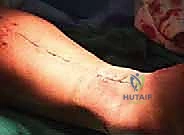
Staged Soft Tissue Expansion for Complex Achilles Tendon Reconstruction: An Intraoperative Masterclass
Key Takeaway
This masterclass details staged soft tissue expansion for complex Achilles tendon reconstruction. We cover meticulous patient positioning, the posteromedial approach, precise expander implantation, and subsequent removal with definitive tendon repair. Emphasis is placed on comprehensive anatomy, intraoperative technique, identifying neurovascular risks like the sural nerve, and managing postoperative complications for optimal patient outcomes in revision scenarios.
Introduction to Complex Achilles Tendon Reconstruction with Soft Tissue Expansion
Alright, fellows, gather 'round. Today, we're tackling a challenging, yet incredibly rewarding, scenario: complex Achilles tendon reconstruction necessitating soft tissue expansion. This isn't your straightforward primary repair; we're dealing with neglected ruptures, revision surgeries, or cases where significant skin contracture or large tendon gaps preclude a tension-free direct closure. Our goal is to create a robust, functional Achilles tendon while ensuring excellent soft tissue coverage – a critical, often overlooked, component of success in these complex cases. We'll approach this as a staged procedure, allowing the body to naturally expand the local skin envelope, paving the way for a truly tension-free definitive repair.
Indications for Staged Soft Tissue Expansion
When do we consider this staged approach?
* Neglected Achilles Tendon Ruptures: Cases presenting weeks or months after injury, where significant retraction of the tendon ends has occurred, leading to a substantial gap.
* Revision Achilles Tendon Surgery: Following failed primary repairs, where scar tissue, poor tendon quality, or persistent skin issues are present.
* Large Tendon Gaps: When the defect is simply too large to bridge with standard techniques without undue tension on the repair or skin.
* Contracted or Compromised Skin: Prior surgeries, trauma, or chronic inflammation can lead to skin that lacks elasticity, making primary closure difficult or impossible without high tension, increasing the risk of wound dehiscence and infection.
* Augmented Procedures: When we anticipate increasing the girth of the distal tendon (e.g., with allografts or FHL transfers), requiring more soft tissue coverage.
Preoperative Planning: The Blueprint for Success
Before we even consider making an incision, meticulous preoperative planning is paramount.
Comprehensive Imaging Review
We start by thoroughly reviewing MRI studies. These are our eyes into the deep tissues, helping us understand:
* Tendon Gap Size and Quality: Is there a significant gap? What's the quality of the remaining tendon ends? Is there extensive scar tissue?
* Soft Tissue Envelope: Assess the thickness and quality of the overlying skin and subcutaneous tissue. Is there evidence of chronic inflammation or previous surgical scarring?
* Ideal Expander Placement: The MRI helps us visualize the optimal subcutaneous plane for expander insertion, ensuring it lies between the skin and the Achilles tendon, not within the tendon substance itself. We're looking for a clear plane to develop.
* Neurovascular Structures: Confirming the general course of the sural nerve and short saphenous vein relative to the planned incision.
Patient Education and Expectation Management
This is a two-stage procedure, typically 3 to 4 weeks apart. It's crucial that the patient understands:
* The rationale behind the staged approach.
* The commitment required for weekly follow-up visits between stages for expander inflation.
* The importance of activity restrictions during the expansion phase.
* The overall timeline for recovery.
Patient Positioning: Setting the Stage
For Achilles tendon surgery, the prone position offers us the best possible access to the posterior aspect of the ankle and lower leg.
Meticulous Padding and Setup
- Chest Rolls: Ensure appropriate chest rolls are placed to allow for adequate diaphragmatic excursion and prevent abdominal compression.
- Head Positioning: The head should be comfortably positioned on a gel donut, free from pressure points, with the neck in a neutral alignment.
- Upper Extremities: Arms should be abducted less than 90 degrees, padded, and secured on arm boards to prevent brachial plexus injury.
- Knee and Ankle Support: A well-padded pillow or gel pad is placed underneath the knees and anterior tibia-ankle region. This ensures the ankle is slightly dorsiflexed, allowing for natural alignment and preventing undue pressure on the anterior shin.
- Pressure Point Protection: Crucially, pay attention to the anterior superior iliac spines, patellae, and dorsum of the feet. Use additional gel padding as needed to prevent nerve compression or skin breakdown.
- Tourniquet Placement: A pneumatic tourniquet is typically applied high on the thigh. While we may not inflate it for the entire procedure, having it available for initial dissection and hemostasis is often beneficial.
Surgical Anatomy: Navigating the Posterior Ankle
Before we make our incision, let's quickly review the critical anatomy we'll encounter and must protect.
The Achilles Tendon Complex
- Tendon Itself: Formed by the gastrocnemius and soleus muscles, inserting onto the posterior aspect of the calcaneus. In complex cases, we'll find varying degrees of degeneration, scarring, and gap formation.
- Paratenon: A thin, delicate layer of connective tissue surrounding the Achilles tendon. This is absolutely vital as it provides the primary blood supply to the tendon, especially in its avascular mid-portion. Meticulous preservation and repair of the paratenon are critical for tendon healing.
Neurovascular Structures
- Sural Nerve: This is our most significant neurovascular risk in this region.
- Course: It originates from the tibial and common peroneal nerves, descends posterolaterally in the calf, then curves around the lateral malleolus to supply sensation to the lateral aspect of the foot and fifth toe.
- Vulnerability: It typically runs superficially in the subcutaneous tissue, often posterolateral to the Achilles tendon. A direct posterior incision or an incision too far laterally can easily injure it, leading to a painful neuroma or permanent sensory deficit.
- Short Saphenous Vein: This vein typically runs alongside the sural nerve in the posterolateral calf and ankle. Injury can lead to troublesome bleeding or postoperative hematoma.
Stage 1: Implantation of the Soft Tissue Expander
Now, let's get scrubbed in.
Anesthesia and Sterilization
- Anesthesia: General anesthesia is typically preferred for patient comfort and muscle relaxation. A regional block (e.g., popliteal block) can be a valuable adjunct for postoperative pain control.
- Sterile Prep and Drape: The entire lower limb, from mid-thigh to toes, is meticulously prepped with an antiseptic solution and draped in a sterile fashion, ensuring adequate exposure of the posterior ankle and calf.
The Incision: A Posteromedial Approach
"Alright team, let's establish our surgical field. We've got our landmarks. Our primary goal here is to create a pocket for the expander while meticulously protecting the critical neurovascular structures."
-
Skin Incision: "Using a #15 blade, I'm making a longitudinal incision along the medial aspect of the ankle, just adjacent to the medial border of the Achilles tendon. This posteromedial approach is our preferred method, as it significantly reduces the risk of injury to the sural nerve and short saphenous vein, which typically lie more laterally."
- "The length of this initial incision should be sufficient to allow for easy insertion of our 70-mL rectangular soft tissue expander. We're aiming for about 4-5 cm initially."
- Potential Incision Extensions: "For the second stage, or if we need more exposure during this stage, we can extend this incision. Options include a lazy-S configuration, an L-shape, or a direct medial extension. The key is to avoid crossing joint lines perpendicular to motion and to ensure adequate skin bridges if multiple limbs are created."
-
Superficial Subcutaneous Elevation: "Now, with careful sharp and blunt dissection using Metzenbaum scissors and a small Cobb elevator, we'll perform superficial subcutaneous elevation. The goal is to create a pocket that is superficial to the paratenon but deep to the dermis. This is crucial. We want the expander to push the skin away from the tendon, not to compress the tendon itself or interfere with its blood supply."
- "We're developing a pocket approximately 6 cm by 4 cm, just large enough to comfortably accommodate our 70-mL McGhan tissue expander. Ensure the pocket is wide enough to prevent expander migration or kinking."
- Hemostasis: "Maintain meticulous hemostasis throughout this dissection using bipolar cautery. Any hematoma formation in this pocket can compromise expander function or increase infection risk."
Expander Insertion
"Once our pocket is well-defined and dry, we're ready for the expander."
-
Expander Placement: "Carefully insert the McGhan 70-mL rectangular soft tissue expander into this cavity. Ensure it lies flat and smoothly within the pocket, without any folds or kinks. Its rectangular shape is ideal for conforming to the posterior calf contour."
- "The injection catheter, which allows us to inflate the expander, must be positioned away from the main incision line. We'll tunnel it subcutaneously a short distance and bring it out through a separate small stab incision, ensuring it's easily accessible but not directly under the primary wound."
-
Initial Inflation: "Before closure, we'll inject a small amount of normal saline – typically 10 mL – into the implant via the injection port. This confirms proper placement and ensures the expander is functional. It also helps to gently distend the pocket, confirming its dimensions."
Wound Closure
"Now for closure. We want a secure, watertight seal."
- Subcuticular Closure: "We'll perform a meticulous subcuticular closure using absorbable suture (e.g., 3-0 or 4-0 Monocryl). This provides strength and minimizes tension on the skin."
- Skin Reapproximation: "Finally, reapproximate the skin edges with fine non-absorbable sutures or staples. A sterile dressing is applied."
Postoperative Care - Stage 1
- Pain Management: Patients will experience some discomfort. Standard oral analgesics are usually sufficient.
- Wound Care: Keep the wound clean and dry. Instruct patients on signs of infection.
- Activity Restrictions: Limited weight-bearing and activity are advised to prevent expander displacement or wound complications.
- Weekly Follow-up and Inflation: "The patient is seen 1 week postoperatively. At this visit, and weekly thereafter, we'll add 10 mL of normal saline to the expander via the injection port. This gradual expansion allows the skin to stretch comfortably over 3 to 4 weeks."
Surgical Warning: Expander Volume Tolerance
"Fellows, remember that patients rarely tolerate more than 30 to 40 mL of total volume within the implant during the expansion phase. Individual skin pliability varies greatly. Always listen to your patient. If they report excessive pain or skin blanching, adjust the inflation rate downward or pause inflation for a week. Pushing too hard can lead to skin necrosis or expander extrusion."
Stage 2: Expander Removal and Definitive Tendon Repair
Approximately 3 to 4 weeks postoperatively, once adequate skin expansion is achieved, we proceed to the definitive repair.
Anesthesia and Positioning
"Back in the OR. Same meticulous prone positioning, same sterile prep and drape."
Expander Removal
- Incision Re-access: "We'll access the previously created incision. The skin here will be noticeably more pliable and abundant. Carefully extend the incision as necessary, using the same posteromedial trajectory, to gain full access to the expander and the underlying Achilles tendon."
- Expander Dissection: "The expansion balloon will be easily identified within its subcutaneous pocket. With gentle blunt and sharp dissection, carefully free the expander from its surrounding fibrous capsule. It should peel away quite readily."
- Removal: "Once fully mobilized, the expander and its injection catheter are removed from the surgical field."
Achilles Tendon Repair: The Definitive Reconstruction
"Now that we have ample skin, we can focus on the tendon itself. This is where we address the underlying pathology."
- Tendon Debridement: "First, we meticulously debride any unhealthy, scarred, or necrotic tendon tissue. We want to work with viable, robust tendon ends. Use a #15 blade or small rongeurs for this."
-
Gap Assessment and Reconstruction Strategy: "Assess the remaining tendon gap. For complex, neglected ruptures, a simple end-to-end repair is often not feasible without excessive tension. We might need to employ augmentation strategies:"
- V-Y Plasty: "If the gap is moderate, a V-Y advancement of the gastrocnemius-soleus complex can effectively lengthen the tendon. We make a V-shaped incision into the musculotendinous junction proximally, advance the flap distally, and then close the V as a Y. This provides significant lengthening."
- Flexor Hallucis Longus (FHL) Transfer: "For larger gaps or poor quality distal stump, an FHL transfer is an excellent option. We identify the FHL tendon in the deep posterior compartment, detach it distally, and then weave it into the calcaneal stump and proximal Achilles tendon using a triple-braided technique. This provides robust biological augmentation."
- Allograft/Autograft Augmentation: "In some cases, especially very large gaps, an allograft (e.g., Achilles tendon allograft) or autograft (e.g., semitendinosus) may be necessary to bridge the defect and provide additional strength."
- "For today, let's assume we're performing a V-Y plasty coupled with a robust end-to-end repair."
-
Tendon Repair Technique: "We'll use a strong, non-absorbable braided suture (e.g., #2 FiberWire or Ethibond) for the core repair. A modified Krackow or Bunnell stitch is excellent for achieving strong, locking purchase on the tendon ends."
- "Pass the sutures through the proximal and distal tendon segments, ensuring multiple locking loops for maximal strength. We want to engage as much tendon substance as possible."
- Tensioning: "Carefully approximate the tendon ends. Flex the knee to 90 degrees and bring the ankle into approximately 10-15 degrees of plantarflexion. This is the optimal position to tension the repair. We want enough tension to bring the ends together securely, but not so much that it causes blanching or undue stress on the repair. Test the repair by gently dorsiflexing the ankle; you should feel firm resistance without feeling like the repair is ripping out. The ankle should allow for free plantarflexion and controlled dorsiflexion."
-
Paratenon Repair: "This step is absolutely critical, fellows! Remember the paratenon's role in blood supply and gliding. Using fine absorbable sutures (e.g., 4-0 or 5-0 Vicryl), meticulously repair the paratenon over the entire Achilles tendon repair site. This re-establishes the fragile blood supply to the healing tendon and prevents adhesions to the overlying skin, promoting smooth gliding."
Wound Closure: The Benefit of Expansion
"Now, the beauty of our staged approach becomes evident."
- Subcutaneous Closure: "Close the subcutaneous layer with interrupted absorbable sutures (e.g., 3-0 Vicryl) to obliterate dead space and take tension off the skin."
- Skin Reapproximation: "Due to the prior soft tissue expansion, we now have abundant, pliable skin. This allows for a truly tension-free skin closure. Reapproximate the wound edges with staples or fine non-absorbable sutures (e.g., 3-0 Nylon)."
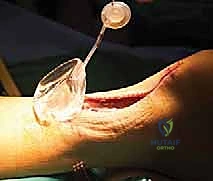
TECH FIG 3 • Tension-free skin closure after Achilles tendon repair.
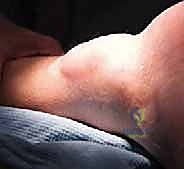
TECH FIG 3 • Tension-free skin closure after Achilles tendon repair.
"Notice how the skin edges come together effortlessly, without any puckering or blanching. This tension-free closure significantly reduces the risk of wound complications like dehiscence or infection, which are common pitfalls in revision Achilles surgery."
Pearls and Pitfalls: Navigating Challenges
Pearls and Pitfalls
Soft Tissue Expander Management
* Patient Tolerance: As discussed, patients rarely tolerate more than 30 to 40 mL of total volume. Always prioritize patient comfort over aggressive expansion. The expansion rate (e.g., 10 mL/week) may need adjustment based on individual skin pliability and pain levels. Gradual, gentle expansion is key to preventing skin necrosis or undue pain.
* Expander Migration/Kinking: Ensure the initial pocket is appropriately sized and the expander is placed flat. If kinking occurs, it can impede inflation.Complications Postoperative Care
* Infection: This is a devastating complication.
* Prevention: Meticulous sterile technique, prophylactic antibiotics (pre-op, intra-op, and sometimes 24 hours post-op), and tension-free wound closure.
* Recognition: Erythema, warmth, swelling, purulent discharge, fever.
* Management: For superficial infections, oral antibiotics and local wound care. For deep infections, surgical debridement, intravenous antibiotics, and potentially expander removal (if in Stage 1) or hardware removal (if augmentation was used).
* Seroma: Collection of serous fluid in the expander pocket (Stage 1) or surgical site (Stage 2).
* Prevention: Meticulous hemostasis during surgery, obliteration of dead space during closure.
* Management: Small seromas may resorb. Larger, symptomatic seromas can be aspirated under sterile conditions. Persistent seromas may require drain placement or surgical evacuation.
* Sural Nerve Injury:
* Prevention: Adherence to the posteromedial incision, careful identification and protection of the nerve during dissection. Always dissect superficially to the paratenon.
* Recognition: Postoperative numbness, paresthesias, or neuropathic pain in the lateral foot/fifth toe distribution.
* Management: Most mild neurapraxias resolve over time. For persistent symptoms, nerve blocks, gabapentin/pregabalin, or referral to a peripheral nerve specialist for potential neurolysis may be considered.
* Fibrotic Reaction: Excessive scar tissue formation around the expander or tendon repair.
* Prevention: Gentle tissue handling, meticulous hemostasis, and early controlled motion in the post-op phase.
* Impact: Can limit tendon gliding and range of motion.
* Wound Dehiscence: Separation of wound edges.
* Prevention: Tension-free closure, adequate skin expansion, avoidance of infection.
* Management: Small dehiscences may heal with local wound care. Larger defects may require surgical debridement and re-closure, or even skin grafting if severe.
* Re-rupture: The most feared complication of Achilles repair.
* Prevention: Robust repair technique, appropriate tensioning, strict adherence to postoperative rehabilitation protocols, and patient education on activity restrictions.
* Management: Typically requires revision surgery, often with extensive augmentation.
Postoperative Rehabilitation and Complication Management
Successful surgical repair is only half the battle; meticulous postoperative care is crucial for optimal outcomes.
Stage 1: Post-Expander Insertion
- Immobilization: The limb is typically placed in a short-leg splint or CAM boot for comfort and to prevent expander displacement for the first week.
- Weight-Bearing: Non-weight-bearing is usually recommended for the first week, then gradual weight-bearing as tolerated during the expansion phase, depending on patient comfort and expander stability.
- Activity: Limited activity, avoiding strenuous exercise or anything that could displace the expander or open the incision.
- Weekly Follow-up: As discussed, weekly visits for expander inflation and wound checks.
Stage 2: Post-Tendon Repair
- Immediate Immobilization: "After expander removal and definitive tendon reconstruction, the operative limb is immediately placed into a short-leg splint or a specialized controlled ankle motion (CAM) boot set in 10 to 15 degrees of plantarflexion. This protects the repair by minimizing tension. The splint is typically non-removable for the initial 2-3 weeks."
- Weight-Bearing Progression:
- Weeks 0-2 (or 0-3): Strict non-weight-bearing (NWB) on the operative limb. Crutches or a knee scooter are essential.
- Weeks 2-6 (or 3-6): Gradual protected weight-bearing (PWB) in the CAM boot with the ankle still in plantarflexion (e.g., 10-15 degrees). The degree of plantarflexion is gradually reduced by adjusting wedges in the boot.
- Weeks 6-12: Full weight-bearing in the CAM boot, with gradual progression to neutral dorsiflexion.
- Beyond 12 Weeks: Transition out of the boot into supportive shoes, with continued physical therapy.
- Range of Motion (ROM) Protocol:
- Weeks 0-2 (or 0-3): No active or passive dorsiflexion. Only gentle plantarflexion within the splint/boot.
- Weeks 2-6 (or 3-6): Initiate controlled passive dorsiflexion to neutral, avoiding excessive stretching. Begin gentle active plantarflexion exercises.
- Weeks 6-12: Progress full passive and active ROM, focusing on regaining dorsiflexion. Initiate light resistance exercises for plantarflexion.
- Beyond 12 Weeks: Advanced strengthening, proprioception, and balance exercises. Gradual return to functional activities.
- DVT Prophylaxis: Standard protocols for deep vein thrombosis prophylaxis are initiated, typically including chemical prophylaxis (e.g., low molecular weight heparin) and mechanical prophylaxis (e.g., sequential compression devices) in the hospital, and potentially continued chemical prophylaxis for several weeks post-discharge, depending on patient risk factors.
- Wound Care: Keep the incision clean and dry. Monitor for any signs of infection or wound dehiscence. Staples or non-absorbable sutures are typically removed at 2-3 weeks post-op.
- Physical Therapy: A structured physical therapy program is paramount. It should guide the patient through each phase of recovery, focusing on pain management, swelling reduction, progressive ROM, strengthening, balance, and eventually sport-specific training.
- Complication Management:
- Wound Dehiscence: Small areas may be managed with local wound care. Larger areas may require surgical debridement, re-closure, or even plastic surgery consultation for skin grafting if the defect is significant.
- Infection: Aggressive management with antibiotics, debridement, and potentially hardware removal (if augmentation was used).
- Re-rupture: Requires prompt re-evaluation. Often necessitates revision surgery with a more robust augmentation technique.
- Persistent Pain/Stiffness: Addressed through physical therapy, pain management, and sometimes further imaging to rule out adhesions or heterotopic ossification.
"Alright, fellows, that concludes our masterclass on staged soft tissue expansion for complex Achilles tendon reconstruction. This is a demanding procedure, but with meticulous planning, precise execution, and dedicated postoperative care, we can achieve excellent, durable results for our patients. Remember, the soft tissue envelope is just as important as the tendon repair itself in these challenging cases. Any questions?"
REFERENCES
- Non–weight-bearing with immobilization in a short-leg cast is maintained for 3 weeks. Range-of-motion exercises are initiated at 3 to 4 weeks postoperatively. Finally, weight bearing is allowed at 6 weeks after surgical repair ( FIG 1 ).
- Abraham E, Pankovich AM. Neglected rupture of the Achilles tendon. J Bone Joint Surg Am 1975;57:253–255.
-
Acevedo JI, Weber KS, Eidelman DI. Avoiding wound complications after neglected Achilles tendon repair: tissue expansion technique. Foot Ankle Int 2007;28:393–395.
-
Ademoglu Y, Ozerkan F, Ada S, et al. Reconstruction of skin and tendon defects from wound complications after Achilles tendon rupture. J Foot Ankle Surg 2001;40:158–165.
-
Dalton G, Wapner K, Hecht P. Complications of Achilles and posterior tibial tendon surgeries. Clin Orthop Relat Res 2001;391: 133–139.
-
Kumta SM, Maffulli N. Local flap coverage for soft tissue defects following open repair of Achilles tendon rupture. Acta Orthop Belg 2003;69:59–66.
-
Leppilahti J, Kaarela O, Teerikangas H, et al. Free tissue coverage of wound complications following Achilles tendon rupture surgery. Clin Orthop Relat Res 1996;328:171–176.
-
Ozaki J, Fujiki J, Sugimoto K, et al. Reconstruction of neglected Achilles tendon rupture with Marlex mesh. Clin Orthop Relat Res 1989;238:204–208.
-
Paavola M, Orava S, Leppilahti J, et al. Chronic Achilles tendon overuse injury: complications after surgical treatment. Am J Sports Med 2000;28:77–82.
-
Parker R, Repinecz M. Neglected rupture of the Achilles tendon: treatment by modified Strayer gastrocnemius recession. J Am Podiatry Assoc 1979;69:548–555.
OUTCOMES
- This technique has been used successfully in our practice with no complications related directly to soft tissue expansion.

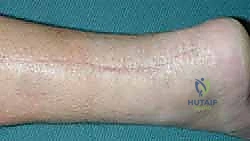
FIG 1 • Outcome 8 weeks after second-stage surgery.