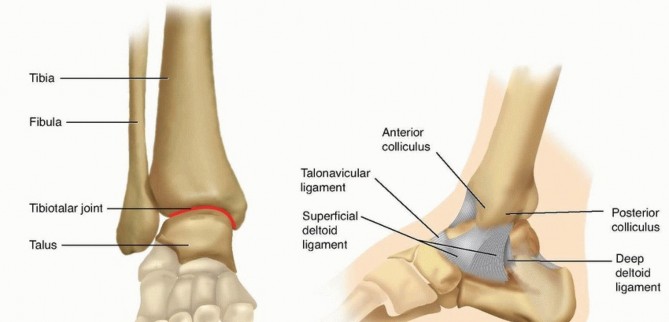
Complex OTA/AO 43-C3 Pilon Fracture: A Detailed Orthopedic Case Study
Key Takeaway
A pilon fracture, specifically an OTA/AO 43-C3, involves a comminuted intra-articular fracture of the distal tibia due to high-energy axial load. Diagnosis relies on plain radiographs and detailed CT scans to assess articular involvement, fragment displacement, and comminution. This guides pre-operative planning, crucial for anatomical reduction and successful management of severe ankle trauma.
Patient Presentation and History
A 42-year-old male, previously fit and active with no significant medical comorbidities or pertinent past surgical history, presented to the emergency department following a fall from a height of approximately 4 meters. The patient reported landing directly on his feet. He experienced immediate, severe pain and deformity in his right ankle, rendering him unable to bear weight. There was no reported loss of consciousness or other systemic injuries. He denied any neurovascular symptoms distal to the ankle at the scene, though increasing swelling was noted. Smoking history was negative.
Mechanism of Injury and Energy Transfer
The mechanism of injury is a classic high-energy axial load combined with a rotational or sheer force vector. In this specific presentation, the talus acts as a hammer, driven forcefully into the tibial plafond. The position of the foot at the exact moment of impact dictates the fracture pattern. A neutrally positioned foot typically results in a Y-shaped or T-shaped fracture pattern with central impaction. An anteriorly positioned foot (dorsiflexion) tends to cause an anterior apical fracture, while a plantarflexed foot drives the force posteriorly, creating a large posterior malleolar (Volkmann) fragment. Given the profound comminution and central depression observed in this patient, a direct axial load with the foot in neutral to slight dorsiflexion is the most probable biomechanical mechanism.
Prehospital and Trauma Bay Assessment
Emergency medical services immobilized the extremity in a rigid splint at the scene. Upon arrival at the trauma bay, the patient was evaluated according to Advanced Trauma Life Support protocols. The primary survey was intact, with the patient maintaining a patent airway, normal respiratory effort, and hemodynamic stability. The secondary survey was isolated to the right lower extremity. Concomitant injuries frequently associated with axial loading mechanisms, such as calcaneus fractures, tibial plateau fractures, and thoracolumbar burst fractures, were systematically ruled out through clinical examination and subsequent radiographic screening.
Clinical Examination Findings
Upon initial assessment, the patient was hemodynamically stable. Local examination of the right ankle revealed gross deformity with significant swelling and ecchymosis, consistent with a high-energy injury. The skin over the anteromedial aspect of the ankle was severely distended, blanched, and showed impending tenting, with a developing blister laterally. There was no obvious open wound, but the skin appeared compromised (Tscherne C2-C3).
Inspection of the Soft Tissue Envelope
Marked ankle swelling and ecchymosis extended proximally into the distal third of the leg and distally into the midfoot. Anterior skin tension presented with a tense, non-compressible soft tissue envelope. There was a complete absence of a "wrinkle sign," suggesting profound interstitial edema and compartment swelling. A palpable bony prominence was noted medially, corresponding to the displaced medial malleolus threatening the overlying skin. The rapid development of fracture blisters—both clear fluid-filled (indicating epidermal-dermal separation) and blood-filled (indicating deeper dermal plexus injury)—further underscored the severity of the soft tissue trauma.
Palpation and Compartment Assessment
Diffuse tenderness was elicited throughout the ankle joint and distal tibia, with marked point tenderness over the anterior compartment. Crepitus was noted with any inadvertent micro-motion. A critical component of the examination was the assessment for acute compartment syndrome. While the anterior compartment was tense, it remained compressible. Delta-p measurements were not immediately indicated as the patient was awake, alert, and capable of participating in a reliable clinical examination, but a low threshold for intracompartmental pressure monitoring was established.
Range of Motion and Motor Function
Actively and passively, ankle dorsiflexion, plantarflexion, inversion, and eversion were severely restricted and exquisitely painful. Due to pain and swelling, a comprehensive assessment of individual muscle strength was challenging. However, the patient could weakly attempt dorsiflexion against gravity, indicating some initial function of the anterior tibialis. The strength of the anterior tibialis was estimated at 3/5, accompanied by significant guarding. Extensor hallucis longus and extensor digitorum longus function were similarly intact but limited by pain.
Neurological and Vascular Status
Peripheral pulses, specifically the dorsalis pedis and posterior tibial arteries, were initially palpable but required careful, continuous monitoring as swelling progressed. Capillary refill at the digits was brisk, occurring in under two seconds. Sensation to light touch and pinprick was intact across all major dermatomes of the foot, including the territories supplied by the superficial peroneal, deep peroneal, sural, saphenous, and medial/lateral plantar nerves. The deep peroneal nerve function, particularly vulnerable in anterior compartment swelling, was clinically intact, confirmed by sensory discrimination in the first dorsal web space.
Imaging and Diagnostics
Initial radiographic assessment was performed in the emergency department to establish the preliminary diagnosis and guide immediate stabilization efforts.
Plain Radiographic Evaluation
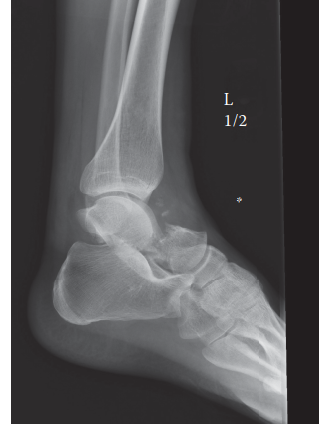
Anteroposterior, lateral, and mortise views of the right ankle demonstrated a highly comminuted intra-articular fracture of the distal tibia, extending into the tibial plafond. Significant articular depression and metaphyseal comminution were evident. There was an associated transverse fibular fracture approximately 5 cm proximal to the ankle joint, accompanied by lateral talar subluxation. The overall pattern was consistent with a high-energy axial load injury. The mortise appeared significantly widened, suggesting syndesmotic disruption and loss of the lateral collateral ligamentous restraint.

Computed Tomography and Three Dimensional Mapping
Following initial stabilization and application of a spanning external fixator, a high-resolution Computed Tomography scan of the ankle with fine 1mm axial cuts and multiplanar reconstructions (coronal and sagittal) was obtained. CT imaging is mandatory in the evaluation of pilon fractures to delineate the extent of articular involvement, fragment displacement, and comminution for precise pre-operative planning.
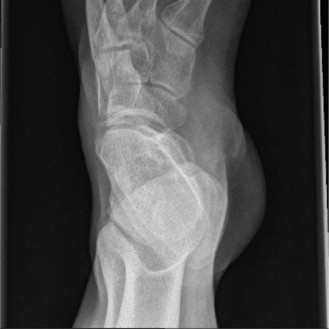
The CT confirmed an OTA/AO 43-C3 pilon fracture with extensive articular depression and displacement of the central die-punch fragments. The articular surface was shattered into the classic three primary fragments described by Topliss et al., the medial malleolus, the anterolateral (Chaput) fragment, and the posterolateral (Volkmann) fragment, alongside severe central impaction. The sagittal reconstructions revealed a 12mm articular step-off and a large central void in the metaphyseal bone where the cancellous bone had been crushed by the impacting talus. The coronal views highlighted the severe varus angulation of the distal tibia and the impaction of the medial shoulder of the talus into the medial plafond.
Preoperative Templating and Surgical Planning
Digital templating was utilized to plan the definitive reconstruction. The primary goal identified was the restoration of the articular block, followed by the attachment of this reconstructed block to the tibial diaphysis. The CT scan allowed for the precise mapping of required surgical approaches. The presence of a large anterolateral fragment necessitated an anterolateral approach, while the medial comminution and extension required a supplementary posteromedial or direct medial approach to address the medial column and prevent varus collapse.
Differential Diagnosis
While the diagnosis of a pilon fracture is readily apparent on plain radiographs, differentiating the exact nature of the injury from other complex ankle trauma is critical for surgical planning and prognostic accuracy. The high-energy nature of the injury requires a thorough evaluation to distinguish between severe rotational injuries and true axial load injuries.
| Diagnostic Consideration | Mechanism of Injury | Radiographic Hallmarks | Articular Involvement | Soft Tissue Compromise |
|---|---|---|---|---|
| OTA/AO 43 Pilon Fracture | High-energy axial loading, often with a rotational component (e.g., fall from height, motor vehicle collision). | Metaphyseal comminution, primary fracture lines extending proximal to the joint line, significant central articular impaction (die-punch). | Severe. Disruption of the weight-bearing tibial plafond. | High risk of severe compromise, blistering, compartment syndrome, and necrosis. |
| OTA/AO 44 Trimalleolar Ankle Fracture | Low to moderate-energy rotational forces (e.g., severe twisting injury, sports trauma). | Fractures of the medial, lateral, and posterior malleoli. Fracture lines typically do not extend significantly into the tibial metaphysis. | Moderate. Involves the malleolar articular surfaces but spares the central weight-bearing dome of the plafond. | Moderate. Swelling is common, but massive soft tissue devitalization or fracture blisters are less frequent than in pilon injuries. |
| OTA/AO 81 Talar Body Fracture | High-energy axial load directed through the talus against the tibial plafond. | Fracture lines through the talar dome or body. The tibial plafond remains relatively intact, while the talus absorbs the impact energy. | Severe. Disruption of the talocrural and subtalar joints. | High risk. Often associated with significant swelling and a high risk of avascular necrosis of the talus. |
Surgical Decision Making and Classification
The management of complex pilon fractures requires a careful balance between the necessity for anatomic articular reduction and the biological constraints of a severely traumatized soft tissue envelope.
Fracture Classification Systems
This injury is classified as an OTA/AO 43-C3 fracture. The "43" designates the distal tibia segment. The "C" indicates a complete articular fracture, meaning the articular surface is completely separated from the diaphysis. The "3" signifies multifragmentary metaphyseal and articular comminution. Under the classic Rüedi-Allgöwer classification system, this represents a Type III injury, characterized by significant comminution and displacement of the weight-bearing articular surface.
Operative Versus Non Operative Management
Non-operative management for an OTA/AO 43-C3 pilon fracture with significant articular displacement and metaphyseal instability is strictly contraindicated. Conservative treatment in this scenario would inevitably lead to rapid post-traumatic arthrosis, severe varus or valgus deformity, ankle stiffness, and profound functional disability. Operative intervention is mandated to restore articular congruity, re-establish the mechanical axis of the lower extremity, and provide stable fixation to allow for early range of motion.
The Staged Damage Control Orthopedics Approach
Historically, immediate definitive open reduction and internal fixation of high-energy pilon fractures resulted in catastrophic soft tissue complication rates, including deep infection, wound dehiscence, and osteomyelitis, often culminating in amputation. Consequently, the standard of care has shifted to a staged protocol, often referred to as "Span, Scan, and Plan."
The decision was made to proceed with a two-stage approach. Stage one involves immediate closed reduction and application of a joint-spanning external fixator. This achieves length, alignment, and rotation, thereby relieving pressure on the compromised soft tissue envelope and allowing the edema to subside. Stage two, definitive open reduction and internal fixation, is delayed until the soft tissue envelope has adequately recovered, typically indicated by the return of skin wrinkles (the "wrinkle sign"), epithelialization of fracture blisters, and resolution of pitting edema. This delay generally ranges from 10 to 21 days post-injury.
Surgical Technique and Intervention
The surgical execution for this complex OTA/AO 43-C3 pilon fracture was divided into two distinct operative events, adhering strictly to the principles of damage control orthopedics followed by meticulous articular reconstruction.
Stage One Spanning External Fixation
The patient was taken to the operating room on the day of admission. Under general anesthesia, the right lower extremity was prepped and draped in standard sterile fashion. The initial goal was to restore the mechanical axis and offload the articular surface.
A delta-frame construct was chosen for its biomechanical stability. Two 5.0mm Schanz pins were placed in the proximal tibial diaphysis, well outside the anticipated zone of definitive fixation. A centrally threaded transcalcaneal pin was placed from medial to lateral, taking care to avoid the neurovascular bundle medially. A transmetatarsal pin was placed through the bases of the first and second metatarsals to control equinus.
Longitudinal traction was applied to restore length, and the frame was assembled using carbon fiber rods and multi-pin clamps. Fluoroscopic imaging confirmed restoration of tibial length, coronal and sagittal alignment, and distraction across the ankle joint. The decision was made to defer fibular fixation at this stage, as immediate open reduction of the fibula through compromised lateral soft tissues carries an unacceptable risk of wound breakdown, and the external fixator provided sufficient temporary stability.

Stage Two Definitive Open Reduction and Internal Fixation
Fourteen days post-injury, clinical evaluation revealed a positive wrinkle sign and resolution of the fracture blisters. The patient was returned to the operating room for definitive osteosynthesis.
Patient Positioning and Preoperative Preparation
The patient was positioned supine on a radiolucent flat Jackson table. A bump was placed under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus and anterolateral tibia into a more accessible position. A thigh tourniquet was applied but not inflated initially. The external fixator was prepped into the surgical field to maintain length during the initial exposure, after which it was systematically removed.
Surgical Approaches
Given the fracture morphology demonstrated on the preoperative CT, a dual-incision technique was employed.
- Anterolateral Approach: An incision was made centered over the distal tibia, approximately 1 cm lateral to the tibial crest, extending distally toward the base of the fourth metatarsal. The superficial peroneal nerve was identified and protected. The extensor retinaculum was incised, and the interval between the extensor digitorum longus and the anterior compartment musculature was developed. The neurovascular bundle (deep peroneal nerve and anterior tibial artery) was gently retracted medially. This approach provided excellent visualization of the Chaput fragment and the central articular impaction.
- Posteromedial Approach: To address the severe medial column comminution and prevent varus collapse, a posteromedial approach was utilized. An incision was made midway between the posterior border of the medial malleolus and the Achilles tendon. The tibialis posterior tendon sheath was incised, and the tendon was retracted anteriorly, allowing direct access to the posterior aspect of the medial malleolus and the posteromedial metaphyseal extension.
Articular Reduction Techniques
The surgical strategy followed the "outside-in" principle. The articular reconstruction began with the reduction of the fibula. An open reduction and internal fixation of the fibula was performed using a 1/3 tubular plate and 3.5mm cortical screws. Restoring the fibula to its anatomic length re-established the lateral column and provided a template for the tibial reduction via the syndesmotic ligaments.
Attention was then turned to the tibial plafond. The anterolateral capsule was incised to directly visualize the joint surface. A femoral distractor was applied with pins in the talar neck and the proximal tibial diaphysis to provide joint distraction and visualization.
The central die-punch fragments were carefully elevated using a Freer elevator and a dental pick. The articular surface was reassembled like a mosaic, referencing the intact portion of the talar dome. The Chaput fragment was reduced to the Volkmann fragment, and the medial malleolus was brought into alignment. Provisional fixation was achieved using multiple 1.6mm and 2.0mm Kirschner wires placed parallel to the joint surface. Fluoroscopy in multiple planes confirmed anatomic restoration of the articular congruity.
Metaphyseal Void Management and Bone Grafting
The elevation of the impacted central articular fragments created a significant metaphyseal void. To prevent late articular subsidence, this void required structural support. Demineralized bone matrix combined with cancellous allograft chips was tightly packed into the defect, providing a scaffold for osteoconduction and mechanical support for the reconstructed articular block.
Definitive Fixation Construct
Definitive fixation was achieved using a dual-plate construct to neutralize the complex deforming forces.
An anatomically contoured 3.5mm anterolateral distal tibia locking compression plate was applied. The plate was slid proximally in a submuscular fashion. Distally, multiple 2.7mm and 3.5mm locking screws were placed in a raft configuration immediately subchondral to the articular surface to support the elevated fragments. Proximally, fixation was secured with a combination of locking and non-locking cortical screws.
To address the medial comminution and prevent varus collapse, a 3.5mm medial distal tibia plate was applied via the posteromedial approach. This plate acted as an anti-glide and buttress plate. Care was taken to ensure that the screws from the anterolateral and medial plates did not intersect.
Wound Closure and Hemostasis
The tourniquet was deflated, and meticulous hemostasis was achieved using electrocautery. The wounds were irrigated with copious amounts of sterile saline. Closure of the surgical incisions in pilon fractures is as critical as the bony reduction. The extensor retinaculum was loosely reapproximated to prevent bowstringing of the tendons. The subcutaneous tissues were closed with 2-0 absorbable sutures. The skin was closed using a non-strangulating Allgöwer-Donati technique with 3-0 nylon to minimize tension on the epidermal edges and preserve the dermal microcirculation. Sterile, non-adherent dressings were applied, followed by a well-padded short leg splint in neutral dorsiflexion.
Post Operative Protocol and Rehabilitation
The postoperative management of a complex pilon fracture requires a protracted and disciplined rehabilitation protocol to optimize functional outcomes and mitigate the risk of complications.
Immediate Postoperative Phase Weeks Zero to Two
The patient was admitted for 48 hours of intravenous antibiotics and pain management. Strict elevation of the operative extremity above the level of the heart was enforced to control edema. The patient was instructed on strict non-weight-bearing status on the right lower extremity. Deep vein thrombosis prophylaxis was initiated with low molecular weight heparin. At the two-week mark, the patient was seen in the clinic. The splint was removed, and the incisions were inspected. Sutures were removed at three weeks once complete epithelialization was confirmed.
Early Rehabilitation Phase Weeks Three to Six
Once the incisions were fully healed, the patient was transitioned to a removable controlled ankle motion (CAM) boot. Strict non-weight-bearing status was maintained. The primary focus of this phase was the initiation of early, active range of motion exercises for the ankle and subtalar joints to prevent arthrofibrosis and nourish the articular cartilage. Patients are instructed to perform active dorsiflexion, plantarflexion, inversion, and eversion exercises multiple times daily out of the boot.
Intermediate Rehabilitation Phase Weeks Six to Twelve
At six weeks postoperatively, clinical and radiographic evaluations were performed. Radiographs were assessed for maintenance of reduction, hardware integrity, and early signs of callus formation at the metaphyseal fracture sites. If radiographic progression of healing was evident, the patient was permitted to begin touch-down weight-bearing (approximately 10-15% of body weight) in the CAM boot. Range of motion exercises were intensified, and gentle strengthening of the extrinsic foot and ankle musculature was initiated using resistance bands.
Advanced Rehabilitation and Return to Function Months Three to Six
At twelve weeks, provided there was radiographic evidence of bridging callus across the metaphyseal fractures and clinical absence of pain at the fracture site, the patient was progressively advanced to full weight-bearing. The CAM boot was gradually weaned, and the patient transitioned to supportive athletic footwear. Physical therapy focused on proprioceptive training, gait normalization, and advanced strengthening of the gastrocnemius-soleus complex, anterior tibialis, and peroneal musculature.
Long Term Prognosis and Expectations
Patients with OTA/AO 43-C3 pilon fractures must be counseled regarding the long-term sequelae of the injury. Despite anatomic articular reduction and stable fixation, the initial impact energy causes irreversible damage to the chondrocytes. The risk of developing post-traumatic osteoarthritis is exceedingly high, often manifesting within two to five years post-injury. Patients are advised that they may experience chronic aching, activity-related swelling, and a permanent reduction in ankle range of motion compared to the contralateral side. Future interventions, such as ankle arthrodesis or total ankle arthroplasty, may be required if arthritic symptoms become functionally limiting.
Clinical Pearls and Pitfalls
The management of complex pilon fractures is fraught with challenges. Adherence to established trauma principles and an awareness of common pitfalls are essential for optimizing outcomes.
Clinical Pearls
- Respect the Soft Tissue Envelope: The condition of the soft tissues dictates the timing of definitive surgery. Proceeding with open reduction through compromised, edematous skin is a reliable recipe for catastrophic wound dehiscence and deep infection. The staged "Span, Scan, and Plan" approach is non-negotiable in high-energy injuries.
- Mandatory Post Fixator CT Scanning: A high-quality CT scan obtained after the application of the spanning external fixator provides an accurate map of the articular fragments after the deforming forces of the tendons and soft tissues have been neutralized by traction. This is paramount for precise surgical planning.
- Anatomic Articular Reduction: The primary goal of internal fixation is the absolute anatomic restoration of the articular surface. Even a 1mm to 2mm step-off significantly alters joint contact pressures and accelerates the onset of post-traumatic arthrosis.
- Address the Fibula Strategically: While fibular fixation restores the lateral column and aids in syndesmotic reduction, it should not dictate a malreduction of the tibia. If the fibula is highly comminuted, it may be preferable to reconstruct the tibial articular block first and plate the fibula subsequently to avoid tethering the tibia into valgus.
Clinical Pitfalls
- Failure to Recognize Compartment Syndrome: The severe swelling associated with pilon fractures can mask the classic signs of compartment syndrome. A high index of suspicion and a low threshold for intracompartmental pressure monitoring are required, particularly for the anterior and deep posterior compartments.
- Inadequate Visualization of the Posterior Plafond: The posterolateral (Volkmann) fragment is often larger and more displaced than appreciated on plain radiographs. Failure to adequately expose and reduce this fragment leads to posterior subluxation of the talus and a poor functional outcome.
- Varus Malunion: The medial column of the distal tibia is under significant compressive forces. Relying solely on an anterolateral plate for a fracture with medial extension often results in late varus collapse. A supplementary medial buttress plate is frequently necessary to stabilize the medial column.
- Strangulating Skin Closure: Aggressive retraction during surgery and tight, tensioned skin closure compromise the delicate dermal microcirculation. Utilizing the Allgöwer-Donati suture technique and accepting a slightly wider scar in favor of lower wound tension significantly reduces the risk of marginal necrosis.
You Might Also Like