Mastering PIP Joint Collateral Ligament Reconstruction via Tendon Graft
Key Takeaway
Chronic instability of the proximal interphalangeal (PIP) joint following a neglected or severe collateral ligament rupture often necessitates surgical reconstruction. Utilizing a free tendon graft, such as the palmaris longus, restores coronal plane stability and joint kinematics. This advanced surgical guide details the biomechanical principles, precise anatomical approaches, graft routing techniques, and postoperative rehabilitation protocols required to achieve optimal functional outcomes in complex PIP joint ligamentous reconstructions.
Introduction to Proximal Interphalangeal Joint Instability
The proximal interphalangeal (PIP) joint is a highly constrained ginglymus (hinge) joint, relying heavily on its ligamentous architecture for stability throughout its extensive arc of motion. The primary static stabilizers are the proper collateral ligaments (PCL), the accessory collateral ligaments (ACL), and the volar plate. Rupture of the collateral ligament complex, typically resulting from forced lateral deviation and rotational torque, can lead to debilitating chronic instability, pain, and diminished grip strength if left untreated or if primary repair fails.
When direct anatomical repair is precluded by tissue retraction, poor tissue quality, or chronicity, reconstruction utilizing a free tendon graft becomes the gold standard. This comprehensive guide delineates the surgical technique for replacing a ruptured collateral ligament of the PIP joint using a tendon autograft, ensuring restoration of coronal stability and functional kinematics.
Biomechanics and Pathoanatomy
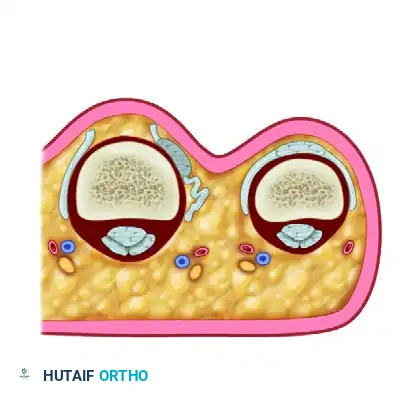
Understanding the intricate biomechanics of the PIP joint is paramount for successful reconstruction. The proper collateral ligament originates from the dorsal-lateral aspect of the proximal phalanx head and inserts into the volar-lateral base of the middle phalanx. It is taut in flexion, providing maximal stability against varus and valgus stress. The accessory collateral ligament originates volar to the PCL and inserts into the volar plate, remaining taut in extension.
Undiagnosed Interphalangeal Dislocations
Failure to diagnose interphalangeal dislocations in the acute setting is a rare but catastrophic clinical error. Rapid onset of edema often obscures the bony landmarks that typically make early diagnosis straightforward.
🚨 SURGICAL WARNING: If a PIP joint dislocation is not diagnosed and reduced within the first week, the articular cartilage may undergo rapid erosion due to abnormal pressure from the articular edge of the dislocated phalanx. In such delayed presentations, closed reduction is frequently impossible, and open reduction with potential ligamentous reconstruction is mandated.
Irreducible and Complex Dislocations
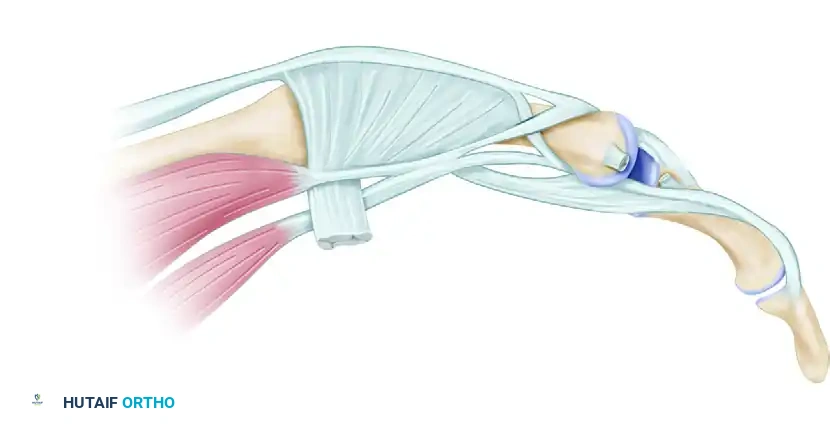
Certain injury patterns result in irreducible dislocations due to soft tissue interposition. A classic example is the rupture of the collateral ligament accompanied by the trapping of the lateral band of the extensor hood within the joint space.

Irreducible dislocation of the proximal interphalangeal joint. The collateral ligament has been torn, and the lateral band of the extensor hood is trapped within the joint (Dorsal view).

Lateral view demonstrating the trapped lateral band preventing concentric reduction.
Similarly, volar dislocations can present with complex pathoanatomy, often suggestive of a central slip injury. In severe cases, the radial condyle of the proximal phalanx may buttonhole through the extensor mechanism, trapping the lateral band volarly.
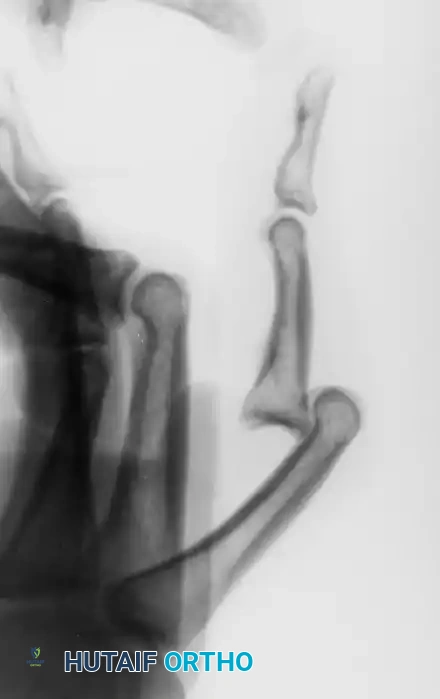
Volar dislocation of the middle finger PIP joint, suggestive of a central slip injury.
Proximal phalangeal radial condyle buttonholed through the extensor mechanism with the lateral band trapped volarly.
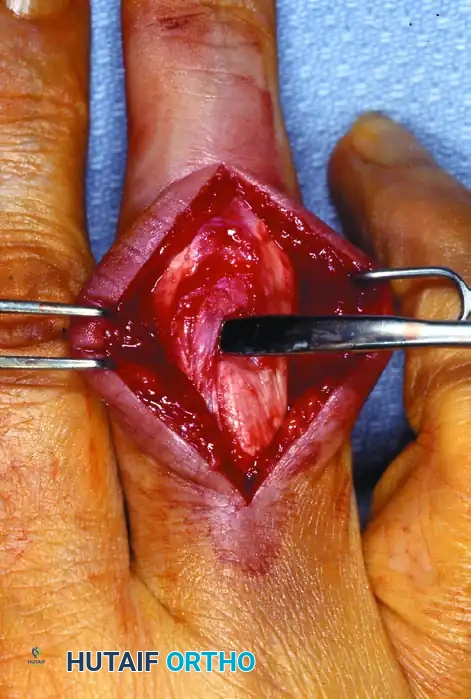
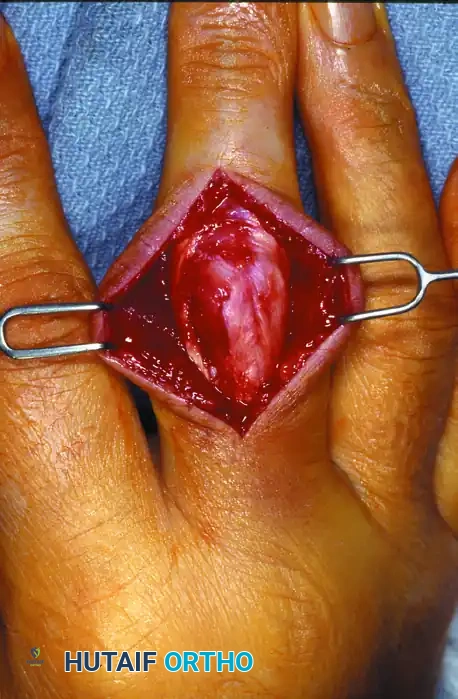
Intraoperative view following the reduction of the trapped lateral band.
Even with acute anatomical repair and restoration of good flexion, patients may experience persistent extensor lags due to the attenuation of the extensor mechanism.
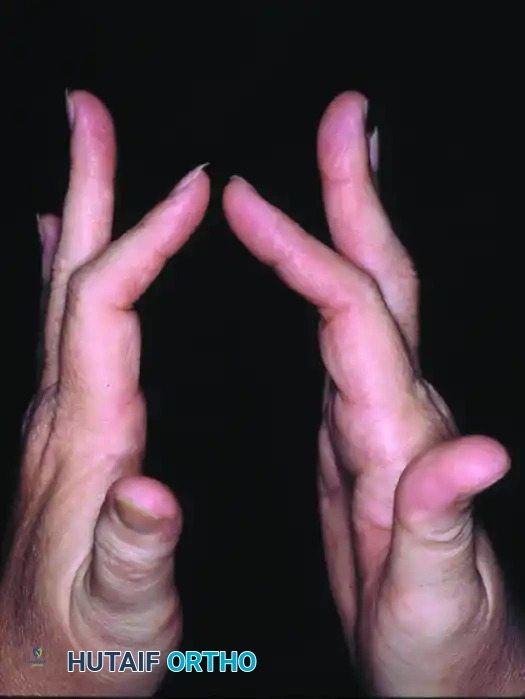
Postoperative clinical presentation demonstrating persistent extensor lag.
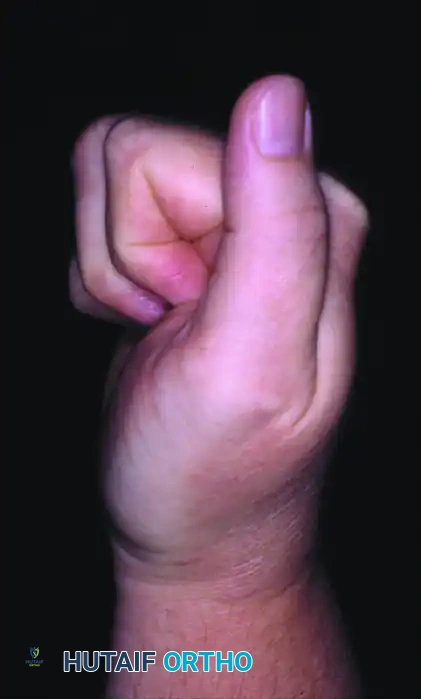
Despite acute repair, an extensor lag of 20 degrees persisted, highlighting the complexity of volar dislocation injuries.
Indications for Tendon Graft Reconstruction
Reconstruction of the PIP joint collateral ligament is indicated in the following scenarios:
* Chronic Instability: Symptomatic varus or valgus instability persisting beyond 6 weeks post-injury, leading to pain on pinch and grip weakness.
* Failed Primary Repair: Recurrent instability following an attempted direct anatomical repair.
* Severe Tissue Loss: Acute injuries with massive soft tissue avulsion or crushing where the native ligament is non-viable.
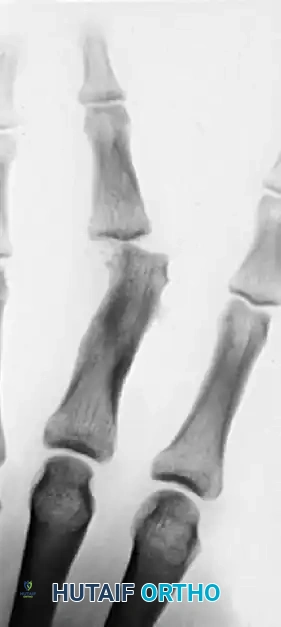
Chronically unstable proximal interphalangeal joint permitting abnormal tilting and producing severe pain during pinch maneuvers.

Restoration of coronal alignment achieved by a segmental graft from the palmaris longus tendon attached through transosseous tunnels.
Alternative Interventions: Dynamic External Fixation
In cases of acute fracture-subluxations where ligamentous reconstruction is not immediately feasible, dynamic external fixation may be employed to maintain joint congruity while allowing early motion.
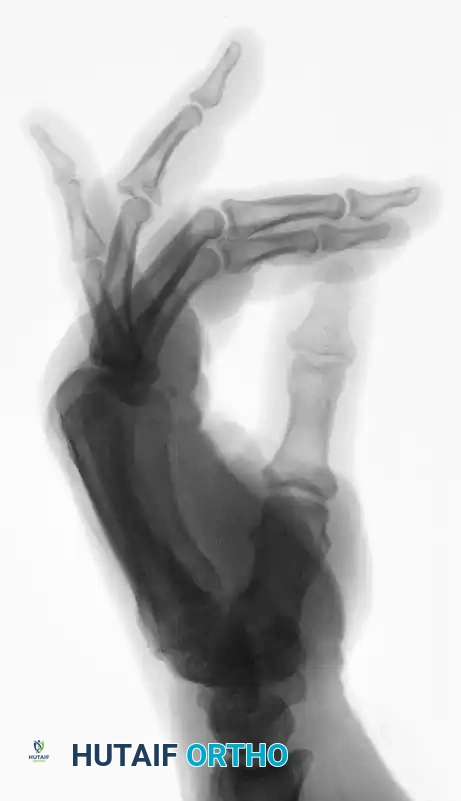
Proximal interphalangeal joint fracture-subluxation.
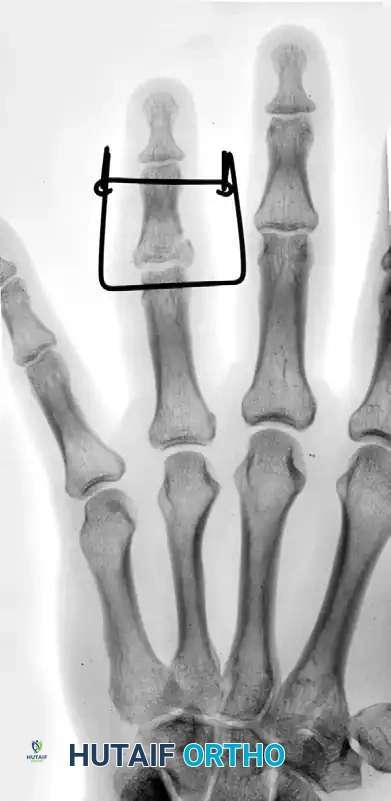
Application of a dynamic external fixator to maintain reduction.
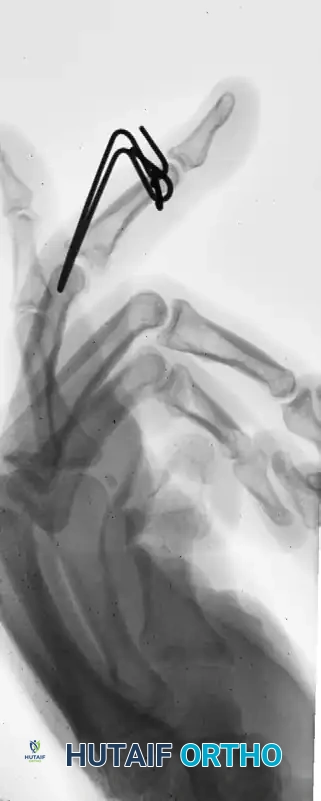
Lateral radiographic view confirming concentric joint reduction with the dynamic external fixator in place.
Preoperative Planning and Positioning
- Anesthesia: Regional block (axillary or supraclavicular brachial plexus block) is preferred to provide excellent intraoperative anesthesia and postoperative analgesia.
- Positioning: The patient is positioned supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A well-padded pneumatic upper arm tourniquet is applied and inflated to 250 mm Hg after exsanguination with an Esmarch bandage to ensure a bloodless surgical field.
- Graft Selection: The palmaris longus tendon is the graft of choice due to its expendability, appropriate caliber, and ease of harvest. Alternative options include a slip of the flexor carpi radialis (FCR) or a toe extensor tendon.
Surgical Technique: Step-by-Step Reconstruction
1. Surgical Approach and Exposure
- Incision: Make a midlateral incision over the proximal interphalangeal joint on the side of the collateral ligament insufficiency. The incision should be centered over the joint line, extending from the mid-proximal phalanx to the mid-middle phalanx.
- Dissection: Carefully dissect through the subcutaneous tissues, taking care to identify and protect the dorsal sensory branches of the digital nerve and the accompanying digital artery.
- Extensor Mechanism Reflection: Identify the transverse retinacular ligament. Incise this ligament longitudinally to mobilize the lateral band. Reflect the extensor mechanism dorsally to expose the underlying joint capsule and the remnants of the collateral ligament.
2. Joint Preparation and Scar Excision
- Debridement: Inspect the joint for any osteochondral fragments or interposed soft tissue. Excise any dense scar tissue from around the anatomical origin (proximal phalanx head) and insertion (middle phalanx base) of the cord fibers of the collateral ligament.
- Preparation of the Bed: Ensure the bony surfaces where the graft will interface are decorticated slightly to promote biological healing of the tendon-to-bone interface.
3. Bone Tunnel Preparation
Precise placement of the bone tunnels is the most critical step to ensure isometric function of the reconstructed ligament.
* Proximal Tunnel: Identify the isometric point on the condyle of the proximal phalanx (slightly dorsal and proximal to the center of rotation). Drill a hole completely through the bone from the injured side to the contralateral side using a 1.5 mm or 2.0 mm drill bit.
* Distal Tunnel: Identify the insertion footprint at the volar-lateral base of the middle phalanx. Drill a second hole completely through the bone on this side of the joint.
4. Graft Harvest
- Palmaris Longus Harvest: Obtain the necessary graft material. Make a small transverse incision at the distal wrist crease over the palmaris longus tendon. Use a tendon stripper to harvest an adequate length of the tendon (typically 6 to 8 cm is required).
- Graft Preparation: Clean the graft of adherent muscle belly or paratenon. Whipstitch both ends of the graft using a non-absorbable 4-0 suture.
5. Graft Passage and Fixation
- Suture/Wire Loop Application: Tie a 4-0 non-absorbable suture or a 34-gauge wire loop around each end of the prepared tendon graft.
- Initial Passage: Bring one end of the graft out through one of the drilled holes (e.g., the proximal phalanx tunnel) to the side opposite the injury.
- Joint Crossing: Pass the other end of the graft across the joint line, mimicking the anatomical trajectory of the native proper collateral ligament, and thread it through the hole in the other bone (middle phalanx) in the appropriate direction.
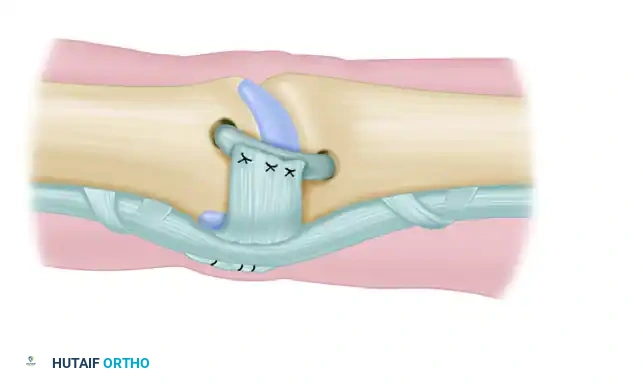
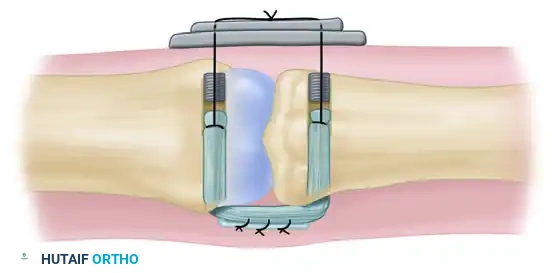
Diagrammatic representation of the reconstruction of the collateral ligament of the proximal interphalangeal joint with a tendon graft. The graft is passed through the transosseous tunnels.
- Button Fixation: Pass each wire loop (or suture ends) on the exiting ends of the graft through a piece of sterile felt (to protect the skin) and then through separate holes in a single sterile button resting on the contralateral intact skin.
- Tensioning: Pull the graft snug to eliminate laxity. Assess the joint for stability and ensure there is no impingement during a trial range of motion. Once optimal tension is achieved, tie the two wires (or sutures) together securely over the button.
6. Creation of an Accessory Collateral Ligament (Optional but Recommended)
To restore the volar stability provided by the accessory collateral ligament and prevent hyperextension:
* Flexor Sheath Utilization: An accessory collateral ligament may be created if necessary. Section a portion of the flexor tendon sheath (typically the A3 pulley or adjacent cruciform tissue) on the side opposite the defect.
* Transposition: Maintain its insertion into the bone on the side of the involved collateral ligament, and fold this fascia-like sheath over the newly grafted tendon.
* Suturing: Suture this sheath tissue to the graft with the finger held in full extension to ensure appropriate tensioning of the volar structures.
Creation of an accessory collateral ligament utilizing a portion of the flexor sheath folded over and sutured to the primary tendon graft.
7. Joint Transfixion and Closure
- K-Wire Stabilization: To protect the reconstruction during the initial phase of biological healing, transfix the PIP joint with an oblique 0.045-inch Kirschner wire (K-wire) with the joint positioned in approximately 20 to 30 degrees of flexion.
- Closure: Repair the transverse retinacular ligament with fine absorbable sutures to prevent dorsal subluxation of the lateral band. Close the skin with interrupted non-absorbable sutures.
- Dressing: Apply a bulky, non-adherent compressive dressing and a volar plaster splint maintaining the PIP joint in the transfixed position and the metacarpophalangeal (MCP) joint in 70 degrees of flexion.
💡 CLINICAL PEARL: Over-tensioning the graft is a common pitfall that leads to severe postoperative stiffness. The graft should be tensioned just enough to eliminate abnormal joint opening under varus/valgus stress, not so tight that it compresses the articular surfaces.
Postoperative Care and Rehabilitation Protocol
The success of a PIP joint collateral ligament reconstruction relies as much on meticulous postoperative rehabilitation as it does on surgical execution.
- Weeks 0 to 3: The finger remains immobilized in the splint. The transarticular K-wire provides rigid protection of the graft. Pin site care is performed weekly.
- Week 3: The transarticular Kirschner wire is removed in the clinic. Active and active-assisted range of motion (ROM) exercises are initiated immediately to prevent tendon adhesions and joint contractures. A buddy strap is applied to the adjacent digit to provide dynamic support during motion.
- Weeks 4 to 6: The pull-out button, felt, and wire loop (or sutures) on the contralateral side of the digit are removed. Passive stretching is gradually introduced if ROM is lagging.
- Weeks 6 to 8: Strengthening exercises are commenced. The buddy strap may be discontinued for light activities but should be worn during strenuous tasks or sports for up to 12 weeks.
Complications and Management
- Joint Stiffness: The most common complication following PIP joint reconstruction. It is mitigated by precise isometric graft placement, avoiding over-tensioning, and strict adherence to the timeline for K-wire removal and initiation of motion.
- Recurrent Instability: Can occur due to graft stretching, premature K-wire removal, or non-isometric tunnel placement. Revision surgery may be required if functional impairment is severe.
- Extensor Lag: Often results from failure to adequately repair the transverse retinacular ligament or from adhesions of the extensor mechanism.
- Pin Tract Infection: Managed with oral antibiotics and local pin care; rarely necessitates premature removal of the K-wire unless deep infection is suspected.
- Skin Necrosis under the Button: Prevented by using an adequately sized piece of felt beneath the button and avoiding excessive tension on the pull-out wires.
By adhering to these rigorous surgical principles and anatomical details, the orthopedic surgeon can reliably restore stability and function to the severely compromised proximal interphalangeal joint.
You Might Also Like