Mastering Tourniquet Principles and Techniques in Operative Orthopaedics
Key Takeaway
A bloodless surgical field is paramount in orthopaedic surgery to ensure precise dissection and protect vital structures. However, tourniquet application carries inherent risks of ischemic and compressive neuromuscular injury. This guide details the evidence-based principles of pneumatic and elastic tourniquet use, including limb occlusion pressure calculations, safe duration limits, exsanguination techniques, and strategies to mitigate post-tourniquet syndrome and nerve paralysis in clinical practice.
INTRODUCTION TO TOURNIQUET USE IN ORTHOPAEDICS
In the realm of operative orthopaedics, the establishment of a bloodless surgical field is not merely a convenience; it is an absolute prerequisite for accurate anatomical dissection. The meticulous identification and preservation of small, vital structures—such as digital nerves, microvascular bundles, and delicate tendinous insertions—demand an environment free of obscuring hemorrhage. However, the application of a tourniquet is a double-edged sword. The inherent dangers of tourniquet use are profound, primarily stemming from ischemia and mechanical compression, which can precipitate devastating complications including ischemic muscle contracture and irreversible nerve paralysis.
Modern orthopaedic practice dictates a rigorous, evidence-based approach to tourniquet application. Because the pressure can be monitored and controlled more reliably with a pneumatic tourniquet, complications are universally believed to be less likely with this modality than with an elastic or rubber bandage tourniquet. Nevertheless, regardless of the specific tourniquet utilized, surgeons must remain vigilant. Temporary or permanent disproportionate or prolonged edema, joint stiffness, diminished sensibility, and motor weakness or paralysis may result from improper use.
Surgical Warning: The tourniquet should never be viewed as a benign surgical adjunct. It is a device that induces controlled, temporary ischemia and mechanical tissue deformation. Respect for physiological time limits and pressure thresholds is mandatory to prevent catastrophic limb morbidity.
PATHOPHYSIOLOGY OF TOURNIQUET-INDUCED INJURY
The morbidity associated with tourniquet use is multifactorial. Based on landmark animal studies, Pedowitz et al. emphasized that biochemical, biomechanical, microvascular, and cellular mechanisms combine to produce significant neuromuscular injury from the use of tourniquets, even at clinically allowable pressures and durations.
Biomechanical Nerve Injury
The primary mechanism of nerve injury under a tourniquet is mechanical deformation rather than pure ischemia. The pressure gradient is steepest at the edges of the tourniquet cuff (the "edge effect"). This shear stress causes longitudinal displacement of the nodes of Ranvier, leading to intussusception of the myelin sheath and subsequent conduction block (neuropraxia). If the pressure is excessive, axonal disruption (axonotmesis) may occur, leading to prolonged or permanent paralysis.
Ischemic and Cellular Mechanisms
Skeletal muscle is highly sensitive to hypoxia. Tourniquet inflation initiates a cascade of ischemic events:
* ATP Depletion: Cellular energy stores are rapidly depleted, leading to the failure of the sodium-potassium pump.
* Intracellular Acidosis: Anaerobic metabolism leads to lactic acid accumulation, dropping tissue pH.
* Microvascular Endothelial Damage: Prolonged ischemia damages the capillary endothelium, increasing permeability.
Ischemia-Reperfusion Injury (IRI)
The most significant cellular damage often occurs not during the ischemic phase, but upon tourniquet deflation. Reperfusion introduces a surge of oxygen to ischemic tissues, generating reactive oxygen species (ROS). These free radicals cause lipid peroxidation of cell membranes, exacerbating tissue edema and leading to the "no-reflow phenomenon," where microvascular perfusion remains impaired despite the restoration of macrovascular flow. This cascade is the primary driver of Post-Tourniquet Syndrome.
INDICATIONS AND CONTRAINDICATIONS
Indications
- Trauma Surgery: Open reduction and internal fixation (ORIF) of fractures in the extremities.
- Elective Hand and Upper Extremity Surgery: Tendon repairs, nerve decompressions, arthroplasties.
- Lower Extremity Arthroplasty: Total knee arthroplasty (TKA), though modern protocols increasingly favor "tourniquet-less" approaches or limited inflation times.
- Foot and Ankle Surgery: Arthrodesis, ligamentous reconstructions, and osteotomies.
Absolute Contraindications
- Severe peripheral vascular disease (PVD) or heavily calcified vessels.
- Sickle cell disease (hypoxia and stasis precipitate sickling crises).
- Deep vein thrombosis (DVT) or a high risk of venous thromboembolism.
- Severe crush injuries or impending compartment syndrome.
- Arteriovenous (AV) fistulas or vascular grafts in the operative limb.
Relative Contraindications
- Poor skin condition (e.g., fragile skin in the elderly, severe psoriasis, or active infection at the cuff site).
- Peripheral neuropathy (e.g., advanced diabetic neuropathy), as the nerves are already compromised and highly susceptible to mechanical compression.
EVIDENCE-BASED TOURNIQUET PARAMETERS
Limb Occlusion Pressure (LOP)
Historically, surgeons utilized arbitrary pressure settings (e.g., 250 mmHg for the upper extremity, 350 mmHg for the lower extremity). This "one-size-fits-all" approach is obsolete and dangerous. Modern practice dictates the use of Limb Occlusion Pressure (LOP).
LOP is defined as the minimum pressure required, at a specific time and in a specific tourniquet cuff applied to a specific patient's limb, to stop the flow of arterial blood into the limb distal to the cuff.
Calculating Target Tourniquet Pressure based on LOP:
* If LOP is < 130 mmHg: Add 40 mmHg.
* If LOP is 130 - 190 mmHg: Add 60 mmHg.
* If LOP is > 190 mmHg: Add 80 mmHg.
* For pediatric patients: Add 50 mmHg to the LOP.
Clinical Pearl: Utilizing LOP minimizes the mechanical shear stress on underlying nerves and soft tissues, significantly reducing the incidence of neuropraxia and postoperative pain compared to standard high-pressure settings.
Duration Limits and "Breathing" the Tourniquet
The universally accepted maximum safe duration for continuous tourniquet inflation is 120 minutes (2 hours).
If the surgical procedure extends beyond this limit, the tourniquet must be deflated to allow for tissue reperfusion—a process colloquially known as "breathing the tourniquet."
* Reperfusion Protocol: Deflate the tourniquet for 10 to 15 minutes for every 2 hours of inflation.
* During this period, the limb must be elevated, and sterile compressive dressings applied to manage hemorrhage.
* Following the reperfusion interval, the limb is re-exsanguinated, and the tourniquet is re-inflated for a maximum of 60 additional minutes.
PREOPERATIVE PREPARATION AND POSITIONING
Skin Protection
The skin beneath the tourniquet must be meticulously protected to prevent blistering, friction burns, and pressure necrosis.
1. Apply two layers of smooth, wrinkle-free cast padding or a specialized tourniquet stockinette over the intended cuff site.
2. Ensure that prep solutions (e.g., Chlorhexidine or Betadine) do not seep under the tourniquet cuff. Chemical burns occur when prep solutions pool beneath the inflated cuff, causing severe full-thickness skin necrosis. Use an adhesive drape (U-drape) or a fluid-impervious barrier distal to the cuff to prevent seepage.
Exsanguination Techniques
Proper exsanguination ensures a truly bloodless field and minimizes the volume of blood trapped in the venous system, which can lead to engorgement and increased bleeding.
* Elevation: Elevating the limb at 45 to 60 degrees for 3 to 5 minutes utilizes gravity to drain venous blood. This is the preferred method for limbs with infections, malignancies, or severe fractures where mechanical compression is contraindicated.
* Esmarch Bandage: For non-infected, non-malignant, and stable limbs, an Esmarch bandage is wrapped tightly from distal to proximal to mechanically exsanguinate the limb prior to tourniquet inflation.
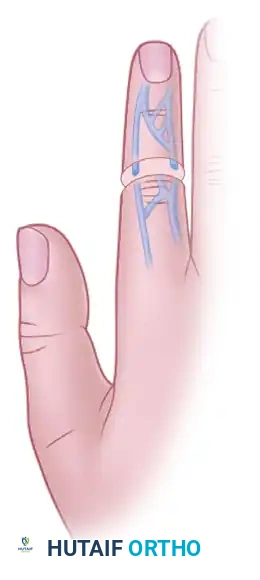
SURGICAL APPROACH: THE ELASTIC (MARTIN) BANDAGE TECHNIQUE
While pneumatic tourniquets are the gold standard for major procedures, elastic exsanguinating bandages remain highly relevant for specific, short-duration procedures. When operations are performed with the patient under local anesthesia and last less than 30 minutes, an elastic (Martin) bandage provides sufficient hemostasis and may be used safely.
This method is highly satisfactory for minor distal procedures, including trigger digit release, small scar revision, and the excision of benign masses from the skin and subcutaneous tissues of the forearm, hand, and fingers.
Step-by-Step Application of the Martin Bandage
- Patient Preparation: Ensure the patient is comfortable and the limb is prepped and draped. Administer local anesthesia (e.g., wide-awake local anesthesia no tourniquet [WALANT] techniques can sometimes bypass the need for a tourniquet entirely, but if a bloodless field is required, proceed with the Martin bandage).
- Distal to Proximal Wrapping: Wrapping of the bandage is begun precisely at the fingertips and proceeds proximally on the forearm.
- Layering and Overlap: The bandage is applied in continuous layers that overlap less than 5 to 6 mm. This specific overlap ensures uniform compression without creating focal areas of extreme high pressure.
- Proximal Fixation: When the midforearm is reached, four or five layers of the elastic are overlapped directly on top of one another to create the tourniquet effect.
- Wrinkle Avoidance: It is absolutely critical that wrinkles are avoided during application. Wrinkles in the elastic bandage create focal pressure spikes that can cause severe skin blistering and localized nerve damage.
- Unwrapping the Distal Segment: Once the proximal "cuff" is established, the distal portion of the bandage covering the hand and surgical site is carefully unwrapped, leaving the proximal overlapping layers in place to maintain arterial occlusion.
- Surgical Dissection: The pressure is increased with each dissection step, as the bloodless field allows for micro-precision.
Pitfall: Never leave an elastic bandage on for more than 30 minutes. Unlike a pneumatic tourniquet, the exact pressure exerted by a Martin bandage is unknown and often exceeds 300-400 mmHg, drastically increasing the risk of rapid mechanical nerve injury.
SURGICAL APPROACH: THE PNEUMATIC TOURNIQUET TECHNIQUE
For procedures lasting longer than 30 minutes or requiring proximal limb occlusion, the pneumatic tourniquet is mandatory.
Step-by-Step Application
- Cuff Selection: Select a cuff that is appropriately sized. The cuff width should be at least half the diameter of the limb. A wider cuff requires lower inflation pressure to achieve arterial occlusion, thereby reducing the risk of nerve injury. Use contour cuffs for highly conical limbs (e.g., obese thighs) to ensure uniform pressure distribution.
- Placement: Apply the cuff at the point of maximum limb circumference (proximal thigh or proximal arm). Ensure the pneumatic tubing is positioned away from the surgical field and does not kink.
- Padding: Apply wrinkle-free padding as described above.
- Exsanguination: Exsanguinate the limb using an Esmarch bandage or elevation.
- Inflation: Inflate the tourniquet rapidly to the calculated LOP target. Slow inflation allows arterial blood to enter the limb while venous return is occluded, leading to severe venous engorgement and a bloody surgical field.
- Monitoring: The circulating nurse must document the exact time of inflation and verbally alert the surgeon at 60, 90, and 120 minutes.
COMPLICATIONS AND MANAGEMENT
Post-Tourniquet Syndrome
Characterized by prolonged edema, stiffness, diminished sensibility, and subjective weakness without objective motor paralysis. It is primarily driven by ischemia-reperfusion injury and microvascular congestion.
* Management: Elevation, aggressive early physical therapy, and non-steroidal anti-inflammatory drugs (NSAIDs). Resolution usually occurs within 1 to 6 weeks.
Tourniquet Paralysis (Nerve Palsy)
A devastating complication resulting from mechanical compression (axonotmesis). The radial nerve in the upper extremity and the sciatic/peroneal nerve in the lower extremity are most vulnerable.
* Management: Baseline electromyography (EMG) and nerve conduction studies (NCS) at 3 to 4 weeks post-injury if no clinical improvement is noted. Most cases are neuropraxic and resolve spontaneously within 3 to 6 months. Surgical exploration is rarely indicated unless there is a complete failure of recovery at 6 months.
Systemic Hemodynamic Shifts
- Inflation: Can cause a transient increase in systemic vascular resistance and central venous pressure, which may be poorly tolerated in patients with severe congestive heart failure.
- Deflation: Results in a sudden drop in systemic blood pressure, a spike in end-tidal CO2 (due to the release of ischemic metabolites), and a transient decrease in core body temperature. The anesthesia team must be alerted prior to deflation to manage these shifts.
POSTOPERATIVE PROTOCOLS AND DEFLATION
The management of the limb immediately following tourniquet deflation is critical to minimizing postoperative hematoma and ensuring tissue viability.
- Hemostasis Before Deflation: In complex reconstructions, the surgeon may choose to deflate the tourniquet prior to wound closure to identify and cauterize bleeding vessels.
- Hemostasis After Closure: Alternatively, the wound is closed, and compressive dressings (and potentially closed-suction drains) are applied before the tourniquet is deflated. This relies on the compressive dressing to tamponade capillary bleeding.
- Monitoring Reperfusion: Upon deflation, the surgeon must visually confirm the return of capillary refill and normal skin color to the distal digits. A hyperemic flush is a normal and expected physiological response.
- Postoperative Elevation: The operated extremity must be strictly elevated above the level of the heart in the immediate postoperative period to counteract the inevitable reactive hyperemia and third-spacing of fluids caused by the ischemia-reperfusion cascade.
By adhering to these strict, evidence-based protocols, the orthopaedic surgeon can harness the indispensable benefits of a bloodless surgical field while systematically mitigating the profound risks associated with tourniquet application.
You Might Also Like