed primary closure).
- Dressing: Apply a non-adherent dressing and a bulky soft tissue dressing. Splint the hand in the "safe position" (intrinsic-plus: wrist extended 20-30 degrees, MCP joints flexed 70-90 degrees, IP joints fully extended).
Postoperative Protocol and Antimicrobial Therapy
- Rehabilitation: If healing progresses satisfactorily and the infection is clinically controlled, active range-of-motion (ROM) exercises should be initiated 24 to 48 hours post-drainage to prevent extensor tendon adhesions and joint stiffness. Daily washing of the wound with soap and water provides sufficient mechanical cleansing.
- Comorbidities: Patients with diabetes mellitus, peripheral vascular disease, or those on systemic corticosteroids will experience prolonged healing and are at a higher risk for complications (osteomyelitis, amputation).
- Antibiotic Regimens: Empiric therapy must cover S. aureus, Streptococcus, anaerobes, and E. corrodens.
- First-line IV: Ampicillin-sulbactam or Cefoxitin. (Historically, Penicillin G, ampicillin, or carbenicillin were used for E. corrodens, combined with a cephalosporin for Staphylococcus. Today, beta-lactamase inhibitor combinations are preferred due to rising penicillin resistance).
- Penicillin-allergic: Doxycycline or a fluoroquinolone (e.g., ciprofloxacin) combined with metronidazole or clindamycin.
- Duration: Antibiotics are typically continued for 7 to 10 days, guided by the clinical course and tailored at 36 to 48 hours based on definitive culture and sensitivity results.
- Tetanus: Ensure tetanus prophylaxis is up to date.
CANINE (DOG) BITE INJURIES
Dog bites account for approximately 80% to 90% of all animal bites. The canine jaw can exert pressures exceeding 400 pounds per square inch (psi), resulting in a combination of puncture wounds, deep lacerations, severe crush injuries, and tissue avulsions.
Microbiology of Dog Bites
The oral flora of canines is highly diverse. Key pathogens include:
* Pasteurella multocida: Isolated in up to 50% of dog bites. It is a gram-negative coccobacillus that causes rapid, intense inflammatory responses.
* Staphylococcus aureus and Streptococcus viridans: Common aerobic isolates.
* Bacteroides species: Common anaerobic isolates.
* Capnocytophaga canimorsus: A fastidious gram-negative rod that can cause overwhelming, fatal sepsis, disseminated intravascular coagulation (DIC), and purpura fulminans, particularly in patients who are asplenic, cirrhotic, or immunocompromised.
SURGICAL WARNING: Most canine oral pathogens, including P. multocida, are highly sensitive to penicillin and ampicillin. However, P. multocida is intrinsically resistant to first-generation cephalosporins (e.g., cephalexin) and clindamycin. Prescribing cephalexin for a dog bite is a common and dangerous clinical error.
Surgical Management of Dog Bites
The management strategy depends heavily on the depth and severity of the tissue injury.
- Deep Wounds and Crush Injuries:
- These injuries require formal surgical exploration in the operating room.
- Aggressive debridement of devitalized muscle, fat, and skin margins is critical, as the crush component creates a necrotic nidus for infection.
- The wound must be irrigated with copious amounts of normal saline.
- Closure: Deep, heavily contaminated, or crush-type dog bites must be left open for secondary intention healing or delayed primary closure.
- Superficial Lacerations:
- More superficial lacerations without underlying crush injury or dead space can be managed in the emergency department.
- Following thorough mechanical cleansing, sharp debridement of the wound margins, and high-volume irrigation, these wounds may be loosely closed (approximated without tension) to optimize cosmetic outcomes, provided the patient presents early and has no signs of infection.
- Prophylaxis: Tetanus prophylaxis is mandatory. Rabies post-exposure prophylaxis (PEP) must be considered based on the vaccination status of the animal and local epidemiological guidelines.
- Antibiotics: Amoxicillin-clavulanate is the oral agent of choice for outpatient management. Intravenous ampicillin-sulbactam is utilized for admitted patients.
FELINE (CAT) BITE INJURIES
While cat bites account for only 5% to 15% of animal bites, they carry the highest rate of infection (up to 50%-80%). The mechanism of injury involves sharp, slender, needle-like teeth that easily penetrate deep into joints, periosteum, and flexor tendon sheaths, leaving a deceptively small puncture wound that rapidly seals over.
Microbiology of Cat Bites
- Pasteurella multocida: This is the hallmark pathogen of feline bites, isolated in 70% to 80% of cases.
- Infections with P. multocida are characterized by an exceptionally rapid onset. Patients often develop severe pain, swelling, and erythema within 12 to 24 hours of the bite.
Surgical Management of Cat Bites
Because cat bites frequently penetrate deep synovial spaces, they carry a high risk of purulent flexor tenosynovitis and septic arthritis.
- Minor/Superficial Bites: If the bite is definitively superficial (e.g., a scratch or shallow puncture not overlying a joint or tendon sheath), treatment includes aggressive local cleansing, oral antibiotics (Amoxicillin-clavulanate), and strict observation.
- Deep Puncture Wounds:
- Deep cat bites to the hand must never be ignored or primarily closed.
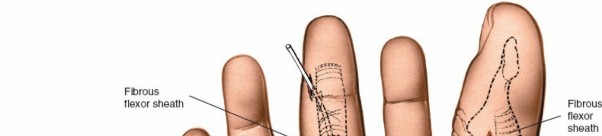
- Operative Technique: The puncture wounds should be connected using a scalpel blade (e.g., a #15 blade) to open the tract completely. This allows for direct visualization, thorough surgical debridement of the inoculated tract, and high-volume irrigation.
- Closure: Severe, deep wounds are strictly left open to drain. Only highly superficial, thoroughly debrided wounds in non-critical areas may be loosely approximated.
- Prophylaxis: As with dog bites, tetanus and rabies prophylaxis must be addressed immediately.
COMPLICATIONS AND PROGNOSIS
Failure to adhere to the strict surgical principles outlined above can lead to catastrophic complications, including:
* Septic Arthritis: Leading to rapid chondrolysis and irreversible joint destruction.
* Osteomyelitis: Particularly common in cat bites where the tooth penetrates the periosteum, or in neglected human bites.
* Tendon Rupture: Secondary to purulent tenosynovitis and enzymatic degradation of the collagen matrix.
* Amputation: In cases of overwhelming sepsis, necrotizing fasciitis, or gangrene, particularly in diabetic or immunocompromised hosts.
The cornerstone of preventing these outcomes remains early recognition, aggressive surgical debridement, avoidance of primary closure in contaminated wounds, and the rational application of culture-directed antimicrobial therapy.
You Might Also Like