Why Abductor Pollicis Longus Matters in Bennett's Fracture Cases
Patient Presentation & History
We present the case of a 32-year-old male, right-hand dominant, who sustained an injury to his right thumb. The mechanism of injury was a direct axial load to a partially flexed and adducted thumb metacarpal, occurring when he punched a solid object. He reported immediate, severe pain and swelling at the base of his thumb, with an inability to move the digit.
His past medical history is unremarkable, with no significant comorbidities such as diabetes, peripheral vascular disease, or known osteopenia/osteoporosis. He is a non-smoker and takes no regular medications. There is no prior history of trauma or surgery to the affected hand. The patient is employed in a physically demanding role requiring fine motor skills and strong grip strength.
Clinical Examination
Upon initial inspection of the right hand, significant swelling and ecchymosis were noted over the base of the thumb and the thenar eminence. A characteristic "thumb-in-palm" deformity with noticeable shortening of the thumb metacarpal was observed, along with a prominent metacarpal base palpable dorsoradially.
Palpation elicited exquisite tenderness directly over the first carpometacarpal (CMC) joint. Axial loading of the thumb metacarpal through the CMC joint, as well as attempts at passive and active range of motion, reproduced severe pain and demonstrated gross instability.
Active and passive range of motion of the right thumb CMC joint was severely limited and painful, particularly abduction and opposition. Flexion and extension of the interphalangeal (IP) and metacarpophalangeal (MP) joints were also restricted due to the proximal instability and associated pain. Grip strength and pinch strength were impossible to assess due to pain.
Neurological examination revealed intact sensation in the median, ulnar, and radial nerve distributions. Capillary refill was brisk in all digits, and radial and ulnar pulses were palpable and strong, indicating no acute neurovascular compromise. Specific attention was paid to the radial sensory nerve distribution, which remained intact throughout the initial assessment.
Imaging & Diagnostics
Initial radiographic evaluation included standard posteroanterior (PA), lateral, and oblique views of the right hand and thumb. Crucially, a Robert's view (a true AP view of the thumb CMC joint obtained by rotating the wrist 20 degrees internally and the hand 45 degrees internally) was obtained, providing optimal visualization of the first CMC joint.
X-ray Findings
The radiographs demonstrated an intra-articular fracture at the base of the first metacarpal. A small, triangular volar-ulnar fragment (the eponymous "Bennett fragment") was clearly visible, remaining anatomically reduced or minimally displaced relative to the trapezium. The main shaft of the first metacarpal was significantly displaced radially, proximally, and dorsally relative to the Bennett fragment and the trapezium. This characteristic pattern of subluxation and fracture indicated a classic Bennett's fracture-dislocation. There was an estimated articular step-off of approximately 3mm and significant subluxation of the metacarpal shaft.
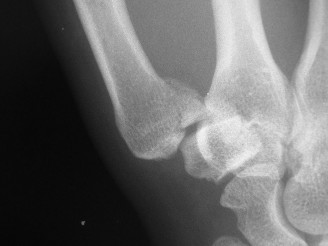
Figure 1: Typical radiographic appearance of a Bennett's fracture-dislocation demonstrating the small volar-ulnar fragment and the proximally, radially, and dorsally displaced metacarpal shaft.
CT/MRI Indications
Given the intra-articular nature of the fracture and the significant displacement observed on plain radiographs, a computed tomography (CT) scan of the right hand was obtained. This was critical for a precise three-dimensional characterization of the articular step-off, the exact size and morphology of the Bennett fragment, potential comminution, and the overall degree of subluxation. The CT confirmed an intra-articular fracture-dislocation with a single, well-defined volar-ulnar fragment and confirmed the main metacarpal shaft's dorsal-radial-proximal displacement. It also ruled out any significant comminution, which would classify it as a Rolando's fracture. Magnetic Resonance Imaging (MRI) was not indicated in this acute setting, as there was no suspicion of significant concomitant ligamentous or tendinous injury requiring detailed soft tissue assessment beyond the fracture itself.
Templating
Pre-operative templating was performed utilizing the CT images to plan the optimal implant size and configuration. The dimensions of the Bennett fragment were assessed to determine if it was amenable to lag screw fixation. If the fragment proved too small for a screw, K-wire fixation or suture anchor through the anterior oblique ligament would be considered. The choice of K-wire diameter and length, or mini-plate size, was estimated to ensure adequate purchase and stability.
Differential Diagnosis
A thorough differential diagnosis is crucial for accurate management. For injuries to the base of the first metacarpal, the primary considerations include:
| Condition | Key Features | Imaging Findings | Treatment Principles |
|---|---|---|---|
| Bennett's Fracture-Dislocation | Axial load on partially flexed/adducted thumb. Intra-articular fracture at 1st CMC joint. Inherent instability due to APL pull. | Small volar-ulnar fragment attached to anterior oblique ligament. Main metacarpal shaft displaced proximally, radially, dorsally. Clear articular incongruity. Robert's view and CT are diagnostic. | Operative: Most require anatomical reduction and stable fixation (CRPP or ORIF with K-wires, lag screw, or mini-plate) due to instability and risk of post-traumatic arthritis. Goals: anatomical reduction of joint surface, stable fixation. |
| Rolando's Fracture | Axial load, often higher energy. Intra-articular, comminuted fracture at 1st CMC joint. | Y-shaped or T-shaped intra-articular fracture pattern with multiple fragments. Often involves dorsal and volar fragments. Significant articular disruption. CT is essential for characterization. | Operative: Complex intra-articular fracture. Often requires ORIF with K-wires, mini-plates, or external fixation with ligamentotaxis. Challenging to achieve anatomical reduction. High risk of post-traumatic arthritis. |
| Extra-articular Fracture of 1st Metacarpal Base | Direct blow or axial load. Fracture proximal to the articular surface. | Transverse or oblique fracture line proximal to the CMC joint. No articular involvement. Metacarpal shaft may be displaced, but joint surface remains intact. | Non-operative: If stable and minimally displaced, thumb spica cast for 4-6 weeks. Operative: If unstable, significantly displaced (>2-3mm), or angulated (>20-30 degrees), CRPP or ORIF (K-wires, small plate). |
| Trapezial Fracture | Less common. Direct trauma or severe axial load through the thumb. Often subtle. | Fracture line within the body of the trapezium. May be associated with 1st CMC joint subluxation or metacarpal base fractures. CT scan is often required for definitive diagnosis due to complex anatomy and overlying structures. | Non-operative: Stable, non-displaced fractures managed with thumb spica. Operative: Displaced, unstable, or intra-articular fragments may require ORIF (K-wires, screws) to restore joint congruity and maintain stability. |
| Ulnar Collateral Ligament (UCL) Injury (Gamekeeper's/Skier's Thumb) | Forced radial deviation of the thumb MP joint. Pain and instability at MP joint. | Radiographs usually normal, but may show avulsion fracture from proximal phalanx base. Stress views may demonstrate instability (>30-35 degrees compared to contralateral side). MRI confirms ligamentous disruption, Bony Bankart lesion or Stener lesion. | Non-operative: Partial tears or stable avulsions treated with thumb spica splint/cast. Operative: Complete tears, Stener lesions, or displaced avulsion fractures require surgical repair/reconstruction to prevent chronic instability and arthritis. |
Surgical Decision Making & Classification
The inherent instability of Bennett's fractures, primarily driven by the deforming forces of the Abductor Pollicis Longus (APL) tendon, mandates careful consideration of operative versus non-operative management.
Why Operative vs. Non-operative?
- Non-operative management: Limited to extremely rare, truly non-displaced Bennett's fractures, or those with minimal articular step-off (<1mm) and no subluxation after reduction, managed with a thumb spica cast. However, due to the biomechanical forces at play, nearly all true Bennett's fractures are unstable and prone to redisplacement. The APL attaches to the base of the first metacarpal shaft, and its unopposed pull causes proximal, radial, and dorsal displacement of the main metacarpal, while the small volar-ulnar fragment remains tethered to the trapezium by the strong anterior oblique ligament (Beak Ligament). This constant deforming force makes maintaining reduction challenging without surgical intervention.
-
Operative management:
Indicated for the vast majority of Bennett's fractures. The primary indications include:
- Any significant articular incongruity (>1-2mm).
- Subluxation of the first metacarpal.
-
Failure to achieve or maintain an acceptable closed reduction.
The goal of surgery is to achieve anatomical reduction of the articular surface and provide stable fixation, thereby restoring the critical thumb CMC joint mechanics and minimizing the risk of post-traumatic osteoarthritis.
Surgical Classifications
While specific classification systems for Bennett's fractures are not as widely used as for other fractures, the concept of reducibility is paramount:
*
Reducible vs. Irreducible:
This dictates the choice between Closed Reduction Percutaneous Pinning (CRPP) and Open Reduction Internal Fixation (ORIF). Most Bennett's fractures are initially reducible but unstable, requiring fixation. Irreducible fractures, often due to interposed soft tissue or impaction, necessitate ORIF.
*
Fragment Size and Comminution:
While not a classification system, the size of the Bennett fragment impacts the choice of fixation. A larger fragment may allow for lag screw fixation, whereas smaller or comminuted fragments might necessitate K-wires or plate fixation. This distinction is critical for differentiating a Bennett's from a Rolando's fracture, where significant comminution changes the surgical strategy considerably.
The role of the Abductor Pollicis Longus is central to surgical decision-making. Its powerful pull is the primary driver of the characteristic metacarpal displacement. Understanding this mechanism is vital for effective reduction maneuvers, which involve counteracting the APL's traction.
Surgical Technique / Intervention
Given the patient's age, activity level, and the significant articular displacement observed, open reduction and internal fixation (ORIF) was chosen to ensure anatomic reduction and rigid fixation, mitigating the risk of future osteoarthritis.
Patient Positioning
The patient was positioned supine on the operating table. The affected right upper extremity was placed on a dedicated hand table. A pneumatic tourniquet was applied to the upper arm. The limb was prepped and draped in a sterile fashion, allowing for a full range of motion of the wrist and thumb.
Approach
A modified dorsal-radial approach to the first CMC joint was utilized. A longitudinal incision approximately 3-4 cm in length was made along the dorsal-radial aspect of the first metacarpal, curvilinearly extending proximally towards the anatomical snuffbox. Careful dissection was performed to protect superficial structures, particularly the sensory branches of the radial nerve and the radial artery, which were identified and retracted. The abductor pollicis longus (APL) tendon sheath was identified and incised to facilitate exposure and allow for manipulation of the metacarpal. The extensor pollicis brevis (EPB) tendon and extensor pollicis longus (EPL) tendon were retracted to visualize the fracture site.
Reduction Techniques
The fracture site was directly visualized. The small volar-ulnar Bennett fragment was found to be anatomically positioned relative to the trapezium, confirming its stable attachment via the anterior oblique ligament. The main shaft of the first metacarpal was significantly displaced dorsally, radially, and proximally.
Reduction involved a multi-pronged approach:
1.
Longitudinal Traction:
Sustained longitudinal traction was applied to the thumb, initially disengaging the metacarpal from its subluxated position.
2.
Abduction:
The thumb metacarpal was then abducted to further release the articular surfaces.
3.
Pronation and Adduction:
While maintaining traction and abduction, the metacarpal was pronated and then gently adducted and pushed distally and ulnarly. This maneuver directly counteracted the deforming forces of the APL and engaged the articular surface of the metacarpal with the stable Bennett fragment. The thumb was effectively brought "out of the palm."
4.
Direct Manipulation:
With direct visualization, specialized reduction forceps were used to gently manipulate the metacarpal shaft back onto the volar-ulnar fragment, achieving an anatomical reduction of the articular surface. A K-wire was temporarily used as a joystick to maneuver the main metacarpal shaft.
The critical insight here is understanding the dynamic role of the Abductor Pollicis Longus. Its tendon inserts into the base of the first metacarpal, proximal to the Bennett fragment. During reduction, continuous traction, coupled with pronation and adduction, helps overcome the APL's deforming pull, bringing the main metacarpal shaft back into alignment with the small, stable fragment. Adequate muscle relaxation also aids in this process.
Fixation Construct
Once anatomical reduction was achieved and confirmed visually, a provisional stabilization with two small K-wires was performed. The articular congruity was meticulously assessed, and no significant step-off or gap was noted.
Definitive fixation was then achieved with a single 1.5mm cortical lag screw, driven from the dorsal-radial aspect of the metacarpal shaft, across the fracture line, and into the Bennett fragment. The fragment was sufficiently large to accommodate the screw, providing rigid interfragmentary compression. The lag screw was carefully placed to avoid penetration into the CMC joint or interference with articular movement.
Additionally, to provide further rotational stability and neutralize potential shear forces, two 0.035-inch K-wires were placed. One K-wire was driven from the tip of the thumb, across the first MP joint, across the CMC joint, and into the trapezium, providing transarticular stabilization. A second K-wire was placed from the base of the first metacarpal into the second metacarpal, providing additional stability against radial displacement. All K-wires were bent and cut outside the skin.
Final intraoperative fluoroscopy confirmed satisfactory reduction and stable internal fixation, with excellent articular congruity and appropriate implant positioning. The wound was copiously irrigated. The APL sheath was loosely repaired. The subcutaneous tissues were closed with absorbable sutures, and the skin was closed with non-absorbable sutures.
Post-Operative Protocol & Rehabilitation
Immobilization
Postoperatively, the patient's hand and wrist were immobilized in a forearm-based thumb spica cast. This cast maintained the thumb in a functional position (slight flexion and abduction) and protected the repair and fixation, ensuring no undue stress on the osteosynthesis. The K-wire tips were incorporated into the cast for protection.
Pin Care
For the percutaneous K-wires, meticulous pin site care was instituted immediately post-operatively, involving daily cleansing with chlorhexidine and sterile dressing changes to minimize the risk of infection.
Radiographic Follow-up
Radiographic follow-up commenced at 1 week post-operatively to confirm maintenance of reduction and implant position. Subsequent X-rays were obtained at 3 weeks, 6 weeks, and 12 weeks to monitor for signs of fracture union and evaluate joint integrity.
Rehabilitation Phases
Phase 1: Immobilization (Weeks 0-6)
*
Goals:
Protect fixation, control pain and edema, maintain motion in uninvolved joints.
*
Activities:
Thumb spica cast worn continuously. Elevation of the hand to reduce swelling. Gentle active range of motion for the shoulder, elbow, and uninjured fingers. Isotonic strengthening for uninvolved wrist and digits. No active or passive motion of the thumb CMC joint. Pin site care as prescribed.
Phase 2: Early Mobilization (Weeks 6-12)
*
Goals:
Restore gentle active and passive thumb range of motion, initiate strengthening.
*
Activities:
At 6 weeks, the thumb spica cast and K-wires were removed following radiographic confirmation of initial fracture healing.
* Initiation of gentle active and passive range of motion exercises for the thumb CMC joint, focusing on flexion, extension, abduction, adduction, and opposition.
* Gentle tendon gliding exercises.
* Scar massage once sutures are removed and wound is healed.
* Progressive strengthening exercises using putty and light resistance bands.
* Referral to an occupational therapist for structured hand therapy.
Phase 3: Advanced Strengthening & Functional Return (Weeks 12+)
*
Goals:
Maximize strength, endurance, and functional use of the hand, return to full activities.
*
Activities:
Progression to advanced strengthening exercises, including grip and pinch strengthening.
* Endurance training.
* Work-specific conditioning.
* Proprioceptive exercises.
* Gradual return to activities of daily living and work, as tolerated and guided by the hand therapist and surgeon. Full return to heavy labor or impact sports is typically advised no sooner than 4-6 months, depending on clinical and radiographic union.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Understanding APL Mechanics: The Abductor Pollicis Longus (APL) is the primary deforming force in Bennett's fractures. It inserts into the base of the first metacarpal shaft, not the stable volar-ulnar fragment. This knowledge is critical for reduction: applying longitudinal traction, pronation, and adduction helps counteract the APL's pull, bringing the metacarpal shaft back into alignment with the fragment.
- Diagnostic Imaging: A Robert's view (true AP of the thumb CMC joint) is indispensable for accurately diagnosing and characterizing the fracture. A CT scan is crucial for surgical planning, assessing articular step-off, fragment size, and any subtle comminution, differentiating it from Rolando's fracture.
- Anatomic Reduction is Paramount: The thumb CMC joint is critical for overall hand function. Any residual articular step-off or incongruity greater than 1-2mm significantly increases the risk of post-traumatic osteoarthritis and chronic pain. Strive for anatomical reduction.
- Fixation Choice: For a single, sufficiently sized Bennett fragment, a lag screw provides excellent interfragmentary compression and rigid fixation. K-wires are versatile, providing temporary stabilization, definitive fixation for smaller fragments, or adjunctive support to a screw or plate construct.
- Ligamentotaxis: For certain reducible fractures, especially if the fragment is very small, ligamentotaxis can be employed (often via external fixation or carefully placed K-wires) to indirectly reduce the articular surface by tensioning the surrounding capsule and ligaments.
- Protection of Radial Sensory Nerve: During an open approach, meticulous dissection is essential to identify and protect the superficial sensory branches of the radial nerve. Injury can lead to painful neuromas or persistent dysesthesias.
Pitfalls
- Inadequate Reduction: The most common pitfall. Failure to achieve or maintain anatomical reduction leads directly to chronic pain, instability, and accelerated post-traumatic osteoarthritis, often necessitating salvage procedures such as CMC arthroplasty or fusion.
- Underestimating Instability: Mistaking a Bennett's for a stable extra-articular fracture or underestimating the deforming force of the APL can lead to non-operative management of an unstable fracture, resulting in malunion and functional impairment.
- Premature Mobilization: Early or aggressive mobilization of the thumb before sufficient healing can disrupt fixation, lead to loss of reduction, and potentially necessitate re-operation. Adherence to a structured rehabilitation protocol is crucial.
- Hardware Prominence/Complications: Prominent K-wire ends can cause irritation or infection. Screw heads or plates placed too superficially can be palpable and uncomfortable, requiring removal. Intra-articular hardware penetration can damage cartilage and lead to arthritis.
- Ignoring Soft Tissue Integrity: While less common than pure bony injury in Bennett's, concomitant ligamentous injuries, especially to the dorsal radial ligament or ulnar collateral ligament of the MP joint, must not be overlooked. Thorough clinical examination and appropriate imaging can identify these.
- Nerve Injury: Iatrogenic injury to the radial sensory nerve during surgical exposure is a significant pitfall, potentially causing chronic pain, paresthesias, or neuromas. Careful surgical technique, including clear identification and protection of nerves, is paramount.
