Johnson Modified Chevron Osteotomy: Comprehensive Surgical Guide
Key Takeaway
The Johnson Modified Chevron Osteotomy is a powerful surgical technique for correcting moderate to severe hallux valgus deformities with intermetatarsal angles up to 16 degrees. By altering the osteotomy limb lengths and utilizing a 2.7-mm lag screw for rigid internal fixation, this modification enhances biomechanical stability. This guide details the precise indications, surgical steps, and postoperative protocols required to achieve optimal clinical outcomes and minimize complications such as avascular necrosis.
Introduction to the Johnson Modified Chevron Osteotomy
The surgical management of hallux valgus demands a nuanced understanding of forefoot biomechanics, vascular anatomy, and precise osteotomy principles. While the traditional Austin or chevron osteotomy—characterized by a 60-degree V-shaped cut with equal dorsal and plantar limbs—has long been the workhorse for mild to moderate deformities, its inherent geometric limitations restrict its utility in more severe presentations.
To address these limitations, Johnson popularized and subsequently modified the chevron osteotomy. By strategically altering the length and position of the osteotomy limbs within the first metatarsal head, Johnson significantly expanded the procedure's indications. The Johnson Modified Chevron Osteotomy features a longer plantar limb, an altered apical angle of approximately 70 degrees, and the routine use of a 2.7-mm cortical lag screw for rigid internal fixation. These modifications allow for greater lateral translation of the capital fragment, extending the procedure's utility to severe deformities with intermetatarsal angles (IMA) of 15 to 16 degrees, while simultaneously providing superior biomechanical stability compared to unfixated or K-wire-fixated alternatives.
This comprehensive guide delineates the precise indications, contraindications, biomechanical rationale, step-by-step surgical technique, and postoperative protocols required to master the Johnson Modified Chevron Osteotomy.
Indications and Patient Selection
The success of any hallux valgus correction is fundamentally predicated on rigorous patient selection. The Johnson modification specifically bridges the gap between distal metaphyseal osteotomies and proximal osteotomies or arthrodesis procedures.
Primary Indications
- Moderate to Severe Hallux Valgus: Patients presenting with a symptomatic hallux valgus angle (HVA) between 30 and 40 degrees.
- Elevated Intermetatarsal Angle: The primary advantage of the Johnson modification is its ability to address an IMA of 15 to 16 degrees. The extended plantar limb allows for a larger surface area of cancellous bone contact even with a lateral translation of 4 to 6 mm.
- Congruent or Subluxated First Metatarsophalangeal (MTP) Joint: The procedure is highly effective in realigning the articular surface and restoring the mechanical axis of the first ray.
- Adequate Bone Stock: Sufficient cancellous bone density in the metatarsal head is required to support the 2.7-mm lag screw and facilitate primary bone healing.
Contraindications
Johnson explicitly outlined several strict contraindications to this modified procedure to prevent catastrophic complications such as avascular necrosis (AVN) or fixation failure.
- Advanced Age (Older than 60 Years): Johnson did not recommend this osteotomy for patients over 60. Older patients frequently exhibit osteopenia or osteoporosis, which compromises the purchase of the 2.7-mm screw and increases the risk of intraoperative fracture or postoperative displacement. Furthermore, age-related microvascular changes increase the risk of AVN.
- Previous Hallux Valgus Surgery: Revision cases are an absolute contraindication. Prior surgical intervention inevitably disrupts the delicate extraosseous vascular network supplying the first metatarsal head, specifically the first dorsal metatarsal artery and the plantar capsular plexus. A subsequent osteotomy carries an unacceptably high risk of capital fragment necrosis.
- Diminished Joint Mobility and Crepitance: Patients with clinical signs of hallux rigidus, advanced degenerative joint disease (DJD), or significant crepitus are poor candidates. Realigning an arthritic joint will not alleviate pain and may exacerbate stiffness. These patients are better served by arthrodesis or arthroplasty.
- Hypermobility of the First Ray: Severe first tarsometatarsal (TMT) joint instability may lead to recurrence if addressed solely with a distal osteotomy. A Lapidus procedure should be considered in these scenarios.
💡 Clinical Pearl: Vascular Preservation
The blood supply to the first metatarsal head is predominantly derived from the plantar-lateral capsular vessels. The Johnson modification, while requiring adequate exposure for a longer plantar limb, demands meticulous surgical technique to avoid excessive lateral and plantar capsular stripping. Preserving this soft tissue envelope is the single most critical factor in preventing avascular necrosis.
Preoperative Planning and Biomechanics
Radiographic Assessment
Standard weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory.
* AP View: Assess the HVA, IMA, distal metatarsal articular angle (DMAA), and the length of the first metatarsal relative to the second.
* Lateral View: Evaluate for dorsal elevatus, plantarflexion, or midfoot degenerative changes.
* Sesamoid Axial View: Determine the degree of fibular sesamoid subluxation and assess the crista for erosive changes.
Biomechanical Rationale of the Modification
The traditional 60-degree chevron osteotomy provides excellent intrinsic stability but limits lateral translation to approximately 30-40% of the metatarsal width before bone contact becomes critically compromised.
Johnson’s modification alters the geometry to an approximate 70-degree angle between the dorsal and plantar limbs. By initiating the plantar limb 5 to 6 mm proximal to the articular surface and extending it further proximally to exit at the inferior aspect of the metatarsal head-neck junction, a longer, more horizontal plantar shelf is created. This extended shelf serves two critical biomechanical functions:
1. It dramatically increases the surface area for cancellous bone healing, allowing for a safe lateral translation of 4 to 6 mm (sufficient to correct an IMA of 16 degrees).
2. It provides a robust osseous platform that resists plantarflexion or dorsiflexion forces during early weight-bearing.
Furthermore, the integration of a 2.7-mm cortical lag screw directed from the dorsal metatarsal shaft into the capital fragment provides rigid interfragmentary compression. This neutralizes shear forces at the osteotomy site, allowing for earlier mobilization and reducing the risk of malunion.
Surgical Technique: Step-by-Step
1. Patient Positioning and Anesthesia
The patient is positioned supine on the operating table. The procedure can be performed under a regional ankle block, spinal anesthesia, or general anesthesia, depending on patient preference and comorbidities. A well-padded calf or thigh tourniquet is applied to ensure a bloodless surgical field, which is critical for identifying anatomical landmarks and protecting neurovascular structures.
2. Surgical Approach and Exposure
- Incision: Make a midline, longitudinal, medial capsular incision centered over the first MTP joint. The incision should extend from the mid-shaft of the proximal phalanx to the mid-shaft of the first metatarsal.
- Dissection: Deepen the incision through the subcutaneous tissues, taking care to identify and retract the dorsal medial cutaneous nerve branches.
- Capsulotomy: Perform a longitudinal capsulotomy in line with the skin incision. Carefully elevate the capsule dorsally and plantarward to expose the medial eminence.
- Exposure Limits: Expose the metatarsal head dorsally and plantarward just enough to visualize the planned dorsal and plantar limbs of the osteotomy, and laterally enough to safely place the 2.7-mm screw.
⚠️ Surgical Warning: Capsular Stripping
Avoid excessive stripping of the lateral and plantar capsule. The principal blood supply to the capital fragment enters via the plantar-lateral retinacular vessels. Overzealous lateral release or circumferential stripping will inevitably lead to avascular necrosis of the metatarsal head.
3. Exostectomy (Removal of the Medial Eminence)
Using an oscillating power saw equipped with a 9-mm blade, resect the medial eminence.
* Critical Angulation: The resection cut must be made at an angle that is parallel to the medial border of the foot, not parallel to the medial border of the metatarsal shaft. Resecting parallel to the shaft often results in excessive bone removal, compromising the medial cortical hinge and destabilizing the subsequent osteotomy.
4. The Plantar Limb of the Osteotomy
The precision of the osteotomy cuts dictates the success of the Johnson modification.
* Apex Placement: Begin the inferior (plantar) limb of the osteotomy 5 to 6 mm proximal to the medial articular surface of the first metatarsal. The apex should be positioned exactly midway between the superior and inferior margins of the metatarsal head in its center portion.
* Trajectory: Direct the saw blade proximally and plantarward. This plantar extension must exit extracapsularly at the inferior aspect of the metatarsal head and neck junction, or just proximal to it.
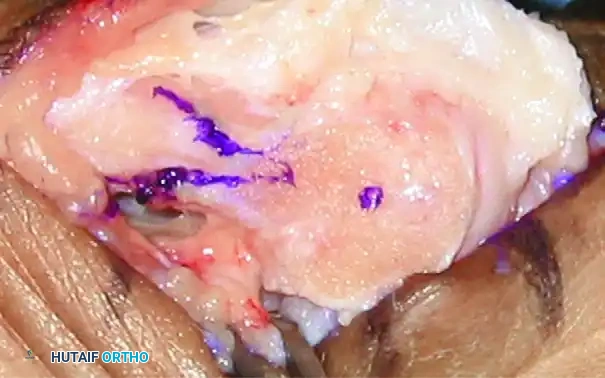
- Execution: The lateral portion of this plantar cut can be technically demanding due to the density of the bone and limited visibility. Ensure that the saw blade passes completely through the lateral cortex before attempting any translation. Incomplete cuts will cause the capital fragment to hinge or fracture during the shift.
5. The Dorsal Limb of the Osteotomy
- Trajectory: Initiate the second (dorsal) limb of the osteotomy from the exact apex of the first cut. Direct the saw blade dorsally at an approximate angle of 70 degrees relative to the plantar limb.
- Exit Point: This limb should exit the dorsal cortex just proximal to the dorsal border of the articular surface of the metatarsal head.
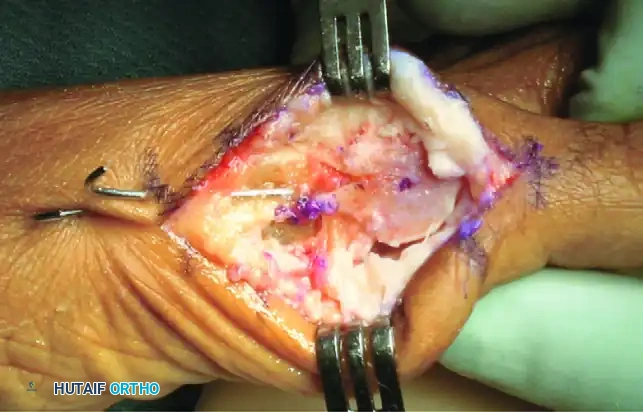
6. Translation and Impaction of the Capital Fragment
- Stabilization: Grasp and stabilize the proximal metatarsal shaft firmly using a manual grip or a towel clip.
- Lateral Shift: Gently displace the capital fragment laterally by 4 to 6 mm. It is imperative that this translation occurs purely in the transverse plane. There must be absolutely no tilting, opening, or hinging of the osteotomy site medially, laterally, superiorly, or inferiorly.
- Impaction: Once the desired lateral translation is achieved, compress the great toe longitudinally against the head of the metatarsal. This axial loading impacts the cancellous bone at the osteotomy site, locking the fragments into the newly translated position and maximizing intrinsic stability prior to fixation.
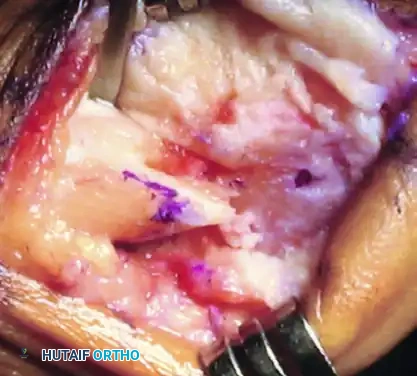
7. Internal Fixation with a 2.7-mm Lag Screw
Rigid internal fixation is a hallmark of the Johnson modification, preventing displacement and allowing for earlier rehabilitation.
* Pilot Hole: Use a 2.0-mm drill bit to create a pilot hole in the dorsal surface of the distal metatarsal shaft, just proximal to the dorsal limb of the osteotomy.
* Bone Ledge: Crucially, leave an approximately 3-mm ledge of intact cortical bone between the drill hole and the superior arm of the osteotomy to prevent the screw head from breaking through the cortex during compression.
* Drill Trajectory: Direct the 2.0-mm drill bit from proximal to distal at a 10-degree plantarward angle, and 10 to 15 degrees lateralward. This trajectory ensures the screw passes centrally into the substance of the transposed capital fragment. Pass the bit through the dorsal cortex, across the osteotomy, through the cancellous bone of the capital fragment, and into the dense subchondral bone just deep to the articular cartilage.
* Creating the Lag Effect: To achieve interfragmentary compression, the proximal cortex must be overdrilled. Ream the proximal aspect of the hole (the metatarsal shaft) with a 2.7-mm drill bit to create a gliding hole.
* Measurement: Use a depth gauge to measure the required screw length. In most adult patients, a 16-mm to 18-mm screw is appropriate.
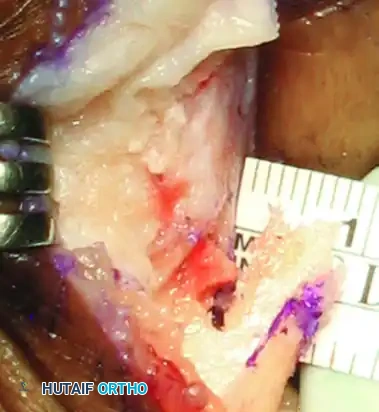
- Tapping and Insertion: Tap the entire drill tract with a 2.7-mm tap. Insert the 2.7-mm cortical screw and tighten it carefully to compress and close the osteotomy site.
⚠️ Pitfall: Articular Penetration
Under no circumstances should the screw be allowed to exit through the articular surface of the metatarsal head. Penetration into the joint space will severely impair sesamoid glide, leading to intractable postoperative pain, limited range of motion, and rapid joint degeneration. Always verify screw length and placement with intraoperative fluoroscopy.
8. Remodeling and Capsulorrhaphy
- Resecting the Overhang: Following the lateral shift of the capital fragment, a prominent bony overhang will remain on the medial aspect of the distal metatarsal shaft. Use a power saw to carefully contour this overhang flush with the medial aspect of the transposed head.
- Avoid Skiving: Do not skive laterally into the center of the metatarsal shaft, as this will create a stress riser and risk a postoperative shaft fracture. Use a small rongeur or a rasp to meticulously smooth the dorsomedial aspect of the metatarsal head, ensuring no sharp edges remain to irritate the capsule.
- Capsular Closure: Position and hold the hallux in neutral flexion and extension, and approximately 10 degrees of varus. Overlap the medial capsule to assess redundancy. Excise any excess capsular tissue (typically 3 to 5 mm).
- Suturing: Close the capsule under tension using multiple interrupted 2-0 or 3-0 nonabsorbable sutures.
- Final Assessment: After capsular closure is complete, release the toe. The hallux should rest naturally in a straight, rectus position, with the medial aspect of the proximal phalanx resting congruently against the medial aspect of the newly displaced capital fragment.
9. Dressing Application
Apply a sterile, compressive dressing designed to hold the hallux in the corrected position. The dressing should splint the toe in slight plantarflexion and neutral alignment, taking tension off the medial capsular repair while controlling postoperative edema.
Postoperative Care and Rehabilitation Protocol
The postoperative protocol for the Johnson Modified Chevron Osteotomy balances the need for osteotomy protection with the desire for early mobilization to prevent joint stiffness.
Days 1 to 4: Immediate Postoperative Phase
- Weight-Bearing: The patient is restricted to partial weight-bearing using crutches. Heel-touch weight-bearing is permissible, but rolling through the forefoot is strictly prohibited.
- Elevation: Strict elevation of the operative extremity above heart level is mandated to minimize edema and throbbing pain.
Days 4 to 14: Cast Immobilization
- Dressing Change: At 3 to 4 days postoperatively, the initial bulky surgical dressing is removed. The wound is inspected for signs of infection or marginal necrosis.
- Casting: A short-leg walking cast is applied. Crucially, the plantar aspect of the cast must extend distal to the great toe to provide a rigid, gentle support platform.
- Mobility: The primary purpose of this cast is patient comfort and mobility. It neutralizes ground reaction forces across the forefoot, allowing the patient to ambulate safely without the need for crutches or a walker.
Weeks 2 to 4: Early Mobilization
- Cast Removal: The walking cast is removed approximately 1 week after application (roughly 10-14 days post-op). Sutures are typically removed at this time if the incision is fully healed.
- Footwear: The patient is transitioned into a stiff-soled postoperative shoe, which must be worn for an additional 3 weeks. This shoe prevents dorsiflexion of the MTP joint during the toe-off phase of gait.
- Range of Motion (ROM): Gentle, active and passive ROM exercises of the great toe are initiated to prevent capsular adhesions and preserve joint mobility.
- Splinting: A hallux valgus night splint or toe spacer is applied to protect the medial capsular repair and maintain soft tissue balance during sleep.
Weeks 5 and Beyond: Maturation Phase
- Transition to Normal Footwear: After approximately 3 to 4 weeks in the stiff-soled shoe (roughly 5-6 weeks post-op), clinical and radiographic evidence of early bone healing should be present. The patient may then transition into a deep, wide, soft-accommodative shoe (e.g., a wide-toe-box running shoe).
- Advanced Rehabilitation: Physical therapy may be prescribed to focus on gait retraining, intrinsic foot muscle strengthening, and maximizing first MTP joint dorsiflexion. High-impact activities and narrow footwear should be avoided for at least 3 to 4 months.
Complications and Management
While the Johnson Modified Chevron Osteotomy is highly successful when executed correctly, surgeons must be prepared to manage potential complications.
- Avascular Necrosis (AVN): The most devastating complication. Risk is minimized by adhering to the age limit (<60 years), avoiding revision cases, and meticulously preserving the lateral/plantar soft tissue attachments. If AVN occurs and leads to collapse, salvage typically requires first MTP joint arthrodesis.
- Hallux Varus: Overcorrection can result from excessive lateral translation of the capital fragment, over-resection of the medial eminence, or over-tightening of the medial capsule. Mild cases may be managed with taping; severe, symptomatic cases require surgical release or reverse osteotomy.
- Undercorrection / Recurrence: Often due to failure to achieve adequate lateral translation (limited by incomplete bone cuts) or failure to recognize hypermobility of the first TMT joint preoperatively.
- Hardware Irritation: The 2.7-mm screw head may become prominent dorsally once edema subsides. If symptomatic after bone healing is complete (typically >6 months), the screw can be removed under local anesthesia.
- Malunion / Dorsal Elevatus: Failure to maintain the capital fragment in a neutral sagittal plane during fixation can lead to dorsal elevatus, resulting in transfer metatarsalgia to the lesser metatarsals. This underscores the importance of the 3-mm dorsal cortical ledge and precise screw trajectory.
📚 Medical References
- Chevron osteotomy and single wire reattachment of the greater trochanter in primary and revision total hip arthroplasty, Clin Orthop Relat Res 294:155, 1993.
- Berman AT, McGovern KM, Paret RS, et al: The use of preoperative computed tomography scanning in total hip arthroplasty, Clin Orthop Relat Res 222:190, 1987.
- Blackley HRL, Howell GED, Rorabeck CH: Planning and management of the diffi cult primary hip replacement: preoperative planning and technical considerations, Instr Course Lect 49:3, 2000.
- Bono JV: Digital templating in total hip arthroplasty, J Bone Joint Surg 86A:118, 2004.
- Bracy D, Wroblewski BM: Bilateral Charnley arthroplasty as a single procedure: a report of 400 patients, J Bone Joint Surg 63B:354, 1981.
- Brander VA, Malhotra S, Jet J, et al: Outcome of hip and knee arthroplasty in persons aged 80 years and older, Clin Orthop Relat Res 345:67, 1997.
- Breusch SJ, Normal TL, Schneider U, et al: Lavage technique in total hip arthroplasty: jet lavage produces better cement penetration than syringe lavage in the proximal femur, J Arthroplasty 159:21, 2000.
- Brien WW, Bruce WJ, Salvati EA, et al: Acetabular reconstruction with a bipolar prosthesis and morselized bone grafts, J Bone Joint Surg 72A:1230, 1990.
- Capello WN: Preoperative planning of total hip arthroplasty, Instr Course Lect 35:249, 1986.
- Charnley J, Ferreira A de SD: Transplantation of the greater trochanter in arthroplasty of the hip, J Bone Joint Surg 46B:191, 1964.
- Chimento GF, Pavone V, Sharrock N, et al: Minimally invasive total hip arthroplasty: a prospective randomized study, J Arthroplasty 20:139, 2005.
- Coventry MB: The surgical technique of total hip arthroplasty, modifi ed from Charnley, as done at the Mayo Clinic, Orthop Clin North Am 4:473, 1973.
- Coventry MB, Scanlon PW: The use of radiation to discourage ectopic bone: a nine-year study in surgery about the hip, J Bone Joint Surg 63A:201, 1981.
- Dall D: Exposure of the hip by anterior osteotomy of the greater trochanter: a modifi ed anterolateral approach, J Bone Joint Surg 68B:382, 1986.
- Dall DM, Miles AW: Reattachment of the greater trochanter: the use of the trochanter cable-grip system, J Bone Joint Surg 65B:55, 1983.
- Davies JP, Harris WH: In vitro and in vivo studies of pressurization of femoral cement in total hip arthroplasty, J Arthroplasty 8:585, 1993.
- De Beer J, Petruccelli D, Zalzal P, et al: Single-incision, minimally invasive total hip arthroplasty: length doesn’t matter, J Arthroplasty 19:945, 2004.
- Demos HA, Rorabeck CH, Bourne RB, et al: Instability in primary total hip arthroplasty with the direct lateral approach, Clin Orthop Relat Res 393:168, 2001.
- DeWal H, Chen F, Su E, et al: Use of structural bone graft with cementless acetabular cups in total hip arthroplasty, J Arthroplasty 18:23, 2003.
- Dias JJ, Johnson GV, Finlay DBL, et al: Preoperative evaluation for uncemented hip arthroplasty: the role of computerized tomography, J Bone Joint Surg 71B:43, 1989.
- DiGioia AM, Jaramaz BA, Levison TJ: Less invasive total hip arthroplasty using navigational tools, Instr Course Lect 53:157, 2004.
- DiGioia M, Plakseychuk AY, Levison TJ, et al: Mini-incision technique for total hip arthroplasty with navigation, J Arthroplasty 18:123, 2003.
- Dunn HK, Hess WE: Total hip reconstruction in chronically dislocated hips, J Bone Joint Surg 58A:838, 1976.
- Ebramzadeh E, Sarmiento A, McKellop H, et al: The cement mantle in total hip arthroplasty: analysis of long-term radiographic results, J Bone Joint Surg 76A:77, 1994.
- Eftekhar NS, Pawluk RJ: Role of surgical preparation in acetabular cup fi xation. In The hip: proceedings of the Eighth Open Scientifi c Meeting of the Hip Society, St Louis, 1980, Mosby. Eggli S, Huckell CB, Ganz R: Bilateral total hip arthroplasty: one-stage versus two-stage procedure, Clin Orthop Relat Res 328:108, 1996.
- Esemenli BT, Toker K, Lawrence R: Hypotension associated with methylmethacrylate in partial hip arthroplasties: the role of femoral canal size, Orthop Rev 20:619, 1991.
- Foster DE, Hunter JR: The direct lateral approach to the hip for arthroplasty: advantages and complications, Orthopedics 10:274, 1987.
- Glassman AH, Engh CA, Bobyn JD: A technique of extensile exposure for total hip arthroplasty, J Arthroplasty 2:11, 1987.
- Goldstein WM, Branson JJ, Berland KA, et al: Minimal-incision total hip arthroplasty, J Bone Joint Surg 85A:33, 2003.
- Goodman S, Pressman A, Saastamoinen H, et al: Technical note: modifi ed sliding trochanteric osteotomy in revision total hip arthroplasty, J Arthroplasty 19:1039, 2004.
- Grosvenor D, Goyal V, Goodman S: Effi cacy of postoperative blood salvage following total hip arthroplasty in patients with and without deposited autologous units, J Bone Joint Surg 82A:951, 2000.
- Hardinge K: The direct lateral approach to the hip, J Bone Joint Surg 64B:17, 1982.
- Harris WH: Extensive exposure of the hip joint, Clin Orthop Relat Res 91:58, 1973.
- Harris WH: A new approach to total hip replacement without osteotomy of the greater trochanter, Clin Orthop Relat Res 106:19, 1975.
- Harris WH, Mulroy RD, Maloney WJ, et al: Intraoperative measurement of rotational stability of femoral components of total hip arthroplasty, Clin Orthop Relat Res 266:121, 1991.
- Healy WL, Iorio R: Total hip arthroplasty: optimal treatment for displaced
You Might Also Like


