Operative Management of Hallux Valgus: Pathoanatomy, Biomechanics, and Surgical Reconstruction
Key Takeaway
Hallux valgus is a complex, three-dimensional deformity of the first ray characterized by lateral deviation of the great toe and medial deviation of the first metatarsal. Successful surgical management requires a profound understanding of first ray biomechanics, precise radiographic evaluation of the intermetatarsal and distal metatarsal articular angles, and meticulous execution of soft tissue balancing combined with appropriate osseous realignment procedures to restore joint congruency and prevent recurrence.
INTRODUCTION TO HALLUX VALGUS
Hallux valgus (lateral deviation of the great toe) is not a single, isolated disorder, as the colloquial term "bunion" implies, but rather a complex, progressive, three-dimensional deformity of the first ray. It is frequently accompanied by secondary deformities and symptomatic pathology in the lesser toes. The condition is characterized by lateral deviation and pronation of the hallux, medial deviation of the first metatarsal, and subluxation of the first metatarsophalangeal (MTP) joint.
Successful management of hallux valgus demands a rigorous understanding of foot biomechanics, precise radiographic analysis, and a tailored surgical approach that addresses both the osseous deformity and the soft-tissue imbalance. Failure to recognize the multiplanar nature of this deformity—particularly the rotational component and articular congruency—inevitably leads to suboptimal outcomes, recurrence, or iatrogenic complications such as hallux varus.
PATHOANATOMY AND BIOMECHANICS
The pathogenesis of hallux valgus is driven by a failure of the medial stabilizing structures of the first MTP joint, followed by the relentless deforming forces of the intrinsic and extrinsic musculature.
The Deforming Cascade
Normally, the angle between the first and second metatarsals (Intermetatarsal Angle, IMA) is less than 8 to 9 degrees, which is considered the upper limit of normal. The valgus angle of the first MTP joint (Hallux Valgus Angle, HVA) is normally less than 15 to 20 degrees.
When the HVA exceeds 30 to 35 degrees, pronation of the great toe invariably results. This abnormal rotation fundamentally alters the biomechanical axes of the first ray:
* Abductor Hallucis Shift: The abductor hallucis, normally positioned plantar to the flexion-extension axis of the first MTP joint, moves further plantarward. It loses its ability to abduct the hallux and instead becomes a plantar flexor and pronator.
* Medial Capsular Attenuation: With the abductor hallucis displaced, the only remaining medial restraint is the medial capsular ligament. This structure consists of the capsulosesamoid portion (inserting into the base of the proximal phalanx) and the capsulophalangeal portion (inserting into the plantar plate). These structures stretch and attenuate, allowing the metatarsal head to drift medially away from the sesamoid apparatus.
* Adductor Hallucis Overdrive: Unopposed by the abductor hallucis, the adductor hallucis pulls the great toe further into valgus.
* Bowstringing Effect: The extrinsic tendons—specifically the extensor hallucis longus (EHL) and flexor hallucis longus (FHL)—along with the flexor hallucis brevis (FHB), bowstring laterally across the MTP joint. This dramatically increases the valgus moment, further exacerbating the deformity.
Clinical Pearl: The deep transverse intermetatarsal ligament runs between the plantar plates at the MTP joints and does not insert into bone on the adjacent sides of the metatarsal heads. Therefore, the sesamoid complex remains tethered to the second metatarsal while the first metatarsal head drifts medially off the sesamoid apparatus.
Sesamoid Subluxation and Transfer Metatarsalgia
As the first metatarsal drifts medially, the sesamoid ridge on the plantar surface of the first metatarsal head (the crista) flattens due to chronic pressure and abutment from the tibial sesamoid. Once this osseous restraint is lost, the fibular sesamoid displaces partially or completely into the first intermetatarsal space.
Consequently, the biomechanical efficiency of the first ray during the push-off phase of gait is severely compromised. The patient bears less weight on the first ray and transfers the load laterally to the lesser metatarsal heads. This biomechanical shift increases the likelihood of transfer metatarsalgia, intractable plantar keratoses (callosities), and stress fractures of the lesser metatarsals (most commonly the second metatarsal).
RADIOGRAPHIC EVALUATION AND ANATOMICAL VARIANTS
Weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory for preoperative planning. The surgeon must meticulously evaluate the articular surfaces of the first MTP joint, as anatomical variants dictate the choice of surgical procedure.
Key Radiographic Angles
- Hallux Valgus Angle (HVA): Normal is < 15 degrees. Formed by the intersection of the longitudinal axes of the first metatarsal and the proximal phalanx.
- Intermetatarsal Angle (IMA): Normal is < 9 degrees. Formed by the intersection of the longitudinal axes of the first and second metatarsals.
- Distal Metatarsal Articular Angle (DMAA): Normal is 10 to 15 degrees. This measures the relationship of the articular surface of the metatarsal head to the longitudinal axis of the metatarsal.
- Phalangeal Articular Angle (PAA): Normal is 7 to 10 degrees. This measures the articular angle of the base of the proximal phalanx in relation to its longitudinal axis.
Articular Congruency and Anatomical Variants
Two critical anatomical variants involving the articular surfaces can lead to hallux valgus and complicate surgical correction:
* The Offset Metatarsal Head (Increased DMAA): The articular surface of the metatarsal head is laterally deviated, resembling a "scoop of ice cream sitting at an angle on a cone."
* The Offset Phalangeal Base (Increased PAA): The articular surface of the proximal phalanx is asymmetric relative to its shaft.
Surgical Warning: Increasing evidence indicates that failure to correct an abnormal DMAA is a primary cause of unsatisfactory results and recurrence. Forceful straightening of the hallux via soft-tissue plication must be avoided if it sacrifices a congruent MTP articulation. If the joint is congruent but deviated, a phalangeal osteotomy (Akin) or a distal metatarsal osteotomy (e.g., biplanar Chevron or Reverdin) must be utilized rather than aggressive tightening of the medial capsule.
SURGICAL DECISION MAKING
The selection of the appropriate surgical procedure is dictated by the severity of the deformity, the presence of joint congruency, the degree of hypermobility at the first tarsometatarsal (TMT) joint, and the presence of degenerative joint disease (DJD).
- Mild Deformity (HVA < 30°, IMA < 13°): Distal metatarsal osteotomy (e.g., Chevron) combined with a lateral soft-tissue release and medial capsulorrhaphy.
- Moderate Deformity (HVA 30°-40°, IMA 13°-20°): Diaphyseal osteotomy (e.g., Scarf) or proximal metatarsal osteotomy (e.g., Ludloff, Crescentic) with lateral release.
- Severe Deformity (HVA > 40°, IMA > 20°) or TMT Hypermobility: First TMT arthrodesis (Lapidus procedure) to correct the deformity at its apex and stabilize the medial column.
- Degenerative Joint Disease (Hallux Rigidus with Valgus): First MTP joint arthrodesis is the gold standard, providing reliable pain relief and deformity correction.
OPERATIVE TECHNIQUES: STEP-BY-STEP
1. Patient Positioning and Preparation
The patient is placed supine on the operating table. A bump is placed under the ipsilateral hip to internally rotate the leg to a neutral position, allowing direct visualization of the dorsal and medial aspects of the foot. A thigh or calf tourniquet is applied to ensure a bloodless surgical field. Prophylactic intravenous antibiotics are administered prior to inflation.
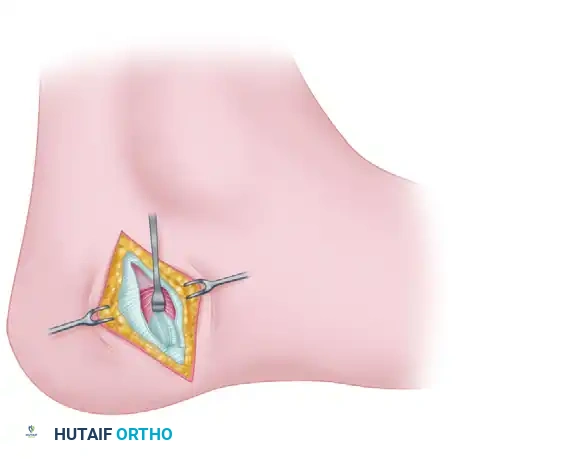
2. The Lateral Soft-Tissue Release
The lateral release is critical for mobilizing the MTP joint and allowing the sesamoid apparatus to reduce beneath the metatarsal head. It can be performed via a dorsal first web-space incision or a transarticular approach through the medial incision.
- Step 1: Identify and protect the terminal branches of the deep peroneal nerve and the first dorsal metatarsal artery.
- Step 2: Release the adductor hallucis tendon from its insertion on the base of the proximal phalanx and the fibular sesamoid.
- Step 3: Transect the deep transverse intermetatarsal ligament to free the fibular sesamoid from the second metatarsal.
- Step 4: Release the lateral metatarsosesamoid suspensory ligament.
- Step 5: Perform a lateral capsulotomy.
Pitfall: Avoid routine excision of the fibular sesamoid, as this significantly increases the risk of iatrogenic hallux varus and alters the biomechanics of the FHB. Excision should be reserved for cases of severe, irreducible arthritic degeneration of the sesamoid.
3. The Medial Approach and Eminence Resection
- Incision: A longitudinal medial incision is made centered over the first MTP joint, extending from the mid-shaft of the proximal phalanx to the mid-shaft of the first metatarsal.
- Capsulotomy: A V-shaped, L-shaped, or longitudinal capsulotomy is performed. The capsular flaps are carefully elevated to expose the medial eminence and the articular surface.
- Exostectomy: The medial eminence is resected using an oscillating saw. The cut should be made parallel to the medial border of the foot, starting 1 to 2 mm medial to the sagittal sulcus.
- Preservation of the Sulcus: It is imperative to preserve the sagittal groove, as resecting too much bone will destabilize the joint and compromise the tibial sesamoid articulation.
4. Osseous Realignment (Osteotomy)
The choice of osteotomy depends on the preoperative plan. For a standard distal Chevron osteotomy:
* A K-wire is placed in the center of the metatarsal head to mark the apex of the osteotomy.
* A V-shaped cut (typically 60 degrees) is made with the apex distal.
* The capital fragment is translated laterally (up to 50% of the metatarsal width).
* If the DMAA is abnormal, a medial closing wedge component can be incorporated into the Chevron cut (biplanar Chevron) to rotate the articular cartilage medially.
* The osteotomy is provisionally fixed with a K-wire, checked under fluoroscopy, and definitively fixed with a headless compression screw or a threaded K-wire.
* The overhanging medial cortical edge of the proximal fragment is resected flush with the translated head.
5. Phalangeal Correction (Akin Osteotomy)
If the hallux remains in valgus despite a congruent MTP joint and a corrected IMA (indicating an abnormal PAA or hallux valgus interphalangeus), a medial closing wedge osteotomy of the proximal phalanx (Akin procedure) is indicated.
* A transverse cut is made at the metaphyseal-diaphyseal junction of the proximal phalanx, leaving the lateral cortex intact to act as a hinge.
* A small medial wedge of bone is removed, the osteotomy is closed, and it is fixed with a staple, screw, or suture.
6. Medial Capsulorrhaphy
The final step is the meticulous repair of the medial capsule to restore the tension of the medial structures and reposition the abductor hallucis.
* The toe is held in neutral alignment (0 degrees of valgus, 10 degrees of dorsiflexion).
* The capsular flaps are imbricated and sutured using non-absorbable or slowly absorbable sutures.
* Crucial Step: Ensure that the capsulosesamoid and capsulophalangeal portions of the ligament are tensioned appropriately to pull the tibial sesamoid back into its anatomical position beneath the metatarsal head.
POSTOPERATIVE PROTOCOL
Postoperative management is as critical as the surgical execution to ensure optimal outcomes and prevent displacement of the osteotomies.
- Immediate Post-Op: The foot is placed in a bulky, compressive dressing. The hallux is splinted in a neutral position using bandages to protect the medial capsulorrhaphy.
- Weight-Bearing: Depending on the stability of the osteotomy, patients are typically allowed heel-weight-bearing or flat-foot weight-bearing in a rigid postoperative shoe or boot immediately after surgery. Lapidus procedures or proximal osteotomies may require 2 to 6 weeks of strict non-weight-bearing.
- Wound Care: Dressings are changed at 10 to 14 days, and sutures are removed. A toe spacer or bunion splint is often utilized for an additional 4 to 6 weeks to maintain alignment while the soft tissues heal.
- Rehabilitation: Active and passive range-of-motion (ROM) exercises of the first MTP joint are initiated at 2 to 3 weeks to prevent arthrofibrosis. Strengthening of the intrinsic foot musculature begins at 6 weeks.
- Return to Activity: Transition to wide-toe-box athletic shoes occurs at 6 to 8 weeks. High-impact activities and sports are generally restricted until 3 to 4 months postoperatively, pending radiographic evidence of complete osseous union.
COMPLICATIONS AND PITFALLS
Despite meticulous technique, complications can arise. Surgeons must be prepared to identify and manage these effectively.
- Hallux Varus: Often caused by over-resection of the medial eminence, over-tightening of the medial capsule, aggressive lateral release (especially excision of the fibular sesamoid), or excessive lateral translation of the metatarsal head. It presents as a medial deviation of the toe and can be highly symptomatic.
- Recurrence: The most common complication, typically resulting from under-correction of the IMA, failure to recognize and correct an abnormal DMAA, or failure to address first TMT hypermobility.
- Avascular Necrosis (AVN) of the Metatarsal Head: The blood supply to the first metatarsal head enters via the distal capsular attachments. Extensive lateral release combined with aggressive medial stripping can disrupt this vascularity. Surgeons must preserve the plantar-lateral soft tissue attachments during osteotomies.
- Transfer Metatarsalgia: If the first metatarsal is excessively shortened or dorsiflexed during the osteotomy, weight-bearing forces will shift to the lesser metatarsals, leading to intractable pain and callosities under the second or third metatarsal heads. Precise execution of plantar-flexing or length-preserving osteotomies is essential.
You Might Also Like