Clavicle Tech Fig: Plate Fixation for Lasting Repair
Key Takeaway
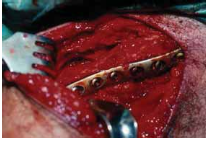
This topic focuses on Clavicle Tech Fig: Plate Fixation for Lasting Repair, Displaced, comminuted clavicle fractures, often resulting from direct blows, risk nonunion and malunion. These can be considered for open reduction and internal fixation using a plate and screws. The risk of nonunion for completely displaced and comminuted fractures is 10-20% (refer to clavicle tech fig 1), potentially causing shoulder deformity or brachial plexus compression.
Introduction and Epidemiology
Clavicle fractures represent a common orthopedic injury, accounting for approximately 2.6% to 4% of all adult fractures and up to 10% of all fractures in the pediatric population. The incidence peaks in young males, typically between 13 and 20 years of age, often associated with high-energy trauma from sports activities or motor vehicle accidents. A secondary peak is observed in elderly females, where low-energy falls from a standing height are more common. While many clavicle fractures can be managed non-operatively with good outcomes, certain fracture patterns carry a significant risk of nonunion and symptomatic malunion, necessitating surgical intervention.
Displaced, comminuted fractures of the clavicle are particularly at risk for nonunion and malunion, with rates varying depending on the literature, but often cited in the range of 10-20% for significantly displaced midshaft fractures managed conservatively. The overall reported nonunion rate for diaphyseal clavicle fractures is approximately 4.5% to 6%, but specific risk factors can elevate this considerably. These risk factors include advanced age, female gender, significant displacement (e.g., >2 cm shortening or 100% displacement), comminution, polytrauma, refracture, and certain lifestyle factors such as smoking. The recognition of these factors has led to an evolving understanding of the indications for open reduction and internal fixation (ORIF) with a plate and screws, shifting the paradigm towards operative management for unstable patterns to restore anatomy and improve functional outcomes.
Surgical Anatomy and Biomechanics
The clavicle is a crucial strut linking the axial skeleton to the upper extremity, acting as a rigid support that holds the upper limb away from the trunk, thereby enhancing the global positioning and extensive range of motion of the limb. This function is particularly important in brachiating animals, underscoring its role in upper limb mobility and mechanical advantage.
The clavicle is named for its distinctive S-shaped curvature, with an apex anteromedially and an apex posterolaterally, resembling the musical symbol clavicula. This unique morphology is functionally significant. The larger medial curvature widens the space for passage of vital neurovascular structures, including the brachial plexus and subclavian vessels, from the neck into the upper extremity through the costoclavicular interval.
Clavicle Morphology and Bone Quality
In cross-section, the clavicle exhibits a gradual change in morphology along its length: a flattened lateral aspect, a more tubular mid-portion, and an expanded, prismatic medial end. This variability dictates optimal plate positioning and screw trajectories. The clavicle is composed of very dense trabecular bone, notably lacking a well-defined medullary canal in its midshaft, which influences intramedullary nail viability and often favors plate fixation for robust stability. The cortical bone, particularly in the midshaft, is relatively thin.
Ligamentous and Muscular Attachments
The clavicle's stability and function are intimately tied to its strong ligamentous and muscular attachments. Laterally, the clavicle articulates with the acromion via the acromioclavicular (AC) joint, stabilized by the AC ligaments and the powerful coracoclavicular (CC) ligaments (conoid and trapezoid). These ligaments are critical for scapular suspension and upper extremity load transmission. Medially, the sternoclavicular (SC) joint, a diarthrodial saddle joint, is supported by strong capsular ligaments, the interclavicular ligament, and the costoclavicular ligament.
Muscular attachments include the sternocleidomastoid superiorly and medially, which can contribute to superior displacement of the medial fragment in midshaft fractures. The pectoralis major inserts inferiorly, while the deltoid attaches anterolaterally and the trapezius posterolaterally. The subclavius muscle originates from the first rib and inserts into the subclavian groove on the inferior aspect of the clavicle.
Neurovascular Structures
The clavicle is subcutaneous throughout its length, contributing prominently to the aesthetic contour of the neck and upper chest. This superficial location, however, places overlying neurovascular structures at risk during surgical exposure. Critically, the supraclavicular nerves, originating from the cervical plexus (C3-C4), run obliquely across the clavicle just superior to the platysma muscle. These nerves provide sensation to the skin over the clavicle, upper chest, and shoulder. Meticulous identification and protection of these nerves during operative exposure are paramount to mitigate the risk of postoperative hyperesthesia, dysesthesia, or anesthesia over the chest wall. Deeper to the clavicle, the subclavian artery and vein, and the cords of the brachial plexus, lie in close proximity to the posterior and inferior aspects of the clavicle, particularly medially. This necessitates careful attention to screw length and trajectory during plate fixation to prevent iatrogenic neurovascular injury.

Indications and Contraindications
The decision for operative versus non-operative management of clavicle fractures is multifactorial, considering fracture morphology, patient demographics, activity level, and associated injuries. The goal of operative fixation is to achieve anatomical reduction, stable internal fixation, facilitate early rehabilitation, and improve functional outcomes, particularly for unstable fracture patterns prone to malunion or nonunion.
Operative Indications
- Midshaft Clavicle Fractures (Group I):
- Significant displacement: Typically >2 cm shortening or 100% displacement (complete cortical apposition loss), which correlate with higher rates of nonunion and functional deficit.
- Extensive comminution: Particularly if leading to significant instability or bone loss.
- Open fractures: Requiring debridement and stabilization.
- Vascular compromise: Rare, but direct neurovascular injury from fracture fragments.
- Polytrauma: Clavicle stabilization may aid overall patient management.
- Floating shoulder: Concomitant ipsilateral scapular neck or glenoid fracture.
- Symptomatic malunion or established nonunion: Requiring revision surgery.
- Bilateral clavicle fractures.
- Lateral clavicle fractures (Group II):
- Neer Type II fractures (fracture medial to the coracoclavicular ligaments with significant displacement of the medial fragment due to the pull of the sternocleidomastoid muscle).
- Neer Type V fractures (comminuted lateral fragment with intact coracoclavicular ligaments).
- Medial clavicle fractures (Group III):
- Significant displacement or sternoclavicular joint instability.
- Posterior displacement with compromise of mediastinal structures (rare, constitutes an orthopedic emergency).
Non-Operative Indications
- Minimally displaced or nondisplaced midshaft clavicle fractures.
- Greenstick or torus fractures in children.
- Certain stable lateral clavicle fractures (e.g., Neer Type I, III, IV).
- Stable medial clavicle fractures.
- Patients with significant comorbidities precluding safe surgical intervention.
- Patient preference after thorough discussion of risks and benefits of both treatment modalities.
Contraindications
- Active infection at the surgical site.
- Severe overlying skin compromise (e.g., crush injury, severe abrasion, burn) that may preclude safe wound closure or increase infection risk.
- Significant medical comorbidities that make the patient an unacceptable anesthetic or surgical risk.
- Skeletal immaturity (relative contraindication for specific physeal fractures; careful consideration required).
- Non-displaced or stable fracture patterns where the risks of surgery outweigh the benefits.
Operative vs. Non-Operative Indications Summary
| Feature | Operative Indications | Non-Operative Indications |
|---|---|---|
| Midshaft Fractures | >2 cm shortening, >100% displacement, significant comminution, open fractures, neurovascular compromise, floating shoulder, polytrauma, symptomatic malunion/nonunion, bilateral fractures. | Minimally displaced fractures, non-displaced fractures, stable comminuted fractures without significant shortening, greenstick fractures in children. |
| Lateral Fractures | Neer Type II (fracture medial to CC ligaments), Neer Type V (comminuted with intact CC ligaments, but unstable). | Neer Type I (nondisplaced), Neer Type III (AC joint disruption but CC ligaments intact), Neer Type IV (pediatric, superior displacement of distal fragment through periosteal sleeve). |
| Medial Fractures | Significant displacement or instability of SC joint, posterior displacement with mediastinal compromise. | Nondisplaced or stable displaced fractures, physeal injuries (conservative in skeletally immature patients unless posterior displacement/mediastinal compromise). |
| Patient Factors | High-demand patients, failed conservative treatment, anticipated high risk of nonunion/malunion based on fracture pattern and patient factors (e.g., smoking, obesity, advanced age for specific fracture types). | Significant medical comorbidities precluding surgery, patient preference (after informed discussion), low-demand patients with stable patterns, young patients with high remodeling potential for minor displacements. |
| Associated Injuries | Floating shoulder (ipsilateral scapular neck/glenoid fracture), associated significant soft tissue injury (e.g., skin tenting at risk of open fracture conversion), impending skin breakdown from fragment prominence, neurovascular compromise due to fracture fragments (rare). | No other associated injuries requiring surgical intervention, stable soft tissue envelope. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is crucial for successful clavicle ORIF, minimizing complications, and optimizing outcomes.
Preoperative Assessment and Imaging
A comprehensive clinical assessment begins with a detailed history of the injury mechanism and patient medical comorbidities. A physical examination must carefully evaluate the neurovascular status of the ipsilateral upper extremity, including pulses, capillary refill, and motor/sensory function, particularly of the brachial plexus. Special attention should be paid to skin integrity over the fracture site due to the subcutaneous nature of the clavicle.
Standard imaging includes an anteroposterior (AP) view of the clavicle, a 30-degree cephalic tilt view (serendipity view), and potentially a true lateral view. For complex fracture patterns, significant comminution, lateral or medial clavicle involvement, nonunion assessment, or suspected concomitant injuries (e.g., rib fractures, pneumothorax), a computed tomography (CT) scan is invaluable. A CT with 3D reconstructions can precisely delineate fracture morphology, displacement, comminution, and the relationship of fragments to critical neurovascular structures, aiding in plate contouring and screw trajectory planning.
Plate Selection and Surgical Strategy
The choice of fixation device depends on the fracture pattern. Contoured locking compression plates (LCPs) are generally preferred due to their angular stable fixation, which is advantageous in comminuted fractures or osteoporotic bone. Plates designed specifically for the clavicle are available and can be placed on the superior or anterosuperior surface. Biomechanically, superior plating is generally stronger, as it better resists bending moments in the sagittal plane. However, anterosuperior plating may offer a lower profile and potentially reduce hardware prominence. For highly comminuted fractures, bridge plating principles are applied, while for simpler transverse or oblique patterns, compression plating or lag screw fixation through the plate may be employed.
Preoperative templating with X-rays or CT models helps in selecting the appropriate plate length and pre-contouring the plate if a non-anatomically contoured plate is used. The number of screws on each side of the fracture should be sufficient to achieve stable fixation, typically at least three bicortical screws per main fragment, aiming for six cortices. For comminuted fractures, longer plates spanning a greater segment of the clavicle are often necessary to achieve adequate working length for bridge plating and distribute stress. Consideration should be given to bone graft (autograft or allograft) for cases with significant bone loss, large comminution, or established nonunion.
Patient Positioning
The patient is typically positioned in a supine or semi-recumbent (beach chair) position. A radiolucent bolster or towel roll placed longitudinally between the scapulae is often beneficial. This maneuver retracts the shoulders posteriorly, making the clavicle more prominent and facilitating easier access to the anterior aspect of the clavicle. The ipsilateral arm should be prepped and draped free to allow for intraoperative manipulation for reduction and assessment of motion. Image intensifier (fluoroscopy) access should be confirmed before sterile draping, ensuring clear AP and oblique views of the entire clavicle.

Detailed Surgical Approach and Technique
The goal of clavicle ORIF is anatomical reduction and rigid internal fixation, minimizing soft tissue stripping, and protecting vital neurovascular structures.
Incision and Exposure
The choice of incision is critical. A transverse or slightly oblique incision, centered directly over the fracture site, typically provides adequate exposure and may result in a more aesthetically favorable scar along Langer's lines. The length of the incision should be sufficient to allow for plate application with adequate working length for screw insertion, typically 5-8 cm.
Careful incision through the skin and subcutaneous tissues is performed. The platysma muscle lies immediately deep to the subcutaneous fat. This muscle should be incised sharply in line with the skin incision. It is paramount to identify and protect the supraclavicular nerves, which originate from the cervical plexus (C3-C4) and typically cross the clavicle obliquely from superomedial to inferolateral. These nerves are usually located just superior to the platysma. Minimal dissection inferiorly along the clavicle and cautious retraction should be employed to reduce the risk of traction neuropraxia or direct injury to these sensory nerves, which can lead to bothersome dysesthesia or hyperesthesia in the distribution over the chest wall.
After incising the platysma, the fracture hematoma is encountered. Sharp dissection is used to open the fracture site, carefully incising the periosteum directly over the fracture. Extensive periosteal stripping should be avoided to preserve vascularity to the bone fragments, which is essential for fracture healing. Gentle self-retaining retractors can be used to hold soft tissues apart, exposing the fracture fragments.

Fracture Reduction
Reduction of clavicle fractures can be achieved through a combination of indirect and direct techniques.
1. Indirect Reduction: Traction on the ipsilateral arm, along with external rotation and abduction, can help restore length and align the fragments. Manipulating the fragments manually can also achieve gross reduction.
2. Direct Reduction: For precise anatomical reduction, pointed reduction clamps or Verbrugge clamps are often employed. These clamps are carefully applied to the main fracture fragments to achieve anatomical length, rotation, and translation. Fluoroscopy is used to confirm optimal alignment. Once satisfactory reduction is achieved, it can be temporarily maintained with K-wires inserted percutaneously or directly into the fragments away from the planned plate path. This provisional fixation frees up hands for plate application.
Plate Application and Fixation
Plate Choice: Contoured locking compression plates (LCPs) designed for the clavicle are the standard. These plates are available in various lengths and contours (e.g., superior, anterosuperior). The superior aspect of the clavicle is generally preferred for plate placement as it provides biomechanically stronger fixation and has a broader, flatter surface. Anterosuperior placement can be considered for specific fracture patterns or to mitigate hardware prominence risks.
Contouring: While many plates are pre-contoured, minor adjustments may be necessary to perfectly match the S-shape of the patient's clavicle. Careful contouring ensures the plate lies flush against the bone, distributing stress evenly and preventing soft tissue irritation.
Fixation Principles:
1. Bridge Plating: For comminuted fractures, the plate acts as a bridge, spanning the comminuted zone without requiring direct reduction of all small fragments. The goal is to restore length and axial alignment of the main proximal and distal fragments.
2. Compression Plating: For simple transverse or short oblique fractures, interfragmentary compression can be achieved by eccentrically placing the first screw, or by using dedicated compression holes if available on the plate, to bring the fracture ends together.
3. Lag Screws: For long oblique or spiral fractures, lag screws can be inserted independently or through the plate to achieve interfragmentary compression, enhancing stability. This should be performed before locking screw insertion.
4. Screw Selection and Trajectory: Locking screws provide angular stability and are particularly beneficial in comminuted fractures or osteoporotic bone. At least three bicortical screws should be placed in each main fragment (proximal and distal to the fracture), totaling at least six cortices. Screw length is critical, especially in the medial clavicle where the subclavian vessels and brachial plexus lie immediately inferiorly and posteriorly. Fluoroscopic guidance, particularly in the lateral view, helps confirm appropriate screw length, avoiding penetration of the posterior cortex into mediastinal structures or neurovascular bundles. With superior plating, it's generally advised to aim screws slightly anteriorly to avoid deep posterior penetration.
Surgical Steps:
1. Once the fracture is reduced and provisionally fixed, place the appropriately contoured plate onto the superior or anterosuperior surface of the clavicle.
2. Secure the plate temporarily with K-wires through plate holes or with reduction clamps.
3. Drill, measure, and insert screws, starting with the outer holes of the plate on each side to secure length and rotation. Progress toward the fracture site.
4. For locking plates, use the drill guide to ensure proper screw trajectory. Drill to the appropriate depth, measure, and insert the locking screws.
5. Confirm reduction, plate position, and screw length and trajectory with fluoroscopy in multiple planes (AP and 30-degree cephalic tilt views). Ensure no screw penetration into critical structures.
6. If there are significant bone defects or in cases of nonunion, consider applying autogenous bone graft (e.g., from the iliac crest) or allograft to enhance biological healing.

Wound Closure
After achieving satisfactory fixation and confirming stability, the wound is thoroughly irrigated. Hemostasis is achieved. The platysma muscle is carefully closed with absorbable sutures to reconstruct the muscle layer. This helps reduce dead space and provides a barrier for the supraclavicular nerves. The subcutaneous tissues are closed with absorbable sutures, and the skin is closed with fine sutures, staples, or adhesive strips, aiming for a cosmetically acceptable scar.

Complications and Management
Despite advancements in surgical technique and implant design, clavicle ORIF is not without potential complications. A thorough understanding of these complications and their management is essential for the orthopedic surgeon.
Specific Complications of Clavicle ORIF
| Complication | Incidence | Salvage Strategies |
|---|---|---|
| Nonunion | 2-10% (post-ORIF) | Revision ORIF with larger, stronger plate and bone grafting (autograft or allograft), potentially adding an intramedullary device. Addressing underlying causes (e.g., smoking cessation, infection control, improved stability). |
| Malunion (symptomatic) | 5-15% (post-ORIF) | Corrective osteotomy and revision ORIF to restore length and alignment. |
| Hardware Prominence / Irritation | 10-30% | Hardware removal after complete fracture union (typically 12-18 months post-op). Can be a significant issue due to the subcutaneous nature of the clavicle. |
| Supraclavicular Nerve Injury | 10-25% (dysesthesia) | Often transient, managed conservatively with observation and neuropathic pain medications (e.g., gabapentin, pregabalin). Persistent, severe dysesthesia may rarely warrant neurolysis or neurectomy, though outcomes are variable. Prevention is key (meticulous dissection, minimal retraction). |
| Infection | 1-5% | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics, irrigation. If union is achieved, hardware removal. If nonunion, may require hardware removal, thorough debridement, and reimplantation with new hardware and bone graft after infection control. |
| Implant Failure / Refracture | <5% | Revision ORIF with stronger construct (longer plate, more screws), bone grafting if bone quality is poor or union is delayed. Addressing patient factors such as premature weight-bearing or trauma. |
| Pneumothorax / Hemothorax | Rare (<1%) | Chest tube insertion for drainage. Careful screw length measurement and fluoroscopic guidance, especially for medial clavicle screws, are crucial for prevention. |
| Brachial Plexus / Vascular Injury | Extremely Rare | Immediate surgical exploration, repair of injured structures (vascular surgery consult), neurolysis/nerve repair. Prevention is paramount through meticulous surgical technique, careful drilling, and appropriate screw length selection with fluoroscopic control, particularly for the posterior cortex of the medial clavicle. |
| Cosmetic Dissatisfaction | Variable | Scar revision or camouflage techniques. Patient counseling on scar formation preoperatively. |
General Surgical Complications
Beyond the specific complications, patients undergoing clavicle ORIF are also at risk for general surgical complications, including:
* Bleeding: Usually well-controlled, but hematoma formation can occur.
* Anesthesia risks: Standard risks associated with general or regional anesthesia.
* Complex Regional Pain Syndrome (CRPS): Rare, but can be debilitating. Early recognition and multidisciplinary pain management are essential.
Prevention remains the cornerstone of complication management. Meticulous surgical technique, careful patient selection, comprehensive preoperative planning, and adherence to postoperative protocols significantly reduce the incidence of adverse events. Prompt recognition and appropriate management are critical for optimizing patient outcomes when complications do arise.
Post Operative Rehabilitation Protocols
A structured and progressive postoperative rehabilitation protocol is crucial following clavicle plate fixation to optimize functional recovery, restore range of motion, and facilitate return to activity, while protecting the healing fracture. The timeline and specific exercises may be individualized based on fracture stability, extent of comminution, bone quality, and surgeon preference.
Phase 1: Immediate Postoperative Period (Weeks 0-2)
- Goals: Pain control, protect surgical repair, minimize stiffness in adjacent joints, promote wound healing.
- Immobilization: Arm in a sling for comfort and protection, worn continuously except for exercises and hygiene.
- Activity:
- No active shoulder range of motion (ROM) of the operative arm.
- Gentle pendulum exercises for the shoulder (gravity-assisted motion without muscle activation).
- Active ROM of the elbow, wrist, and hand to prevent stiffness and promote circulation.
- Scapular setting exercises (gentle retraction and protraction) to maintain scapulothoracic rhythm.
- Avoid lifting, pushing, pulling, or supporting body weight with the operative arm.
- Wound Care: Keep incision clean and dry. Monitor for signs of infection.
Phase 2: Early Mobilization (Weeks 2-6)
- Goals: Gradually restore passive and active-assisted shoulder ROM, maintain protected healing.
- Immobilization: Sling discontinued as comfort allows, typically by 3-4 weeks.
- Activity:
- Initiate passive range of motion (PROM) and active-assisted range of motion (AAROM) for shoulder flexion, abduction, and external rotation, respecting pain limits. This can be performed with the unaffected arm or by a therapist.
- Continue pendulum exercises and scapular mobilization.
- Gentle isometric exercises for the rotator cuff and deltoid, without resistance.
- Begin light functional activities of daily living (ADLs), avoiding overhead reaching or lifting.
- Precautions: Avoid active, unresisted shoulder abduction or flexion beyond 90 degrees initially. No heavy lifting, pushing, or pulling. Avoid direct pressure on the clavicle.
Phase 3: Intermediate Strengthening (Weeks 6-12)
- Goals: Restore full active shoulder ROM, begin progressive strengthening, improve endurance.
- Imaging: Radiographic assessment of fracture union typically performed around 6-8 weeks.
- Activity:
- Progress to active range of motion (AROM) exercises for the shoulder in all planes.
- Initiate light resistance strengthening exercises for the rotator cuff (internal/external rotation), deltoid, and scapular stabilizers (e.g., resistance bands, light weights).
- Gradual progression of weight-bearing and functional activities.
- Low-impact cardiovascular exercise (e.g., walking, stationary bike).
- Precautions: Continue to avoid heavy lifting or high-impact activities. Progress resistance slowly and only with good form.
Phase 4: Advanced Strengthening and Return to Activity (Months 3-6+)
- Goals: Maximize strength, power, and endurance; return to sport-specific or work-specific activities.
- Activity:
- Progressive resistive exercises with increasing weights and resistance levels.
- Plyometric exercises and sport-specific drills as appropriate.
- Emphasis on proprioception and neuromuscular control.
- Gradual return to full activities, including overhead sports, typically between 4-6 months, provided radiographic union is confirmed and strength is symmetrical.
- Hardware Removal: Hardware removal is typically considered after 12-18 months, or once full union is achieved and symptoms of hardware prominence or irritation become bothersome. It is not routinely performed.
Throughout all phases, patient education regarding the importance of adherence to the protocol, proper body mechanics, and warning signs of complications is essential. Close collaboration between the surgeon and physical therapist ensures optimal progression and prevents overstressing the healing fracture.
Summary of Key Literature and Guidelines
The management of clavicle fractures, particularly midshaft injuries, has evolved significantly over the past two decades, with a growing body of evidence supporting operative fixation for specific fracture patterns. Historically, non-operative management was the mainstay, often with good outcomes for minimally displaced fractures. However, meta-analyses and randomized controlled trials (RCTs) have highlighted superior outcomes with surgical intervention for significantly displaced and comminuted midshaft clavicle fractures.
Evidence for Operative Fixation
Several seminal studies have shaped current practice:
* Canadian Orthopaedic Trauma Society (COTS) Trial (2007): This multicenter RCT compared plate fixation to non-operative treatment for displaced midshaft clavicle fractures. It demonstrated significantly higher rates of nonunion (18% vs. 2%) and symptomatic malunion in the non-operative group. Operative fixation led to earlier functional recovery and higher Constant scores at 1 year. This study was a major catalyst for the paradigm shift towards operative management for significantly displaced midshaft fractures.
* Meta-analyses: Numerous meta-analyses have consistently confirmed that ORIF with plate and screws for displaced midshaft clavicle fractures results in lower rates of nonunion, improved functional outcomes (e.g., Constant score, DASH score), and reduced rates of symptomatic malunion compared to non-operative treatment.
* Indications Consensus: While exact thresholds vary, a consensus has emerged for operative indications including >2 cm shortening, >100% displacement, significant comminution, open fractures, and polytrauma. These criteria are based on studies correlating these fracture characteristics with poor conservative outcomes.
Plate Fixation Biomechanics and Techniques
- Superior vs. Anterosuperior Plating: Biomechanical studies generally indicate that superior plate fixation provides greater stiffness and strength compared to anterosuperior or anterior plating, particularly in resisting bending and torsional forces. However, anterosuperior plating may offer a lower profile, potentially reducing hardware prominence, which remains a common complaint due to the subcutaneous nature of the clavicle.
- Locking Plate Technology: The advent of locking compression plates (LCPs) has enhanced fixation stability, especially in comminuted fractures or osteoporotic bone, by creating an angular stable construct. This allows for bridge plating techniques without relying solely on screw purchase in potentially compromised bone segments.
- Complication Rates: While operative fixation reduces nonunion and malunion rates, it introduces surgical risks. Hardware-related issues (prominence, irritation) are the most common complication, often necessitating hardware removal. Supraclavicular nerve dysesthesia, while often transient, is also frequently reported. Serious complications such as infection, neurovascular injury, or pneumothorax are rare but require meticulous surgical technique for prevention.
Guidelines and Future Directions
Major orthopedic societies, such as the American Academy of Orthopaedic Surgeons (AAOS) and the AO Foundation, provide guidelines that reflect this evidence-based shift, recommending surgical intervention for unstable and significantly displaced clavicle fractures to optimize patient outcomes.
Future research continues to explore refined surgical techniques, novel implant designs (e.g., intramedullary devices, resorbable implants), and patient-specific factors influencing outcomes. The role of biologics (e.g., PRP, bone marrow aspirate) in augmenting healing, particularly in high-risk patients or for nonunions, is also an active area of investigation.
In conclusion, plate fixation for clavicle fractures has become an established and highly effective treatment modality for specific unstable fracture patterns. By achieving anatomical reduction and stable internal fixation, it reliably improves functional outcomes, reduces the incidence of nonunion and symptomatic malunion, and facilitates a timely return to activity for appropriately selected patients. Adherence to sound surgical principles and comprehensive postoperative rehabilitation protocols remains paramount for successful results.
You Might Also Like


