Introduction & Epidemiology
Complex soft tissue defects of the hand, wrist, and distal forearm present significant reconstructive challenges, often exposing vital structures such as tendons, nerves, bones, joints, and hardware. These critical wounds, resulting from trauma, oncological resection, infection, or chronic ulcers, necessitate robust and reliable soft tissue coverage to preserve function, prevent desiccation, and allow for subsequent reconstructive procedures. Without appropriate coverage, these exposed structures are highly susceptible to infection, necrosis, and fibrosis, leading to devastating functional impairment and potential limb loss.
The reconstructive ladder, a foundational concept in plastic and reconstructive surgery, guides the selection of the most appropriate coverage option, ranging from primary closure to free tissue transfer. Regional pedicled flaps occupy a crucial rung on this ladder, offering a balance between the simplicity of local flaps and the complexity of microsurgical free flaps. Among these, the reverse radial forearm flap (RRFF), also known as the distally based radial forearm flap, has emerged as a workhorse flap for medium to large defects of the dorsal and volar aspects of the hand, wrist, and distal forearm.
Epidemiologically, hand trauma accounts for a substantial proportion of emergency department visits and surgical interventions. Penetrating injuries, crush injuries, degloving injuries, and burns are common etiologies leading to complex soft tissue loss. The incidence of such critical wounds requiring advanced reconstructive techniques is significant, particularly in industrial and agricultural settings, as well as in high-velocity trauma scenarios. The RRFF provides a predictable and versatile solution, leveraging the inherent vascularity and pliability of forearm skin and subcutaneous tissue. Its primary advantage lies in its reliable vascular pedicle, based on reverse flow through the radial artery, which permits transfer of a substantial skin paddle to the recipient site while minimizing donor site morbidity compared to free tissue transfer.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy of the forearm is paramount for successful reverse radial forearm flap harvest and transfer. The flap is an axial pattern flap based on the radial artery and its accompanying venae comitantes, perfused by retrograde flow via the collateral circulation around the elbow, primarily from the ulnar artery through the palmar and dorsal carpal arches.
Radial Artery and Perforators
The radial artery originates from the brachial artery in the cubital fossa and descends along the radial aspect of the forearm, positioned between the brachioradialis laterally and the flexor carpi radialis medially in its proximal two-thirds. Distally, it lies between the brachioradialis and the pronator quadratus. Throughout its course, the radial artery gives off numerous fasciocutaneous perforators that supply the overlying skin and subcutaneous tissue. These perforators can be classified as septocutaneous, running along the intermuscular septum between the brachioradialis and flexor carpi radialis, or musculocutaneous, traversing through muscle bellies. For the RRFF, the perforators typically originate more proximally in the forearm and run distally to supply the skin paddle. The design of the flap must incorporate a sufficient number of these perforators to ensure robust vascularity.
Venous Drainage
The venous drainage of the radial forearm flap is critical for its survival. The flap typically incorporates two large venae comitantes that accompany the radial artery. These veins are crucial for retrograde venous drainage. Superficial veins, such as the cephalic vein, may also be included in the flap design, offering additional venous outflow, although the primary drainage relies on the deep venae comitantes. Patency and integrity of these veins are as vital as the arterial supply.
Innervation
The sensory innervation of the radial forearm skin is primarily supplied by branches of the superficial radial nerve, the medial antebrachial cutaneous nerve, and the lateral antebrachial cutaneous nerve. For sensate reconstruction, a segment of the superficial radial nerve (SRN) can be harvested with the flap. The SRN runs along the radial border of the forearm, deep to the brachioradialis proximally, becoming superficial in the distal third of the forearm to supply sensation to the dorsum of the hand and thumb, index, and middle fingers. Inclusion of a sensory nerve graft within the flap can provide protective sensation to the reconstructed area, significantly enhancing functional outcome. However, harvesting the SRN leads to sensory deficit in its native distribution, a trade-off that must be carefully considered and discussed with the patient.
Biomechanical Considerations
The radial forearm flap offers pliable, thin, and hairless (in many individuals) skin, making it an excellent choice for hand reconstruction where contour, flexibility, and minimal bulk are desirable. The flap can be harvested as fasciocutaneous, preserving the underlying muscle, or as a composite flap including radial periosteum, tendon, or nerve depending on the reconstructive needs. The biomechanical properties of the donor site, specifically the potential for radial artery insufficiency post-harvest, necessitate rigorous preoperative assessment of the ulnar artery's collateral circulation. The pivot point for the reverse flow is typically around the mid-forearm, where the largest perforators are located. The arc of rotation allows the flap to reliably reach the dorsal and volar aspects of the hand, wrist, and proximal digits.
Indications & Contraindications
The reverse radial forearm flap is a versatile and reliable option within the reconstructive armamentarium for hand and wrist surgeons. Its indications are well-defined, leveraging its anatomical advantages, while specific contraindications must be respected to avoid significant morbidity.
Indications for Reverse Radial Forearm Flap
The primary indication for the RRFF is the reconstruction of medium to large soft tissue defects of the hand, wrist, and distal forearm, especially when local tissue options are insufficient or unsuitable. These defects often involve exposure of critical structures such as:
- Exposed bone and joint capsules: Especially around the wrist (radiocarpal, midcarpal joints), metacarpals, and phalanges, where adequate padding is essential.
- Exposed tendons and paratenon: To prevent desiccation, adhesion, and subsequent rupture.
- Exposed nerves and blood vessels: Providing essential coverage for protection and facilitating subsequent repair or grafting.
- Exposed hardware: Following internal fixation of fractures or arthrodesis, the flap offers a robust vascularized bed, reducing infection risk and promoting osteosynthesis.
- Dorsal hand defects: Common after crush injuries, burns, or degloving injuries, where the thin, pliable skin of the forearm matches well.
- Volar wrist defects: Following trauma or tumor resection, particularly when the median nerve or flexor tendons are exposed.
- Web space reconstruction: For deep defects requiring both volume and pliability.
- Proximal digit reconstruction: When defects extend from the hand onto the base of the fingers.
- Chronic ulcers and osteomyelitis: Providing well-vascularized tissue to eradicate infection and promote healing.
- Reconstruction requiring a sensate flap: If the superficial radial nerve is harvested with the flap, it can provide protective or even discriminative sensation to the recipient site.
Contraindications for Reverse Radial Forearm Flap
Absolute and relative contraindications must be carefully evaluated pre-operatively to ensure patient safety and flap viability.
- Compromised ulnar artery (Absolute): This is the most critical contraindication. The entire principle of the reverse radial forearm flap relies on retrograde flow from the ulnar artery via the palmar and dorsal carpal arches. A negative Allen's test, confirming inadequate ulnar artery collateral circulation, makes the use of this flap unsafe as it risks significant ischemia to the entire hand following radial artery harvest. Doppler ultrasound or angiography may be used for further confirmation in ambiguous cases.
- Compromised radial artery in the donor forearm (Absolute): Previous trauma, surgical intervention, or severe atherosclerotic disease affecting the radial artery or its perforators in the planned donor forearm will compromise flap vascularity.
- Active infection in the donor site (Absolute): Harvesting through an infected field risks spreading infection and compromising flap viability.
- Severe scarring or previous trauma to the donor forearm (Relative): Extensive scarring from previous burns, trauma, or surgery in the forearm can compromise the vascular pedicle or flap harvest.
- Need for free tissue transfer (Relative): For very large defects extending beyond the reach of the RRFF, or when specific tissue characteristics (e.g., bone, large muscle bulk) are required, a free flap might be a more appropriate choice.
- Patient preference / concerns about donor site morbidity: While not a medical contraindication, the patient must be thoroughly counseled on the potential for an aesthetically unappealing donor site scar, sensory changes, and possible donor site pain.
Summary of Operative vs. Non-Operative Indications
| Category | Operative Indications (Reverse Radial Forearm Flap) | Non-Operative / Alternative Indications (Not RRFF) |
|---|---|---|
| Soft Tissue Defects | Exposed tendon, bone, joint, nerve, vascular structures; chronic ulcers; complex trauma requiring stable coverage; large defects. | Small, superficial wounds amenable to secondary intention, simple closure, or skin grafts (if healthy, well-vascularized bed). |
| Vascular Status | Patent ulnar artery collateral circulation (positive Allen's test); intact radial artery in donor forearm. | Compromised ulnar artery (negative Allen's test); previous radial artery injury/harvest in donor forearm. |
| Flap Dimensions/Quality | Medium to large defects of the hand, wrist, distal forearm requiring pliable, durable, often sensate, coverage. | Very small defects (local flaps sufficient); very large or composite defects requiring free tissue transfer (e.g., large muscle, vascularized bone). |
| Recipient Bed | Recipient site with exposed critical structures or compromised local vascularity requiring a robust pedicled flap. | Granulating wounds without exposed critical structures, where secondary intention or skin grafting is viable. |
| Patient Factors | Medically stable; able to tolerate prolonged surgery and anesthesia; compliance with post-op care. | Unstable patient; uncontrolled systemic infection; severe comorbidities precluding surgery. |
| Functional Goals | High functional demands requiring protective sensation, durable coverage, and minimal bulk. | Defects where aesthetic outcome or sensation is less critical, and simpler methods suffice. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes with the reverse radial forearm flap, encompassing patient assessment, vascular evaluation, and surgical strategy.
Patient Assessment
-
Detailed History and Physical Examination:
- Etiology of defect: Trauma, infection, tumor resection, chronic wound. Understand the mechanism and extent of injury.
- Comorbidities: Diabetes, peripheral vascular disease, smoking status, connective tissue disorders, previous surgeries, and medication use (especially anticoagulants). These factors can significantly impact healing and flap viability.
- Hand dominance: The non-dominant forearm is generally preferred as a donor site to minimize functional impact.
- Hair distribution: For aesthetic considerations, especially on the dorsum of the hand, the hair pattern of the forearm should be noted and discussed with the patient.
- Forearm skin quality: Assess for scars, radiation damage, or other conditions that might compromise flap harvest.
-
Vascular Assessment:
- Allen's Test: This is an essential and mandatory screening test. Occlude both radial and ulnar arteries at the wrist, ask the patient to clench and unclench the fist several times until the hand blanches. Release ulnar compression and observe capillary refill in the hand. Normal refill within 5-7 seconds confirms adequate ulnar collateral circulation, making radial artery harvest safe. A delayed or absent refill indicates an unsafe ulnar collateral system and is an absolute contraindication for RRFF.
- Doppler Ultrasound: Used to confirm radial and ulnar artery patency and flow, especially if the Allen's test is equivocal or if there's a history of trauma to the forearm vessels.
- Angiography (rarely): Reserved for complex cases with suspected vascular anomalies or extensive trauma to the forearm vasculature, or for patients with significant peripheral vascular disease.
-
Defect Templating and Flap Design:
- Accurate measurement: The recipient defect should be precisely measured, and a template created from sterile material (e.g., glove wrapper, suture packet).
- Flap dimensions: The template is then placed on the planned donor forearm. The skin paddle is typically designed as an ellipse or spindle shape, centered over the course of the radial artery. The distal margin of the flap should be at least 2-3 cm proximal to the radial styloid to preserve the distal perforators for hand blood supply and minimize donor site morbidity. The proximal margin depends on the required length, but it's important to ensure sufficient perforators are included, and the pivot point is around the mid-forearm.
- Sensate flap consideration: If a sensate flap is desired, the course of the superficial radial nerve should be identified and marked.
- Donor site closure plan: Consider whether the donor site can be closed primarily (small flaps, typically <3-4 cm width) or will require a skin graft (larger flaps). The expected cosmetic and functional outcome of the donor site should be discussed.
Patient Positioning and Anesthesia
- Anesthesia: General anesthesia is typically employed. Regional nerve blocks (e.g., axillary block) can be used as an adjunct or for post-operative analgesia.
- Positioning: The patient is positioned supine with the affected arm and the donor forearm extended on separate hand tables. This allows for simultaneous access to both the recipient and donor sites by the surgical team. The arm should be abducted, pronated, and appropriately padded to prevent nerve compression. A pneumatic tourniquet is applied to the upper arm of the donor limb to facilitate a bloodless field during flap elevation.
Additional Pre-operative Considerations
- Antibiotics: Prophylactic broad-spectrum antibiotics are administered prior to incision.
- Sterile preparation: Both the recipient and donor sites, as well as the entire upper extremity, are prepped and draped in a sterile fashion.
- Instrumentation: Ensure availability of microsurgical instruments, loupe magnification (2.5x to 4.5x), and Doppler probe for intra-operative flow assessment.
Detailed Surgical Approach / Technique
The successful harvest and transfer of the reverse radial forearm flap require meticulous technique and a systematic approach to ensure flap viability and optimize functional outcomes.
1. Recipient Site Preparation
- The recipient site on the hand or wrist is thoroughly debrided of all non-viable tissue, including necrotic skin, subcutaneous tissue, muscle, and bone.
- Hemostasis is achieved.
- The wound bed is irrigated copiously. All exposed critical structures (tendons, nerves, bones, hardware) are identified and prepared for coverage.
- Measurements of the final defect are re-confirmed.
2. Flap Design on the Forearm
- With the arm positioned on a hand table, the radial artery course is identified and marked using a Doppler probe.
- The proposed skin paddle is drawn as an ellipse or spindle shape on the volar aspect of the forearm, centered over the radial artery.
- The distal margin of the skin paddle should be at least 2-3 cm proximal to the radial styloid to preserve distal perforators to the hand and minimize aesthetic concerns at the wrist.
- The proximal extent of the flap is determined by the required length to reach the recipient site, typically extending to the mid-forearm or even more proximally, depending on the pivot point and arc of rotation.
- The superficial radial nerve, if intended for harvest with the flap (for a sensate flap), is also marked.
- The entire extremity is then sterilely prepared and draped, and the tourniquet is inflated.
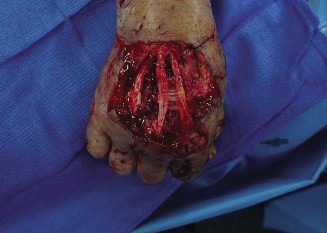
Figure 1: Intraoperative marking of the reverse radial forearm flap on the volar forearm, illustrating the planned skin paddle centered over the radial artery. The distal margin is typically maintained 2-3 cm proximal to the radial styloid to preserve local circulation and minimize donor site morbidity.
3. Flap Elevation (Proximal-to-Distal or Distal-to-Proximal)
Two main approaches exist for flap elevation:
A. Proximal-to-Distal Dissection (Commonly preferred):
* An incision is made along the ulnar border of the planned skin paddle, extending down to the deep fascia.
* The plane of dissection is then developed subfascially, lifting the skin and subcutaneous tissue, including the deep fascia. The flexor carpi ulnaris and flexor digitorum superficialis muscles are encountered. Care is taken to preserve the paratenon of these muscles if possible.
* The radial artery and its venae comitantes are identified proximally. The artery is ligated and divided at the proximal extent of the flap.
* Dissection proceeds distally, meticulously identifying and preserving the radial artery and its two venae comitantes. All small muscular and septocutaneous branches originating proximally from the radial artery and entering the deep muscles are ligated and divided.
* The flexor carpi radialis tendon is usually left intact, and the radial artery is freed from its attachment to the forearm musculature.
B. Distal-to-Proximal Dissection:
* This approach begins by incising the skin paddle distally. The radial artery and its venae comitantes are identified near the distal limit of the flap.
* Dissection then proceeds proximally, identifying and preserving the vascular pedicle. This approach allows for early confirmation of flap vascularity and retrograde flow.
4. Pedicle Dissection and Inclusion of SRN
- The radial artery, with its two accompanying venae comitantes, is carefully dissected from its surrounding tissues. All branches originating from the radial artery that do not supply the flap skin paddle must be ligated and divided to ensure maximal retrograde flow through the main pedicle.
- The superficial radial nerve (if a sensate flap is desired) is identified and dissected proximally with the pedicle. It typically lies deep to the brachioradialis muscle proximally and becomes superficial in the distal forearm. A segment of the nerve is included with the flap and can be coapted to a suitable recipient nerve branch at the defect site (e.g., digital nerve stumps).
- The cephalic vein (a superficial vein) may also be harvested with the flap to provide additional venous drainage, particularly for larger flaps or in cases where venous congestion is anticipated.
5. Flap Transposition and Inset
- Once the flap is completely elevated and confirmed to have robust retrograde arterial flow and venous drainage (visualized after brief release of the tourniquet, if desired, or relying on visual appearance and Doppler signals), it is ready for transposition.
- The flap can be transferred to the recipient site via a subcutaneous tunnel or by creating a direct defect connecting the donor and recipient sites. Tunneling should be wide enough to prevent compression of the vascular pedicle.
- The flap is meticulously inset into the recipient defect using interrupted sutures. Care is taken to ensure that there is no tension on the flap and that the pedicle is not twisted or compressed.
- Confirm flap viability again: color, turgor, capillary refill, and Doppler signals over the pedicle and within the flap.
6. Donor Site Closure
- The donor site defect can be closed primarily if the flap is narrow (typically <3-4 cm) and tension-free. This is generally preferred to minimize morbidity.
- For wider flaps, primary closure is not feasible, and the defect is covered with a full-thickness or split-thickness skin graft. If a skin graft is used, the paratenon of the flexor tendons must be preserved to ensure a viable bed for the graft.
- A non-adherent dressing is applied, followed by a bolus dressing over the skin graft to ensure good coaptation.
- A drain is often placed in the donor site to prevent hematoma formation.
7. Tourniquet Deflation and Final Assessment
- The tourniquet is deflated.
- The flap is reassessed for perfusion immediately and over the next several minutes. The flap should be pink, warm, and have good capillary refill. Doppler signals are re-checked.
- The donor site is checked for adequate hemostasis before final dressing.
- A gentle, non-constricting dressing is applied to both the donor and recipient sites. The hand is typically immobilized in a position of function with a splint.
Complications & Management
Despite its reliability, the reverse radial forearm flap is not without potential complications, which can affect both the flap itself and the donor site. Prompt recognition and appropriate management are crucial for salvage and optimal outcomes.
1. Flap-Related Complications
-
Partial Flap Necrosis:
- Incidence: 5-15%, often involving the distal-most portion of the skin paddle.
- Cause: Insufficient retrograde arterial flow, venous congestion (most common), or excessive tension during inset.
- Management: Conservative management for superficial necrosis (dressing changes, debridement), re-exploration for deeper or progressive necrosis to assess the pedicle. If the pedicle is patent, local debridement and secondary intention or smaller local flaps may suffice. If the pedicle is compromised, alternative coverage might be necessary.
-
Total Flap Necrosis:
- Incidence: <1%, a rare but devastating complication.
- Cause: Complete pedicle compromise (arterial occlusion or venous thrombosis), severe infection, or technical error during harvest/transfer.
- Management: Urgent re-exploration is mandatory. If a vascular compromise is identified (e.g., pedicle kinking, thrombosis), revision of the vascular repair or release of compression may be attempted. If the flap is unsalvageable, it must be debrided, and an alternative reconstructive option (e.g., free flap) should be planned.
-
Venous Congestion:
- Incidence: Variable, often associated with partial necrosis.
- Cause: Inadequate venous drainage, twisting of pedicle, external compression.
- Management: Elevate the extremity, apply warm compresses to the pedicle, consider releasing tight sutures, leeches, or heparin paste. If severe, re-exploration may be necessary to identify and revise the congested veins or incorporate additional venous outflow.
-
Hematoma/Seroma under Flap:
- Incidence: 1-3%.
- Cause: Inadequate hemostasis, poor drainage.
- Management: Small hematomas/seromas can be aspirated. Larger or expanding collections require surgical evacuation, hemostasis, and placement of a drain.
2. Donor Site Complications
-
Donor Site Pain/Scarring:
- Incidence: Very common, almost universal to some degree. The scar can be conspicuous, especially if a skin graft is used.
- Cause: Inherent consequence of tissue harvest. Nerve irritation contributes to pain.
- Management: Patient counseling pre-operatively is paramount. Post-operatively, pain management, scar massage, silicone sheeting, and sometimes revision surgery for hypertrophic or keloid scars.
-
Donor Site Nerve Injury (Superficial Radial Nerve):
- Incidence: 5-10% if SRN is not harvested. Higher if specifically harvested, leading to planned sensory deficit.
- Cause: Direct trauma during dissection, neuroma formation, or nerve entrapment in the scar. If the SRN is harvested for a sensate flap, a sensory deficit in its distribution is an expected outcome.
- Management: Conservative management for mild neurapraxia. Neuropathic pain may require medication. For painful neuromas, surgical excision and burying the nerve ending into muscle or bone can be considered. For a sensate flap, the planned sensory deficit should be explained.
-
Donor Site Functional Deficit:
- Incidence: 2-5%, typically mild loss of grip strength or wrist flexion.
- Cause: Removal of deep fascia, scar contracture, or secondary effects of nerve injury.
- Management: Aggressive hand therapy, range of motion exercises, strengthening. Usually resolves with time and rehabilitation.
-
Skin Graft Loss at Donor Site:
- Incidence: Variable, depending on technique and patient factors.
- Cause: Hematoma, seroma, infection, shear forces, inadequate immobilization, poor graft take.
- Management: Debridement of necrotic graft, local wound care, possible re-grafting.
-
Radial Artery Insufficiency (Extremely rare if Allen's test positive):
- Incidence: <0.1% when proper pre-operative assessment is performed.
- Cause: Failure to identify compromised ulnar collateral circulation, or concurrent injury/disease in the ulnar artery.
- Management: Urgent surgical exploration, possible radial artery reconstruction (e.g., vein graft), or revascularization procedures. This can lead to hand ischemia and potential limb loss if not promptly addressed.
-
Infection:
- Incidence: 2-8%, affecting either the donor or recipient site.
- Cause: Contamination during surgery, hematoma, compromised circulation.
- Management: Culture-directed antibiotics, local wound care, debridement of infected tissue.
Table of Common Complications and Management
| Complication | Incidence (Approx.) | Primary Management Strategy | Salvage Strategies (if primary fails) |
|---|---|---|---|
| Partial Flap Necrosis | 5-15% | Conservative wound care, debridement, address venous congestion. | Local flap advancement, secondary intention, small skin graft. |
| Total Flap Necrosis | <1% | Urgent exploration, vascular revision (if pedicle compromise found). | Debridement, alternative coverage (e.g., free flap, distant pedicled flap). |
| Venous Congestion | Variable | Elevate, warm compresses, release tight sutures, leeches, heparin paste. | Surgical revision of venous outflow, additional venous anastomosis. |
| Donor Site Pain/Scarring | Common | Counseling, pain management, scar massage, silicone sheeting. | Scar revision, neuroma excision if nerve involved. |
| Donor Site Nerve Injury (SRN) | 5-10% | Conservative, neuropathic pain meds, physical therapy. | Neuroma excision and implantation, nerve grafting (rare). |
| Donor Site Functional Deficit | 2-5% | Aggressive hand therapy, range of motion, strengthening. | Continued physical therapy, functional splinting. |
| Skin Graft Loss (Donor) | Variable | Local wound care, serial debridement, bolster dressing. | Re-grafting, local flap for persistent defects. |
| Radial Artery Insufficiency | <0.1% (with Allen's) | Urgent re-exploration, radial artery reconstruction (e.g., vein graft). | Vascular bypass, embolectomy, consider amputation in extreme cases. |
| Infection | 2-8% | Culture-directed antibiotics, incision & drainage, debridement. | Further debridement, flap removal if recalcitrant, alternative coverage. |
| Hematoma/Seroma | 1-3% | Aspiration, compressive dressing. | Surgical evacuation, hemostasis, drain placement. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as crucial as the surgical technique itself for maximizing functional outcomes and minimizing complications following reverse radial forearm flap reconstruction. A multidisciplinary approach involving the surgeon, hand therapist, and patient is essential.
1. Immediate Post-Operative Period (Day 0-7)
- Immobilization: The reconstructed hand and donor forearm are typically immobilized in a custom thermoplastic or plaster splint in a position of safety (wrist slightly extended, MP joints flexed 70-90 degrees, IP joints extended) for optimal flap protection and healing. This also supports the donor site skin graft if applicable.
- Elevation: The entire upper extremity is continuously elevated above heart level to minimize edema in both the flap and the hand.
- Flap Monitoring: Frequent (hourly for the first 24-48 hours, then every 2-4 hours) monitoring of flap color, capillary refill, temperature, and Doppler signals is critical. Any changes (pallor, cyanosis, coldness, absent Doppler) warrant immediate surgical notification.
- Pain Management: Adequate pain control is provided.
- Wound Care: Donor site dressings (especially over skin graft) are typically left undisturbed for 5-7 days. The recipient site dressing is kept clean and dry.
- Early Mobilization (Non-operated joints): Gentle active range of motion (AROM) exercises for non-immobilized joints (e.g., shoulder, elbow) are encouraged to prevent stiffness and promote venous return.
2. Early Rehabilitation Phase (Weeks 1-4)
- Splinting: The immobilization splint is maintained, but may be adjusted for comfort or to allow access for gentle wound care.
- Edema Management: Continued elevation, light compression gloves (if flap stability allows), and gentle retrograde massage (avoiding direct pressure on the flap or pedicle).
- Wound Care: Donor site skin graft dressings are changed. If the graft has taken well, gentle massage and moisturization can begin on surrounding skin. Recipient site suture removal typically occurs at 10-14 days.
- Gentle AROM: If the flap is stable and without signs of vascular compromise, and depending on the structures covered (e.g., if tendons were not involved or were repaired), very gentle, pain-free active range of motion of the fingers or wrist may begin under therapist guidance. Passive range of motion (PROM) is generally avoided early to protect the healing flap.
- Sensory Re-education (if sensate flap): If a sensate flap was performed, early sensory re-education (e.g., protective sensation awareness, localization) may begin cautiously, though significant return takes months.
3. Intermediate Rehabilitation Phase (Weeks 4-12)
- Gradual Increase in ROM: Progressive active and passive range of motion exercises for the hand and wrist. The focus is on regaining full joint mobility without stressing the flap.
- Strengthening: Gentle isometric exercises are introduced, gradually progressing to light resistance exercises as healing allows and flap stability is confirmed.
- Scar Management: Aggressive scar management using silicone products, massage, and custom compression garments for both donor and recipient sites to minimize hypertrophy and contracture.
- Sensory Re-education: Continued, more intensive sensory re-education if a sensate flap was performed, focusing on discrimination and texture recognition.
- Donor Site Care: Continued scar management and exercises for the donor forearm.
- Functional Activities: Incorporation of light, functional activities of daily living (ADLs).
4. Advanced Rehabilitation Phase (Months 3-6+)
- Progressive Strengthening: Increase resistance and intensity of strengthening exercises.
- Endurance Training: Activities to improve muscular endurance.
- Coordination and Dexterity: Fine motor tasks, grip strengthening, and dexterity exercises.
- Return to Activity: Gradual return to work, sports, and avocational activities, guided by functional tolerance and flap maturity.
- Sensory Reintegration: Continued focus on sensory return and cortical integration for sensate flaps.
- Psychosocial Support: Address any body image concerns related to the donor site scar or functional limitations.
Throughout all phases, close communication between the surgeon and hand therapist is paramount to adjust protocols based on individual patient progress, flap healing, and potential complications. Strict adherence to rehabilitation guidelines helps achieve the best possible functional and aesthetic outcomes.
Summary of Key Literature / Guidelines
The reverse radial forearm flap has a rich history and a robust evidence base supporting its utility in hand and wrist reconstruction. Its development and refinement have been documented extensively in the plastic and orthopedic literature, establishing it as a cornerstone technique.
-
Historical Context: The radial forearm flap was first described as a free flap by Yang et al. in 1981 in China for head and neck reconstruction. Its application as a distally-based (reverse) pedicled flap for hand reconstruction was subsequently popularized by numerous authors, including Song et al., and extensively reviewed by Orthopedic and Plastic surgeons globally, solidifying its place in the reconstructive ladder.
-
Reliability and Versatility: Numerous studies and systematic reviews consistently report high success rates for the RRFF, with complete flap survival ranging from 90% to 99%. Its versatility stems from its consistent vascular anatomy, ability to harvest a large, thin, and pliable skin paddle, and the option to include sensory nerves for re-innervation. It can be tailored to various defect sizes and locations on the dorsal and volar aspects of the hand, wrist, and distal digits.
-
Comparison to Other Regional Flaps:
- Posterior Interosseous Artery Flap (PIAF): While also a reliable regional flap for hand coverage, the PIAF is technically more demanding due to the smaller, less consistent caliber of the posterior interosseous artery and its perforators. It also requires more extensive dissection and has a more limited arc of rotation compared to the RRFF. However, the PIAF has the advantage of preserving the main forearm vessels (radial and ulnar arteries) and causing less visible donor site morbidity.
- Ulnar Artery Perforator Flap: Similar to the RRFF in principle, but based on the ulnar artery. Its harvest is generally considered more complex due to the deeper course of the ulnar artery and variability of its perforators.
- Local Flaps: For smaller, less complex defects, local flaps (e.g., V-Y advancement, rotation flaps) are often the first choice. However, they are limited by the availability of healthy adjacent tissue and may not provide sufficient bulk or reach.
- Cross-Finger Flaps / Thenar Flaps: Useful for specific digital defects but limited in size and typically require a two-stage procedure.
-
Comparison to Free Flaps: For very large or complex defects involving multiple tissue types (e.g., large bone defects, extensive muscle loss), free tissue transfer (e.g., anterolateral thigh flap, gracilis muscle flap) offers superior versatility in terms of tissue volume and type. However, free flaps require microsurgical expertise, longer operative times, and have a higher risk of total flap loss if the anastomoses fail. The RRFF provides a bridge between simpler local options and complex free flaps, offering a robust and relatively straightforward solution with acceptable donor site morbidity.
-
Donor Site Morbidity: While the RRFF is highly successful, donor site morbidity remains a significant consideration. The prominent scar on the volar forearm, potential for skin graft complications, and the intentional sacrifice of the radial artery are often cited drawbacks. Studies have shown variable degrees of donor site pain, sensory changes, and reduced grip strength, though often clinically minor. Patient counseling regarding these aspects is critical. The meticulous pre-operative Allen's test is a non-negotiable guideline to prevent radial artery insufficiency to the hand.
-
Sensate Flap Reconstruction: The ability to incorporate the superficial radial nerve to create a sensate flap for critical areas requiring protective or discriminative sensation (e.g., thumb pulp reconstruction, web space) is a major advantage highlighted in literature. While the quality of sensation varies, it often provides protective sensation and improves functional outcomes.
-
Current Guidelines: Contemporary surgical guidelines emphasize a systematic approach to hand reconstruction, prioritizing the simplest effective method. The RRFF is considered a reliable and primary option for medium-to-large soft tissue defects of the hand and wrist when local options are inadequate and free tissue transfer is deemed overly complex or unnecessary. Rigorous preoperative vascular assessment and meticulous surgical technique remain the cornerstones of successful outcomes. Ongoing research continues to explore modifications to flap design, donor site closure techniques, and rehabilitation protocols to further minimize morbidity and optimize functional results.
