Introduction & Epidemiology
Radial polydactyly, or thumb duplication, is the most common congenital anomaly of the hand, with an incidence estimated at 1 in 3,000 live births. While frequently an isolated anomaly, it can also be associated with various genetic syndromes, including Fanconi anemia, Holt-Oram syndrome, VACTERL association, and Diamond-Blackfan anemia, necessitating a thorough systemic evaluation. The primary goal of surgical management is the creation of a single, stable, mobile, sensate, and aesthetically acceptable thumb that allows for effective prehension and opposition.
The universally accepted classification system for thumb duplication was introduced by Wassel in 1969, categorizing duplications based on the level of skeletal involvement:
- Type I: Bifid distal phalanx (rare)
- Type II: Duplication of the distal phalanx (most common, ~43% of cases)
- Type III: Bifid proximal phalanx
- Type IV: Duplication of the proximal phalanx (second most common, ~20% of cases)
- Type V: Bifid metacarpal
- Type VI: Duplication of the metacarpal
- Type VII: Triphalangism (thumb with three phalanges)
This discussion specifically focuses on Wassel Type IV thumb duplication, which involves duplication at the level of the proximal phalanx, with two distinct proximal phalanges articulating with a single metacarpal head. This presents unique surgical challenges due to the involvement of the metacarpophalangeal (MP) joint and the complex interplay of tendons, ligaments, and neurovascular structures around this critical articulation.
Surgical Anatomy & Biomechanics
Wassel Type IV thumb duplication presents a complex anatomical challenge, as the anomaly occurs at the metacarpophalangeal joint, a critical fulcrum for thumb function. A detailed understanding of the skeletal, ligamentous, tendinous, and neurovascular aberrations is paramount for successful reconstruction.
Skeletal Anatomy
At the level of Type IV duplication, two proximal phalanges articulate with a single, often broadened or bifid, metacarpal head.
*
Metacarpal:
The first metacarpal is typically broad distally, sometimes exhibiting a central notch or a partial sagittal septum, indicating an incomplete duplication. The epiphyseal plate of the metacarpal head may be distorted or duplicated, which has implications for future growth.
*
Proximal Phalanges:
Two distinct proximal phalanges are present. They often differ in size, shape, and articular congruity. One phalanx (commonly the ulnar) may be larger and better formed, while the other (radial) may be hypoplastic, angulated, or exhibit less developed articular surfaces. The epiphyses of these phalanges can also be asymmetric or irregular.
*
Distal Phalanges:
Each proximal phalanx typically articulates with its own distal phalanx, which may also show varying degrees of development.
Ligamentous Structures
The collateral ligaments of the duplicated MP joint are usually anomalous.
*
Radial and Ulnar Collateral Ligaments (RCL, UCL):
These are often present for each duplicated joint, but they may be attenuated, absent, or aberrantly inserted. A common finding is shared or interconnected collateral ligaments between the two components. The primary goal is to centralize and reconstruct a robust collateral ligament system for the single, reconstructed MP joint.
*
Volar Plate:
The volar plate may be duplicated, shared, or attenuated, contributing to joint instability. Reconstruction may require capsular repair or advancement.
Tendon Anatomy
The musculotendinous units of the thumb are crucial for motion and stability, and their anomalies significantly complicate surgical planning.
*
Extensor Pollicis Longus (EPL) and Extensor Pollicis Brevis (EPB):
The extensor mechanism is highly variable. The EPL may insert into one component, both, or bifurcate. The EPB may also be duplicated or have an aberrant insertion. Often, one extensor slip is stronger or better positioned. The strategy typically involves centralizing the most robust extensor tendon slip onto the retained or reconstructed thumb axis.
*
Flexor Pollicis Longus (FPL):
The FPL is usually a single tendon inserting into one of the duplicated distal phalanges, or it may bifurcate to insert into both. Its course and insertion need careful assessment to ensure smooth gliding and effective flexion post-reconstruction. Occasionally, a single FPL may attach predominantly to the smaller, less functional component, necessitating careful re-routing or re-insertion.
*
Intrinsic Muscles (Abductor Pollicis Brevis (APB), Flexor Pollicis Brevis (FPB), Adductor Pollicis):
These muscles are critical for opposition, pinch strength, and MP joint stability. They are frequently anomalous, with insertions into one or both components, or into soft tissue adjacent to the joint. The presence of well-developed intrinsic musculature is often a determining factor in selecting which component to preserve. The adductor pollicis may have an aberrant insertion, potentially contributing to adduction contracture or instability. Rebalancing and re-inserting these intrinsic muscles to the retained thumb is a cornerstone of functional reconstruction.
Neurovascular Bundles
- Digital Nerves: Typically, there are two distinct neurovascular bundles for each duplicated digit. However, in Wassel Type IV, the nerves and vessels may be shared, intimately associated with the duplicated components, or present as a single bundle that bifurcates distally. Careful identification and preservation of these bundles are paramount to ensure sensibility of the reconstructed thumb. The neurovascular supply to the component planned for retention must be meticulously protected.
- Arterial Supply: Similarly, the digital arteries follow the nerves, and their aberrant course or sharing must be anticipated.
Biomechanics
The biomechanical consequences of Type IV duplication include:
*
Instability:
Lack of a single, stable MP joint axis results in inherent instability, particularly in lateral pinch.
*
Weakness:
The absence of properly functioning intrinsic muscles, coupled with an inefficient flexor/extensor mechanism, leads to reduced pinch and grip strength.
*
Deformity:
Progressive angular deformity (e.g., clinodactyly, radial or ulnar deviation) is common due to asymmetric growth, unbalanced muscle pull, and inadequate ligamentous support.
*
Impaired Opposition:
The abnormal axis and muscle insertions hinder effective opposition, impacting fine motor skills.
The goal of surgical reconstruction is to create a single thumb with a stable MP joint, proper alignment, sufficient range of motion, and balanced muscle power, enabling functional opposition and pinch. This often involves careful consideration of the specific anomalies to select the best component for reconstruction and to utilize redundant tissues from the resected component for soft tissue augmentation.
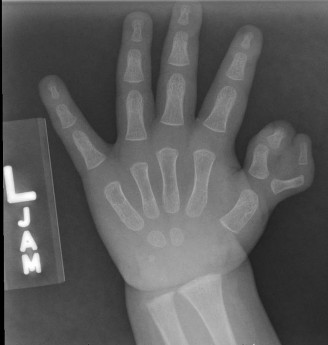
Indications & Contraindications
The decision for operative intervention in Wassel Type IV thumb duplication is primarily driven by functional impairment and the potential for long-term disability, alongside aesthetic concerns. Early intervention is generally preferred to facilitate normal development of pinch and grasp.
Operative Indications
| Indication Type | Description | Wassel Type IV Relevance |
|---|---|---|
| Functional Impairment | Inability to perform effective pinch and grasp due to instability, malalignment, or lack of opposition. Impaired tactile sensation due to splaying or poor definition. | Primary Indication: Type IV duplications inherently compromise MP joint stability and muscle balance, severely impairing pinch and the development of a functional thumb. Surgical reconstruction aims to establish a stable, mobile joint. |
| Cosmetic Concerns | The presence of a duplicated, often smaller or misshapen, digit which is aesthetically undesirable to the family or, later, to the child. | Aesthetically, duplicated thumbs are noticeable. While secondary to function, cosmesis is a valid concern for Type IV, especially given the prominent location of the deformity. |
| Progressive Deformity | Worsening angular deformity (clinodactyly, radial or ulnar deviation) or increasing joint instability due to unbalanced growth or muscle pull. | Common in Type IV due to asymmetric growth of the duplicated epiphyses and unbalanced muscle forces. Early surgery can prevent severe fixed deformities. |
| Syndactyly | Presence of webbing between the duplicated thumbs, further restricting motion and growth. | May coexist with Type IV, requiring comprehensive surgical planning to address both duplication and web space. |
| Age-Appropriate Timing | Optimal surgical window typically between 6-18 months of age, allowing for adequate tissue development for surgery while minimizing psychological impact and allowing for normal motor skill development. | Crucial for Type IV. Early surgery allows for optimal molding of developing bone and soft tissues, promoting better functional outcomes and adaptation during critical developmental periods. |
Non-Operative Indications / Contraindications
| Indication Type | Description | Wassel Type IV Relevance |
|---|---|---|
| Minor Duplication (No Deficit) | Extremely rare for Wassel Type IV. Applies to cases with minimal, asymptomatic accessory digits that do not interfere with function and are not cosmetically bothersome. | Not applicable for Type IV. Type IV almost invariably presents with significant functional and/or cosmetic issues requiring intervention. Rarely observed as minor. |
| Severe Comorbidities | Medical conditions (e.g., severe cardiac anomalies, severe prematurity, uncontrolled systemic diseases) that place the child at unacceptably high anesthetic or surgical risk. | In these cases, surgery may be delayed or contraindicated until the child's medical status stabilizes or improves. A multidisciplinary approach is essential. |
| Active Infection | Local or systemic infection that would significantly increase the risk of surgical complications. | Surgery should be postponed until the infection is completely resolved. |
| Unrealistic Expectations | Parents/guardians with unrealistic expectations regarding the functional or cosmetic outcome of surgery, despite thorough pre-operative counseling. | Requires extensive counseling to ensure understanding of potential limitations and realistic outcomes. |
| Patient/Parental Refusal | If, after comprehensive counseling, the family declines surgical intervention. | While rare given the functional implications of Type IV, the decision ultimately rests with the legal guardians after informed consent. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful surgical reconstruction for Wassel Type IV thumb duplication, aiming to optimize functional and aesthetic outcomes while minimizing complications.
Clinical Assessment
-
Detailed History:
- Family History: Inquire about congenital anomalies, especially hand deformities, to assess for genetic predisposition.
- Syndromic Associations: Specifically ask about cardiac, renal, hematologic (e.g., Fanconi anemia), and upper limb anomalies (e.g., Holt-Oram syndrome, VACTERL), as these require systemic workup before elective surgery.
- Perinatal History: Any complications during pregnancy or delivery.
-
Physical Examination:
- General Assessment: Evaluate overall health, nutritional status, and screen for syndromic features.
-
Hand Examination:
- Visual Inspection: Note the relative size, alignment, and morphology of the duplicated components. Identify any syndactyly, webbing, or skin creases. Assess for angular deformities (clinodactyly, radial/ulnar deviation) or rotational deformities.
- Palpation: Assess for bone texture, joint stability, and the presence of underlying skeletal abnormalities.
- Range of Motion (ROM): Actively and passively assess the MP and IP joints of both duplicated components. Note any stiffness, hypermobility, or pain (in older children).
- Sensibility: While challenging in infants, gross assessment of withdrawal reflex or response to light touch can be performed. In older children, two-point discrimination and Semmes-Weinstein monofilament testing can be used.
- Motor Function: Assess for intrinsic and extrinsic muscle function. Observe grasp, pinch (tip-to-tip, key pinch), and opposition patterns relative to age-appropriate norms. Identify which component demonstrates superior motor control or intrinsic muscle development.
- Neurovascular Status: Assess capillary refill and skin color of both components.
Imaging Studies
-
Radiographs:
- Standard AP and Lateral Views: Essential for Wassel classification, detailed assessment of the skeletal anatomy (number of phalanges, metacarpals), relative size of the components, joint congruity, epiphyseal development, and any angular deformities. These views are critical for selecting the component to retain and for planning osteotomies.
- Oblique Views: Can provide additional insights into complex joint architecture.
- Contralateral Hand Radiographs: Useful for comparison if the contralateral hand is normal, or to assess for bilateral involvement.
- Dynamic Stress Views (rarely needed for Type IV): May be considered in older children to assess ligamentous stability if clinical examination is inconclusive, but usually less critical than in other Wassel types.
- Advanced Imaging (CT/MRI): Generally not required for routine Wassel Type IV cases. May be considered in extremely complex situations, particularly if there is significant syndactyly, severe bone deformity, or suspicion of more extensive soft tissue involvement (e.g., for detailed mapping of neurovascular structures or tendon origins/insertions), or if associated with other complex hand anomalies.
Surgical Timing
- The optimal surgical window for Wassel Type IV is generally between 6 and 18 months of age .
- Rationale: At this age, the hand structures are sufficiently developed for precise dissection and reconstruction. The child is old enough to tolerate general anesthesia well, but young enough to avoid significant psychological impact and to adapt readily to the reconstructed thumb's motor patterns during crucial developmental stages for pinch and grasp. Delaying surgery beyond 2 years can lead to more established compensatory patterns and potentially less favorable long-term functional outcomes.
Pre-Operative Markings
Before sterile draping, with the patient awake if possible (or immediately after induction), the surgeon should:
* Mark the
planned incision lines
(e.g., racquet or dorsal curvilinear) to ensure adequate skin envelope and facilitate soft tissue redistribution.
* Identify and mark the
axis of the proposed new thumb
, considering the relative contribution of each duplicated component.
* Mark the
neurovascular bundles
if they are clearly palpable or visualized with a Doppler, though their exact course will be identified intraoperatively.
* Outline the
areas of intended bone resection
.
Patient Positioning and Setup
- Position: Supine position on the operating table.
- Arm Preparation: The affected upper extremity is placed on a dedicated hand table or arm board.
- Tourniquet: An upper arm pneumatic tourniquet is applied to maintain a bloodless field.
- Magnification: Loupe magnification (e.g., 2.5x to 4.5x) is essential for meticulous dissection of neurovascular structures, tendons, and joint capsule.
- Instrumentation: Fine hand instruments, microsurgical instruments (if necessary for neurovascular repair), K-wire driver, and small osteotomes are required.
- Sterile Prep and Drape: Standard sterile preparation and draping of the entire upper extremity to allow full range of motion during the procedure.
Detailed Surgical Approach / Technique
Surgical reconstruction for Wassel Type IV thumb duplication primarily involves ablating one component and reconstructing the remaining thumb or, less commonly now, utilizing a Bilhaut-Cloquet type procedure. The choice between these two approaches depends on the morphology of the duplication, with a growing preference for component ablation and reconstruction (i.e., preserving the better component and augmenting it with tissues from the ablated component).
Core Principles for Wassel Type IV Reconstruction
Regardless of the specific technique, the following principles guide reconstruction:
1.
Preservation of Sensibility:
Meticulous dissection and protection of neurovascular bundles.
2.
Centralization of the Thumb Axis:
Creating a single, well-aligned thumb.
3.
Achievement of Stability:
Reconstructing a stable MP joint.
4.
Maintenance of Mobility:
Ensuring good range of motion at the MP and IP joints.
5.
Rebalancing of Musculature:
Ensuring effective flexion, extension, opposition, and pinch.
6.
Optimal Skin Coverage:
Achieving a good skin envelope without tension or dog ears.
Selection of the Retained Component
The decision of which component to retain is crucial. Generally, the component with the following characteristics is preferred:
*
Larger size and better overall development.
*
More congruent articular surface at the MP joint.
*
Better intrinsic muscle insertions (APB, FPB, Adductor Pollicis).
Often, the ulnar component demonstrates superior intrinsic muscle attachments and better alignment for opposition.
*
Better alignment:
Less angular deformity.
*
More robust neurovascular supply.
In Wassel Type IV, the ulnar component is often chosen as it tends to have better intrinsic muscle development and a more favorable axis for opposition.
Surgical Steps (Component Ablation and Reconstruction – Current Preferred Approach)
1. Incision and Initial Dissection
- Skin Incision: A dorsal curvilinear or racquet-shaped incision is typically used. The racquet incision outlines the radial component for excision while providing ample skin for closure and often includes a dorsal-ulnar extension to facilitate access for soft tissue centralization. A Y-V plasty may also be incorporated to provide extra skin for web space deepening or to manage skin deficiencies.
- Subcutaneous Dissection: Carefully elevate skin flaps, identifying and protecting the dorsal veins. The neurovascular bundles for both duplicated thumbs must be identified. The neurovascular bundle supplying the component to be resected is dissected proximally. The nerve may be preserved and coapted to its counterpart in the retained digit if a nerve graft is not required, or the radial-sided nerve branch can be identified, protected, and potentially advanced to the ulnar side of the retained digit to enhance sensibility if needed. The vessels to the ablated digit are ligated. The neurovascular bundle to the retained digit must be meticulously protected throughout the procedure.
2. Soft Tissue Dissection and Tendon Management
- Extensor Mechanism: Identify the extensor pollicis longus (EPL) and extensor pollicis brevis (EPB) tendons. If duplicated, the stronger, more centrally located slip is preserved and centralized on the retained thumb. Redundant slips are released from the ablated component and may be used for soft tissue reconstruction (e.g., tenodesis) if needed.
- Flexor Pollicis Longus (FPL): The FPL is usually common. Ensure it has a clear, unhindered path to the retained distal phalanx. If it bifurcates, the slip to the ablated component is divided.
- Intrinsic Muscles: This is a critical step. Dissect the abductor pollicis brevis (APB) and flexor pollicis brevis (FPB) insertions. If they insert into the ablated component, they are carefully detached with a small piece of periosteum/bone (if possible) and reinserted to the base of the proximal phalanx of the retained component in an anatomically correct position to enhance opposition and stability. The adductor pollicis attachment is similarly assessed and rebalanced. This step is crucial for achieving a stable and functional MP joint.
3. Bone Resection and Joint Reconstruction
- Ablation of Redundant Component: The decision has already been made regarding which component to ablate (usually the smaller, radial, or less functional digit). The entire metacarpophalangeal joint of this component, including its proximal phalanx and distal phalanx, is excised. A small portion of the metacarpal head may also be resected if it is significantly broadened or bifid, aiming to create a single, well-contoured metacarpal head for the retained thumb. Care is taken to preserve the growth plate of the retained metacarpal.
- Metacarpal Head Contouring: If the first metacarpal head is significantly broadened or bifid, it is carefully osteotomized and reshaped to provide a single, rounded articular surface for the retained proximal phalanx. This may involve resecting a small sagittal wedge of bone.
-
MP Joint Reconstruction:
- Collateral Ligaments: The preserved collateral ligaments (often from the ulnar side of the retained thumb and salvaged from the ablated component) are centralized and tightened to create a stable MP joint. If laxity persists, the capsular tissue and tendinous slips (e.g., from the extensor mechanism) from the ablated component can be used for augmentation. The goal is to create a functional check-rein mechanism.
- Volar Plate: The volar plate is repaired or advanced to enhance volar stability.
4. K-wire Fixation and Soft Tissue Closure
- K-wire Fixation: After achieving optimal MP joint alignment (neutral rotation, slight flexion, and abduction), smooth Kirschner wires (typically 0.028" or 0.035") are inserted. Usually, two K-wires are placed: one across the MP joint from the proximal phalanx into the metacarpal to maintain stability, and potentially another across the interphalangeal (IP) joint if there is concern for instability or if a corrective osteotomy of the phalanx was performed. The wires are cut flush with the skin or bent and buried to minimize irritation. Ensure wires do not cross or damage the growth plate unnecessarily.
- Skin Closure: The skin flaps are meticulously closed. Any redundant skin or dog ears are carefully trimmed. A Z-plasty may be performed at the web space if there is any syndactyly or to deepen the web space. The goal is a tension-free closure with a good aesthetic result.
Alternative: Bilhaut-Cloquet Procedure (Less Common for Type IV)
While classically described for Wassel Type IV, the Bilhaut-Cloquet procedure involves creating a single digit by longitudinally fusing the radial and ulnar halves of the duplicated digits (after resecting the redundant central portions).
*
Steps:
1. Longitudinal skin incision.
2. Careful dissection of neurovascular bundles and tendons.
3. Resection of the opposing halves of the duplicated proximal phalanges and distal phalanges. This involves precise osteotomies to create congruent bone surfaces.
4. Fusion of the remaining halves, creating a single, broader phalanx. This often results in a wider, cosmetically less appealing thumb.
5. Centralization of tendons and ligamentous reconstruction.
6. K-wire fixation across the new MP and IP joints.
*
Disadvantages:
Often results in a broad, "sausage-shaped" thumb, reduced motion (due to fusion), and potential for epiphyseal damage impacting growth. For Wassel Type IV, it specifically involves fusing at the MP joint level. Due to these drawbacks, component ablation and reconstruction (as described above) is generally preferred for Wassel Type IV, as it allows for better preservation of motion, creation of a more normal-sized thumb, and better long-term stability.
Complications & Management
Despite meticulous surgical technique, complications can arise following reconstruction for Wassel Type IV thumb duplication. Early recognition and appropriate management are crucial for optimizing long-term outcomes.
| Complication | Incidence (approx.) | Management / Salvage Strategy |
|---|---|---|
| MP Joint Instability | 10-30% (Lateral deviation, laxity) | Early: Prolonged immobilization, bracing. Late: Ligamentous reconstruction (e.g., using extensor tendon slips, tenodesis), capsulorrhaphy, corrective osteotomy of the proximal phalanx or metacarpal, intrinsic muscle rebalancing/transfer. |
| MP Joint Stiffness / Reduced ROM | 5-15% | Early: Aggressive occupational/physical therapy, serial casting. Late: Tenolysis, capsulotomy, arthrolysis. May be challenging if related to excessive scarring or heterotopic ossification. |
| Angular Deformity | 5-20% (Radial or ulnar deviation, clinodactyly) | Early: K-wire revision, casting. Late: Corrective osteotomy (closing wedge, opening wedge, dome osteotomy) of the proximal phalanx or metacarpal, combined with physeal arrest (epiphysiodesis) if growth plate issues are contributing, or soft tissue release/tightening. |
| Growth Plate Arrest/Deformity | <5% (typically minor) | Close radiographic monitoring. Corrective osteotomy if significant angular deformity develops. Reassurance for minor shortening if functional. Rarely requires further intervention if minor. |
| Neurovascular Injury / Sensory Deficit | <1% (Transient paresthesia more common) | Intraoperative: Micro-surgical repair. Post-op: Observation for transient deficits. Neurolysis or nerve grafting in severe, persistent cases (rare). Careful dissection is the best prevention. |
| Infection | 1-5% (Superficial vs. Deep) | Superficial: Oral antibiotics, local wound care. Deep (Osteomyelitis/Septic Arthritis): IV antibiotics, surgical debridement, possibly K-wire removal. |
| Nonunion / Malunion | <5% (More common with Bilhaut-Cloquet, less with ablation) | Nonunion: Revision surgery with bone grafting and rigid internal fixation. Malunion: Corrective osteotomy after appropriate healing. |
| Recurrence of Deformity | 5-10% (Especially angular deformities) | Often related to growth and development. Requires careful long-term follow-up. Salvage involves repeat osteotomy, soft tissue balancing, or re-doing ligamentous reconstruction. |
| Cosmetic Dissatisfaction | Variable, subjective | Scar revision, debulking procedures for a wide thumb, revision osteotomy for improved alignment. Thorough pre-operative counseling about realistic expectations is crucial. |
| Web Space Contracture | 5-10% | Z-plasty or four-flap Z-plasty for web space deepening. Skin grafting if significant tissue loss or scarring. Prevention during initial surgery by careful skin flap design. |
Discussion of Key Complications
- Instability and Stiffness: These are the most common long-term functional problems. Instability often manifests as lateral deviation (ulnar or radial) during pinch. Stiffness can occur due to extensive soft tissue dissection, prolonged immobilization, or inflammatory response. Meticulous soft tissue handling, precise ligamentous reconstruction, and early, guided rehabilitation are crucial preventative measures.
- Angular Deformity: Often a consequence of asymmetric growth from uncorrected epiphyseal abnormalities, unbalanced muscle pull, or inadequate initial correction. Long-term follow-up through skeletal maturity is essential to monitor for this. Corrective osteotomies are the primary salvage strategy.
- Growth Plate Issues: While K-wires across epiphyses can theoretically cause growth arrest, the use of small-diameter smooth wires and prompt removal minimizes this risk. Significant growth arrest is rare, but asymmetric growth can contribute to angular deformities.
- Neurovascular Injury: Fortunately rare with proper magnification and careful dissection. Any signs of neurovascular compromise post-operatively (pallor, coolness, delayed capillary refill, severe pain) demand immediate investigation and intervention.
- Recurrence: The developing nature of a child's hand means that the initial correction can be altered by growth. Regular follow-up allows for early detection and intervention for any developing issues.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an integral component of the overall management plan for Wassel Type IV thumb duplication, aimed at preserving surgical correction, preventing stiffness, and optimizing functional recovery. The protocol must be tailored to the child's age, the specific surgical procedure performed, and the stability achieved during surgery.
Phase 1: Immobilization and Protection (0-4 to 6 weeks)
-
Immobilization:
- Immediately post-operatively, a short arm thumb spica cast or custom splint is applied. This cast typically includes the forearm, wrist, and thumb, leaving the interphalangeal (IP) joint of the thumb and other fingers free.
- Positioning: The thumb is immobilized in a position of slight flexion (15-20 degrees) at the MP joint, slight abduction, and neutral rotation. This position minimizes tension on the repair, protects the osteotomy/fusion site, and helps maintain the reconstructed web space. The IP joint is often immobilized, especially if an IP fusion or osteotomy was performed, or if it contributes to overall stability.
-
Cast/Splint Care:
- Parents are educated on cast care, including keeping it dry and clean, and monitoring for signs of circulatory compromise (color changes, swelling, excessive pain) or skin irritation.
-
Pin Care (if K-wires are exposed):
- If K-wires are left exposed, meticulous pin site care is crucial to prevent infection. This typically involves daily cleaning with sterile saline or antiseptic solution as per institutional protocol.
- Monitoring: Regular clinical follow-up is necessary to assess wound healing, cast integrity, and monitor for any signs of complications (e.g., infection, nerve compromise, vascular compromise).
- Duration: The immobilization period generally lasts for 4 to 6 weeks , or until radiographic evidence of adequate bone healing is observed, and soft tissue stability is deemed sufficient.
Phase 2: Early Mobilization (4-6 weeks to 12 weeks)
- Pin Removal: K-wires are typically removed in clinic after 4-6 weeks, once radiographic healing is confirmed.
- Initiation of Therapy: Once immobilization devices and pins are removed, a structured hand therapy program, ideally supervised by an occupational or physical therapist specializing in pediatric hand conditions, is initiated.
-
Goals:
- Regain active and passive range of motion (ROM) of the thumb MP and IP joints.
- Maintain the reconstructed web space.
- Prevent joint stiffness and contractures.
- Facilitate normal motor skill development.
-
Exercises:
- Gentle Active ROM: Encouraging active flexion, extension, abduction, and opposition of the thumb. These exercises are often incorporated into play-based activities for children.
- Gentle Passive ROM: The therapist (and parents, under guidance) may perform gentle passive stretches to restore full ROM, avoiding forceful manipulation.
- Scar Management: Begin scar massage, desensitization, and potentially silicone sheeting or gel application to minimize hypertrophic scarring once the wound is completely healed.
- Custom Splinting: A removable custom splint (e.g., dynamic MP flexion splint or static night splint) may be fabricated to maintain gains in ROM, particularly at night, and to prevent contractures.
Phase 3: Strengthening and Functional Integration (12 weeks onwards)
-
Strengthening:
- Gradually introduce gentle strengthening exercises for the thumb, focusing on pinch and grip strength. This might involve using soft clay, small toys, or resistance bands adapted for pediatric use.
- Emphasis on specific muscle groups: abductor pollicis brevis (opposition), flexor pollicis longus (tip pinch), and adductor pollicis (key pinch).
-
Fine Motor Skills:
- Integrate the reconstructed thumb into age-appropriate fine motor activities, such as grasping small objects, buttoning, zipping, drawing, and manipulating toys.
- Focus on bimanual activities and coordinated hand use.
- Desensitization: Continue desensitization activities for the scar and any areas of altered sensation.
-
Long-Term Follow-up:
Regular clinical and radiographic follow-up is essential through skeletal maturity (up to 16-18 years) to monitor for:
- Development of angular deformities (due to asymmetric growth).
- Progression of joint instability or stiffness.
- Overall functional outcome and satisfaction.
- The need for revision surgery or further therapy.
The success of the surgical reconstruction is highly dependent on consistent and appropriate post-operative rehabilitation, which empowers the child to maximize the functional potential of their new thumb.
Summary of Key Literature / Guidelines
The management of Wassel Type IV thumb duplication has evolved significantly since the original classification, drawing upon foundational studies and contemporary reconstructive principles.
Foundational Literature:
- Wassel, H. D. (1969). The results of surgery for polydactyly of the thumb. A review of 57 cases. This seminal paper established the universally accepted classification system for radial polydactyly based on the level of skeletal duplication, guiding diagnosis and treatment planning. Wassel's work highlighted the commonality of Type IV (duplication of the proximal phalanx) and provided early insights into surgical outcomes.
- Manske, P. R., & McCarroll, H. R., Jr. (1983). Abductor pollicis longus reconstruction for congenital absence or hypoplasia of the thumb. While not specific to polydactyly, Manske's work on congenital thumb deficiencies underscores the critical importance of intrinsic muscle balance and its role in functional reconstruction, principles directly applicable to rebalancing muscles in duplicated thumbs.
- Goldfarb, C. A., Manske, P. R., & Dobyns, J. H. (2009). Classification and management of thumb duplication. This work, and many others by the St. Louis group, provides comprehensive insights into the evaluation and surgical decision-making for various Wassel types, emphasizing the importance of selecting the appropriate component and meticulously reconstructing soft tissue.
Current Trends and Controversies:
-
Ablation and Reconstruction vs. Bilhaut-Cloquet:
- Bilhaut-Cloquet (B-C) Procedure: Traditionally described for Wassel Type IV, this involves longitudinal fusion of opposing halves of the duplicated digits to create a single, centralized, albeit often broad, thumb. Early literature supported this for its perceived simplicity in centralizing bone.
- Component Ablation and Reconstruction (CAR): This technique involves ablating the smaller or less functional component (typically the radial component in Type IV) and using tissues (tendons, ligaments, skin) from the resected digit to augment the retained, better-formed component. The retained component's MP joint is reconstructed, often involving metacarpal head contouring, intrinsic muscle reinsertion, and collateral ligament repair.
- Current Consensus: CAR is now generally favored over the B-C procedure for Wassel Type IV. CAR typically yields a more aesthetically pleasing, narrower thumb with better long-term range of motion and fewer growth disturbances. The B-C procedure often results in a broad thumb with less mobility and a higher risk of physeal arrest or angular deformity from the fusion. Studies by Tsuchiya et al. and others have demonstrated superior functional and cosmetic results with CAR.
-
Timing of Surgery:
- Optimal Window: There is a strong consensus that surgery should be performed between 6 and 18 months of age . This allows sufficient tissue development for intricate surgery, minimizes the psychological impact on the child, and importantly, allows the child to integrate the newly reconstructed thumb into critical fine motor and prehensile skill development during infancy. Delaying beyond 2 years can result in established compensatory patterns and less favorable neurological adaptation.
-
Decision-Making for Component Selection:
-
The choice of which component to retain (typically the ulnar for Type IV) is critical. Factors guiding this decision include:
- Overall size and development.
- Articular congruity and stability of the MP joint.
- Presence and quality of intrinsic muscle insertions.
- Neurovascular supply.
- Axial alignment.
- Many studies show the ulnar component often has better intrinsic muscle attachments and a more favorable axis for opposition, contributing to better long-term function.
-
The choice of which component to retain (typically the ulnar for Type IV) is critical. Factors guiding this decision include:
-
Role of Advanced Imaging:
- While standard AP/Lateral radiographs remain the primary diagnostic tool, the increasing use of 3D CT reconstructions or MRI in select complex cases (e.g., severe syndactyly, unusual skeletal configurations, suspected vascular anomalies) can aid in precise pre-operative planning, although this is not routine for typical Wassel Type IV.
Guidelines and Principles:
- American Society for Surgery of the Hand (ASSH): Emphasizes a comprehensive approach to congenital hand conditions, focusing on early intervention, meticulous surgical technique, and long-term functional rehabilitation.
- International Federation of Societies for Surgery of the Hand (IFSSH): Promotes standardized classification and evidence-based treatment strategies for congenital anomalies.
- Key Surgical Tenets: Regardless of the specific Wassel type, the principles of creating a single, stable, mobile, sensate, and aesthetically acceptable thumb remain paramount. This involves careful dissection to preserve neurovascular structures, precise bone resections, robust ligamentous reconstruction, and meticulous rebalancing of the intrinsic and extrinsic musculature. Long-term follow-up through skeletal maturity is crucial to address potential growth-related deformities.
In conclusion, Wassel Type IV thumb duplication requires a detailed anatomical understanding and a carefully planned surgical approach, favoring component ablation and reconstruction over Bilhaut-Cloquet, performed within the optimal developmental window, to achieve the best functional and cosmetic outcomes. Continuous monitoring through skeletal maturity is vital for addressing potential growth-related complications.
