Master the Hip Anterolateral Approach: Techniques & Key Uses
Key Takeaway
Learn more about Master the Hip Anterolateral Approach: Techniques & Key Uses and how to manage it. The hip anterolateral approach is a surgical technique commonly used for total joint replacements and other hip procedures. It exploits the intermuscular plane between the tensor fasciae latae and gluteus medius. This approach often involves partial or complete detachment of the abductor mechanism, providing excellent exposure of the acetabulum and safety during femoral shaft reaming.
Introduction and Epidemiology
The anterolateral approach to the hip remains one of the most foundational and versatile surgical exposures in orthopedic surgery. Originally popularized by Watson-Jones for the open reduction and internal fixation of proximal femur fractures, the approach was subsequently modified by Charnley, Harris, Hardinge, and Müller to accommodate the evolving demands of total joint arthroplasty. This approach combines excellent, direct visualization of the acetabulum with a safe, reproducible trajectory for the reaming and preparation of the femoral shaft.
In contemporary orthopedic practice, the anterolateral approach is predominantly utilized for primary total hip arthroplasty (THA), hemiarthroplasty for displaced femoral neck fractures, and the surgical management of specific synovial or osseous pathologies requiring biopsy. Epidemiologically, while the posterior approach has gained immense popularity due to its preservation of the abductor mechanism, the anterolateral approach remains highly favored in various global regions, particularly throughout Europe. Its enduring relevance is largely attributed to its inherently low postoperative dislocation rate. By preserving the posterior capsule and short external rotators, the anterolateral approach provides substantial posterior stability, making it an excellent choice for non-compliant patients or those with neuromuscular disorders.
The fundamental principle of all variations of the anterolateral approach is the exploitation of the intermuscular plane between the tensor fasciae latae (TFL) anteriorly and the gluteus medius posteriorly. Depending on the specific modification employed, the approach involves either a partial or complete detachment of the abductor mechanism—via soft tissue release or trochanteric osteotomy—to facilitate the necessary adduction and external rotation required for femoral preparation.
Historical Context and Evolution
The evolution of the anterolateral approach reflects the broader history of hip arthroplasty and reconstructive surgery. The classic Watson-Jones approach utilized the interval between the TFL and the gluteus medius without formally detaching the abductors, relying instead on vigorous retraction. However, as the requirements for extensive acetabular and femoral preparation grew with the advent of modern THA, retraction alone proved insufficient and led to iatrogenic muscle necrosis. Hardinge subsequently introduced the direct lateral transgluteal approach, frequently categorized within the anterolateral family, which involves splitting the anterior third of the gluteus medius and minimus in continuity with the vastus lateralis. This modification provided unparalleled exposure of the acetabulum while maintaining the continuity of the tendinous repair.
Current Epidemiological Trends
Global joint registry data indicate that approach selection is highly regionalized. Scandinavian and certain Central European registries report the anterolateral and direct lateral approaches as the most frequently utilized exposures for primary THA. Conversely, the posterior approach dominates in North America and the United Kingdom. The incidence of dislocation following the anterolateral approach is consistently reported in the literature as ranging from 0.4% to 1.2%, which is statistically lower than the historical dislocation rates of the posterior approach prior to the widespread adoption of meticulous posterior capsular repair techniques.
Surgical Anatomy and Biomechanics
A profound understanding of the osteology, myology, and neurovascular topography of the lateral hip is mandatory for the safe execution of the anterolateral approach.
Osteology and Superficial Landmarks
The primary osseous landmarks guiding the incision and dissection are the anterior superior iliac spine (ASIS) and the greater trochanter of the femur. The ASIS serves as the origin for the sartorius muscle and the inguinal ligament, while the greater trochanter serves as the critical insertion site for the abductor complex (gluteus medius and minimus). The shaft of the femur can be palpated distally beneath the vastus lateralis fascia.
The greater trochanter is a complex, multi-faceted structure. The lateral facet serves as the primary insertion for the gluteus medius, while the anterior facet accommodates the gluteus minimus. The vastus ridge marks the inferior border of the trochanter and the origin of the vastus lateralis. Understanding these facets is critical when performing a transgluteal split or a trochanteric osteotomy, as the repair must anatomically restore these insertions to maintain abductor tension.
Myology and The Intermuscular Plane
The classic Watson-Jones anterolateral approach utilizes the interval between the TFL and the gluteus medius. It is critical to note that this is an intermuscular plane, not a true internervous plane, as both the TFL and the gluteus medius are innervated by the superior gluteal nerve. Consequently, aggressive retraction or proximal extension of this interval places the terminal branches of the superior gluteal nerve at significant risk.
The tensor fasciae latae originates from the anterior aspect of the iliac crest and the ASIS, inserting into the iliotibial band. The gluteus medius originates from the external surface of the ilium between the anterior and posterior gluteal lines. Developing the plane between these two muscles requires careful sharp and blunt dissection, as the fascial covering blends proximally.
The Abductor Mechanism Biomechanics
The abductor mechanism is the primary dynamic stabilizer of the pelvis during the single-leg stance phase of gait. The gluteus medius originates from the outer surface of the ilium and inserts onto the lateral and superoposterior facets of the greater trochanter.
Biomechanically, the hip operates as a class I lever system. The center of rotation is the femoral head. The body weight exerts a downward force medial to the center of rotation, creating an adduction moment. The abductor musculature exerts a counteracting force lateral to the center of rotation, creating an abduction moment. The ratio of the lever arms (abductor lever arm vs. body weight lever arm) is typically 1 to 2.5 or 1 to 3. Therefore, the abductors must generate a force approximately three times body weight to maintain a level pelvis during single-leg stance. Any surgical approach that compromises the abductor insertion, either through failed repair or denervation, drastically reduces this force generation, resulting in a Trendelenburg gait and dramatically increased joint reaction forces.
Neurovascular Topography
The superior gluteal nerve (SGN) is the most critical neurological structure at risk during the anterolateral approach. It exits the pelvis through the greater sciatic foramen above the piriformis muscle and courses anteriorly between the gluteus medius and minimus, supplying both, before terminating in the TFL. The nerve typically lies 3 to 5 centimeters proximal to the tip of the greater trochanter. Proximal extension of the intermuscular split beyond this "safe zone" risks denervating the anterior portion of the gluteus medius and the entire TFL.
Vascularly, the ascending branch of the lateral femoral circumflex artery (LFCA) crosses the distal portion of the intermuscular interval. This vessel must be routinely identified, ligated, or cauterized to prevent significant postoperative hematoma formation.
Indications and Contraindications
The anterolateral approach is highly versatile but must be selected based on patient-specific pathology, surgeon familiarity, and the reconstructive goals.
Primary Indications for Anterolateral Exposure
The approach is primarily indicated for primary total hip arthroplasty in patients with osteoarthritis, rheumatoid arthritis, or avascular necrosis. It is particularly advantageous for patients at high risk for postoperative dislocation, such as those with cognitive impairment, Parkinson's disease, cerebral palsy, or a history of recurrent posterior instability. Furthermore, it is the approach of choice for hemiarthroplasty in the setting of displaced femoral neck fractures, as the preservation of the posterior soft tissue envelope minimizes the risk of dislocation in a patient population that frequently struggles with postoperative hip precautions.
Other indications include synovial biopsy, management of benign osseous lesions of the femoral neck, and certain extra-articular procedures such as core decompression for early-stage osteonecrosis.
Relative and Absolute Contraindications
Contraindications are largely relative and depend on the extent of exposure required. Complex revision arthroplasty requiring extensive posterior column exposure, placement of posterior column plates, or removal of well-fixed long femoral stems may be exceedingly difficult through a standard anterolateral window. In such scenarios, an extensile posterior approach or an extended trochanteric osteotomy is preferred. Additionally, patients with pre-existing abductor deficiency or a history of multiple lateral hip surgeries with compromised musculature may benefit from an alternative approach to avoid further insult to the abductor mechanism.
| Clinical Scenario | Operative Management via Anterolateral Approach | Non Operative or Alternative Approach |
|---|---|---|
| Primary Osteoarthritis | Excellent choice; provides stable THA with low dislocation risk. | Conservative management until end-stage; alternative approaches (Posterior, Direct Anterior) based on surgeon preference. |
| Displaced Femoral Neck Fracture | Preferred for hemiarthroplasty/THA in elderly/non-compliant patients due to posterior stability. | Non-operative only if patient is non-ambulatory or medically unfit for anesthesia. |
| High Dislocation Risk Patients | Strongly indicated (e.g., neuromuscular disorders, cognitive decline). | Posterior approach relatively contraindicated unless utilizing dual-mobility components. |
| Complex Acetabular Revision | Relative contraindication; limits access to the posterior column and ischium. | Extensile posterior approach or ilioinguinal approach depending on defect location. |
| Pre existing Abductor Tear | Relative contraindication; further compromise of the gluteus medius can worsen limp. | Posterior approach or Direct Anterior approach to preserve remaining abductor integrity. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning and meticulous patient positioning are fundamental to achieving optimal component alignment, restoring leg length, and minimizing intraoperative complications.
Templating and Imaging Modalities
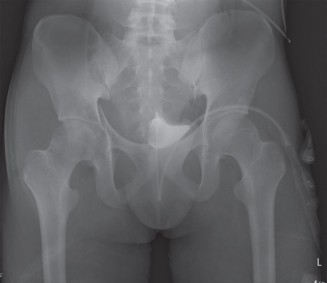
Standard preoperative imaging includes an anteroposterior (AP) radiograph of the pelvis and a cross-table lateral view of the affected hip. Digital templating is utilized to determine the approximate size of the acetabular and femoral components, the center of rotation, the necessary offset, and the expected leg length discrepancy.
When utilizing the anterolateral approach, restoring femoral offset is particularly critical. Inadequate offset leads to laxity of the abductor mechanism, which, combined with the surgical trauma of the approach, drastically increases the risk of a postoperative Trendelenburg gait.
Patient Positioning and Operating Room Setup
The anterolateral approach can be performed with the patient in either the lateral decubitus or the supine position. The lateral decubitus position is most commonly employed, as it allows gravity to assist in retracting the soft tissues and provides excellent visualization of the acetabulum.
The patient is placed on the operating table in the true lateral position. Pelvic positioners, such as a pegboard or a specialized beanbag, are utilized to secure the pelvis. The anterior support is placed at the level of the pubic symphysis, and the posterior support is placed at the sacrum. It is imperative to ensure that the pelvis is strictly perpendicular to the floor to prevent errors in acetabular cup positioning; excessive anterior tilt can lead to retroversion of the cup, while posterior tilt can lead to excessive anteversion.
The operative leg must be draped free to allow for full manipulation, including flexion, adduction, and external rotation, which are required for femoral dislocation and preparation. A sterile Mayo stand or a dedicated leg holder can be utilized to support the leg during the procedure.
Detailed Surgical Approach and Technique
The surgical execution of the anterolateral approach requires precision in tissue handling to preserve the abductor mechanism and the superior gluteal neurovascular bundle.
Incision and Superficial Dissection
The skin incision is centered over the greater trochanter. It begins approximately 2 to 3 centimeters posterior to the ASIS, curving distally over the anterior half of the greater trochanter, and extending longitudinally down the axis of the femoral shaft for approximately 5 to 7 centimeters.
Subcutaneous tissues are divided in line with the incision down to the fascia lata. Hemostasis is achieved using electrocautery. The fascia lata is incised longitudinally directly over the center of the greater trochanter. Proximally, the fascial incision is directed slightly anteriorly, following the interval between the tensor fasciae latae and the gluteus maximus. Distally, the incision splits the iliotibial band.
Deep Dissection and Interval Development
Once the fascia lata is incised, Charnley or self-retaining retractors are placed to expose the underlying musculature. The interval between the TFL anteriorly and the gluteus medius posteriorly is identified. This interval is often marked by a fat stripe and small perforating vessels.
Blunt dissection is utilized to separate the TFL from the gluteus medius. As the dissection proceeds proximally, extreme caution must be exercised to avoid stretching or transecting the superior gluteal nerve, which crosses the field approximately 3 to 5 centimeters proximal to the trochanteric tip. Distally, the vastus lateralis is identified originating from the vastus ridge.
In the modified Hardinge (transgluteal) approach, rather than solely retracting the muscles, an incision is made through the anterior third of the gluteus medius tendon, continuing distally through the gluteus minimus and into the vastus lateralis. This creates a continuous musculotendinous flap that is reflected anteriorly. The split in the gluteus medius must not extend more than 3 to 4 centimeters proximal to the tip of the greater trochanter to protect the superior gluteal nerve.
Capsulotomy and Hip Dislocation
Deep to the abductor musculature, the precapsular fat is excised to expose the anterior hip capsule. The reflected head of the rectus femoris may be identified and released if it impedes capsular exposure.
A capsulotomy is performed based on surgeon preference, typically an H-shaped, T-shaped, or Z-shaped incision. The anterior capsule is robust and requires a strong release to allow for dislocation. The capsular flaps are tagged with heavy non-absorbable sutures to facilitate later repair.
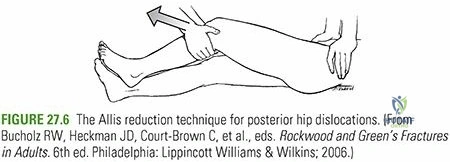
Dislocation of the hip is achieved by placing the leg in a position of external rotation, extension, and adduction. A bone hook may be placed around the femoral neck to assist in delivering the femoral head out of the acetabulum. If the hip is severely stiff or protrusio is present, an in situ femoral neck osteotomy should be performed prior to dislocation to prevent iatrogenic fracture of the femur or acetabulum.
Acetabular Exposure and Preparation
Once the femoral head is removed, retractors are positioned to provide a 360-degree view of the acetabulum. A blunt Hohmann retractor is placed over the anterior column, carefully avoiding the femoral neurovascular bundle. A second retractor is placed inferiorly beneath the transverse acetabular ligament, and a third is placed posteriorly to retract the femur posteriorly and distally.
The labrum is excised, and osteophytes are removed to identify the true floor of the acetabulum (the cotyloid fossa). Reaming is initiated with a small reamer directed medially to establish depth, followed by sequential reaming in the planned functional orientation of the cup—typically 40 degrees of abduction and 15 to 20 degrees of anteversion. The anterolateral approach provides a direct, unencumbered trajectory for acetabular reaming and component impaction.
Femoral Exposure and Preparation
To expose the femur, the leg is placed in a figure-of-four position (flexion, adduction, and extreme external rotation). In the lateral decubitus position, the leg is often placed in a sterile pouch anterior to the table.
A retractor is placed under the proximal femur to elevate it into the operative field. The remaining lateral capsule and the insertion of the gluteus minimus may need to be released to mobilize the proximal femur adequately. The femoral canal is entered with a box osteotome or a starting awl, ensuring a lateral starting point to prevent varus malalignment of the stem. Sequential broaching is performed until rotational stability and appropriate cortical chatter are achieved. Trial components are inserted, and the hip is reduced to assess leg length, offset, and stability.
Closure and Abductor Repair
Following the implantation of the definitive components, closure must be meticulous. The capsule is repaired if possible. The critical step is the repair of the abductor mechanism. If a transgluteal split was utilized, the gluteus medius, minimus, and vastus lateralis must be reapproximated using heavy, non-absorbable, or slowly absorbable sutures. Transosseous sutures through the greater trochanter may be required if the tendinous tissue is of poor quality.
Failure to achieve a robust repair will result in postoperative abductor escape, leading to a profound and often permanent limp. The fascia lata is closed continuously, followed by the subcutaneous tissues and skin.
Complications and Management
While the anterolateral approach boasts a low dislocation rate, it is associated with specific complications primarily related to the abductor mechanism and surrounding neurovascular structures.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage and Management Strategies |
|---|---|---|---|
| Abductor Weakness / Limp | 4% - 12% | Failure of tendinous repair, SGN injury, inadequate offset restoration. | Prolonged physical therapy; use of a cane. Surgical revision with gluteus maximus flap or Achilles allograft in severe, refractory cases. |
| Superior Gluteal Nerve Injury | 1% - 3% (Clinical) | Proximal extension of the intermuscular split >5cm above the GT, aggressive retraction. | Often neuropraxia that resolves in 3-6 months. Electromyography (EMG) at 3 months if no improvement. |
| Heterotopic Ossification | 15% - 30% (Radiographic) | Extensive muscle trauma, bone debris left in soft tissues. | Prophylaxis with NSAIDs (Indomethacin) or single-dose localized radiation. Surgical excision only after maturation (12-18 months) if symptomatic. |
| Dislocation | 0.4% - 1.2% | Component malposition, extreme non-compliance, impingement. | Closed reduction. Revision arthroplasty for recurrent instability (correction of version, use of larger head, or dual mobility). |
| Greater Trochanter Fracture | 1% - 2% | Aggressive retraction, osteoporotic bone, improper reaming trajectory. | Intraoperative: Cable grip system or tension band wiring. Postoperative: Protected weight-bearing if minimally displaced. |
Superior Gluteal Nerve Injury
The superior gluteal nerve is vulnerable during the proximal dissection. Injury can occur via direct transection, traction from rigid retractors, or entrapment in sutures during closure. Clinical presentation involves a profound Trendelenburg gait and an inability to actively abduct the hip against gravity. Management is initially expectant, as many injuries represent neuropraxia. If clinical weakness persists beyond three months, electromyography (EMG) is indicated to assess the extent of denervation.
Abductor Dysfunction and Heterotopic Ossification
Even in the absence of nerve injury, failure of the abductor repair can lead to significant morbidity. Patients present with lateral hip pain and a persistent limp. MRI with metal artifact reduction sequence (MARS) is the modality of choice to evaluate the integrity of the abductor tendons.
Heterotopic ossification (HO) is radiographically more common following the anterolateral and direct lateral approaches compared to the posterior approach, likely due to the extensive muscular dissection and stripping. While often asymptomatic, severe HO (Brooker Class III or IV) can lead to profound stiffness. Routine prophylaxis with NSAIDs or localized radiation is recommended for high-risk patients.
Dislocation and Instability
The primary advantage of the anterolateral approach is its inherent posterior stability. When dislocations do occur, they are typically anterior, resulting from excessive combined anteversion of the components or impingement of the anterior neck against the anterior acetabulum in extension
Clinical & Radiographic Imaging
You Might Also Like