Operative Management of Freiberg Disease and Brachymetatarsia: Advanced Surgical Techniques
Key Takeaway
Freiberg disease and brachymetatarsia present complex challenges in forefoot reconstruction. Surgical management of Freiberg disease often involves joint debridement, metatarsal head remodeling, or a dorsal closing wedge osteotomy to restore articular congruity. For brachymetatarsia, restoring the metatarsal parabolic arc requires precise one-stage lengthening with interpositional grafting or gradual distraction osteogenesis, depending on the magnitude of the deformity. Strict adherence to biomechanical principles ensures optimal functional outcomes.
INTRODUCTION TO FOREFOOT RECONSTRUCTION
The structural integrity and biomechanical function of the forefoot rely heavily on the preservation of the metatarsal parabolic arc and the congruity of the metatarsophalangeal (MTP) joints. Disruptions to this delicate architecture—whether through avascular necrosis, as seen in Freiberg disease, or through congenital or acquired shortening, as seen in brachymetatarsia—can lead to profound functional impairment, transfer metatarsalgia, and significant cosmetic deformity.
This comprehensive masterclass details the evidence-based surgical management of these two distinct yet biomechanically related pathologies. The techniques described herein are designed for the postgraduate orthopedic surgeon, focusing on joint preservation, restoration of the metatarsal cascade, and meticulous soft-tissue balancing.
PART I: SURGICAL MANAGEMENT OF FREIBERG DISEASE
Freiberg disease (infraction) is an osteochondrosis or avascular necrosis primarily affecting the lesser metatarsal heads, most commonly the second metatarsal. The pathophysiology is multifactorial, involving repetitive microtrauma, vascular compromise, and altered biomechanics (e.g., a long second metatarsal). The disease process typically leads to subchondral collapse, dorsal flattening of the metatarsal head, and subsequent secondary osteoarthritis.
Surgical intervention is indicated when conservative measures (e.g., offloading orthotics, metatarsal pads, immobilization) fail. The choice of procedure is dictated by the Smillie classification, with joint-preserving osteotomies favored for early-to-intermediate stages, and debridement or arthroplasty reserved for advanced degenerative changes.
Dorsal Closing Wedge Osteotomy (Chao et al. Technique)
The dorsal closing wedge osteotomy is a highly effective, joint-preserving procedure for Smillie Stage II and III lesions. The biomechanical rationale is elegant: the avascular, collapsed dorsal portion of the metatarsal head is rotated proximally and dorsally, away from the primary weight-bearing articulation. This maneuver simultaneously brings the healthy, uninvolved plantar articular cartilage into direct articulation with the base of the proximal phalanx.
Biomechanical Pearl: Do not attempt to excise the necrotic dorsal lesion. Excision creates a massive osteochondral defect that inevitably leads to joint incongruity and rapid arthrosis. Instead, utilize the osteotomy to redirect the mechanical axis, leveraging the preserved plantar cartilage.
Preoperative Planning and Positioning
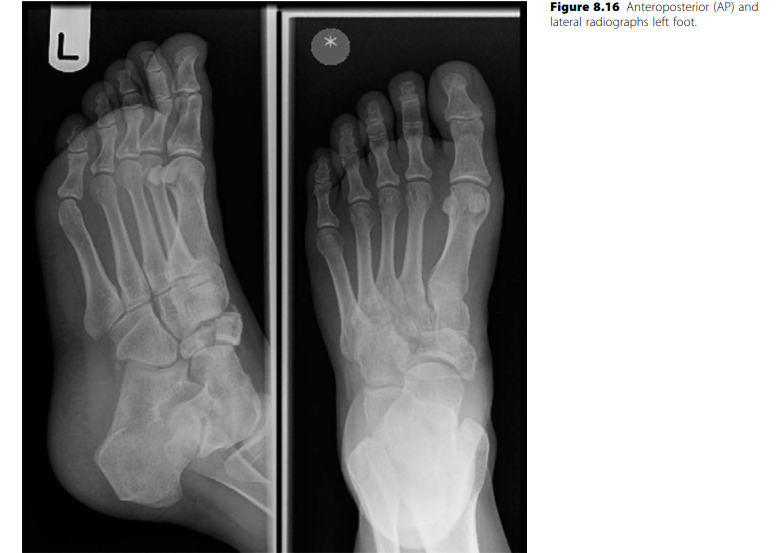
- Imaging: Weight-bearing anteroposterior (AP), lateral, and oblique radiographs of the foot. MRI may be utilized to assess the extent of avascular necrosis and the viability of the plantar cartilage.
- Positioning: Supine with a bump under the ipsilateral hip to maintain the foot in a neutral position. A calf or thigh tourniquet is applied for hemostasis.
Step-by-Step Surgical Technique
- Surgical Approach: Make a 3 to 4 cm longitudinal dorsal incision centered over the affected MTP joint. Deepen the dissection through the subcutaneous tissue, taking care to identify and retract the dorsal cutaneous nerves.
- Capsulotomy and Joint Inspection: Perform a longitudinal incision in the dorsal capsule. Extensively debride the joint, removing any loose osteochondral fragments, hypertrophic synovium, and debris. Perform a partial synovectomy to improve visualization and reduce postoperative inflammation.
- Osteotomy Execution:
- Identify the distal normal metaphysis, just proximal to the necrotic segment.
- Using a microsagittal saw under continuous saline irrigation, create a dorsal closing wedge osteotomy.
- The apex of the wedge must remain strictly at the plantar cortex, preserving a plantar cortical hinge to maintain stability and blood supply.
- Remove sufficient dorsal bone to allow the metatarsal head to rotate dorsally. This rotation brings the healthy plantar articular cartilage into the functional MTP articulation.
- Length Preservation: The angle of the closing wedge must be meticulously calculated to maintain the length of the involved metatarsal bone as much as possible. Excessive shortening will precipitate transfer metatarsalgia to the adjacent lesser metatarsals.
- Fixation:
- Reduce the osteotomy by closing the dorsal gap.
- Temporarily provision the osteotomy with crossed percutaneous Kirschner wires (K-wires) (typically 0.045-inch or 0.062-inch).
- Alternative Fixation: Bioabsorbable pins or low-profile titanium screws can be utilized to provide rigid internal fixation, thereby avoiding a secondary procedure or clinic visit for K-wire removal.
Surgical Pitfall: Breaching the plantar cortical hinge during the osteotomy will destabilize the metatarsal head, making rotational control exceedingly difficult and increasing the risk of nonunion or malunion.
Postoperative Protocol
- 0-4 Weeks: A light compressive dressing is applied. The foot is immobilized in a short-leg walking cast or a rigid postoperative boot. Weight-bearing is permitted as tolerated on the heel and lateral border of the foot.
- 4 Weeks: If percutaneous K-wires were used, they are removed in the clinic. The patient transitions to a stiff-soled shoe with a metatarsal pad.
- 8+ Weeks: Patients are restricted from running, jumping, or engaging in strenuous physical activity for a minimum of 8 weeks to ensure complete radiographic and clinical consolidation of the osteotomy.
Joint Debridement and Metatarsal Head Remodeling
In advanced stages of Freiberg disease (Smillie Stage IV and V), where the metatarsal head is severely flattened, pitted, and arthritic, a simple osteotomy is insufficient. In these cases, comprehensive joint debridement, soft-tissue decompression, and metatarsal head remodeling (cheilectomy/arthroplasty) are required to restore a functional, pain-free range of motion.
Step-by-Step Surgical Technique
- Incision and Exposure:
- Make an angled or lazy-S incision, with the apex positioned at the lateral margin of the MTP joint. This prevents dorsal scar contracture.
- Carefully ligate any crossing veins returning to the dorsal venous arch to prevent postoperative hematoma.
- Extensor Apparatus Management:
- Expose the entire extensor expansion over the MTP joint.
- Identify the extensor digitorum brevis (EDB) tendon as it joins the extensor digitorum longus (EDL). Section the EDB at this juncture to reduce dorsal tethering.
- Incise the extensor hood just lateral to the EDL tendon, and retract the EDL medially.
- Capsular Release:
- Through a longitudinal capsulotomy, enter the MTP joint. Reflect the capsule medially and laterally via sharp dissection to fully expose the metatarsal head.
- Note: The degree of macroscopic cartilaginous degeneration is often strikingly more severe than preoperative radiographs suggest.
- Debridement and Microfracture:
- Excise all loose osteochondral fragments and perform a thorough synovectomy.
- If a focal, full-thickness chondral defect is present with a viable subchondral base, utilize a 0.045-inch K-wire to perform microfracture. Penetrate the subchondral bone at 2-mm intervals to stimulate fibrocartilage ingrowth.
- Joint Distraction and Arthroplasty Assessment:
- Manually distract the toe and flex it acutely to expose the entire plantar aspect of the metatarsal head. It may be necessary to release one or both collateral ligaments to achieve adequate exposure.
- Assess the remaining articular surface. If the cartilage has remodeled and appears functional, limit the bony work to debridement and perform a Z-plasty lengthening (8 to 12 mm) of the EDL tendon. This decompresses the joint and relieves extensor pressure.
- Metatarsal Head Contouring:
- If the metatarsal head is severely pitted and irregular, it must be contoured. Remove the diseased articular cartilage using a rongeur or a high-speed burr.
- Crucially, ensure that no osteophytes remain on the plantar aspect of the metatarsal head, as these will cause intractable plantar pain during the toe-off phase of gait.
- The dorsal and central surfaces of the metatarsal head are usually depressed. Round the remainder of the head to match this depth. This typically requires the circumferential removal of 3 to 4 mm of bone, effectively creating a resection arthroplasty.
- Closure:
- Copiously irrigate the joint while taking it through a full range of motion to flush out any retained cartilage or bone debris.
- Secure hemostasis by direct pressure. Do not rely solely on the tourniquet release; meticulous hemostasis is critical to prevent arthrofibrosis.
- Close the capsule with fine absorbable sutures (e.g., 3-0 or 4-0 Vicryl), ensuring the joint is held in a reduced, neutral position.
Clinical Pearl: The Z-plasty lengthening of the EDL and the tenotomy of the EDB are not merely adjunctive steps; they are critical to the success of the remodeling procedure. Failing to decompress the extensor apparatus will result in continued dorsal impingement and recurrent pain.
Postoperative Protocol
- 0-48 Hours: Strict, continuous elevation of the foot above heart level to minimize edema.
- 0-2 Weeks: The patient is permitted to walk in a rigid, wooden-soled postoperative shoe.
- 2 Weeks: Skin sutures are removed. The forefoot is redressed, holding the toe in the desired neutral alignment.
- 4 Weeks: The patient transitions to a wide toe-box shoe. Active and gentle active-assisted range of motion (ROM) exercises of the MTP joint are initiated to prevent capsular contracture and promote fibrocartilage formation.
PART II: SURGICAL MANAGEMENT OF BRACHYMETATARSIA
Brachymetatarsia is a condition characterized by an abnormally short metatarsal, most frequently affecting the fourth metatarsal, followed by the first. The etiology may be congenital or acquired. Acquired forms typically result from premature physeal closure secondary to trauma, iatrogenic injury (surgery), infection, or systemic pathological conditions. In the pediatric population, brachymetatarsia is frequently associated with syndromic processes, including Down syndrome, Apert syndrome, Albright hereditary osteodystrophy, sickle cell anemia, diastrophic dwarfism, and poliomyelitis.
Biomechanics and Indications for Surgery
Brachymetatarsia disrupts the normal parabolic arc of the metatarsal heads (the Maestro curve). While the shortened metatarsal itself rarely causes pain, the disruption of the weight-bearing cascade forces the adjacent, normal-length metatarsals to bear excessive loads. This frequently results in severe transfer metatarsalgia, intractable plantar keratoses under the adjacent metatarsal heads, and dorsal impingement of the shortened digit against footwear. Furthermore, the cosmetic appearance of the "floating toe" is a primary driver for patients seeking surgical consultation.
Nonoperative management—such as metatarsal padding, custom orthotics, and accommodative footwear—can palliate symptoms in adjacent joints but cannot correct the deformity.
Surgical Indications: Surgery is generally indicated when a metatarsal is 10 mm or more shorter than the adjacent metatarsals, accompanied by pain, transfer lesions, or significant psychological distress regarding the cosmetic deformity.
Surgical Decision Making:
1. One-Stage Lengthening (with interpositional bone graft): Indicated for lengthening requirements of less than 15 mm.
2. Gradual Lengthening (Distraction Osteogenesis): Indicated for lengthening requirements of greater than 15 mm.
3. Shortening of Adjacent Metatarsals: Often used as an adjunct to reduce the "target length" required for the brachymetatarsal, thereby reducing the risk of neurovascular compromise.
One-Stage Lengthening with Interpositional Bone Graft
For deficits under 15 mm, acute one-stage lengthening is highly effective. The cited advantages of this approach include a shorter time to achieve clinical union, a smaller surgical scar, the avoidance of prolonged external fixation, and a significantly lower risk of neurovascular impairment or excessive soft-tissue stretching.
However, if an autograft (e.g., iliac crest) is utilized, operative times are extended, and the patient is subjected to donor site morbidity, including pain, hematoma, and potential infection. To circumvent this, structural allografts are frequently employed.
Surgical Technique (Giannini et al.)
Giannini and colleagues popularized a highly successful one-stage lengthening technique utilizing allograft interposition, reporting an average length gain of 13 mm.
- Approach: A dorsal longitudinal incision is made over the affected metatarsal shaft. The extensor tendons are retracted, and the periosteum is carefully elevated to preserve the blood supply.
- Osteotomy: A transverse osteotomy is performed in the proximal metaphysis or diaphyseal-metaphyseal junction of the metatarsal shaft using a microsagittal saw.
- Distraction and Soft Tissue Release: The osteotomy is acutely distracted using a lamina spreader. If resistance is encountered, a sequential release of the contracted dorsal soft tissues, including an EDL Z-plasty or MTP capsulotomy, may be required.
- Graft Interposition: A structural tricortical allograft (or autograft) is meticulously contoured to match the exact dimensions of the distraction gap. The graft is impacted into the defect.
- Fixation: The construct is stabilized using a stout, intramedullary K-wire driven antegrade through the metatarsal head, across the graft, and into the proximal metatarsal base. Alternatively, a dorsal locking plate can be utilized for rigid construct stability, allowing for earlier mobilization.
Surgical Pearl: When multiple metatarsals are involved, a combined shortening and lengthening procedure can be executed. Intercalary autogenous bone grafts harvested from the intentionally shortened adjacent metatarsals can be utilized as the interpositional graft for the brachymetatarsal, eliminating the need for iliac crest harvest.
Gradual Lengthening via Distraction Osteogenesis
When the required length gain exceeds 15 mm, acute stretching of the neurovascular bundle and soft tissue envelope poses an unacceptable risk of toe ischemia and severe contracture. In these scenarios, distraction osteogenesis (callotasis) based on Ilizarov principles is the gold standard.
Good to excellent results are reported in 80% to 100% of patients treated with this modality. The advantages are profound: no structural bone grafting is required, the tendons and neurovascular structures are gradually accommodated to the new length, weight-bearing can be initiated earlier, and massive length gains can be achieved. Lee et al. demonstrated mean length gains of 17.2 mm in the first metatarsal and 16.3 mm in the fourth metatarsal using this technique.
Surgical Technique and Protocol
- External Fixator Application: Through minimal incisions, half-pins are inserted into the proximal and distal segments of the metatarsal, taking care to avoid the extensor tendons and neurovascular bundles. A mini-rail external fixator is applied dorsally.
- Corticotomy: A low-energy, multiple drill-hole osteotomy (corticotomy) is performed in the metaphysis to preserve the endosteal blood supply, which is critical for regenerate bone formation.
- Latency Phase: The osteotomy is left undisturbed for 5 to 7 days to allow for the initial stages of fracture healing and hematoma organization.
- Distraction Phase: Distraction is initiated at a rate of 0.5 to 0.75 mm per day, typically divided into two or three increments. The patient is monitored weekly with radiographs to assess the quality of the regenerate bone and the alignment of the MTP joint.
- Consolidation Phase: Once the target length is achieved (restoring the parabolic arc), the fixator is locked. The device remains in place until the regenerate bone demonstrates corticalization on at least three out of four sides on radiographs (typically 2 to 3 times the duration of the distraction phase).
Complications of Distraction Osteogenesis
While highly effective, distraction osteogenesis is fraught with potential complications, particularly when the metatarsal is lengthened by more than 40% of its original length.
* MTP Joint Stiffness: This is the most common complication, resulting from the increased tension on the extensor tendons and joint capsule. Prophylactic pinning of the MTP joint during the distraction phase is often recommended to prevent subluxation and stiffness.
* Axial Deviation/Malalignment: Unequal tension from the soft tissues can cause the distal fragment to drift into plantarflexion or dorsal elevation.
* Pin Track Infections: Superficial infections are common and usually resolve with local pin care and oral antibiotics.
* Premature Consolidation or Nonunion: Requires surgical revision, either by repeating the corticotomy or by applying bone graft to a nonunion site.
Surgical Pitfall: Failing to pin the MTP joint in a neutral position prior to initiating distraction osteogenesis will almost certainly result in severe dorsal subluxation or dislocation of the toe as the extensor tendons tighten during the lengthening process.
CONCLUSION
The operative management of Freiberg disease and brachymetatarsia requires a profound understanding of forefoot biomechanics and meticulous surgical execution. Whether performing a joint-preserving dorsal closing wedge osteotomy, a complex joint remodeling, or a precise metatarsal lengthening, the ultimate goal remains the same: the restoration of a pain-free, congruent, and biomechanically sound metatarsal parabolic arc. Strict adherence to the indications and techniques outlined in this masterclass will ensure optimal outcomes for these challenging pathologies.
You Might Also Like