Patient Presentation & History
A 32-year-old right-hand dominant male presented to the emergency department approximately 2.5 hours after sustaining a laceration to his left volar distal forearm. The mechanism of injury involved a broken glass pane while he was performing home renovations. He reported immediate, significant bleeding controlled by direct pressure applied by himself and a bystander, followed by profound numbness and an inability to move his thumb and index finger.
The patient is a self-employed electrician, highlighting the critical importance of left-hand function for bimanual tasks. His past medical history was notable for well-controlled essential hypertension, for which he took amlodipine 5mg daily. He denied any history of diabetes, peripheral neuropathy, or coagulopathy. He was a non-smoker and consumed alcohol occasionally. There were no known drug allergies. Tetanus immunization status was up-to-date.
Upon initial assessment in the emergency department, he was hemodynamically stable, though anxious. Examination revealed a circumferential dressing applied by pre-hospital personnel.
Clinical Examination
Following removal of the temporary dressing, a focused neurovascular and musculoskeletal assessment of the left upper extremity was performed.
Inspection
A jagged, approximately 5 cm oblique laceration was present on the volar aspect of the left distal forearm, positioned just proximal to the wrist crease, extending from the radial aspect towards the central forearm. There was evidence of active oozing from the wound. No obvious deformity or gross instability was noted. The overlying skin appeared viable, without signs of pallor or cyanosis.
Palpation
Palpation around the wound elicited tenderness. The radial and ulnar pulses were both strong and palpable at the wrist. Capillary refill in all digits was brisk, estimated at <2 seconds. Sensation to light touch was intact on the dorsal hand and digits, and in the ulnar nerve distribution on the palmar aspect.
Range of Motion
- Wrist: Active range of motion was pain-limited but present for both flexion and extension. Passive range of motion was full but elicited pain at extremes.
-
Digits:
- Thumb: Complete inability to actively flex the interphalangeal (IP) joint and a profound inability to abduct or oppose the thumb metacarpophalangeal (MCP) joint.
- Index Finger: Complete inability to actively flex the distal interphalangeal (DIP) joint and marked weakness in active flexion of the proximal interphalangeal (PIP) joint.
- Middle Finger: Similar to the index finger, there was significant weakness in active flexion of both DIP and PIP joints.
- Ring and Little Fingers: Active flexion of DIP and PIP joints was intact, suggesting preservation of the ulnar innervated flexor digitorum profundus (FDP) to these digits.
Neurological Assessment
A detailed neurological examination was crucial for localizing the injury.
*
Median Nerve:
*
Sensory:
Complete anesthesia to light touch, pinprick, and two-point discrimination over the palmar aspect of the thumb, index finger, middle finger, and the radial half of the ring finger. Sensation was also absent on the dorsal aspect of the distal phalanges of the index and middle fingers.
*
Motor:
Absent active thumb abduction (abductor pollicis brevis - APB) and opposition (opponens pollicis). Inability to flex the IP joint of the thumb (flexor pollicis longus - FPL) and the DIP joints of the index and middle fingers (FDP to index/middle). Significant weakness in PIP joint flexion of the index and middle fingers (flexor digitorum superficialis - FDS to index/middle).
*
Ulnar Nerve:
Sensory function was intact in the ulnar distribution (palmar and dorsal aspects of the little finger and ulnar half of the ring finger). Motor function was intact, with preserved intrinsic muscle function (e.g., first dorsal interosseous strength, adductor pollicis strength, little finger abduction).
*
Radial Nerve:
Sensory and motor function was intact throughout its distribution.
This constellation of deficits strongly indicated a combined injury to the median nerve and multiple flexor tendons at the level of the distal forearm. The presence of both sensory and motor deficits within the median nerve distribution, coupled with specific flexor tendon deficiencies (FPL, FDP index/middle, FDS index/middle), necessitated surgical exploration.
Imaging & Diagnostics
Plain Radiographs
Anteroposterior, lateral, and oblique radiographs of the left wrist and hand were obtained.
*
Findings:
No acute fractures, dislocations, or subluxations were identified. No radio-opaque foreign bodies, such as glass shards, were visualized within the soft tissues. This suggested a relatively clean transection rather than a crush injury with retained fragments.
Other Imaging Modalities
- Ultrasound: While sometimes utilized for evaluating soft tissue injuries, an acute, open laceration often limits its diagnostic utility due to air in the wound, pain, and the need for immediate surgical intervention. Its role is primarily in diagnosing occult injuries or in delayed presentations.
- Computed Tomography (CT) Scan: Not indicated acutely in this case, as there was no suspicion of bony involvement (fracture) or deeply embedded, non-radio-opaque foreign bodies that would alter immediate surgical management.
- Magnetic Resonance Imaging (MRI): Not indicated acutely. MRI offers superior soft tissue contrast for nerve and tendon evaluation but is time-consuming, expensive, and generally contraindicated in the acute setting of an open wound requiring emergent exploration. Its role is more in chronic non-unions, missed diagnoses, or post-surgical complications.
Laboratory Investigations
Pre-operative blood tests included a complete blood count (CBC), coagulation profile (PT/INR, aPTT), and type and screen. All results were within normal limits, confirming the patient's suitability for immediate surgical intervention.
Differential Diagnosis
The clinical presentation of a traumatic hand injury with neurological and motor deficits warrants a structured approach to differential diagnosis to ensure accurate and timely management.
| Feature | Median Nerve Transection + Tendon Lacerations (Likely Case) | Acute Forearm Compartment Syndrome | Isolated Flexor Tendon Lacerations | Arterial Laceration with Ischemia (e.g., Ulnar/Radial Artery) |
|---|---|---|---|---|
| Mechanism | Sharp trauma (glass, knife), laceration | Crush injury, reperfusion injury, high-pressure injection, tight cast | Sharp trauma, laceration, avulsion | Sharp trauma, laceration, blunt trauma, fracture |
| Pain | Moderate, localized to wound, may radiate with nerve irritation | Severe, out of proportion to injury, exacerbated by passive stretch | Moderate, localized to wound, with movement | Variable, may be severe if concomitant nerve injury, often less prominent |
| Sensory Deficit | Specific median nerve distribution (thumb, IF, MF, radial RF palmar) | Paresthesias, then anesthesia (late sign) distal to compartment | Intact sensation distal to injury | Global distal paresthesias/anesthesia, progressing to full loss |
| Motor Deficit | Absent median-innervated muscle function, specific tendon deficits | Progressive paralysis of involved muscles distal to compartment | Absent/weak specific digit flexion corresponding to injured tendons | Global distal paralysis (late sign) |
| Vascular Exam | Intact pulses, brisk capillary refill, normal skin color/temperature | Intact pulses early, diminished/absent late, prolonged capillary refill, tense compartment | Intact pulses, brisk capillary refill, normal skin color/temperature | Absent/diminished pulses, prolonged capillary refill, pallor, coolness |
| Edema/Swelling | Localized to wound, minimal generalized swelling | Significant, diffuse, tense forearm swelling | Localized to wound, potentially minimal swelling | Variable, may be absent or localized to wound |
| Pressure | Normal tissue pressure | Elevated compartment pressures (>30 mmHg or ΔP < 30 mmHg) | Normal tissue pressure | Normal or slightly elevated, but not typically compartment syndrome levels |
| Management | Urgent surgical exploration, primary repair of nerve and tendons | Emergent fasciotomy | Urgent surgical repair of tendons | Emergent vascular repair/reconstruction, often with nerve/tendon repair |
In the presented case, the clear presence of a laceration, discrete sensory and motor deficits corresponding specifically to the median nerve distribution, and preserved distal pulses effectively ruled out acute compartment syndrome and significant arterial transection as primary diagnoses. While isolated tendon lacerations would explain the motor deficits, the co-occurrence of sensory deficits definitively implicated the median nerve. Therefore, the leading diagnosis was median nerve and flexor tendon transections.
Surgical Decision Making & Classification
Operative vs. Non-Operative
Given the nature of a sharp, open laceration with clear evidence of median nerve and flexor tendon transections, immediate surgical exploration and repair are unequivocally indicated. There is no role for non-operative management in such injuries, as spontaneous recovery of a completely transected nerve (Sunderland Grade V neurotmesis) or tendon is not possible. Delaying surgical intervention significantly compromises functional outcomes, particularly for nerve repair.
Timing of Intervention
Optimal outcomes for both nerve and tendon repairs are achieved with primary repair, ideally within 6-12 hours of injury. For nerve injuries, delaying beyond 72 hours can lead to retraction of nerve stumps, scar formation, and degeneration, making direct repair more challenging and potentially requiring nerve grafting. For tendon injuries, primary repair within 1-2 weeks is generally acceptable, but immediate repair minimizes retraction, inflammation, and scar tissue formation, facilitating a smoother rehabilitation course. In this case, the patient was taken to the operating theatre within 4 hours of injury.
Classification of Nerve Injury
The Sunderland classification is a widely used system to describe the severity of nerve injuries:
*
Grade I (Neurapraxia):
Conduction block without axonal disruption. Recovery is complete and rapid.
*
Grade II (Axonotmesis):
Axonal disruption but intact endoneurium. Wallerian degeneration occurs, but regeneration is typically good as the endoneurial tubes are preserved.
*
Grade III (Neurotmesis):
Axonal and endoneurial disruption, but intact perineurium. Regeneration is less predictable due to potential disorganization within the fascicles.
*
Grade IV (Neurotmesis):
Disruption of axons, endoneurium, and perineurium, but the epineurium is intact. Requires surgical repair as disorganization is significant.
*
Grade V (Neurotmesis):
Complete transection of the entire nerve trunk. Requires surgical repair.
Based on the clinical findings of complete sensory and motor loss following a sharp laceration, a Sunderland Grade V neurotmesis of the median nerve was highly suspected.
Classification of Tendon Injury
Flexor tendon injuries are typically classified by anatomical zones:
*
Zone I:
Distal to the FDS insertion, involving only FDP.
*
Zone II ("No Man's Land"):
From the FDS insertion to the A1 pulley. Involves both FDS and FDP, often with complex adhesions due to synovial sheath. This is a common and challenging zone for repair.
*
Zone III:
From the A1 pulley to the distal carpal tunnel. Involves intrinsic muscles, lumbricals, and proximal FDS/FDP.
*
Zone IV:
Within the carpal tunnel. Involves multiple flexor tendons and the median nerve.
*
Zone V:
Proximal to the carpal tunnel in the forearm. Involves FDS, FDP, FPL, and often median and ulnar nerves, and radial/ulnar arteries.
The patient's laceration was located on the volar distal forearm, proximal to the wrist crease, consistent with a Zone V flexor tendon injury involving the FPL, FDP to index and middle fingers, and FDS to index and middle fingers, alongside the median nerve.
Surgical Technique / Intervention
Patient Positioning and Anesthesia
The patient was positioned supine on the operating table. The left arm was abducted onto a specialized hand table, allowing full access to the volar forearm and wrist. A pneumatic tourniquet was applied to the upper arm. General anesthesia was induced, supplemented with a regional axillary block for post-operative pain management.
Approach and Exploration
The existing laceration was extended proximally and distally in a curvilinear fashion, avoiding perpendicular extensions that could lead to scar contracture. This provided wide exposure of the underlying neurovascular bundles and flexor tendons. The wound was meticulously irrigated. Under loupe magnification (2.5x), a systematic exploration was performed to identify all injured structures.
- Initial Findings: Profuse bleeding from small vessels was controlled with bipolar cautery. A complete transection of the median nerve was identified, with retraction of both proximal and distal stumps. The flexor pollicis longus (FPL), flexor digitorum profundus (FDP) to the index and middle fingers, and flexor digitorum superficialis (FDS) to the index and middle fingers were all completely lacerated. The radial and ulnar arteries were found to be intact.
Repair Sequence
The general principle for repairing multiple structures in the hand is to prioritize vascular repair if present, followed by nerve, and then tendon. In this case, with intact vascularity, nerve and tendon repair were performed. Often, tendons are repaired first to restore anatomical relationships, then the nerve. However, if the nerve stumps are difficult to approximate, it might be beneficial to first identify and mobilize them.
-
Tendon Repair:
- The proximal and distal ends of each lacerated tendon (FPL, FDP index/middle, FDS index/middle) were identified. Retrieval of retracted proximal stumps often required careful distal milking of the forearm or utilizing a small tendon grabber.
- Each tendon was repaired using a modified Kessler core suture technique (3-0 or 4-0 non-absorbable braided polyester suture), providing robust strength. This was reinforced with a circumferential epitendinous repair (6-0 non-absorbable monofilament suture) to improve strength, reduce gapping, and create a smoother gliding surface.
- Care was taken to ensure correct anatomical orientation and tension of each tendon, testing smooth gliding through the tendon sheath.
-
Nerve Repair (Median Nerve):
- The proximal and distal stumps of the median nerve were identified. Both ends were sharply debrided back to healthy, unscarred fascicular tissue using a fresh razor blade on a tongue depressor.
- Under operating microscope magnification (10-15x), the nerve stumps were coapted. Due to the relatively clean laceration and minimal retraction, a primary, tension-free epineurial repair was feasible.
-
Eight to ten interrupted 8-0 non-absorbable monofilament Nylon sutures were placed circumferentially through the epineurium, ensuring precise alignment of the nerve fascicles and avoiding rotation. The goal was accurate apposition with no tension or gapping at the repair site.
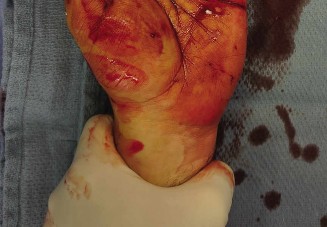
- The repair site was inspected for any signs of tension or misalignment. The wrist was gently flexed to approximately 20 degrees to further reduce any potential strain on the repair.
Wound Closure
After achieving meticulous hemostasis, the wound was copiously irrigated with sterile saline. The subcutaneous tissue was closed with absorbable sutures. The skin was closed with interrupted 5-0 non-absorbable monofilament sutures. A sterile, non-adherent dressing was applied.
Post-Operative Immobilization
A bulky soft dressing was applied, followed by a dorsal plaster splint that held the wrist in 20-30 degrees of flexion and the MCP joints in 70-90 degrees of flexion with the IP joints in extension (Duran protocol equivalent for flexor tendon protection), to offload tension on both the nerve and tendon repairs.
Post-Operative Protocol & Rehabilitation
Rehabilitation following combined median nerve and flexor tendon repair is a complex, prolonged, and multidisciplinary process involving the orthopedic surgeon and a specialized hand therapist. The protocol balances protection of the delicate repairs with the need for early, controlled motion to prevent stiffness and optimize functional recovery.
Phase 1: Immobilization and Protection (Weeks 0-3/4)
- Goals: Protect nerve and tendon repairs, minimize swelling, reduce pain.
- Immobilization: The dorsal plaster splint, maintaining the wrist in 20-30 degrees of flexion, MCPs in 70-90 degrees flexion, and IP joints in extension, is worn continuously. For nerve repair, wrist flexion is crucial to minimize tension on the coaptation site.
-
Activities:
- Strict adherence to splinting.
- Elevation of the hand to reduce edema.
- Gentle, passive range of motion (PROM) for uninvolved joints (shoulder, elbow, uninjured digits).
- Active extension of the fingers to the splint (Kleinert/Duran concepts adapted for controlled motion).
- Pain management (analgesics).
- Regular neurovascular checks.
Phase 2: Controlled Active Motion & Early Nerve Regeneration Monitoring (Weeks 3/4-6)
- Goals: Initiate gentle active range of motion for tendons, protect nerve, begin sensory re-education.
- Splinting: The dorsal splint is progressively adjusted or replaced with a custom thermoplastic splint. Wrist flexion is gradually reduced.
-
Activities:
- Tendons: Under the guidance of a hand therapist, controlled active flexion and passive extension exercises for the repaired flexor tendons are initiated. Modified Duran or Kleinert protocols are commonly employed. Care is taken to avoid forceful gripping or full active extension against resistance.
- Nerve: Continue to protect the median nerve. Gentle, passive wrist extension to neutral, then gradually to minimal extension.
- Sensory Re-education (Early): Desensitization techniques for hypersensitive areas around the incision. Passive sensory input (different textures).
- Tinel's Sign: Serial assessment of Tinel's sign (light percussion over the nerve path) to track the regenerating axon front. This provides an early indication of nerve regeneration, typically advancing at approximately 1 mm per day or 1 inch (2.5 cm) per month. For a distal forearm repair, the progression towards the thenar eminence and digits is closely monitored.
Phase 3: Progressive Strengthening & Advanced Nerve Regeneration Monitoring (Weeks 6-12)
- Goals: Restore full range of motion, increase strength, continue nerve recovery monitoring.
- Splinting: Splint use is gradually weaned, primarily for protection during sleep or strenuous activities.
-
Activities:
- Tendons: Progressive strengthening exercises for grip and pinch, gradually increasing resistance. Functional activities are incorporated.
-
Nerve:
- Sensory Assessment: Regular quantitative sensory testing (e.g., Semmes-Weinstein monofilament testing, static and moving two-point discrimination) in the median nerve distribution. Improvement from absent sensation to protective sensation (e.g., 6.65 monofilament) is a primary benchmark, followed by return of 2-point discrimination (initially >15mm, aiming for <10mm).
- Motor Assessment: Manual muscle testing of median-innervated muscles (APB, opponens pollicis, FPL, FDP/FDS index/middle). Early muscle flicker and then progressive strength return are monitored.
-
Nerve Regeneration Rate:
As previously noted, the typical rate of nerve regeneration is
approximately 1 mm per day, or 1 inch (2.5 cm) per month
. This is the critical answer to the case title. For a repair in the distal forearm, a distance of approximately 10-15 cm to the thenar muscles (APB/Opponens) means motor return might be expected around 4-6 months, while sensory return to the fingertips (a longer distance of 20-25 cm) might take 8-10 months, with full maturation taking 18-24 months. This rate is influenced by numerous factors.
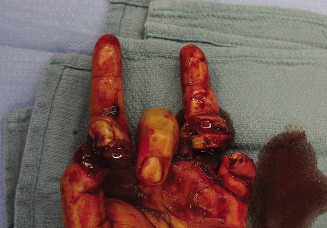
-
Factors influencing regeneration rate and outcome:
- Patient Age: Younger patients generally have better regenerative capacity.
- Type of Injury: Clean transections (as in this case) tend to have better outcomes than crush or avulsion injuries.
- Level of Injury: More distal injuries have shorter distances for axons to regenerate, leading to faster reinnervation of target organs. Proximal injuries carry a poorer prognosis.
- Surgical Technique: Tension-free, anatomically accurate repair under magnification is paramount.
- Gap Length: Longer nerve gaps requiring grafting have poorer outcomes than primary repairs.
- Patient Comorbidities: Diabetes, smoking, and peripheral vascular disease can impair nerve regeneration.
- Rehabilitation Adherence: Proper sensory re-education and motor retraining are crucial for integrating new nerve signals.
- Electromyography (EMG) and Nerve Conduction Studies (NCS): These may be considered at 3-6 months post-operatively if clinical recovery is not progressing as anticipated, to assess for reinnervation potentials or to rule out a block to regeneration (e.g., neuroma in continuity).
Phase 4: Functional Recovery & Long-Term Monitoring (Months 3-24+)
- Goals: Maximize functional return, return to work/activities, manage residual deficits.
- Activities: Continuation of strengthening, endurance, and fine motor dexterity exercises. Work-specific training.
- Outcome: While protective sensation is often achieved, full return of two-point discrimination and normal motor strength can be elusive. Patients frequently have some degree of residual sensory deficit (e.g., diminished two-point discrimination) and mild motor weakness. The patient in this case, being an electrician, would require excellent fine motor control and sensation. Long-term follow-up for up to 2 years is essential to assess maximal recovery.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Urgent Definitive Repair: For sharp transections of nerves and tendons, prompt surgical exploration and primary repair (ideally within hours, certainly within 72 hours for nerves) are paramount for optimal outcomes. Delay leads to retraction, fibrosis, and poorer prognosis.
- Magnification is Non-Negotiable: Nerve repair must be performed under adequate magnification (loupes at minimum, operating microscope preferably) to ensure precise epineurial or fascicular coaptation and avoid rotation or tension.
- Tension-Free Repair: This is the cardinal rule for both nerve and tendon repairs. Excessive tension leads to failure, gapping, and poor regeneration. Mobilize nerve stumps, flex joints (e.g., wrist for median nerve), or consider nerve grafting for significant gaps (>2-3 cm for median nerve).
- Anatomic Reduction & Alignment: Critical for both tendons and nerves. For nerves, ensuring proper fascicular orientation, particularly in mixed nerves like the median nerve, optimizes reinnervation patterns. For tendons, correct tensioning is vital to prevent lag or excess tightness.
- Multidisciplinary Team Approach: A specialized hand therapist is an indispensable partner in post-operative rehabilitation. Their expertise in controlled motion protocols, sensory re-education, and progressive strengthening is crucial for maximizing functional recovery.
- Realistic Patient Expectations: Counsel patients that full recovery, especially of fine discriminative sensation, is rare after nerve transection and repair. The goal is often protective sensation and functional motor recovery.
- Thorough Exploration: Always assume concomitant injuries in sharp trauma. A single laceration can involve multiple nerves, tendons, and vessels. Systematic identification of all structures is essential.
Pitfalls
- Missed Injuries: Inadequate wound exploration or rushing the assessment can lead to missed partial or complete nerve/tendon lacerations, resulting in persistent deficits and requiring revision surgery.
- Inadequate Debridement: Poor debridement of non-viable tissue in the wound can lead to infection and impaired healing of delicate repairs.
- Excessive Tension on Repair: The most common technical error leading to repair failure. Results in gapping, poor healing, or complete disruption.
-
Poor Surgical Technique:
- Inaccurate coaptation of nerve ends (e.g., rotation, inclusion of epineurium in fascicular repair).
- "Fish-mouthing" of nerve stumps, where the cut ends are not flush.
- Inappropriate suture material or technique (e.g., too many sutures causing fibrosis, too few causing gapping).
- Inadequate tendon core suture leading to pull-out.
-
Inappropriate Post-Operative Management:
- Premature mobilization leading to re-rupture of tendons or disruption of nerve repair.
- Prolonged immobilization leading to joint stiffness, adhesion formation, and poorer functional outcomes.
- Lack of specialized hand therapy.
- Infection: As with any open injury and surgical intervention, infection remains a significant risk, which can severely compromise healing and functional outcome.
- Neuroma Formation: A common complication after nerve injury, often presenting as a painful mass at the repair site, sometimes requiring further intervention.
- Delayed Recognition of Complications: Failure to monitor for signs of re-rupture (tendons), persistent sensory/motor deficits (nerves), or progression of infection can lead to suboptimal long-term results.
- Poor Patient Adherence: Non-compliance with splinting protocols or rehabilitation exercises is a major impediment to recovery.
